ECZEMA and nIMPETIGO
-
Upload
hadios999 -
Category
Health & Medicine
-
view
522 -
download
0
Transcript of ECZEMA and nIMPETIGO

ECZEMA & IMPETIGO
Submitted by, MAHDY ALI AHMAD OSMAN 4th Pharm.D Pharmacotherapeutics 1&2 2014/15 JSS College of Pharmacy Oooty
1

What is Eczema
•Eczema is a type of skin inflammation (dermatitis)
•The most common form of eczema is atopic dermatitis
•Eczema can affect people of any age•Family history of asthma and hay fever •Eczema is more common in girls than in
boys •It occurs in people of all races
2

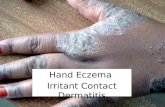
What Eczema Looks Like 3

Causes of Eczema
4
Etiology

Prevention (2)7. Avoiding foods that cause allergic reactions 8. Exercise, meditation, or other stress-management
techniques can help those for whom stress is a trigger
9. Wearing protective gloves for activities that require frequent submersion of the hands in water
10. Avoiding activities that make you hot and sweaty as well as abrupt changes in temperature and humidity
11. A humidifier should be used in both winter12. Maintaining cool temperatures in sleeping areas13. Practicing good skin hygiene
5

PATHOPHYSIOLOGY•The exact cause of eczema is unknown. But
it is thought to involve dry sensitive skin alteration of the immune system ,genetic factors
•Eczematous conditions primarily affect the outermost layer of the epidermis.
•Skin damage due to sun burn , use of harsh soaps , certain cosmetics or environmental factors can reduce the content of ceramides .
6

•This results in increased water loss , causing dry( xerosis ),irritated and itchy skin.
•Immunologic dysfunctions have been noted in patients with eczema. Increased IgE production and increased cytokine levels have been detected.
•Although some patients don’t have elevated IgE levels , approximately 80% with various types of atopic disease will show increased levels.
7

IMMUNOLOGIC FACTORS•Studies have shown acute lesions have
increased levels of IL-4 and IL-13,while chronic lesions are rich in IL-5,interferon and IL-12.
•Cytokines play a very important role in skin inflammation , erythema and edema.
•T helper cells(TH1 & TH2) play an important role in skin inflammation.TH2 are overexpressed in acute lesions.
8

CLINICAL PRESENTATION 9

DIAGNOSIS:•Patient age and hormonal status in
women should be considered in the initial evaluation of patients with skin disorders.
•Menopausal women tend to develop brown hyperpigmentation or melasma. Pregnant women may develop hyperpigmentation of the areola and genetelia as well as melasma.
10

11

Medications• Corticosteroids are highly effective in controlling or
suppressing symptoms in most cases The duration of therapy is one week to 3 months .( topically ointment & creams & orally eg: Dexa 0.5mg ) applied twice daily.
• Immunosuppressant drugs are sometimes prescribed. These dampen the immune system and can result in dramatic improvements to the patient's eczema
• Anti-itch drugs, often antihistamine, Hydrocortisone applied to the skin aids in temporary itch relief
• Coal Tar• UV light • Interferon-γ• Moisturizers • Lifestyle :Various measures may reduce the amount
of mite antigens, in particular swapping carpets
12

13

14

antihistamine•Anti histamines are frequently used. A
sedating antihistamine(hydroxyzine,diphenhydramine) can offer an advantage by facilitating sleep because pruritis is often worse at night.
•Doxepin is a tricyclic anti depressant that inhibit histamine receptors. 10 to 75mg is given at night.
15

Immunosuppressant•The topical immunomodulators tacrolimus
and pimecrolimus inhibit calcineurin, which normally initiates T-cell activation.Tacrolimus 0.03% and 0.1% twice daily. Pimecrolimus 1% twice daily.
•Coal tar preparations reduce itching and skin inflammation and are available as crude coal tar(1%-3%)or liquor carbonis detergens(5-20%) in combination with topical corticosteroids.
16

17

Alternative Therapies • Sea water: there is some anecdotal evidence that
salt water baths may help some children with atopic eczema
• Sulfur has been used for many years as a topical treatment in the alleviation of eczema
• Probiotics are live microorganisms taken orally, such as the Lactobacillus bacteria
• Traditional Chinese medicine• Diet :”What you Eat What You Are”
18

IMPETIGO

• Impetigo is a superficial skin infection that is seen most commonly in children.
• Most common during hot, humid weather, which facilitates microbial colonization of the skin.
• Minor trauma, such as scratches or insect bites, allows entry of organisms into the superficial layers of skin, and infection ensues.
• The infection is generally classified as bullous or nonbullous based on clinical presentation.
Etiology• Most cases of impetigo were caused by S. pyogenes, but
recently S. aureus, either alone or in combination with S. pyogenes, has emerged as the principal cause of impetigo.
• The bullous form is caused by strains of S. aureus capable of producing exfoliative toxins (neonates)

21

Presentation•Exposed skin, especially the face, is the most common site.
Symptoms•Pruritus is common, and scratching of the lesions may
further spread infection through excoriation of the skin.•Weakness, fever, and diarrhea sometimes are seen with
bullous impetigo
Signs•Nonbullous impetigo manifests initially as small, fluid-
filled vesicles.•Purulent discharge from the lesions dries to form golden
yellow crusts that are characteristic of impetigo

Diagnosis•Crusted tops of lesions should be raised so that purulent
material at the base of the lesion can be cultured.•A complete blood count is often performed because
leukocytosis is common.

Treatment• Although impetigo may resolve spontaneously, antimicrobial
treatment is indicated to relieve symptoms, prevent formation of new lesions, and prevent complications, such as cellulitis.
• Penicillinase- resistant penicillins are preferred for treatment because of the increased incidence of infections caused by S. aureus.
• Penicillin, administered as a single intramuscular dose of benzathine penicillin G (300,000 to 600,000 units in children, 1.2 million units in adults) or as oral penicillin G, is effective for infections known to be caused by S. pyogenes.
• Penicillin-allergic patients can be treated with clindamycin.• The duration of therapy is 7 to 10 days.• Topical therapy with mupirocin ointment (applied three times daily
for 7 days) is as effective as erythromycin.• Removal of crusts by soaking in soap and warm water also may be
helpful in providing symptomatic relief.

References •Clinical medicinl Kumar & Clark•Pharmacotherapy textbook Dipiro •NICE guideline
25

THANK YOU
26