The cost-effectiveness of hypertension management in low … · KostovafiD etfial BMJ Global Health...
Transcript of The cost-effectiveness of hypertension management in low … · KostovafiD etfial BMJ Global Health...
-
1Kostova D, et al. BMJ Global Health 2020;5:e002213. doi:10.1136/bmjgh-2019-002213
The cost- effectiveness of hypertension management in low- income and middle- income countries: a review
Deliana Kostova ,1 Garrison Spencer,2 Andrew E Moran,3,4 Laura K Cobb,3 Muhammad Jami Husain,1 Biplab Kumar Datta,1 Kunihiro Matsushita,5 Rachel Nugent2
Original research
To cite: Kostova D, Spencer G, Moran AE, et al. The cost- effectiveness of hypertension management in low- income and middle- income countries: a review. BMJ Global Health 2020;5:e002213. doi:10.1136/bmjgh-2019-002213
Handling editor Lei Si
► Additional material is published online only. To view please visit the journal online (http:// dx. doi. org/ 10. 1136/ bmjgh- 2019- 002213).
Received 9 December 2019Revised 31 May 2020Accepted 15 June 2020
For numbered affiliations see end of article.
Correspondence toDr Deliana Kostova; Kiv0@ cdc. gov
© Author(s) (or their employer(s)) 2020. Re- use permitted under CC BY- NC. No commercial re- use. See rights and permissions. Published by BMJ.
ABSTRACTHypertension in low- income and middle- income countries (LMICs) is largely undiagnosed and uncontrolled, representing an untapped opportunity for public health improvement. Implementation of hypertension control strategies in low- resource settings depends in large part on cost considerations. However, evidence on the cost- effectiveness of hypertension interventions in LMICs is varied across geographical, clinical and evaluation contexts. We conducted a comprehensive search for published economic evaluations of hypertension treatment programmes in LMICs. The search identified 71 articles assessing a wide range of hypertension intervention designs and cost components, of which 42 studies across 15 countries reported estimates of cost- effectiveness. Although comparability of results was limited due to heterogeneity in the interventions assessed, populations studied, costs and study quality score, most interventions that reported cost per averted disability- adjusted life- year (DALY) were cost- effective, with costs per averted DALY not exceeding national income thresholds. Programme elements that may reduce cost- effectiveness included screening for hypertension at younger ages, addressing prehypertension, or treating patients at lower cardiovascular disease risk. Cost- effectiveness analysis could provide the evidence base to guide the initiation and development of hypertension programmes.
INTRODUCTIONHypertension in low- income and middle- income countries (LMICs) remains largely undiagnosed, untreated and uncontrolled despite being a leading factor in prevent-able death and disability (Chow et al, 20131; Ibrahim and Damasceno, 20122; Lozano et al, 20183; and WHO, 20134). The subop-timal treatment of hypertension in LMICs represents an untapped opportunity for public health improvement (Frieden and Bloomberg, 2018).5 Recent estimates suggest that nearly 40 million hypertension- related deaths can be avoided over the next 25 years
by scaling up hypertension treatment to 70% (Kontis et al, 2019).6
Hypertension management depends on consistent and reliable access to healthcare. Areas with documented shortages of health-care workers and with limited access to formal healthcare, such as sub- Saharan Africa, have fared the worst in addressing hypertension (Geldsetzer et al, 2019).7 At the population level, weak hypertension control and insuffi-cient cardiovascular disease (CVD) prevention in LMICs can have broad implications that exceed the direct health consequences. For example, clustering of hypertension- related
Key questions
What is already known? ► Implementation of hypertension control strategies in low- resource settings depends in large part on cost considerations, but evidence on the cost- effectiveness of hypertension interventions from low- income and middle- income countries (LMICs) is sparse and varied across geographical, clinical and evaluation contexts.
What are the new findings? ► Most interventions that reported cost per averted disability- adjusted life- year were cost- effective using national income thresholds, but gaps in evi-dence exist on programme elements that can affect cost- effectiveness in LMICs, such as task- sharing, risk- based treatment and standardised treatment protocols.
What do the new findings imply? ► Hypertension control is found to be a cost- effective intervention for many LMICs. Gaps in evidence can be filled by economic evaluation of programme ele-ments that include shifting some healthcare tasks to non- physician providers, integrating cardiovascular disease (CVD) risk assessment into treatment deci-sions and incorporating standardised CVD preven-tion programmes. on June 29, 2021 by guest. P
rotected by copyright.http://gh.bm
j.com/
BM
J Glob H
ealth: first published as 10.1136/bmjgh-2019-002213 on 9 S
eptember 2020. D
ownloaded from
http://gh.bmj.com/http://crossmark.crossref.org/dialog/?doi=10.1136/bmjgh-2019-002213&domain=pdf&date_stamp=2020-09-10http://orcid.org/0000-0003-2414-0166http://gh.bmj.com/
-
2 Kostova D, et al. BMJ Global Health 2020;5:e002213. doi:10.1136/bmjgh-2019-002213
BMJ Global Health
disease in younger adults, which is disproportionately more common in LMICs than high- income countries (Roth et al, 2018),8 has considerable socioeconomic effects, contributing to productivity and income losses at the household level and impeding macroeconomic growth (Bloom et al, 2011).9
While the value of addressing hypertension in LMICs has gained recognition over the past decade, resources in this area remain limited, revealing a gap between health targets and current needs (United Nations (UN), 201110;UN, 201511; and WHO, 2018a12). The transition from goal setting to actual implementation of hyper-tension control strategies in LMICs depends in large part on cost considerations. Although some economic modelling suggests that both population- level and clin-ical interventions for hypertension control can be cost- effective (Murray et al, 200313; Jha et al, 201214; Nugent and Brouwer, 201515; Bertram et al, 201816; and WHO, 2018b17), policymakers in individual countries might regard aggregate global estimates to be insufficient evidence for policy formulation in specific country circumstances. To inform policy decisions regarding hypertension approaches in LMICs, we reviewed the current evidence on costs and cost- effectiveness of hyper-tension interventions across LMICs. The contribution of this study is twofold. First, it provides the first comprehen-sive review of the evidence on cost- effectiveness of hyper-tension management programmes in LMICs. This review summarises the available evidence most relevant to poli-cymakers in countries where hypertension management is currently limited or absent, and where decision- makers may be considering additions to health benefit packages without detailed cost or cost- effectiveness information. Second, this review documents the variation among existing studies across study designs and study quality. It produces a standardised quality score and explores contextual differences such as those that may arise between programmes based exclusively on pharmaceu-tical intervention and programmes that incorporate non- pharmaceutical components; programmes that target hypertension populations with different levels of CVD risk; or programmes applied in countries with different income levels. This too provides informative evidence to decision- makers in LMICs. The results describe a range of clinical programmes and corresponding programme cost and cost- effectiveness estimates from different settings, with varying levels of quality. We found gaps in evidence on programme elements that can affect cost- effectiveness in LMICs, such as shifting of healthcare tasks to non- physician providers, integrating CVD risk assessment into treatment decisions and standardising CVD prevention approaches.
Patient and public involvementNo patients or human subjects were involved in the process of conducting this literature review.
METHODSIn March 2019, we searched for articles on economic evaluation of hypertension treatment programmes in LMICs using PubMed, the Cochrane Collaboration Data-base of Systematic Reviews, the Tufts Cost- Effectiveness Analysis Registry, the UK’s National Institute for Health and Care Excellence (NICE) guidelines, the Univer-sity of York Centre for Reviews and Dissemination and the Disease Control Priorities (3rd Edition). To guide the search eligibility criteria, we developed a PICOTS table summarising the inclusion and exclusion criteria across the following elements: population, intervention, comparator, outcomes, time frame, settings and study design (Liberati et al, 2009)18 (see online supplementary appendix table A1). The search was performed using Medical Subject Headings (MeSH) and search terms related to hypertension and the pharmacological treat-ment, diagnosis, screening and management of hyper-tension. The list of MeSH terms can be found in online supplementary appendix table A2. We also used search terms for world regions; all low- income, lower middle- income and upper middle- income country names; newly classified high- income countries in South America, the Caribbean and the Pacific; and economic terms related to costs and cost- effectiveness. The PubMed search strategy can be found in online supplementary appendix table A3. We performed a supplemental ad hoc literature scan without MeSH terms in May 2020 to account for the lag in indexing and to capture any recent articles. The initial search identified 60 articles for inclusion in the review while the supplemental scan identified an additional 11 relevant publications. Results were not limited by publi-cation date.
An inclusion/exclusion guide was created for reviewing the abstracts and full- text of articles (see online supple-mentary appendix table A4). Articles were included if they involved an intervention related to clinical screening, treatment and management of hypertension. Articles were excluded if they were designed for other diseases for which hypertension may be a risk factor or common comorbidity, or if they were for surgery patients to address acute events related to hypertension. Articles were excluded if they looked only at the cost of hyperten-sion, with no reference to a specific intervention; only studied the prevalence of hypertension; if they did not involve any clinical setting; or, if they studied knowledge or awareness of hypertension. Studies that were conducted in high- income countries, or in territories or associated states of high- income countries (with the exception of South America, the Caribbean and the Pacific), studies that were published in a foreign language, and any article that was an editorial, review, correspondence or abstract related to study design and protocol were also excluded.
Overall, 595 references were identified: 534 from PubMed and 61 from other databases and sources. Screening abstracts identified 163 articles for full- text review of which 71 were identified as relevant for inclu-sion in the analysis (see online supplementary appendix
on June 29, 2021 by guest. Protected by copyright.
http://gh.bmj.com
/B
MJ G
lob Health: first published as 10.1136/bm
jgh-2019-002213 on 9 Septem
ber 2020. Dow
nloaded from
https://dx.doi.org/10.1136/bmjgh-2019-002213https://dx.doi.org/10.1136/bmjgh-2019-002213https://dx.doi.org/10.1136/bmjgh-2019-002213https://dx.doi.org/10.1136/bmjgh-2019-002213https://dx.doi.org/10.1136/bmjgh-2019-002213https://dx.doi.org/10.1136/bmjgh-2019-002213https://dx.doi.org/10.1136/bmjgh-2019-002213https://dx.doi.org/10.1136/bmjgh-2019-002213https://dx.doi.org/10.1136/bmjgh-2019-002213http://gh.bmj.com/
-
Kostova D, et al. BMJ Global Health 2020;5:e002213. doi:10.1136/bmjgh-2019-002213 3
BMJ Global Health
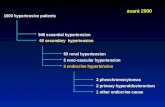
table A5). Of these, 42 studies across 15 countries provided estimates of cost- effectiveness, with the rest evaluating costs only. A diagram of the search process is depicted in figure 1. Each of the 42 cost- effectiveness studies underwent a quality assessment based on a 13- question checklist informed by Drummond guide-lines for economic evaluation of healthcare programmes (Evers et al, 2005).19 These studies were reviewed and assigned a total score equal to the sum of positive answers to the checklist questions.
Reported indicators included: cost per mm Hg reduc-tion in systolic and/or diastolic blood pressure (table 1), cost per patient with controlled hypertension (table 2), cost per patient with hypertension (table 3), cost per averted disability- adjusted life year (DALY) (table 4) and cost per gained quality- adjusted life year (QALY) (table 5). Estimates were converted to constant 2017 US dollars (US$) and were adjusted to reflect annual amounts where applicable. Two studies reported esti-mates in purchasing- power- parity (PPP)- adjusted inter-national dollars, which were not converted into US$
because appropriate conversion factors were not avail-able for the blend of countries examined (Ortegon et al, 201220 and Murray et al, 2003). Studies in the above cost- effectiveness categories were further categorised according to intervention type, as follows. ‘Pharm only’ indicates interventions where pharmacotherapy is the only treatment element, encompassing various combina-tions of drugs and drug classes, different providers and delivery platforms. ‘Pharm plus’ indicates combination programmes that incorporate other forms of treatment for hypertension in addition to medications, such as patient education or lifestyle changes. ‘Other’ indicates interventions that did not evaluate changes in pharma-cological treatment. Cost elements included costs of medication, laboratory work, labour, equipment, trans-portation, provider training and others.
RESULTSStudy characteristicsThirty- six of the identified studies were conducted in upper- middle- income countries (UMICs), 30 studies were from low- income and lower- middle- income countries (LLMICs) and five studies included countries of different income levels. Studies reported costs of hypertension treatment, cost- effectiveness of hypertension treatment or both. Twenty- five of the studies included only medi-cation costs, while the remaining studies included health system costs and other services such as laboratory tests, health provider time and other screening costs. Study designs included longitudinal (seven studies), cross- sectional (four studies), modelled or simulated (22 studies), randomised control trials (seven studies) and retrospective cohort studies (two studies).
After conducting the quality assessment based on the 13- question checklist informed by Drummond guide-lines for economic evaluation of healthcare programmes (Evers et al, 2005),19 the average quality score of the studies was 7.8. Modelled studies and randomised control trials tended to be higher quality, with average scores of 9.6 and 8.4, respectively. Longitudinal, cross- sectional and retrospective cohort studies were lower quality, with average scores of 5.0, 4.3 and 3.0, respectively (table 6).
Fifty- four studies described pharmaceutical- only inter-ventions using various combinations of antihypertensive drugs and drug classes. Fifteen studies assessed pharma-ceutical treatment plus at least one other component, such as providing physician training, implementing treatment guidelines or offering lifestyle advice. A small number of studies did not include pharmaceutical treat-ment and instead assessed cost- effectiveness of activities such as physician training, lifestyle education (Bai et al, 201321 and Jafar et al, 2011),22 or loaning out blood pressure self- measurement devices (Calvo- Vargas et al, 2001).23 Four different delivery platforms were repre-sented across studies: community- based services; health centres providing basic medical care and staffed by a physi-cian, nurse or mid- level healthcare provider; first- level
Figure 1 Summary diagram of the costs and cost- effectiveness literature search process. *Other sources searched include the Cochrane Collaboration Database of Systematic Reviews, the Tufts Cost- Effectiveness Analysis Registry, the UK’s National Institute for Health and Care Excellence (NICE) guidelines, the University of York Centre for Reviews and Dissemination and the Disease Control Priorities (3rd Edition). These databases were hand searched using similar terms as the PubMed search strategy found in online supplementary appendix table A3.
on June 29, 2021 by guest. Protected by copyright.
http://gh.bmj.com
/B
MJ G
lob Health: first published as 10.1136/bm
jgh-2019-002213 on 9 Septem
ber 2020. Dow
nloaded from
https://dx.doi.org/10.1136/bmjgh-2019-002213https://dx.doi.org/10.1136/bmjgh-2019-002213http://gh.bmj.com/
-
4 Kostova D, et al. BMJ Global Health 2020;5:e002213. doi:10.1136/bmjgh-2019-002213
BMJ Global Health
Tab
le 1
C
ost
per
mm
Hg
red
uctio
n in
sys
tolic
and
/or
dia
stol
ic b
lood
pre
ssur
e (2
017
US
$)C
oun
try
inco
me
gro
upC
oun
try
Aut
hor
Stu
dy
typ
eS
amp
le
size
Stu
dy
des
ign
Pro
vid
erIn
terv
enti
on
det
ails
Tim
e p
erio
dC
ost
ele
men
tsIn
terv
enti
on
sub
gro
up
Co
st –
sy
sto
lic
(201
7 U
S$)
Co
st –
d
iast
olic
(2
017
US
$)
Low
er
mid
dle
Ind
iaA
ncha
laP
harm
plu
s16
38C
lust
er
rand
omis
ed
cont
rol s
tud
y
Doc
tors
Prim
ary
heal
thca
re p
hysi
cian
s re
ceiv
ed
trai
ning
to
use
dec
isio
n su
pp
ort
syst
em
(DS
S) s
oftw
are
for
man
agem
ent
of
HTN
or
rece
ived
cha
rt- b
ased
sup
por
t w
ith H
TN g
uid
elin
es o
n a
pos
ter.
1 ye
arD
rugs
, lab
orat
orie
s, la
bou
r, tr
avel
/tra
nsp
orta
tion/
per
die
m,
bui
ldin
g ov
erhe
ad c
osts
, d
epre
ciat
ion,
eq
uip
men
t co
sts
and
offi
ce s
upp
lies,
tra
inin
g co
sts,
in
terv
entio
n d
evel
opm
ent
cost
s,
tran
slat
ion
char
ges.
Dec
isio
n su
pp
ort
syst
em37
.82
Cha
rt- b
ased
sup
por
t99
.29
Up
per
m
idd
leS
outh
A
fric
aA
nder
son
AP
harm
onl
y14
73M
eta-
anal
ysis
Not
sp
ecifi
edC
omp
aris
on o
f the
ang
iote
nsin
re
cep
tor
blo
cker
s (A
RB
s) c
urre
ntly
av
aila
ble
in S
outh
Afr
ica:
can
des
arta
n,
losa
rtan
, irb
esar
tan
and
val
sart
an.
1 ye
arD
rugs
Can
des
arta
n4.
6
Losa
rtan
5.47
Irb
esar
tan
6.11
Vals
arta
n6.
77
Up
per
m
idd
leA
rgen
tina
Aug
usto
vski
Pha
rm p
lus
1432
Clu
ster
ra
ndom
ised
co
ntro
l stu
dy
Com
mun
ity
heal
th w
orke
rs,
doc
tors
Mul
ticom
pon
ent
stra
tegy
tha
t in
clud
ed
com
mun
ity h
ealth
wor
ker
hom
e- b
ased
in
terv
entio
n, p
hysi
cian
ed
ucat
ion
and
a
text
- mes
sagi
ng in
terv
entio
n.
1.5
year
sD
rugs
, lab
orat
orie
s, la
bou
r, co
sts
of m
edic
al v
isit
or s
cree
ning
- n
ot
furt
her
dis
aggr
egat
ed, e
qui
pm
ent
cost
s an
d o
ffice
sup
plie
s,
inte
rven
tion
dev
elop
men
t co
sts,
tr
aini
ng c
osts
, hea
lth e
duc
atio
n/p
rom
otio
n/ m
edia
cos
ts.
Con
trol
gro
up15
.37
29.5
7
Inte
rven
tion
grou
p19
.51
32.7
2
Up
per
m
idd
leC
hina
Bai
Pha
rm p
lus
818
Ob
serv
atio
nal
stud
yD
octo
rs, n
urse
s,
pha
rmac
ists
, ot
her
Com
mun
ity h
ealth
cen
tres
tha
t ar
e p
art
of a
chr
onic
dis
ease
con
trol
go
vern
men
t p
rogr
amm
e. C
omp
onen
ts
of in
terv
entio
n in
clud
e cl
assi
fyin
g p
atie
nts
into
four
gro
ups
bas
ed o
n B
P a
nd r
isk;
con
duc
t d
iet,
exe
rcis
e,
smok
ing
and
drin
king
inte
rven
tions
co
nsis
ting
of e
duc
atio
nal s
essi
ons,
su
per
visi
on a
nd fa
ce- t
o- fa
ce
cons
ulta
tion
as n
eces
sary
; sta
ndar
dis
e d
rug
ther
apie
s ac
cord
ing
to 2
005
Chi
nese
nat
iona
l gui
del
ines
for
hyp
erte
nsio
n p
reve
ntio
n an
d c
ontr
ol;
cond
uct
follo
w- u
p v
isits
on
a re
gula
r b
asis
; pro
vid
e ot
her
serv
ices
, suc
h as
phy
sici
an r
ecom
men
dat
ions
, if
nece
ssar
y.
1 ye
arLa
bou
r, b
uild
ing
over
head
cos
ts,
dep
reci
atio
n, e
qui
pm
ent
cost
s an
d
offic
e su
pp
lies,
hea
lth e
duc
atio
n/p
rom
otio
n co
sts.
Bes
t ca
se s
cena
rio -
bas
ed
on t
he lo
wes
t p
er c
apita
cos
t an
d g
reat
est
blo
od p
ress
ure
red
uctio
n of
the
com
mun
ity
heal
th c
entr
es
0.35
0.75
Com
mun
ity h
ealth
cen
tre
in B
eijin
g0.
611.
05
Ove
rall
- al
l thr
ee c
omm
unity
he
alth
cen
tres
0.67
1.33
Com
mun
ity h
ealth
cen
tre
in
Han
gzho
u0.
751.
61
Com
mun
ity h
ealth
cen
tre
in
Che
ngd
u0.
831.
62
Wor
st c
ase
scen
ario
- b
ased
on
the
hig
hest
per
cap
ita
cost
and
sm
alle
st b
lood
p
ress
ure
red
uctio
n of
the
co
mm
unity
hea
lth c
entr
es
1.76
3.43
Ble
ndB
lend
Bas
uP
harm
onl
y -
mod
elle
dN
ot
app
licab
leH
ypot
hetic
al
pop
ulat
ion-
leve
l m
odel
Not
sp
ecifi
edA
‘tre
at- t
o- ta
rget
’ (TT
T) s
trat
egy
in
whi
ch B
P t
hera
py
is t
itrat
ed u
ntil
blo
od
pre
ssur
es fa
ll b
elow
a t
hres
hold
, a
‘ben
efit-
bas
ed, t
ailo
red
’ (B
BT)
str
ateg
y in
whi
ch B
P t
hera
py
is in
itiat
ed fo
r p
atie
nts
with
hig
h es
timat
ed C
VD
ris
k,
and
a h
ybrid
str
ateg
y th
at c
omb
ines
TT
T an
d B
BT.
Sim
ulat
ion
per
iod
: 10
year
s
Dru
gs, c
osts
of m
edic
al s
ervi
ces
- in
clud
ing
pat
ient
- bor
ne c
osts
BB
T -
Chi
na0.
12
Hyb
rid -
Chi
na0.
13
TTT
- C
hina
0.14
BB
T -
Ind
ia0.
17
TTT
- In
dia
0.2
Hyb
rid -
Ind
ia0.
28
Con
tinue
d
on June 29, 2021 by guest. Protected by copyright.
http://gh.bmj.com
/B
MJ G
lob Health: first published as 10.1136/bm
jgh-2019-002213 on 9 Septem
ber 2020. Dow
nloaded from
http://gh.bmj.com/
-
Kostova D, et al. BMJ Global Health 2020;5:e002213. doi:10.1136/bmjgh-2019-002213 5
BMJ Global Health
Co
untr
y in
com
e g
roup
Co
untr
yA
utho
rS
tud
y ty
pe
Sam
ple
si
zeS
tud
y d
esig
nP
rovi
der
Inte
rven
tio
n d
etai
lsT
ime
per
iod
Co
st e
lem
ents
Inte
rven
tio
n su
bg
roup
Co
st –
sy
sto
lic
(201
7 U
S$)
Co
st –
d
iast
olic
(2
017
US
$)
Up
per
m
idd
leA
rgen
tina
He
Pha
rm p
lus
1357
Clu
ster
ra
ndom
ised
co
ntro
l stu
dy
Com
mun
ity
heal
th w
orke
rs,
doc
tors
Inte
rven
tion
clin
ics
imp
lem
ente
d
a co
mm
unity
hea
lth w
orke
r- le
d
hom
e- b
ased
pro
gram
me
incl
udin
g he
alth
coa
chin
g, a
nd B
P m
onito
ring.
P
hysi
cian
s at
the
clin
ics
rece
ived
on
line
educ
atio
n co
urse
on
HTN
m
anag
emen
t, a
nd p
atie
nts
rece
ived
in
div
idua
lised
tex
t m
essa
ges.
Con
trol
cl
inic
s m
aint
aine
d u
sual
car
e: m
onth
ly
visi
ts a
fter
initi
atio
n of
ant
ihyp
erte
nsiv
e tr
eatm
ent
and
eve
ry 3
to
6 m
onth
s fo
r p
atie
nts
with
con
trol
led
BP.
18 m
onth
sD
rugs
, lab
orat
orie
s, la
bou
r, co
sts
of m
edic
al v
isits
or
scre
enin
g no
t fu
rthe
r d
isag
greg
ated
, eq
uip
men
t co
sts,
inte
rven
tion
dev
elop
men
t co
sts,
tra
inin
g co
sts,
med
ia c
osts
Usu
al c
are
5.59
10.5
6
Inte
rven
tion
9.25
14.0
6
Low
er
mid
dle
Pak
ista
nJa
far
Oth
er10
44C
lust
er
rand
omis
ed
cont
rol s
tud
y
Com
mun
ity
heal
th w
orke
rs,
doc
tors
Fam
ily- b
ased
hom
e he
alth
ed
ucat
ion
by
com
mun
ity h
ealth
wor
kers
and
sp
ecia
l tra
inin
g of
gen
eral
pra
ctiti
oner
s on
tre
atm
ent
and
man
agem
ent
of H
TN.
2 ye
ars
Dru
gs, l
abor
ator
ies,
lab
our,
cost
of
med
ical
vis
it or
scr
eeni
ng -
not
fu
rthe
r d
isag
greg
ated
, tra
vel/
tran
spor
tatio
n/p
er d
iem
, bui
ldin
g ov
erhe
ad c
osts
, tra
inin
g co
sts,
he
alth
ed
ucat
ion/
pro
mot
ion/
ab
sent
eeis
m o
r lo
st p
rod
uctiv
ity
and
frui
ts a
nd v
eget
able
s.
Hom
e he
alth
ed
ucat
ion
and
ge
nera
l pra
ctiti
oner
tra
inin
g54
.72
Hom
e he
alth
ed
ucat
ion
only
83.0
1
Gen
eral
pra
ctiti
oner
tra
inin
g on
ly11
3.53
Low
Nep
alK
rishn
anP
harm
plu
s –
mod
elle
dN
ot
app
licab
leH
ypot
hetic
al
pop
ulat
ion-
leve
l m
odel
Com
mun
ity
heal
th w
orke
rsC
omm
unity
hea
lth w
orke
rs p
rovi
de
blo
od p
ress
ure
scre
enin
g, li
fest
yle
coun
selli
ng, r
efer
rals
and
follo
w- u
p
on a
dhe
renc
e to
ant
ihyp
erte
nsiv
e m
edic
atio
n vi
a ho
me
visi
ts
1 ye
ar
Dru
gs, l
abou
r, tr
avel
, tra
inin
g co
sts,
ad
min
istr
ativ
e co
sts
Ad
ults
age
d 2
5 to
65
with
hy
per
tens
ion
1.64
All
adul
ts a
ged
25
to 6
50.
51
Up
per
m
idd
leB
razi
lO
bre
li- N
eto
Pha
rm p
lus
200
Ran
dom
ised
co
ntro
lled
cl
inic
al t
rial
Doc
tors
, nur
ses,
p
harm
acis
tsTh
e co
ntro
l gro
up r
ecei
ved
the
usu
al
care
offe
red
by
the
prim
ary
heal
thca
re
unit
(med
ical
and
nur
se c
onsu
ltatio
ns).
The
inte
rven
tion
grou
p r
ecei
ved
the
us
ual c
are
plu
s a
pha
rmac
eutic
al c
are
inte
rven
tion.
3 ye
ars
Dru
gs, l
abou
r an
d c
ost
of m
edic
al
visi
t or
scr
eeni
ng -
not
furt
her
dis
aggr
egat
ed.
Inte
rven
tion
grou
p (c
ost
per
p
atie
nt d
ivid
ed b
y av
erag
e ch
ange
dur
ing
stud
y p
erio
d)
12.6
719
.69
Low
er
mid
dle
Ind
iaP
atel
Pha
rm o
nly
60O
bse
rvat
iona
l st
udy
Not
sp
ecifi
edC
omp
arin
g tw
o b
eta
blo
cker
s -
neb
ivol
ol a
nd m
etop
rolo
l.2
mon
ths
Dru
gsN
ebiv
olol
2.5
mg
0.57
0.81
Neb
ivol
ol 5
mg
0.64
1.02
Met
opro
lol 2
5 m
g0.
891.
07
Met
opro
lol 5
0 m
g1.
071.
31
Neb
ivol
ol 1
0 m
g1.
091.
3
Met
opro
lol 1
00 m
g1.
131.
29
Up
per
m
idd
leB
razi
lTs
uji
Pha
rm o
nly
418
Ob
serv
atio
nal
stud
yN
ot s
pec
ified
Trad
ition
al t
reat
men
t (h
ydro
chlo
roth
iazi
de
and
ate
nolo
l) an
d c
urre
nt t
reat
men
t (lo
sart
an a
nd
amlo
dip
ine)
wer
e ev
alua
ted
in p
atie
nts
with
gra
de
1 or
2 h
yper
tens
ion.
For
p
atie
nts
with
gra
de
3 hy
per
tens
ion,
a
third
dru
g w
as a
dd
ed t
o th
e tr
eatm
ent
com
bin
atio
ns: e
nala
pril
was
ad
ded
to
the
tra
diti
onal
tre
atm
ent,
and
hy
dro
chlo
roth
iazi
de
was
ad
ded
to
the
curr
ent
trea
tmen
t.
1 ye
arD
rugs
Trad
ition
al: G
rad
e 1
or 2
H
TN44
.68
66.4
7
Trad
ition
al: G
rad
e 3
HTN
81.7
310
7.88
Cur
rent
: Gra
de
3 H
TN82
.82
103.
52
Cur
rent
: Gra
de
1 or
2 H
TN90
.45
130.
77
Tab
le 1
C
ontin
ued
Con
tinue
d
on June 29, 2021 by guest. Protected by copyright.
http://gh.bmj.com
/B
MJ G
lob Health: first published as 10.1136/bm
jgh-2019-002213 on 9 Septem
ber 2020. Dow
nloaded from
http://gh.bmj.com/
-
6 Kostova D, et al. BMJ Global Health 2020;5:e002213. doi:10.1136/bmjgh-2019-002213
BMJ Global Health
Co
untr
y in
com
e g
roup
Co
untr
yA
utho
rS
tud
y ty
pe
Sam
ple
si
zeS
tud
y d
esig
nP
rovi
der
Inte
rven
tio
n d
etai
lsT
ime
per
iod
Co
st e
lem
ents
Inte
rven
tio
n su
bg
roup
Co
st –
sy
sto
lic
(201
7 U
S$)
Co
st –
d
iast
olic
(2
017
US
$)
Up
per
m
idd
leC
hina
Wan
g X
Pha
rm p
lus
436
Ran
dom
ised
co
ntro
lled
tria
lD
octo
rsP
rovi
der
tra
inin
g in
gui
del
ine-
orie
nted
p
rimar
y he
alth
care
HTN
man
agem
ent
pro
gram
me
cove
ring
det
ectio
n,
eval
uatio
n, n
on- p
harm
aceu
tical
and
p
harm
aceu
tical
tr e
atm
ent,
follo
w- u
p
and
man
agem
ent,
tw
o- w
ay r
efer
ral,
pre
vent
ion
and
hea
lth e
duc
atio
n fo
r hy
per
tens
ion.
1 ye
arD
rugs
, lab
our,
trav
el/
tran
spor
tatio
n/p
er d
iem
and
tr
aini
ng c
osts
.
PP
ana
lysi
s ru
ral i
nter
vent
ion
3.73
5.99
ITT
anal
ysis
rur
al in
terv
entio
n3.
856.
22
ITT
anal
ysis
rur
al c
ontr
ol4.
89.
1
ITT
anal
ysis
urb
an
inte
rven
tion
5.32
15.2
2
PP
ana
lysi
s ur
ban
in
terv
entio
n5.
3715
.76
PP
ana
lysi
s ru
ral c
ontr
ol5.
5511
.09
ITT
anal
ysis
urb
an c
ontr
ol7.
9434
.8
PP
ana
lysi
s ur
ban
con
trol
9.06
51.9
6
Up
per
m
idd
leC
hina
Wan
g Z
Pha
rm o
nly
623
Ob
serv
atio
nal
stud
yN
ot s
pec
ified
Trea
tmen
t w
ith n
itren
dip
ine
with
hy
dro
chlo
roth
iazi
de,
or
trea
tmen
t w
ith
nitr
end
ipin
e w
ith m
etop
rolo
l.
6 m
onth
sD
rugs
, cos
t of
med
ical
vis
it or
scr
eeni
ng -
not
furt
her
dis
aggr
egat
ed, t
rave
l/tr
ansp
orta
tion/
per
die
m
Nitr
end
ipin
e +
hy
dro
chlo
roth
iazi
de.
Wom
en.
1.47
3.05
Nitr
end
ipin
e +
hy
dro
chlo
roth
iazi
de.
Men
.1.
472.
95
Nitr
end
ipin
e +
hy
dro
chlo
roth
iazi
de.
65
year
s an
d o
lder
.
1.47
2.95
Nitr
end
ipin
e +
hy
dro
chlo
roth
iazi
de.
All
pat
ient
s.
1.47
2.95
Nitr
end
ipin
e +
hy
dro
chlo
roth
iazi
de.
Und
er
65 y
ears
old
.
1.58
3.37
Nitr
end
ipin
e +
met
opro
lol.
Wom
en.
1.89
3.89
Nitr
end
ipin
e +
met
opro
lol.
65 y
ears
and
old
er.
23.
89
Nitr
end
ipin
e +
met
opro
lol.
All
pat
ient
s.2
4
Nitr
end
ipin
e +
met
opro
lol.
Men
.2.
14.
1
Nitr
end
ipin
e +
met
opro
lol.
Und
er 6
5 ye
ars
old
.2.
314.
52
‘Pha
rm o
nly’
ind
icat
es in
terv
entio
ns o
r st
udie
s in
whi
ch p
harm
acot
hera
py
is t
he o
nly
form
of t
reat
men
t fo
r hy
per
tens
ion.
Thi
s in
clud
es t
estin
g va
rious
com
bin
atio
ns o
f dru
gs a
nd d
rug
clas
ses,
diff
eren
t p
rovi
der
s an
d d
eliv
ery
pla
tfor
ms.
‘Pha
rm p
lus’
ind
icat
es c
omb
inat
ion
pro
gram
mes
tha
t in
corp
orat
ed o
ther
form
s of
tr
eatm
ent
for
hyp
erte
nsio
n, s
uch
as p
atie
nt e
duc
atio
n or
life
styl
e ch
ange
s. ‘O
ther
’ ind
icat
es a
pro
gram
me
in w
hich
the
re w
as n
o p
harm
acol
ogic
al t
reat
men
t.B
P, b
lood
pre
ssur
e; C
VD
, car
dio
vasc
ular
dis
ease
; HTN
, hyp
erte
nsio
n; IT
T, in
tent
ion-
to- t
reat
; PP,
per
pro
toco
l; U
S$,
US
dol
lars
.
Tab
le 1
C
ontin
ued
on June 29, 2021 by guest. Protected by copyright.
http://gh.bmj.com
/B
MJ G
lob Health: first published as 10.1136/bm
jgh-2019-002213 on 9 Septem
ber 2020. Dow
nloaded from
http://gh.bmj.com/
-
Kostova D, et al. BMJ Global Health 2020;5:e002213. doi:10.1136/bmjgh-2019-002213 7
BMJ Global Health
Tab
le 2
A
nnua
l cos
t p
er p
atie
nt w
ith c
ontr
olle
d h
yper
tens
ion
(blo
od p
ress
ure
bro
ught
bel
ow d
efine
d t
hres
hold
) (20
17 U
S$)
Co
untr
y in
com
e g
roup
Co
untr
yA
utho
rIn
terv
enti
on
typ
eS
amp
le
size
Stu
dy
des
ign
Pro
vid
erIn
terv
enti
on
det
ails
Co
st e
lem
ents
Inte
rven
tio
n su
bg
roup
Co
st (2
017
US
$)
Up
per
mid
dle
Mal
aysi
aA
lefa
nP
harm
onl
y60
0O
bse
rvat
iona
lD
octo
rs, n
urse
s,
pha
rmac
ists
Com
par
ing
diff
eren
t an
tihyp
erte
nsiv
e d
rug
clas
ses
and
com
bin
atio
ns: D
iure
tics,
BB
, AC
EIs
, C
CB
s, p
razo
sin,
diu
retic
s an
d A
CE
Is a
nd o
ther
co
mb
inat
ions
Dru
gs, l
abor
ator
ies,
la
bou
r, an
d t
rave
l/tr
ansp
orta
tion/
per
die
m.
Diu
retic
s62
6.78
Bet
a b
lock
ers
840.
89
AC
E In
hib
itors
977.
54
Pra
zosi
n10
04.0
7
Diu
retic
s an
d
bet
a b
lock
ers
1172
.96
Cal
cium
cha
nnel
b
lock
ers
1446
.8
Oth
er
com
bin
atio
ns25
09.7
Up
per
mid
dle
Thai
land
Pan
naru
noth
aai
Pha
rm o
nly
81C
ross
- se
ctio
nal
Not
sp
ecifi
edA
ll ca
ses
of d
iab
etes
and
hyp
erte
nsio
n th
at
regi
ster
ed a
nd m
ade
use
of t
he u
rban
hea
lth
cent
re fr
om 1
994
to 1
996
wer
e in
clud
ed in
gr
oup
1. A
ll d
iab
etic
and
hyp
erte
nsio
n p
atie
nts
who
res
ided
in t
he c
atch
men
t ar
ea o
f the
ho
spita
l, an
d v
isite
d t
he r
egio
nal h
osp
ital f
rom
19
94 t
o 19
96, w
ere
incl
uded
in g
roup
2. G
roup
3
incl
uded
pat
ient
s id
entifi
ed b
y th
e ac
cid
enta
l sa
mp
ling
of d
iab
etic
and
hyp
erte
nsio
n p
atie
nts
atte
ndin
g th
e re
gion
al h
osp
ital i
n 19
97.
Dru
gs, c
ost
of m
edic
al
visi
t or
scr
eeni
ng -
not
fu
rthe
r d
isag
greg
ated
, an
d tr
avel
/tra
nsp
orta
tion/
per
die
m.
Gro
up 1
183.
97
Gro
up 2
229.
18
Gro
up 3
231.
05
AC
EIs
, AC
E in
hib
itors
; BB
, bet
a b
lock
ers;
CC
Bs,
cal
cium
cha
nnel
blo
cker
s; U
S$,
US
dol
lars
.
on June 29, 2021 by guest. Protected by copyright.
http://gh.bmj.com
/B
MJ G
lob Health: first published as 10.1136/bm
jgh-2019-002213 on 9 Septem
ber 2020. Dow
nloaded from
http://gh.bmj.com/
-
8 Kostova D, et al. BMJ Global Health 2020;5:e002213. doi:10.1136/bmjgh-2019-002213
BMJ Global Health
Tab
le 3
A
nnua
l cos
t p
er h
yper
tens
ion
pat
ient
(201
7 U
S$)
Co
untr
y in
com
e g
roup
Co
untr
yA
utho
rS
tud
y ty
pe
Sam
ple
siz
eS
tud
y d
esig
nP
rovi
der
Inte
rven
tio
n d
etai
lsC
ost
ele
men
tsIn
terv
enti
on
sub
gro
upC
ost
(201
7 U
S$)
Up
per
m
idd
leM
exic
oA
rred
ond
oP
harm
onl
y -
mod
elle
dN
ot a
pp
licab
leH
ypot
hetic
al
pop
ulat
ion-
leve
l m
odel
Not
sp
ecifi
edA
naly
sis
of h
ealth
care
cos
ts o
f cha
nges
in
ep
idem
iolo
gica
l pro
file
in M
exic
o, u
sing
hy
per
tens
ion
as o
ne o
f fou
r tr
acer
dis
ease
s.
Dru
gs, l
abor
ator
ies,
lab
our,
equi
pm
ent
cost
s an
d o
ffice
sup
plie
sTo
tal h
osp
ital a
nd
amb
ulat
ory
cost
s p
er
case
of h
yper
tens
ion
904.
73
Up
per
m
idd
leM
alay
sia
Ale
fan
Pha
rm o
nly
600
Ob
serv
atio
nal
Doc
tors
, nu
rses
, p
harm
acis
ts
Com
par
ing
diff
eren
t an
tihyp
erte
nsiv
e d
rug
clas
ses
and
com
bin
atio
ns: D
iure
tics,
BB
, A
CE
Is, C
CB
s, p
razo
sin,
diu
retic
s an
d A
CE
Is
and
oth
er c
omb
inat
ions
Dru
gs, l
abor
ator
ies,
lab
our,
and
tra
vel/
tran
spor
tatio
n/p
er d
iem
.D
iure
tics
522.
32
Diu
retic
s +
bet
a b
lock
ers
614.
41
Bet
a b
lock
ers
626.
32
AC
E in
hib
itors
651.
69
Cal
cium
cha
nnel
b
lock
ers
723.
4
Pra
zosi
n75
3.06
Oth
er c
omb
inat
ions
826.
64
Low
er
mid
dle
Ind
iaA
ncha
laP
harm
plu
s16
38C
lust
er
rand
omis
ed
cont
rol t
rial
Doc
tor
Prim
ary
heal
thca
re p
hysi
cian
s re
ceiv
ed
trai
ning
to
use
dec
isio
n su
pp
ort
syst
em
(DS
S) s
oftw
are
for
man
agem
ent
of H
TN
or r
ecei
ved
cha
rt- b
ased
sup
por
t w
ith H
TN
guid
elin
es o
n a
pos
ter .
Dru
gs, l
abor
ator
ies,
lab
our,
trav
el/
tran
spor
tatio
n/p
er d
iem
, bui
ldin
g ov
erhe
ad
cost
s, d
epre
ciat
ion,
eq
uip
men
t co
sts
and
of
fice
sup
plie
s, t
rain
ing
cost
s, in
terv
entio
n d
evel
opm
ent
cost
s, t
rans
latio
n ch
arge
s.
Cha
rt- b
ased
sup
por
t35
6.47
Dec
isio
n su
pp
ort
syst
em38
3.15
Up
per
m
idd
leA
rgen
tina
Aug
usto
vski
Pha
rm p
lus
1432
Clu
ster
ra
ndom
ised
co
ntro
l tria
l
Com
mun
ity
heal
th w
orke
rs,
doc
tors
Mul
ticom
pon
ent
stra
tegy
tha
t in
clud
ed
com
mun
ity h
ealth
wor
ker
hom
e- b
ased
in
terv
entio
n, p
hysi
cian
ed
ucat
ion
and
a t
ext-
m
essa
ging
inte
rven
tion.
Dru
gs, l
abor
ator
ies,
lab
our,
cost
s of
m
edic
al v
isit
or s
cree
ning
- n
ot fu
rthe
r d
isag
greg
ated
, eq
uip
men
t co
sts
and
of
fice
sup
plie
s, in
terv
entio
n d
evel
opm
ent
cost
s, t
rain
ing
cost
s, h
ealth
ed
ucat
ion/
pro
mot
ion/
med
ia c
osts
.
Inte
rven
tion
grou
p20
2.85
Con
trol
gro
up10
2.49
Up
per
m
idd
leC
hina
Bai
Oth
er81
8O
bse
rvat
iona
l st
udy
Doc
tors
, nu
rses
, p
harm
acis
ts,
othe
r
Com
mun
ity h
ealth
cen
tres
tha
t ar
e p
art
of a
chr
onic
dis
ease
con
trol
gov
ernm
ent
pro
gram
me.
Com
pon
ents
of i
nter
vent
ion
incl
ude
clas
sify
ing
pat
ient
s in
to fo
ur g
roup
s b
ased
on
BP
and
ris
k; c
ond
uct
lifes
tyle
ed
ucat
ion
sess
ions
, sup
ervi
sion
, and
one
- on
- one
ses
sion
s; s
tand
ard
ise
dru
g th
erap
ies
acco
rdin
g to
200
5 C
hine
se n
atio
nal
guid
elin
es; c
ond
uct
follo
w- u
p v
isits
on
a r e
gula
r b
asis
; pro
vid
e ot
her
serv
ices
, suc
h as
phy
sici
an r
ecom
men
dat
ions
, if n
eces
sary
.
Lab
our,
bui
ldin
g ov
erhe
ad c
osts
, d
epre
ciat
ion,
eq
uip
men
t co
sts
and
offi
ce
sup
plie
s, a
nd h
ealth
ed
ucat
ion/
pro
mot
ion
cost
s.
Com
mun
ity h
ealth
ce
ntre
in B
eijin
g6.
19
Com
mun
ity h
ealth
ce
ntre
in C
heng
du
6.35
Ove
rall
- al
l thr
ee
com
mun
ity h
ealth
ce
ntre
s
8.19
Com
mun
ity h
ealth
ce
ntre
in H
angz
hou
13.3
8
Ble
ndB
lend
Bas
uP
harm
onl
y -
mod
elle
dN
ot a
pp
licab
leH
ypot
hetic
al
pop
ulat
ion-
leve
l m
odel
Not
sp
ecifi
edA
‘tre
at- t
o- ta
rget
’ (TT
T) s
trat
egy
in w
hich
B
P t
hera
py
is t
itrat
ed u
ntil
blo
od p
ress
ures
fa
ll b
elow
a t
hres
hold
, a ‘b
enefi
t- b
ased
, ta
ilore
d’ (
BB
T) s
trat
egy
in w
hich
BP
the
rap
y is
initi
ated
for
pat
ient
s w
ith h
igh
estim
ated
C
VD
ris
k, a
nd a
hyb
rid s
trat
egy
that
co
mb
ines
TTT
and
BB
T.
Dru
gs, c
osts
of m
edic
al s
ervi
ces
- in
clud
ing
pat
ient
- bor
ne c
osts
TTT
- In
dia
48.8
8
TTT
- C
hina
57.4
1
BB
T -
Ind
ia76
.57
Hyb
rid -
Chi
na87
.69
Hyb
rid -
Ind
ia90
.72
BB
T -
Chi
na99
.14
Up
per
m
idd
leB
razi
lB
ueno
Pha
rm o
nly
377
Cro
ss- s
ectio
nal
stud
yN
ot s
pec
ified
Ana
lysi
s of
the
ass
ocia
tion
bet
wee
n p
hysi
cal
activ
ity le
vel a
nd h
ealth
care
cos
ts a
mon
g hy
per
tens
ive
non-
inst
itutio
nalis
ed o
lder
p
eop
le.
Dru
gs, c
ost
of m
edic
al v
isit
or s
cree
ning
-
not
furt
her
dis
aggr
egat
edA
ctiv
ity le
vel:
activ
e36
.08
Act
ivity
leve
l: in
suffi
cien
tly a
ctiv
e14
4.51
Act
ivity
leve
l: se
den
tary
158.
81
Con
tinue
d
on June 29, 2021 by guest. Protected by copyright.
http://gh.bmj.com
/B
MJ G
lob Health: first published as 10.1136/bm
jgh-2019-002213 on 9 Septem
ber 2020. Dow
nloaded from
http://gh.bmj.com/
-
Kostova D, et al. BMJ Global Health 2020;5:e002213. doi:10.1136/bmjgh-2019-002213 9
BMJ Global Health
Co
untr
y in
com
e g
roup
Co
untr
yA
utho
rS
tud
y ty
pe
Sam
ple
siz
eS
tud
y d
esig
nP
rovi
der
Inte
rven
tio
n d
etai
lsC
ost
ele
men
tsIn
terv
enti
on
sub
gro
upC
ost
(201
7 U
S$)
Up
per
m
idd
leM
exic
oC
alvo
- Var
gas
Pha
rm o
nly
Not
rep
orte
dLo
ngitu
din
al
stud
yN
ot s
pec
ified
Ana
lysi
s of
the
ann
ual c
ost
of
antih
yper
tens
ive
med
icat
ions
with
the
cos
t of
med
ical
con
sulta
tions
and
lab
orat
ory
test
s.
Dru
gs, l
abor
ator
ies,
cos
t of
med
ical
vis
it or
scr
eeni
ng -
not
furt
her
dis
aggr
egat
edA
nnua
l cos
t of
tr
eatm
ent
with
d
iure
tics
90.3
Ann
ual c
ost
of
trea
tmen
t w
ith b
eta
blo
cker
s
176.
54
Ann
ual c
ost
of
trea
tmen
t w
ith
calc
ium
cha
nnel
b
lock
ers
451.
65
Ann
ual c
ost
of
trea
tmen
t w
ith A
CE
in
hib
itors
701.
3
Up
per
m
idd
leB
razi
lC
azar
imP
harm
plu
s51
Qua
si-
Exp
erim
enta
l st
udy
Doc
tors
, p
harm
acis
tsP
rior
to in
terv
entio
n, t
he p
ublic
hea
lth
serv
ice
did
not
offe
r p
harm
aceu
tical
car
e fo
r hy
per
tens
ion.
Inte
rven
tion
invo
lved
b
lood
pre
ssur
e m
easu
rem
ents
and
CV
ris
k m
easu
res,
ana
lysi
s of
med
icat
ions
and
tes
t re
sults
, ed
ucat
ion
in h
ealth
mat
ters
with
gu
idel
ines
on
pat
ient
beh
avio
urs,
ad
here
nce
to t
reat
men
t an
d, w
hen
nece
ssar
y,
inte
rven
tions
in p
harm
acot
hera
py
Dru
gs, l
abor
ator
ies,
lab
our,
cost
of
med
ical
vis
it or
scr
eeni
ng -
not
furt
her
dis
aggr
egat
ed, t
rave
l/tra
nsp
orta
tion/
per
die
m, b
uild
ing
over
head
cos
ts,
equi
pm
ent
cost
s an
d o
ffice
sup
plie
s, a
nd
abse
ntee
ism
or
lost
pro
duc
tivity
.
Inte
rven
tion
per
iod
203.
85
Pre
- int
erve
ntio
n p
erio
d20
5.15
Pos
t- in
terv
entio
n p
erio
d22
2.31
Up
per
m
idd
leS
outh
Afr
ica
Gaz
iano
Pha
rm p
lus
- m
odel
led
Not
ap
plic
able
Hyp
othe
tical
p
opul
atio
n- le
vel
mod
el
Not
sp
ecifi
edIn
terv
entio
n in
clud
ed s
cree
ning
for
HTN
and
si
x d
iffer
ent
elig
ibili
ty c
riter
ia fo
r in
itiat
ing
pha
rmac
olog
ical
tre
atm
ent
(two
BP
- bas
ed
crite
ria a
nd fo
ur r
isk-
bas
ed c
riter
ia) a
nd a
no
trea
tmen
t sc
enar
io in
whi
ch in
div
idua
ls a
re
scre
ened
but
not
tre
ated
.
Dru
gs a
nd c
ost
of m
edic
al v
isit
or
scre
enin
g -
not
furt
her
dis
aggr
egat
ed.
Scr
eene
d -
no
trea
tmen
t80
.55
Elig
ibili
ty: a
bso
lute
ris
k >
40%
80.6
6
Elig
ibili
ty: a
bso
lute
ris
k >
30%
81.3
Elig
ibili
ty: a
bso
lute
ris
k >
20%
84.5
7
Elig
ibili
ty: a
bso
lute
ris
k >
15%
87.9
Elig
ibili
ty: 1
995
Sou
th
Afr
ican
gui
del
ines
-
targ
et le
vel 1
60/9
5
88.8
3
Elig
ibili
ty: C
urre
nt
guid
elin
es -
tar
get
leve
l 140
/90
93.2
2
Up
per
m
idd
leA
rgen
tina
He
Pha
rm p
lus
1357
Clu
ster
ra
ndom
ised
co
ntro
l stu
dy
Com
mun
ity
heal
th w
orke
rs,
doc
tors
Inte
rven
tion
clin
ics
imp
lem
ente
d a
co
mm
unity
hea
lth w
orke
r- le
d h
ome-
bas
ed
pro
gram
me
incl
udin
g he
alth
coa
chin
g,
and
BP
mon
itorin
g. P
hysi
cian
s at
the
cl
inic
s re
ceiv
ed o
nlin
e ed
ucat
ion
cour
se o
n H
TN m
anag
emen
t, a
nd p
atie
nts
rece
ived
in
div
idua
lised
tex
t m
essa
ges.
Con
trol
clin
ics
mai
ntai
ned
usu
al c
are:
mon
thly
vis
its a
fter
in
itiat
ion
of a
ntih
yper
tens
ive
trea
tmen
t an
d e
very
3 t
o 6
mon
ths
for
pat
ient
s w
ith
cont
rolle
d B
P.
Dru
gs, l
abor
ator
ies,
lab
our,
cost
s of
m
edic
al v
isits
or
scre
enin
g no
t fu
rthe
r d
isag
greg
ated
, eq
uip
men
t co
sts,
in
terv
entio
n d
evel
opm
ent
cost
s, t
rain
ing
cost
s, m
edia
cos
ts
Inte
rven
tion
119.
07
Usu
al c
are
45.0
7
Tab
le 3
C
ontin
ued
Con
tinue
d
on June 29, 2021 by guest. Protected by copyright.
http://gh.bmj.com
/B
MJ G
lob Health: first published as 10.1136/bm
jgh-2019-002213 on 9 Septem
ber 2020. Dow
nloaded from
http://gh.bmj.com/
-
10 Kostova D, et al. BMJ Global Health 2020;5:e002213. doi:10.1136/bmjgh-2019-002213
BMJ Global Health
Co
untr
y in
com
e g
roup
Co
untr
yA
utho
rS
tud
y ty
pe
Sam
ple
siz
eS
tud
y d
esig
nP
rovi
der
Inte
rven
tio
n d
etai
lsC
ost
ele
men
tsIn
terv
enti
on
sub
gro
upC
ost
(201
7 U
S$)
Low
er
mid
dle
Pak
ista
nJa
far
Oth
er10
44C
lust
er
rand
omis
ed
cont
rol s
tud
y
Com
mun
ity
heal
th w
orke
rs,
doc
tors
Fam
ily- b
ased
hom
e he
alth
ed
ucat
ion
by
com
mun
ity h
ealth
wor
kers
and
sp
ecia
l tr
aini
ng o
f gen
eral
pra
ctiti
oner
s on
tre
atm
ent
and
man
agem
ent
of H
TN.
Dru
gs, l
abor
ator
ies,
lab
our,
cost
of
med
ical
vis
it or
scr
eeni
ng -
not
furt
her
dis
aggr
egat
ed, t
rave
l/tra
nsp
orta
tion/
per
d
iem
, bui
ldin
g ov
erhe
ad c
osts
, tra
inin
g co
sts,
hea
lth e
duc
atio
n/p
rom
otio
n/
abse
ntee
ism
or
lost
pro
duc
tivity
and
frui
ts
and
veg
etab
les.
Hom
e he
alth
ed
ucat
ion
only
232.
42
Hom
e he
alth
ed
ucat
ion
and
ge
nera
l pra
ctiti
oner
tr
aini
ng
295.
49
Gen
eral
pra
ctiti
oner
tr
aini
ng o
nly
317.
89
Up
per
m
idd
leC
hina
LeP
harm
onl
y93
96C
ross
- sec
tiona
l st
udy
Not
sp
ecifi
edE
stim
atio
n of
the
eco
nom
ic b
urd
en o
f hy
per
tens
ion
usin
g cr
oss-
sect
iona
l hea
lth
exam
inat
ion
and
que
stio
nnai
re s
urve
y. C
are
incl
udes
out
pat
ient
vis
its, h
osp
italis
atio
n an
d m
edic
atio
n.
Dru
gs, c
ost
of m
edic
al v
isit
or s
cree
ning
-
not
furt
her
dis
aggr
egat
ed, t
rave
l/tr
ansp
orta
tion/
per
die
m, a
bse
ntee
ism
or
lost
pro
duc
tivity
, oth
er u
nsp
ecifi
ed
Men
609.
38
Wom
en51
1.14
Age
19
to 4
4 ye
ars
old
326.
33
Age
45
to 5
9 ye
ars
old
427.
73
Age
60
year
s an
d
old
er65
4.35
Ove
rall
547.
78
Up
per
m
idd
leS
outh
Afr
ica
Mak
kink
Pha
rm o
nly
28 1
65O
bse
rvat
iona
l st
udy
Not
sp
ecifi
edA
CE
inhi
bito
rs c
omp
ared
with
ang
iote
nsin
re
cep
tor
blo
cker
s (A
RB
s) in
man
agem
ent
of h
yper
tens
ion.
Dat
a an
alys
ed fo
r 2
year
s,
2010
and
201
1.
Dru
gs a
nd o
ther
uns
pec
ified
cos
ts.
AC
E in
hib
itor
(yea
r 20
10)
574.
06
AC
E in
hib
itor
(yea
r 20
11)
625.
06
AR
B (y
ear
2010
)72
7.3
AR
B (y
ear
2011
)86
6.27
Com
bin
ed (y
ear
2010
)20
19.9
3
Com
bin
ed (y
ear
2011
)24
17.8
5
Up
per
m
idd
leB
razi
lO
bre
li- N
eto
Pha
rm p
lus
200
Ran
dom
ised
co
ntro
lled
clin
ical
tr
ial
Doc
tors
, nu
rses
, p
harm
acis
ts
The
cont
rol g
roup
rec
eive
d t
he u
sual
car
e of
fere
d b
y th
e p
rimar
y he
alth
care
uni
t (m
edic
al a
nd n
urse
con
sulta
tions
). Th
e in
terv
entio
n gr
oup
rec
eive
d t
he u
sual
car
e p
lus
a p
harm
aceu
tical
car
e in
terv
entio
n.
Dru
gs, l
abou
r an
d c
ost
of m
edic
al v
isit
or
scre
enin
g -
not
furt
her
dis
aggr
egat
ed.
Con
trol
gro
up73
.15
Inte
rven
tion
grou
p97
.14
Low
er
mid
dle
Ken
yaO
yand
oP
harm
onl
y21
2C
ross
- sec
tiona
l st
udy
Not
sp
ecifi
edE
xam
inat
ion
of p
atie
nt c
osts
ass
ocia
ted
with
ob
tain
ing
care
for
HTN
in p
ublic
hea
lthca
re
faci
litie
s.
Dru
gs, l
abor
ator
ies,
cos
t of
med
ical
vis
it or
scr
eeni
ng -
not
furt
her
dis
aggr
egat
ed,
trav
el/t
rans
por
tatio
n/p
er d
iem
Ove
rall
med
ian
annu
al h
yper
tens
ion
care
cos
t at
a p
ublic
fa
cilit
y
282.
7
Ove
rall
mea
n an
nual
hy
per
tens
ion
care
co
st a
t a
pub
lic
faci
lity
476.
5
Tab
le 3
C
ontin
ued
Con
tinue
d
on June 29, 2021 by guest. Protected by copyright.
http://gh.bmj.com
/B
MJ G
lob Health: first published as 10.1136/bm
jgh-2019-002213 on 9 Septem
ber 2020. Dow
nloaded from
http://gh.bmj.com/
-
Kostova D, et al. BMJ Global Health 2020;5:e002213. doi:10.1136/bmjgh-2019-002213 11
BMJ Global Health
Co
untr
y in
com
e g
roup
Co
untr
yA
utho
rS
tud
y ty
pe
Sam
ple
siz
eS
tud
y d
esig
nP
rovi
der
Inte
rven
tio
n d
etai
lsC
ost
ele
men
tsIn
terv
enti
on
sub
gro
upC
ost
(201
7 U
S$)
Up
per
m
idd
leA
rgen
tina
Per
man
Pha
rm p
lus
- m
odel
led
Not
ap
plic
able
Hyp
othe
tical
p
opul
atio
n- le
vel
mod
el
Doc
tors
, m
edic
al
stud
ents
, he
alth
wor
kers
Usu
al h
yper
tens
ion
care
(prim
ary
care
p
hysi
cian
s) c
omp
ared
with
a n
ew
hyp
erte
nsio
n p
rogr
amm
e th
at a
dd
ed
per
sona
l and
tel
epho
ne c
onta
ct w
ith
pat
ient
s b
y m
edic
al s
tud
ents
; sup
por
t w
ith
die
t an
d a
ctiv
ity; e
duc
atio
nal m
ater
ial;
wor
ksho
ps;
and
, ele
ctro
nic
heal
th r
ecor
ds.
P
rogr
amm
e w
as fo
r m
idd
le- c
lass
pat
ient
s 65
ye
ars
or o
lder
.
Dru
gs, l
abor
ator
ies,
lab
our,
bui
ldin
g ov
erhe
ad c
osts
, eq
uip
men
t co
sts
and
offi
ce s
upp
lies,
hea
lth e
duc
atio
n/p
rom
otio
n
Hyp
erte
nsio
n p
rogr
amm
e24
0.43
Usu
al c
are
196.
50
Low
er
mid
dle
Ind
iaP
rave
enP
harm
onl
y62
194
Cro
ss- s
ectio
nal
stud
yN
ot s
pec
ified
Com
par
ing
the
BP
low
erin
g tr
eatm
ent
elig
ibili
ty s
tand
ard
s co
mp
ared
with
an
untr
eate
d p
opul
atio
n. T
he d
iffer
ent
trea
tmen
t st
and
ard
s w
ere:
(1) c
urre
nt p
ract
ice
(not
fu
rthe
r d
efine
d);
(2) t
reat
ing
peo
ple
with
H
TN u
sing
the
140
/90
mm
Hg
thre
shol
d;
(3) t
reat
men
t ac
cord
ing
to t
he n
ew
Ind
ian
NP
CD
CS
gui
del
ines
(dru
g th
erap
y re
com
men
ded
in p
atie
nts
with
CV
D r
isk
20%
to
30%
and
BP
leve
ls ≥
140/
90 m
m
Hg
or C
VD
ris
k of
≥30
% a
nd B
P le
vels
≥1
30/8
0 m
m H
g; (4
) tre
atin
g ev
eryo
ne in
th
e in
term
edia
te a
nd h
igh
risk
cate
gorie
s (re
gard
less
of B
P le
vel);
and
(5) t
reat
ing
only
th
ose
in t
he h
igh
risk
cate
gory
(reg
ard
less
of
BP
leve
l).
Dru
gs, c
osts
of m
edic
al v
isit
or s
cree
ning
-
not
furt
her
dis
aggr
egat
edTr
eatm
ent
of a
ll ab
ove
55 y
ears
of a
ge34
.92
Trea
tmen
t of
all
at
high
ris
k35
.07
Trea
tmen
t of
all
abov
e 45
yea
rs o
f age
35.0
8
Trea
tmen
t ac
cord
ing
to N
PC
DC
S
guid
elin
es
35.1
3
Trea
tmen
t of
all
at
inte
rmed
iate
and
hi
gh r
isk
35.1
8
Cur
rent
pra
ctic
e (u
ndefi
ned
)35
.23
Trea
tmen
t of
pat
ient
s w
ith B
P g
reat
er t
han
140/
90 m
m H
g
54.5
6
Tab
le 3
C
ontin
ued
Con
tinue
d
on June 29, 2021 by guest. Protected by copyright.
http://gh.bmj.com
/B
MJ G
lob Health: first published as 10.1136/bm
jgh-2019-002213 on 9 Septem
ber 2020. Dow
nloaded from
http://gh.bmj.com/
-
12 Kostova D, et al. BMJ Global Health 2020;5:e002213. doi:10.1136/bmjgh-2019-002213
BMJ Global Health
Co
untr
y in
com
e g
roup
Co
untr
yA
utho
rS
tud
y ty
pe
Sam
ple
siz
eS
tud
y d
esig
nP
rovi
der
Inte
rven
tio
n d
etai
lsC
ost
ele
men
tsIn
terv
enti
on
sub
gro
upC
ost
(201
7 U
S$)
Low
er
mid
dle
Ken
yaS
ubra
man
ian
Pha
rm o
nly
Not
rep
orte
dO
bse
rvat
iona
l st
udy
Doc
tors
and
ot
hers
Ana
lysi
s of
pay
men
t d
ata
on C
VD
, dia
bet
es,
bre
ast
and
cer
vica
l can
cer
and
res
pira
tory
d
isea
ses
from
Ken
yatt
a N
atio
nal H
osp
ital,
the
mai
n te
rtia
ry p
ublic
hos
pita
l and
the
K
iber
a S
outh
Hea
lth C
entr
e -
a p
ublic
ou
tpat
ient
faci
lity,
and
priv
ate
sect
or
pra
ctiti
oner
s an
d h
osp
itals
. A t
reat
men
t fr
amew
ork
was
dev
elop
ed u
sing
an
item
isat
ion
cost
ap
pro
ach
to e
stim
ate
pay
men
ts.
Dru
gs, l
abor
ator
ies,
lab
our,
cost
of
med
ical
vis
it or
scr
eeni
ng -
not
furt
her
dis
aggr
egat
ed
Pub
lic fa
cilit
y -
mon
othe
rap
y -
cost
s to
pat
ient
25.6
4
Pub
lic fa
cilit
y -
two
dru
g co
mb
inat
ion
ther
apy
- co
sts
to
pat
ient
67.2
5
Pub
lic fa
cilit
y -
thre
e d
rug
com
bin
atio
n tr
eatm
ent
- co
sts
to
pat
ient
81.2
Pub
lic fa
cilit
y -
four
d
rug
com
bin
atio
n th
erap
y -
cost
s to
p
atie
nt
110.
33
Pub
lic fa
cilit
y -
pat
ient
s w
ith r
esis
tant
hy
per
tens
ion
(hig
h B
P d
esp
ite u
se
of c
omb
inat
ion
med
icat
ions
) - c
osts
to
pat
ient
159.
36
Priv
ate
faci
lity
- m
onot
hera
py
- co
sts
to p
atie
nt
418.
2
Priv
ate
faci
lity
- tw
o d
rug
com
bin
atio
n th
erap
y -
cost
s p
er
pat
ient
596.
44
Priv
ate
faci
lity
- th
ree
dru
g co
mb
inat
ion
ther
apy
- co
sts
per
p
atie
nt
948.
06
Priv
ate
faci
lity
- re
sist
ant
hyp
erte
nsio
n (h
igh
BP
des
pite
the
us
e of
com
bin
atio
n m
edic
atio
ns) -
cos
ts
to p
atie
nt
987.
17
Tab
le 3
C
ontin
ued
Con
tinue
d
on June 29, 2021 by guest. Protected by copyright.
http://gh.bmj.com
/B
MJ G
lob Health: first published as 10.1136/bm
jgh-2019-002213 on 9 Septem
ber 2020. Dow
nloaded from
http://gh.bmj.com/
-
Kostova D, et al. BMJ Global Health 2020;5:e002213. doi:10.1136/bmjgh-2019-002213 13
BMJ Global Health
Co
untr
y in
com
e g
roup
Co
untr
yA
utho
rS
tud
y ty
pe
Sam
ple
siz
eS
tud
y d
esig
nP
rovi
der
Inte
rven
tio
n d
etai
lsC
ost
ele
men
tsIn
terv
enti
on
sub
gro
upC
ost
(201
7 U
S$)
Up
per
m
idd
leC
hina
Wan
g X
Pha
rm p
lus
436
Ran
dom
ised
co
ntro
lled
tria
lD
octo
rsP
rovi
der
tra
inin
g in
gui
del
ine-
orie
nted
H
TN m
anag
emen
t p
rogr
amm
e co
verin
g d
etec
tion,
eva
luat
ion,
non
- pha
rmac
eutic
al
and
pha
rmac
eutic
al t
reat
men
t, fo
llow
- up
and
man
agem
ent,
tw
o- w
ay r
efer
ral,
pre
vent
ion
and
hea
lth e
duc
atio
n fo
r hy
per
tens
ion.
Dru
gs, l
abou
r, tr
avel
/tra
nsp
orta
tion/
per
d
iem
, and
tra
inin
g co
sts.
Rur
al in
terv
entio
n gr
oup
- in
tent
ion-
to-
trea
t an
alys
is
70.5
8
Rur
al in
terv
entio
n gr
oup
- p
er p
roto
col
anal
ysis
73.0
3
Rur
al c
ontr
ol g
roup
-
inte
ntio
n- to
- tre
at
anal
ysis
80.1
2
Rur
al c
ontr
ol g
roup
-
per
pro
toco
l ana
lysi
s86
.52