Swallowing Assessment
-
Upload
m0701453515 -
Category
Documents
-
view
66 -
download
7
Transcript of Swallowing Assessment

Swallowing Assessment in
Stroke Patients
Sharanya Kumar

Objectives
Why is it important?
NICE Guidelines Advice
Normal physiology of swallowing.
Pathophysiology of swallowing in
Stroke.
The Swallowing Assessment

Objectives
Why is it important?
NICE Guidelines Advice
Normal physiology of swallowing.
Pathophysiology of swallowing in
Stroke.
The Swallowing Assessment

Swallowing is often affected by stroke.
◦ The frequency of dysphagia has been documented to be as high as 81% in one study (1)
Dysphagia is a poor prognostic factor
◦ Therefore must be recognised early
Dysphagia in following stroke increases your risk of:
◦ Chest infection
◦ Aspiration Pneumonia
◦ Malnutrition
◦ Persistent Disability
◦ Prolonged Hospital Stay
◦ Institutionalisation on Discharge
◦ Mortality

Infection Post Stroke
Infection during the acute phase
following stroke reported in up to 40%
of patients (2)
Most common infection = Pneumonia
◦ Complicates 1 out of 3 cases of Acute
Stroke
◦ 50% of cases within first 48 hours of
admission
◦ Rest: all within the first 7 days of
admission

Why prevent infection?
Estimated 10% of deaths within 30
days of admission with stroke are due
to pneumonia (2)
Pneumonia is associated with poor
functional outcome at 3 months post
stroke
N.B. Dysphagia is a strong predictor
for Pneumonia

Prophylactic Antibiotics?
Currently there is no NICE guidance
recommendation for the use of
prophylactic antibiotics, as there is not
enough evidence proving its efficacy.

Evidence Base Van De Beek et al. 2009
Systematic review and meta – analysis of studies looking at preventative antibiotics for infections in acute stroke
Between 1996 – 2009: 4 RCTs were identified
Antibiotics regimens used:
◦ 2 : Fluoroquinolones
◦ 1: Tetracycline
◦ 1: Beta - lactam Abx + B - lactamase inhibitor
Therapy had to be started within 24 hours of stroke onset in all studies
The duration of antibiotic therapy varied between 3 and 5 days.

Results
Overall number of participants with infection: ◦ Significantly smaller in Antibiotic Group
NNT to prevent infection = 7
Mortality:
◦ Antibiotic group = 10 ( out of 210)
◦ Placebo / control = 13 (out of 216)
NNT to prevent death = 83
Van De Beek D et al. Preventive antibiotics for infections in acute stroke: a Systematic review and meta-analysis. Arch Neurol 2009;
66(9):1076-81.

Results
Van De Beek D et al. Preventive antibiotics for infections in acute stroke: a Systematic review and meta-analysis. Arch Neurol 2009;
66(9):1076-81.

Prophylactic Antibiotics?
Further evidence is required.
However, interestingly, there were no
complications with safety.

Choosing the right antibiotic for
prophylaxis
Needs to be effective against the common causative bacteria of aspiration pneumonia:
◦ Streptococcus pneumoniae
◦ Haemophilus Influenzae
◦ Staphyloccus aureus
◦ Enterbacteriaceae
Some antibiotics have been shown to also offer neuroprotective effects:
◦ Minocycline Reduces microglial activation
Inhibits apoptosis
◦ Ceftriaxone

Objectives
Why is it important?
NICE Guidelines Advice
Normal physiology of swallowing.
Pathophysiology of swallowing in
Stroke.
The Swallowing Assessment

Swallowing should be assessed by a trained Healthcare Professional
Before the patient takes any: ◦ Food
◦ Fluid (incl. water)
◦ Medications PO
Ideally within 24 hours of admission to hospital
Definitely within 3 days of admission to hospital

Objectives
Why is it important?
NICE Guidelines Advice
Normal physiology of swallowing.
Pathophysiology of swallowing in
Stroke.
The Swallowing Assessment

Swallowing “Process by which food and drink passes from the mouth to
stomach”
Complex series of neurologically controlled events.
Involves:
◦ Oral Cavity
◦ Pharynx
◦ Oesophagus
Allows individuals to SAFELY manage:
◦ Wide range of food and drink
◦ Varying volumes
◦ Varying textures
◦ Varying consistencies

Swallowing
Three main phases:
All reliant on both motor activity and sensory feedback

Real Time MRI
Normal Swallowing
http://upload.wikimedia.org/wikipedia/co
mmons/b/be/Real-time_MRI_-
_Swallowing_%28Pineapple_Juice%2
9.ogv

Swallowing – Oral Phase Function: Preparation of the bolus for safe transit.
Voluntary phase
Food and drink detected and recognised by taste, texture, consistency
◦ Cranial Nerve XI1
Lips and cheek muscles contract to retain food (orbicularis oris, buccinator)
◦ Cranial Nerve VII
Tongue manipulates food to aid mastication
Submental, Suprahyoid muscles at floor of mouth contract to elevate soft palate
◦ CN V, XII
At the end:
◦ Bolus is formed and held midline by tongue
◦ Then propelled towards the pharynx

Swallowing – Oral Phase
Therefore it requires functioning:
◦ Trigeminal Nerve
◦ Facial Nerve
◦ Glossopharyngeal Nerve
◦ Vagus Nerve (esp sup. Laryngeal branch)
◦ Hypoglossal Nerve
◦ Afferent fibres

Swallowing – Pharyngeal
Phase Function: Ensuring airway is protected during swallowing
Involuntary, Reflex
◦ Medulla – Swallowing Centre
Initiated by
◦ Backward movement of tongue (CNXII)
◦ Detection of bolus in pharynx
Series of well controlled, timed steps:
◦ Elevation of soft palate Therefore cannot enter nasal cavity
◦ Cessation of breathing & Closure of the airway Vocal cords in larynx draw together
◦ Opening of Upper Oesophageal Sphincter Upward forward movement of larynx
◦ Epiglottis closes over larynx Diverting food towards oesophagus
◦ Pharyngeal muscles contract Forcing food into oesophagus (CN X)

Swallowing – Pharyngeal
Phase Therefore it requires functioning:
◦ Medulla
◦ Vagus Nerve (esp the sup. Laryngeal branch)
◦ Hypoglossal Nerve
◦ Afferent fibres

Swallowing – Oesophageal
Phase Function Movement of bolus through
oesophagus into stomach
Active Transport ◦ Muscular contractions
◦ (Peristaltic waves)
Opening of Lower Oesophageal Sphincter ◦ Reflex on detection of bolus in oesophagus
Therefore requires functioning: ◦ Vagus Nerve
◦ Glossopharyngeal Nerve
◦ Sympathetic Nervous System

Objectives
Why is it important?
NICE Guidelines Advice
Normal physiology of swallowing.
Pathophysiology of swallowing in
Stroke.
The Swallowing Assessment

Dysphagia
“Any difficulty which disrupts the safe delivery of a food bolus to the stomach”
Either due to:
Structural dysfunction
Neurological dysfunction
N.B. Neurological Control is bilateral, therefore pathology may be unilateral / bilateral

Dysphagia
As the oral phase and pharyngeal phases are closely linked, dysphagia is commonly classified as being either:
Oropharyngeal Dysphagia ◦ Commonly due to nerve and muscle
pathology e.g. stroke
Oesophageal Dysphagia ◦ Commonly due to obstruction from
strictures / tumours

What can go wrong? Any Stroke lesion can affect swallowing, whether it be cerebral,
cortical, cerebellar or in the brain stem
Cerebral
◦ Interrupt voluntary control of mastication
◦ Bolus transport
◦ Cognitive impairment
Reduced concentration
Selective attention
Cortical Lesions (esp Pre Central Gyrus)
◦ Contralateral impairment in required facial / lip / tongue motor control
◦ Contralateral impairement of pharyngeal muscles required for peristalsis
Brain Stem
◦ Loss of sensation in mouth / tongue/ cheek
◦ Impaired timing of pharyngeal phase sequence
Laryngeal elevation, Closure of epiglottis etc

What can go wrong?
Oral Phase
◦ Sensory / Cognitive Disturbance Failure to detect material in mouth
◦ Motor Control Impairment Disrupting retention / preparation of bolus
Reduced power of muscles involved in mastication
Inappropriate drools / spills into unprepared
pharynx
Pharyngeal Phase
◦ Loss of sensation in pharynx Failure to initiate pharyngeal phase
Aspiration before swallow
◦ Incomplete closure of vocal cords Aspiration during swallow
◦ Incomplete elevation of larynx Failure to clear all material from pharynx
Aspiration after swallow
Oesophageal Phase
◦ Loss of Peristalsis

N.B.
Normally when you aspirate, you cough
to try and expel the material, however
loss of sensation can lead to a weak
cough / loss of coughing reflex:
Silent Aspiration

Objectives
Why is it important?
NICE Guidelines Advice
Normal physiology of swallowing.
Pathophysiology of swallowing in
Stroke.
The Swallowing Assessment

The Swallowing Assessment
Can be assessed by the bedside
Instrumental investigations can
provide more detailed information
Videofluroscopy is the gold standard
test for assessing swallowing

Bedside Swallowing
Assessment 1. Detailed History
From Patient and Care Giver
Onset
Duration
Severity (Solids / Liquids / Both)
Regurgitation, Coughing before / during / after swallow
Associated:
◦ Change in breathing pattern whilst eating
◦ Pain
◦ Hoarseness
◦ Weight Loss
Past Medical History
◦ Other causes, such as strictures secondary to GORD
Medications
◦ Certain drugs, such as anti-epileptics, can affect swallowing
SCREEN FOR RISK OF ASPIRATION

Risk of Aspiration
From: Kedlaya D, Brandstater ME. Swallowing, nutrition and hydration during acute stroke care. Top Stroke Rehabil 2002; 9 (2): 23 - 38

Bedside Swallowing
Assessment II. Examination
General Inspection
Gross Oro – Motor Examination
◦ Voice Quality Assessment
◦ Effect of compensatory strategies
Direct Test of Swallowing Safety

II. Examination
General Inspection
Posture (Able to sit up etc)
Cognitive Status
Ability to co – operate with test
Nutritional & Resp Status
Gross Oro – Facial Motor Assessment
Test Structure & Function & Sensation of Face, Lips, Tongue and Palate
Reflexes – abnormal gag reflex?
Reduced laryngo – pharyngeal sensation
Weak voluntary cough?
Wet Voice?

Safety of Swallow
1. Test with small sips of water
Monitoring for: ◦ Coughing
◦ Respiratory distress
◦ Voice changes
◦ Laryngeal movement
◦ Prolonged swallow
2. If no difficulties, test with larger volumes of water / yoghurt / normal foods
Monitoring as above.

Deemed Safe?
Yes
Watch oral intake and respiratory status for 48 hours.
Effort
Soft smooth diet
Referral to Speech and Language Therapy
Fail
NBM
Site NGT and request CXR to check site
Refer to Speech and Language Therapist for detailed assessment

Swallowing Assessment
Video of Swallowing Assessment from
SLT

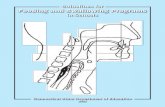
Videofluroscopy

VFS image illustrating the anatomy of the oropharynx.
Singh S , Hamdy S Postgrad Med J 2006;82:383-391
Copyright © The Fellowship of Postgraduate Medicine. All rights reserved.

Serial VFS images showing the normal passage of a barium bolus through the pharynx.
Singh S , Hamdy S Postgrad Med J 2006;82:383-391
Copyright © The Fellowship of Postgraduate Medicine. All rights reserved.

References 1. NICE. Diagnosis and Initial Management of Acute Stroke and
Transient Ischaemic Attack (TIA). Clinical Guidelines, CG68. Issued: July 2008
2. Ertekin C, Aydogdu I. Neurophysiology of Swallowing. Clin Neurophysiol. Dec 2003; 114 (12): 2226 – 44.
3. Kedlaya D, Brandstater ME. Swallowing, nutrition and hydration during acute stroke care. Top Stroke Rehabil 2002; 9 (2): 23 - 38
4. Ramsey DJC, Smithard DG, Kalra L. Early Assessments of Dysphagia and Aspiration Risk in Acute Stroke Patients;
5. Singh S, Hamdy S. Dysphagia in Stroke Patients [Review]. Postgrad Med J 2006; 82: 383 – 391
6. Palmer JB, Drennan JC, Baba M. Evaluation and Treatment of Swallowing Impairments. Am Fam Physician. 2000 Apr 15; 61 (8): 2453 – 2462
7. Blue Book
8. Van De Beek D et al. Preventive antibiotics for infections in acute stroke: a Systematic review and meta-analysis. Arch Neurol 2009; 66(9):1076-81.