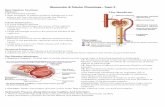
Urine Formation: Tubular Processing of the Glomerular Filtrate
description
Transcript of Urine Formation: Tubular Processing of the Glomerular Filtrate

Urine Formation: Tubular Processing of the Glomerular
Filtrate
Jethro Macallan, MD

Flow of urine pix

Urinary Excretion = Glomerular Filtration – Tubular
Reabsorption + Tubular secretion


Filtration = Glomerular filtration rate x Plasma
concentration


Tubular Reabsorption
Very large compared to urinary excretionHighly selective Completely reabsorbed: glucose and
amino acids Variable reabsorption: Na, Cl, HCO3 Poorly reabsorbed: urea and creatinine


Filtration, Reabsorption, and Excretion Rates of Different Substances by the Kidneys
Amount Filtered
Amount Reabsorbed
Amount excreted
% of Filtered Load Reabsorbed
Glucose (g/day)
180 180 0 100
Bicarbonate (mEq/day)
4,320 4,318 2 >99.9
Sodium (mEq/day)
25,560 25,410 150 99.4
Chloride (mEq/day)
19,440 19,260 180 99.1
Potassium (mEq/day)
756 664 92 87.8
Urea (g/day) 46.8 23.4 23.4 50
Creatinine (g/day)
1.8 0 1.8 0


Table 41-2 Composition of urine
Substance Concentration
Na+ 50-130 mEq/L
K+ 20-70 mEq/L
NH4+ 30-50 mEq/L
Ca++ 5-12 mEq/L
Mg++ 2-18 mEq/L
Cl- 50-130 mEq/L
Pi 20-40 mEq/L
Urea 200-400 mM

Creatinine 6-20 mM
pH 5.0-7.0
Osmolality 500-800 mOsm/kg H2O
Glucose 0
Amino acids 0
Protein 0
Blood 0
Ketones 0
Leukocytes 0
Bilirubin 0

Tubular Reabsorption
Involves both active and passive mechanisms
Transcellular route Paracellular route Ultrafiltration (bulk flow)




Tubular Reabsorption
Active Transport Against an electrochemical gradient Requires ATP 2 types:
1. Primary
2. Secondary


Tubular Reabsorption
Osmosis Water diffusion from a region of low solute
concentration to a region of high solute concentration


Primary Active Transport
Can move solutes against an electrochemical gradient
Energy comes from the hydrolysis of ATP Includes the following:
1. Na-K ATPase
2. Hydrogen ATPase
3. H-K ATPase
4. Ca ATPase


Primary Active Transport
Na-K ATPase Transports Na ions into the interstitium Maintains: 1) low intracellular Na and 2)
high intracellular K End result: -70mV inside the cell

Primary Active Transport
Na- K ATPase Involves 3 steps:
1. Na diffuses across the apical membrane into the cell membrane
2. Na is transported by the Na-K ATPase pump
3. Na, water and other substances are reabsorbed to the peritubular capillaries by ultrafiltration

Na- K pump pix

Secondary Active Transport
2 or more substances interact with a carrier molecule and are transported together across the membrane
Does not require energy directly from ATP and from high energy phosphate sources
Can either be co-transport and counter-transport



Glucose and amino acid co-transport

Na-H countertransport

Secondary Active Transport
Pinocytosis Reabsorbs large molecules eg. Proteins Requires energy


Secondary Active Transport
Transport maximum Limit to transport of solute (reabsorption
and/or secretion) Saturation of specific transport systems Tubular load exceeds the capacity of the
carrier proteins Can be increased by hormones, eg.
aldosterone

Secondary Active Transport
Glucose Transport System Found in the proximal tubule All filtered glucose is reabsorbed Transport maximum: 375mg/min – all
nephrons have reached their maximal capacity to reabsorb glucose
Filtered load of glucose: 125mg/min

Secondary Active Transport
Threshold for glucose Appearance of glucose in the urine Occurs before the transport maximum is
reached Reason: not all nephrons have the same
transport maximum for glucose


Transport Maximum of Substances Actively Reabsorbed
Substance Transport Maximum
Glucose 375mg/minPhosphate 0.10 mM/minSulfate 0.06 mM/min
Amino acids 1.50 mM/min
Urate 15 mg/min
Lactate 75 mg/minPlasma protein 30 mg/min

Transport Maximum of Substances Actively Secreted
Substance Transport Maximum
Creatinine 16 mg/min
PAH 80mg/min

Actively Transported but No Transport Maximums
Substances that are passively reabsorbed do NOT demonstrate a transport maximum
Gradient-Time Transport Also seen in some actively transported
substances, eg. Na reabsorption Determined by:1. Electrochemical gradient for diffusion2. Permeability of the membrane for the
substance3. Time a substance takes inside the fluid

Water Reabsorption
Occurs through osmosisOsmotic flow of water occurs through the
tight junctionsSeen in the proximal tubule – high
permeability for water and most ions

Water Reabsorption
Solvent Drag Solutes carried when water moves across
the tight junctions by osmosis Changes in Na reabsorption influence
reabsorption of water and solutes

Water Reabsorption
Proximal Tubule – highLoop of Henle – lowLast part of the tubules – high or low


Passive Diffusion of Cl, urea and other solutes
Cl ion diffusion Caused by electric potentials brought
about by Na Na goes out leaving the inside negatively
charged compared to the interstitial fluid Diffuses through the paracellular pathway Can be reabsorbed by secondary active
transport, eg. Na-Cl co-transport

Na+ reabsorption
H2O reabsorption
Lumen negative potential
Luminal Cl- concentration
Luminal urea concentration
Passive Cl- reabsorption
Passive urea reabsorption

Passive Diffusion of Cl, urea and other solutes
Urea Passively reabsorbed from the tubule Increases as water is reabsorbed from the
tubules Urea transporters- In the inner medullary collecting duct- ½ that is filtered is reabsorbed

Passive Diffusion of Cl, urea and other solutes
Creatinine Larger than urea All that is filtered is excreted in the urine


10 minute break

Reabsorption and Secretion Along the Different Parts of
the Nephron



Proximal Tubule
Reabsorbs about 65% of the filtered load of Na and water
Highly metabolic and have large numbers of mitochondria
Extensive brush border on the luminal side Rapid Na reabsorption Loaded with protein carrier molecules- Co-transport: glucose and amino acids- Counter-transport: hydrogen ions

Proximal Tubule
Na-K ATPase pump Major force for the reabsorption of NaCl
and water 1st half of the tubule: co-transport with aa,
glucose 2nd half of the tubule: co-transport with Cl

Proximal Tubule
Solute concentration along the Proximal tubule
[Na] remains constant Glucose, amino acids and HCO3 are
avidly reabsorbed [creatinine] increases

Proximal Tubule
Secretion of Organic acids and bases eg. Bile salts, oxalate, urate,
cathecholamines Secretion + filtration + no reabsorption =
rapid excretion Penicillin and salicylates: rapidly excreted
by the kidneys PAH: rapidly excreted
- Used to estimate renal plasma flow

Loop of Henle
Divided into 3 segments:
1. Thin descending segment
2. Thin ascending segment No brush borders Few mitochondria Minimal levels of metabolic activity
3. Thick ascending segment

Loop of Henle
Descending Segment Highly permeable to water Moderately permeable to most solutes~Na
and urea Function: simple diffusion through its walls Reabsorbs almost 20% of the filtered
water Does not reabsorb Ca, Mg, HCO3

Loop of Henle
Ascending Limb Both thin and thick Impermeable to water – important in
concentrating the urine Na-K 2Cl co-transport- Mediates movement of Na across the
luminal membrane


Loop of Henle
Thick Ascending Limb High metabolic activity Active reabsorption of Na, Cl and K ~25% Also reabsorbs Ca, Mg and HCO3 Na-K ATPase pump- Low intracellular [Na] Site of action of loop diuretics (furosemide,
ethacrynic acid, bumetanide)


Loop of Henle
Thick Ascending Limb Na-H counter-transport- Mediates Na reabsorption- Secretes hydrogen ions Impermeable to water


Early Distal Tubule
Forms part of the juxtaglomerular complex – provides feedback control of GFR and blood flow
Reabsorbs Na (5%), K and Cl Impermeable to water and urea Na-Cl co-transport Moves Na and Cl from the lumen into the cell Na-K ATPase Pumps Na out of the cell across the basolateral
membrane Site of action of thiazide diuretics


Late Distal Tubule and Cortical Collecting tubule
Composed of 2 distinct cell types:
1. Principal Cells Reabsorb Na and water from the lumen Secrete K ions to the lumen
2. Intercalated Cells Reabsorb K ions Secrete hydrogen ions into the lumen


Late Distal Tubule and Cortical Collecting tubule
Principal Cells Depends on the activity of the Na-K
ATPase pump Na reabsorption and K secretion Primary sites of K sparing diuretics
1. Aldosterone antagonists: spironolactone, eplerenone
2. Na channel blockers: amiloride, triamterene

Late Distal Tubule and Cortical Collecting tubule
Intercalated Cells Mediated by a hydrogen ATPase
mechanism Secrete hydrogen ions and reabsorbs K Plays a key role in acid base regulation of
body fluids


Late Distal Tubule and Cortical Collecting tubule
Functional characteristics:
1. Completely impermeable to urea
2. Reabsorb Na ions – controlled by aldosterone
3. Intercalated cells – acid-base regulation
4. ADH/ vasopressin – controls permeability to water

Medullary Collecting Duct
Absorbs <10% of filtered Na and waterFinal site of processing of urine Important role in final urine output of water
and solutesEpithelial cells are cuboidal in shapeRelatively few mitochondria

Medullary Collecting Duct
Special characteristics:
1. Permeability is controlled by ADH
2. Permeable to urea
3. Secretes hydrogen ions – role in acid-base balance

Medullary Collecting Duct
> 1.0 : more water is reabsorbed than solute; net secretion of the solute into the tubular fluid
< 1.0 : more solute has been reabsorbed than water
1.0 : concentration of the substance in the tubular fluid is the same as the concentration in plasma

Measurement of Water Reabsorption
Inulin Used to measure GFR Not secreted or reaborbed Changes in inulin reflect changes in the
amount of water in the tubular fluid



10 minute break

Regulation of Tubular Reabsorption


Glomerulotubular Balance
Most basic mechanism for controlling tubular reabsorption
Intrinsic ability of the tubules to increase their rate of reabsorption in response increased tubular load
Occurs independent of hormones

Glomerulotubular Balance
Total rate of reabsorption increases as the filtered load increases
Helps prevent the overloading of the distal tubular segments when GFR increases
Second line of defense: buffers spontaneous changes in GFR on urine output (first line: autoregulatory mechanisms~ tubuloglomerular feedback)

review autoregulation

Peritubular Capillary and Renal Interstitial Fluid Physical Forces
Normal rate of peritubular capillary reabsorption: 124 ml/min
Reabsorption = Kf x Net reabsorptive forces

Peritubular Capillary and Renal Interstitial Fluid Physical Forces
Starling Hypothesis Qf = k[ (Pc + πi) – (Pi + πp)]where:- Qf: fluid movement- k: filtration constant- Pc: capillary hydrostatic pressure- Pi: interstitial fluid hydrostatic pressure- πp: plasma oncotic pressure- πi: interstitial fluid oncotic pressure

Peritubular Capillary and Renal Interstitial Fluid Physical Forces
Net reabsorptive forces Peritubular hydrostatic pressure (Pc):
opposes reabsorption ~ 13mmHg Interstitial fluid hydrostatic pressure (Pif):
favors reabsorption ~ 6mmHg

Peritubular Capillary and Renal Interstitial Fluid Physical Forces
Net reabsorptive forces Peritubular colloid oncotic pressure (πc):
favors reabsorption ~ 32mmHg Interstitial fluid colloid oncotic pressure
(πif): opposes reabsorption ~ 15mmHg

Peritubular Capillary and Renal Interstitial Fluid Physical Forces
Hydrostatic pressure: Pc - Pif
13mmHg – 6 mmHg = 7mmHg: opposes reabsorption
Oncotic pressure: πc - πif
32mmHg – 15 mmHg = 17mmHg: favors reabsorption

Peritubular Capillary and Renal Interstitial Fluid Physical Forces
Net reabsorptive forces Net hydrostatic forces - Net oncotic forces 7mmHg – 17 mmHg = 10mmHg Favors net reabsorption

Peritubular Capillary and Renal Interstitial Fluid Physical Forces
Filtration Coefficient (Kf) Contributes to the high rate of fluid
reabsorption Review:
Reabsorption = Kf x Net reabsorptive forces
Normal Kf = 12.4 ml/min/mmHg

Peritubular Capillary and Renal Interstitial Fluid Physical Forces
Regulation of Peritubular Capillary Physical Forces
determined by Pc and πc
Pc - influenced by:
1. Arterial pressure- Increases cause an increase in Pc and a
decrease in reabsorption
2. Resistances of the afferent and efferent arterioles
- Increase in resistance causes an decrease in Pc and an increase in reabsorption


Peritubular Capillary and Renal Interstitial Fluid Physical Forces
Regulation of Peritubular Capillary Physical Forces
πc - is determined by: 1. Systemic plasma colloid oncotic pressure- Directly correlated to an increase in
[plasma protein] : reabsorption2. Filtration Fraction (GFR/ renal plasma
flow)- Directly correlated to reabsorption rate Kf is directly correlated to peritubular
capillary reabsorption rate

Factors That Can Influence Peritubular Capillary Reabsorption
↑PC →↓Reabsorption ↓RA →↑PC
↓RE →↑Ra
↑Arterial Pressure→↑PC
↑πC →↑Reabsorption ↑πA →↑πC
↑FF →↑πC
↑Kf →↑Reabsorption

Peritubular Capillary and Renal Interstitial Fluid Physical Forces
Renal Interstitial and Colloid Oncotic Pressures
Peritubular capillary reabsorption is directly correlated with tubular reabsorption of water and solutes

Effect of Arterial Pressure
Increased arterial pressure causes: Much larger increases in GFR A decrease in the filtered load of Na and
water that is reabsorbed in the tubules

Hormonal Control
AldosteroneAngiotensin IIADHANPParathyroid Hormone

Hormonal Control
Aldosterone Secreted by the zona glomerulosa of the
adrenal cortex Acts on the principal cells of the cortical
collecting tubule Stimulates Na reabsorption and K
secretion More important regulator of K than Na Addison’s disease – decreased
aldosterone Conn’s syndrome – increased aldosterone


Hormonal Control
Angiotensin II Most powerful Na retaining hormone Increases during times of: low BP,
hemorrhage and loss of water and Na Effects:1. Stimulates aldosterone secretion2. Constricts afferent arterioles3. Directly stimulates Na reabsorption


Hormonal Control
ADH Key role in the degree of
dilution/concentration of the urine Increases water permeability of the distal
tubule, collecting tubule and collecting duct
Binds to V2 receptors Stimulates AQP-2: form water channels
and permit rapid diffusion of water


Hormonal Control
ANP Secreted by cells of the cardiac atria Responds to plasma volume expansion Acts on the collecting duct Inhibits reabsorption of Na and water Increases urine excretion

Hormonal Control
Parathyroid Hormone Important in Ca regulation Increases tubular reabsorption of Ca Inhibits phosphate reabsorption Stimulates Mg reabsorption

Hormones That Regulate Tubular Reabsorption
Hormone Site of Action Effects
Aldosterone Collecting tubule and duct
↑ NaCl, H2O reabsorption, ↑K+
secretion
Angiotensin II Proximal tubule, thick ascending loop of Henle/distal tubule, collecting tubule
↑ NaCl, H2O reabsorption, ↑H+ secretion
Antidiuretic hormone
Distal tubule/ collecting tubule and duct
↑ H2O reabsorption
Atrial natriuretic peptide
Distal tubule/ collecting tubule and duct
↓ NaCl reabsorption
Parathyroid hormone
Proximal tubule, thick ascending loop of Hental/distal tubule
↓ PO4--- reabsorption,
↑ Ca- reabsorption

Sympathetic Nervous System
Constricts the renal arteriolesDecreases Na and water excretionReduces GFR Increases Na reabsorption Increases renin release and Angiotensin II
formation



10 minute break

Clearance Methods to Quantify Renal Function

Inulin
Polyssacharide molecule with MW = 5200Not produced in the bodyRequires IV infusionFreely filteredNot reabsorbed or secretedUsed to determine GFR ~ radioactive
iothalamate and creatinine

Inulin
Generalizations:
1. Filtered and not reabsorbed or secreted – clearance rate of a substance equals that of inulin
2. Reabsorbed - clearance rate of a substance is less than that of inulin
3. Secreted - clearance rate of a substance is greater than that of inulin

Creatinine
By-product of muscle metabolismCleared almost entirely by glomerular
filtrationCa also be used to assess GFRErrors: A small amount is secreted by the tubules:
excreted creatinine exceeds amount filtered
Error in measurin plasma creatinine: overestimate of plasma cratinine


Creatinine
Changes in GFR = [plasma creatinine]: inversely proportional to GFR
Creatinine excretion rate equals its production
Excretion = GFR x Pcreatinine

Table 40-1 Major hormones that influence GFR and RBF
Stimulus Effect on GFR Effect on RBF
Vasoconstrictors
Sympathetic nerves
↓ ECV ↓ ↓
Angiotensin II ↓ ECV, renin ↓ ↓
Endothelin Shear stress, angiotensin II, bradykinin, epinephrine
↓ ↓
Vasodilators
Prostaglandins (PGI2, PGE2)
↓ ECV, shear stress, angiotensin II
NC ↑
Nitric oxide Shear stress, acetylcholine, histamine, bradykinin, adenosine triphosphate
↑ ↑
Bradykinin Prostaglandin, ↓ angiotensin converting enzyme
↑ ↑

Renal Plasma Flow
Clearance rate of a substance that is completely cleared of plasma
No known substance that is completely cleared by kidneys
Para-aminohippuric acid 90% cleared from the plasma ~ extraction
ratio of PAH


Filtration Fraction
= GFR/ RPF= inulin clearance/ PAH clearance= 125/ 650= 0.19

Use of Clearance to Quantify Kidney Function
Term Equation Units
Clearance rate (Cs) ml/min
Glomerular filtration rate (GFR)
Clearance ratio None
Effective renal plasma flow (ERPF)
ml/min

Renal plasma flow (RPF)
ml/min
Renal blood flow (RBF) ml/min
Excretion rate Excretion rate = Us x V mg/min, mmol/min, or mEq/min
Reabsorption rate Reabsorption rate = Filtered load – Excretion rate = (GFR x Ps) – (Us x V)
mg/min, mmol/min, or mEq/min
Secretion rate Secretion rate = Excretion rate – Filtered load mg/min, mmol/min, or mEq/min

Substance Clearance rate (ml/min)
Glucose 0
Sodium 0.9
Chloride 1.3
Potassium 12.0
Phosphate 25.0
Inulin 125.0
Creatinine 140.0

Summary

Table 41-3 NaCl transport along the nephron
Segment Percentage filtered reabsorbed
Mechanism of Na+ entry across the apical membrane
Major regulatory hormones
Proximal tubule 67% Na+-H+exchange, Na+-cotransport with amino acids and organic solutes, Na+/H+-Cl-/anion exchange
Angiotensin II
Norepinephrine
Epinephrine
Dopamine
Paracellular
Loop of Henle 25% 1 Na+-1K+-2Cl- symport
Aldosterone
Distal tubule ~4% NaCl symport Aldosterone
Late distal tubule and collecting duct
~3% Na+ channels Aldosterone
Atrial natriuretic peptide
Urodilatin

Table 41-4 Water transport along the nephron
Segment Percentage of filtered load reabsorbed
Mechanism of water
reabsorption
Hormones that regulate
water permeability
Proximal tubule 67% Passive None
Loop of Henle 15% DTL only; passive
None
Distal tubule 0% No water reabsorption
None
Late distal tubule and collecting duct
~8%-17% Passive ADH, ANP


Hormones That Regulate Tubular Reabsorption
Hormone Site of Action Effects
Aldosterone Collecting tubule and duct
↑ NaCl, H2O reabsorption, ↑K+
secretion
Angiotensin II Proximal tubule, thick ascending loop of Henle/distal tubule, collecting tubule
↑ NaCl, H2O reabsorption, ↑H+ secretion
Antidiuretic hormone
Distal tubule/ collecting tubule and duct
↑ H2O reabsorption
Atrial natriuretic peptide
Distal tubule/ collecting tubule and duct
↓ NaCl reabsorption
Parathyroid hormone
Proximal tubule, thick ascending loop of Hental/distal tubule
↓ PO4--- reabsorption,
↑ Ca- reabsorption


Thank You!!!