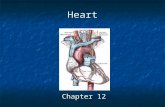
heart and vessels
-
Upload
mark-cofie-nutsukpui -
Category
Documents
-
view
222 -
download
0
Transcript of heart and vessels
-
8/8/2019 heart and vessels
1/97
Husni Rousan 1
CARDIOCARDIO
VASCULARVASCULARSYSTEMSYSTEM
-
8/8/2019 heart and vessels
2/97
Husni Rousan 2
THE HEARTTHE HEART
Anatomy and PhysiologyAnatomy and Physiology
Theheart compose of three layers
Endocardium: the inner layer ofendothelial
tissue
Myocardium: the middle layer of the muscle
fiber responsible for pumping action
Epicardium: the outer layer
it is encased in a thin fibrous sac epicardium
-
8/8/2019 heart and vessels
3/97
Husni Rousan 3
THE HEARTTHE HEART
Anatomy and PhysiologyAnatomy and Physiology
Pericardium consists of Veseral, parital
pericardium layers and space in between,
pericardium space is filled with 30 ml of
lubricating fluid
-
8/8/2019 heart and vessels
4/97
Husni Rousan 4
Heart ChampersHeart Champers
Right heart consists of Rt atrium, Rt ventricle,
distribute deoxygenated blood
Left heart consists of Lt atrium, Lt ventricle ,
distribute oxygenated blood
Varying thickness of a trial and ventricular wall
and left and right ventricles related to work load
-
8/8/2019 heart and vessels
5/97
Husni Rousan 5
Heart ChampersHeart ChampersHEART VALVES:
Atrioventricular, separate atria fromventricles
Semilunar valves ( threehalf-moon
leaflet
-
8/8/2019 heart and vessels
6/97
Husni Rousan 6
Coronary ArteriesCoronary Arteries
Theheart has large metabolic requirement, 70-
80% of delivered oxygen
Coronary arteries are perfused during diastole
Left coronary artery branches ( LAD & LCX )
Right coronary artery branch ( RCA )
Posterior wall received blood by ( PDCA )
-
8/8/2019 heart and vessels
7/97
Husni Rousan 7
CONDUCTING SYSTEMCONDUCTING SYSTEM
cardiac electrical cell is characterized by
Atomicity: ability to initiateelectricalimpulses
Exitability: ability to respond to impulses
Conductivity: ability to transmit impulses( SA AV bundle ofhis bundle branch )
-
8/8/2019 heart and vessels
8/97
Husni Rousan 8
CONDUCTING SYSTEMCONDUCTING SYSTEMPhysiology of cardiac conduction
Electrical activity (ions move acrosscell membrane)
Polarization, Depolarization,
electromechanical coupling andrepolarization
-
8/8/2019 heart and vessels
9/97
Husni Rousan 9
contcont
Cardiac homodynamic
Cardiac cycle ( flow of blood )Cardiac output ( ejection of blood )
= stroke volume x heart rate
Heart Rate: affected by central
nervous system and baroreceptors
-
8/8/2019 heart and vessels
10/97
Husni Rousan 10
cont.cont.
STROKE VOLUME : the amount of blood
ejected by Lt ventricle in each beat which is 70 ml
determined by preload, after load and contractility
EJECTION FRACTION: 42% for right heart
and 50% for the left heart
-
8/8/2019 heart and vessels
11/97
Husni Rousan 11
ASSESSMENTASSESSMENT
Theextent of assessment is determined by:
Purpose of nursing assessment
Severity of pts condition
Practice setting of the nurse
-
8/8/2019 heart and vessels
12/97
Husni Rousan 12
ASSESSMENTASSESSMENT Healthhistory and clinical manifestations
Acute symptoms: current medication,
allergies, general appearance,
homodynamic status
Stable patients: completehistory, spouse
or partner, demographic information
-
8/8/2019 heart and vessels
13/97
Husni Rousan 13
ASSESSMENTASSESSMENTCardiac symptoms: pt will have one of
the followingShortness of breath, dizziness,
syncope, loss of consciousness,
edema and weight gain, fatigue,palpitation and chest discomfort
-
8/8/2019 heart and vessels
14/97
Husni Rousan 14
NURSING DIAGNOSISNURSING DIAGNOSIS
Decrease cardiac output related to structural
disorders
Activity intolerance related to decrease cardiacoutput orexcessive fluid volume
Anxiety related to change in health status and
change in role functionCOLLABRATIVE PROBLEMS
Congestiveheart failure, ventricular
dysrhythmias, and atrial dysrhythmias
-
8/8/2019 heart and vessels
15/97
Husni Rousan 15
PLANNING AND GOALSPLANNING AND GOALS
Improve and maintain cardiac output
Increase activity toleranceReduction of anxiety
Absence of complications
-
8/8/2019 heart and vessels
16/97
Husni Rousan 16
NURSING IMPLEMENTATIONNURSING IMPLEMENTATION
Encourage rest, leaning back in a chair
Oxygen through nasal prongs
Careful monitoring to correlate intervention
with patients response to adjust treatment plan
Decrease sodium diet intake
Change position frequently
-
8/8/2019 heart and vessels
17/97
Husni Rousan 17
PHYSICAL ASSESSMENTPHYSICAL ASSESSMENT
Performed to confirm the data in healthhistoryIt should include the following
Effectiveness ofheart as a pump, filling
volume and pressure, cardiac output,compensatory mechanisms
-
8/8/2019 heart and vessels
18/97
Husni Rousan 18
PHYSICAL ASSESSMENTPHYSICAL ASSESSMENT
General appearance
Level of consciousness, thought
process, heart ability to perfuse brain
tissue, distress and anxiety
-
8/8/2019 heart and vessels
19/97
-
8/8/2019 heart and vessels
20/97
Husni Rousan 20
Pulse pressure:
Difference between systolic and diastolic, 30-40mmhg, reflects strock volume & ejection velocity,
vascular resistance,
Less than 30 mmhg = serious reduction in output
-
8/8/2019 heart and vessels
21/97
Husni Rousan 21
PHYSICAL ASSESSMENTPHYSICAL ASSESSMENT Postural hypotension
Orthostatic hypotension, may indicates low
intravascular volume, inadequate vaso
constrictor mechanism or autonomic
insufficiency
Arterial pressure Rate, rhythm, quality, volume, configration (
contor)
-
8/8/2019 heart and vessels
22/97
Husni Rousan 22
PHYSICAL ASSESSMENTPHYSICAL ASSESSMENT Jugular venous pressure
Reflects Rt heart function, provideestimation
of CVP, increase incase of HF decrease in FVD
Heart
Inspection, palpation, percussion , auscultation,
S1 S2
-
8/8/2019 heart and vessels
23/97
Husni Rousan 23
PHYSICAL ASSESSMENT
Inspection of Extremities
Capillary refill time (CHF, hypertension ),
hematoma (surgery & cath ), vascular changes,peripheral edema, lowerextremeties ulcer
Lungs
Tachypnea ( HF, pain, anxiety ), chynestokesbreathing ( pulmonary edema ), dry cough, crackles
and whezes
-
8/8/2019 heart and vessels
24/97
Husni Rousan 24
PHYSICAL ASSESSMENTPHYSICAL ASSESSMENT Abdomen
Hepatojugular reflux, bladder distention
RISK FACTORS
Nonmodifiable: age, positive family history,
race &gender
Modifiable: hyperglycemia, hyperlipidemia,hypertension, inactivity, smoking, obesity &
type A personality
-
8/8/2019 heart and vessels
25/97
Husni Rousan 25
DIAGNOSTIC EVALUATIONDIAGNOSTIC EVALUATION
Laboratory tests
Cardiac enzymes
Released from injured cells when ruptured
the membrane
Most of them are not specific for one type
of cell
Iso enzymes are more specific, createninekinase ( CK ) and its iso enzyme( CK-MB ),
lactic dehydrogenase (LDH) , troponin I
-
8/8/2019 heart and vessels
26/97
Husni Rousan 26
DIAGNOSTIC EVALUATIONDIAGNOSTIC EVALUATION Blood chemistry
Lipid profile
A- cholesterol (less than 200 mg / dl ),required forhormonal synthesis, found
mainly in brain tissue and liver
B- triglycerides ( 40 150 mg / dl )
source ofenergy, cell wall, store in adipose tissue
-
8/8/2019 heart and vessels
27/97
Husni Rousan 27
DIAGNOSTIC EVALUATIONDIAGNOSTIC EVALUATION C- LDL ( less than 130 mg / dl ) transportcholesterol from blood to peripheral
tissues, synthesized from VLDL
D- HDL ( 35 65 mg / dl M, 35 85 mg/ dl F ) transport cholesterol from
peripheral tissues to the liver, cardio
protectiveeffect, increase withexercise
and decrease with smoking DM and
obesity
-
8/8/2019 heart and vessels
28/97
Husni Rousan 28
Serum electrolytes
K, Na, Ca and otherelectrolytes can reflect theheart
function as well as fluid & electrolyte disturbances
BUN
May indicates impaired renal function and impaired
cardiac output
-
8/8/2019 heart and vessels
29/97
Husni Rousan 29
DIAGNOSTIC EVALUATIONDIAGNOSTIC EVALUATION Coagulation studies
Partial ThromboplastineTime ( PTT ) 25 40 sec, used
to regulateheparin dosage, 1.5 2.5 is the theraputicrange
Prothrombin Time ( PT ) less than 13 sec, used to
regulate warfarin, 1.5 2.5 times ofPT is the theraputic
range
International Normalized Ratio ( INR ) standarized
method for reporting PT level, used for regulating
warfarin dosage
-
8/8/2019 heart and vessels
30/97
Husni Rousan 30
Chest X-Ray ( CXR )Assess size, position of theheart,
cardiothoracic ratio ( CTR ), position of central
lines
Electrocardiography ( ECG )
Can beeither on bed side or from a distance,
12 leads ECG, continuous monitoring,
telemetry monitoring 2 or 3 leads monitoring )
-
8/8/2019 heart and vessels
31/97
Husni Rousan 31
DIAGNOSTIC EVALUATIONDIAGNOSTIC EVALUATION Cardiac Stress Test
During time of increased demand, abnormalities
in cardiovascular functions are more likely tobe detected, used to evaluate theheart function,
coronary arteries as well as the cause of chest
pain
-
8/8/2019 heart and vessels
32/97
Husni Rousan 32
Con.
Exercise stress test: pt walk on a treadmill or
pedals (stationary bicycle), the goal is toincrease HR and monitored for ECH changes,
arrhythmias, hypotension, pain, dyspnea and
dizziness.P
t fast 4 hours before test, nurseneeds to instruct pt about the test
-
8/8/2019 heart and vessels
33/97
Husni Rousan 33
DIAGNOSTIC EVALUATIONDIAGNOSTIC EVALUATION Echocardiography: a non invasive ultrasound used
to examine size shape and cardiac motion, used
also to evaluateheart function, valves andperipheral effusion
Pharmacologic stress test: used for pts
unable to achieve target HR, Dipyridamole,
Adenosine & dobutamine are used for this
purpose
-
8/8/2019 heart and vessels
34/97
Husni Rousan 34
Cardiac catheterizationInvasive diagnostic procedure involves introduction
of specific catheter into Rt & Lt side blood vessels
under fluoroscopy. Its used to evaluate coronary
arteries patency, heart function as a pump, vascularsystem and heart structure
Its considered as a highly critical procedure
Take in consideration: monitoring IV line, BP
, ECG
,LOC, well prepared staff to provide ACLS, revission
of lab tests
-
8/8/2019 heart and vessels
35/97
Husni Rousan 35
CORONARYCORONARYVASCULARVASCULAR
DISORDERSDISORDERS
-
8/8/2019 heart and vessels
36/97
Husni Rousan 36
ATHEROSCLEROSISATHEROSCLEROSIS
Definition: abnormal accumulation of lipid or
fatty substances and fibrous tissues in vessel wall
PathophysiologyIt begins as a fatty streak, this streak develop into
advanced lesion which involves inflammatory
response, T.lymphocytes and monocytes ingest the
lipid and form fibrous cap called Atheroma Plaque,
this protrude into the lumen of the vessel narrowing
and obstruct it
-
8/8/2019 heart and vessels
37/97
Husni Rousan 37
ATHEROSCLEROSISATHEROSCLEROSIS Clinical manifestations
Acute onset chest pain, ECG changes,
dyarhythmias & death
Risk factors
Age, family history of non modifiable risk
factors, high cholestrol, cigarette smoking,hypertension & DM
-
8/8/2019 heart and vessels
38/97
Husni Rousan 38
PREVENTION
Control cholestrol level, LDL less than normal
Dietary control decrease fat & increase fiber
Medication to decrease serum fat & cholesterolQuit smoking
Early detection & control hypertension
Control DMGender & estrogen level
Behavior pattern
-
8/8/2019 heart and vessels
39/97
Husni Rousan 39
ANGINA PECTORISANGINA PECTORIS
Definition: its a clinical syndrome ch.ch
by episodes of pain or pressure in the
anterior chest
Pathophysiology
Caused by atherosclerotic disease,
associated with significant obstruction ofCA and any cause that increase demand
or decrease supply
-
8/8/2019 heart and vessels
40/97
-
8/8/2019 heart and vessels
41/97
Husni Rousan 41
ANGINA PECTORISANGINA PECTORIS
Medical Management: the objectives are to
decrease the demand and increase blood supply to
theheart
Pharmacological therapy & control risk factorsNitroglycerides, beta blockers, Ca channel blockers &
antiplatlet agents ( aspirin heparin )
Revascularization procedures
Coronary artery bipass ABG
Percutaneus transluminal coronary angioplasy PTCA
O2 administration
-
8/8/2019 heart and vessels
42/97
Husni Rousan 42
MYOCARDIAL INFARCTION MIMYOCARDIAL INFARCTION MI
Definition: death ofheart tissue caused by
ischemia, a process by whichareas of the
myocardial cells destroyedClinical manifestation
Sudden sever chest pain radiated to left arm
anxious & restlessness,cool pale moist skin, sweating
tachypnea & tachycardia
-
8/8/2019 heart and vessels
43/97
Husni Rousan 43
MYOCARDIAL INFARCTION MIMYOCARDIAL INFARCTION MI
Diagnostic findings and assessment
Pt history, ECG: T wave & STsegment changes echo & lab tests
Medical management: objectives are to
- minimize myocardial damage,
- preserve function & preventcomplications
-
8/8/2019 heart and vessels
44/97
Husni Rousan44
MYOCARDIAL INFARCTION MIMYOCARDIAL INFARCTION MI
Emergent PTCA to open occluded
arteryPharmacologic therapy:
thrombolytic ( STK, TPA ),
Analgesics ACE inhibitors
-
8/8/2019 heart and vessels
45/97
Husni Rousan45
MITRAL STENOSISMITRAL STENOSIS
Definition: an obstruction of blood flowing from
the left atrium into the left ventricle, most often
caused by rheumatic endocarditis
Clinical manifestation
Progressive fatigue due to low cardiac output,
hemoptesis, dyspnea
cough & repeated respiratory infections
-
8/8/2019 heart and vessels
46/97
Husni Rousan46
MITRAL STENOSISMITRAL STENOSIS
ManagementAntibiotic
Valvuloplasty
medication in case of surgical failure PTCA may relieve symptoms
-
8/8/2019 heart and vessels
47/97
Husni Rousan47
MITRAL REGURGITATIONMITRAL REGURGITATION
Definition: blood flowing back from the leftventricle into the left atrium during systole, the
margins of the mitral valves cannot close during
systole
-
8/8/2019 heart and vessels
48/97
Husni Rousan48
MITRAL REGURGITATIONMITRAL REGURGITATIONClinical manifestation
Chronic often asymptomatic
Acute :severe congestiveheart failure,
dyspnea, palpitation, fatigue & weakness,
shortness of breath & cough from pulmonary
congestion
ManagementSurgical mitral valve replacement
Valvuloplasty
-
8/8/2019 heart and vessels
49/97
Husni Rousan49
AORTIC STENOSISAORTIC STENOSIS
Definition: narrowing of the orifice between the
left ventricle &the aorta, congenital malformation
Clinical manifestationMany pts are asymptomatic
Exertional dyspnea, dizziness, fainting,
angina pectoris, low pulse pressure ( 30 mmhgor less )
-
8/8/2019 heart and vessels
50/97
Husni Rousan50
AORTIC STENOSISAORTIC STENOSIS
Management
Prophylactic antibiotic to prevent
endocarditis
Medication as prescribed for
dysrhythmias
Surgical replacement for the aortic valve
One-or-two-balloon percotaneous
valvuplasty
-
8/8/2019 heart and vessels
51/97
Husni Rousan51
AORTIC REGURGITATIONAORTIC REGURGITATION
Definition: flow of blood back into the left
ventricle from the aorta during diastole,
congenital deformities, endocarditis, syphilis,
dissecting aneurysm
Clinical manifestation
Force full heart beat ( head & neck ),
arterial pulsation
exertional dyspnea and fatigue, difficult
breaths specially at night
-
8/8/2019 heart and vessels
52/97
Husni Rousan52
AORTIC REGURGITATIONAORTIC REGURGITATION Management
Prophylactic antibiotic to prevent
endocarditis
Treatment ofheart failure and dysrhythmiasAortic valve replacement ( treatment of
choice )
Surgery is recommended for pt with Ltventricularhypertrophy regardless the
presence or absence of symptoms
-
8/8/2019 heart and vessels
53/97
-
8/8/2019 heart and vessels
54/97
Husni Rousan54
CARDIOMYOPATHIESCARDIOMYOPATHIES Clinical manifestations
A symptomatic for many years
Shortness of breath, nocturnal dyspnea, cough,
chest pain, palpitation, dizziness & fatigue
Medical management
Mange precipitating cause, correct heart failure,
diet & exercise regimen, control dysrhythmias, Implanted electrical device
myomectomy & heart transplantation
-
8/8/2019 heart and vessels
55/97
Husni Rousan55
RHEUMATIC ENDOCARDITISRHEUMATIC ENDOCARDITIS
Definition: inflammation ofendocardium result from rheumaticfever caused by a group A streptococcal infection
Clinical manifestation
Tiny translucent growth, pin-head size beats of the valve flaps, seriousdysrhythmias, pneumonia, valvular deformities, murmur, thrill &palpitation
Medical management
Eradicate organism & prevent complications
Penicillin as a drug of choice ( long term therapy )
Nursing management
Teach pt about disease, prevention & treatment
Instruct about long term therapy
Instruct for prophylactic therapy
-
8/8/2019 heart and vessels
56/97
Husni Rousan56
PERICARDITISPERICARDITIS
Definition: inflammation of the pricardium
Clinical manifestations
Pain over pericardium, clavicle, neck &scapula
friction rub, aggravated by breathing&turning in bed, relieved by sitting up
dyspnea, low cardiac output, increase WBC,pt appears extremely ill
-
8/8/2019 heart and vessels
57/97
Husni Rousan57
PERICARDITISPERICARDITIS Medical management
Determine& treat cause, bed rest,
analgesics NSAID, corticosteroidsprevent pericardial effusion
Nursing management
Medication as prescribed, gradualincrease in activity unless fever, pain and
friction rub reappear
-
8/8/2019 heart and vessels
58/97
Husni Rousan58
ACUTE PULMONARY EDEMAACUTE PULMONARY EDEMA
Definition: abnormal accumulation of fluids inthe lungs either in interstitial space or in alveoli
Clinical manifestationsRestlessness, confusion, breathlessness
sense of suffocation, rapid weak pulse
distended neck veins, cold hands, cyanosed nail
beds, gray skincough & decrease O2 saturation
-
8/8/2019 heart and vessels
59/97
Husni Rousan59
ACUTE PULMONARY EDEMAACUTE PULMONARY EDEMA
Medical management: to improve res.
Exchange
O2 therapy, medication and nursingsupport
Intubation and mechanical ventilator in
severe failurePEEP, oximetry ABGs
Morphine ( 2-5 mg ) to reduce anxiety
-
8/8/2019 heart and vessels
60/97
Husni Rousan6
0
ACUTE PULMONARY EDEMAACUTE PULMONARY EDEMA
Duretic therapy
To increase rate of urin production, decrease
ECF, thiazide & loopduretics ( dose depends onindication, clinical signs & renal function )
Medications to increase myocardial
contractility & cardiac output ( digitalis )
-
8/8/2019 heart and vessels
61/97
Husni Rousan6
1
ACUTE PULMONARY EDEMAACUTE PULMONARY EDEMA
Nursing management
Position pt to promote circulation
Psychological support
Monitor medication
-
8/8/2019 heart and vessels
62/97
Husni Rousan 62
CARDIAC FAILURECARDIAC FAILURE
congestive heart failurecongestive heart failure
Definition: inability ofheart to pump sufficient blood
to meat needs of tissue for O2 & nutrient
Clinical manifestations
In adequate tissue perfusion, dizziness, confusion,
fatigue, cool extremities,
exercise & heat intolerance
low urine output, high venous pressure,
pulmonary & peripheral edema, weight gain
-
8/8/2019 heart and vessels
63/97
-
8/8/2019 heart and vessels
64/97
Husni Rousan 64
CARDIAC FAILURECARDIAC FAILURE
congestive heart failurecongestive heart failureNursing management
I&O, daily wt, daily auscultate lungsounds,jugular vein assessment,
edema, pulse rate, BP, skin turgur &
manage complications
-
8/8/2019 heart and vessels
65/97
Husni Rousan 65
VASCULARVASCULARSYSTEMSYSTEM
-
8/8/2019 heart and vessels
66/97
Husni Rousan 66
The vascular system consists of two interdependentsystems
Right side of theheart pump
Left side of theheart pump
BLOOD VESSELS
Arteries and arteriolsHigh-pressure system, thick wall, transport oxygenated blood
away from theheartLocated in protected areas away from skin surface
Wall of arteries and arteriols composed of 3 layersIntema: inner indothelial layer, contact with blood
Media: smmothelastic tissue, constrict & dilate vessels
Adventitia: connective tissue, anchors vessels to surroundingCapillaries
Single layer ofendothelial cells, permits rapid & effectivetransport of nutrients to the cells & removal of metabolic waste
-
8/8/2019 heart and vessels
67/97
Husni Rousan 67
Veins and venulesLarger in diameter than arteries but the wall are
thinner because there is a less muscle & elastic tissue
in the tonic & media, this allow these vessels to
distend more than arteriesEquipped by one-way bicusped valves that prevent
blood to back flow
Valves composed ofendothelial leaflets
Transport deoxygenated blood from the body to the
heart
Health History and ClinicalHealth History and Clinical
-
8/8/2019 heart and vessels
68/97
Husni Rousan 68
Health History and ClinicalHealth History and Clinical
ManifestationsManifestations
A muscular cramp-type pain in theextremitiesreproduce with the same degree ofexercise oractivity & relieved by rest is experienced bypatients with peripheral arterial insufficiency
Intermittent claudication: its due to inability ofarterial system to provide adequate blood flow tothe tissues in the face of increased demand for
nutrients during exerciseRest pain: worse at night & may interfere with sleep
As general role, the pain of intermittent claudicationoccurs onejoint level below the disease process
-
8/8/2019 heart and vessels
69/97
Husni Rousan 69
Changes in skin appearance and temperature
Inadequate blood flow cause cool & paleextremities
Redish-blue discoloration ofextremities (rubor)
Additional changes resulting from chronicallyreduced nutrients supply like: loss ofhair, brittle
nails, dry skin, atrophy, ulceration, gangrene bytraumatic events
Pulses
Determining the presence or absence as well as
quality of peripheral pulses to assess the status ofperipheral arterial circulation
Absence of pulse may indicates the size of stenosis(narrowing or constriction )
-
8/8/2019 heart and vessels
70/97
Husni Rousan 70
Diagnostic EvaluationDiagnostic Evaluation
Doppler ultrasoundWhen pulses cannot be reliably palpated, use of a
microphne-likehand held doppler ultrasound device
(tranceducer or prob) may behelpful in detecting and
assessing peripheral flowProcedure
Exercise testing
Used to determinehow long can a pt walk &measure ankle systolic BP in response to walking
A normal response is little or no drop in systolic BP,
it drops in true claudication
-
8/8/2019 heart and vessels
71/97
Husni Rousan 71
Angiography
Used to confirm the diagnosis of occlusive arterial disease
when considering surgery or interventionInjecting radiopaque contrast agent directly into vascular
system to visualize the vessels
Pts experience temporary warmth during injection, side
effects are local irritation, allergic reactions, dyspnea, N & V,sweating tachycardia, numbness
Additional risks: vessel injury, bleeding & strock
Contrast plebography ( venography )
Performed if pt is to undergo thrombolytic therapyContrast is injected via dorsal foot vein then X-ray image will
disclos an unfilled vein
Injection may cause brief painful inflammation of the vein
-
8/8/2019 heart and vessels
72/97
-
8/8/2019 heart and vessels
73/97
Husni Rousan 73
Medical management
Modification of risk factors to improve circulationSurgical management
Radiologic intervention
PERIPHERAL ARTERIALPERIPHERAL ARTERIAL
-
8/8/2019 heart and vessels
74/97
Husni Rousan 74
PERIPHERAL ARTERIALPERIPHERAL ARTERIAL
OCCLUSIVE DISEASEOCCLUSIVE DISEASE
Arterial Insufficiency ofextremities is usually found in older
than 50 yrs, most often in men, legs are most frequently affected
Distal occlusive disease frequently seen in pts with DM &elderly pts
Clinical manifestation
Intermittent claudication described as aching, cramp, fatigue,
weakness in joint muscles below stenosis or occlusion area
Decrease ability to walk, increase pain with ambulation
Ischemic pain at rest & worse at night
Bruit sound on auscultation
Absence of peripheral pulse
-
8/8/2019 heart and vessels
75/97
Husni Rousan 75
PERIPHERAL ARTERIALPERIPHERAL ARTERIAL
OCCLUSIVE DISEASEOCCLUSIVE DISEASE Medical management
Exercise program with weight reduction
Smoking cessationSurgical management
- Grafting
- Endarterectomy
Nursing ManagementNursing Management
-
8/8/2019 heart and vessels
76/97
Husni Rousan 76
Nursing ManagementNursing Management
Maintaining circulation
Check pulses of affected extremities, note symmetry,
color, temp., capillary refill, sensory & motorhourly
Dopplerevaluation of vessels distal to bypass graftMonitoring & managing potential complications
Urine output, CVP, pulse, leak, hematoma & edema
Promoting home & community based careDischarge plan, pt education, assess ability to change
life style & self care
AORTIC ANEURYSMAORTIC ANEURYSM
-
8/8/2019 heart and vessels
77/97
Husni Rousan 77
AORTIC ANEURYSMAORTIC ANEURYSM
Its a localized sac or dilation involving an artery
formed at a weak point in vessel wall
THORASIC AORTIC ANEURYSM
Caused by atherosclerosis in men aged ( 40-70 yrs )
Most common is dissecting aneurysm, 1/3 of cases
die of rupture
-
8/8/2019 heart and vessels
78/97
Husni Rousan 78
AORTIC ANEURYSMAORTIC ANEURYSM
Clinical manifestation
Pain in supine position, dyspnea, hoarseness or
aphonia ( complete loss of voice ), dysphagia
Medical management
Surgical repair, control BP, correcting risk
factors
-
8/8/2019 heart and vessels
79/97
Husni Rousan 79
ABDOMINAL AORTIC ANEURYSM
most common cause is atherosclerosis, affect men
4 times than women, occur mostly below renal stenosis,
untreated outcome is rupture & death
Clinical manifestations
Abdominal heart beat on lying position,
abdominal mass
thrombing
-
8/8/2019 heart and vessels
80/97
-
8/8/2019 heart and vessels
81/97
Husni Rousan 81
ARTERIAL EMBOLISM
Its acute vascular occlusion due to an embolus or acutethrombosis
Causes
Iatrogenic injury ( insertion of catheters ), trauma
from fractures, crush injury, penetrating wound,
thrombi development in heart champers as a result of
(AF, MI, CHF)
Clinical manifestationsCessation of distal bld flow, gradual loss of sensory
& motor function, pain, pallor, cold, paresthesia,
pulse lessens & paralysis
-
8/8/2019 heart and vessels
82/97
Husni Rousan 82
ARTERIAL EMBOLISMARTERIAL EMBOLISM
Medical management Surgery ( embolectomy ),
Medication ( heparin bolus5000-10000 then contentiousinfusion) Thrombolytic therapy (STK; streptokainase)
Nursing management
Pre-op. bed rest, warm at room temp. protection
from traumaPost-op. encourage movement & continue
anticoogulants
VENOUS DISORDERSVENOUS DISORDERS
-
8/8/2019 heart and vessels
83/97
Husni Rousan 83
VENOUS DISORDERSVENOUS DISORDERS
DVT, THROMBOPHLEBITIS and
PHLEBOTHROMBITIS
Clinical manifestationsMassive swelling, tenderness,
warmer affected extremity,
homans sign,heaviness & functional loss
-
8/8/2019 heart and vessels
84/97
Husni Rousan 84
VENOUS DISORDERSVENOUS DISORDERS
Medical management
Anti coagulants (heparin 5-7 days), lowmolecular-weight heparin, thrombolytic therapy
Surgical management: thromboectomy whenanti coagulant is contraindicated or danger of
pulmonary embolism is extreme
Nursing management
MonitorPT, PTT, Hb, platlets, report bleeding,assess anti coagulant therapy, monitor &manage complications, provide comfort &apply elastic pressure stockings.
-
8/8/2019 heart and vessels
85/97
Husni Rousan 85
CHRONIC VENOUS INSUFFICIENCY
Obstruction of venous valves in the legs or a
reflux of blood back through the valves
Clinical manifestations
Chronic venous stasis, altered pigmentation, pain,
stasis dermatitis, stasis ulceration, dry skin, cracks &itches
-
8/8/2019 heart and vessels
86/97
-
8/8/2019 heart and vessels
87/97
Husni Rousan 87
LEG ULCERS
Its an excavation of the skin surface that occurswhen inflamed necrotic tissue sloughs off
Clinical manifestations
Open inflamed sore, pain & edema, discharge maybe present, heaviness, itching, area may covered with
eschar, gangrene
Medical management
Pharmacologic therapy (antibiotics based on culture)
depridement, topical therapy, stimulated healing by
Epigram
-
8/8/2019 heart and vessels
88/97
Husni Rousan 88
VARICOSE VEINS
Abnormally dilated torturous superficial veins
caused by incompetent venous valvesClinical manifestations
Dull aches, muscle cramps, increase muscle fatigue,
ankleedema, S&S of venous insufficiency if obstruct
-
8/8/2019 heart and vessels
89/97
Husni Rousan 89
VARICOSE VEINSVARICOSE VEINS
Medical management
Surgery ( ligation ) & sclerotherapy
Nursing management
Bed rest 1st 24 hours & start walking at 2nd day
5-10 min /2 hours, elastic pressure stockings,
elevate foot, discourage standing & sitting,promote comfort (analgesia), home &
community based care
NURSING PROCESSNURSING PROCESS
-
8/8/2019 heart and vessels
90/97
Husni Rousan 90
NURSING PROCESSNURSING PROCESS
Assessment
Sub. (interview) & obj. (physical assessment)
Diagnosis
Alteration in peripheral tissue perfusion
Pain, risk for impaired skin integrity, knowledge
deficit regarding self care activities
-
8/8/2019 heart and vessels
91/97
Husni Rousan 91
NURSING PROCESSNURSING PROCESS
Implementation
Lower theextremity below level of theheart
Encourage moderate amount of walking
Maintain warm & discourage nicotine use
Administer prescribed vasodilators, adrenergic blockagents
Evaluation
Goal met evidenced by: extremities warm to touch,color improved, decrease muscle pain, tolerate
performing exercise 6 times / day
HYPERTENTIONHYPERTENTION
-
8/8/2019 heart and vessels
92/97
Husni Rousan 92
Definition: its a raise of blood pressure above normal
range
systolic above 140 mmhg & diastolic above 90mmhg over sustained period
A multifactorial condition
A sign ,a risk factor , and a disease .
-
8/8/2019 heart and vessels
93/97
Husni Rousan 93
HYPERTENTIONHYPERTENTION Types & causes
1- Primary (idiopathic essential ) hypertention
80-90% of cases are of unknown cause butpredisposed by: old age over 60 yrs, obesity,
black race, atherosclerosis Benign or chronic hypertention
Rise is usually slight to moderate & continueto rise slowly often asymptomatic ( silentkiller )
Malignant (accelerated) hypertention
BP very high & continue to raise rapidly,diastolic pressure in excess of 120 mmhg &theeffects arequickly apparent
-
8/8/2019 heart and vessels
94/97
Husni Rousan 94
HYPERTENTIONHYPERTENTION
2- Secondary hypertention: Increase BP
from an identified cause resulting from
other disease Causes
Renal disease, endocrine disorders, age & sex,
stressful occupation & situation, familytendency, DM, dyslipidemia, smoking &
alcohol
-
8/8/2019 heart and vessels
95/97
Husni Rousan 95
HYPERTENTIONHYPERTENTION
Clinical manifestations
High blood pressure reading
Headache, epistaxis, angina,
dizziness, dyspnea, ringing in ears
Retinal changes may be papilledema
a common consequence M.I. & CAD
-
8/8/2019 heart and vessels
96/97
Husni Rousan 96
HYPERTENTIONHYPERTENTION
Medical management
Treatment of underlying cause
Life stile modification :- Management of predisposing factors (
low salt diet, decease weight, stop
smoking, decrease stress level)Pharmacologic therapy (diuretics,
vasoconstrictive agents & agents todecrease cardiac output )
Nursing ProcessNursing Process
-
8/8/2019 heart and vessels
97/97
Nursing ProcessNursing Process
Nursing Diagnosis
Knowledge deficit ( medication & disease process )
Non compliance with therapeutic regimen
E.O
Pt will understand disease process & its treatment
Pt will participate in self care program
Implementation
Allow pt to rest & relax, medication as prescribed, report sideeffects, educate pt about rebound hypertention that occurs if
therapy suddenly stoppedMeasure BP routinely, follow up appointments,
Educate pt about arthostatic hypotention so to stand gradually
Life style modification