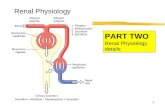
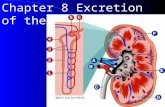
Renal system physiology
-
Upload
elfritzson-peralta -
Category
Science
-
view
863 -
download
1
Transcript of Renal system physiology


PHYSIOLOGY OF EXCRETORY SYSTEM
LIM, Tristan JonelMADRONA, Vivien Alexandra MANZANO, Ross JosePERALTA, ElfritzsonGroup 54BIO5

INTRODUCTION
Kidney→ excretory and regulatory
filters water and solutes in the blood, to excrete excess water, waste products , and foreign materials
regulates:1. plasma osmolarity2. plasma volume3. acid-base balance4. electrolyte balance

INTRODUCTION
between posterior abdominal wall and the abdominal peritoneum
right kidney is slightly lower than the left
~1M nephrons (functional unit)

INTRODUCTION
Filtrate Flow:
→ Bowman’s capsule→ proximal convoluted tubule→ loop of Henle→ distal convoluted tubule→ collecting duct→ minor calyces

INTRODUCTION
Afferent arteriole: Brings blood to the nephron to be filtered
Efferent arteriole: Removes blood from nephron (minus filtered components)
Glomerulus: Capillary tuft where filtration occurs
Bowman's Capsule: First part of nephron where filtrate is collected
Proximal Convoluted Tubule: Where selective reabsorption occurs

INTRODUCTION
Loop of Henle: Important for establishing a salt gradient in the medulla
Distal Convoluted Tubule: Final site of selective reabsorption
Collecting Duct: Feeds into ureter and is where osmoregulation occurs
Vasa Recta: Blood network that reabsorbs components from the filtrate

OBJECTIVES
The students aim to determine:
a) the effect of arteriole radius on glomerular filtration
b) the effect of pressure on glomerular filtration
c) renal response to altered blood pressure
d) impacts of solute gradient to urine concentration
e) reabsorption of glucose via carrier proteins
f) the effect of hormones on urine formation

METHODOLOGY
The students made use of the simulation procedure provided in the PhysioEx 9

RESULTS AND DISCUSSION
Glomerular Capillary Pressure
Fluid pressure exerted by blood within glomerular capillaries
Major force producing glomerular filtration
Depends on:
Contraction of the heart
Resistance to blood flow offered by afferent and efferent
arterioles
ACTIVITY 1: The Effect of Arteriole Radius on Glomerular Filtration

RESULTS AND DISCUSSION
Table 1. Glomerular capillary pressure (GCP) and filtration rate (FR)
Decrease of afferent arteriole radius GCP and FR decrease Increase of afferent arteriole radius GCP , FR and urine vol. increase Decrease of efferent arteriole radius GCP, FR, and urine vol. increase Increase of efferent arteriole radius GCP and FR decrease

RESULTS AND DISCUSSION
ACTIVITY 2: The Effect of Pressure on Glomerular Filtration
Glomerular Filtration
Passive process
Glomerular capillaries Glomerular capsules
Starling Forces (hydrostatic and osmotic pressure gradients)
Glomerular Filtration Rate
Index of kidney function
In humans, filtration ranges from 80 – 140 mL/min.
Can be altered by arteriole resistance or arteriole hydrostatic
pressure

RESULTS AND DISCUSSION
Table 2. The Effect of Pressure on Glomerular Filtration
Increase in blood pressure GCP, FR and urine vol. increases Decrease in blood pressure GCP , FR and urine vol. decreases Closing the valve while pressure is constant GCP is constant, FR decreases, and urine
vol. is 0 Closing the valve while increasing pressure GCP and FR increases, urine vol. is 0

RESULTS AND DISCUSSION
ACTIVITY 3: Renal Response to Altered Blood Pressure
• Cellular metabolism
o produces a complex mixture of waste products
• Excretory function is performed by a combination of
organs such as the paired kidneys
• Each nephron carries out 3 crucial processes:
1. glomerular filtration
2. tubular reabsorption
3. tubular secretion

RESULTS AND DISCUSSION
ACTIVITY 3: Renal Response to Altered Blood Pressure
• Blood pressure in glomerular capillaries and filtrate
pressure in the renal tubule can have a significant impact
on the glomerular filtration rate
• Approximately 20% of the blood that enters the
glomerular capillaries is filtered into the Bowman’s
capsule, where it is referred to as filtrate

RESULTS AND DISCUSSION
ACTIVITY 3: Renal Response to Altered Blood Pressure

RESULTS AND DISCUSSION
Afferent arteriole• Brings blood to the glomeruli
Efferent arteriole• Draws blood away from the glomeruli

RESULTS AND DISCUSSION
Table 3. Renal Response to Altered Blood Pressure
Constricting the Afferent Arteriole causes : Decrease in Glomerular Pressure Decrease in Glomerular Filtration
Rate Decrease in Urine Production
Constricting the Efferent Arteriole causes : Increase in Glomerular Pressure Increase in Glomerular Filtration Rate Increase in Urine Production

RESULTS AND DISCUSSION
ACTIVITY 4: Solute Gradients and Their Impact on Urine Concentration
NOTE: The movement of solutes and water relies on the total solute concentration gradient in the interstitial spaces surrounding the tubule lumen
When the nephron is permeable to solutes or water, equilibrium will be reached between the interstitial fluid and the tubular fluid contents
Interstitial fluid- mostly NaCL and urea
Antidiuretic hormone (ADH)- increases water permeability of the collecting duct

RESULTS AND DISCUSSION
Table 4. Solute Gradients and Their Impact on Urine Concentration
Decrease of urine vol. Urine conc. & solute conc. increase No ADH Urine vol. increases
Most of the tubular filtrate is reabsorbed to prevent fluid loss and maintainhomeostasis
Movement of solutes into peritubular capillaries decreases the soluteconcentration of the tubular fluid but increases the solute concentration in theperitubular capillaries

RESULTS AND DISCUSSION
ACTIVITY 4: Solute Gradients and Their Impact on Urine Concentration
Tubule fluid osmolarity will always be the greatest in the bottom of
the loop of Henle
Tubule fluid volume will always be the greatest in the proximal
convoluted tubule
ADH directly alter the urine volume in the collecting duct

RESULTS AND DISCUSSION
ACTIVITY 5: Reabsorption of Glucose via Carrier Proteins
Reabsorption- movement of filtered solutes and water from the lumen of the renal tubules back into the plasma
Glucose is filtered out of the plasma into Bowman’s capsule as part of the filtrate.
-First absorbed by secondary active transport at the apical membrane of proximal tubule cells
-It then leaves via facilitated diffusion along the basolateralmembrane.
-Excess glucose is eliminated in urine.
RESULTS AND DISCUSSION

ACTIVITY 5: Reabsorption of Glucose via Carrier Proteins
RESULTS AND DISCUSSION
Glucose carrier proteins-Present in the proximal tubule cells of the nephron to ensure glucose is reabsorbed into the body so that it can fuel cellular metabolism.- Finite number - Constant in a human kidney and that is the plasma glucose that varies during the day.
Transmembrane proteins → Carrier proteins that transport these molecules across the tubule membranes.
NOTE: ADH has no direct effects on renal processing of plasma glucose.

RESULTS AND DISCUSSION
Table 5. Reabsorption of Glucose via Carrier Proteins
Increase of glucose carriers Decrease of glucose conc.
Glucose concentration is the same in both Bowman's capsule and the urinary bladder BECAUSE glucose cannot be reabsorbed in the absence of carriers.
When the number of glucose carriers becomes great enough, all of the glucose is reabsorbed

ACTIVITY 5: Reabsorption of Glucose via Carrier Proteins
RESULTS AND DISCUSSION
APPLICATION:
Why do we expect to find glucose in the urine of a diabetic person?
The lack of insulin causes a high glucose concentration OR an excessive amount of glucose is present in their filtrate. The glucose can’t all be absorbed

RESULTS AND DISCUSSION
ACTIVITY 6: The Effect of Hormones on Urine Formation
Aldosterone• Acts on the distal convoluted tubules to increase reuptake of NaCl and secretion of Potassium• Water is reabsorbed due to increased amounts of NaCl• Leads to a decrease in urine volume and an increase in potassium concentration of urine
ADH• Increases the permeability of the collecting duct• Increases water reabsorption• Leads to a decrease in urine volume and an increase in potassium concentration in urine

RESULTS AND DISCUSSION
Table 6. The Effect of Hormones on Urine Formation

CONCLUSION
Constriction of the afferent arteriole decreases the blood flow into the glomerulusand thus the glomerular hydrostatic pressure, which leads to a decrease in GFR.Constriction of the efferent arteriole decreases blood flow out of the glomerulus, and this increases the glomerular hydrostatic pressure and leads to an increase in GFR.Blood pressure and flow are directly proportionalAn increase in blood pressure leads to an increase in glomerular hydrostatic pressure, which increases GFR.A decrease in blood pressure leads to a decrease in glomerular hydrostatic pressure, which decreases GFR.Altering arteriole radii is an important mechanism in regulating GFR during changes in blood pressureIncreasing the solute conc. would increase urine conc. and decrease urine vol.An increase of glucose carriers would decrease glucose conc.The actions of hormones like aldosterone and ADH have an effect in urine formation

REFERENCES
http://www.ib.bioninja.com.au/higher-level/topic-11-human-health-and/113-the-kidney.html
http://www.scribd.com/doc/31017235/Exercise-9-Renal-System-Physiology-1
Sherwood, L., Klandorf, H., & Yancey, P. (2013). Neuronal Physiology. In Animal Physiology: From
Genes To Organisms (Second ed.). Cengage Learning.






![Exercise 9 - Renal System Physiology[1]](https://static.fdocuments.in/doc/165x107/553dd6134a7959502f8b47ca/exercise-9-renal-system-physiology1.jpg)