Underweight and Malnutrition
-
Upload
jack-sinaga -
Category
Documents
-
view
216 -
download
0
Transcript of Underweight and Malnutrition
-
7/30/2019 Underweight and Malnutrition
1/61
by
Thaddee Katembo, BSND,MPH, DrPHApril, 2012
Underweight and
Malnutrition
-
7/30/2019 Underweight and Malnutrition
2/61
Introduction Obesity is no more only a health problem in adult
people, but currentdatarevealthatchildrenarenotsaved.
WHO specifies that at least 20 million children underthe age of 5 years were overweight globally in2005(WHO, 2006).
In parallel to the development in adults, theprevalence of overweight children and adolescentsis also increasing worldwide, illustrating thatchildren and adolescents are part of the worldwide
epidemic of obesity. (McArdle, Katch&Katch,2007) In many countries, about 15 to 35% of the children
and adolescents are now classified as beingoverweight and about 5% are classified obese.
-
7/30/2019 Underweight and Malnutrition
3/61
A Double Burden
In developing countries, obesity coexists with
undernutrition, with prevalence rates higher in urbanthan in rural population. (McArdle, Katch and Katch,2007).
This double burden of malnutrition refers to the dual
burden of under- and overnutrition occurringsimultaneously within a population in the developingcountries (FAO, 2006).
According to WHO, globally, it is estimated that thereare nearly 20 million children who are severely andacutely malnourished.
Most of them live in South Asia and in Sub-Saharan
Africa.
-
7/30/2019 Underweight and Malnutrition
4/61
Mortality
Estimates suggest that about 1 million
children die every year from severe acute
malnutrition(WHO, 2007)
Malnutrition is directly responsible for
300,000 deaths per year in children younger
than 5 years in developing countries and
contributes indirectly to over half the deathsin childhood worldwide (Shashidhar et al.,
2011)
-
7/30/2019 Underweight and Malnutrition
5/61
Vulnerable People and Regions
Women and young
children are the most
adversely affected groups;
one quarter to one half of
women of child-bearingage in Sub-Saharan Africa
and South Asia are
underweight, whichcontributes to the
number of low birth
weight infants born
annually.
-
7/30/2019 Underweight and Malnutrition
6/61
Double Burden
WHO specifies that at least 20 million children
under the age of 5 years were overweight
globally in 2005(WHO, 2006).
Public health professionals should address
both undernutrition and overnutrition health
problems.
-
7/30/2019 Underweight and Malnutrition
7/61
Inpatient Health Problem
Malnutrition is globally the most important risk
factor for illness and death, contributing to more
than half of deaths in children worldwide; child
malnutrition was associated with 54% of deaths
in children in developing countries in 2001.[1, 2]
Protein-energy malnutrition (PEM), has been
described with increasing frequency inhospitalized and chronically ill children in the
United States.[3]
-
7/30/2019 Underweight and Malnutrition
8/61
Currently
More than halfof young children in South Asia have
PEM, which is 6.5 times the prevalence in the western
hemisphere.
In sub-Saharan Africa, 30% of children have PEM.
Despite marked improvements globally in theprevalence of malnutrition, rates of undernutrition and
stunting have continued to rise in Africa, where rates of
undernutrition and stunting have risen from 24% to
26.8% and 47.3% to 48%, respectively, since 1990, with
the worst increases occurring in the eastern region of
Africa.
-
7/30/2019 Underweight and Malnutrition
9/61
By 2015
The World Health Organization estimates that the
prevalence of malnutrition will have decreased to 17.6%
globally, with 113.4 million children younger than 5
years affected as measured by low weight for age.
The overwhelming majority of these children, 112.8million, will live in developing countries with 70% of
these children in Asia, particularly the south central
region, and 26% in Africa.
An additional 165 million (29.0%) children will have
stunted length/height secondary to poor nutrition.
-
7/30/2019 Underweight and Malnutrition
10/61
Thats why
This presentation will focus on strategies ofweight management for underweight childrenin terms of prevention and treatment
Many presentations have been focused onoverweight and obesity, ignoring the
malnutrition as an important public healthissue related undernutrition and infectiousdisease
-
7/30/2019 Underweight and Malnutrition
11/61
1.Definitions of cases
Child. The United Nations Convention on the
Rights of the Child defines a child as "a human
being below the age of 18 years. In thispresentation, the focus is on the under-five years
old who are at high risk.
Underweight. From age 2 to 20 years , it refers to aBMI that is less than the 5th percentile.
-
7/30/2019 Underweight and Malnutrition
12/61
Concepts
Underweight. For children aged 059 months,
using the standard of NCHS/WHO, moderate
underweight is the index weight/age below
- 2SD from median weight for age and severe
underweight is the index weight/age below
-3SD from median weight for age of theNCHS/WHO reference population.
-
7/30/2019 Underweight and Malnutrition
13/61
Malnutrition
The World Health Organization defines
malnutrition as "the cellular imbalance
between supply of nutrients and energy and
the body's demand for them to ensuregrowth, maintenance, and specific functions.
-
7/30/2019 Underweight and Malnutrition
14/61
2. Factors of Underweight among children
1. Low birth-weight(
-
7/30/2019 Underweight and Malnutrition
15/61
Factors
The effects of changing environmental
conditions in increasing malnutrition is
multifactorial. Poor environmental conditions
may increase insect and protozoal infectionsand also contribute to environmental
deficiencies in micronutrients.
-
7/30/2019 Underweight and Malnutrition
16/61
Factors
Overpopulation, more commonly seen in
developing countries, can reduce food
production, leading to inadequate food intake
or intake of foods of poor nutritional quality.Conversely, the effects of malnutrition on
individuals can create and maintain poverty,
which can further hamper economic andsocial development.
-
7/30/2019 Underweight and Malnutrition
17/61
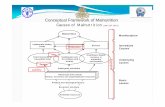
Causal Framework as Developed by
UNICEF (1998)
This conceptual framework on the causes of
malnutrition was developed in 1990 as part
of the UNICEF Nutrition Strategy. The framework shows that causes
ofmalnutrition are multisectoral, embracing
food, health and caring practices.
-
7/30/2019 Underweight and Malnutrition
18/61
UNICEF conceptual framework
They are also classified as immediate (individual level),
underlying (household or family level) and basic(societal level)
The immediate causes are inadequate dietary intake
and infectious disease;
The underlying causes are household food insecurity,
inadequate maternal and child care and inadequate
health services and health environment;
The basic causes include formal and non-formalinstitutions, political and ideological superstructure,
economic structure and potential resources.
-
7/30/2019 Underweight and Malnutrition
19/61
Conceptual Framework
Although more refined versions of this
framework have since been developed, (e.g.,
adding female educationjust below the
underlying causes and distinguishing human,economic and organizational resources),
-
7/30/2019 Underweight and Malnutrition
20/61
-
7/30/2019 Underweight and Malnutrition
21/61
3. Typology
Kwashiorkor and marasmus are 2
forms of PEM that have been
described. The distinction between
the 2 forms of PEM is based on the
presence of edema (kwashiorkor) orabsence of edema with
emaciation(marasmus).
Edema is significant in kwashiorkorbut can also be present in marasmus
or in the frequently encountered
mixedforms of PEM.
-
7/30/2019 Underweight and Malnutrition
22/61
Acute Malnutrition and Wasting
Acute malnutrition (defined as the
presence of bi-pedal edema or
weight for height
-
7/30/2019 Underweight and Malnutrition
23/61
Stunting as Chronic Malnutrition
Stunting, or low height for
age, is caused by long-term
insufficient nutrient intake
and frequent infections.Stunting generally occurs
before age two, and effects
are largely irreversible.
Malnutrition and Stunting in
Guatemala
-
7/30/2019 Underweight and Malnutrition
24/61
Origin of the concept Kwashiorkor
Following brief descriptions by Procter (1926) in
Kenya and Lieurade (1932) in the Cameroons,
Jamaican pediatrician Dr Cecily Williams (1933,
1935), working at Accra in the Gold Coast, first
adequately described the syndrome.
She noted the disease only among children and
she considered that it was a new clinical entity.
She suggested the term kwashiorkor, because
the Ga tribe around Accra called it thus: (kwashi
=the name of a boy born on Sunday - orkor
=red, that is a Red boy).
-
7/30/2019 Underweight and Malnutrition
25/61
4.Pathophysiology of Underweight
and Malnutrition
Although significant clinical differences
between kwashiorkor and marasmus are
noted, some studies suggest that marasmus
represents an adaptation to starvationwhereas kwashiorkor represents a
dysadaptation to starvation.
The presence of edema caused by poornutrition defines kwashiorkor.
-
7/30/2019 Underweight and Malnutrition
26/61
Proteins or Energy?
Kwashiorkor was thought to be primarily
caused by insufficient protein consumption
but with sufficient calorie intake,
distinguishing it from marasmus.
But know, it is believed that the fundamental
problem is related to both insufficient energy
and proteins, leading to the imbalanced use of
calories from the three energy-yieldingmacronutrients
That is why the name PEM (Protein-Energy
Malnutrition)
-
7/30/2019 Underweight and Malnutrition
27/61
From PEM to Pluricarential syndrome
More recently, micronutrient and antioxidant
deficiencies have come to be recognized as
contributory of malnutrition, thus the name of
Pluricarential syndrome
-
7/30/2019 Underweight and Malnutrition
28/61
Several structural and functional
side effects
Malnutrition affects virtually every organ
system. Dietary protein is needed to provide
amino acids for synthesis of body proteins and
other compounds that have various functionalroles. Energy is essential for all biochemical
and physiologic functions in the body.
Furthermore, micronutrients are essential inmany metabolic functions in the body as
components and cofactors in enzymatic
processes.
Digestive functions
-
7/30/2019 Underweight and Malnutrition
29/61
Digestive functions
Atrophy of the mucosa from the mouth to
intestine (small and colon)
Deficiency of enzyme secretion
Liver: hepatomegaly (enlargement of the liver)
due to fat accumulation (steatosis or fatty
degeneration )
Pancreas athrophy ( which may be related to
malnutrition diabetes)
-
7/30/2019 Underweight and Malnutrition
30/61
Immunity functions
Immune response changes occur early in the
course of significant malnutrition in a child. These
immune response changes correlate with poor
outcomes and mimic the changes observed in
children with acquired immune deficiencysyndrome (AIDS).
Loss of delayed hypersensitivity, fewer T
lymphocytes, impaired lymphocyte response,impaired phagocytosis secondary to decreased
complement and certain cytokines, and decreased
secretory immunoglobulin A (IgA)
-
7/30/2019 Underweight and Malnutrition
31/61
Immune functions
These immune changes predispose children to
severe and chronic infections, most
commonly, infectious diarrhea, which further
compromises nutrition causing anorexia,decreased nutrient absorption, increased
metabolic needs, and direct nutrient losses.
-
7/30/2019 Underweight and Malnutrition
32/61
-
7/30/2019 Underweight and Malnutrition
33/61
Cerebral and Mental functions
Changes in the developing brain, including, a
slowed rate of growth of the brain, lower
brain weight, thinner cerebral cortex,
decreased number of neurons, insufficientmyelinization, etc. These changes are similar
to those described in patients with mental
retardation of different causes
http://emedicine.medscape.com/article/289117-overviewhttp://emedicine.medscape.com/article/289117-overviewhttp://emedicine.medscape.com/article/289117-overviewhttp://emedicine.medscape.com/article/289117-overview -
7/30/2019 Underweight and Malnutrition
34/61
Why?
Edema? Due to the oncotic pressure, or
colloid osmotic pressure, a form of osmotic
pressure exerted by proteins in blood plasma
that usually tends to pull water into thecirculatory system
Depigmentation ? Lack of melanin, protein in
the skin and keratin, a protein of hairs
Diarrhea? Malabsorption syndrome due the
digestive mucosa atrophy
-
7/30/2019 Underweight and Malnutrition
35/61
Other Affected Functions
Renal functions
Cardiac functions
Pulmonary functions
Skeletomuscular functions
-
7/30/2019 Underweight and Malnutrition
36/61
5. Management of Malnutrition
a. Assessment of Nutritional Status
Table 1: Weight Status Categories for the Calculated BMI-for-
age PercentileWeight Status Category Percentile Range of BMIUnderweight Less than the 5th percentile (
-
7/30/2019 Underweight and Malnutrition
37/61
T bl 2 W i h f H i h I d i Z
-
7/30/2019 Underweight and Malnutrition
38/61
Table 2: Weight for Height Index in Z-scores
(Children aged 0-59 months)
Z-scores of the median Nutritional status
-
7/30/2019 Underweight and Malnutrition
39/61
The Mid-Upper Arm Circumference (MUAC)
In children aged 659 months
Green: >135mm (normal)
Yellow: 125-134mm (risk of
malnutrition)
Orange: 110-124mm(moderate malnutrition)
Red:
-
7/30/2019 Underweight and Malnutrition
40/61
The Kwashiorkor: Child presents oedema
-
7/30/2019 Underweight and Malnutrition
41/61
b. Dietary Assessment
Childs and familys eating habits should be
performed to identify food preferences and eating
patterns through an interview with the child or
teenager as well as the parent, and with food
records and a food frequency check list. The same process should be followed, in case of
undernutrition to identify the different factors
related to the child and/or to the family for asustainable intervention.
-
7/30/2019 Underweight and Malnutrition
42/61
c. Environmental Assessment
Factors to be assessed are such as family composition,
family income,
family schedules,
childcare arrangements,
food availability,
school environments,
community environments, etc. (Copperman &Jacobson, 2004)
d P h i l A t B h i
-
7/30/2019 Underweight and Malnutrition
43/61
d. Psychosocial Assessment or Behavior
Modification
An assessment of the childs/ adolescents and
parents readiness to make lifestyle changes
is an important measure of whether the
weight management program will besuccessful.
-
7/30/2019 Underweight and Malnutrition
44/61
Primordial and Primary Prevention of
Malnutrition
Primordial prevention is defined as prevention
of risk factors themselves, beginning with
change in social and environmental conditions
in which these factors are observed todevelop, and continuing for high risk
Primary prevention is the prevention of the
occurrence of the disease given the existingrisk factors
a- Breastfeeding Promotion
-
7/30/2019 Underweight and Malnutrition
45/61
a Breastfeeding Promotion
Promote breastfeeding(exclusive upto 6 months and with complementaryfood up to 2 years)
Adequate transition from exclusive
breastfeeding to family foods, referred to ascomplementary feeding, from 6 to 18-24months of age ( whole grains flour )
Adequate weaning The Baby-Friendly Hospital Initiative (BFHI) is
a global program sponsored by the WorldHealth Organization (WHO) and the UnitedNations Childrens Fund (UNICEF) toencourage and recognize hospitals andbirthing centers that offer an optimal level ofcare for infant feeding.
Mother Friendly Workplace
-
7/30/2019 Underweight and Malnutrition
46/61
Mother-Friendly Workplace
A workplace providing private lactation
designated areas for mothers to express and
store breast milk
A workplace offering flexible breaks for mothers
expressing milk throughout the work day
A workplace providing access to a lactation
consultant for mothers expressing milk at work
A workplace having a written policy supporting
breastfeeding women
-
7/30/2019 Underweight and Malnutrition
47/61
B-Medical checkups for preschool children
To prevent and detect certain diseases
Prevent malnutrition
Surveillance of diseases of children.
Screening of infections
-
7/30/2019 Underweight and Malnutrition
48/61
C-Prevention and control of infants
diseases
Expanded Program on Immunization (EPI)
Prevention of micronutrient deficiencies
(Vitamine A, Iron,)
Diarrheal diseases
Prevention of verminosis (parasitic worms)
Prevention of ARI
-
7/30/2019 Underweight and Malnutrition
49/61
-
7/30/2019 Underweight and Malnutrition
50/61
E-Family planning
Important to increase food
availability
To improve health and
nutritional status for both
infants and mothers
-
7/30/2019 Underweight and Malnutrition
51/61
Secondary and Tertiary Prevention
Case-management : Applied for severe
malnutrition
Phase 1 - Recovering normal metabolic function and
-
7/30/2019 Underweight and Malnutrition
52/61
Phase 1 - Recovering normal metabolic function and
rehydration (Hospital level).
Patients without inadequateappetite and/or a major medicalcomplications are initiallyadmitted in the hospital for Phase1 treatment.
During this phase patients aregiven a Therapeutic milk formulacalled F-75(meaning 75kcal/100ml of solution ) and
energy intake is 100 kcal/Kg/day. ReSoMal(oral rehydration salts
solution for severely malnourishedchildren).
Infectious diseases treatment
Phase 2 - Gaining weight with the right kind of
-
7/30/2019 Underweight and Malnutrition
53/61
Phase Gaining weight with the right kind of
therapeutic food. (Community level)
Use of the Community-based
Management of Acute Malnutrition
strategy (CMAM)
The principle of treatment is the use of
the Ready-to-Use Therapeutic Food
(RUTF)
No use of milk like the formula F-100
because it needs to be prepared bytrained personnel and presents a risk of
contamination due to its high water
content.
-
7/30/2019 Underweight and Malnutrition
54/61
Background of CMAM
The Community Therapeutic Care (CTC)
approach to treating acute malnutrition
(defined as the presence of bi-pedal edema or
weight for height
-
7/30/2019 Underweight and Malnutrition
55/61
Background of CMAM
Prior to that, the standard response wasprovided through therapeutic feeding centers
(TFCs) or Nutrition Rehabilitation Units (RHUs);
in-patient facilities which treated all cases with
therapeutic milk-based formulas (F75 and F100)
administered by medical staff.
Disadvantages:
Facilities often overcrowded,
cross-infections,
lengthy stays that led to high default rates
mothers absence from her other children for extended
eriods at the TFC
-
7/30/2019 Underweight and Malnutrition
56/61
Three key innovations
Three key innovations allowed the evolution
from in-patient to community-based care:
1. The development of ready-to-use therapeutic
foods (RUTF or RUF) such as Plumpynut,
which are lipid-based and thus resistant to
contamination and which do not require
medical oversight;2. A new classification distinguishing between
severe cases with and without medical
complications; and
-
7/30/2019 Underweight and Malnutrition
57/61
Three key innovations
3. The use of simple, color-coded Mid-Upper Arm
Circumference (MUAC)
measuring tapes for diagnosisthat allow community
members to be trained to
identify acute malnutrition for
referral to treatment.
Plumpy Nut
-
7/30/2019 Underweight and Malnutrition
58/61
Plumpy Nut
Ingredients :
Plumpy Nut is composed of peanut
butter, vegetable fat, dry skimmed milk,lactoserum, maltodextrines, sugar,mineral and vitamin complex.
How to use it ?
1. Child of height >85cm: 5 sachets/day ( that is 2500 Kcal)
2. Child of height
-
7/30/2019 Underweight and Malnutrition
59/61
2 BP 100
Ingredients of BP100: It is a solid
F-100 with added iron, Wheatflour (backed)
Oat flour (backed), Vegetable oil,Sugar, Milk proteins, Skimmedmilk powder
Minerals, Milk calcium, Aminoacids, Vitamins
How to serve it?
Child of height >85cm: 9 bars /day( 2700 Kcal)
Child of height
-
7/30/2019 Underweight and Malnutrition
60/61
Correctly used
Mean weight gain is 10-
20g/Kg/day
Recovery intervenes
within 21-30 days.
-
7/30/2019 Underweight and Malnutrition
61/61
DOUBLE BURDEN