Urinary elimination Dr. Dergham M. Hameed. Urinary System Kidneys and ureters Bladder Urethra.
Urinary System. Introduction Consists of Consists of 1. Two kidneys 2. Two ureters 3. One urinary...
-
Upload
mervin-ramsey -
Category
Documents
-
view
224 -
download
3
Transcript of Urinary System. Introduction Consists of Consists of 1. Two kidneys 2. Two ureters 3. One urinary...

Urinary SystemUrinary System

IntroductionIntroduction
Consists of Consists of
1.1. Two kidneysTwo kidneys
2.2. Two uretersTwo ureters
3.3. One urinary bladderOne urinary bladder
4.4. One urethraOne urethra


IntroductionIntroduction
Urine is excreted from each kidney Urine is excreted from each kidney through its ureter and is stored in the through its ureter and is stored in the urinary bladderurinary bladder


IntroductionIntroduction
Urine is expelled from the body Urine is expelled from the body through the urethrathrough the urethra


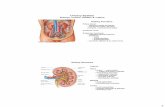
Anatomy of KidneysAnatomy of Kidneys
Retroperitoneal organsRetroperitoneal organs

External Anatomy of KidneysExternal Anatomy of Kidneys
Hilus – A vertical fissure near the Hilus – A vertical fissure near the center of the concave medial bordercenter of the concave medial border

External Anatomy of KidneysExternal Anatomy of Kidneys
Ureters leave and blood vessels, Ureters leave and blood vessels, lymphatic vessels, and nerves enter lymphatic vessels, and nerves enter and exit at the hilusand exit at the hilus


Internal Anatomy of KidneysInternal Anatomy of Kidneys
Consists of Consists of 1.1. CortexCortex2.2. MedullaMedulla3.3. PyramidsPyramids4.4. PapillaePapillae5.5. ColumnsColumns6.6. Minor and Major calycesMinor and Major calyces7.7. Renal pelvisRenal pelvis


Internal Anatomy of KidneysInternal Anatomy of Kidneys
Nephron – functional unit of the Nephron – functional unit of the kidneykidney


Blood and Nerve Supply of the Blood and Nerve Supply of the KidneysKidneys
Blood enters the kidney through the Blood enters the kidney through the renal arteryrenal artery


Blood and Nerve Supply of the Blood and Nerve Supply of the KidneysKidneys
Blood exits via the renal veinBlood exits via the renal vein


NephronsNephrons
Consists of Consists of
1.1. Renal corpuscleRenal corpuscle
2.2. Renal tubuleRenal tubule


Renal CorpuscleRenal Corpuscle
Where fluid is filteredWhere fluid is filtered


Renal CorpuscleRenal Corpuscle
Consists of Consists of
1.1. GlomerulusGlomerulus
2.2. Glomerular CapsuleGlomerular Capsule


Renal CorpuscleRenal Corpuscle
Glomerulus – capillary knotGlomerulus – capillary knot


Renal CorpuscleRenal Corpuscle
The glomerular capsule consists of The glomerular capsule consists of
1.1. Visceral layerVisceral layer
2.2. Parietal layerParietal layer
3.3. Capsular SpaceCapsular Space


Renal CorpuscleRenal Corpuscle
The visceral layer consists of The visceral layer consists of modified simple squamous epithelial modified simple squamous epithelial cells called cells called podocytespodocytes


Renal CorpuscleRenal Corpuscle
The parietal layer consists of simple The parietal layer consists of simple squamous epithelium and forms the squamous epithelium and forms the outer wall of the capsuleouter wall of the capsule


Renal CorpuscleRenal Corpuscle
Fluid filtered from the glomerular Fluid filtered from the glomerular capillaries enters the capillaries enters the capsular spacecapsular space


Renal CorpuscleRenal Corpuscle
Capsular space – the space between Capsular space – the space between the two layers of the glomerular the two layers of the glomerular capsulecapsule


Renal TubuleRenal Tubule
Filtered fluid passes through hereFiltered fluid passes through here


NephronNephron
Renal tubuleRenal tubule
1.1. Proximal convoluted tubuleProximal convoluted tubule
2.2. Loop of HenleLoop of Henle
3.3. Distal convoluted tubuleDistal convoluted tubule


NephronNephron
Distal convoluted tubules of several Distal convoluted tubules of several nephrons drain into to a single nephrons drain into to a single collecting ductcollecting duct


NephronNephron
Many collecting ducts drain into a Many collecting ducts drain into a small number of papillary ductssmall number of papillary ducts


NephronNephron
These empty urine into the minor These empty urine into the minor calycescalyces


NephronNephron
Loop of henle consists of Loop of henle consists of
1.1. Descending limbDescending limb
2.2. Thin ascending limbThin ascending limb
3.3. Thick ascending limbThick ascending limb


NephronNephron
Two types of nephronsTwo types of nephrons
1.1. Cortical nephronCortical nephron
2.2. Juxtamedullary nephronJuxtamedullary nephron

Cortical NephronCortical Nephron
Has its glomerulus in the outer Has its glomerulus in the outer portion of the cortex portion of the cortex

Cortical NephronCortical Nephron
And a short loop of Henle that And a short loop of Henle that penetrates only into the outer region penetrates only into the outer region of the medullaof the medulla

Juxtamedullary NephronJuxtamedullary Nephron
Has its glomerulus deep in the cortex Has its glomerulus deep in the cortex close to the medullaclose to the medulla

Juxtamedullary NephronJuxtamedullary Nephron
Its long loop of Henle stretches Its long loop of Henle stretches through the medulla and almost through the medulla and almost reaches the papillareaches the papilla

Renal Tubule and Collecting DuctRenal Tubule and Collecting Duct
Most of the cells of the distal Most of the cells of the distal convoluted tubule have receptors for convoluted tubule have receptors for ADH and aldosteroneADH and aldosterone

Juxtaglomerular Apparatus (JGA)Juxtaglomerular Apparatus (JGA)
Helps regulate blood pressure and Helps regulate blood pressure and the rate of blood filtration by the the rate of blood filtration by the kidneyskidneys

Juxtaglomerular Apparatus (JGA)Juxtaglomerular Apparatus (JGA)
Consists of Consists of
1.1. Juxtaglomerular cellsJuxtaglomerular cells
2.2. Macula DensaMacula Densa


Juxtaglomerular CellsJuxtaglomerular Cells
Located on an afferent arterioleLocated on an afferent arteriole




Macula DensaMacula Densa
Located on the distal convoluted Located on the distal convoluted abutting the JG cellsabutting the JG cells



Renal PhysiologyRenal Physiology
Nephrons and collecting ducts Nephrons and collecting ducts perform three basic processes while perform three basic processes while producing urineproducing urine

Renal PhysiologyRenal Physiology
1.1. Glomerular filtrationGlomerular filtration
2.2. Tubular secretionTubular secretion
3.3. Tubular reabsorption Tubular reabsorption


Glomerular FiltrationGlomerular Filtration
Glomerular filtrate - the fluid that Glomerular filtrate - the fluid that enters the capsular space enters the capsular space


Glomerular FiltrationGlomerular Filtration
The principle of filtration – to force The principle of filtration – to force fluids and solutes through a fluids and solutes through a membrane by pressuremembrane by pressure

Glomerular FiltrationGlomerular Filtration
Glomerular Filtration rate (GFR) – the Glomerular Filtration rate (GFR) – the amount of filtrate formed by both amount of filtrate formed by both kidney per minutekidney per minute

Glomerular FiltrationGlomerular Filtration
GFR – 125ml/minuteGFR – 125ml/minute

Glomerular FiltrationGlomerular Filtration
This amounts of 180 liters of filtrate This amounts of 180 liters of filtrate per dayper day

Glomerular FiltrationGlomerular Filtration
Because of further processing we Because of further processing we only excrete 1-2 liters of urine per only excrete 1-2 liters of urine per dayday

Glomerular FiltrationGlomerular Filtration
Only call it urine after it drips out of Only call it urine after it drips out of the collecting ducts into the calyceal the collecting ducts into the calyceal systemsystem

Neural AutoregulationNeural Autoregulation
Through the ANSThrough the ANS

Neural AutoregulationNeural Autoregulation
During extreme emergencies such as During extreme emergencies such as shock, sympathetics to afferent shock, sympathetics to afferent arterioles cause them to constrictarterioles cause them to constrict

Neural RegulationNeural Regulation
Blood flow into glomerular capillaries Blood flow into glomerular capillaries is greatly decreased and GFR dropsis greatly decreased and GFR drops

Neural RegulationNeural Regulation
Lowering of renal blood flow has two Lowering of renal blood flow has two consequencesconsequences

Neural RegulationNeural Regulation
1. Reduces urine output, which 1. Reduces urine output, which conserves blood volumeconserves blood volume

Neural RegulationNeural Regulation
2. It permits greater blood flow to 2. It permits greater blood flow to other body tissuesother body tissues

Neural RegulationNeural Regulation
Severe hypotension can cause death Severe hypotension can cause death of part of the tubules, decreases of part of the tubules, decreases urine output, and kidney failureurine output, and kidney failure

Hormonal RegulationHormonal Regulation
With mild drops of BP sympathetics With mild drops of BP sympathetics stimulate renin secretion on JG cell stimulate renin secretion on JG cell by targeting B1 receptorsby targeting B1 receptors

Hormonal RegulationHormonal Regulation
Renin converts angiotensinogen to Renin converts angiotensinogen to angiotensin Iangiotensin I

Hormonal RegulationHormonal Regulation
Angiotensin I is converted by Angiotensin I is converted by angiotensin converting enzyme to angiotensin converting enzyme to angiotensin IIangiotensin II

Hormonal RegulationHormonal Regulation
Angiotensin II causes efferent Angiotensin II causes efferent arteriole to constrict more than arteriole to constrict more than afferent arterioles, maintaining afferent arterioles, maintaining filtrationfiltration

Hormonal RegulationHormonal Regulation
Angiotensin II also leads to the Angiotensin II also leads to the formation of aldosteroneformation of aldosterone

Hormonal RegulationHormonal Regulation
Aldosterone causes sodium and Aldosterone causes sodium and water retention and potassium water retention and potassium excretionexcretion

Principles of Renal TransportPrinciples of Renal Transport
Reabsorption – returns most of the Reabsorption – returns most of the filtered water and many of the filtered water and many of the filtered solutes (such as glucose, filtered solutes (such as glucose, sodium, etc.) to the bloodstreamsodium, etc.) to the bloodstream


Principles of Renal TransportPrinciples of Renal Transport
Tubular secretion – the transfer of Tubular secretion – the transfer of materials from the blood and tubule materials from the blood and tubule cells into tubular fluidcells into tubular fluid


Principles of Renal TransportPrinciples of Renal Transport
Tubular secretion helps control blood Tubular secretion helps control blood pH and helps eliminate other pH and helps eliminate other substances from the bodysubstances from the body

Principles of Renal TransportPrinciples of Renal Transport
Solute reabsorption drives water Solute reabsorption drives water reabsorptionreabsorption

Reabsorption in the Proximal Reabsorption in the Proximal Convoluted TubuleConvoluted Tubule
The majority of the solute and water The majority of the solute and water reabsorption from filtered fluid reabsorption from filtered fluid occurs in the proximal convoluted occurs in the proximal convoluted tubulestubules


Reabsorption in the Proximal Reabsorption in the Proximal Convoluted TubuleConvoluted Tubule
Reabsorption of Na and other solutes Reabsorption of Na and other solutes creates an osmotic gradient that creates an osmotic gradient that promotes reabsorption of water by promotes reabsorption of water by osmosisosmosis


Reabsorption in the Proximal Reabsorption in the Proximal Convoluted TubuleConvoluted Tubule
Proximal convoluted Na transporters Proximal convoluted Na transporters promote reabsorption of organic solutes promote reabsorption of organic solutes such as such as
1.1. GlucoseGlucose2.2. Amino acidsAmino acids3.3. Bicarbonate ionsBicarbonate ions4.4. WaterWater5.5. NaNa6.6. KK7.7. ClCl8.8. Other ions and vitaminsOther ions and vitamins


Secretion of NH3 and NH4 in the Secretion of NH3 and NH4 in the Proximal Convoluted TubuleProximal Convoluted Tubule
The deamination of the amino acid The deamination of the amino acid glutamine by PCT cells generates glutamine by PCT cells generates NH3 and new HCO3-NH3 and new HCO3-

Secretion of NH3 and NH4 in the Secretion of NH3 and NH4 in the Proximal Convoluted TubuleProximal Convoluted Tubule
Most NH3 quickly binds to H+ and Most NH3 quickly binds to H+ and becomes NH4+becomes NH4+

Secretion of NH3 and NH4 in the Secretion of NH3 and NH4 in the Proximal Convoluted TubuleProximal Convoluted Tubule
NH4+ can substitute H+ aboard the NH4+ can substitute H+ aboard the Na+/H+ antiporters and be secreted Na+/H+ antiporters and be secreted into tubular fluidinto tubular fluid


Reabsorption in the Loop of HenleReabsorption in the Loop of Henle
Water reabsorption is not directly Water reabsorption is not directly coupled with sodium reabsorptioncoupled with sodium reabsorption


Reabsorption in the Loop of HenleReabsorption in the Loop of Henle
In the descending limb, water is In the descending limb, water is reabsorbed via osmosisreabsorbed via osmosis

Reabsorption in the Loop of HenleReabsorption in the Loop of Henle
As water is reabsorbed from the As water is reabsorbed from the descending limb, the osmolality of descending limb, the osmolality of the filtrate increasesthe filtrate increases


Reabsorption in the Loop of HenleReabsorption in the Loop of Henle
In the ascending limb, Na+, K+, Cl- In the ascending limb, Na+, K+, Cl- symporters reclaim Na+, Cl-, and K+ symporters reclaim Na+, Cl-, and K+ ions from the tubular lumen fluid.ions from the tubular lumen fluid.



Reabsorption in the Loop of HenleReabsorption in the Loop of Henle
As sodium and chloride are As sodium and chloride are reabsorbed from the ascending limb, reabsorbed from the ascending limb, the osmolality of the filtrate the osmolality of the filtrate decreasesdecreases


Reabsorption in the DCTReabsorption in the DCT
As fluid flows along the DCT, As fluid flows along the DCT, reabsorption of Na+ and Cl- reabsorption of Na+ and Cl- continues due to Na+ - Cl- continues due to Na+ - Cl- symporterssymporters


Reabsorption in the DCTReabsorption in the DCT
The DCT serves as the major site The DCT serves as the major site where parathyroid hormone where parathyroid hormone stimulates reabsorption of Ca2+ and stimulates reabsorption of Ca2+ and excretion of phosphateexcretion of phosphate

Reabsorption and Secretion in the Reabsorption and Secretion in the Collecting DuctCollecting Duct
Aldosterone increases Na+ and Aldosterone increases Na+ and water reabsorption as well as K+ water reabsorption as well as K+ secretion by the collecting ducts and secretion by the collecting ducts and late distal convoluted tubuleslate distal convoluted tubules



Reabsorption and Secretion in the Reabsorption and Secretion in the Collecting DuctCollecting Duct
Some cells secrete H+ into the Some cells secrete H+ into the filtrate and reabsorb HCO3- into the filtrate and reabsorb HCO3- into the bloodstreambloodstream

Reabsorption and Secretion in the Reabsorption and Secretion in the Collecting DuctCollecting Duct
These cells help maintain body fluid These cells help maintain body fluid pH by excreting excess H+ when the pH by excreting excess H+ when the pH is too low or by reabsorbing less pH is too low or by reabsorbing less HCO3- when the pH is too high.HCO3- when the pH is too high.

Reabsorption and Secretion in the Reabsorption and Secretion in the Collecting DuctCollecting Duct
ADH regulates water reabsorption by ADH regulates water reabsorption by increasing permeability in the increasing permeability in the Collecting Duct and DCTCollecting Duct and DCT

Production of Dilute and Production of Dilute and Concentrated UrineConcentrated Urine
The rate at which water is lost from The rate at which water is lost from the body depends mainly on ADH the body depends mainly on ADH

Production of Dilute and Production of Dilute and Concentrated UrineConcentrated Urine
When ADH level is very low, the When ADH level is very low, the kidneys produce dilute urine and kidneys produce dilute urine and excrete excess water excrete excess water

Production of Dilute and Production of Dilute and Concentrated UrineConcentrated Urine
When ADH level is high, the kidneys When ADH level is high, the kidneys secrete concentrated urine and secrete concentrated urine and conserve waterconserve water

UretersUreters
Each of the two ureters connects the Each of the two ureters connects the renal pelvis of one kidney to the renal pelvis of one kidney to the urinary bladderurinary bladder

Urinary BladderUrinary Bladder
Located in the pelvic cavity posterior Located in the pelvic cavity posterior to the pubic symphysisto the pubic symphysis


Urinary BladderUrinary Bladder
In the floor of the urinary bladder is a In the floor of the urinary bladder is a small, smooth triangular area, the small, smooth triangular area, the trigone.trigone.

Urinary BladderUrinary Bladder
The ureters enter the urinary bladder The ureters enter the urinary bladder near two posterior points in the near two posterior points in the triangletriangle


Urinary BladderUrinary Bladder
The urethra drains the urinary The urethra drains the urinary bladder from the anterior point of the bladder from the anterior point of the triangletriangle


Urinary BladderUrinary Bladder
In the area around the opening to the In the area around the opening to the urethra, the circular fibers of the urethra, the circular fibers of the muscularis form the internal urethral muscularis form the internal urethral sphinctersphincter

Urinary BladderUrinary Bladder
The internal urethral sphincter The internal urethral sphincter contracts in response to contracts in response to sympathetics, and relaxes in sympathetics, and relaxes in response to parasympathetic response to parasympathetic stimulationstimulation

Urinary BladderUrinary Bladder
Below the internal sphincter is the Below the internal sphincter is the external urethral sphincter, which is external urethral sphincter, which is composed of skeletal musclecomposed of skeletal muscle

UrethraUrethra
A tube leading from the floor of the A tube leading from the floor of the urinary bladder to the exteriorurinary bladder to the exterior

UrethraUrethra
Functions to discharge urine from the Functions to discharge urine from the bodybody

UrethraUrethra
The male urethra also serves as the The male urethra also serves as the duct for ejaculation of semenduct for ejaculation of semen

IncontinenceIncontinence
A lack of voluntary control over A lack of voluntary control over urinationurination

RetentionRetention
Failure to void urine completely or Failure to void urine completely or normallynormally