Autonomic Nervous System: Introduction to neurotransmitter and receptor specificity
description
Transcript of Autonomic Nervous System: Introduction to neurotransmitter and receptor specificity

Autonomic Nervous System:Introduction to neurotransmitter and receptor specificity
Thomas GuenthnerProfessor of PharmacologyCollege of MedicineTel. 996-7635Room E418, CMWE-mail: [email protected] Thanks to Dr. Richard Ye for Powerpoint concepts and slides

Identify the key conceptual similarities and differences between autonomic cholinergic and adrenergic pathways including receptor subtypes, neurotransmitters, transmitter synthesis, storage, and release, and relative specificities of drugs that stimulate or inhibit each branch or activity.
Knowledge objectives introduced by these two lectures:
List the major systems or organs innervated by the autonomic cholinergic and adrenergic systems.
Describe the organ system effects of cholinergic and adrenergic stimulation or antagonism.
Relate the tissue expression profiles of cholinergic and adrenergic receptors to their specific functions.




• All preganglionic and parasympathetic postganglionic neurons use acetylcholine as neurotransmitter. Ach is the neurotransmitter at ganglia, nmj, and muscarinic tissue synapses.
• Most postganglionic sympathetic neurons use norepinephrine which is an adrenergic neurotransmitter.
Pharmacological division of cholinergic vs. adrenergicneurotransmission
• There are exceptions: Cholinergic transmission in sympathetic system – all ganglia, adrenal medulla, sweat glads use Ach (nicotinic or muscarinic). Dopaminergic innervation in sympathetic system – renal blood vessels.

Pre-synapticnerve cell
Post-synapticnerve cell
Synapticcleft
Ca2+
Na+
Precursors(choline/tyrosine)
Synapse – site most amenable to pharmacologic manipulation:
Precursor
Neurotransmitter
Storage
Release
Recognitionby receptors
Metabolicdisposition
Manipulation possible at pre-synaptic neuron, where neurotransmitter is synthesized, stored and released upon cell activation, or at post-synaptic neuron or effector cell, where neurotransmitter is detected and its action is translated into cellular activities.

Synthesis & Storage
Actionpotential
Metabolism
Recognition(action)
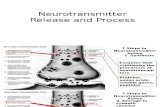
Key Steps in Neurotransmission:
Strategies for Pharmacological Intervention:
Block synthesis and storage: Usually rate-limiting steps; produce long-term effectsBlock release: Rapid action and effectiveBlock reuptake increases synaptic neurotransmitter concentrations Can be selective or non-selectiveInterfere with metabolism: Can be reversible or irreversible; blocking metabolism
increases effective neurotransmitter concentrationsInterfere with recognition: Receptor antagonists & agonists; high specificity
Release
Reuptake

Agonist: (1) A natural ligand that activates a receptor. (2) A drug that has properties similar to a natural ligand in activating the same receptor.
Antagonist: (1) A receptor-specific blocker. (2) A molecule, such as a drug (e.g., enzyme inhibitor) or a physiologic agent (e.g., hormone), that diminishes or prevents the action of another molecule.
Direct-acting: Molecule that physically binds to the target for its effect.Example: carbachol activates cholinergic receptors.
Indirect-acting: Molecule that exerts effect on the target by interacting withanother non-target site.Example:neostigmine blocks AchE, causing Ach accumulation.
Definition of Agonist and Antagonist:
Mode of Action:
Mode of action and agonism are different concepts. For example, a direct- acting molecule can be either agonistic or antagonistic.

•Discovered that stimulation of the vagus of a frog heart causes release of a substance that, when applied to a second heart, could slow heart rate. He called this “Vagusstoff”, demonstrating the chemical basis of neurotransmission.
Otto Loewi (Nobel Laureate, 1936)
• Also found that atropine can prevent the inhibitory action, but not the release, of “Vagusstoff”.
• Exposure of “Vagusstoff” to frog heart homogenate inactivates it.
• Physostigmine enhances the effect of vagus stimulation on the heart, and prevents the destruction of “Vagusstoff”.

Synthesis of acetylcholine:
CH3
CH3
CH3
N+–CH2–CH2–OH
CoA–S–C–CH3
O
Choline
Acetyl-CoA
+
Cholineacetyltransferase
CH3
CH3
CH3
N+–CH2–CH2–O –C–CH3
O
CoA-SH
+
CoA
Acetylcholine

Synthesis, storage and release of acetylcholine:
Pre-synapticcell
Post-synapticcell
Ach
Ca2+
Na+Choline(10 M)
Choline
Recognitionby receptors
Ca2+
Ach
Ach
Ach
Nerveimpulse
NN
NM
AchAc-CoA
ChAT
Ach
AchE
AchE
choline+ acetic acid
CAT = choline acetyltransferaseAchE = acetylcholinesterase
Synapticcleft
Antiporter

CH3COOH+AchE
(CH3)3 N+–CH2–CH2–OH(CH3)3 N+–CH2–CH2–O –C–CH3
OH2O
OH(-)AchE
Glu202Tyr337
Ser203Glu334His447
Degradation of acetylcholine:
Steps involved in the action of acetylcholinesterase:
1. Binding of substrate (Ach)
2. Formation of a transient intermediate (involving -OH on Serine 203, etc.)
3. Loss of choline and formation of acetylated enzyme
4. Deacylation of AchE (regeneration of enzyme)
600,000 Ach molecules / AchE / min= turnover time of 150 microseconds
Choline Acetic acid

Drug intervention -- Cholinergic transmission
Precursor transport
Synthesis
Hemicholinium
Storage Vesamicol
Release Botulinum toxin
Degradationby AchE
Receptor+ action
Ach
Cholinergic agonists(direct acting)
CarbacholPilocarpine
(Rate-limiting)
AntiChE
Reversible (neostigmine)Irreversible (organo- phosphate)
: Stimulatory : InhibitorySolid: AgonisticDotted: Antagonistic
Cholinergic antagonists
Atropine (anti-M)Succinylcholine (anti-NM)Trimethaphan (anti-NN)

Physostigmine’s effect on acetylcholine receptor is indirect. This effect is mediated through the inhibition of cholinesterase, which causes an increase in the local concentration of acetylcholine. The net effect is agonistic on acetylcholine receptor.
An example of indirect-acting pharmacological agents:

HO
HO
CH2
NHCH3
OH
CH
Epinephrine
HO
HO
CH2
NH2
OH
CH
Norepinephrine
HO
HO
CH2
NH2
CH2
Dopamine
HO
HO
HC
NH2
CH2
DOPA
COOHHO HC
NH2
CH2
Tyrosine
COOHTH
DD (L-AAD)
DBHPNMT
Adrenal medulla
Synthesis of Catecholamines Tyrosine hydroxylase
Dopa decarboxylase (L-amino acid decarboxylase)
Dopamine -hydroxylase
Phenylethanolamine-N-methyl transferase
13
Julius Axelrod (Nobel Laureate, 1970)
His discoveries concern the mechanisms which regulate the formation of norepinephrinein the nerve cells and the mechanisms which are involved in the inactivation of this important neurotransmitter.

Pre-synapticPost-synaptic
Ca2+
Na+
Tyrosine
Cellular messengersand effects
Diffusion, metabolism
Tyrosine
Dopa
THDD Dopamine
(DA)
NE
DBH
ATP
Ca2+
NE
DBH
ATP NE
NE
COMT
R
R
R
NE
(-)
Signal
Regulation of Norepinephrine Synthesis and Metabolism:
Uptake-1
Normetanephrine (NMN)

Drug intervention -- Adrenergic transmission
Tyrosine
DopaDA
Metyrosine
Vesicle (DANE)
Reserpine
ReleaseBretylium, guanethidine
Recaptureby Uptake-1
Receptor+ action
NE
Adrenergic agonists(direct acting)
IsoproterenolAlbuterol
(Rate-limiting)
CocaineTricyclic antidepressants (e.g. imipramine)
Adrenergic antagonists
Phentolamine (-blocker)Propranolol (-blocker)
TH
Amphetamine, tyramine,ephedrine
: Stimulatory : InhibitorySolid: AgonisticDotted: Antagonistic

PNS Receptor Functions

PNS Receptors - Pharmacological Classification:
Cholinergic R
Adrenergic R
Dopamine R
Muscarinic R
Nicotinic R
M1, M3, M5 (Gq coupled)
M2, M4 (Gi coupled)
NM (neuromuscular, or muscle type)
NN (neuronal, or ganglion type)
1,
21,
2,
D1, D2, D3, D4, D5
Other receptors (receptors for NANC transmitters,e.g. nitric oxide, vasoactive intestinal peptide, neuropeptide Y)
(mAChR)
(nAChR)

Thor
acol
umba
rC
rani
alS
acra
l
CNS Pre-ganglionic Ganglion Post-ganglionic
Parasympathetic Ach
Nicotinic
Ach
Nicotinic
Ach
Nicotinic
Ach
Nicotinic
Ach
Nicotinic
Epi
Sympathetic
Sympathetic
Sympathetic
Sympathetic (adrenal medulla)
Motor (somatic)
Ach
Ach
Muscarinic
Muscarinic
NE
Adrenergic()
D
Dopaminergic(D1)
Ach
Nicotinic
Cardiac & smoothmuscles, gland cells,nerve terminals
Cardiac & smoothmuscles, gland cells,nerve terminals
Sweat glands
Renal vascularsmooth muscle
Released intoblood
Skeletal muscle
Ach = acetylcholine NE = norepinephrineEpi = epinephrineD = dopamine
Effectors

Adrenergic receptors

Classification of adrenergic receptors by agonist potency
-- NE Epi > Iso
-- Iso > Epi > NE
NE = norepinephrineEpi = epinephrineIso = isoproterenol
HO
HO
CH2
NHCH3
OH
CH
Epi
HO
HO
CH2
NH2
OH
CH
NE
HO
HO
CH2
NH
OH
CH
Iso CH(CH3)2

Agonist
Signaling properties of adrenergic receptors
AgonistAgonist1 2 1,2,3
Gq Gi Gs
Inositol phosphates (IP3)
Diacyl glycerol (DAG)
cAMP cAMP
Calcium channels
K+ conductance
Mostly excitatory Mostly inhibitory Mostly excitatory
NorepinephrineEpinephrinePhenylephrine
NorepinephrineMethyl NEClonidine
IsoproterenolAlbuterol (2)Dobutamine (1)

Gs and Gi proteins have different functionsGs and Gi proteins have different functions
Agonist
s
Agonist
iACAC
s
i
Gs = stimulatory G protein
Gi = inhibitory G protein
AC = adenylyl cyclase (convert ATP to cAMP)

1: postsynaptic effector cells, especially smooth muscleVasoconstriction, relaxation of gastrointestinal smooth muscle, hepaticglycogenolysis
2 presynaptic adrenergic nerve terminals (autoreceptor), platelets, lipocytes, smooth muscle
Inhibition of transmitter release, platelet aggregation, contraction ofsmooth muscle
1 postsynaptic effector cells: heart, lipocytes, brain, presynaptic adrenergic / cholinergic terminals
Increased cardiac rate & force, relaxation of gastrointestinal smooth muscle
2 postsynaptic effector cells: smooth muscle, cardiac muscleBronchodilation, vasodilation, relaxation of visceral smooth muscle, hepaticglycogenolysis
postsynaptic effector cells: lipocytesLipolysis
Distribution and functions of adrenergic receptors:



O
OH
NH
CH3
CH3
Propranolol
NH
O
OH
NH
CH3
CH3
Pindolol
O
OH
NH
CH3
CH3
NHO
CH3
CH3
Acebutolol
O
OH
NH
CH3
CH3
OH
OH Nadolol
O
OH
NH
CH3
CH3
OCH3
Metoprolol
O
OH
NH
CH3
CH3
NH2
O
Atenolol1 antagonistic half-life
1 and 2 antagonistic
half-life 2 antagonistic effect
1 antagonisticPartial 2 agonistic
1 antagonisticPartial 2 agonistic

Dopaminergic receptors

HO
HO
CH2
NHCH3
OH
CH
Epinephrine
HO
HO
CH2
NH2
OH
CH
Norepinephrine
HO
HO
CH2
NH2
CH2
Dopamine
HO
HO
HC
NH2
CH2
DOPA
COOHHO HC
NH2
CH2
Tyrosine
COOHTH
DD (L-AAD)
DBHPNMT
Tyrosine hydroxylase
Dopa decarboxylase (L-amino acid decarboxylase)
Dopamine -hydroxylase
Phenylethanolamine-N-methyl transferase
13

Dopaminergic receptors in the periphery
Dopamine receptors play important roles in CNS. Notably, dopamine neurotransmission is involved in several diseases including Parkinson’s disease, schizophenia, and attention deficiency disorder.
There are 5 types of dopamine receptors (D1 – D5). In periphery, D1 dopamine receptor mediates renal vasodilation, and increased myocardial contractility.
Agonist AgonistD2,3,4D1,5
GiGs
cAMP cAMP

Cholinergic receptors

“Nicotinic actions” -- similar to those induced by nicotine; action mediated by nicotinic cholinergic receptors:
• stimulation of all autonomic ganglia (NN)• stimulation of voluntary muscle (NM)• secretion of epinephrine from the adrenal medulla (NN)
Cholinergic receptors: Nicotinic
Nicotiana tabacum(cultivated tobacco)

Nicotinic acetylcholine receptor: Function
Ligand-gated ion (Na+) channel
- an “Ionotropic Receptor”
• Acetylcholine binds to the -subunits of the receptor making the membrane more permeable to cations (sodium) and causing a local depolarization. The local depolarization spreads to an action potential, or leads to muscle contraction when summed with the action of other receptors. The ion channel is open during the active state.
• Nicotine in small doses stimulates autonomic ganglia and adrenal medulla. When large doses are applied, the stimulatory effect is quickly followed by a blockade of transmission.

Nicotinic receptor antagonistsCompetitive vs. depolarizing
CompetitivePhysically blocks Ach binding
INHIBITOR
DepolarizingBinds and locks the receptoropen

“Muscarinic actions” -- reproduced by injection of muscarine, from Amanita muscaria (fly agaric). Similar to those of parasympathetic stimulation
• Neural/enteric (M1): CNS, ENS, gastric parietal cells (excitatory; Gq)• Cardiac (M2): atria & conducting tissue; presynaptic (inhibitory; Gi)• Glandular/endothelial (M3): exocrine glands, vessels (excitatory; Gq)• Neural (M4): CNS (inhibitory; Gi)• Neural (M5): CNS (excitatory; Gq)(Sites of primary expression are listed; all are found in CNS)
Cholinergic receptors: Muscarinic
Multiple muscarinic cholinergic receptors distributed in different tissues. Therefore, the “muscarinic actions” are dependent on the receptors in different tissues and cells.

Agonist
Muscarinic acetylcholine receptors –G Protein-Coupled Receptors (“Metabotropic” Receptors)
Agonist
M1(enteric, neuronal)
M2(cardiac)
M3(glandular, vascular )
Gq Gi IP3, DAG
(Depolarization)
(Stimulation) Intracellular Ca2+
cAMP Ca2+ channel
K+ conductance K+ conductance
Mostly excitatoryCNS excitationGastric acid secretionGastrointestinal motility
Mostly inhibitoryCardiac inhibitionPresynaptic inhibitionNeuronal inhibition
Glandular secretionContraction of visceral smooth muscleVasodilation (via NO) (Slow IPSP)
(Inhibition)
M5(CNS)
M4(CNS)

Intracellular signaling triggered by acetylcholine in the Heart
Main molecular players: M2, heterotrimeric G Protein Gi, Adenylyl cyclase

Clinical manifestation of excessive cholinergic effects
D – DefecationU – Urination M – MiosisB – BradycardiaE – EmesisL – Lacrimation S – Salivation
(DUMBELS)

Effects of muscarinic antagonists
“DRY AS BONE, RED AS A BEET, MAD AS HATTER.”• Decreased sweating, salivation and lacrimation• Reflex peripheral (cutaneous) vasodilation to
dissipate heat (hyperthermia) • CNS effects of muscarinic inhibition -- restlessness,
delerium, hallucination ALSO:BronchodilationTachycardiaMydriasis (pupil dilation) and Cycloplegia (loss of focus)GI and Bladder atony

Physiological Effects of ANSStimulation and Inhibition


Receptor distribution and effects in the autonomic nervous system:
Organ Receptor Parasympathetic Receptor
HeartRateForce Automaticity
Automaticity Force
Rate Force Conduction velocity AV block
M2M2M2
Arterioles
SA nodeAtrial muscleAV node
Ventricular muscle
Blood vessels
CoronarySkeletal muscleVisceraSkinBrainErectile tissueSalivary gland
ContractionRelaxationContractionContractionContractionContractionContractionContractionRelaxation
RelaxationRelaxation
Vein
M3M3
Sympathetic
(Continued, next page)
M3

Organ Sympathetic Receptor Parasympathetic Receptor
Relaxation
Motility Contraction
ContractionRelaxation
Viscera
Bronchiolar SMC GlandsGI track Smooth muscle Sphincters Glands
Uterus
Secretion
Motility RelaxationSecretionGastric acid secretion
Variable
M3
M3M3M3M1
Skin Pilomotor SMC Contraction (piloerection)
Salivary glands Secretion Secretion M3
Lacrimal glands Secretion M3
Kidney Renin release
Liver GlycogenolysisGluconeogenesis
Fat Lipolysis
M3Contraction
From: Rang et al. Pharmacology, 6th Ed. p. 169. Also, see Katzung, Basic & Clinical Pharmacology, 10th Ed. p.86.


Cardiovascular Pharmacology(Blood Pressure)


Cardiovascular effects of intravenous infusion of epinephrine, norepinephrine, and isoproterenolin man. Norepinephrine (predominantly -agonist) causes vasoconstriction and increased systolicand diastolic BP, with a reflex bradycardia. Isoproterenol (-agonist) is a vasodilator, but stronglyincreases cardiac force and rate. Mean arterial pressure falls. Epinephrine combines both actions.

Two kinds of effects produced by Ach. A. Ach causes a fall in BP due to vasodilation.B. A larger dose of Ach also produces bradycardia, further reducing BP.C. Atropine blocks the effect of Ach in lowering BP.D. Still under the influence of atropine, a much larger dose of Ach causes a rise in BP and tachycardia.
Sir Henry Hallett Dale(Nobel laureate, 1936)
A, B: Muscarinic effects of Ach (M3, M2)C: Muscarinic antagonistic effect (M)D. Stimulation of sympathetic ganglia (NN)
(Arterial pressure of ananesthetized cat wasmeasured)

Intracellular signaling triggered by acetylcholine in the endothelium
eNOS
●NO
L-Arg
L-Citruline
Major molecular players: M3, heterotrimeric G Protein Gq, Ca(2+)-CaM, eNOS, NO
eNOS Nitric oxide synthase

Nitric oxide (NO) signaling pathway for SMC relaxation
Secondmessenger
Inhibition of PDE causes sustained levelof cGMP that maintains SMC relaxation.
Sildenafil (Viagra)is an inhibitor forPDE 5.

Pulmonary Pharmacology(Asthma and COPD)



Ocular Pharmacology(Glaucoma)


Lens
Pupillary dilator muscle ()Pupillary constrictor muscle (M3)
Secretion of aqueous humor ()(M3)
Cholinergic effects: Adrenergic effects:
• Contraction of pupillary constrictor muscle-- miosis• Contraction of ciliary muscle - bulge of lens-- near vision, outflow of aqueous humor
• Contraction of pupillary dilator muscle-- mydriasis• Stimulation of ciliary epithelium-- production of aqueous humor
Trabecular meshwork(opened by pilocarpine)