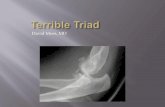
Terrible triad - elbow
-
Upload
jatinder12345 -
Category
Health & Medicine
-
view
2.271 -
download
9
Transcript of Terrible triad - elbow

Terrible Triad - Elbow


Elbow anatomy—coronoid process• Anterior aspect of the
greater sigmoid notch– Articulates with trochlear– Brachialis insertion
• Laterally– Lesser semilunar notch
articulates with radial head
• Medially– Attachment of anterior
fibers of MCL

Medial Collateral Ligament

Lateral Collateral Ligament

Stabilizers of elbow
• Primary stabilizers
Ulnohumeral jointMCL -( Ant. Bundle)LCL -
• Secondary stabilizers
Radiohumeral jointCapsuleOrigin of flexor & extensor
tendons
Dynamic stabilizers - Muscle crossing elbowAnconeusBrachialis
Triceps

Simple dislocations
• Universal disruption of the LCL
• MCL partially or completely torn
Bony congruence
• Secondary stabilizers intact
• Recurrent instability rare

Complex fracture dislocations
transolecranon fracture dislocation
posterior Monteggiadislocation, radial head, coronoid
TERRIBLE TRIAD

Terrible Triad
• Elbow dislocation • Coronoid fracture • Radial head fracture


The “terrible triad“• Subluxation—ligamentous injury
• Coronoid fracture
• Radial head fracture
• Primary and secondary stabilizers disrupted
• Recurrent instability the rule

Why terrible
• Recurrent / persistent subluxation or dislocation
• Chronic instability
• Arthrosis and pain

Terrible Triad Fracture-Dislocation
• What is so terrible about it?– Extremely unstable
• Loss of joint congruency
• Instability
– Fracture fragments are usually quite small
• Difficult to repair
– Patients don’t routinely do “well”
• Unaware of the magnitude of the injury for the elbow
• Residual instability
• Stiffness

The “terrible triad“
Ring et al (2002) J Bone Joint Surg Am
• 11 patients with terrible triad
– 4 radial head resection, 5 radial head ORIF
– None of the coronoid fractures fixed
• 5 patients redislocated in postoperative splint
– All radial head resections dislocated acutely
• 1 total elbow performed
• 9 out of 10 with native elbow developed arthrosis

Mechanism of injury
• Fall on outstretched hand
• Axial load, supination & Valgus stress

Stages
I Ulnar lateral collateral ligament disruption
II Anterior and posterior soft issue disruption with coronoid under trochlea
III a Intact MCL anterior bandIII b Ruptured MCL anterior
bandIII c All soft tissue stripped

Terrible triad - Presentation
• Pain • Clicking• Locking of elbow in extension
• Varus instability• Valgus instability – ( If MCL injured )

What are the Dilemna
• Surgical techniques challenging
• Debate in surgical steps
• Choices in management

Critical components to achieve treatment goals
• Obtaining and maintaining a concentrically reduced articulation
• Management of coronoid & radial head fracture if present
• Early range of motion

Examination
• Unstable elbow with wrist injury - High risk of compartment syndrome
• Combined distal radius and elbow fracture – 9/59 ( 15%)
• Isolated distal radius # - 3/869 ( .3%)

• Baseline neural examination
• 20% patient – Terrible ulnar nerve palsy

• High risk of developing heterotopic ossification

Management
• Dislocated elbow – reduce in emergency dept
• Unstable – Do not perform rpt rereduction
• Plan under anaesthesia

Imaging
• X- rays – Ap and lateral
• Ct scan – Include 3D reconstruction

Pathoanatomy
• Capsuloligamentous injury • Avulsion of flexor & extensor muscle from
epicondyle
• Coronoid fracture – transverse fragment with anterior capsule attached, involves 30% of height
• Radial head – anterolateral or entire radial head

Standard treatment protocolsPugh DMW, et al (2004) J Bone Joint Surg Am
• Fixation or replacement of radial head
• Fixation of coronoid fracture
• Repair of associated capsular and lateral soft-tissue injuries
• Evaluation of stability and repair of MCL as necessary
• Adjuvant hinged external fixation if residual instability

Aim of management
• Ulnohumeral joint reduced – 4 - 6 weeks
• Prevent injury and treatment related complication

Non operative treatment• Small coronoid and radial head fracture
• Concentrically reduced ulnohumeral and radiocapitellar joint
• Ct scan – insignificant fracture
• Elbow unstable in only < 30 deg flexionIMMOBILIZE IN 90 Deg
FLEXION

•Planning operative treatment of terrible triad

Positioning
• Arm on hand table
• Rotate the shoulder and work on either side

Approach
• Posterior approach
- Lateral flap
- Medial flap – ulnar nerve / MCL

Operative treatment
• Work on primarily lateral side
• Work from “outside” to “inside”
LCL / common extensor Radial head fracture Coronoid fracture

Operative treatment
• Stabilize in reverse order “inside” to “outside’’
• Repair coronoid Repair / replace radial head reattach common extensor/LCL

Lateral Interval
• Kocher ‘s - ECU and anconeus
• Boyd’s - Ulna and anconeus
• Kaplan- Extensor elevated off the ridge
“ AVAILABLE WINDOW”

Lateral: Kaplan Approach
•Anterior column exposure– Supracondylar ridge– Anterior to mid-axis of
radiocapitellar joint– Utilize LCL tear– Incise anterior capsule– Exposes anterior coronoid– Replacement or fixation

Lateral Approach: Deep dissection• Access to anterior ulno-humeral
joint– Elevate the extensors– Stay superior to the LCL– Able to visualize the PIN
• Arthrotomy– Release of the lateral capsule
and annular ligament

Medial Interval
• Medial
- Between the two head FCU
- Over the top - Hotchkiss

Approach
• Medial and lateral approach
- Large repairable radial head in the way

Surgical Planning: Approaches•What’s injured?– Radial head only– Radial head
• type 1 coronoid– Radial head
• type 2 or 3 coronoid– Proximal ulna / olecranon
• Medial Approach Needed if:• plate coronoid fracture• transpose ulnar nerve• repair or reconstruct MCL

Surgical protocol
• Fixation / replacement radial head• Fixation of coronoid fracture – if possible• Repair of associated capsule and collateral
ligament
In recalcitrant cases • Repair of MCL • Adjuvant hinged fixator
PUGH et al 2004

Radial Head Fractures:Modified - Mason Classification
•Type I: nondisplaced– No block to forearm rotation, displacement < 2mm
•Type II: displaced– Internal fixation possible
•Type III: displaced, severely comminuted– Judged to be irreparable
•Type IV: fracture + dislocation

Radial Head - ORIF
• One / Two part articular fracture• Entire head – one piece
• Preserve head when possible

Radial Head – Excise / replace
Fracture < 25% Osteoporotic Extraarticular
Elbow stable Elbow Unstable
Excise Replace

Radial head – Fix / replace
• Operative repair / replacement - similar short term result ( 7 year)
• Limited size ( 23 pt .)

Do not excise without replacement
• Restore radial head • If not possible replace • Repair lateral collateral lig• Orif of coronoid

Safe Zone – Radial Heal ORIF
• Forearm neutral rotation – mark AP diameter radial head
• Safe zone – 65 deg. anterior and 45 deg. Posterior to this mark

Radial Head Fixation - Safe Zone

Radial head replacement
• Plane of radial head – 0.9 mm proximal to lateral edge of coronoid
• Preop x- rays of opposite elbow

Radial head replacement
• Overstuffing – early joint degeneration
• Understuffing – Valgus instability
• Intraop – visible ulnohumeral gap – suggests radial lengthening.


Coronoid fracture
• Classification
- Regan and Moorey
- O’ Driscoll

Coronoid Fracture – Regan & Moorey Classification
• Type 1 - # tip
• Type 2 - < 50 %
• Type 3 - >50%

Classification: Coronoid fractures•O’Driscoll Classification•Type I: tip•Type II: anteromedial facet•Type III: base

Coronoid fractures—nonoperative treatment
Type I
• Usually early motion
Type II
• Early motion, unless unstable
• Internal fixation if associated injuries

Coronoid fractures—surgical treatment
Type III
• Internal fixation
• Screw or anterior plate
• Reconstruction with bone bone graft (tip of olecranon)

Coronoid fracture – Associated condition
• Posteromedial rotatory instability
• Posterolateral rotatory instability
• Terrible triad
• Large fracture of olecranon

Test for posterolateral instability

• Large coronoid fracture- olecranon frac
dislocation
• Small transverse fracture – Terrible triad The average height 39 % ( 19% - 59 % )
• Anteromedial facet fracture – varus posteromedial

Coronoid fracture
• Small fragments – Type 1
• Fix with suture - #5 non absorbale suture



Type 1 & 2 – No fixationRepair / replacement of radial
head and LUCL complex – stable elbow

Coronoid fracture
• Type 2 ( < 50%)• Type 3 ( >50%)
Fix with screw passed from ulnar cortex
Large fragement – plate fixation – medial approach

Coronoid fracture
• Approach – lateral – Thru the fracture radial head
• Large fragment – separate medial approach

Lateral Collateral Ligament Complex
• Avulsed from lateral condyle along with common extensor
• Unstable elbow to varus test
• Local bruising

Lateral Collateral ligament
• Repair done elbow – 90 deg
• MCL intact forearm – pronated• MCL injured – forearm supinated

Lateral Collateral ligament
• Repair with suture anchors
• Transosseous tunnels

Medial Collateral ligament
• After repairing radial head • Coronoid • LCL
• Test elbow stability – Fluoroscopically
• Elbow unstable from 30 to 130 – repair MCL

Terrible Triad: Medial Instability ?
– Repair MCL– Reconstruct through bone tunnels• Suture Anchors• Palmaris autograft or allograft tendon
– Repair muscle origins Pronator
FCU
Nerve
Medial Epicondyle
FCUUlnar Nerve
Medial Epicondyle
Ulnohumeral joint reduced


Hanging arm test
• Check intraop stability of elbow• Elbow in full extension ,• forearm supinated• Bump under the arm

Hinge / static fixator
• After repairing radial head • Coronoid • LCL• MCL
Elbow still unstable – Hinge / static fixator
Ulnohumeral transfixation – inferior option



Hinge / static fixator
• Static fixator – removed at 3 weeks
• Hinge Fixator – remove at 6 – 8 weeks


Post op Rehabiliattion
• Position of immobilization• MCL intact &LCL repaired – 90 deg flexion /full
pronation• MCL & LCL repaired – splint in neutral
• LCL repaired & MCL unrepaired – 90 deg flexion and full supination

Post op Rehabiliattion
• Begin Range of motion - 2 – 5 days
• Stable arc of motion – intraop determined
• Resting splint – 6 weeks
• Night splint - 12 weeks



Complications
• Instability
• Failure of internal fixation
• Post traumatic stiffness
• Heterotopic ossification
• Post traumatic arthritis

32-year-old male, fell from roof
• Left elbow injury
• Neurovascular structure intact
• Closed injury
• Moderate swelling

CT scan

Approach
• Fix the coronoid? What technique?
• Radial head fix or replace?
• How do you repair collateral ligaments:– Drill holes or suture anchors
• What are the sequence of events for
treatment

Treatment• Posterior approach
• Pieced together radial head on back table
• Suture anchor in coronoid base
• Fix head to plate
• Weave sutures through LCL
• Run sutures in capsule over coronoid



Terrible Triad Injuries: Summary
• Not so Terrible– Isolated injury & cooperative patient– Stable repairs & motion
• Coronoid fixation• Radial head arthroplasty vs. ORIF• LCL repair
• Terrible– Poor stability after repairs complete– Multi-trauma
• ICU stay• Head injuries• Non-weight bearing on lower extremities
– Uncooperative patient

Summary
• Complex bony and soft-tissue injury
• Will lead to unstable elbow if not properly treated
• Requires coronoid process stability
• Radial head fixation or replacement
• LCL repair

Terrible Triad
• Only patients with INSTABILITY had CORONOID fractures (4 patients)

The “terrible triad”—coronoid fracture surgical technique
Access
• Lateral if radial head out
• Medial-over the top for direct repair
• Indirect percutaneous from subcutaneous ulna

The “terrible triad”—coronoid fracture surgical technique
Repair
• Anterior capsule may be captured by nonabsorbable sutures
• Screw or small plate

The “terrible triad”—radial head surgical technique
Repair or replace
• After coronoid repair
• May need to subluxate elbow to insert prosthesis

Final check for stability• Excessive valgus instability repair MCL
• If unstable in progressive extension or the fixation is tenuous
– Hinged external fixation
– Splint in flexion and plan staged capsular release

Radial Head fracture
• Mason Classification
• Hotchkiss modification