Community acquired pneumonia
-
Upload
anvesh-narimeti -
Category
Health & Medicine
-
view
53 -
download
1
description
Transcript of Community acquired pneumonia

Community Acquired Pneumonia

Acute infection of pulmonary parenchyma in pts who has acquired infection in community
Def:-

Commonly caused by : streptococcus pneumoniae Other organisms : hemophilus influenzae Atypical bacteria ( Mycoplasma pneumoniae, Chlymadophila pneumoniae ,legionella ) Respiratory viruses Gram negetive bacteria( enteobacteriaceae , pseudomonas aeruginosa) Rarely mycobacterium tuberculosis, C.psittaci, C. burnetii,endemic fungi Recently increased incidence of S.aureus is noted (methicillin resistant strains)
Etiology :-

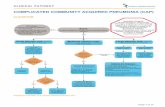
Clinical evaluation
Chest radiography { with or without microbiological testing}
Diagnostic approach to Community Acquired Pneumonia

Cough FeverPleuritic chest pain(30%)DyspneaSputum productionGI symptoms-
nausea,vomiting,diarrhoeaMental status changesChills & Rigors
Clinical Features of CAP

Pt is febrileRespiratory rate :- > 24 cpm Auscultation :- rales are present1/3 rd pts present with signs of
consolidation
Blood examination :- leucocytosis ( 15,000 – 30,000/mm3)
Leucopenia – poor prognosis.
O/E :-

Infiltrates on plain chest x-ray – gold standard for diagnosing pneumonia
Radiological appearances CAP : lobar consolidation(typical bacteria) interstitial infiltrates(pneumocystis carinii & viruses)
CT scan – higher sensitivity for CAP
Radiological Evaluation:



Treatment is best when it is pathogen-directed
Includes:- blood - culture & sensitivity. sputum – Gram staining & culture. urinary antigen tests (legionella &
pneumococcus) Newer tests :- PCR
Diagnostic testing for microbial etiology

Based on severity of diseaseOther features – ability to maintain oral intake likelihood of compliance h/o substance abuse cognitive impairement living situation functional status of pt.
Indications for Hospitalisation:_

Commonly used prediction rules i)PSI (pneumonia severity index)ii) CURB 65 Confusion (based on specific mental
test, disorientation to time place or person) blood urea > 7mmol/lit (20 mg/dl) respiratory rate > 30cpm blood pressure (systolic < 90mm hg
diastolic <60mm hg) age >= 65 yrs Score : 0-1 – treated on outpatient basis 2-3 – admitted in hospital >3 – admitted in icu

Choice of initial treatment complicated by emergence of antibiotic resistance of S. pneumoniae
Antibiotic therapy started on empiric basis since causative organism is not identified in proportinate no. of pts.
Treatment

In pts without risk factors or microbiological eveidence of pseudomonas aeruginosa or MRSA :
Combination of I.V. beta lactam { ceftrioxone :1-2 gms daily cefotaxim : 1-2 gms every 8th hrly or ampicillin :1.5-3 gms 6th hrly.}
PLUS
Either Macrolide {azithromycin 500mg daily} or fluoroquinolone {levofloxicin 750 mg daily or moxifloxicin 400mg daily}

In pts who may be infected with pseudomonas aeruginosa or other resistant pathogens ( those with COPD or Bronchiectasis or frequent antimicrobial or glucocorticoid use) combination therapy with beta lactam and fluoroquinolones is used :
Piperacillin-Tazobactam(4.5 gms every 6 hrs) orImipenem (500mg every 6 hours) orMeropenam (1 gm every 8 hrs) orCefipime ( 2gms every 8 hrs) orCeftazidime (2gms every 8 hrs)
PLUS
Ciprofloxacin (400mg every 8 hrs) orLevofloxacin( 750 mg daily)

In pts allergic to penicillin by skin testing cephalosporins can be continued ( 3rd generation)
In cases of mild reaction ( not IgE mediated) initially 1/10 of dose is given observed for 1 hr, then remaining 9/10 dose is given & observed for another hr.
In pts with past allergic reaction to cephalosporins, Aztreonam (2mg I.V every 6-8 hrs) can be given.(exception to those allergic to ceftazidime)

Empirical treatment to CA-MRSA should be given to hospitalised pts with severe CAP.
It includes addition of vancomycin (15mg/kg I.V every 12 hrs). In severly ill pts loading dose of 25-30 mg/kg is given .
OR
Linezolid (600mg I.V every 12 hrs)Clindamycin (600mg I.V/oral 3 times daily) can
be given if pathogen is susceptable.If sputum culture reveals meticillin suscptible
staphylococcus therapy can be changed to nafcillin (2gm I.V every 4hrs) or oxacillin (2gm I.V every 4 hrs)

Switch to oral therapy – initially hospitalized pts are treated intravenously. Oral treatment can be syarted once pt is hemodynamically stable,improving clinically,able to take oral medicines & have normally functioning GIT.

Pts treated with intravenous betalactam & macrolides have high risk of developing drug resistant s. pneumoniae(DRSP).
High dose of amoxicillin ( 1gm orally 3 times daily) is given instead of I.V beta lactams
An alternative to pts without risk of DRSP, is to give macrolide or doxycyclin alone to complete course.
Doses for macrolides and doxycyclin is: Azithromycin : 500mg once daily Clarithromycin :500mg once daily Clarithromycin XL :500mg two tablets once
daily Doxycyclin : 100mg twice daily

Duration of therapy :- recommended duration for pts with good response in first 2-3 days is 5-7 days.
Before stopping therapy- pt should be afebrile for 48- 72 hrs , breathing without supplement oxygen ,and have no more than one clinical instability factor (i.e PR > 100bpm RR > 24cpm , systolic BP < 90mmhg)
Longer treatment is required in cases of : initial treatment not efficient against
subsequent isolated pathogen in extrapulmonary infection (meningitis or
endocarditis) if pt has empyema or lung abscess pneumonia caused by P.aeruginosa S.aureus
legionella or other unusual pathogens

Procalcitonin can be evaluated for guiding decision of stopping antibiotic treatment as its level correlate with likelihood of bacterial infection.
Follow up chest radiography- x-ray findings clear more slowly than clinical features.pts responding clinically do not require follow up x-ray.
Follow up x-ray is adviced for pts > 50 yrs , males , smokers. 7- 12 wks following treatment

Treatment failure:-may be due to delayed host response despite
appropiate treatment infection with organism not covered in
initial antibiotic regimen drug resistant organisms pt related factors – neoplasia ,aspiration
pneumonia severity of illness, neurologic disease etc.
infectious complications – lung abscess, empyema

Further evaluation : repeat histroy, x-ray , blood cultures ,
sputum cultures , Chest CT Broncoscopy Lung biopsy

Adjuvant therapy :- Glucocorticoids Tissue factor pathway inhibitors (Tifacogin –
systemic inhibitor of coagulation) Statins – antiinflammatory Vaccination - against influenza &
pnemococcal infections. Smoking cessation