ACLS Arrhythmias & Defibrillation
-
Upload
mojakomojaja -
Category
Documents
-
view
233 -
download
0
Transcript of ACLS Arrhythmias & Defibrillation
-
7/27/2019 ACLS Arrhythmias & Defibrillation
1/143
SARAWAK GENERAL HOSPITAL
-
7/27/2019 ACLS Arrhythmias & Defibrillation
2/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
3/143
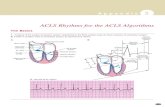
Conduction System
SA Node
AV node
His bundle
Right bundle branch
Left bundle branch
Anterior fascicle
Posterior fascicle
Purkinje fibers
-
7/27/2019 ACLS Arrhythmias & Defibrillation
4/143
1
2
3
4
5
5
6
-
7/27/2019 ACLS Arrhythmias & Defibrillation
5/143
Physiology of Action Potential An electrical impulse precedes each
heartbeat (mechanical contraction). Each heart muscle cell is stimulated to
contract by electrical process called actionpotential. (composed of five phases) The ECG records the summation of action
potential of the muscle cells in the atria
and ventricles. i.e records only theelectrical event Echocardiogram records the mechanical
contraction from the electrical event
-
7/27/2019 ACLS Arrhythmias & Defibrillation
6/143
Action Potential
Electrical Activity
Mechanical Activity
Muscle Cells
ECG Tracing
Cardiac Muscle
-
7/27/2019 ACLS Arrhythmias & Defibrillation
7/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
8/143
Causes Three mechanisms:
(1) Disturbances in AUTOMATICITY
speeding up (tachycardia),
slowing down (bradycardia), abnormal depolarization (ectopic or escape beat)
May involve
SA node atrium
AV node
ventricles
-
7/27/2019 ACLS Arrhythmias & Defibrillation
9/143
Causes
(2) Disturbances in CONDUCTION
Either too rapid (WPW syndrome) or
Too slow ( AV heart block)
(3) Combination of altered
automaticity and conduction
-
7/27/2019 ACLS Arrhythmias & Defibrillation
10/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
11/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
12/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
13/143
Normal Pacemaker Rate
SA NODE
RATE 60-100AV JUNCTION
RATE 40-60
VENTRICLES
RATE 15-40
-
7/27/2019 ACLS Arrhythmias & Defibrillation
14/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
15/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
16/143
NORMAL SINUSRHYTHM
Pacemaker impulses are
initiated in the sinoatrial (SA) node,
through atrial pathways,
delayed at atrioventricular (AV) node.
down the bundle branches to Purkinje
fibers in the ventricles
Atrial depolarization P wave.
Ventricular depolarization QRS
-
7/27/2019 ACLS Arrhythmias & Defibrillation
17/143
Normal Sinus Rhythm
Sinus Arrhythmias
Sinus Tachycardia
Sinus Bradycardia
Sinus Rhythm & its variants
-
7/27/2019 ACLS Arrhythmias & Defibrillation
18/143
NORMAL SINUSRHYTHM
CHARACTERISTICS
The P wave is usually upright in leads II, III, aVF,
and V1. Its morphology remains constant at all times.
P-P and R-R intervals are equal and regular.
Atrial and ventricular rates are identical range between 60 and 100 bpm.
There is no ectopic activity.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
19/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
20/143
SINUS ARRHYTHMIA
(SINUSDYSRHYTHMIA)
a sinus rhythm with a rate that varies with
respiration (respiratory sinus arrhythmia)
characterized by alternate speeding up andslowing down of the heart rate
usually benign
Rarely non respiratory sinus arrhythmia
-
7/27/2019 ACLS Arrhythmias & Defibrillation
21/143
SINUS ARRHYTHMIA
(SINUSDYSRHYTHMIA)
In respiratory sinus arrhythmia,
the rate increases with inspiration &
decreases with expiration.
In non respiratory sinus arrhythmia,
the irregularity of the rhythm, not
correlated with the respiratory cycle.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
22/143
SINUS ARRHYTHMIA (SINUS
DYSRHYTHMIA)ETIOLOGY
Respiratory sinus arrhythmia
Normal in children and young adults.
Non respiratory sinus arrhythmia may be
with cardiac disease and
MI esp with sinus bradycardia,digoxin therapy
enhanced vagal tone.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
23/143
ExpirationInspiration
-
7/27/2019 ACLS Arrhythmias & Defibrillation
24/143
SINUS TACHYCARDIAsinus rhythm at a rate 100 bpm.
ETIOLOGY
1. increased physiologic demand for oxygen
(stress, exercise, pain, excessive caffeine)2. Hyperthyroidism, heart failure, myocardial
infarction, pulmonary embolism, medications(e.g., atropine, epinephrine, isoproterenol), fever,anemia, hypoxia, and shock
3. Physiologic ST commonly observed in neonates(HR may btw 100 - 160 bpm)
-
7/27/2019 ACLS Arrhythmias & Defibrillation
25/143
SINUS TACHYCARDIA
CHARACTERISTICS
same characteristics as NSR
except the ventricular rate 100 bpm
gradual acceleration of sinus node discharge
-
7/27/2019 ACLS Arrhythmias & Defibrillation
26/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
27/143
Sinus Bradycardia
Characteristics
same as for NSR,except the ventricular rate 60bpm
-
7/27/2019 ACLS Arrhythmias & Defibrillation
28/143
Sinus BradycardiaEtiology
1. physiologic causes (athletes, sleep)
2. Vagal stimulation
3. Sick sinus syndrome4. hypothyroidism, hypothermia, electrolyte
imbalances (e.g., hyperkalemia), Inferiormyocardial infarction
5. medications (e.g., blk, ca2+ channel blk,digoxin)
-
7/27/2019 ACLS Arrhythmias & Defibrillation
29/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
30/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
31/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
32/143
Atrial Premature Complexes
Atrial Tachycardia
Multifoci Atrial Tachycardia Paroxymal Supraventriculat Tachycardia
Atrial Flutter
Atrial Fibrillation Junctional Premature Complexes
Supraventricular Arrhythmias
-
7/27/2019 ACLS Arrhythmias & Defibrillation
33/143
ATRIAL PREMATURE COMPLEXES
(APC)DEFINITION
results from apremature supraventrictilar
impulse that originates somewhere in theatria outside of sinoatrial (SA) node.
also called atrial ectopic complexes
-
7/27/2019 ACLS Arrhythmias & Defibrillation
34/143
ATRIAL PREMATURE
COMPLEXESCHARACTERISTICS
1. R-R interval is irregular. The premature complexdisturbs the regularity of the underlying rhythm
2. The morphology of the ectopic/premature Pwave is different from the sinus P wave.
3. The premature P wave is followed by a QRS
complex if the impulse conducted into theventricles.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
35/143
ATRIAL PREMATURE
COMPLEXES1. QRS complex is narrow if conduction in the
ventricles is disturbed.
2. If the AV node conducts a premature impulseinto the ventricle when they have not fully
repolarized, the resulting QRS complex may
appear wide and abnormally shaped.
3. This is known as an APC conducted withaberration and must be differentiated from a
ventricular premature complex
-
7/27/2019 ACLS Arrhythmias & Defibrillation
36/143
Clinical tips
The best leads for assessment of atrial
rhythm disturbances are
II, III, aVF, and V1,
P waves are usually most prominent in these
leads.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
37/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
38/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
39/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
40/143
WANDERING ATRIAL
PACEMAKERDEFINITION
a supraventricular rhythm in which
pacemaker impulses originate from 2
sites in the SA node, atria, or AV junction
discharge at a rate of 60 to 100 beats per
minute
-
7/27/2019 ACLS Arrhythmias & Defibrillation
41/143
WANDERING ATRIAL
PACEMAKERCHARACTERISTICS1. P wave morphologies vary because impulses
originate from different sites.
2. P-P intervals (and subsequent R-R intervals) mayalso vary because each impulse travels throughthe atria via a slightly different route.
3. One P wave for every QRS complex.
4. Overall atrial and ventrictilar rates remain
between 60 and 100 bpm.5. QRS complexes are usually unchanged. They are
narrow as long as ventricular depolarization isundisturbed.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
42/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
43/143
MULTIFOCAL ATRIALTACHYCARDIA
DEFINITION
Multifocal atrial tachycardia (MAT) is an
ectopic supraventricular tachycardia originates from three or more atrial foci
rate of 100 to 250 bpm.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
44/143
MULTIFOCAL ATRIALTACHYCARDIA
CHARACTERISTICS
1. Three or more P wave morphologies
(multiple foci)
2. One P wave for every QRS complex
(1: 1 conduction)3. Irregular rhythm; varying P-P and R-R intervals
4. PR intervals varying slightly from beat to beat
5. QRS complexes possibly identical to each otheror slightly widened secondary to aberrantintraventricular conduction
6. Rate than 100 bpm
-
7/27/2019 ACLS Arrhythmias & Defibrillation
45/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
46/143
ATRIAL TACHYCARDIA
DEFINITION
a supraventrictilar rhythm originating
outside of the SA node
rate between 120 and 250 bpm.
frequently a result of digitalis toxicity.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
47/143
ATRIAL TACHYCARDIA
CHARACTERISTICS
rhythm is regular(R-R intervals are equal)
atrial rate is 120 to 250 bpm. P-P intervals are equal
Conduction is commonly 1:1 (one P wave forevery QRS complex).
Conduction may be 2: 1 or greater especially inthe presence of digitalis toxicity.
(atrial tachycardia with AV block)
-
7/27/2019 ACLS Arrhythmias & Defibrillation
48/143
ATRIAL TACHYCARDIA
PR interval is short when conduction through theAV node is 1: 1.
P wave morphology is often different from NSR
shape of the QRS is unchanged from NSR unlessconduction in the ventricles is disturbed.
Atrial tachycardia may occur in paroxysms;
when it terminates, there may be a long pausebefore NSR resumes.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
49/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
50/143
PAROXYSMAL SUPRAVENTRICULAR
TACHYCARDIA (PSVT)
DEFINITION
supraventricular impulses are conductedabnormally between atria and ventricles.
ventricles are depolarized 100 bpm.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
51/143
ETIOLOGY1. AV nodal reentry tachycardia (AVNRT)
Micro reentry circuit
A supraventricular impulse is conducted slowly
down one pathway in the AV node toward the
ventricles and is then conducted rapidly back
into the atria along a secondpathway within the
AV node.
The atria and ventricles are depolarized almost
simultaneously.
60-70% of PSVT
-
7/27/2019 ACLS Arrhythmias & Defibrillation
52/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
53/143
ETIOLOGY2. Atrioventricular Reentrant Tachycardia
(AVRT) Uses a macro reentry circuit, such as bundle of
Kent, that bypasses the AV node to form anaccessory bridge from the atria to the ventricles
Most well known Wolff-Parkinson-White(WPW) syndrome
Manifest AP
Concealed AP
Less common form of PSVT
The atria and ventricles are depolarizedsequentially.
As with AVNRT, the cycle in AVRTperpetuates itself as the impulse repeatedlytravels the same route.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
54/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
55/143
ATRIAL FLUTTER
DEFINITION
a supraventricular dysrhythmia
characterized by the appearance of sawtooth-shaped flutter waves
rate between 250 and 350 bpm.
associated with a reentry mechanismwithin the atria esp around the pulmonaryveins
-
7/27/2019 ACLS Arrhythmias & Defibrillation
56/143
CHARACTERISTICS1. P waves are absent.
2. flutter (F) waves represent abnormaldepolarization of the atria.
1. They assumed a saw tooth that is
2. most easily seen in leads II, III, and aVF, and V1.
3. The flutter waves appear contiguously with noisoelectric baseline visible.
Some flutter waves may be obscured by theQRS complex.
1. atrial rate (flutter rate) ranges btw 250 - 350 bpm(average is 300bpm).
2. The ventricular rate is usually slower than the
atrial rate
-
7/27/2019 ACLS Arrhythmias & Defibrillation
57/143
CLINICAL TIP Flutter waves may be difficult to identify if 2:1 conduction Vent rate of 150 bpm
Vagal maneuvers like carotid sinus massage or drugs toincrease block at the AV node
slowing the ventricular resp enough to unmask hidden flutter waves.
Atril flutter must be differentiated from atrial tachycardiaby closely examine the P wave.
In atrial flutter, F waves is contiguous
In atrial tachycardia, ectopic P waves are separated by anisoelectric baseline.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
58/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
59/143
ATRIAL FIBRILLATION
DEFINITION
A supraventricular dysrhythmia
characterized bv multiple ectopic atrial foci,uncoordinated atrial contractions, and aclassically irregular ventricular rate.
May occur intermittently, (paroxysmal atrialfibrillation), but it frequently becomes achronic condition.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
60/143
CHARACTERISTICS
1. There are no P waves.2. fibrillatory (f) waves arise within the atria. small,
poorly defined, and distort the baseline, may be fine orcoarse in appearance.
3. R-R intervals are irregularbecause conduction throughthe AV node is highly variable.
4. QRS complexes are usually narrow unless conduction inthe ventricles is abnormal. As impulses are conductedirregularly through the AV node with some of these
impulses aberrantly conducted thru the ventricular5. Ashman's phenomenon (characterized by wide QRS
complexes that can easily be mistaken for (VPCs).
-
7/27/2019 ACLS Arrhythmias & Defibrillation
61/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
62/143
JUNCTIONAL PREMATURE COMPLEXES
DEFINITION
a premature (ectopic) supraventricular
impulse that originates from the area
in and around the AV junction.
is also known as a premature
junctional complex (PJC).
-
7/27/2019 ACLS Arrhythmias & Defibrillation
63/143
AV NODAL
EXTRASYSYTOLES
Conduction
1. Retrogadely to the
Atria and
2. Antegradely to theventricle
Antegrade conduction
To ventricle only
(retrograde conductionis blocked)
-
7/27/2019 ACLS Arrhythmias & Defibrillation
64/143
CHARACTERISTICS R-R interval is irregular. The premature
complex disturbs the regularity of theunderlying rhythm.
A visible P wave may or may not be associatedwith a premature QRS complex
If the P wave is visible, commonly occurs eitherjust before or just after the QRS complex
usually inverted in II, III, aVF
-
7/27/2019 ACLS Arrhythmias & Defibrillation
65/143
JUNCTIONAL PREMATURE
COMPLEXES
An inverted P wave implies that the ectopic impulsefrom the AV junction was conducted retrogradely(backward) into the atria.
If the P wave appears before the QRS complex, theatria were depolarized before the ventricles.
If the P wave occurs immediately after the QRScomplex, the atria were depolarized after theventricles.
If the P wave is buried in the QRS complex, it isassumed that the atria and ventricles weredepolarized simultaneously)
-
7/27/2019 ACLS Arrhythmias & Defibrillation
66/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
67/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
68/143
JUNCTIONAL EXCAPE
RHYTHMDEFINITION
A passive escape rhythm that originates in
the AV junction and usually appearssecondary to depression of the higher sinus
pacemaker.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
69/143
CHARACTERISTICS1. The ventricular rate is between 40 and 60 bpm
2. The R-R interval is regular.
3. There is one P wave for every QRS complex (1: 1conduction). The P wave may appearbefore the QRSorafterthe QRS, or it may beburied within the QRS
complex.4. The P wave is usually inverted in the inferior leads (II,
III, aVF).
5. If the ectopic P wave precedes the QRS complex, theresultant PR interval is abnormally short-often less
than 0. 1 2 second.6. The QRS complex is narrow as long as intraventricular
conduction is undisturbed.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
70/143
ACCELERATED JUNCTIONAL
RHYTHM AND JUNCTIONAL
TACHYCARDIA
DEFINITION
Represent supraventricular dysrhythmias
arising from the AV junction at ratesexceeding the inherent junctional escape
rate of 40 to 60 bpm.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
71/143
CHARACTERISTICS
All the characteristics described for junctionalescape rhythm apply, except for ventricularrate.
In accelerated junctional rhythm theventricular rate is between 60 and 100 bpm.
Injunctional tachycardia the ventricular rate is
100 bpm or faster.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
72/143
Is there a normal looking QRS
complex ? If there is a abnormal looking QRS complex
considerVentricular arrhythmias.
If there is no QRS complexes at all,considerAsystole
-
7/27/2019 ACLS Arrhythmias & Defibrillation
73/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
74/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
75/143
Ventricular Arrhythmias
VENTRICULAR PREMATURE BEAT (VPB)
VENTRICULAR ESCAPE COMPLEXES
VENTRICULAR TACHYCARDIA (VT)
TORSADE DE POINTES
ACCELERATED IDIOVENTRICULAR
RHYTHM
VENTRICULAR FIBRILLATION (VF)
-
7/27/2019 ACLS Arrhythmias & Defibrillation
76/143
VENTRICULAR PREMATURE BEATS
early occurring widened QRS complexes
microreentry at the level of the Purkinje fiber
bizarre morphology QRS complex of a VPB is widened, bizarre, and often
notched, with a QRS duration >0.16 seconds
It may have a morphology which resembles a right or
left bundle branch block depending upon the location oforigin.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
77/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
78/143
VENTRICULAR PREMATURE BEATS
Unifocal VPBs
all have a single morphology;
the interval between the VPB and the preceding sinus
beat is usually identical (fixed coupling cycle).
Multifocal VPBs
multiple different QRS morphologies
caused by various different reentrant circuits
varying coupling cycles between the sinus beat and theVPB.
In general there is no P wave identified before apremature QRS complex.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
79/143
VENTRICULAR PREMATURE BEATS
A full compensatory pause usually follows theVPB;
interval between the QRS complexes before andafter the premature beat is 2X the interval btw twosuccessive sinus beats.
On occasion, the VPB may be interpolated,
ie, it occurs between two normal sinus QRScomplexes and does not alter the underlying sinusor ventricular rate.
Other findings on the ECG include markedrepolarization abnormalities, manifested as STsegment and T wave abnormalities.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
80/143
VENTRICULAR PREMATURE BEATS
Ventricular bigeminy
ventricular premature beat follows each sinus
beat often becomes self perpetuating, asituation known as the rule of bigeminy. This
occurs because the long cycle length tends to
precipitate a VPB.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
81/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
82/143
VENTRICULAR PREMATURE BEATS
Ventricular trigeminy
two sinus beats are followed by the ventricular
premature beat. Thus, every third beat is aventricular premature beat (show ECG 3).
-
7/27/2019 ACLS Arrhythmias & Defibrillation
83/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
84/143
VENTRICULAR PREMATURE BEATS
Ventricular couplets
two VPBs in a row (show ECG 4)
there is often a compensatory pause after the secondpremature beat
the two premature beats may have an identicalmorphology (unifocal couplet), or their morphologymay differ (multifocal couplet)
the RR interval between the two successive VPBs varies
widely.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
85/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
86/143
VENTRICULAR PREMATURE BEATS
Interpolated VPBs
VPB may be interpolated between two successive sinusbeats without altering the underlying sinus RR interval(show ECG 5).
-
7/27/2019 ACLS Arrhythmias & Defibrillation
87/143
VENTRICULAR ESCAPE
-
7/27/2019 ACLS Arrhythmias & Defibrillation
88/143
VENTRICULAR ESCAPE
COMPLEXES OR RHYTHM when there is failure of the sinus and AV node togenerate an impulse
absence of P wave activity
associated with a widened QRS complex thatresembles a VPB and occurs after a pause ofvariable duration (but always greater than thenormal sinus RR interval)
persistence of this activity leads to multiplesuccessive ventricular complexes representing anescape ventricular rhythm with a rate that isslower than the normal sinus rhythm
-
7/27/2019 ACLS Arrhythmias & Defibrillation
89/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
90/143
VENTRICULAR TACHYCARDIA
is defined as three or more successive ventricularcomplexes.
non sustained VT is a series of repetitive
ventricular beats which have a duration of lessthan 30 seconds; sustained VT lasts for more than30 seconds.
the rate of VT is generally greater than 100 beats
per minute, but may vary widely
the rhythm is usually regular, although there maybe slight irregularity of the RR intervals.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
91/143
VENTRICULAR TACHYCARDIA
features of ventricular tachycardia include:
abnormal morphology of the QRS complex, the QRS
axis is typically shifted (often to the left), the width of
the QRS complex is generally >0.16 sec.
positive or negative concordance of the QRS complex
across the precordial leads (eg, R waves or S waves
only)
a monophasic Rr' pattern in lead 1 (termed rabbit ears)with a taller left ear.
an indeterminate axis (between -90 and -180)
-
7/27/2019 ACLS Arrhythmias & Defibrillation
92/143
VENTRICULAR TACHYCARDIA
Monomorphic VT
all QRS complexes of an episode are identical
often displays subtle changes of the QRScomplexes with regard to
morphology and
width
-
7/27/2019 ACLS Arrhythmias & Defibrillation
93/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
94/143
VENTRICULAR TACHYCARDIA
Polymorphic VT
QRS complexes within each episode displaymarkedly different morphologies
the RR intervals may be grossly irregular(showECG 9).
The differences in QRS morphology result
from changes in the direction (vector) ofmyocardial activation due to markedheterogeneity of the electrophysiologiccharacteristics of the ventricular myocardium.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
95/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
96/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
97/143
Torsade de pointes
is an atypical, rapid, and bizarre form ofventricular tachycardia
it means "twisting of points" a name that refers to
the continuously changing axis of polymorphicQRS morphologies that are observed during eachepisode
the polymorphic VT is associated with a
congenital or acquired prolongation of the QTinterval, suggesting a prolonged refractory periodand repolarization time
-
7/27/2019 ACLS Arrhythmias & Defibrillation
98/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
99/143
Torsade de pointes
there often is heterogeneity of repolarization
or dispersion of refractoriness.
Torsade is usually initiated by a long RRinterval (often a post VPB compensatory
pause) followed by a short RR cycle,
generally due to another VPB
ACCELERATEDIDIOVENTRICULAR RHYTHM
-
7/27/2019 ACLS Arrhythmias & Defibrillation
100/143
IDIOVENTRICULAR RHYTHM
a repetitive ventricular rhythm occurring at a ratebetween 60 and 100 beats per minute
it may be the result of an accelerated ventricular
focus which generates an impulse faster than the
sinus node and therefore assumes control
if the idioventricular rhythm represents an escape
rhythm (generally the result of third degree AV
nodal block), the P waves are dissociated from the
QRS impulses and the atrial rate is faster than the
ventricular rate.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
101/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
102/143
VENTRICULAR FIBRILLATION complete absence of properly formed QRS complexes and
no obvious P waves
no uniform activation of the ventricular myocardium and
therefore no distinct ventricular complexes
coarse fibrillatory waves when the fibrillation is recent in
onset (eg, only a few minutes)
high amplitude oscillations occurring at rate greater than
320 beats per minute which manifest random changes in
morphology, width, and height, leading to the appearanceof a completely chaotic rhythm.
fibrillatory waves become fine when VF continues for a
longer time and may not be obvious; they may resemble
asystole in these cases.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
103/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
104/143
Class IA Quinidines, Procaninamide, Disopyramide
Class IB
Mexilitine, Lignocaine
Class IC Flecanide, Propafenone
Class II
Blocker
Class III
Sotalol, amiodarone
Class IV
Diltiazam, Verapamil
Anti Arrhythmic
-
7/27/2019 ACLS Arrhythmias & Defibrillation
105/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
106/143
Heart Block
SA Block AV Block
First degree
Second degree
Third degree
Bundle Branch Block
LBBB
RBBB
Fascicular Block
Anterior
Posterior
-
7/27/2019 ACLS Arrhythmias & Defibrillation
107/143
Atrioventricular block
FIRST DEGREE ATRIOVENTRICULARBLOCK
SECOND DEGREEATRIOVENTRICULAR BLOCK
Mobitz type I (Wenckebach)
Mobitz type II
THIRD DEGREE ATRIOVENTRICULARBLOCK
FIRST DEGREE
-
7/27/2019 ACLS Arrhythmias & Defibrillation
108/143
FIRST DEGREE
ATRIOVENTRICULAR BLOCK defined as a prolonged PR interval(>0.20
seconds)
most often occurs when there is a prolongation or
delay in impulse conduction through the AV node
(show ECG 1).
The PR interval generally varies with the heart
rate; in the presence of sinus bradycardia (usually the result
of enhanced vagal tone), the PR interval lengthens.
the PR interval becomes shorter during sinus
tachycardia.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
109/143
SECOND DEGREE
-
7/27/2019 ACLS Arrhythmias & Defibrillation
110/143
SECOND DEGREE
ATRIOVENTRICULAR BLOCK Mobitz type I (Wenckebach) or Mobitz type II.
Mobitz type I
Wenckebach second degree AV block
result of an intermittent block of the impulse within the
AV node, with subsequent failure to conduct an atrialimpulse from the atria to the ventricles.
SECOND DEGREE
-
7/27/2019 ACLS Arrhythmias & Defibrillation
111/143
SECOND DEGREE
ATRIOVENTRICULAR BLOCK The ECG correlates of these electrical eventsinclude the following (show ECG 2):
There is a progressive lengthening of the PR interval
unti l a normally occurr ing P wave is not followed by
a QRS complexbecause of failure of the node to
conduct the impulse to the ventricle.
The completely blocked P wave is on time; the
surrounding RR interval is prolonged. The impulse that arrives at the node following the
completely blocked beat is conducted normally again
because the node has had time to become totally
repolarized.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
112/143
SECOND DEGREE
-
7/27/2019 ACLS Arrhythmias & Defibrillation
113/143
SECOND DEGREE
ATRIOVENTRICULAR BLOCK Mobitz type IIusually indicative of underlying structural
disease involving the AV node that is
characterized by episodic and unpredictablefailure of the node to conduct the impulse fromthe atria to the ventricles.
The block occurs below the AV node in some
cases, within the bundle of His, or within bothbundle branches.
SECOND DEGREE
-
7/27/2019 ACLS Arrhythmias & Defibrillation
114/143
SECOND DEGREE
ATRIOVENTRICULAR BLOCKIn contrast to Mobitz type I, there is no changein the PR intervalprior to or after the non-conducted P wave (show ECG 3).
There may be more than one successive non-conducted P wave, resulting in several P wavesin a row without QRS complexes.
An escape ventricular focus may generate a
QRS complex in some cases after a variableduration
-
7/27/2019 ACLS Arrhythmias & Defibrillation
115/143
THIRD DEGREE
-
7/27/2019 ACLS Arrhythmias & Defibrillation
116/143
THIRD DEGREE
ATRIOVENTRICULAR BLOCK occurs when there is complete failure of the AVnode to conduct any impulses from the atria to theventricles.
Causes: intrinsic AV nodal disease.
Drugs that depress and block nodal conduction such asdigoxin, beta blockers, or calcium channel blockers
Enhanced vagal tone, such as that occurring duringsleep
Infrequently it is congenital.
result of infranodal block occurring within the bundleof His or in both bundle
THIRD DEGREE
-
7/27/2019 ACLS Arrhythmias & Defibrillation
117/143
THIRD DEGREE
ATRIOVENTRICULAR BLOCK The P waves are completely dissociatedfrom the QRS complexes on the ECG (showECG 4).
Thus, the PR intervals are irregularlyvariable.
The atrial and ventricular rates are both
stable; the former is faster than the latter.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
118/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
119/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
120/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
121/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
122/143
-
7/27/2019 ACLS Arrhythmias & Defibrillation
123/143
ECG l i
-
7/27/2019 ACLS Arrhythmias & Defibrillation
124/143
ECG analysis
Rate
Rhythm
AxisInterval & Morphology
P, PR, QRS duration & Amplitude, Q, ST, T, QT,
Ischaemia, infarction
ECG l i
-
7/27/2019 ACLS Arrhythmias & Defibrillation
125/143
ECG analysis
Three simple questions:
(1) Is there a normal looking QRS complex ?
(2) Is there a P wave ?(3) What is the relationship between the P
wave and QRS complexes ?
I th P ?
-
7/27/2019 ACLS Arrhythmias & Defibrillation
126/143
Is there a P wave ?
If the QRS complexes are normal proceed
to examine P wave
If P wave is normal, consider sinus rhythmand its variants
If P wave is absent or abnormal, consider
supraventricular tachycardia.
-
7/27/2019 ACLS Arrhythmias & Defibrillation
127/143
P l l El t i l A ti it
-
7/27/2019 ACLS Arrhythmias & Defibrillation
128/143
Pulseless Electrical Activity
Electrical Mechanical Dissociation
Any rhythm or electrical activity that fails
to generate a palpable pulse The one major action is to search for
reversible cause while non-specific
interventions is administered
-
7/27/2019 ACLS Arrhythmias & Defibrillation
129/143
D fib ill ti
-
7/27/2019 ACLS Arrhythmias & Defibrillation
130/143
Defibrillation
Therapeutic use of electric current delivered
in large amounts over very brief periods of
time The defibrillation shock temporarily
STUNS an irregularly beating heart and
thus allows normal electrical activity to
occur (more coordinated contractile activity
to resume)
R ti l f l d fib ill ti
-
7/27/2019 ACLS Arrhythmias & Defibrillation
131/143
Rationale for early defibrillation
The most frequent initial rhythm in suddencardiac arrest is VF
The only effective treatment for VF iselectrical defibrillation
The probability of successful defibrillationdiminishes rapidly over time
VF tends to convert to asystole within a fewminutes
-
7/27/2019 ACLS Arrhythmias & Defibrillation
132/143
Cardio ersion
-
7/27/2019 ACLS Arrhythmias & Defibrillation
133/143
Cardioversion
Cardioversion is the delivery of energy
that is synchronized to the QRS
complex, while defibrillation isnonsynchronized delivery of energy, ie,
the shock is delivered randomly during
the cardiac cycle.
Cardioversion
-
7/27/2019 ACLS Arrhythmias & Defibrillation
134/143
Cardioversion
terminates arrhythmia by the delivery of asynchronized shock that depolarizes thetissue involved in a reentrant circuit and make
the tissue refractory (the circuit is no longerable to propagate or sustain reentry).
terminates those arrhythmias resulting from asingle reentrant circuit (as atrial flutter,
atrioventricular nodal reentrant tachycardia,atrioventricular reentrant tachycardia ormonomorphic ventricular tachycardia.)
FACTORS AFFECTING
DEFIBRILLATION AND
-
7/27/2019 ACLS Arrhythmias & Defibrillation
135/143
DEFIBRILLATION AND
CARDIOVERSION SUCCESSElectrodes The placement of defibrillation electrodes on
the thorax, while determining the
transthoracic current pathway for externaldefibrillation, may have only a minimal effecton the myocardial distribution of the 4 to 5percent of energy that actually reaches the
heart There are two conventional positions:
Anterolateral orientation
Anteroposterior orientation
Several studies have suggested that less
-
7/27/2019 ACLS Arrhythmias & Defibrillation
136/143
Several studies have suggested that lessenergy is required and the success rate is
higher with the anteroposterior electrodeposition in patients cardioverted for atrialfibrillation
In some patients one, but not the other position,
may be effective; thus, it has been suggestedthat if initial shocks are unsuccessful interminating the arrhythmia, the electrodesshould be relocated and cardioversion repeated
FACTORS AFFECTING
DEFIBRILLATION AND
-
7/27/2019 ACLS Arrhythmias & Defibrillation
137/143
DEFIBRILLATION AND
CARDIOVERSION SUCCESS Electrode pad size is an importantdeterminant of transthoracic current flowduring external countershock
A larger pad or paddle surface is associatedwith a decrease in resistance and increase incurrent
However, there appears to be an optimal
electrode size (approximately 12.8 cm); anincrease in electrode area beyond this sizecauses a decline in current density
Transthoracic impedance
-
7/27/2019 ACLS Arrhythmias & Defibrillation
138/143
Transthoracic impedance
During transthoracic defibrillation, a
considerably larger current must be
delivered to the thorax to compensate
for transthoracic impedance.
Impedance results in the dissipation of
energy due to shunting to the lungs, the
thoracic cage, and other elements of the
chest.
Transthoracic impedance
-
7/27/2019 ACLS Arrhythmias & Defibrillation
139/143
Transthoracic impedance
Transthoracic impedance is determined bymultiple factors including: Energy level
Electrode size
Electrode-to-skin interface
Interelectrode distance
Electrode pressure
Phase of ventilation
Thoracic impedance
Myocardial tissue and blood conductive properties
Transthoracic impedance
-
7/27/2019 ACLS Arrhythmias & Defibrillation
140/143
Transthoracic impedance
To reduce impedance, the operator should
always apply electrode gel or specifically
made paste/ gelled pad
Asystole
-
7/27/2019 ACLS Arrhythmias & Defibrillation
141/143
Asystole
No evidence to support the use of
defibrillation in asystole
Empiric shocks of asystole can inhibit therecovery of natural pacemakers in the heart
and completely eliminate any chance of
recovery
Ventricular Asystole
-
7/27/2019 ACLS Arrhythmias & Defibrillation
142/143
(Cardiac Standstill)
Total absence of ventricular electricalactivity and subsequently no ventricularcontraction.
May occur as primary event or follow VF orpulseless electrical activity
Can occur also in patients with compete
heart block without escape pacemaker Must always differentiate it from fine VF
(different management)
What is the relationship between the
P d QRS l ?
-
7/27/2019 ACLS Arrhythmias & Defibrillation
143/143
P wave and QRS complexes ?
In the normal ECG every QRS complexes is
preceded by a P wave
The interval between P and QRS is less than0.21 second
Consider heart block when the above
relationship is disturbed.