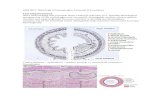
Enforce of pfysical, chemical and biological factors in pathogenesis of diseases 1.
Pathogenesis of Diseases of the Oesophagus
description
Transcript of Pathogenesis of Diseases of the Oesophagus

Pathogenesis of Diseases of the
Oesophagus
Dr Paul L. Crotty
Departement of Pathology
AMNCH, Tallaght
October 2008

Classification of Disease by Aetiology
• Congenital• Acquired• Infection• Physical/Trauma• Chemical/Toxic• Circulatory disturbances• Immunological disturbance• Degenerative disorders• Iatrogenic• Idiopathic• Multifactorial• Various: radiation, nutritional deficiency, psychosomatic• Pre-neoplastic/ Neoplastic

Classification of Disease by Aetiology
• Congenital• Acquired• Infection Disease A• Physical/Trauma• Chemical/Toxic• Circulatory disturbances• Immunological disturbance Pathogenetic process• Degenerative disorders• Iatrogenic• Idiopathic Disease B• Multifactorial• Various: radiation, nutritional deficiency, psychosomatic• Pre-neoplastic/ Neoplastic

Oesophagus: classification by aetiology
• Congenital: atresia, stenosis, fistulas, webs
• Acquired
• Infection: fungal infection, viral infection, Chagas’ disease
• Physical/Trauma: lacerations
• Chemical/Toxic: gastro-oesophageal reflux disease (GORD)
• Circulatory disturbances: oeophageal varices
• Immunological disturbance: eosinophilic oesophagitis
• Degenerative disorders
• Iatrogenic: pill oesophagitis
• Idiopathic: achalasia
• Multifactorial
• Various: radiation, nutritional deficiency, psychosomatic
• Pre-neoplastic/ Neoplastic: Barrett’s oesophagus -> adenocarcinoma squamous cell carcinoma

Normal Oesophagus

Normal Oesophagus
• Functions– Tube to conduct food into stomach– Prevent reflux of gastric contents– Prevent passive diffusion of food, bacteria
• To achieve these functions– peristalsis, coordinated with swallowing– sphincter at lower oesophagus: tonic, relax for
swallow– lined by stratified squamous mucosa

Manometry: normal oesophagus

Gastro-Oesophageal Reflux Disease (GORD)
• Abnormal retrograde movement of stomach contents to oesophagus
• Hydrochloric acid, pepsin
• Very common
• ~ 1 in 12 people heartburn daily
• ~ 1 in 6 heartburn weekly
• Oesophagitis in ~5%

Gastro-Oesophageal Reflux Disease (GORD)
• Normally, reflux prevented by:
• Lower oesophageal sphincter
• Anatomic structure (acute angle with stomach, crus of diaphragm)
• Oesophageal peristaltic clearance
• Swallowed saliva
• Gravity

Gastro-Oesophageal Reflux Disease (GORD)
• Reflux more likely to occur when:
• Decreased tone of sphincter
• Sliding hiatal hernia
• Decreased oesophageal clearance
• Decreased saliva production
• When lying down

Gastro-Oesophageal Reflux Disease (GORD)
• Hydrochloric acid and pepsin
• -> H+ ions diffuse into cells
• -> acidification of mucosa
• -> inflammation, necrosis

Gastro-Oesophageal Reflux Disease (GORD)
• Clinical: symptoms of heartburn• Endoscopic: red/congested mucosa• Manometric: decreased sphincter
pressure• pH: number, duration of dips: pH<4• Pathological: microscopic evidence of
oesophagitis

Clinical Endoscopic
Microscopic
Definition of GORD?

Endoscopic appearance
Normal Inflamed

Hiatal Hernia

Hiatal hernia
• Sliding type in 95% (5% para-oesophageal)
• Common anatomic abnormality
• Up to 20% of adults
• Associated with GORD
• Loss of acute angle with stomach
• Right crus of diaphragm contributes to functional level of sphincter pressure

Complications of GORD
• Ulceration
• Haemorrhage
• Perforation
• Fibrotic stricture
• Aspiration
• Barrett’s oesophagus
– risk of dysplasia and malignancy

Complications of GORD
Stricture Ulceration

Barrett’s oesophagus• As a long term complication of reflux, the
normal squamous mucosa of the oesophagus becomes replaced by glandular mucosa: ?stem cell differentiation
• Clinical importance is when it is replaced by intestinal-type cells, esp goblet cells: intestinal metaplasia
• Risk of progression to dysplasia and adenocarcinoma




Barrett’s oesophagus
• Long segment (>3cm)
• Short segment (<3cm)
• Risk of adenocarcinoma in long segment disease is ~30-40X the general population risk
• Risk is proportional to length of disease
• Surveillance programmes

Fungal infection
• Usually Candida
• Normal oral flora
• Colonises, proliferates in oesophagus– Debilitated patients– Immunosuppressed (steroids, HIV, other)– Broad spectrum antibiotics
• Inflammation, erosions, ulceration

Candida oesophagitis

Viral infection
• Usually Herpes simplex virus (HSV)• Usually re-activation• Virus infects squamous cells -> cell death• Vesicles, erosions, ulceration• Clinical setting
– Debilitated patients– Immunosuppressed (steroids, HIV, other)– Can occur in immunocompetent patients

Herpes simplex oesophagitis

Oesophagus: classification by aetiology
• Congenital: atresia, stenosis, fistulas, webs
• Acquired
• Infection: fungal infection, viral infection, Chagas’ disease
• Physical/Trauma: lacerations
• Chemical/Toxic: gastro-oesophageal reflux disease (GORD)
• Circulatory disturbances: oeophageal varices
• Immunological disturbance: eosinophilic oesophagitis
• Degenerative disorders
• Iatrogenic: pill oesophagitis
• Idiopathic: achalasia
• Multifactorial
• Various: radiation, nutritional deficiency, psychosomatic
• Pre-neoplastic/ Neoplastic: Barrett’s oesophagus -> adenocarcinoma squamous cell carcinoma

Achalasia
• “failure to relax”
• idiopathic disorder of muscle of oesophagus
• loss of peristalsis
• increased resting tone of lower sphincter
• loss of normal relaxation with swallowing
• muscular spasm

Manometry in achalasia
Normal Achalasia

Achalasia
• Dysphagia, pain
• Food bolus stuck
• Aspiration
• Mega-oesophagus
• Risk of squamous cell carcinoma

Chagas’s disease
• Infection with Trypanosoma cruzi
• Mexico, Central and South America
• Destruction of nerve plexuses in oesophagus
• Also rest of GI tract, ureter
• Functional impairment similar to achalasia

Mega-oesophagus

Oesophagus: classification by aetiology
• Congenital: atresia, stenosis, fistulas, webs
• Acquired
• Infection: fungal infection, viral infection, Chagas’ disease
• Physical/Trauma: lacerations
• Chemical/Toxic: gastro-oesophageal reflux disease (GORD)
• Circulatory disturbances: oeophageal varices
• Immunological disturbance: eosinophilic oesophagitis
• Degenerative disorders
• Iatrogenic: pill oesophagitis
• Idiopathic: achalasia
• Multifactorial
• Various: radiation, nutritional deficiency, psychosomatic
• Pre-neoplastic/ Neoplastic: Barrett’s oesophagus -> adenocarcinoma squamous cell carcinoma

Pill oesophagitis
• Chemical injury
• Pill temporarily held up in oesophagus
• Contact time
• Chemical nature of medication
• Size, solubility, coating
• Common with KCl, NSAIDs

Oesophagus: classification by aetiology
• Congenital: atresia, stenosis, fistulas, webs
• Acquired
• Infection: fungal infection, viral infection, Chagas’ disease
• Physical/Trauma: lacerations
• Chemical/Toxic: gastro-oesophageal reflux disease (GORD)
• Circulatory disturbances: oeophageal varices
• Immunological disturbance: eosinophilic oesophagitis
• Degenerative disorders
• Iatrogenic: pill oesophagitis
• Idiopathic: achalasia
• Multifactorial
• Various: radiation, nutritional deficiency, psychosomatic
• Pre-neoplastic/ Neoplastic: Barrett’s oesophagus -> adenocarcinoma squamous cell carcinoma

Eosinophilic oesophagitis
• Exposure to allergen -> allergic pattern inflammation (IgE, eosinophils)
• Cow’s milk, soy, egg, often unknown
• Associated with asthma
• Children, young adults

Eosinophilic oesophagitis

Oesophagus: classification by aetiology
• Congenital: atresia, stenosis, fistulas, webs
• Acquired
• Infection: fungal infection, viral infection, Chagas’ disease
• Physical/Trauma: lacerations
• Chemical/Toxic: gastro-oesophageal reflux disease (GORD)
• Circulatory disturbances: oesophageal varices
• Immunological disturbance: eosinophilic oesophagitis
• Degenerative disorders
• Iatrogenic: pill oesophagitis
• Idiopathic: achalasia
• Multifactorial
• Various: radiation, nutritional deficiency, psychosomatic
• Pre-neoplastic/ Neoplastic: Barrett’s oesophagus -> adenocarcinoma squamous cell carcinoma

Oesophageal varices
• Oesophageal submucosal veins connect portal and systemic venous systems
• Normal low pressure gradient between two venous systems (~5mmHg)
• If portal venous pressure increases (portal hypertension), gradient increases (>10mmHg)
• Increased flow in submucosal veins in oesophagus: Can bleed massively

Oesophageal varices

Oesophagus: classification by aetiology
• Congenital: atresia, stenosis, fistulas, webs
• Acquired
• Infection: fungal infection, viral infection, Chagas’ disease
• Physical/Trauma: lacerations
• Chemical/Toxic: gastro-oesophageal reflux disease (GORD)
• Circulatory disturbances: oeophageal varices
• Immunological disturbance: eosinophilic oesophagitis
• Degenerative disorders
• Iatrogenic: pill oesophagitis
• Idiopathic: achalasia
• Multifactorial
• Various: radiation, nutritional deficiency, psychosomatic
• Pre-neoplastic/ Neoplastic: Barrett’s oesophagus -> adenocarcinoma squamous cell carcinoma