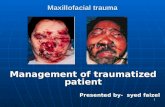
Maxillofacial trauma
-
Upload
vladimir-turner -
Category
Documents
-
view
33 -
download
5
description
Transcript of Maxillofacial trauma

Features of the maxillofacial area (MFA) Features of the maxillofacial area (MFA) injuries. Classification, debridement of injuries. Classification, debridement of
soft tissue wounds MFA. Nongunshot soft tissue wounds MFA. Nongunshot damage of the lower and upper jaws: damage of the lower and upper jaws:
Anatomy injury, pathogenesis, Anatomy injury, pathogenesis, classification, statistics, symptoms, classification, statistics, symptoms,
diagnosis, transportation diagnosis, transportation immobilization. Damage to the immobilization. Damage to the zygomatic bone, nasal bones in zygomatic bone, nasal bones in
peacetime: classification, incidence, peacetime: classification, incidence, clinical features, diagnosis and clinical features, diagnosis and
treatment.treatment.

2
Maxillofacial traumaMaxillofacial trauma
Management of traumatized patient

3
Organization of trauma servicesOrganization of trauma services
Pre-hospital care (field triage) Care delivered by fully trained paramedic in maintaining airway, controlling
cervical spine, securing intravenous and initiating fluid resuscitation
Hospital care (inter-hospital triage) Senior medical staff organized team to ensure that medical resources are
deployed to maximum overall benefit
Mass casualty triage
triage decisions are crucial in triage decisions are crucial in determining individual patients survivaldetermining individual patients survival

4
Primary surveyPrimary survey
Ⓐ Airway maintenance with cervical spine control
Ⓑ Breathing and ventilation
Ⓒ Circulation with hemorrhage control
Ⓓ Disability assessment of neurological status
Ⓔ Exposure and complete examination of the patient

5
AirwayAirway
Satisfactory airway signifies the implication of breathing and ventilation and cerebral function
Management of maxillofacial trauma is an integral part in securing an unobstructed airway
Immobilization in a natural position by a semi-rigid collar until damaged spine is excluded

6
Is the patient fully conscious? And able to maintain adequate airway?
Semiconscious or unconscious patient rapidly suffocate because of inability to cough and adopt a posture that held tongue forward
Sequel of facial injurySequel of facial injury
Obstruction of airway
asphyxia
Cerebral hypoxia
Brain damage/ death

7
Breathing and ventilationBreathing and ventilationChest injuries:
Pneumothorax, haemopneumothorax, flail segments, reputure daiphram, cardiac tamponade
signs
Clinical Deviated trachea
Absence of breath sounds
Dullness to percussionParadoxical movementsHyper-response with a large pneumothoraxMuffled heart sounds
RadiographicalLoss of lung markingDeviation of trachea
Raised hemi-diaphragmFluid levels
Fracture of ribs

8
Circulation Circulation
Circulatory collapse leads to low blood pressure, increasing pulse rate and diminished capillary
filling at the periphery
Patient resuscitationPatient resuscitationRestoration of cardio-respiratory functionRestoration of cardio-respiratory function
Shock managementShock managementReplacement of lost fluidReplacement of lost fluid

9
Glasgow coma scale (GCS)Glasgow coma scale (GCS)(Teasdale and Jennett, 1974)(Teasdale and Jennett, 1974)
Eye Eye openingopening
Motor Motor responseresponse
Verbal Verbal responseresponse
SpontaneousSpontaneous 44 Move to Move to commandcommand
66 ConverseConverse 55
To speechTo speech 33 Localizes to Localizes to painpain
55 ConfusedConfused 44
To painTo pain 22 Withdraw Withdraw from painfrom pain
44 GibberishGibberish 33
nonenone 11 flexesflexes 33 gruntsgrunts 22
ExtendsExtends 22 nonenone 11nonenone 11
Score 8 or less indicates poor prognosis, moderate head injury between 9-12 and mild refereed to 13-15

10
Exposure Exposure
All trauma patient must be fully exposed in a warm environment to disclose any other hidden
injuries
When the airway is adequately secured the second survey of the whole body is to be carried out for:
Accurate diagnosis Maintenance of a stable state Determination of priorities in treatment Appropriate specialist referral

11
Head injuryHead injury
Many of facial injury patients sustain head Many of facial injury patients sustain head injury in particular the mid face injuriesinjury in particular the mid face injuries
Open
Closed
it is ranged from Mild concussion to brain death

12
Signs and symptoms of head injurySigns and symptoms of head injury Loss of conscious OR History of loss of conscious History of vomiting Change in pulse rate, blood pressure and pupil reaction to
light in association with increased intracranial pressure
Assessment of head injury (behavioral responses “motor and verbal responses” and eye opening)
Skull fracture Skull base fracture (battle’s sign) Temporal/ frontal bone fracture Naso-orbital ethmoidal fracture

13
slow reaction and fixation of dilated pupil denotes a rise in intra-cranial pressure
Rise in intercranial pressure as a result of acute subdural or extradural hemorrhage deteriorate the
patient’s neurological status
Apparently stable patient with suspicion of head injury must be monitored at intervals up to one hour for 24 hour after the
trauma

14
Hemorrhage Hemorrhage
Acute bleeding may lead to hemorrhagic shock and circulatory collapse
Abdominal and pelvis injury; liver and internal organs injury (peritonism)
Fracture of the extremities (femur)

15
Preliminary treatment in complex Preliminary treatment in complex facial injuryfacial injury
Soft tissue laceration (8 hours of injury with no delay beyond 24 hours)
Support of the bone fragments
Injury to the eye As a result of trauma, 1.6 million are blind, 2.3 million are
suffering serious bilateral visual impairment and 19 million with unilateral loss of sight (Macewen 1999)
Ocular damage Reduction in visual acuity Eyelid injury

16
Prevention of infectionPrevention of infectionFractures of jaw involving teeth bearing areas Fractures of jaw involving teeth bearing areas are compound in nature and midface fracture are compound in nature and midface fracture
may go high, leading to CSF leaks may go high, leading to CSF leaks (rhinorrhoea, otorrhoea) and risk of meningitis,(rhinorrhoea, otorrhoea) and risk of meningitis,
and in case of perforation of cartilaginous and in case of perforation of cartilaginous auditory canalauditory canal
Diagnosis: Laboratory investigation, CT and MRI scan Management:
– Dressing of external wounds– Closure of open wounds– Reposition and immobilization of the fractures– Repair of the dura matter– Antibacterial prophylaxis (as part of the general management (Eljamal,
1993)

17
Control of painControl of pain Displaced fracture may cause severe pain but Displaced fracture may cause severe pain but
strong analgesic ( Morphine and its derivatives) strong analgesic ( Morphine and its derivatives) must be avoided as they depress cough reflex, must be avoided as they depress cough reflex, constrict pupils as they may mask the signs of constrict pupils as they may mask the signs of
increasing intracranial pressureincreasing intracranial pressure
Management:
☞ Non-steroidal anti-inflammatory drugs can be prescribed (Diclofenac acid)
☞ Reduction of fracture
☞ sedation

18
In patient careIn patient care
Necessary medications
Diet (fluid, semi-fluid and solid food) intake and output (fluid balance chart)
Hygiene and physiotherapy
Proper timing for surgical intervention

AnatomyAnatomy

AnatomyAnatomy

Physical ExaminationPhysical Examination
Inspection of the face for asymmetry.Inspect open wounds for foreign bodies.Palpate the entire face.
– Supraorbital and Infraorbital rim– Zygomatic-frontal suture– Zygomatic arches

Physical ExaminationPhysical Examination
Inspect the nose for asymmetry, telecanthus, widening of the nasal bridge.
Inspect nasal septum for septal hematoma, CSF or blood.
Palpate nose for crepitus, deformity and subcutaneous air.
Palpate the zygoma along its arch and its articulations with the maxilla, frontal and temporal bone.

Physical ExaminationPhysical Examination
Check facial stability. Inspect the teeth for malocclusions, bleeding and
step-off. Intraoral examination:
– Manipulation of each tooth.– Check for lacerations.– Stress the mandible.– Tongue blade test.
Palpate the mandible for tenderness, swelling and step-off.

Physical ExaminationPhysical Examination
Check visual acuity.Check pupils for roundness and reactivity.Examine the eyelids for lacerations.Test extra ocular muscles.Palpate around the entire orbits..

Physical ExaminationPhysical Examination
Examine the cornea for abrasions and lacerations.
Examine the anterior chamber for blood or hyphema.
Perform fundoscopic exam and examine the posterior chamber and the retina.

Physical ExaminationPhysical Examination
Examine and palpate the exterior ears.Examine the ear canals.Check nuero distributions of the
supraorbital, infraorbital, inferior alveolar and mental nerves.

Frontal Sinus/ Bone FracturesFrontal Sinus/ Bone FracturesPathophysiologyPathophysiology
Results from a direct blow to the frontal bone with blunt object.
Associated with:– Intracranial injuries– Injuries to the orbital roof– Dural tears

Frontal Sinus/ Bone FracturesFrontal Sinus/ Bone FracturesClinical FindingsClinical Findings
Disruption or crepitance orbital rim
Subcutaneous emphysema
Associated with a laceration

Frontal Sinus/ Bone FracturesFrontal Sinus/ Bone FracturesDiagnosisDiagnosis
Radiographs:– Facial views should
include Waters, Caldwell and lateral projections.
– Caldwell view best evaluates the anterior wall fractures.

Frontal Sinus/ Bone FracturesFrontal Sinus/ Bone FracturesDiagnosisDiagnosis
CT Head with bone windows:– Frontal sinus fractures. – Orbital rim and
nasoethmoidal fractures.
– R/O brain injuries or intracranial bleeds.

Frontal Sinus/ Bone FracturesFrontal Sinus/ Bone FracturesTreatmentTreatment
Patients with depressed skull fractures or with posterior wall involvement.– ENT or nuerosurgery consultation.– Admission.– IV antibiotics.– Tetanus.
Patients with isolated anterior wall fractures, nondisplaced fractures can be treated outpatient after consultation with neurosurgery.

Frontal Sinus/ Bone FracturesFrontal Sinus/ Bone FracturesComplicationsComplications
Associated with intracranial injuries:– Orbital roof fractures.– Dural tears.– Mucopyocoele.– Epidural empyema.– CSF leaks.– Meningitis.

Naso-Ethmoidal-Orbital Naso-Ethmoidal-Orbital FractureFracture
Fractures that extend into the nose through the ethmoid bones.
Associated with lacrimal disruption and dural tears.
Suspect if there is trauma to the nose or medial orbit.
Patients complain of pain on eye movement.

Naso-Ethmoidal-Orbital Naso-Ethmoidal-Orbital FractureFracture
Clinical findings:– Flattened nasal bridge or a saddle-shaped
deformity of the nose.– Widening of the nasal bridge (telecanthus)– CSF rhinorrhea or epistaxis.– Tenderness, crepitus, and mobility of the nasal
complex.– Intranasal palpation reveals movement of the
medial canthus.

Naso-Ethmoidal-Orbital Naso-Ethmoidal-Orbital FractureFracture
Imaging studies:– Plain radiographs are insensitive.– CT of the face with coronal cuts through the
medial orbits.
Treatment:– Maxillofacial consultation.– ? Antibiotic

Nasal FracturesNasal Fractures
Most common of all facial fractures.Injuries may occur to other surrounding
bony structures.3 types:
– Depressed– Laterally displaced– Nondisplaced

Nasal FracturesNasal Fractures
Ask the patient:– “Have you ever broken your nose before?”– “How does your nose look to you?”– “Are you having trouble breathing?”

Nasal FracturesNasal Fractures
Clinical findings:– Nasal deformity– Edema and tenderness– Epistaxis– Crepitus and mobility

Nasal FracturesNasal Fractures
Diagnosis:– History and physical
exam.– Lateral or Waters view
to confirm your diagnosis.

Nasal FracturesNasal Fractures
Treatment:– Control epistaxis.– Drain septal
hematomas.– Refer patients to ENT
as outpatient.

Orbital Blowout FracturesOrbital Blowout Fractures
Blow out fractures are the most common.Occur when the the globe sustains a direct
blunt force2 mechanisms of injury:
– Blunt trauma to the globe– Direct blow to the infraorbital rim

Orbital Blowout FracturesOrbital Blowout FracturesClinical FindingsClinical Findings
Periorbital tenderness, swelling, ecchymosis.
Enopthalmus or sunken eyes.
Impaired ocular motility.
Infraorbital anesthesia. Step off deformity

Orbital Blowout FracturesOrbital Blowout FracturesImaging studiesImaging studies
Radiographs:– Hanging tear drop sign– Open bomb bay door– Air fluid levels– Orbital emphysema

Orbital Blowout FracturesOrbital Blowout FracturesImaging studiesImaging studies
CT of orbits– Details the orbital
fracture– Excludes retrobulbar
hemorrhage.
CT Head– R/o intracranial
injuries

Orbital Blowout FracturesOrbital Blowout FracturesTreatmentTreatment
Blow out fractures without eye injury do not require admission– Maxillofacial and ophthalmology consultation– Tetanus– Decongestants for 3 days– Prophylactic antibiotics– Avoid valsalva or nose blowing
Patients with serious eye injuries should be admitted to ophthalmology service for further care.

Zygoma FracturesZygoma Fractures
The zygoma has 2 major components:– Zygomatic arch– Zygomatic body
Blunt trauma most common cause.Two types of fractures can occur:
– Arch fracture (most common)– Tripod fracture (most serious)

Zygoma Arch FracturesZygoma Arch Fractures
Can fracture 2 to 3 places along the arch– Lateral to each end of the arch– Fracture in the middle of the arch
Patients usually present with pain on opening their mouth.

Zygoma Arch FracturesZygoma Arch FracturesClinical FindingsClinical Findings
Palpable bony defect over the arch
Depressed cheek with tenderness
Pain in cheek and jaw movement
Limited mandibular movement

Zygoma Arch FracturesZygoma Arch FracturesImaging Studies & TreatmentImaging Studies & Treatment
Radiographic imaging:– Submental view
(bucket handle view)
Treatment:– Consult maxillofacial
surgeon– Ice and analgesia– Possible open elevation

Zygoma Tripod FracturesZygoma Tripod Fractures
Tripod fractures consist of fractures through:– Zygomatic arch– Zygomaticofrontal
suture– Inferior orbital rim and
floor

Zygoma Tripod FracturesZygoma Tripod FracturesClinical FeaturesClinical Features
Clinical features:– Periorbital edema and
ecchymosis– Hypesthesia of the
infraorbital nerve– Palpation may reveal
step off– Concomitant globe
injuries are common

Zygoma Tripod FracturesZygoma Tripod FracturesImaging StudiesImaging Studies
Radiographic imaging:– Waters, Submental and
Caldwell views
Coronal CT of the facial bones:– 3-D reconstruction

Zygoma Tripod FracturesZygoma Tripod FracturesTreatmentTreatment
Nondisplaced fractures without eye involvement– Ice and analgesics– Delayed operative consideration 5-7 days– Decongestants – Broad spectrum antibiotics – Tetanus
Displaced tripod fractures usually require admission for open reduction and internal fixation.

Maxillary FracturesMaxillary Fractures
High energy injuries.Impact 100 times the force of gravity is
required .Patients often have significant multisystem
trauma.Classified as LeFort fractures.

Maxillary FracturesMaxillary FracturesLeFort ILeFort I
Definition:– Horizontal fracture of
the maxilla at the level of the nasal fossa.
– Allows motion of the maxilla while the nasal bridge remains stable.

Maxillary FracturesMaxillary FracturesLeFort ILeFort I
Clinical findings:– Facial edema– Malocclusion of the
teeth– Motion of the maxilla
while the nasal bridge remains stable

Maxillary FracturesMaxillary FracturesLeFort ILeFort I
Radiographic findings:– Fracture line which
involves Nasal aperture Inferior maxilla Lateral wall of maxilla
CT of the face and head – coronal cuts– 3-D reconstruction

Maxillary FracturesMaxillary FracturesLeFort IILeFort II
Definition:– Pyramidal fracture
Maxilla Nasal bones Medial aspect of the
orbits

Maxillary FracturesMaxillary FracturesLeFort IILeFort II
Clinical findings:– Marked facial edema– Nasal flattening– Traumatic telecanthus– Epistaxis or CSF
rhinorrhea – Movement of the upper
jaw and the nose.

Maxillary FracturesMaxillary FracturesLeFort IILeFort II
Radiographic imaging:– Fracture involves:
Nasal bones Medial orbit Maxillary sinus Frontal process of the
maxilla
CT of the face and head

Maxillary FracturesMaxillary FracturesLeFort IIILeFort III
Definition:– Fractures through:
Maxilla Zygoma Nasal bones Ethmoid bones Base of the skull

Maxillary FracturesMaxillary FracturesLeFort IIILeFort III
Clinical findings:– Dish faced deformity– Epistaxis and CSF
rhinorrhea – Motion of the maxilla,
nasal bones and zygoma
– Severe airway obstruction

Maxillary FracturesMaxillary FracturesLeFort IIILeFort III
Radiographic imaging:– Fractures through:
Zygomaticfrontal suture Zygoma Medial orbital wall Nasal bone
CT Face and the Head

Maxillary FracturesMaxillary FracturesTreatmentTreatment
Secure and airwayControl BleedingHead elevation 40-60 degreesConsult with maxillofacial surgeonConsider antibioticsAdmission

Mandible FracturesMandible FracturesPathophysiologyPathophysiology
Mandibular fractures are the third most common facial fracture.
Assaults and falls on the chin account for most of the injuries.
Multiple fractures are seen in greater then 50%.
Associated C-spine injuries – 0.2-6%.

Mandible FracturesMandible FracturesClinical findingsClinical findings
Mandibular pain. Malocclusion of the teeth Separation of teeth with
intraoral bleeding Inability to fully open
mouth. Preauricular pain with
biting. Positive tongue blade test.

Mandible FracturesMandible Fractures
Radiographs:– Panoramic view– Plain view: PA, Lateral and a Townes view

Mandibular FracturesMandibular FracturesTreatmentTreatment
Nondisplaced fractures:– Analgesics– Soft diet– oral surgery referral in 1-2 days
Displaced fractures, open fractures and fractures with associated dental trauma– Urgent oral surgery consultation
All fractures should be treated with antibiotics and tetanus prophylaxis.

Mandibular DislocationMandibular Dislocation
Causes of mandibular dislocation are:– Blunt trauma– Excessive mouth opening
Risk factors:– Weakness of the temporal mandibular ligament– Over stretched joint capsule – Shallow articular eminence– Neurologic diseases

Mandibular DislocationMandibular Dislocation
The mandible can be dislocated:– Anterior 70%– Posterior– Lateral– Superior
Dislocations are mostly bilateral.

Mandibular DislocationMandibular Dislocation
Posterior dislocations:– Direct blow to the chin– Condylar head is pushed against the mastoid
Lateral dislocations:– Associated with a jaw fracture– Condylar head is forced laterally and superiorly
Superior dislocations:– Blow to a partially open mouth– Condylar head is force upward

Mandibular DislocationMandibular Dislocation
Clinical features:– Inability to close
mouth– Pain– Facial swelling
Physical exam:– Palpable depression– Jaw will deviate away– Jaw displaced anterior

Mandibular DislocationMandibular Dislocation
Diagnosis:– History & Physical
exam– X-rays– CT

Mandibular DislocationMandibular Dislocation
Treatment:– Muscle relaxant– Analgesic– Closed reduction in the
emergency room

Mandibular DislocationMandibular Dislocation
Treatment:– Oral surgeon consultation:
Open dislocations Superior, posterior or lateral dislocations Non-reducible dislocations Dislocations associated with fractures

Mandibular DislocationMandibular Dislocation
Disposition:– Avoid excessive mouth opening– Soft diet– Analgesics– Oral surgery follow up

THANK YOU FOR THANK YOU FOR ATTENTIONATTENTION