Scrotal masses
-
Upload
mohamed-shaaban -
Category
Health & Medicine
-
view
156 -
download
7
Transcript of Scrotal masses


• Testis
• Epididymis
• Spermatic cord
• Their fascial coverings




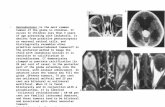
• The first imaging procedure to evaluate the
scrotum.
• The study has to be performed with high frequency
transducers (>10 MHz) with color Doppler facilities.


• MRI can be useful in the evaluation of scrotal
masses as a problem-solving technique:
1. Discrepancies between US and clinical
findings.
2. Diffuse, non-specific testicular involvement
seen on US scanning.
3. Fibrous lesions, lipomas or hemorrhage are
suspected.

• Testis.
• Tunica albuginea.
• The mediastinum testis.
• The epididymis.

• Most solid lesions originating from the testes are
malignant, while most lesions originating from
extratesticular structures are benign
• The most common extratesticular neoplasms are benign
lipomas, usually originating from the spermatic cord,
and adenomatoid tumors, most often from the
epididymis.

• In patients with a scrotal mass, imaging is requested to
answer the following five questions:
1. Is there a definite mass?
2. Is the mass intra- or extratesticular?
3. Is the mass bilateral?
4. Is the mass cystic or solid?
5. Is the nature of the lesion identifiable?

1. Is there a definite mass?
• US is almost 100% sensitive in the identification of
presence of scrotal masses.
• Diagnostic difficulties leading to false-negative results
are rarely encountered, and are mostly due to:
o Presence of isoechogenic intratesticular lesions
o Diffuse testicular involvement, especially in children
with yolk-sac tumors
o Extratesticular lipomas can be difficult to identify,
being often isoechoic to surrounding subcutaneous
tissue.

2. Is the mass intra- or extratesticular?
• Differentiation can be made by US in almost all
cases.
• Palpation during US examination can help to localize
the mass.

3. Is the mass bilateral?
• Testicular tumors can be bilateral (38% of
lymphomas, 2% of seminomas).

4. Is the lesion cystic or solid?
• US can easily differentiate a solid from a cystic
lesion.
• A lesion may be defined as a ‘cyst’ only if it is
completely anechoic, with increased through
transmission and presence of thin walls, without
any vegetations or irregularities.

5. Is the nature of the lesion identifiable?
• Identification of the nature of scrotal masses
cannot be based on imaging methods alone.
• Localization of the mass is important in predicting
the nature of the lesion.
o Most extratesticular lesions are benign
o Most intratesticular masses are malignant.
• The structural pattern of the mass is the second
important factor to consider.
o Most cystic lesions are benign, while solid
nodules are more often malignant.


Testicular Tumors
Age:
• First Decade → Yolk Sac Tumors – Teratomas.
• Second & Third Decade → Teratoma & Choriocarcinoma.
• Forth And Fifth Decade → Seminoma.

Testicular Tumors
Tumors Markers:
• Alpha Fetoprotein → All Yolk Sac Tumors – 75% Of
Embryonal Carcinoma.
• Human Chorionic Gonadotrophin (hCG) → All
Choriocarcinoma - 60% Embryonal Carcinoma.


• A common benign lesion (retention cyst).
• It is a cyst filled with cheesy laminated material
that appears solid on imaging.

• A rare benign tumor (approximately 1% of all
testicular tumors).
• It is a cyst filled with cheesy laminated material
that appears solid on imaging.

• At US, the lesion is seen as rounded or oval shaped nodule
with regular outer margins.
• The lesion tends to be hyperechoic, sometimes calcific outer
wall is seen, and an internal ’onion ring’ structure is
characteristic of an epidermoid cyst. No vascular signals are
seen at Doppler evaluation

• At MRI, a laminated appearance, with alternate low-and high-
signal intensity areas can be detected on T2-weighted images.

• US: Seminomas are well
defined and homogeneously
hypoechoic

• On MRI, Homogeneously hypointense on T2-weighted images.
Larger tumors may be more heterogeneous

• Non-seminomatous lesions are more heterogenous with areas of
hemorrhage and calcification.
• The tunica albuginea may be invaded.



• US findings are usually sufficient to suggest the diagnosis. The
testis is typically replaced by infiltrative hypoechoic
hypervascular lymphoid tissue.

• MR imaging findings are similar, with the testis being replaced
by tissue that is low signal intensity on T1- and T2-weighted
images, with low-level enhancement (less than the normal testis)

• “Burned-out" Germ Cell Tumor
• Extra-Testicular pseudo-tumors
• Testicular pseudo-tumors