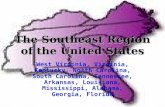
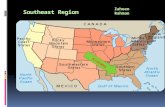
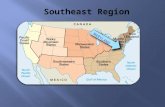
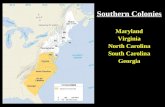
The Southern Colonies Virginia Maryland North Carolina South Carolina Georgia.
West Virginia North Carolina Pennsylvania Virginia West Virginia North Carolina Pennsylvania...
-
Upload
regina-anthony -
Category
Documents
-
view
221 -
download
3
Transcript of West Virginia North Carolina Pennsylvania Virginia West Virginia North Carolina Pennsylvania...

West Virginia North Carolina Pennsylvania Virginia
www.spilmanlaw.com
West Virginia North Carolina Pennsylvania Virginia
www.spilmanlaw.com
HR Wellness
King F. Tower, Spilman Thomas & Battle

Large Employers are only required to provide health insurance to full-time employees if they have 50 full-time employee equivalents.
But...
ACA changes the definition of full-time employees:
30 hours per week, not 40.
Employer Mandate

What is a Full-time Equivalent?
1)Calculate total hours of service for all non-full-time employees (but not more than 120 hours of service for any one employee).2)Divide total by 120.3)Add this number to the number of full-time employees.4)If this is 50 or more, the ACA pay or play mandate applies to you.
Employer Mandate

“I run a holding company that owns more than one company. I get to count each company separately, right?”
No. You have to consider whether there is a control group, which will be a single entity for ACA purposes.
Employer Mandate

Control Groups
Companies that are part of the same control group generally must be combined for the purpose of determining whether they collectively employ 50 or more full-time or full-time equivalent employees under the ACA. Where the combined total of full-time or full-time equivalent employees in a controlled group is at least 50, each individual employer is subject to the employer mandate, even if each individual employer itself does not employ enough employees to meet the threshold.
Employer Mandate

There generally are three types of controlled groups:
Parent/subsidiary
Where one or more businesses are connected through stock ownership with a common parent.
• 80% of the stock of each corporation (except the parent) is owned by one or more corporations in the group;
• Parent owns at least 80% of at least one other corporation
Control Groups

Brother/sister
Where two or more corporations with five or fewer common owners own a controlling interest of each group and have “effective control.”
• A common owner must be an individual, trust or estate.• Controlling interest means 80% or more of the stock of each
business.• Effective control means more than 50% of the stock of each
business, but only to the extent that the stock ownership is identical with each corporation.
Control Groups

Combined
Three or more organizations that:
• Each organization is member of one of the two prior types• At least corporation is the common parent and is also a
member of the brother/sister group.
Control Groups

Control Groups
Penalties will apply separately to each member organization of a control group. •For example, if one member organization fails to provide minimum coverage to all its full-time employees, the penalty would be based on the number of full-time employees in that particular organization, not the total number of employees in the entire control group. The “not counting the first 30 rule” that applies where the employer offers no coverage would apply proportionality to each member entity. So, a member entity that accounts for 50% of the total full-time employees in the control group would pay a penalty of $2000 per year times the number of full-time employees in that specific entity not counting the first 15 (50% of 30).
Employer Mandate

Ongoing Employees
Look back at standard measurement period and calculate average hours worked.
If 30 or more, employee is full-time for the next stability period. (If employee works 1560 hours, he/she is full-time.)
If under 30, employee is not full-time for the next stability period.
Employer Mandate

New Employees
If expected to work full-time, must offer coverage in 90 days.
If expected to work variable hours (reasonably expected to average fewer than 30 hours), may use initial measurement period and administrative period to determine status.
No obligation to provide coverage in this period.
But, entire time cannot extend beyond the last day of the first calendar month beginning after employee’s one-year anniversary.
Employer Mandate

Variable-Hour Employees
If 30 hours or more, must treat as full-time for the next stability period.
If under 30, may treat as not full-time for the next stability period.
EXCEPT
If the employee transitions to on-going and is full-time in the next standard measurement period, employee must be treated as full-time for the next standard stability period.
Employer Mandate

Determining Full-Time StatusMeasurement period – 3 to 12 consecutive month period set by employer.
Can be any period the employer chooses, as long as it is uniform.
Stability period – Period during which determination of full-time status remains stable.Must be at least six months, but cannot be shorter than
measurement period.
Administrative period – Period of up to 90 days used to notify and enroll employees.Cannot shorten the measurement or the stability period.
Employer Mandate

Employer Shared Responsibility (Pay or Play)
For any penalty to apply, the employer must have an employee who:
a)Enrolls in an exchange plan; andb)Receives the premium tax credit (i.e. has a family income less than 400% of the FPL or approximately $95,000 in 2014).
Employer Mandate

Minimum Essential Coverage (MEC) vs. Minimum Value (MV)Minimum Essential Coverage (MEC)
“Any” employer sponsored health planNo IRS Guidance yet
Minimum Value (MV)Employer plan must have an actuarial value of at least 60%
Based on population based actuarial assumptions, not plan design or covered benefits under a particular plan
IRS/HHS minimum value Calculatorhttp://cciio.cms.gov/resources/regulations
Employer determination of plan’s Minimum ValueUse MV calculatorHire an actuary for plans that do not “fit”Use MV benchmark plans as a guide
Plan Value Requirements

Employer Shared Responsibility
Penalty Scenario #1: Large employers who do not offer coverage to all* full-time employees:
Monthly penalties for every full-time employee beyond the first 30 employees. The penalty is assessed per month, at one-twelfth of $2000. The penalty amount will be adjusted annually to reflect growth in premium costs.
*95% = all.
Employer Mandate

Employer Shared Responsibility
Penalty Scenario #2: Large employers who offer coverage
If a large employer offers coverage, but it is “unaffordable” (employee cost exceeds 9.5% of household income or it doesn’t provide actuarial value of at least 60%) and at least 1 employee receives a subsidy on the Exchange, employer will pay a monthly assessment.
Employer Mandate

Employer Shared Responsibility
Penalty amount in Scenario #2 is the lesser of
a)The penalty for being uninsured (Scenario #1), orb)A monthly assessment based on a yearly fee of $3000 for each employee who declines the employer’s coverage and buys through the exchange.
Employer Mandate

Rule = Employee premium is 9.5% of household income.
Safe Harbor #1 = Employee premium is 9.5% of W-2 income.
Safe Harbor #2 = Employee premium is 9.5% of hourly wage for 130 hours.
Safe Harbor #3 = Employee premium is 9.5% of Federal Poverty Limit.
What is affordable?

Summary of Benefits and Coverage
Employers must give these to employees on first day of first open enrollment that begins on or after September 23, 2012. It must describe the benefits and coverage rules for each benefit that is offered.
What is required of employers?

Summary of Benefits and Coverage
Cannot exceed four double-sided pagesAt least 12-point fontCulturally and linguistically appropriateEmployer must make best effort to describe plan termsTemplate available at
www.dol.gov/ebsa/pdf/SBCtemplate.pdf
What (else) is required of employers?

Notice to Employees
Employers must give written notice to employees describing the Exchange, including a description of the services, and the manner in which the employee may contact the Exchange to request assistance.
Applies to all employers covered by the FLSA.
Employers must provide notice to each current employee by October 1, 2013 and for each new employee at the time of hiring beginning October 1, 2013.
What (else) is required of employers?

Notice to Employees (During employment)
Notice must be written so that it will be understood by the average employee and must cover:
The existence of the new Marketplace;The contact information and description of services provided by a Marketplace;That the employee may be eligible for premium tax credit if the employee purchases a qualified health plan through the Marketplace; andThat the employee may lose the employer contribution, if any, to any health plans offered by the employer.
Model Notice is available at: http://www.dol.gov/ebsa/healthreform/.
What (else) is required of employers?

Reporting Requirements
W-2 reporting of total value of employer-sponsored health coverage (health, dental, eye).
Self-Insured: COBRA premiumFully insured: Actual premium paid
Employers that file fewer than 250 W-2s for 2011 are not subject to the 2012 reporting requirements.
Exemptions from W-2 reporting – Multiemployer plans, salary reduction contributions under Health Flexible Spending Accounts, and stand-alone dental and vision benefits.
What (else) is required of employers?

Other employer reporting – in 2014, large employers will file a tax return providing the following information as to coverage offered:
The length of any waiting period;Months coverage was available;Premiums for the lowest-cost option;The employer’s share of covered expenses; andThe number and identifying information of full-time employees
What (else) is required of employers?

Health Flexible Spending Accounts – Employee contributions limited to $2500 for plan years beginning on 1/1/13Medicare Hospitalization Insurance Tax – the employee’s portion of this tax will be increased on wages in excess of $200,000 for plan years beginning on 1/1/2013 (no change to employer’s portion of tax).
What (else) is required of employers?

In 2014, employers may increase the reward or penalty on employees related to health-related standards (tobacco use, weight loss, etc.) under wellness programs.
Wellness Programs

Two Types:1. Participatory programs: Programs that provide
the same benefit as long as you participate.Reimbursing for costs of membership in a fitness centerRewarding employees for attending health seminars
2. Health-contingent programs: Programs that require an individual to meet a certain health standard to qualify.
Altering premiums based on tobacco useRewarding employees for meeting certain biometric standards
Wellness Programs

Health-Contingent Programs
Must meet five conditions:
1.Must be eligible to qualify at least yearly.2.Cannot be too large.3.Must have uniform availability and reasonable alternative standards.4.Must be reasonably designed to promote health.5.Must provide notice of alternative methods of qualifying.
Wellness Programs

In 2014, affordability determined by assuming each employee satisfies wellness program requirements
Starting in 2015, affordability determined by assuming that each employee fails wellness program requirements except that employers may look at premiums for non-tobacco users.
How do wellness programs impact affordability?

West Virginia North Carolina Pennsylvania Virginia
www.spilmanlaw.com
West Virginia North Carolina Pennsylvania Virginia
www.spilmanlaw.com
Federal Law Side-Effects
King F. Tower, Spilman Thomas & Battle

Break Time for Nursing Mothers
FLSA now requires employers to provide a “reasonable break time” for an employee to express breast milk
Up to 1 year after birthEmployer must offer a private place, other
than bathroomDo not have to compensate for timeEmployers with 50+ employees – smaller
employers not required if can establish undue hardship
Employers and the ACA

Notice to Employees (COBRA)
Employers must provide notify employees who are eligible for COBRA coverage that they may want to consider and compare health coverage alternatives to COBRA continuation coverage that are available in the Marketplace
Model Election Notice is available at: http://www.dol.gov/ebsa/cobra/.
What (else) is required of employers?

Automatic Enrollment
Employers with more than 200 full-time employees that offer employees enrollment in one or more health benefit plans are going to be required to automatically enroll new full-time employees in one of the offered plans and must continue enrollment of current employees in a health benefits plan.
But in a set of frequently asked questions issued December 22, 2010, the DOL deferred enforcement until the issuance of regulations.
According to the FAQs, “the Department of Labor has concluded that its automatic enrollment guidance will not be ready to take effect by 2014.” Therefore, employers are not required to comply with FLSA section 18A until after 2014.
Employers and the ACA

RetaliationAn employer may not discriminate against any employee because the employee has:
received a premium tax credit or health care subsidy, provided information about a violation of this new law, testifies, participates or assists in a proceeding about such violation or objected to, or refused to participate in, any activity, policy, practice, or assigned
task that the employee reasonably believed to be in violation of the ACA.
Enforced by a complaint brought under 15 U.S.C. § 2087(b) (Whistleblower Provisions of the Consumer Product Safety Act).
Employee must file complaint within 180 days after violation with Secretary of Labor. Available relief is order for employer to take affirmative action to abate the violation, reinstatement with back pay and benefits, and compensatory damages, costs and expenses.
Employers and the ACA

Discrimination
Plans cannot discriminate in favor of highly compensated individualsEnforcement delayed
Requirement will be similar to current Section 105(h)Benefits need not be identical between categories but must meet
certain testsHighly compensated employees are top 25%Excludes some employees (part-time, union). PenaltiesSelf-funded = excess benefits provided to highly compensated
individuals is treated as taxable income.Fully-insured = $100 per day per individuals discriminated against.
Employers and the ACA

Mini-Health plans
What about preventative only, or mini-health plansThey don’t meet minimum value standards
Recipients could still qualify for subsidized coverage in the exchange
IRS has not yet said if they would meet minimum essential coverage.
May protect employers from penalty for not offering any insurance (or may not depending on what the IRS says).
Employers and the ACA

West Virginia North Carolina Pennsylvania Virginia
www.spilmanlaw.com
West Virginia North Carolina Pennsylvania Virginia
www.spilmanlaw.com