What’s New (and What’s Not) in Acne and Rosacea Adam O. Goldstein, MD Assistant Professor...
-
Upload
shaylee-dixie -
Category
Documents
-
view
221 -
download
0
Transcript of What’s New (and What’s Not) in Acne and Rosacea Adam O. Goldstein, MD Assistant Professor...

What’s New (and What’s Not) in Acne and Rosacea
Adam O. Goldstein, MD
Assistant Professor
Department of Family Medicine
University of North Carolina at Chapel Hill
Email: [email protected]


Objectives
1. Know differential diagnosis acne/rosacea
2. Increased knowledge treatment strategies
3. Increased familiarity new products
4. Learn 2 new patient education tips
GOAL: Improved therapeutic outcomes


Acne• Most common dermatologic disease
• Onset usually adolescence but anytime
• More frequent and severe in males
• 70% women premenstrual flares

Acne Quiz (T/F)
1. Certain foods make acne worse...
2. Dirty skin makes acne worse...
3. Acne worsens with sexual activity...
4. Acne improves within 24 hours of tx...
5. Sweating may make acne worse...
6. Humidity may exacerbate acne...
7. Acne may worsen during menstruation...
8. Stress may make acne worse...

Art of acne treatment:
• Negotiating long-term treatment• Increasing compliance by using fewer
medications• Contracting with adolescents• Thorough explanation of natural history of
disease• Patience with acne’s emotional toil • Combining drugs @ different mechanisms

Art of acne treatment:• “Quality of Life” scale
0 1 2 3
1. Feeling self-conscious
2. Decrease in socialization
3. Difficulties in relationships
(partner, friends, family)
4. Feeling like an outcast
5. People making fun of you
6. Feeling rejected (romance, friends)

Common pitfalls in acne treatment
• Using more than two medications
• Insufficient patient education or unrealistic expectations
• Frustration all around

Acne: Etiology• Combination hormonal (androgen), bacterial
(Proprionibacterium acnes) and follicular (hyperkeratosis)causing debris and occlusion
• Bacteria multiply and inflammatory response• Comedones: “Blackheads” and “Whiteheads”• Blackheads = open comedones• Whiteheads = closed comedones


Acne: Morphology
• Comedones
• Papules
• Pustules
• Nodules
• Cysts





Acne: Differential Diagnosis• Rosacea: No comedones, erythema striking,
central face• Hidradenitis: Axilla & inguinal, nodules & cysts,
scarring• Keratosis Pilaris: Upper arms & trunks, follicular-
based papules • Perioral Derm.: Papulovesicles & erythema,
perioral, topical steroid use • Senile Comed.: Face & neck, comedones and cysts
in damaged skin• Topical steroids: Lesions same stage, no comedones

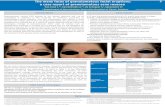
Rosacea

Hidradenitis

Keratosis Pilaris

Keratosis Pilaris

Perioral Dermatitis

Perioral Dermatitis

Senile Comedones

Topical Steroids

Acne Keloidalis

Acne Keloidalis

Acne: Treatment
• Treatment goal is to prevent new lesions/scarring• Treatment will not improve outcomes for 4-6
weeks• (Acne exacerbated by iodides, bromides,
hydantoin, chlorinated hydrocarbons, occluding topical preparations, vigorous washing, and mechanical occlusion)

Acne and Iodides

Acne and Dilantin

Acne and Topical Steroids

Acne and Topical Steroids


Mechanical occlusion

Mild acne: • Apply one agent thinly to entire face
• If two agents selected, use at separate times
• Apply after washing with water or mild soap
• Choices:
– Benzoyl peroxide Topical antibiotics
– Tretinoin Birth Control Pills
– Azelaic acid Salicylic acid
• Use for 6-8 weeks before judging if effective

Mild acne
• Benzoyl peroxide ($)
– Antibacterial, drying and peeling actions– Rx: 2.5-10% gel/cream/wash– OTC: 2.5-10% gel/lotion/cream
– Usually start with 2.5-5%, thin layer QD-BID

Mild acne • Benzoyl peroxide
– Water based preps are milder and less drying– Alcohol/acetone preps useful in oily skin– Washes and soaps are good for acne on the
chest, back and shoulders (5-10%)– Benzamycin gel- 23.3 grm- benzoyl peroxide
and erythromycin- must be kept refrigerated

Mild acne: Benzoyl peroxide
• Side Effects– Occasional hypersensitivity reactions (1-5%)
– Oxidating agent: will bleach clothes and hair

Mild acne • Topical antibiotics (all Px) ($$)
– Erythromycin 2%- pledgettes, pads, gel (oily skin), solution, ointment (dry skin)
– Clindamycin 1%- solution, gel, lotion • (e.g. Cleocin T)
– Meclocycline- cream; useful in patient with very dry skin• (e.g. Meclan)

Mild acne: Topical antibiotics
• Sodium sulfacetamide 10%, Sulfur 5%, Sodium thiosulfate 10% – Numerous keratolytic/astringent agents
– Useful if lotion preparation preferred and other topical antibiotics not working or tolerated
– Sulfacet R- tinted (can cover redness)
– Novacet- untinted
• Bacterial resistance may develop after 6-12 months of use

Mild acne: Topical Retinoids
• Especially good for comedonal or papular acne
• Modulates keratinization
• Use pea size amount to entire face
• Apply 3x week for 2 weeks, then nightly
• Increases photosensitivity
• Flare reaction frequent
• Web Sites: http://www.healthsquare.com/pdrfg/pd/ monos/retin-a.htm

Topical Retinoids Retin A (Renova) ($$$)• Vehicles:0.025%, 0.05%, 0.1% cream; 0.01%, 0.025% gel• Start with 0.025% strength• Apply at bedtime 30 minutes after washing
Avita• Vehicles: 0.025% cream/gel• Slow release polymer may be less irritating
Retin A Micro• Vehicle: 0.1% gel; Thick and yellow• Slow release may be less irritating

Retinoid-Like
• Adapalene (Differin) ($$$)– Vehicles: 0.1% gel, solution
– May apply right after washing at bedtime
• Tazarotene (Tazorac)– Vehicles: 0.05, 0.1% gel
– Irritating initially
– May be useful with oily skin
– Short contact therapy

Retinoids-Comparisons• Adapalene 0.1% gel vs. Tretinoin 0.025% gel, meta-analysis of 5
RCT’s (BMJ, 139S 1998)– equivalent efficacy reducing total lesions – Adapalene with significant difference in reduction of
inflammatory and total lesions at week 1
– Adapalene with greater local tolerability
• Adapalene 0.1% gel vs. Tretinoin 0.05% gel, Split-face clinical and bio-instrumental comparison (Dermatology. 198(2):218-22, 1999)– Tretinoin with better comedolysis and clinical improvement than
adapalene – Erythema transiently more pronounced with tretinoin

Salicylic acid: 2%
• OTC ($)
• Keratolytic
• Many preparations
• Useful in combo with tretinoin or topical antibiotics

20% Azelaic acid (Px)
• Mechanism unknown ($$)
• Useful for patients intolerant to tretinoin or benzoyl peroxide
• Avoid on broken skin
• Use qd-bid, usually in combination with other topicals

Acne and Birth Control Pills
• Lowers hormonal factors exacerbating acne
• Use pill with low androgenic potential
• Know side effects and contraindications
• Acne often improves during pregnancy

Moderate acne

Moderate acne
• Mild treatment +
• Add oral antibiotics– Tetracycline- 500 mg bid or doxycycline 50-100
mg/day
– Erythromycin- 500 mg bid
– Minocycline- 50-100 mg/day
– Trimethoprim/Sulfamethoxazole 1 DS qd-bid
• Comedo removal

Minocycline has fewer GI side effects, but it is more expensive


Severe acne
• Moderate regimen X 3 months
• Isotretinoin for severe nodulocystic acne
• Steroid injections– TAC acetonide 10 mg/ml diluted to 3 mg/ml– Inject 0.1 ml into fresh cyst
• Prednisone rarely
• Consultation





Isotretinoin (Accutane)• 0.5-1 mg/kg/day 16-20 weeks• 80% success rate• Indications wider than previous thought• Improvement continues after treatment stops• Very teratogenic: (2 forms birth control for one month
beforehand)• Laboratory monitoring: (HCG before & monthly, CBC, LFT, TG,
LDH, TG’s, Cholesterol, Q 2 weeks, then monthly)
• Use moisturizers, lip balms and artificial tears• Monthly costs $200-400

Acne: Myths
• NO relation to junk foods
• NO relation to “hygiene”
• NO relation to masturbation or other sexual activity
• NO way to make acne go away overnight

Acne: Truths
• YES acne may worsen premenstrual
• YES sweating may worsen acne
• YES humid environments may worsen acne
• YES stress can exacerbate acne

Acne: Patient Education• 6-8 week response• Avoid scrubbing
• Keep regimen simple• Compliance is key to FTIP; Have
patient bring medications to office

Acne: Patient Education
• Use water-based makeup
• “Oil-free” moisturizers
• Web Sites: http://www.pslgroup.com/ACNE.htm Useful
general information for clinicians
http://www.derm-infonet.com/acnenet/toc.html Comprehensive site
http://www.m2w3.com/acne/ Patient support group

Acne Rosacea
• “Rosy” dilatation of the central face: – eyes, nose, chin, cheek, forehead
• Diverse spectrum of disease- (papules, pustules, nodules, cysts)
• Rhinophyma -hyperplasia of the nose in middle aged men













Acne Rosacea
• Look for periodic facial flushing after temperature increase, spicy food ingestion or alcohol
• Absence of comedones
• Disease is chronic: Treatment goal is control

Acne Rosacea: Differential Diagnosis
• Acne Vulgaris: comedones, younger patient, lack of
flushing, less erythema
• Seb. dermatitis: no acneiform lesions• Lupus: no papules and pustules• Carcinoid: flushing is transient

Acne Rosacea: Treatment
• Topical – Antibiotics, Benzoyl peroxide, Tretinoin
• Oral antibiotics
• Isotretinoin for severe, recalcitrant cases
• Referral for surgery, dermabrasion, laser
• Potent topical steroids often worsen disease

Acne Rosacea: Topical Therapy
• Preferred topical antibiotic: – Metronidazole
• 0.1% cream (Noritate): qday
• 0.75% cream or gel: bid
– Alternatives:• Sodium sulfacetamide 10%/sulfur 5% lotion
• Clindamycin 1% lotion, gel or solution
• Erythromycin 2% solution

Acne Rosacea: Topical Therapy
• Benzoyl peroxide at 2.5% & up to 10% if tolerated
• Tretinoin 0.025%, 0.05% 0.1% cream – Start with lowest dose– May be used in combination with other
products

Acne Rosacea: Oral antibiotics
• Useful for nodular lesions
• Doxycycline 50-100 mg/day or tetracycline 500-1000 mg/day
• Minocycline 50-100 mg at bedtime
• Treat until improvement occurs, then taper for control

Acne Rosacea: Patient Education
• Control vs cure• Avoid excessive sunlight, alcohol, temperature
extremes and precipitating foods• Flares may require higher “pulse” treatment• Good web sites:
– National Rosacea Societyhttp://www.rosacea.org/home.html
– Patient education brochure– http://www.aad.org/pamphlets/rosacea.html

On the Horizon….
• New retinoids
• Combination products: retinoids and topical antibiotics
• Glycolic acid, salicylic acid peels
• Hormonal treatments
• Antibiotic alternatives

Cases
• 14, Sports PE & whiteheads- incidental• 16, with comedones and mild inflammation• 16, before the prom• 20, with sensitive skin, papular lesions and skin
irritation• 21, moderate acne on 0.1% Retina cream and 5%
Benz. Peroxide, wanting referral to dermatologist• 22, with extensive cystic acne for 5 years

Conclusion
• Be confident
• Use 1-2 agents if at all possible
• Define expectations
• Think about acne rosacea in adults