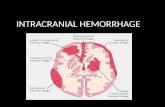
Progression of Intracranial Hemorrhage after Acute Head Injury
Intracranial hemorrhage newborn
-
Upload
singarampaed -
Category
Documents
-
view
4.631 -
download
2
description
Transcript of Intracranial hemorrhage newborn

INTRACRANIAL HEMORRHAGE IN
NEWBORNS


OVERVIEW Incidence varies from 2% to >30% in
newborns
depends on the gestational age (GA) at birth and the type of ICH
Diagnosis typically depends on clinical suspicion
The presence and severity of parenchymal injury is the best predictor of outcome

SUBDURAL HEMORRHAGE (SDH)
Rupture of the draining veins and sinuses of the brain
molding, fronto-occipital elongation, and torsional forces acting on the head during delivery
provoke laceration of dural leaflets of tentorium cerebelli or falx cerebri

Often results from trauma in the full-term infant
SDH in the supratentorial space results from rupture of the bridging veins

ETIOLOGY large head size, rigid pelvis (e.g., in a primiparous or
older multiparous mother), nonvertex presentation (breech, face,
etc.), very rapid or prolonged labor or
delivery, difficult instrumental delivery, or rarely, a bleeding diathesis

CLINICAL PRESENTATION Large collection especially in
infratentorial SDH results in rapid deterioration.
Systemic signs like hypovolemia and anemia
Seizures may occur in up to half of neonates with SDH, particularly with SDH over the cerebral convexity

DIAGNOSIS suspected on the basis of history and
clinical signs and confirmed with a computed tomography (CT) scan.
ultrasonic imaging subdural space is inadequate
MRI- timing of the lesion and for detecting other lesions
Lumbar puncture after CT

MANAGEMENT Most infants with do not require
surgical intervention
prompt stabilization with volume replacement
Open surgical evacuation of the clot in case of large SDH
The outcome for infants with nonsurgical SDH is usually good

SUBARACHNOID HEMORRHAGE (SAH)
Primary SAH is probably frequent but clinically insignificant.
normal “trauma” associated with the birth process.
source of bleeding is usually ruptured bridging veins of the subarachnoid space or ruptured small leptomeningeal vessels

Usual scenario is a well appearing term infant
developing SAH on day 2 or 3 of life

Clinical presentation is similar to other forms of ICH
The diagnosis is best established with a CT scan or MRI, or by LP to confirm or diagnose small SAH
Ultrasonography is not sensitive for the detection of small SAH
Management of SAH usually requires only symptomatic therapy, such as anticonvulsant therapy for seizures

INTRAPARENCHYMAL HEMORRHAGE (IPH) Rare
Intracerebral or intracerebellar variety
More commonly a secondary event
Hypoxic ischemic brain injury, venous infarction or thrombosis, ECMO therapy, large ICH in another compartment

Presentation and management similar to SDH
MRI – extent and age of hemorrhage and other associated parenchymal lesions
LP to rule out meningitis
Symptomatic management
Treat any coexisting pathology or predisposing factors
Monitoring for hydrocephalus

INTRAVENTRICULAR HEMORRHAGE 15-20% at <32 weeks gestation
Venous (or sinus)thrombosis and thalamic infarction in term infants
Related to birth trauma or perinatal asphyxia
No identifiable risk factors in 25%

PRETERM IVH PATHOGENESIS
Intravascular factors
(Pressure passive circulation)
• Ischemia/Reperfusion• Fluctuating or increase
CBF• Increase in cerebral
venous pressure• Platelet dysfunction• Coagulation
disturbances
Vascular factors • Fragile, involuting capillaries with large diameter lumen
Extravascular factors • Deficient vascular support
• Excess fibrinolytic activity

CLINICAL PRESENTATION Usually a clinically silent syndrome in
preterms
Term newborns – seizures, apnea, irritability, lethargy, vomiting, full fontanelle
Catastrophic presentation less likely
Complications

DIAGNOSIS Routine CUS in all infants born at <32
weeks and in older infants at risk for IVH
Days 3,7,30 and 60 days
Monitoring for complications
Grading of GMH/IVH is important for determining management and prognosis

Grading Severity Description
Papile (CT)
IIIIIIIV
Isolated GMH (no IVH)IVH without ventricular dilatationIVH with ventricular dilatationIVH with parenchymal hemorrhage
Volpe (CUS)
I
II
III
Separate notation
GMH with no or minimal IVH (<10% ventricular volume)IVH occupying 10-50% of ventricular area on parasagittal viewIVH occupying >50% of ventricular area, usually distending lateral ventricle
Periventricular echodensity

PREVENTION OF IVH Antenatal steroids
Slow infusion of colloid or hyperosmolar solutions
Avoid rapid fluctuations in CBF and hypotension
Sedative or paralytic medication in ventilated babies

IVH IN PRETERM BABIES Supportive care and watch for
complications
Maintaining Normal BP, electrolytes and blood gases
Transfusions as necessary
Correct thrombocytopenia and coagulation disturbances

IVH IN TERM INFANTS Supportive care and treatment of
seizures
Serial LPs and eventual VP shunts
Prognosis relates to factors other than IVH alone

Monitor OFC and fontanelle daily, Serial CUS q2-7 days to assess ventricle size, shape and RI
No PVD Slowly Progressive Ventricular dilation (over weeks)
Rapidly progressive ventricular dilatation(over days)
No further treatment Close surveillance for 2-4 wk
Dilatation stops Continued dilatation
No therapy, close observation for 1 yr
Serial LP Every 1-3 d, depending on rate of ventricular dilatation

THANK YOU!!