Learning Objectives - CMEinfo...Sep 01, 2020 · PE: FUTURE MI/ STROKE: 16,925 PE; 65,793 controls...
Transcript of Learning Objectives - CMEinfo...Sep 01, 2020 · PE: FUTURE MI/ STROKE: 16,925 PE; 65,793 controls...

Contemporary Management of VTE
Samuel Z. Goldhaber, MD
Associate Chief and Clinical Director
Division of Cardiovascular Medicine
Brigham and Women’s Hospital
Professor of Medicine
Harvard Medical School
DISCLOSURES
Research Support:
Bayer; Boehringer-Ingelheim; BMS; Boston Scientific BTG EKOS; Daiichi; Janssen; NHLBI
Consultant:
Agile; Bayer; Boehringer-Ingelheim

Learning Objectives
•Epidemiology—PE mortality, COVID•Pathophysiology—Inflammation; PE links MI, stroke, and HF
•Optimal duration of anticoagulation•Cancer and VTE—DOACs•Advanced therapy beyond heparin—
systemic and catheter lysiscatheter/ surgical embolectomy
(Woolf SH. JAMA 2019; 322: 1996-2016)
Age-Adjusted Mortality in the USA:Increasing since 2015

Socioeconomically Disadvantaged
•Decline in life expectancy is greater among individuals with limited education and income.
•The gradient in life expectancy based on income has widened over time.
(Woolf SH. JAMA 2019; 322: 1996-2016)
2000—Age 732017—Age 68
All-cause and PE mortality: Increasing in the USA,
but decreasing in Canada/ Europe
Median Age of Death from PE in the USA
(Barco S, et al. Lancet Resp Med 2020; in press)

PE Mortality Over Time: USA vs. Canada
PE-Related Mortality: 2000-2015
(Barco S, et al.Lancet Resp Med 2020; in press)

PE: Underlying vs. Contributing Cause of Death
1-Year PE Mortality among Socioeconomically Disadvantaged
(Wadhera R…Goldhaber SZ. JAMA Cardiology 2020; submitted

COVID-19
New COVID Cases: CDC

Corona-VTE (N=1114): MACE
(Piazza G…Goldhaber SZ. JACC 2020; in press)
Corona-VTE (N=1114): Symptomatic VTE
(Piazza G…Goldhaber SZ. JACC 2020; in press)

Corona-VTE (N=1114): Summary
(Piazza G…Goldhaber SZ. JACC 2020; submitted)
COVID Coagulopathy
• Decreased platelets
• Increased D-dimer, fibrinogen, prothrombin time, FDPs
• Increased factor VIII levels
(Spyropoulos AC, Weitz JI. Circulation 2020; 142: 129-132)

Hemostatic Abnormalities and Adverse Clinical Outcomes
(Bikdeli B, et al. JACC 2020; 75: 2950-2973)
VTE in COVID Patients
1) PE >> DVT
2) Rate of PE in COVID ICU patients can exceed 20%
3) In situ thrombosis with microthrombi in lung arteries
4) “Breakthrough” VTE in-hospital, despite standard VTE prophylaxis

COVID Autopsy Findings
(Fox SE. Lancet Respir Med 2020; 8: 681-686)
Bilateral pulmonary edema
Thrombi in small
peripheral vessels
RV Dilatation
COVID Microscopy Findings
Enlarged Pneumocytes
Multinucleated; Virally Infected
Cardiac Myocytes; Focal Degeneration(black arrows)
NETs; red=dsDNA;green=RNA
Normal Lung
(Fox SE. Lancet Respir Med 2020; 8: 681-686)

ARDS: Transudative fluid in hyaline membrane of alveolus
ARDS: Activated macrophages and viral inclusion bodies
RVThrombus(Yellow Box Delineates“Chevron”)

Thrombus in Pulmonary Venule
VTE Dosing Weight Adjustment
CrCl ≥ 30mL/min CrCl < 30mL/min
StandardEnoxaparin 40mg
BIDUFH 7,500 units
Q8H
Obese (> 120kg or BMI > 35)
Enoxaparin 0.5mg/kg BID
(max dose 100mg BID)
UFH 10,000 units Q8H
Low Body Weight (< 60kg)
Enoxaparin 30mg BID
UFH 7,500 units Q8H
Revised BWH ICU VTE Prophylaxis Dosing – COVID
Do not use therapeutic dose anticoagulation unless clinically indicated

AGE-ADJUSTED D-DIMER (>50 y.o.)
• (Adjusted for age) D-dimer upper limit of normal in those > 50 y.o. is:
10 X Age (in years) ng/ml
• Accurate in ADJUST-PE Trial
• 5-times as many negative D-dimer tests in patients > 75 y.o. using this adjusted definition of normal D-dimer
(JAMA 2014; 311: 1117-1124)

Inflammation-Linked Conditions that Can Trigger PE or DVT
• Ulcerative colitis/ Crohn’s disease
• Rheumatoid arthritis/ psoriasis
• Elevated LDL cholesterol or LP(a)
• Obesity/ metabolic syndrome
• Acute coronary syndrome/ stroke
• Pneumonia/ COPD
• Cigarette smoking
PE: FILLED WITH WBCs and PLATELETS—INFLAMMATION
(Savchenko AS.J Thromb Haemostas2014; 12: 860-870)

Secreted Mitochondria From Activated Platelets Promote Inflammation
(Boudreau LH. Blood2014; 124: 2173-2183)
DUAL TARGETS:FIBRIN AND PLATELETS

COMMON PATHOPHYSIOLOGY: VTE AND ATHEROSCLEROSIS
(Piazza, Goldhaber. Circulation 2010;121: 2146)
Shared Risk Factors• Obesity• Hypertension• Tobacco Use• Dyslipidemia
• Diabetes• Diet• Stress• Estrogen Therapy
PE: FUTURE MI/ STROKE:16,925 PE; 65,793 controlsAdjusted Relative Risk of Future
MI or Stroke after Acute PECondition 1 Year 2-20 Yrs
Acute MI 2.60 1.32
Stroke 2.93 1.29
(Sorensen HT. Lancet 2007; November 24)

VASCULAR MEDICINE PERSPECTIVE ON PE
PE
MI
HF
MI
PE
HF
Stroke
Stroke
Inflammation: A Common Underlying Process
Samuel Z. Goldhaber J Am Coll Cardiol 2020;75:159-162
2020 American College of Cardiology Foundation
Heart Failure: Linked to Incident VTE
(Goldhaber SZ. JACC 2020; 75: 159-162)

Optimal Durationof Anticoagulation To
Prevent Recurrent VTE
Requiem for “Provoked”/ “Unprovoked” VTE
2019 ESC PE Guidelines
“Terminology such as ‘provoked’ vs. ‘unprovoked’ PE/ VTE is no longer supported by the Guidelines, as it is potentially misleading and not helpful for decision-making regarding the duration of anticoagulation."
(European Heart Journal 2019; epubl August 31)

ESC: Anticoagulation Duration
(European Heart Journal 2019; epubl August 31)
“Extended oral anticoagulation of indefinite duration should be considered for patients with a first episode of PE and:
1) No identifiable risk factor
2) A persistent risk factor
3) A minor transient or reversible risk factor”
Risk of Recurrent VTE:Danish Cohort Study (N=73,993)
6 Months
6 months
(Albertsen IE. Am J Med 2018; 131: 1067-1074)

VTE Subtype: Event-Free SurvivalFramingham Heart Study (N=9,754)
Unprovoked
Provoked
Cancer
(Puurunen MK. Thromb Res 2016; 145: 27-33)
EINSTEIN CHOICE: 60% PROVOKED and 40% UNPROVOKED VTE—PREVENTING RECURRENCE
(Weitz JI. Thromb Haemost 2015; 114: 645-650)
N=3,396

EFFICACY: RIVAROXABAN20 MG vs. 10 MG vs. ASPIRIN
(Weitz JI. NEJM 2017; 376: 1211-1222)
PROVOKED RISK FACTORS PREDISPOSE TO RECURRENCE“Minor Persistent”:
• Heart failure
• Obesity
• Chronic kidney disease
• Family history of VTE
• Hereditary thrombophilia
“Minor Transient”: Immobility(Prins MH, Blood Advances 2018; 2: 788-796)

2019 ESC PE Guidelines: Risk of Recurrent VTE
(European Heart Journal 2019; epubl August 31)
Risk of Recurrence
Risk Factors for Index VTE Examples
Low (<3%/ year) Transient, reversible factors; >10-fold increased risk of index VTE
Major surgeryMajor trauma
Intermediate (3% to 8%/ year)
Transient, reversible factors; ≤10-fold increased risk of index VTE
Minor surgeryHospitalized with acute medical illnessPregnancy/ estrogensLong-haul flight
Persistent risk factors IBD; Autoimmune Disease
No identifiable risk factor
High (>8%/ year) Active cancerAntiphospholipid syndrome
CAN DOACS REPLACE
LMWH MONOTHERAPY
IN CANCER PATIENTS
WITH VTE?

CHALLENGES ANTICOAGULATING CANCER PATIENTS WITH VTE
• Cancer is thrombogenic: High rates of recurrent thrombosis despite A/C
• Cancer chemotherapy is also thrombogenic and thrombocytopenic
• Occult metastases are bleeding sources
• Interactions among anticoagulants and novel chemotherapeutic agents—uncharted territory
• Frailty
DALTEPARIN HALVES VTE RECURRENCE IN CANCER
PATIENTS (vs. warfarin) (N=676)
(NEJM 2003; 349:146-153)
CLOT TRIAL

CANCER / ACUTE VTE:DOAC vs. Dalteparin
DOAC Trial Result
Edoxaban(Hokusai)
Better efficacy; Less GI safety
Rivaroxaban(SELECT-D)
Better efficacy; Less GI safety
Apixaban(Caravaggio)
Same efficacy; Same safety
ADVANCED THERAPY:
Beyond Anticoagulation Alone: Thrombolysis, Surgical or Catheter
Embolectomy

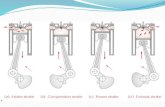
RV Pressure Overload
RV Dysfunction
LV Preload
RV Ischemia or Infarction
LV Cardiac Output
SystemicPressure
RV Wall Tension
CoronaryPerfusion
PE PATHOPHYSIOLOGY

PE RESPONSE TEAM (PERT)PERT Team Activationvia Paging System
PERT Evaluation by On‐Call Physician
Web‐Based Video Conference
Discussion and Consensus
Vascular Medicine
Interventional Cardiology
PulmonaryCritical Care
Echocardiography
Cardiothoracic Surgery
Radiology
Options and Recommendations Presented to the Patient, Family, and Care Team
ACTION
(Dudzinski D, Piazza G. Circulation 2016; 133: 98-103)
PE THROMBOLYSIS1. Systemic thrombolysis:
a) 100 mg/2h (“full dose”) TPA (FDA Approved 1990)
2. Catheter-directed, Ultrasound-facilitated TPA 24 mg (“1/4 dose”)
(FDA Approved 2014)3. OPTALYSE-PE Dose: TPA 8 mg/2h
(“< one-tenth dose”) (JACC Cardiovasc Interventions 2018)
4. Catheter Embolectomy without TPA(“zero dose TPA”)


TPA 12 mg TPA 12 mg
TPA 24 mg/12h = total TPA dose
RV/LV Ratio: Pre- and Post-Procedure
RV/LV = 2.5 RV/LV = 0.7Courtesy of Keith M. Sterling, MD
Pre Post

OPTALYSE PE—DOSE STUDYwith BILATERAL PA CATHETERSDOSE per CATHETER (N) RV/ LV RATIO
at 48h (%)
2 mg/h X 2h=8 mg TPA (26) -0.40 (24%)
1 mg/h X 4h=8 mg TPA (26) -0.35 (23%)
1 mg/h X 6h=12 mg TPA (27) -0.42 (26%)
2 mg/h X 6h=24 mg TPA (18) -0.48 (26%)
(Tapson V…Goldhaber SZ. JACC Cardiovasc Interventions 2018; 11: 1401-1410)
Large-Bore Aspiration Mechanical Thrombectomy: (No TPA Needed) (N=46)
(Wible BV. J Vasc Interv Radiol 2019; epubl July 30)

FlowTriever: FLARE Study(N=106 from 18 U.S. sites)
RV/LV Ratio Pre and Post Rx
(Tu, T. JACC CV Interventions 2019;12: 859-869)
BWH FlowTriever Pulmonary Embolectomy

Benefits1) Rapidly optimize BP, RV2) Maximize clot removal3) 2%: Mortality in non-CPR patients
Risks1) 18%: Ventilator > 72 hours2) 18%: Hemodialysis required3) 25%: Mortality in CPR patients
ECMO and/or Surgical Embolectomy
(Goldhaber SZ. JACC 2020; 76: 912-915)
ECMO and/or Surgical Embolectomy
Venoarterial Extracorporeal Membrane Oxygenation Circuit
(Guglin M. JACC 2019; 73: 698-716)

VA-ECMO for PE: Rest the heart and lungs or lyse or operate
(Guglin M. JACC 2019; 73: 698-716)
BWH Surgical Embolectomy

Betrixaban1) FDA approval: 20172) Reduce MACE3) Reduce rehospitalization
Betrixaban1) EMA refusal: 20182) ASH strong recommendation
against out-of-hospital VTE prophylaxis: 2018
3) Low absolute reduction in VTE4) Poor U.S. market penetration5) Cost-benefit analysis did not
convince clinicians
Rivaroxaban1) FDA approval: 20192) Reduce MACE3) Clinician familiarity: 23%
market share and > $2B sales per year in USA
Rivaroxaban1) FDA checklist of major
bleeding exclusions is too complicated to deal with
2) 1% absolute VTE reduction is not enough to spawn “local champions” at US hospitals
3) Hospital budgets strained post-COVID-19
Proactive Inertia
Uphill Battle
Out-of-Hospital VTE Prophylaxis: Easier Said
Than Done
(Goldhaber SZ. JACC 2020; 75: 3148-3150)
VTE Prophylaxis: Hospital Discharge
CONCLUSIONS1. The age-adjusted overall mortality rate and PE
mortality rate are increasing in the USA.
2. Beware: COVID-19: high rate of PE in ICU pts.
3. PE confers increased risk of MI/ stroke.
4. Provoked VTE predisposes to almost as much recurrence as unprovoked VTE, after D/C AC.
5. Consider extended duration AC in most VTE patients rather than a fixed “stop date.”
5. Consider DOACs > LMWH: non-GI cancer pts.
6. Advanced therapy: thrombolysis,catheter or surgical embolectomy, ECMO