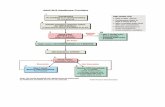
Acls Algorithms Rapid Rates
-
Upload
anonymous-nerc5jyis -
Category
Documents
-
view
2 -
download
0
description
Transcript of Acls Algorithms Rapid Rates

ACLS
ALGORITHMS

Acute Pulmonary Edema / Hypotension / Shock Algorithm
Volume problemIncludes PVR problems
Systolic BP < 70Signs of shock
Administer• Fluids• Blood transfusions• Cause-specific interventions• Consider vasopressors
Too SlowGo to Fig 5
Rate ProblemPump Problem
Systolic BP 70 - 100 mmHgSigns of shock
Too FastGo to Fig 6
Systolic BP> 100 mmHg
Systolic BP70 - 100 mmHgNo Signs of shock
Clinical signs of hypoperfusion, congestive heart failure, acute pulmonary edemaAssess ABC’s Assess vitalsSecure airway Review historyAdminister O2 Perform physical examStart IV 12 lead ECG, chest x-rayAttach monitor, pulse oximetry and B/P Cuff
What is the nature of the problem?
What is the BP ?
Figure 8

Bradycardia Algorithm(Patient is not in Cardiac Arrest)
Assess ABC’s Assess vitalsSecure airway Review historyAdminister O2 Perform physical examStart IV 12 lead ECG, chest x-rayAttach monitor, pulse oximetry and B/P Cuff
Intervention sequence• Atropine 0.5 - 1.0 mcg,d (I and IIa)• TCP, if available (I)• Dopamine 5 - 20 mcg/kg/min (IIb)• Epinephrine 1 - 10 mcg/min (IIb)• Norepinephrine 0.5 –30 mcg/min (IIb)
Bradycardia, either absolute(<60 BPM) or relative
Type II second-degree AV heart blockor
Third-degree AV heart Block?e
Serious signs and symptoms?a,b
No
No Yes
Yes
Observe• Prepare for transvenous pacer• Use TCP as a bridge device
Figure 5

Tachycardia Algorithm (Patient is not in Cardiac Arrest)
Assess ABC’s Assess vitalsSecure airway Review historyAdminister O2 Perform physical examStart IV 12 lead ECG, chest x-rayAttach monitor, pulse oximetry and B/P Cuff
If ventricular rate > 150 BPM• Prepare for cardioversion• May give brief trial of Rx • Immediate cardioversion is seldom needed for heart rates < 150 BPM
Wide-complextachycardia of uncertain type
VentricularTachycardia (VT)
ParoxysmalSupraventricularTachycardia(PSVT)
Atrial FibrillationAtrial Flutter
Unstable, with serious signs or symptoms?a
Yes
No
Figure 6

Pulseless Electrical Activity (PEA) Algorithm(Electromechanical Dissociation [EMD])
Includes Electromechanical dissociation (EMD) Postdefibrillation idioventricular rhythms Pseudo - EMD Bradyasystolic rhythms Idioventricular rhythms Ventricular escape rhythms
• Continue CPR / Intubate at once / Obtain IV Access• Assess blood flow using Doppler ultrasound, endtidal CO2, echocardiography, or arterial line
Consider possible causesHypovolemia (volume infusion) Drug overdoses - tricyclics, digitalisHypoxia (ventilation) Beta-blockers, calcium channel blockersCardiac tamponade (pericardiocentesis) HyperkalemiaTension Pneumothorax AcidosisHypothermia ( see hypothermia algorithm) Massive acute myocardial infarctionMassive pulmonary embolism (surgery, lysine) Massive acute MI (go to Fig 9)
Epinephrine 1 mg IV push,a,c repeat q 3 - 5 min
• If absolute bradycardia (< 60 BPM) or relative bradycardia• give atropine 1 mg IV• Repeat q 3 -5 min to a total of 0.03 - 0.04 mg/kg
Figure 3

Asystole Treatment Algorithm
• Continue CPR• Intubate at once• Obtain IV Access• Confirm asystole in more than 1 lead
• Atropine 1 mg IV push repeat q 3 - 5 min up to a total
of 0.03 - 0.04 mg/kgd,e
• Epinephrine 1mg IV push,b,c
repeat q 3 - 5 min
Consider possible causes Hypoxia Pre-existing acidosis Hyperkalemia Drug Overdose Hypokalemia Hypothermia
Consider termination of efforts
Consider immediatetranscutaneous pacing (TCP)a
Figure 4

Ventricular Fibrillation (VF)&
Pulseless Ventricular Tachycardia (VT)•ABCs•Perform CPR until defibrillator Arrives• VF/VT present on defibrillator
Defibrillate up to 3 times if needed for persistent VF/VT200 J, 200 - 300 J, 360 J
Rhythm after the first 3 shocks? b
AsystoleGo to Fig 4
PEAGo to Fig 3
VF/VT ROSC
Figure 2

• Continue CPR• Intubate / IV Access
VF & Pulseless VT
Defibrillate 360 J, 30 - 60 sec after Rx
Epinephrine c,d 1 mg/IV
2 mg/ETT q 3 - 5 min
Administer Rx Class IIaprobable benefit f, g
Defibrillate 360 Jwithin 30 - 60 sec
Figure 2