07 Glomerulonephritis HAEMATUjlRIA I
description
Transcript of 07 Glomerulonephritis HAEMATUjlRIA I

HAEMATURIA
Dr. Shaman Rajindrajith

Causes of Haematuria
• Glomerulour Diseases– Recurrent gross H’urea– Post streptococcal nephritis– Membranous– SLE– HSP– HUS– Goodpasture syndrome
• Infections– UTI– Tuberculosis

Causes of Haematuria Cont…
• Haemtological– Coagulopathies– Thrombocytopaenia
• Others– Hypaercalciuria– Stones– Trauma– PKD– Renal vein
thrombosis– Tumours– Drugs– Exercise

Causes of Dark Colour Urine
• RED– Blood– Haemoglobin– Myoglobin– Porphyrins– Food colourings– Drugs– Urates
• BROWN/BLACK– Blood– Homogentisic acid– Melanin– Methaemoglobim

Evaluation
• History
• Examination

Evaluation
• History– Infections
(Skin/Throat/GI)– Urinary symptoms– Skin rashes– Joint involvement– Drugs– Trauma– Family history
• Examination– Oedema– Rashes– Joints– Renal masses– Genitalia– BP

Investigations• Basic Investigations
– UFR+- Culture– FBC– Renal function– USS abdomen & pelvis
• Others– Evidence of Streptococcal infection– C3 levels– 24 hour urine collection for – protein, creat, Ca– Coagulation screen
• Invasive Procedures– Biopsy– Cystoscopy

Post-Streptococcal Glomerulonephritis

Aetiology• Commonest cause of Nephritic syndrome in
children• Components of Nephritic syndrome
– Haematurea– Oedema– Hypertension– Renal insufficiency
• Lansfield’s Group A Streptococci• Nephritogenic strains
– Serotype 12- Throat infection– Serotype 49- Skin infection– Serotype 4 &25

Pathogenesis
• Precise mechanism is not known
• ? Circulating immune complexes
• ? Complement activation

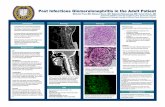
Pathology
• All glomeruli enlarged
• Diffuse mesangial cell proliferation
• PMN infiltration
• Crescents formation
• Immuno-histochemistry– Deposition of C3 & Ig

Clinical Picture
• Antecedent Streptococcal infection 1-3 wk• Peri-orbital oedema• Low urine output• Red colour urine• Lethargy• Flank pain• Mild temperature

Investigations
• Urine microscopy– Red cells– Granular casts– White cells– Protein
• Renal functions– Electrolytes– Urea/Creatinine
• Evidence of Strep. Infection– ASOT– Anti Dnase B
• Immunological– Low C3

Management• Monitoring
– Temperature chart– Daily weight– BP– Intake –output chart– Daily urine protein
• Antibiotics– Oral penicillin for 10 days
• Investigations• Control Blood pressure• Other aspects
– ? Restriction of activity

Complications
• Acute Renal Failure
• Hypertensive Encephalopathy
• Pulmonary Oedema

Management of Complications
• Acute Renal Failure– Fluid restriction– Protein restriction– Monitoring– Electrolyte balance– Dialysis
• Encephalopathy– Intensive care– Control BP– Sedatives/
anticonvulsants

Prognosis
• Complete recovery > 95%
• May progress to ‘crescent nephritis’
• Haematurea may persist for 1-2 years
• Recurrences – extremely rare

Other Causes of Glomerulonephritis
• Membranous
• SLE nephritis
• Mesangiocapillary nephritis
• Goodpasture Syndrome
• Haemolytic- Uraemic syndrome

Crescent Nephritis
• Rapidly progress to renal failure
• Crescents in glomeruli
• Aetiology– Post-streptococcal– SLE– HSP– Vasculitic syndromes