Traumatic Delivery
description
Transcript of Traumatic Delivery

1

2
Predisposing FactorsMaternal factors: Primigravida Cephalopelvic disproportion,
small maternal stature maternal pelvic anomalies
Prolonged or rapid labor Dystocia Oligohydramnios

3
Predisposing factors
Fetal factors: Abnormal presentation
Breech, face VLBW or extreme prematurity Fetal macrosomia Large fetal head Fetal anomalies

4
Predisposing Factors
Obstetrical Interventions: Use of mid-cavity forceps or vacuum
extraction Versions and extractions

5
Types of Injury
Soft tissue injuries Head and Skull Face Musculoskeletal injuries Intra-abdominal injuries Peripheral nerve injuries

6
Soft Tissue Injuries
Erythema & Abrasions- Forceps, Dystocia
Petechiae-head/neck/chest/back- Cord around neck
/breech - thrombocytopenia Ecchymoses
-breech/prematurity

7

8
Soft Tissue InjuriesLacerations
scalp, buttocks, thighs(Fetal scalp electrodes, surgeons knife!)
Infection a risk, but most heal uneventfully
Management: careful cleaning, application of antibiotic
ointment, and observation Bring edges together using Steri-Strips Lacerations occasionally require suturing

9
Soft Tissue InjuriesSubcutaneous fat Necrosis (SFN) Not usually detected at birth Irregular, hard, non-pitting, subcutaneous
plaques with overlying dusky red-purple discoloration on the extremities, face, trunk, or buttocks
May be caused by pressure during delivery Hypothermia/ischemia/asphyxia appear @ 6-10 days resolve @ 6-8 wk/atrophy Sometimes calcifies

10

11
Soft Tissue Injuries
SFN: TreatmentTreat symptomatic hypercalcemia
aggressively increased fluid intake low calcium/ vit. D diet furosemide -calcium-wasting diureticSteroids-inhibit metabolism of vit. DBiphosphonates-reduce bone resorption

12
Injuries to the HeadCaput Succedaneum most frequently observed lesion pressure on the scalp against cervix subcutaneous, extraperiosteal accumulation of
blood/serum presenting part involved overlying bruising/Petechiae crosses suture lines resolves within days

13
Injuries to the Head
Cephalhematoma 0.4%-2.5% of all live births sub-periosteal hemorrhage from rupture of blood
vessels between the skull and the periosteum buffeting of fetal head against the pelvis no extension across suture lines most commonly parietal, may occasionally be
observed over the occipital bone

14
Injuries to the Head
Cephalhematoma increases in size with time 15% bilateral
18% associated skull fracture Forceps
Vacuum

15
Injuries to the Head
Subgaleal HemorrhageDiagnosis is generally clinical: fluctuant boggy mass developing over the scalp
(especially over the occiput) develops gradually 12-72 hours after delivery hematoma spreads across the whole calvarium Usually insidious and may not be recognized for
hours swelling may obscure the fontanelle and cross
suture lines (distinguishing it from cephalhematoma)

16
Injuries to the Head
Subgaleal HemorrhageRx if signs of substantial volume loss: compression wrap restore blood volume surgical drainage 25% mortality

17

18
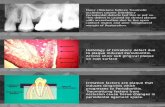
Cephalhematoma
Caput Succedaneum
Subgaleal hemorrhage with skull fracture

19
SkinEpicranial aponeuroses
Periosteum
Skull
Dura
Caput CephalhematomaSubgaleal hemorrhage
extradural hemorrhage
Lesion External swelling ↑ after birth
Crosses suture lines
↑↑↑acute blood loss
Caput succedaneum Soft, pitting No Yes No
Cephalhematoma Firm, tense Yes No No
Subgaleal hematoma Firm, fluctuant Yes Yes Yes

20
Injuries to the Head
Skull FracturesUncommon because of compressible skull & open
suturesForceps/Prolonged laborLinear/DepressedUsually asymptomaticAssociated intracranial hemorrhage may produce symptoms

21

22
Injuries to the Head
Skull Fractures
Rx – conservative - elevation of depressed fracture
- Thumb pressure- Hand pump
- Vacuum extractor Surgical elevation Healing within a few months

23
Injuries to the Head
Intracranial hemorrhage
- Subdural/Subarachnoid/IVH- Usually asymptomatic- Forceps/Vacuum- Prolonged labor- Usually associated with fracture

24
Injuries to the Head
Subarachnoid hemorrhage-more frequent than realized
-usually asymptomatic
-may cause seizures (day 2-3)
-bloody CSF
- CT/MRI

25

26
Injuries to the Head
Subdural Hematoma- may be silent for several days-head circumference- poor feeding /vomiting /lethargy- altered consciousness/seizures - DX- CT/MRI- RX- Subdural taps/surgical drainage

27

28
Injuries to the Head
Fractures of Facial bones-nasal fracture/dislocation
-deviated nasal septum
-maxillary fracture
-mandibular fracture

29
EYE INJURIES
Eye Lids
edema/ecchymoses/laceration Subconjuntival hemorrhage Orbital fracture/hemorrhage Extra Ocular Muscle injury Corneal Abrasion Intra Ocular hemorrhage

30
Injuries to the Ear
Ecchymoses Abrasion Avulsion Hematoma

31
Neck and Shoulder injuries
Fractured Clavicle-most frequently fractured bone-difficult delivery-shoulder dystocia-breech -Crepitus or deformity at the site-movement/moro on affected side-associated brachial plexus palsy

32
Neck and Shoulder injuriesFractured Clavicle
DX- X-ray
RX- conservativeimmobilizationreduce pain pain subsides in 7-10 days
good prognosis

33
Neck and Shoulder injuries
Fracture of the Humerus second most common fracture difficult delivery/traction shoulder dystocia breech
deformity

34
Neck and Shoulder injuries
Fractured Humerus: Management Splinting/immobilization in adduction Closed reduction and casting when displaced Watch for evidence of radial nerve injury Callus formation occurs, and complete
recovery expected in 2-4 weeks In 8-10 days, the callus formation is sufficient
to discontinue immobilization

35
Intra-abdominal Organ Injury
Uncommon sometimes overlooked as a cause of death in
the newborn Hemorrhage is the most serious acute
complication liver is the most commonly damaged internal
organ

36
Nerve Palsies
Facial NerveEtiology Compression Of peripheral nerve
-forceps
-prolonged labor
-in-utero compression CNS Injury
-temporal bone fracture
-tissue destruction

37
Nerve Palsies
Facial NerveClinical Manifestation Paralysis apparent day 1-2 Unilateral/bilateral Affected side smooth/drooping Amplified by crying

38
Nerve PalsiesFacial Nerve: central nerve injury asymmetric facies with crying mouth is drawn towards the normal side wrinkles are deeper on the normal side movement of the forehead and eyelid is
unaffected the paralyzed side is smooth with a swollen
appearance absent nasolabial fold on affected side corner of the mouth droops on affected side no evidence of trauma is present on the face

39
Nerve Palsies
Facial Nerve: peripheral nerve injury asymmetric facies with crying Unable to close eye on affected side may be evidence of forceps mark

40

41
Nerve Palsies
Facial Nerve Palsy: prognosis 85% recover in 1 week 90% recovery in 1 year Surgery if no resolution in 1 yr Palsy due to trauma usually resolves or
improves palsy that persists is often due to absence of
the nerve

42
Nerve Palsies
Brachial Plexus injury
Types of Injury Stretch Rupture Avulsion

43
Nerve Palsies
Brachial Plexus injury
Types of Injury Stretch- 90-100% recovery in 1 year Rupture-needs surgical repair Avulsion-needs surgical repair

44
Nerve Palsies
Brachial Plexus injury Weakness or total paralysis of muscles
innervated by the brachial plexus C-5 to C-8 and T1
Erb's Palsy C5-C7- proximal muscle weakness Klumpke’s Palsy C8 and T1- weakness in the
intrinsic muscles of the hand

45

46
Nerve Palsies
Brachial Plexus injuryNeurological FeaturesErb's Palsy (C5-C6)The involved extremity lies: in adduction in pronation and internally rotated Moro, biceps and radial reflexes are absent Grasp reflex is usually present 2-5% ipsilateral phrenic nerve paresis The "waiter's tip" posture

47

48
Nerve PalsiesBrachial Plexus InjuryNeurological Features
Klumpke’s Palsy (C7-8, T1) weakness of the intrinsic muscles of the
hand grasp reflex is absent

49
Nerve PalsiesBrachial Plexus InjuryNeurological Features
Total Plexus Palsy Erb's Palsy + absent grasp reflex Sensory loss worse than Erb's

50
Nerve Palsies
Brachial PlexusPrognosis Depends on severity and extent of
lesion 88% resolved by 4 months 92% by 12 months 93% by 48 months

51
Nerve Palsies
Brachial PlexusPrognosis Depends on severity and extent of
lesion 88% resolved by 4 months 92% by 12 months 93% by 48 months

52
Nerve PalsiesBrachial Plexus Management Prevention of contractures immobilize limb gently across the abdomen
for first week and then start passive range of motion exercises at all
joints supportive wrist splints

53
Nerve Palsies
Brachial PlexusManagement Electrotherapy-controversial Surgical exploration-if no significant
functional recovery by 3 months Exploration after 6 months is of little
benefit

54
Nerve Palsies
Laryngeal nerve injury The infant presents with a hoarse cry or
respiratory stridor most often unilateral nerve paralysis Swallowing may be affected if the superior
branch is involved Bilateral paralysis may be caused by trauma to
both laryngeal nerves or, more commonly, by a CNS injury such as hypoxia or hemorrhage involving the brain stem
Patients with bilateral paralysis often present with severe respiratory distress or asphyxia

55
Nerve PalsiesLaryngeal nerve injury
& Prognosis: Paralysis often resolves in 4-6 wk, although full
recovery may take 6-12 months
Treatment symptomatic Small frequent feeds, once infant is stable Minimize the risk of aspiration Infants with bilateral involvement may require
gavage feeding and tracheotomy

56