NOTES: CH 42, part 1 (Circulation in Animals)
Transcript of NOTES: CH 42, part 1 (Circulation in Animals)

NOTES: CH 42, part 1
(Circulation in Animals)

● Diffusion alone is NOT adequate for
transporting chemicals over distances in
animals
● The circulatory system ensures that no
substance must diffuse very far to enter
or leave a cell

The circulatory system…
provides oxygen and nutrients to tissues
and removes wastes.

STRUCTURE OF THE HEART
Size:
● about 14 cm long and 9
cm wide
Location:
● 2/3 left of midline
● below 2nd rib and rests
on diaphragm

STRUCTURE OF THE HEART
Heart Covering:
● fibrous, outer pericardium:
parietal pericardium
● serous, inner pericardium:
visceral pericardium
● space between the layers =
pericardial cavity (cushions
and lubricates heart)

4 Heart Chambers: (heart is divided into right and left sides)
● RIGHT:
RIGHT ATRIUM receives blood from the superior and inferior venae cavae and coronary sinus
pumps blood into the RIGHT VENTRICLE
right ventricle pumps blood out of the heart into the PULMONARY ARTERIES (take blood to the lungs)

● LEFT:
LEFT ATRIUM
receives blood from the
pulmonary veins (from
the lungs)
pumps blood into the
LEFT VENTRICLE
left ventricle pumps
blood out of the heart
into the AORTA (takes
blood to all of the body)

Heart Valves: designed to prevent backflow of blood!
ATRIOVENTRICULAR VALVES:
-TRICUSPID VALVE: separates R atrium from R ventricle
-BICUSPID VALVE(a.k.a. MITRAL VALVE): separates L atrium from L ventricle

● Structure of AV valves:
-CHORDAE TENDINAE: strong fibrous
structures that attach to the flaps of the
valves
-PAPILLARY MUSCLES:
muscles embedded
in the endocardium;
attach to the
chordae tendinae

SEMILUNAR VALVES:
-PULMONARY VALVE:
separates R ventricle
from pulmonary arteries
-AORTIC VALVE:
separates L ventricle
from aorta

Path of Blood Through the Heart:
● blood low in oxygen and high in CO2
enters the RIGHT SIDE through the venae
cavae and is then pumped into
pulmonary circulation (to the lungs)

Path of Blood Through the Heart:
● after blood is oxygenated
in the lungs, it returns to
the LEFT SIDE through
the pulmonary veins and
is then pumped into
systemic circulation via
the aorta (to the body)


Heart Blood Supply:
● the CORONARY ARTERIES supply blood
to the myocardium
● blood returns to the R atrium through the
cardiac veins and coronary sinus

**500,000 Americans die per year of
coronary artery disease
**3.5 million Americans have coronary
problems

Cardiac Cycle
● ATRIAL SYSTOLE: atria
contract while the ventricles relax
(VENTRICULAR DIASTOLE)
● VENTRICULAR SYSTOLE:
ventricles contract while the atria
relax (ATRIAL DIASTOLE)
● all chambers relax for a brief
period…; then the cycle repeats!

Diastole Systole

Initiation of Cardiac Cycle:
● electrical impulses originate in the SA
node: stimulate the atria to contract
● impulses pass slowly to the AV node,
then to the Purkinje fibers: stimulate the
ventricles to contract



ELECTROCARDIOGRAM (ECG):
● records the electrical changes in the
myocardium during a cardiac cycle
● the pattern has several characteristic
waves:
1) P wave: atrial depolarization
2) QRS complex: ventricular
depolarization
3) T wave: ventricular repolarization



Regulation of Cardiac Cycle:
● heartbeat is affected by:
-physical exercise
-body temperature
-concentration of ions (calcium, potassium)

Blood Vessels and
Blood Pressure

Blood vessels form
a closed circuit of
tubes that carry
blood from the
heart to body cells
and back again.

ARTERIES and ARTERIOLES
● Arteries are adapted to carry blood under
HIGH PRESSURE away from the heart.
● Arteries eventually
branch into smaller
structures called
ARTERIOLES


CAPILLARIES
● smallest diameter blood vessel
● connect arterioles to venules
● capillary wall = a single layer of cells; forms a semipermeable membrane

RBCs in a
capillary!

CAPILLARIES● tissues that use more
energy/oxygen have the most
capillaries (i.e. muscle tissue,
nerve tissue)
● tissues that use less
energy/oxygen have the
fewest capillaries (i.e.
epidermis, cartilage)

Exchanges in Capillaries:
● blood in capillaries drops off
their nutrients and oxygen in
exchange for metabolic
wastes (CO2, etc.)
● large molecules (e.g. plasma
proteins) remain in the blood
● most materials move across
the capillary wall by
DIFFUSION

VEINS and VENULES
● VENULES continue from capillaries and merge with VEINS
● veins carry blood TOWARD THE HEART
● venous walls are similar in structure to artery walls, but thinner and contain less muscle tissue


ARTERIES
-carry blood
away
from heart
-largest artery =
AORTA
ARTERIOLES
CAPILLARIES
-walls are only
1 cell thick
VENULES
VEINS
-carry blood to the
heart
-thinner walls
-are less muscular
than arteries

BLOOD PRESSURE:
Blood pressure is the force blood exerts
against the sides of blood vessels.

BLOOD PRESSURE:
● SYSTOLIC PRESSURE: pressure produced in the arteries when the ventricles contract; highest pressure
● DIASTOLIC PRESSURE: pressure in the arteries when the ventricles are relaxed

Venous blood pressure is much lower than arterial
blood pressure…how does blood flow through
veins (in some cases, against gravity?)
skeletal muscle contractionsqueezes blood from one segment to the next
breathing movements change pressure in thoracic and abdominal cavities pulling/pushing blood upward toward the heart
VALVES prevent blood from flowing backward into a previous segment

2 MAJOR PATHS OF CIRCULATION:
● PULMONARY CIRCUIT: vessels that
carry blood from the heart to the lungs
and back
R ventricle pulmonary trunk R and L
pulmonary arteries arterioles and
capillaries in the R and L lungs venules
veins pulmonary veins L atrium


2 MAJOR PATHS OF CIRCULATION:
● SYSTEMIC CIRCUIT: carries blood from the heart to all other body parts and back again; includes coronary circulation
L atrium L ventricle aorta various arteries, arterioles, capillaries in body tissues venules veins superior and inferior venae cavae R atrium


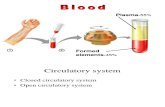
BLOOD AND BLOOD CELLS
Blood can be separated into:
• Formed elements:
-mostly red blood cells (RBCs)
-include white blood cells (WBCs) and platelets
• Liquid portions = PLASMA
-transports water, gases, nutrients, hormones,
electrolytes, and cellular wastes

Red Blood Cells (RBCs)
• contain HEMOGLOBIN,
which combines with oxygen
• hemoglobin synthesis requires IRON

White Blood Cells (WBCs)
• function in defense against disease
• also called: LEUKOCYTES
• WBCs include:
neutrophils monocytes
eosinophils lymphocytes
basophils

White Blood Cells (WBCs)
• normal WBC count is 5,000 – 10,000 cells
per mm3 of blood
this number may vary in response to
infection, emotional disturbances, loss of
body fluids, leukemia

Platelets
• fragments of larger cells
• help close breaks in blood vessels / clot
the blood

PLASMA
Plasma transports gases and nutrients,
helps regulate fluid and electrolyte
balance, and helps maintain a stable pH.

PLASMA
Gases in plasma:
-oxygen
-carbon dioxide
-nitrogen
Plasma nutrients:
-simple sugars
-amino acids
-lipids

ABO Blood Group:
• blood is grouped according to the presence or
absence of antigens A and B.
Type A = A antigens; plasma has anti-B antibodies
Type B = B antigens; plasma has anti-A antibodies
Type AB = A and B antigens; no antibodies
Type O = neither antigen; both anti-A and B antibodies


ABO Blood Group:
• mixing RBCs that contain an antigen with plasma that contains the corresponding antibody results in a negative reaction (AGGLUTINATION)
*the anti-A and anti-B
antibodies are too large
to cross the placenta,
so mother and child can
safely have different ABO blood groups


Rh Blood Group:
• Rh-positive blood: RBCs possess the Rh antigens
• Rh-negative blood: RBCs do not possess the Rh antigens, but DO possess anti-Rh antibodies
RESULT: mixing Rh-positive RBCs with plasma that has the anti-Rh antibodies can result in agglutination

Rh Blood Group:
*the anti-Rh antibodies are small enough to
cross the placenta…
So, the anti-Rh antibodies in a mother’s
blood could react with the RBCs of an Rh-
positive fetus

The “Rh Issue”…
Mom = Rh-; Baby #1 = Rh+

A note
about blood
pressure…

How do we measure B.P.?
● To measure arterial blood pressure, we
use a device known as a
sphygmomanometer …
…GUESS WHAT…????

SPHYGMOMANOMETER!
***word #5 on my list!!!...the list is complete!
1) Okazaki fragments
2) plasmodesmata
3) cholecystokinin
4) acetylcholinesterase
5) sphygmomanometer
6) rubisco
7) chaperonins
8) Islets of Langerhans
9) Batesian mimicry
10) nodes of Ranvier

SPHYGMOMANOMETER:
● This device consists of an inflatable cuff
connected by rubber hoses to a hand
pump and to a pressure gauge.
● The cuff is wrapped around the upper arm
and inflated to a pressure greater than the
expected systolic pressure, thus closing
down the brachial artery in the arm.

SPHYGMOMANOMETER:
● The examiner
places the bell of a
stethoscope in the
inside of the elbow
below the biceps
muscle to pick up
the sounds of the
blood in the artery as
the pressure in the cuff is allowed to fall.
(This is done gradually by opening a screw valve
next to the hand pump.)

SPHYGMOMANOMETER:
● At first there is no sound; then, a sharp, tapping
sound of blood spurting through the partially-
opened artery at systolic pressure;
● and ultimately, no sound as even the low-
pressure blood (@ diastolic pressure) can get
through the completely open artery.
**(The various sounds heard with the stethoscope
are known as the sounds of Korotkoff.)



BLOOD PRESSURE:
● Blood pressure is recorded as: systolic pressure (mm Hg) / diastolic pressure (mm Hg).
● A normal blood pressure measurement for a given individual depends on the person’s age, sex, heredity, emotional state, body weight, etc.
● For young men and women at age 17-18, the normal BP’s will range from 100-120 mm Hg systolic pressure, and from 60-80 mm Hg diastolic pressure.

“Is my blood pressure too high?”
● One “high” BP reading may not indicate a health problem;
● BP needs to be measured over several days at different times of the day by a health care professional before a true measure is achieved.
● Blood pressure measurements that arechronically elevated may indicate poor cardiovascular health.
● This condition, called hypertension, is a major contributor to heart disease and stroke.