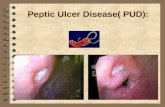
Peptic Ulcer Disease
Transcript of Peptic Ulcer Disease

Peptic Ulcer Disease
Vanessa Ting Ching Ching

Introduction
Heterogeneous group of disorders involving upper GI tract
Caused by imbalance between aggressive factors and defensive factors
Acute: specific patient population and clinical situation (eg stress ulcers)
Chronic: usually H.Pylori or NSAID ulcers with risk factors. Has remission and recurrence episodes

Physiology of upper GI tract
Stomach consists of: Cardia Body – contains
parietal cells (secrete acid and intrinsic factor) and chief cells (secrete pepsinogen)
Antrum – contains G cells (secrete gastrin)
Adapted from www.nlm.nih.com

Aggressive factors
K+-H+-ATPase pump secretes acid and is stimulated by:
Acetylcholine – neurologic impulses of sight, smell and taste of food or due to food distension or food protein.
Gastrin - released by stimulation of Ach on antral G cells
Histamine - Secreted by parietal cells Pepsinogen
forms pepsin in pH<3.5 combines with acid to form proteolytic
complex

Defensive factors
Prostaglandin E and somatostatin inhibit gastric acid secretion, maintain mucosal blood
flow, and stimulate production of mucus and bicarbonate epithelial cells and mucous cells
secrete mucus Gastric mucus
traps microorganisms, prevents back difussion of H ions from the mucosa, and acts as a lubricant
Bicarbonate secretion neutralises H ions
Network of vascular capillaries transport oxygen and substrates to the mucosa and
remove acids

Risk factors
Established Age >60 years H.pylori infection Previous PUD and UGIB Concomitant
corticosteroid therapy High dose, multiple
NSAID use Concomitant
anticoagulant use / coagulopathy
Chronic major organ impairment
Possible NSAID-related dyspepsia Duration of NSAID use Cigarette smoking Rheumatoid arthritis
Questionable Alcohol consumption Psychological stress Dietary factors* Combinations of risk
factors are additive

Signs and Symptoms
Epigastric pain (burning, cramping, fullness)
Nocturnal pain that awakes patient
Heartburn, belching, bloating
Nausea, vomiting, anorexia
Weight loss Complications eg
ulcer bleeding, perforation, penetration, obstruction

Diagnosis
Laboratory Tests Gastric acid secretory
studies Fasting serum gastrin
concentrations FBC – low haematocrit
and haemoglobin Tests for H.pylori
Other diagnostic tests Fibreoptic upper
endoscopy routine single-barium
contrast techniques

Treatment Aims
Decrease gastric acidity Inhibit gastric secretion (PPIs, H2-antagonists) Neutralise gastric acid (antacids) Duodenal ulcers associated with ↑acid secretion
Increase mucosal defences Protect GI mucosa (sucralfate, misoprostol) Gastric ulcers associated with normal/↓acid
secretion
Eliminate H.pylori Antibiotics, bismuth

Proton Pump Inhibitors
Potency: esomeprazole=rabeprazole> pantoprazole=lansoprazole=omeprazole
Inhibit K+H+ATPase covalently Up to 72 hours antisecretory effect Faster onset compared to H2-
antagonists, but similar rate of healing Metabolised by CYP450 system therefore
drug interactions with diazepam, phenytoin, warfarin, tolbutamide Except pantoprazole – metabolised by
cytosolic sulfotransferase

H2-Receptor Antagonists
Potency: famotidine > nizatidine=ranitidine >cimetidine
Block histamine receptors – decrease acid secretion
Cimetidine metabolised by CYP450 – decrease theophylline elimination by 20-30%
Cimetidine, ranitidine excreted by renal tubular secretion – decrease procainamide elimination
Alter gastric pH – decrease ketoconazole absorption

Sucralfate
At pH 2-2.5, binds to damaged and ulcerated tissue thus creates physical barrier Take with an empty stomach to prevent binding
to phosphate and protein in food Efficacy same as H2-antagonists, but requires
complicated dosage regimens Multiple daily doses, large size
Affect bioavailability of other drugs Space out 2 hours before sucralfate Consider other antiulcer therapy if giving
fluoroquinolones

Misoprostol
Synthetic PGE1 analogue, inhibits gastric acid production dose-dependent – 50-200mcg cytoprotective – >200mcg
Causes dose-dependent diarrhoea take with meals or at bedtime
Uterotropic – contraindicated in pregnant women

Bismuth
Antidiarrhoeal agent with ulcer-healing effects Antibacterial effect Local gastroprotective effect Stimulates endogenous PGs
Used in combination regimens for eradication of H.pylori
Safe but may cause salicylate sensitivity

Antacids
Neutralize acids, cytoprotective (stimulates PG production), stimulate restitution of gastric mucosa
Effective at low doses; as effective as H2-antagonists but short duration of action (~2hrs)
MgOH – diarrhoea; AlOH – constipation; CaCO3 – ↑gastric acid production at ↑doses; NaCO3 – systemic alkalosis at prolonged periods
↑ gastric pH: ↓bioavailability of ketoconazole; alter profile of e/c drugs; form complex with fluoroquinolones and tetracyclins

H. Pylori infection
Spiral Gram negative bacilli that colonizes the body of the stomach
Transmission: oral-oral, fecal-oral, iatrogenic Direct mucosal damage
By cytotoxins, bacterial enzymes and adherence to stomach wall
Altered inflammatory response Cell-mediated immune mechanisms or
phagocytosis Increased gastric acid secretion
HP products eg ammonia

Detection of H.pylori
Adapted from Pharmacotherapy: A pathophysiologic approach
Test Description Comments
Histology Microbiologic examination
Gold standard; >95% sensitive and specific; results are not immediate
Culture Culture of biopsy Sensitivity testing; results are not immediate; tests for active infection
Biopsy urease
Detects ammonia released by HP urease
>90% sensitive and specific; easily performed; rapid results
Antibody detection
Detects antibodies to HP in serum
Quantitative; unable to determine if antibody is caused by active or cured infection
Urea breath test
HP urease breaks down ingested labeled C-urea, labeled CO2 exhaled
Tests for active HP infection; 95% sensitive and specific; results take about 2 days
Stool antigen Identifies HP antigen in stool
Tests for active HP infection; as effective as urea breath test

Treatment of H.pylori
Eradication of H.pylori with combination therapy = ↓ulcer recurrence
7-day treatment is minimally effective but 14-day treatment is recommended
Use of single antibiotic has variable and marginal eradication rates and ↑antibiotic resistance
Clarithromycin is single most effective antibiotic

H.Pylori Eradication Regimens
Adapted from Pharmacotherapy: A pathophysiologic approach
Regimen Duration Comments
Omeprazole 20mg bd + clarithromycin 500mg bd + metronidazole 400mg bd or amoxycillin 500mg bd
1 week All combos of 3 antibiotics similarly effective; usually clarith + amoxy; ↑eradication rates with clarith1.5g/day
Omeprazole 20mg bd + amoxycillin 500mg tds or clarithromycin 500mg tds
2 weeks Marginal and variable eradication rates
Bismuth salicylate 120 mg qid + metronidazole 400mg tds + amoxycillin 500mg tds or tetracycline 500mg tds
2 weeks Similar to PPI-based triple-therapy; tetracycline more effective than amoxycillin
Ranitidine 300mg + amoxycillin 500mg tds + metronidazole 400mg tds
2 weeks Better eradication rate using PPI

NSAID use
2 mechanisms:1. Direct irritant effect –
acidic properties 2. COX-1 inhibition –
inhibition of PG release causing decrease in GI mucosal integrity and platelet homeostasis
Leukotrienes stimulate neutrophil adherence which damages endothelium
Taken from www.medscape.com

Treatment of NSAID Ulcers
Withdrawal/reduction of NSAID Replace with paracetamol/selective COX-2
inhibitors Duodenal ulcers/smaller gastric ulcers – full
dose H2-antagonist for min 8 weeks Ranitidine 150mg bd
Gastric ulcers/continued NSAID use – PPI for 8 weeks Omeprazole 20mg/day
Misoprostol 800mcg/day in divided doses

Zollinger-Ellison Syndrome
Non-β-islet cell tumours (gastrinoma) secrete additional gastrin –hyperstimulation of gastric acid secretion
Characterised by severe recurrent PUD Basal acid output >15mEq/h; fasting serum gastrin
>1000 pg/mL Treat with high dose PPIs in divided bd/tds doses
Eg omeprazole 60-80mg/day, up to 360mg/day Octreotide (synthetic somatostatin) inhibits gastric acid
secretion s/c 100-250mcg tds

Acute Upper GI Bleeding
Endoscopic therapy if active bleeding, exposed visible vessel or clot-covered ulcer Adrenaline injection up to 15 mL
Concomitant high-dose continuous IV infusion of PPI Omeprazole 80mg load, then 8mg/h for 3
days Less severe bleeders: IV 40mg bd Continue PPI for 4-6 weeks then H2-
antagonist for another 4-6 weeks

Stress Ulcers
Acute in nature; occur in critically-ill patients ↓ gastric mucosal blood flow in
haemorrhagic, cardiogenic and septic shock ↓ rate of proliferation and cellular turnover of
gastric mucosa No prostaglandin and mucous formation Risk factors: mechanical ventilation >48 hrs,
high-dose CCS therapy, sepsis, coagulopathy Others: shock, burns, multiple organ failure,
trauma, CNS injury

Stress Ulcer Prophylaxis
Improve physiological conditions
Inotropic drugs Vasodilators Intravascular volume
replacement Prevention of infection Analgesia and sedation Enteral nutrition
Adequate neutralisation of gastric acid
At pH 3.5-4, ↓frequency of bleeding; at pH<7, impaired clot stability
Sucralfate 1g qid via nasogastric tube
IV ranitidine (bolus 50mg tds or infusion 6.25-12mg/h)
IV omeprazole 40mg od has ↑antisecretory effects but also ↑nosocomial pneumonia

References
Dipiro JT, Talbert RL, Yee GC, et al, Pharmacotherapy: A pathophysiologic approach. 6th edition. New York: McGraw-Hill; 2006
Koda-Kimble MA. Applied therapeutics: the clinical use of drugs. 8th edition. USA: Lippincott Williams & Wilkins; 2005.
Kew ST, Tan SS et al. Consensus of Management of Peptic Ulcer Disease. Malaysian Clinical Practice Guidelines.
Rang, Dale, Ritter, Moore. Pharmacology. Elsevier Science Limited; 2003