Cardiovascular System
-
Upload
donna-cotton -
Category
Documents
-
view
45 -
download
0
description
Transcript of Cardiovascular System

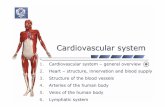
Cardiovascular System
Chapter 17

Cardiovascular SystemCardiovascular System – circulates blood continuously
thought the body to deliver oxygen and nutrients to the body’s organs and tissue and to dispose of waste.Heart (pump) and vasculature (plumbing)The heart is composed of:
Cardiac muscle AtriaVentriclesValvesCardiac arteries and veinsElectrical conduction systemCardiac Nerves
Problems or failure of any of these system can lead to serious health concerns.
Review Anatomy

Figure 17.3 Structural components of the heart.

HeartHeart – pump composed of synchronized structures
Cardiac VesselsCoronary Arteries – extensive network of arteries supplying the heartCoronary Veins – network for venous blood drainage
Conduction system – heart has it own conduction system which can initiate and transmit an electrical impulse via cardiac muscle fibersThis electrical charge stimulates muscular contraction of the heartSA node, AV node, Bundle of His, Right and Left Bundle Branch Block,
and Purkinje fibersNerves
Sympathetic – stimulate the heart, increases heart rate, force of contraction, and dilation of coronary arteries.
Parasympathetic – opposite effect CNS – influences the activation and interaction of nerves through
information supplies by the cardiac plexus.

Cardiac Musculature
Heart MuscleBase Apex – point of maximum impulse so heart beat is more
easily palpated over the apex – 5th intercostal spaceThree Layers:
Epicardium – outer layerMyocardium – thick muscular layerEndocardium - smooth inner lining of chambers

ChambersChambers in the Heart – 4 chambers
Left and right atria – receiving chambers for blood and pump blood into the ventricles
Left and right ventricles – eject blood into vessels

ValvesValves - Permit the Flow of Blood Between
Chambers and into Blood VesselsAtrioventricular (AV)
TricuspidMitral
SemilunarPulmonaryAortic

Heart SoundsHeart Sounds – Closure of valves which are associated
with the contraction and relaxation phases of the heart.Systole – refers to ventricular contraction and begins with
closure of the AV valves (S1) and ends with the closure of the aortic and pulmonic valve (S2)
Diastole – refers to ventricular relaxation and begins with closure of the aortic and pulmonic valve (S2) and ends with closure of AV valves (S1).
S1 (lub)S2 (dub)

Figure 17.5 Heart sounds in systole and diastole.

Table 17.3 Distinguishing Heart Murmurs

Table 17.3 (continued) Distinguishing Heart Murmurs

Table 17.4 (continued) Classifications of Heart Murmurs

Circulation of HeartPulmonary Circulation – carries deoxygenated
blood to the lungs, where carbon dioxide is exchanged for oxygen.
Systemic Circulation – supplies freshly oxygenated blood to the body’s periphery carrying oxygen and nutrients to cells.

ElectrocardiogramElectrocardiogram (EKG) - Paper Recording
of Deflections That Represent the Cardiac Cycle – Signifies electrical conductionElectrical deflections
P wavePR intervalQRS intervalT wave

Figure 17.11 Electrocardiogram wave.

Cardiac FunctionStroke volume - Amount of blood that is ejected with
each heartbeatCardiac output - Amount of blood ejected from the left
ventricle over one minuteCardiac index - Measurement accounting for an
individual’s weight when evaluating the pumping action of the heart

Landmarks for Cardiac AssessmentLandmarks for Cardiac Assessment
SternumClaviclesRibsSecond through fifth intercostal spaces
Correlating assessment findings over body landmarks provides vital information related to underlying pathologic mechanisms.

Figure 17.18 Landmarks in precordial assessments.

InteviewGeneral QuestionsSpecific Questions
IllnessSymptomsBehaviorsInfants and childrenPregnant femaleOlder adultEnvironment

EquipmentExamination gownExamination drapeStethoscopeMetric rulersDoppler

TechniquesPhysical Assessment of the Cardiovascular System
TechniquesInspectionPalpationPercussionAuscultation

Specific AreasSpecific Areas of the Cardiovascular Assessment
Inspection of the face, lips, ears, and scalp Skin colorMovementEarlobe creases
Inspection of the jugular veinsPulsations Distention
Inspection of the carotid arteriesPulse characteristics
Inspection of the hands and fingersColorShape of fingers

Figure 17.17 Splinter hemorrhage.

Specific AreasInspection of the chest, abdomen, legs, and
skeletal structureLandmarks
Right sternal border, 2nd intercostal spaceLeft sternal border, 2nd intercostal spaceLeft sternal border, 3rd – 5th intercostal space
Heaves and lifts

PalpationPalpation of the chest, including the following
Precordium at the right and left second intercostal spaces
Left third intercostal spaceLeft fourth intercostal spaceLeft fifth intercostal space at the midclavicular line
Position patient at a 30 degree angle or lessNo thrills, heaves or lifts should be palpated
in any of the five locations

Figure 17.19 Landmarks for palpation of the chest.

PalpationCarotid pulses (sequentially)Client may be supine or sitting upright
Asses:Presence – diminished or absent may indicate carotid disease
or dissecting aortic aneurysmStrength – should be strong but not boundingRhythm – regular patternEquality – consistent bilaterally
Palpate each artery separately – may obstruct blood flow to the brain, resulting in severe bradycardia or asystole

Figure 17.20 Palpating the carotid artery.

PercussionPercussion of the chest for cardiac border
5th intercostal space at the left anterior axillary lineNormal findings would be resonance because you will be
over lung tissueNext, percuss the mid clavicular line and the left
sternal borderShould change to dull as you percuss over the heart
Advance to the 3rd and 2nd intercostal space on the left side.
Should change from resonnance to dullness as you percuss over the heart

Figure 17.21 Percussing the chest.

Auscultation
Auscultation of the chest using the diaphragm and bell in various positions to include the following locations
Aortic area at the right second intercostal space—S2 is louder than S1Pulmonic area at the left second intercostal space—S2 is louder than S1Erb’s point at the left third intercostal space—S1 and S2 are heard
equallyTricuspid area at the left fourth intercostal space—S1 is louder than S2Apex at the left fifth intercostal space at the midclavicular line—S1 is
louder than S2

Figure 17.22 Auscultating the chest over five key landmarks.

Figure 17.24A Positions for auscultation of the heart. A. Supine.

Figure 17.24B Positions for auscultation of the heart. B. Lateral

Figure 17.24C Positions for auscultation of the heart. C. Sitting.

Auscultation of Apical PulseSpecific Areas of the Cardiovascular
AssessmentAuscultation of the carotid arteries using the
diaphragm and bellComparison of the apical pulse to a carotid pulse

Figure 17.23 Comparing the carotid and apical pulses.

Abnormal FindingsAbnormal Findings in the Cardiovascular System
Myocardial and pump disordersValvular diseaseSeptal defectsCongenital heart diseaseElectrical rhythm disturbances

Muscular and Pump DisordersMyocardial and Pump Disorders
Myocardial ischemiaMyocardial infarctionCongestive heart diseaseVentricular hypertrophy

Valvular DisordersValvular Diseases
Mitral, aortic, tricuspid, and pulmonic stenosisMitral and aortic regurgitationMitral valve prolapse

Figure 17.25 Mitral stenosis.

Figure 17.26 Aortic stenosis.

Figure 17.27 Mitral regurgitation.

Figure 17.28 Pulmonic stenosis.

Figure 17.29 Tricuspid stenosis.

Figure 17.30 Mitral valve prolapse.

Figure 17.31 Aortic regurgitation.

Setal DefectsSeptal Defects
Openings between the right and left atria or right and left ventricles

Figure 17.32 Ventricular septal defect.

Figure 17.33 Atrial septal defect.

Congenital Heart DiseasesCongenital Heart Diseases
Coarctation of the aortaPatent ductus arteriosusTetralogy of Fallot

Figure 17.34 Coarctation of the aorta.

Figure 17.35 Patent ductus arteriosus.

Figure 17.36 Tetralogy of Fallot.

Figure 17.36 (continued) Tetralogy of Fallot.

Rhythm DisturbancesElectrical Rhythm Disturbances
Ventricular tachycardiaVentricular fibrillation

Figure 17.37 Ventricle tachycardia.

Figure 17.38 Ventricular fibrillation.

Figure 17.39 Heart block.

Figure 17.40 Atrial flutter.

Figure 17.41 Atrial fibrillation.

Developmental ConsiderationsPediatric
Fetus receives oxygen and nutrients from the motherChanges occur in the newborn’s cardiovascular systemInfant’s heart rate

Developmental ConsiderationsPregnant Female
Heart is displaced to the left and upwardBlood volume increases 30 to 50 percentCardiac output and stroke volume increaseResting pulse may increaseMurmurs may be auscultated

Developmental ConsiderationsGeriatric
Loss of ventricular compliance and vascular rigidityConduction system loses automaticity

Psychosocial Considerations
Stress and workload of the heart

Cultural and Environmental Considerations
RaceEthnicityDietSubstance abuse

Healthy People 2010Focus Areas Outlined in the Healthy People 2010
Coronary heart diseaseHigh blood cholesterol

Healthy People 2010Key Objectives for Coronary Heart Disease
Reduce deathsIncrease awareness of symptoms of heart attack and
the need for rapid emergency careIncrease the numbers of adults who can administer
cardiopulmonary resuscitationReduce the number of obese individualsIncrease physical activityIncrease the number of adults who are aware of risk
factors and take action to reduce risks

Healthy People 2010Key Objectives for High Blood Cholesterol
Reduce the number of adults with elevated cholesterol levels
Increase the number of adults who have cholesterol levels measured