Community Acquired Pneumonia, A Case Study
Transcript of Community Acquired Pneumonia, A Case Study

PEDIATRIC COMMUNITY ACQUIRED PNEUMONIA
A Case Study Presented to
The Faculty of the College of Nursing
LORMA COLLEGES
City of San Fernando, La Union
In Partial Fulfillment
of the Requirements for the
Degree of Bachelor of Science in Nursing
By:
Abaggo, Hershey Clarisse
Agaid, Grethel Joey
Aguda, Tia Marie
Bautista, Nikkola
Cabagbag, Kristel
Elumba, Penny Joy
Galindo, Ellen Lorie
Gaona, Elemyr
Laroco, Abegael L.
Vendiola, Loryn
August 2010

I. INTRODUCTION
Pediatric community-acquired is diseases in which individuals
who have not recently been hospitalized develop on infection of the lungs
(pneumonia). PCAP is a common illness that affects infants and children.
PCAP often causes problems like difficulty in breathing, fever, chest pain and
cough. PCAP occurs because the atmosphere or the areas of the lungs which
absorb oxygen (alveoli) from the atmosphere become filled with fluid and
cannot work effectively.
PCAP occurs throughout the world and is a leading cause of illness and
death. The cause of PCAP includes bacteria, viruses, fungi and parasites.
PCAP can be diagnosed by symptoms and physical examination alone,
through x-rays, examination of the sputum and other tests are often used.
Individuals with PCAP are primarily treated with antibiotic medication in the
hospital some forms of PCAP can be prevented by vaccination.
PCAP usually acquired via inhalation or aspiration of pulmonary
pathogenic organisms into a lung segment or lobe. Less commonly, PCAP
results from secondary bacteria from a distant source, such as Escherichia
coli urinary tract infection and/or bactericidal. PCAP is due to aspiration of
oropharyngeal contents is the only form of PCAP involving multiple
pathogens.
The proportion of children with pneumonia who are diagnosed with a
specific etiology is low. Unlike adults, children usually do not produce
adequate sputum specimens for Gram stain and culture. Blood cultures have
a yield of less than 10% in patients with bacterial pneumonia. “Lung
puncture” studies that are conducted in developing countries are obviously
not met with enthusiasm in general pediatric practices. Prospective studies
that have employed sensitive antibody tests and polymerase chain reaction
techniques have suggested that in up to 20% of pediatric community-
acquired pneumonias, the infection is “mixed” (i.e., both S. pneumoniae and

M. pneumoniae or C. pneumoniae); in these cases, the primary pathogen is
not clear. Authors of these studies have also suggested that mixed infection
with bacteria and respiratory viruses is likely to be common as well.
Many studies have looked at causes of pediatric pneumonia as it
relates to certain readily available laboratory measurements. Many clinicians
consider S. pneumoniae to be the likely cause of the lower respiratory
infection if the picture is characterized by acute onset of high fever, lobar
pneumonia on chest radiograph, leukocytosis, and a rapid response to β-
lactam antibiotics. Numerous studies have found that chest radiographs do
not readily distinguish between bacterial, atypical bacterial, and viral
pneumonia. A variety of laboratory tests have been used in the attempt to
distinguish bacterial from viral pneumonia, including the C-reactive protein
and absolute neutrophil counts. One problem in using “screening” tests is
that specific cutoff levels have often not been established. A recent study
done in Europe found that although white blood cell count and C-reactive
proteins were statistically higher in patients with pneumococcal infections,
other clinical and laboratory and radiographic studies were of little value.
Given the clinical, epidemiologic, and laboratory difficulties in pinpointing the
cause of pediatric pneumonia, an additional approach is to divide patients by
age.
The primary bacterial pathogen in neonatal pneumonia is group B
streptococci, although Escherichia coli and Listeria monocytogenes have also
been reported. The mechanism is similar to that in neonatal sepsis, where
colonization from the mother results in neonatal colonization and
breakthrough infection.
Chlamydia trachomatis is the most common sexually transmitted infection in
the United States. The organism may reside in the genital tract of pregnant
women and be transmitted in about 60% of cases to infants at the time of

delivery. About one half of infants who acquire the organism develop
conjunctivitis, and 20% eventually develop lower respiratory disease.
Pneumonia caused by bacteria such as group B streptococcus typically
occurs in the first weeks of life, presenting with fever, increased work of
breathing, and hypoxia. C. trachomatis infection usually occurs between 2
and 19 weeks after birth. The infants are afebrile, have increased respiratory
rate, and cough. Children with chlamydial pneumonia often have
hyperinflation, and bilateral infiltrates on chest x-ray, eosinophilia, and
elevated serum immunoglobulin levels. Cultures of the blood, urine, and
even cerebrospinal fluid are often obtained and intravenous antibiotic
started. C. trachomatis can be diagnosed by culture or direct fluorescent
antibody staining of nasopharyngeal secretions.
The management of the febrile tachypneic neonate suspected of
having pneumonia is similar to that of neonatal fever. Empiric intravenous
antibiotics are started until culture results are final. Empiric treatment
usually consists of ampicillin combined with gentamicin or a third-generation
cephalosporin. Treatment of C. trachomatis is with oral erythromycin, 50
mg/kg per day in four divided doses for 2 weeks. In the past, erythromycin
was given to neonates exposed to C. trachomatis at the time of delivery.
Recently, there has been an association reported between oral erythromycin
and the subsequent development of hypertrophic pyloric stenosis in infants
younger than 6 weeks of age. The current recommendation is to treat with
oral erythromycin, 50 mg/kg per day in four divided doses for 14 days all
infants with chlamydial conjunctivitis and pneumonia. Patients who are
exposed at the time of delivery are not presumptively treated, but rather
monitored closely for the development of disease. Routine screening of all
pregnant women for sexually transmitted disease is helpful in reducing
disease by C. trachomatis.

The peak incidence of this viral pathogen is in the first 6 months of life.
Respiratory syncytial virus (RSV) typically occurs annually during the winter
months. The spectrum of disease includes significant bronchiolitis and
pneumonia in infants and younger children to a mild upper respiratory
infection in older children. Patients with underlying conditions such as
bronchopulmonary dysplasia, congenital heart disease, or underlying
immunodeficiency are at risk for a more severe course. RSV is diagnosed
rapidly using a direct fluorescent antibody on nasal secretions. An
aerosolized antibiotic agent, ribavirin, has been used in the treatment of RSV
disease in infants. The use of ribavirin remains the subject of continuing
debate. Citing new evidence, the American Academy of Pediatrics changed
its recommendation in the 1990s regarding the use of ribavirin and now has
a less stringent “may be considered” recommendation for its use in RSV
infections in children with underlying conditions such as immunodeficiency,
congenital heart disease, or chronic lung disease. Children with less serious
disease need only supportive treatment.
Pneumonia in children 4 months to 5 years of age was caused by viral
pathogens again predominate in this age group, with RSV, parainfluenza,
influenza, and adenovirus being common pathogens. The primary bacteria
causing pneumonia in infants and children remains S. pneumoniae. Some
studies also report M. catarrhalis, and nontypeable H. influenzae as
pathogens.
STATISTICS:
World Wide
According to WHO and BTS criteria, severe CAP was present in 57 (50%) and in
96 (85%) cases, respectively; 29 (26%) were aged less than 1 year. The median age (months)
was 22 (mean 24 ± 14, range 2-58). Overall, radiographic finding was right-sided in 77
(68%) cases and the upper lobe was compromised in 36 (32%) cases. By analyzing data

stratified to age, the frequency of upper lobe involvement was significantly higher among
severe cases (WHO criteria) only for those patients aged 1 year (13/35 [37%] vs. 7/45
[16%], P = 0.03, OR [95% CI] 3.2 [1.1-9.2]). The specificity and positive predictive value of
upper lobe involvement for severity among the latter group of patients were 84% (95% CI
70-93%) and 65% (95% CI 41-84%), respectively. No association was found by using the
BTS criteria. The admission chest radiography was useful to predict severity of children aged
1 year hospitalized with CAP. Pediatr Pulmonol. 2009; 44:249-252. © 2009 Wiley-Liss,
Inc.
National
Regional 1=
Lorma Medical Center =
REASON FOR CHOOSING THE CASE:
It is due to the motive to learn and apply our knowledge and skills in
caring the patient with pediatric community acquired pneumonia (PCAP).
This is a rare case since the patient is only 6 month old.
Family Centered Objectives:
Our family centered objectives would remain to be our most significant
motive in conducting this case study. They are as follows:

The parents of the patient will be able to understand the causes and
therapeutic management regimen
The parents will be able to consider and demonstrate the proper way
of breastfeeding and guidelines for the condition.
The parents will be able to verbalize the importance of increase fluid
intake.
The parents will be able to identify potential complications and how to
initiate appropriate preventive or corrective actions.
II. NURSING HEALTH HISTORY:
A. BIOGRAPHIC DATA
Client MT is a 6 month old, female, was born January 28, 2010 in Biday,
San Feranando City La Union. She is the youngest daughter of Mr and Mrs
NT. She is a Roman Catholic.
She was admitted on July 31, 2010 9:40 PM at Lorma Medical Center by
Dr. Rapisura, Carie Q.,MD and Dr. Orlindo, Maria Teresa V.,MD as her
attending physician.
B. CHIEF COMPLAINT
The patient was admitted due to the chief complaint of high grade
fever, 38.6 C via axilla, productive cough and difficulty of breathing.
C. HISTORY OF PRESENT ILLNESS
The present condition started 3 days prior to admission when the
patient had dry cough with associated difficulty of breathing. No other
associated signs and symptoms such as diarrhea and vomiting. No
consultation done or medication taken.

2 days prior to admission, the above condition persisted associated with
neither fever, still no consultation done nor medication taken.
Few hours prior to admission, due to persistence of the above
condition, she was then brought in the institution and was then admitted on
July 31, 2010 at 9:40PM with the vital signs of T-38.6ºC, PR-135bpm, RR-
68bpm, O2sat-98%, weight-6.4kg, height-58.5cm and a BMI of 18.90 kg/m2
(healthy weight) 22 as ideal with a range of 18.5-25
D. PAST MEDICAL HISTORY
The mother stated that the patient was not hospitalized nor had
illnesses before. The patient had no allergies to drugs. The mother also
claimed that the patient already received her BCG and Hepa B vaccines, 1
dose each, 1 week after her birth at the health center, and had her vaccines
in DPT and OPV with 1 dose each when she was 6th week old.
E. PEDIA HISTORY
The patient was born to a 33 year old mother with a 38-39 weeks age
of gestation via NSD at home. The mother stated that there were no
complications happened nor the mother acquired illnesses during her
pregnancy period.
F. FAMILY HEALTH HISTORY
The mother of the patient claimed that both sides of the patient has
history of asthma. And no other hereditary illnesses present such as
diabetes, cancer and hypertension.
G. LIFESTYLE
In an interview, mother said that their house is a concrete bungalow,
located along the highway and near to other houses.

The patient is a pure breastfed baby, the mother verbalized that she
didn't introduced any solid foods yet. The family is using firewood in cooking
their foods. While their drinking water comes from a well which the mother
boils before giving to her children. They are also using dipper in taking a
bath and flushing their toilet.
The mother also claimed that the patient's uncle who lives with the
family is an active smoker. And this can one of the precipitating factors that
contributed on the patient’s case for her lungs are still sensitive since patient
is still 6 month old. Health teaching was done to the mother by encouraging
the mother to advice the uncle to minimize smoking and not to smoke near
their house.
H. SOCIAL HISTORY
The mother also claimed that, their family are active and concern
citizen of the community, they also mingles with their neighbors and always
active participates in activities, education in their community.
Just like a typical family relationships, there are some
misunderstanding experienced by the family but usually it only lasted for a
day, they fix the problem in a calm manner.
The patient's mother described their family as a traditional Filipino
family, wherein they eta together, live together and giving respect with one
another.
I. EALTH PRACTICES
When a member of the family got sick, they always consult to a
medical doctor. They don't have any private family physician. They also
believe in “hilot” but they never use any herbal medicines that were being
prescribed to them, they only taking medicines which are prescribed only by
a physician.

J. DEVELOPMENTAL TASK
According to Erik Erikson's Psychosocial Theory of Human
Development, the patient is under Trust vs. Mistrust Stage. Wherein the
patient always depend all her needs on her mother, which is the main
caregiver of the child. When trust did not develop well it will result to
mistrust which can be developed when the needs of the patient were not
given attention.
From Freud’s Psychosexual Theory, the patient is under Oral stage.
Wherein, the child cries when she needs something. And during also this
stage that mouth or oral is only the means of her satisfaction.
According to Piaget’s Cognitive Theory, she is under the Pre-
operational Stage. The id personality dominates during this age. The infant
only wanted to be supplied with all her pleasures like attending and
pampering her all the time.
III. PHYSICAL ASSESSMENT
Date examined: August 3, 2010
Time Examined: 12:30 PM
I. GENERAL STATISTICS
A Filipino female client, conscious and with a normal body built.
A. Vital signs

RR: 60 bpm
TEMP: 36.5 ˚C
CR: 142 bpm
OXYGEN SAT: 99%
B. Height and weight:
Height – 58.5 cm
Weight- 6.4kg
BMI- 18.90 kg/m2 (healthy weight) 22 as ideal with a range of 18.5-25
II. HEAD AND NECK
A. Head
The head is round with no nodules or masses and depressions.
B. Eyes
The eyes are symmetrically aligned and eyebrows are evenly
distributed with no discharge or discoloration on the eyelids.
Conjunctiva on both eyes is pinkish in color, and the sclera is normal in
color. The pupils are black round and equal in size and are reactive to
light and accommodation.
C. Ears
The ears are symmetrically aligned and the color is same as the facial
skin, it is firm and not tender. No serum and discharges noted.
D. Nose
The nose is symmetrically aligned with the face, no discharges, with
flaring nares. It is the same color with the face. It is not tender and no
lesions present. The mucosa is pink. The sinuses are not tender when
palpated.
E. Mouth
The lips are pinkish in color and moist. No ulcerations or lesions noted.
The tongue moves freely and not tender. The client possesses pink
gums with no teeth yet.

III. INTEGUMENT:
1. Skin
The skin of the client is moist, pale and has a good skin turgor.
Has a fair skin complexion.
2. Hair and Scalp
The hair are equally distributed with a thin hair strands; well
kept; no lice or dandruff seen/noted.
3. Nails
Client’s nails are normally transparent and convex. The
surrounding cuticles are intact and without inflammations noted. Has a
normal capillary refill with 1 to 2 seconds.
IV. THORAX and LUNGS
The chest contour is symmetrical, the spine is vertically aligned.
The chest wall is intact, no tenderness or no masses noted. Upon
auscultation rales was being noted.
V. HEART
There is no presence of abnormal pulsations when the heart was
auscultated. No murmurs and friction rubs heard upon auscultation.
VI. BREAST
The breasts are even with the chest wall, skin is smooth and
intact. Areola is round and bilaterally the same. The nipples are round
and equal in size, no discharge noted. The breast are not tender, no
masses or nodules noted.
VII. ABDOMEN
The abdomen is intact, round and with normal bowel sound heard upon
auscultation. Has a darken umbilicus. No deformities seen.

VIII. EXTREMITIES:
On the upper extremities no deformities noted. The has a D5IMB
½ L at the left hand. While on the lower extremities, no deformities were
noted.
IX. GENITAL AND RECTAL:
Upon inspection there were no deformities, no rashes, no
abnormal secretions were present.
IV. ANATOMY AND PHYSIOLOGY

Anatomically, the respiratory system structures are divided into:
Upper respiratory tract and Lower respiratory tract
The upper respiratory tract is located in the head and neck and consists
of the:
Nose
Pharynx
Larynx
NOSE:
Regions of the nose include the external nose and the nasal cavity. Air
moves from the nostrils to the back of the nasal cavity where it exits through
the posterior nares. The function of the nasal cavity is to clean, warm and
dampen the air that enters so that it can travel throughout the body.

REGIONS OF THE PHARYNX:
Air moves into the nasal cavity through the nostrils (nasopharynx). The
oropharynx opens into the oral cavity which encloses the lips, teeth, cheek,
hard and soft palates, tongue and tonsils. Extending from the tip of the
epiglottis to the glottis and the esophagus is the laryngopharynx and
positioned in the anterior neck is the larynx.
LARYNX
The larynx is a passageway between the pharynx and the lower airway
structures. It is a short tube made up of supportive cartilage, ligaments,
muscle and mucosal lining. The supportive cartilage prevents food and drink
from entering the larynx while swallowing.
The lower respiratory tract is located in the chest and makes up the:
Trachea
Bronchial tree
Lungs
Air passes from the larynx to the lungs (trachea).The trachea divides
into the right and left primary bronchi (bronchial tree) and the large pair of
spongy organs (lungs) are used for respiration.
TRACHEA:
Also known as the windpipe, the trachea is a 10-12cm tube that runs
through the lower neck and chest. The wall of the trachea is made of hyaline
cartilage which enables the trachea to stay open so that air can be
conducted between the larynx and primary bronchi.
BRONCHIAL TREE
The bronchial tree consists of a primary, secondary (lobar) and tertiary

bronchi (segmental bronchi). The trachea splits into the right and left bronchi
at the level of the sternal angle. The secondary bronchi forms when the
primary bronchus enters the lung; and conducts air directly to one of the five
lobes within the lung. Tertiary bronchi derive from the secondary bronchi and
conduct air to and from the bronchial segment. There are 8 bronchial
segments in the left lung and 10 in the right lung.
LUNGS:
The lungs are paired cone-shaped organs which take-up most of the
space in the chest with the heart. Their role is to take oxygen into the body,
which we need for the cells to live and function properly, and to help us get
rid of carbon dioxide, which is a waste product. There are two division of the
lungs, the left and the right lung. These are divided up into lobes or big
secretions of tissues separated by “fissures” or dividers. The right lung has
three lobes but the left lung has only two, it is because the heart takes up
some of the space in the left side of the chest. The lungs can also be divided
up into even smaller portions, called bronchopulmonary segments. These are
pyramidal-shaped areas which are also separated from each other by
membranes. There are about 10 of them in each lung. Each segment
receives it's own blood supply and air supply. Air enters the lungs through a
system pipes called the bronchi. Theses pipe start from the bottom of the
trachea as the left and right bronchi and branch many times through out the
lungs, until they eventually form little thin-walled air sacs or bubbles, known
as the alveoli. The alveoli are important in the gas exchange where it takes
place between the air and the blood. Covering alveolus is a whole network of
little blood vessel called capillaries, which are very small branches of the
pulmonary arteries. It is important that the air in the alveoli and the blood in
the capillaries are very close together, so that oxygen and carbon dioxide
can diffuse between them.
Mechanics of Breathing
To take a breath in, the external intercostals muscles contract, moving

the ribcage up and out. The diaphragm moves down at the same time,
creating negative pressure within the thorax. The lungs are held to the
thoracic wall by the pleural membranes, and so expand outwards as well.
This creates negative pressure within the lungs, and so air rushes in through
the upper and lower airways.
Expiration is mainly due to the natural elasticity of the lungs, which
tend to collapse if they are not held against the thoracic wall. This is the
mechanism behind lung collapse if there is air in the pleural space
(pneumothorax).
Physiology of Gas Exchange
Each branch of the bronchial tree eventually sub-divides to form very
narrow terminal bronchioles, which terminate in the alveoli. There are many
millions of alveloi in each lung, and these are the areas responsible for
gaseous exchange, presenting a massive surface area for exchange to occur
over.
Each alveolus is very closely associated with a network of capillaries
containing deoxygenated blood from the pulmonary artery. The capillary and
alveolar walls are very thin, allowing rapid exchange of gases by passive
diffusion along concentration gradients.

CO2 moves into the alveolus as the concentration is much lower in the
alveolus than in the blood, and O2 moves out of the alveolus as the
continuous flow of blood through the capillaries prevents saturation of the
blood with O2 and allows maximal transfer across the membrane.
Resource: An Online Examination of Human Anatomy and Physiology.
GetBodySmart:Interactive by ConceptCreators Inc
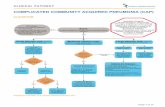
V. DISEASE ENTITY/ PATHOPHYSIOLOGY

Precipitating Factor
ENVIRONMENT
LIFESTYLE
Passes to the pharynx, larynx & trachea
Leukocytes increased
Mucus and phlegm
COUGHING
INEFFECTIVELY
Narrowing of air passage
DIFFICULTY BREATHING
Microorganisms enters the affects both the lung parenchyma
Infection lodges and stimulates in the parenchyma
Lung invasion
Lung Invasion
Predisposing Factor
AGE (6months old)
Enters through nose or mouth by Inhalation
Streptococal Infection

VI. DIAGNOSTIC EXAMINATION / LABORATORY RESULTS
LORMA MEDICAL CENTER
HEMATOLOGY SECTION
July 31, 2010
RESULT NORMAL INTERPRETATIO
N
Hemoglobin 105 127-183 g/L -Decrease
hemoglobin
indicates anemia
Hematocrit 0.31 0.40-0.50 -Decreased
hematocrit
indicates anemia,
such as that
caused by iron
deficiency
-it may also
indicate that the
patient has
vitamin or mineral
deficiency
White Blood Cell 11.1 5-10 x 10^9 g/L -Increase WBC
may be due to
inflammation

-bands
-segmenters 0.56 0.50-0.70 Normal
-eosinophils 0.05 0.00-0.05 Normal
-basophils 0.00-0.01
-lymphocytes 0.32 0.20-0.40 Normal
-monocytes 0.07 0.00-0.07 normal
Platelet count 402 150-400 x
10^9/L
-high platelet
count is a reaction
to inflammation,
infection, anemia,
Irene J. Frigillana, RMT
Medical Technologist

LORMA MEDICAL CENTER
CHEST X-RAY
Chest x-ray including the anterior, posterior, and lateral was conducted
last July 31, 2010. The result indicates opacities on the both lung fields.
Notably the upper lobes and paracardiac areas. The heart is not enlarged.
And the diaphragm and bony thorax are intact.
The impression of the above results indicates that the patient has a
bilateral pneumonia.
IMPRESSION: BILATERAL PNEUMONIA
Robert Rana, MD, FPOR (Radiologist)

IX. EVALUATION
Good adherence to health care teachings provided to our client and
parents became the reason of meeting our family centered objectives.
Before any nursing intervention, we made it a point that we were able to
understand the disease itself and its proper management. Rendering health
teaching is one of the important tools to help promote the health of the
patient. We established a trusting relationship with the parents especially
the mother which enable us to provide efficient nursing care. A good nurse-
patient interaction plays a vital role in meeting the objectives. This is met
through creating an environment of trust in listening to the mother of the
patient concern and being available to client’s side. This enables us to
established rapport and respect needed before the mother of the patient will
be willing to take part in the learning process.
We the student discussed about the disease of the patient to the
mother and how it is acquired. Maybe, caused by their environment, lifestyle
and also hereditary. To prevent such disease, the parents or the family
should clean their surroundings and before handling the baby they must do
handwashing to prevent spread of microorganism. Most important thing is
for them to give vitamin C to protect her immune system and the importance
of completing all the immunizations provided by the Department of Health
especially the DPT vaccine which helps the child to prevent in having
pneumonia.
Certain health teaching was discussed to the mother like the
importance of adhering therapeutic management regimens like taking the
medications and knowing its advantages or benefits and the effects and
adhering to proper hygiene like cleaning the breast with water before the
baby will suck and washing the hands before handling the baby. We also
imparted to them knowing the potential complications and how to initiate
appropriate preventive or corrective action. Lastly we were able to

encourage the patients mother on the proper positioning while breast
feeding or when propping –up the baby in order to increase its intake and
prevent aspirations and to help immobilizing secretions. The patient is still
confine in the 3B- pedia at Lorma Medical Center.