Management of Brain Metastases and Superior Vena Cava Syndrome(1)
-
Upload
belthazorsg -
Category
Documents
-
view
8 -
download
0
description
Transcript of Management of Brain Metastases and Superior Vena Cava Syndrome(1)

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 1/45
Recognising and managing a
patient with brain metastasisPalliative Medicine Lecture Series
Dr Chay Wen Yee

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 2/45
• Signs and Symptoms – Neurological deficits – Seizures – Giddiness/Headache – Confusion, drowsiness – Change in Mentation – Gradual onset vs stroke sudden
Brain metastases

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 3/45
• Differential Diagnosis – Intracranial events – Sepsis – Metabolic – Drugs (e.g. morphine)
Brain metastases

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 4/45
Brain Metastases & Raised ICP
Mayo Clin Proc (2006) 81:835-848

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 5/45
Mdm CMK• 32 chinese female• Previously diagnosed with L breast Ca (T1b N1 M0 ) after
she self palpated breast lump• - WEAC done 2006• - histo 10 mm , 1/10 LN positive , SBR Grade 3 , extensive
LVSI , margins -ve• - ER /PR -ve Her2Neu -ve ie triple negative• - s/p AC #4 then RT
• Currently admitted from clinic May 2010 for• headache last 3 months• Any further history you would like to take?

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 6/45
Mdm CMK• 32 chinese female• Previously diagnosed with L breast Ca (T1b N1 M0 ) after she self palpated
breast lump• - WEAC done 2006• - histo 10 mm , 1/10 LN positive , SBR Grade 3 , extensive LVSI , margins -
ve• - ER /PR -ve Her2Neu -ve ie triple negative• - s/p AC #4 then RT
• Currently admitted from clinic May 2010 for• headache last 3 months a/w vomitting• - headache worse on straining during BO• - otherwise no visual disturbances / diplopia• - no focal neurological signs• - no fits

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 7/45
• Patient alert• Afebrile• VS stable•
H S1S2• L clear• A soft NT no HPM• moving all 4 limbs• no sensory deficit• Left dysmetria

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 8/45
Further investigations you would like toperform?

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 9/45
Further investigations you would liketo perform:
• Hypocount• Baseline CLC•
CT• MRI• If plan for op – preop bloods• Septic workup if infection is a differential

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 10/45
• CT brain: Left cerebellar rim enhancing lesions compatiblewith metastases. There is some mass effect on to the 4thventricle and the left quadrigeminal cistern is effaced.
• - MRI brain : A solitary lobulated rim enhancing cystic lesion
in the left cerebellar hemisphere represents a cerebralmetastasis. Associated perilesional oedema is seen withsome mass effect on the 4th ventricle but nohydrocephalus is identified. Some old blood product withinthis cerebellar metastasis is also noted
• CT T/A/P : Metastatic deposits to the right lung upper lobeand right hilar nodal station and the left iliac bone arenoted.

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 11/45
CT Brain

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 12/45
MRI brain

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 13/45
• - patient started on IV dexamethasone andreferred to NES and TRD
• CT T/A/P : Metastatic deposits to the rightlung upper lobe and right hilar nodal stationand the left iliac bone are noted.
• - S/B Neurosurgery : offered surgery• - S/B Radiation Oncology with plan is to offer
RT to patient after surgery

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 14/45
Case 2• Metastatic colon Ca dx August 2009.• OGD: normal; colonoscope 12/8/09: sigmoid Ca (malignant
stricture); CEA 12/08/09: 28.1• - underwent left hemicolectomy on 24/8/09.• Histo: Moderately differentiated adenocarcinoma reaching
pericolonic fat ( pT3). 16 benign lymph nodes.• - Post-operatively Xelox #2, underwent liver resection ( left
hemihepatectomy and segment VI resection 3/12/2009) then Xeloxx 6 cycles
• Histo: Metastatic adenocarcinoma.• - noted lung nodules Sep 2010 s/p #4 Xeliri• -PD at anastomotic site, s/p extended AR in April 2011 subsequently
declined further chemo

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 15/45
• Currently admitted for• 1) Left sided weakness x1/52• -unable to raise arm or leg•
-a/w numbness• -acute in onset, no preceding fall or head injury• 2) Drowsiness x 1 day• -no fever, chills or rigors• -no URTI or abdo pain• -no headache, visual distubance

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 16/45
MRI Brain

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 17/45

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 18/45
• Management – IV Steroids - reduces oedema & provides symptomatic relief – Consider iv Mannitol – effective within min; last several
hours – Whole brain RT (whether or not op done) – Refer Neurosurgery for decompression/ VP shunt if:
• Solitary brain met• Large brain metastasis• Posterior fossa lesion• Hydrocephalus
Brain metastases

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 19/45
• Then patient’s son starts to press the call bellurgently as patient appears to be jerking….

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 20/45
Management of fits• Ensure respiratory and circulatory status ( and supportive
therapy eg mechanical ventilation given as needed)• Blood sugar level – ensure fits not due to hypoglycemia• Benzodiazepines eg diazepam 0.1 – 0.3 mg/kg ( stat dose
either IV or rectal suppository) for rapid control• Phenytoin ( given up to 20mg/kg)
– Increased risk of hypotension and cardiac arrthymias with fasterinfusion rates
– Cardiac monitoring required• IV midazolam infusion/ use of barbiturates if statusepilepticus• More details on fit management coming up from Pall med
lecture by Dr D Watkinson later…

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 21/45
• Thank you and any questions?

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 22/45
Pericardial Tamponade

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 23/45
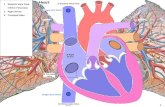
Pericardial Tamponade
Signs and SymptomsBreathlessness, chest pain, orthopnoea, lethargyBeck’s Triad tamponade
Raised JVPMuffled heart soundsHypotension
Pulsus Paradoxus

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 24/45
DiagnosisCXR: GLOBULARheart with distinct heartbordersECG small voltages
Small bilateral pleural effusions
*ACC/AHA definition for low QRS voltage is amplitude<5mm in standard limb leads or <10mm in precordialleads
Pericardial Tamponade

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 25/45

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 26/45

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 27/45
Confirmatory Diagnosis2DE – separation of pericardial layers can be detectedwhen fluid exceeds 15 – 35 ml; early diastolic collapse ofRV wall (tamponade)CT Chest
Pericardial Tamponade

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 28/45
Acute pericardial tamponade with diastolic collapse of theRV wall

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 29/45

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 30/45
ManagementIV Drip to maintain intravascular volume
Avoid diuretics
Refer to CVM and CTSPericardial windowIn the meantime - pericardiocentesis
Pericardial Tamponade

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 31/45
Superior Vena Cava Obstruction

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 32/45
Superior Vena Cava Syndrome

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 33/45
Superior Vena Cava Obstruction
>90% caused by malignant tumors85% by lung cancer (small cell lung cancer, squamous-cell lung cancer)Malignant lymphomas<2% thymoma or germ cell tumorsOther metastatic tumors
Non-malignantLong-term central venous catheters, thrombosis

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 34/45
SymptomsSOB 63%Facial swelling 50%Cough 24%
Arm swelling 18%Chest pain 15%Dysphagia 9%
Symptoms may be aggravatedby bending forward, stoopingor lying down
SignsNeck veins distended66%Venous distension ofchest wall 54%Facial oedema 46%Stridor from laryngealoedemaCyanosis 20%Facial plethora 19%Oedema of arms 14%Papilloedema
Superior Vena Cava Obstruction

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 35/45
Investigations
CXR- superior mediastinal widening and pleuraleffusion most common
CT Chest
Superior Vena Cava Obstruction

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 36/45
Rarely causes life threatening situationExcept with sudden obstruction leading to brain edema
>50% symptomatic before cancer diagnosis made
Superior Vena Cava Obstruction

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 37/45

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 38/45

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 39/45

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 40/45

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 41/45
Management: Relieve symptoms + treat underlyingcause
ABCs of resuscitation
OxygenNurse at 45Diuretics (iv lasix 40mg) if SBP >100mmHgIV dexamethasone 8mg tds (withhold in patientswithout histological diagnosis as may precipitate tumorlysis syndrome in eg. lymphoma)IV in lower limbs
Superior Vena Cava Obstruction

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 42/45
If goal is palliative or when urgent treatment ofvenous obstruction is required:
Radiation therapy to lesion is primary treatmentEndovascular stenting and angioplasty +/-thrombolysisSurgery (rare)
Superior Vena Cava Obstruction

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 43/45
50% of malignant causes due to small cell lung ca,lymphoma, germ cell tumours- all are chemo-sensitive tumors and potentially curable – chemowill be primary treatment
If 1st presentation and no diagnosis esp in youngpts where lymphoma likely – intubate if necesssaryto protect airway and obtain biopsy
Superior Vena Cava Obstruction

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 44/45
Chemotherapy- malignant lymphoma
- small cell lung carcinoma
- chemo-naïve non-small cell lung carcinomaSignificant response: 1-2 wks
Radiotherapy
- recurrent non small cell lung ca
- chemo-insensitive tumour
Significant response: 2 wks
Superior Vena Cava Obstruction

7/21/2019 Management of Brain Metastases and Superior Vena Cava Syndrome(1)
http://slidepdf.com/reader/full/management-of-brain-metastases-and-superior-vena-cava-syndrome1 45/45
Nursing care
• Assessment of worsening neurological,pulmonary and cardiac function
• Elevation of HOB, oxygen and allaying anxiety• Decrease exertion• Fluid balance