STUDY GUIDE THE RESPIRATORY SYSTEM AND DISORDERS...Able to manage major lung diseases (TBC, asthma,...
Transcript of STUDY GUIDE THE RESPIRATORY SYSTEM AND DISORDERS...Able to manage major lung diseases (TBC, asthma,...


Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
2
STUDY GUIDE THE RESPIRATORY SYSTEM AND DISORDERS
Planners
Prof. Dr.dr.Ida Bagus Ngurah Rai, Sp.P
Dr. dr. I Made Muliarta, M.Kes
Prof. dr.Wiryana, Sp.An KIC
Prof.dr I Gusti Made Aman, Sp.FK
dr. Winarti, Sp.PA
Dr. dr. Desak Wihandani, M.Kes
dr. Putu Gede Sudira, Sp.S
Contributors
Prof. Dr. dr. Ida Bagus Ngurah Rai, SpP
dr. IGN Sri Wiryawan, M.Repro
dr. Gede Wardana, M.Biomed
Dr. dr. Dsk Made Wihandani, M.Kes
Dr. dr. Ida Bagus Subanada, Sp.A
dr. Dewa Artika, Sp.P
dr. Ida Bagus Suta, Sp.P
dr. Made Bagiada, Sp.PD-KP
Prof. dr I Gst. Md. Aman, Sp.FK
Dr. dr. Muliarta, M.Kes
dr. IGN Bagus Artana, Sp.PD
Dr. dr. Ketut Putu Yasa, Sp.BTKV
Dr. dr. Elysanti Martadiani, Sp.Rad
dr. Putu Ekawati, M.Repro, Sp.PA
dr. Aryabiantara, Sp.An KIC
dr.Putu Siadi Purniti, Sp.A
dr. Ayu Setyorini, Sp.A
dr. DGA Eka Putra, Sp.THT
dr. Luh Made Ratnawati, Sp.THT(KL)
dr. Putu Andrika, Sp.PD-KIC
dr. Gede Ketut Sajinadiyasa, Sp.PD
Prof. Dr. dr. Suardana, Sp.THT
Editors
dr. Putu Gede Sudira, Sp.S
dr. IGA Sri Darmayani, Sp.OG
Layout
Anak Agung Istri Sarastriyani Dewi
First Edition February 2017
All rights reserved. No part of this publication mayy be reproduced, stored in a retrieval system,
or transmitted in any form or by any means, electronic, mechanical, photocopying, recording, or
otherwise without prior written permission of the publisher.
Published by Department of Medical Education Medicine Programme, Faculty of Medicine,
Universitas Udayana.

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
3
CONTENTS
STUDY GUIDE THE RESPIRATORY SYSTEM AND DISORDERS ............................................... 2
CONTENTS........................................................................................................................................... 3
PREFACE ............................................................................................................................................. 5
GENERAL CURRICULUM RESPIRATORY SYSTEM AND DISORDERS .................................... 6
PLANNERS AND LECTURERS .......................................................................................................... 9
FACILITATORS .................................................................................................................................. 10
LEARNING ACTIVITY ........................................................................................................................ 11
IMPORTANT INFORMATIONS ......................................................................................................... 11
STUDENT PROJECT ......................................................................................................................... 12
ARTICLE REVIEW ASSESSMENT FORM ...................................................................................... 14
SELF ASSESSMENT ......................................................................................................................... 15
ASSESSMENT METHOD .................................................................................................................. 15
GENERAL TIME TABLE FOR A AND B CLASSES ........................................................................ 15
TIME TABLE OF CLASSES .............................................................................................................. 16
LEARNING PROGRAMS ................................................................................................................... 22
LECTURE 1......................................................................................................................................... 22
LECTURE 2......................................................................................................................................... 23
LECTURE 3......................................................................................................................................... 24
LECTURE 4......................................................................................................................................... 26
LECTURE 5......................................................................................................................................... 26
LECTURE 6......................................................................................................................................... 27
LECTURE 7......................................................................................................................................... 28
LECTURE 8......................................................................................................................................... 29
LECTURE 9......................................................................................................................................... 30
LECTURE 10 ...................................................................................................................................... 30
LECTURE 11 ...................................................................................................................................... 31
LECTURE 12 ...................................................................................................................................... 32
LECTURE 13 ...................................................................................................................................... 33
LECTURE 14 ...................................................................................................................................... 34

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
4
LECTURE 15 ...................................................................................................................................... 35
LECTURE 16 ...................................................................................................................................... 38
LECTURE 17 ...................................................................................................................................... 40
LECTURE 18 ...................................................................................................................................... 42
LECTURE 19 ...................................................................................................................................... 44
LECTURE 20 ...................................................................................................................................... 44
BASIC CLINICAL SKILLS .................................................................................................................. 47
REFERENCES ................................................................................................................................... 50
CURRICULUM MAP........................................................................................................................... 51

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
5
PREFACE
The medical curriculum has become increasingly vertically integrated, with stronger basic
concept and support by clinical examples and cases to help in the understanding of the
relevance of the underlying basic science. Basic science concepts may help in the
understanding of the pathophysiology and treatment of diseases. Respiratory system and
disorders block has been written to take account of this trend, and to integrate core aspects of
basic science, pathophysiology and treatment into a single, easy to use revision aid.
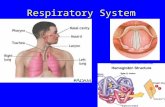
The respiratory system consists of a pair of lungs within the thoracic cage. Its main
function is gas exchange, but other roles include speech, filtration of microthrombin arriving from
systemic veins and metabolic activities such as conversion of angiotensin I to angiotensin II and
removal or deactivation of serotonin, bradykinin, norepinephrine, acetylcholine and drugs such
as propranolol and chlorpromazine. So this block will discuss about anatomy, histology,
symptom and signs of lung disease and its pathophysiology, major upper respiratory diseases,
major lung diseases, major pediatric lung disease, and basic principle concept to education,
prevention, treatment and rehabilitation in respiratory system disorder in patient, family and
community.
The learning process will be carried out for 4 weeks (20 working days) starts from 20th of
February 2017 as shown in the time table. The final examination will be conducted on 30th of
March 2017 in the form of MCQ. The learning situation include lecture, individual learning, small
group discussion, plenary session, practice, and clinical skills.
Most of the learning material should be learned independently and discuss in SGD by the
students with the help of facilitator. Lecture is given to emphasize the most important thing of
the material. In small group discussion, the students gave learning task to lead their discussion.
This simple study guide need more revision in the future, so that the planners kindly invite
readers to give any comments and critics for its completion. Thank you.
Planners

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
6
GENERAL CURRICULUM RESPIRATORY SYSTEM AND DISORDERS
Aims:
Comprehend the structure, physiologic, and pathologic of the respiratory system. Interpret the laboratory and imaging examination of the respiratory system disorders. Diagnose and treat the patient with common respiratory system disorders. Plan education, prevention, management and rehabilitation of respiratory system
disorders to patient, family and community.
Learning outcomes:
Concern about the size of problem and diversity of respiratory disease in the community.
Able to describe the structure and function of the respiratory system. Able to interpret the result of examination (physical, laboratory, function test, blood gas
analysis and chest imaging). Able to explore patients with respiratory problem (runny nose, cough, dyspnea, non
cardiac chest pain, hemoptysis). Able to manage major upper respiratory diseases (tonsillitis, rhinitis, sinusitis). Able to manage major lung diseases (TBC, asthma, COPD, lung cancer, pneumonia,
occupational lung disease, pleural disease) on patient, family and community. Able to manage major pediatric lung disease (bronchiolitis, TB, asthma). Able to implement DOTS program against TB. Able to implement the strategy of smoking cessation, especially in patient with
respiratory disease.
Curriculum contents:
Structural and function of the respiratory system. Physiology of lung in related with oxygen consumption and acid base balance. Symptoms and signs of lung disease. Pathophysiology of respiratory system disorders. Basic physical, laboratory and imaging examination. Interpretation of examination results. Drugs that commonly used in respiratory system disorders (decongestant, anti-asthma &
bronchodilators, antitussive, expectorant. Basic principle concept to education, prevention, treatment and rehabilitation in
respiratory system disorders in patient, family and community.
Curriculum structure:
Structure of curriculum mainly is derive from general competences of Indonesian general
practioner. Those competences in diagnosing diseases and doing clinical skills should be
mastered by all the general practioners here. Local values of our institutions are also considered
as added values in this curriculum.

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
7
No Daftar Penyakit sesuai SKDI 2012 Tingkat Kemampuan 1 Influenza 4A 2 Pertusis 4A 3 Acute Respiratory distress syndrome (ARDS) 3B 4 SARS 3B 5 Flu burung 3B
Laring dan Faring 6 Faringitis 4A 7 Tonsilitis 4A 8 Laringitis 4A 9 Hipertrofi adenoid 2 10 Abses peritonsilar 3A 11 Pseudo-croop acute epiglotitis 3A 12 Difteria (THT) 3B 13 Karsinoma laring 2 14 Karsinoma nasofaring 2
Trakea 15 Trakeitis 2 16 Aspirasi 3B 17 Benda asing 2
ParuParu 18 Asma bronkial 4A 19 Status asmatikus (asma akut berat) 3B 20 Bronkitis akut 4A 21 Bronkiolitis akut 3B 22 Bronkiektasis 3A 23 Displasia bronkopulmonar 1 24 Karsinoma paru 2 25 Pneumonia, bronkopneumonia 4A 26 Pneumonia aspirasi 3B 27 Tuberkulosis paru tanpa komplikasi 4A 28 Tuberkulosis dengan HIV 3A 29 Multi Drug Resistance (MDR) TB 2 30 Pneumothorax ventil 3A 31 Pneumothorax 3A 32 Efusi pleura 2 33 Efusi pleura masif 3B 34 Emfisema paru 3A 35 Atelektasis 2 36 Penyakit Paru Obstruksi Kronik (PPOK) eksaserbasi akut 3B 37 Edema paru 3B 38 Infark paru 1 39 Abses paru 3A 40 Emboli paru 1 41 Kistik fibrosis 1 42 Haematothorax 3B 43 Tumor mediastinum 2 44 Pnemokoniasis 2 45 Penyakit paru intersisial 1 46 Obstructive Sleep Apnea (OSA) 1

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
8
No Keterampilan Klinis sesuai SKDI 2012 Tingkat Keterampilan
PEMERIKSAAN FISIK
1 Inspeksi leher 4A
2 Palpasi kelenjar ludah (submandibular, parotid) 4A
3 Palpasi nodus limfatikus brakialis 4A
4 Palpasi kelenjar tiroid 4A
5 Rhinoskopi posterior 3
6 Laringoskopi, indirek 2
7 Laringoskopi, direk 2
8 Usap tenggorokan (throat swab) 4A
9 Oesophagoscopy 2
10 Penilaian respirasi 4A
11 Inspeksi dada 4A
12 Palpasi dada 4A
13 Perkusi dada 4A
14 Auskultasi dada 4A
PEMERIKSAAN DIAGNOSTIK
15 Persiapan, pemeriksaan sputum, dan interpretasinya
(Gram dan Ziehl Nielsen [BTA]) 4A
16 Pengambilan cairan pleura (pleural tap) 3
17 Uji fungsi paru/spirometri dasar 4A
18 Tes provokasi bronkial 2
19 Interpretasi Rontgen/foto toraks 4A
20 Ventilation Perfusion Lung Scanning 1
21 Bronkoskopi 2
22 ip)B superfisial 2
23 Trans thoracal needle aspiration (TINA) 2
TERAPEUTIK
24 Dekompresi jarum 4A
25 Pemasangan WSD 3
26 Ventilasi tekanan positif pada bayi baru lahir 3
27 Perawatan WSD 4A
28 Pungsi pleura 3
29 Terapi inhalasi/nebulisasi 4A
30 Terapi oksigen 4A
31 Edukasi berhenti merokok 4A

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
9
PLANNERS AND LECTURERS
No Name Department Phone
1 Prof. Dr. dr. Ida Bagus Ngurah Rai, Sp.P
(Coordinator) Pulmonology 08123804579
2 Dr. dr. I Made Muliarta, M.Kes (Secretary) Physiology 081338505350
3 Prof. dr. Wiryana, Sp.An KIC (member) Anaesthesiology 0811392171
4 Prof. dr I Gst. Md. Aman, SpFK (member) Pharmacology 081338770650
5 dr.Winarti, Sp.PA (member) Pathology Anatomy 08123997328
6 Dr. dr. Desak Wihandani, M.Kes (member) Biochemistry 081338776244
7 dr. Putu Gede Sudira, Sp.S (member) DME 081805633997
8 dr. I GN Sri Wiryawan, M.Repro Histology 08123925104
9 dr. Gede Wardana, M.Biomed Anatomy 0361-7864957
10 Dr. dr. Ida Bagus Subanada, Sp.A Paediatric Dept. 0812399533
11 dr. Dewa Artika, Sp.P Pulmonology 08123875075
12 dr. Ida Bagus Suta, Sp.P Pulmonology 08123990362
13 dr. Made Bagiada, Sp.PD-KP Pulmonology 08123607874
14 dr. IGN Bagus Artana, Sp.PD Pulmonology 08123994203
15 Dr. dr. Ketut Putu Yasa, Sp.BTKV Thorax surgery 08123843260
16 Dr. dr. Elysanti Martadiani, Sp.Rad Radiology 08123807313
17 dr. Putu Ekawati, M.Repro, Sp.PA Pathology Anatomy 08123958158
18 dr. Aryabiantara, Sp.An KIC Anaesthesiology 08123822009
19 dr. Putu Siadi Purniti, Sp.A Paediatric 08123812106
20 dr. Ayu Setyorini, Sp.A Paediatric 081353286780
21 dr. DGA Eka Putra, Sp.THT Otorhinolaryngology 0813387826317
22 dr. Luh Made Ratnawati, Sp.THT(KL) Otorhinolaryngology 08123806108
23 dr. Putu Andrika, Sp.PD-KIC Pulmonology 08123989192
24 dr. Gede Ketut Sajinadiyasa, Sp.PD Pulmonology 085237068670
25 Prof. Dr. dr. Suardana, Sp.THT Otorhinolaryngology 0811385299

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
10
FACILITATORS
Regular Class (Class A)
No Name Group Departement Phone Venue
(2ndfloor)
1 dr Muliani M.Biomed A1 Anatomy 085103043575 3rd floor: R.3.09
2 dr IA Dewi Wiryanthini M.Biomed
A2 Biochemistry 081239990399 3rd floor: R.3.10
3 dr Ni Putu Wardani M.Biomed Sp.An
A3 DME 08113992784 3rd floor: R.3.11
4 dr I Kadek Swastika M.Kes A4 Parasitology 08124649002 3rd floor: R.3.12
5 dr I Putu Adiartha Griadhi M.Fis
A5 Physiology 081999636899 3rd floor: R.3.13
6 dr Putu Aryani MPH A6 Public Health 082237285856 3rd floor: R.3.14
7 dr Ni Putu Ekawati M.Repro Sp.PA
A7 Pathology of Anatomy
08113803933 3rd floor: R.3.15
8 dr Ni Nyoman Metriani Nesa Sp.A M.Sc
A8 Pediatry 081337072141 3rd floor: R.3.16
9 dr Ni Made Ayu Surasmiati M.Biomed Sp.M
A9 Ophtalmology 081338341860 3rd floor: R.3.17
10 dr.IGAA.Dwi Karmila,SpKK A10 Dermatovenerology
08123978446 3rd floor: R.3.19
English Class (Class B)
No Name Group Departement Phone Venue
(2ndfloor)
1 dr Putu Gede Sudira Sp.S B1 DME 081805633997 3rd floor: R.3.09
2 Dr rer nat dr Ni Nyoman Ayu Dewi M.Kes
B2 Biochemistry 081337141506 3rd floor: R.3.10
3 dr IGA Dewi Ratnayanti M.Biomed
B3 Histology 085104550344 3rd floor: R.3.11
4 dr NN Dwi Fatmawati Sp.MK PhD
B4 Microbiology 087862200814 3rd floor: R.3.12
5 dr Agung Nova Mahendra M.Sc
B5 Pharmacology 087861030195 3rd floor: R.3.13
6 dr I Wayan Juli Sumadi Sp.PA
B6 Pathology of Anatomy
082237407778 3rd floor: R.3.14
7 Dr dr IBG Fajar Manuaba Sp.OG MARS
B7 Obsgyn 081558101719 3rd floor: R.3.15
8 dr Dewa Gede Mahiswara S Sp.Rad
B8 Radiology 08123846307 3rd floor: R.3.16
9 dr I Made Putra Swi Antara Sp.JP FIHA
B9 Cardiology 08123804782 3rd floor: R.3.17
10 dr Kumara Tini Sp.S FINS B10 Neurology 081238701081 3rd floor: R.3.19

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
11
LEARNING ACTIVITY
There are several types of learning activity:
Lecture
Plenary session
Independent learning based on the lecture’s topic
Small group discussion to solve the learning task
Practicing
Student project
Clinical skill and demonstration
Self assessment at the end of every topic
Lecture will be held at room 3.01 (3rd floor), while discussion rooms available at 3rd floor
(room A309-A317, A319).
IMPORTANT INFORMATIONS
Meeting of the students’ representative
In the middle of block schedule, a meeting is designed among the student representatives
of every small group discussions, facilitators, and resource persons. The meeting will discuss
the ongoing teaching learning process, quality of lecturers and facilitators as a feedback to
improve the next process. The meeting will be taken based on schedule from Medical Education
Unit.

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
12
STUDENT PROJECT
Title of student project
Group discussion Topic
A1
A2
A3
A4
A5
A6
A7
A8
A9
A10
B1
B2
B3
B4
B5
B6
B7
B8
B9
B10
About Topic, Presentation’s place and schedules, Task rules, Assessment, and Evaluator will
be discussed at lecture of block introduction 20th February 2017.

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
13
TITLE
(subject/ topic: choose from compentency list)
Name
NIM
Faculty of Medicine, Udayana University
2017
______________
1. Introduction (Pendahuluan)
2. Content (Isi, sesuai topik yang dibahas)
3. Summary (Ringkasan)
4. Refferences: (Daftar Pustaka) Van Couver style
Example:
Journal
Sheetz MJ, King GL. Molecular understanding of hyperglycemia’s adverse effect for
diabetic complications. JAMA. 2002;288:2579-86.
Textbook
Libby P. The Pathogenesis of atherosclerosis. In: Braunwald E, Fauci A, Kasper D,
Hoster S, Longo D, Jamason S (eds). Harrison’s principles of internal medicine. 15th ed.
New York: McGraw Hill; 2001. p. 1977-82.
Internet
WHO. Obesity: preventing and managing the global epidemic. Geneva: WHO 1998.
[cited 2005 July]. Available from:
http://www.who.int/dietphysicalactivity/publications/facts/ obesity/en.
6 – 10 pages, 1.5 space, Times new romance 12

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
14
ARTICLE REVIEW ASSESSMENT FORM
Faculty of Medicine, Udayana University
___________________________________________________________________________
Block : Respiratory System and Disorders
Name : ________________________________________
Student No. (NIM) : ________________________________________
Facilitator : ________________________________________
Title :
__________________________________________________
__________________________________________________
Time table of consultation
Point of discussion Week Date Tutor sign
1. Title 1
2. Refferences 1
3. Outline of paper 2
4. Content 3
5. Final discussion 4
Assessment
A. Paper structure : 7 8 9 10
B. Content : 7 8 9 10
C. Discussion : 7 8 9 10
Total point : ( A + B + C ) : 3 = _____________
Denpasar, ______________________
Facilitator,

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
15
SELF ASSESSMENT
Self assessment of each lecture will be given after each lecture session, and will be
marked. This mark can determine whether the student pass this block or not. Any final mark
between 62 - 64 will be reconsidered with self assessment’s mark to see the student’s status.
Any student with self assessment’s mark 65 or more will pass this block. And for the lower one
will have to attend the remedial examination. It is important to do this self assessment
cautiously, because this activity may be your ticket to pass this block just at first examination.
ASSESSMENT METHOD
Assessment in this theme consists of:
SGD : 5%
Final Exam : 80%
Student Project : 15%
Final mark 65 or more considered to pass this block. Certain conditions applied for those
with final mark between 62 – 64. These students will be analyzed using their self assessment’s
mark. Students with final mark 62 – 64 and self assessment’s mark equal or more than 65 will
also considered pass this block. The value of marking:
A ≥ 80
B+ >70-79
B 65-70
GENERAL TIME TABLE FOR A AND B CLASSES
CLASS A CLASS B
TIME ACTIVITIES TIME ACTIVITIES
08.00-09.00 Lecture 09.00-10.00 Lecture
09.00-10.30 Independent learning 10.00-11.30 Student project
10.30-12.00 SGD 11.30-12.00 Break
12.00-12.30 Break 12.00-13.30 Independent learning
12.30-14.00 Student project 13.30-15.00 SGD
14.00-15.00 Plenary session 15.00-16.00 Plenary session

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
16
TIME TABLE OF CLASSES
DAY/DATE Class A Class B ACTIVITY VENUE PIC
1
Monday
Feb 20,
2017
08.00-08.30 09.00-09.30 Introduction Class room Prof.I.B. Rai
08.30-09.00 09.30-10.00
Lecture 1 Anatomy of
Respiratory System
Class room dr.Wardana
09.30-10.30 12.00-13.30 Independent learning
10.30-12.00 13.30-15.00 SGD Disc room Facilitator
12.00-12.30 11.30-12.00 Break
12.30-14.00 10.30-11.30 Student project
14.00-15.00 15.00-16.00 Plenary session Class room dr.Wardana
2
Tuesday
Feb 21,
2017
08.00-09.00 09.00-10.00
Lecture 2 Histology of
Respiratory System
Class room
dr. Sri
Wiryawan
09.00-10.30 12.00-13.30 Independent learning
10.30-12.00 13.30-15.00 SGD Disc room Facilitator
12.00-12.30 11.30-12.00 Break
12.30-14.00 10.00-11.30 Student project
14.00-15.00 15.00-16.00 Plenary session Class room dr. Sri
Wiryawan
3
Wednesda
y
Feb 22,
2017
08.00-09.00 09.00-10.00
Lecture 3 Physiology of
Respiratory System:
Ventilation
Class room dr. Muliarta
09.00-10.30 12.00-13.30 Independent learning
10.30-12.00 13.30-15.00 SGD Disc room Facilitator
12.00-12.30 11.30-12.00 Break
12.30-14.00 10.00-11.30 Student project
14.00-15.00 15.00-16.00 Plenary session Class room dr. Muliarta
4
Thursday
Feb 23,
2017
08.00-09.00 09.00-10.00
Lecture 4 Physiology of
Respiratory System:
Gas Exchange, diving,
altitude
Class room dr. Muliarta
09.00-15.00 10.00-16.00
Independent learning
Practice:
Anatomy, Histology
Anatomy: 1st
floor
dr. Wardana
Histology: 4th
floor
dr. Sri
Wiryawan

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
17
5
Friday
Feb 24,
2017
08.00-09.00 09.00-10.00
Lecture 5 Carriage of oxygen and
Carbon dioxide
Class room dr. Desak
Wihandani
09.00-10.30 12.00-13.30 Independent learning
10.30-12.00 13.30-15.00 SGD Disc room Facilitator
12.00-12.30 11.30-12.00 Break
12.30-14.00 10.00-11.30 Student project
14.00-15.00 15.00-16.00 Plenary session Class room dr. Desak
Wihandani
6
Monday
Feb 27,
2017
08.00-09.00 09.00-10.00
Lecture 6 Control of acid base
balance, Arterial Gas
Analysis (AGA)
Class room dr. Desak
Wihandani
09.00-10.30 12.00-13.30 Independent learning
10.30-12.00 13.30-15.00 SGD Disc room Facilitator
12.00-12.30 11.30-12.00 Break
12.30-14.00 10.00-11.30 Student project
14.00-15.00 15.00-16.00 Plenary session Class room dr. Desak
Wihandani
7
Tuesday
Feb 28,
2017
08.00-09.00 09.00-10.00
Lecture 7 Control of Respiratory
Function and Blood
Gas Analyzes
Class room dr. Arya
Biantara
09.00-10.30 12.00-13.30 Independent learning
10.30-12.00 13.30-15.00 SGD Disc room Facilitator
12.00-12.30 11.30-12.00 Break
12.30-14.00 10.00-11.30 Student project
14.00-15.00 15.00-16.00 Plenary session Class room Prof. Wiryana
8
Wednesda
y
March 1,
2017
08.00-09.00 09.00-10.00
Lecture 8 Pathology of
Respiratory Tract
Class room dr. Ekawati
09.00-10.30 12.00-13.30 Independent learning
10.30-12.00 13.30-15.00 SGD Disc room Facilitator
12.00-12.30 11.30-12.00 Break
12.30-14.00 10.00-11.30 Student project Hospital Visit
14.00-15.00 15.00-16.00 Plenary session Class room dr. Ekawati
9
Thursday
March 2,
2017
08.00-09.00 09.00-10.00
Lecture 9 Lung Defense
Mechanism
Class room dr. Ekawati
09.00-15.00 10.00-16.00
Independent learning
Practice : Physiology,
Pathology Anatomy (PA)
Physiology:
2nd floor dr. Muliarta
PA: Joint Lab
(4th floor) dr. Ekawati

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
18
10
Friday
March 3,
2017
08.00-09.00 09.00-10.00
Lecture 10
Pharmacological and
non pharmacological
interventions
Class room Prof. Aman
09.00-10.30 12.00-13.30 Independent learning
10.30-12.00 13.30-15.00 SGD Disc room Facilitator
12.00-12.30 11.30-12.00 Break
12.30-14.00 10.00-11.30 Student project
14.00-15.00 15.00-16.00 Plenary session Class room Prof. Aman
11
Monday
March 6,
2017
08.00-09.00 09.00-10.00
Lecture 11
Pharmacological and
non pharmacological
interventions
Class room
Prof. Aman
09.00-10.30 12.00-13.30 Independent learning
10.30-12.00 13.30-15.00 SGD Disc room Facilitator
12.00-12.30 11.30-12.00 Break
12.30-14.00 10.00-11.30 Student project Hospital Visit
14.00-15.00 15.00-16.00 Plenary session Class room Prof. Aman
12
Tuesday
March 7,
2017
08.00-09.00 09.00-10.00 Lecture 12
Respiratory Imaging Class room dr. Elysanti
09.00-10.30 12.00-13.30 Independent learning
10.30-12.00 13.30-15.00 SGD Disc room Facilitator
12.00-12.30 11.30-12.00 Break
12.30-14.00 10.00-11.30 Student project Hospital Visit
14.00-15.00 15.00-16.00 Plenary session Class room dr. Elysanti
13
Wednesda
y
March 8,
2017
08.00-09.00
09.00-10.00
09.00-10.00
10.00-11.00
Lecture 13
Bronchiolitis, asthma in
children, Pneumonia,
Bronkopneumonia,
Class room
dr. IB
Subanada
dr. Ayu
Setyorini
10.00-11.30 12.00-13.30 Independent learning
11.30-13.00 13.30-15.00 SGD Disc room Facilitator
13.00-13.30 11.30-12.00 Break
13.30-14.00 11.00-11.30 Student project
14.00-15.00 15.00-16.00 Plenary session Class room dr. IB
Subanada
14
Thursday
March 9,
2017
08.00-09.00
09.00-10.00
09.00-10.00
10.00-11.00
Lecture 14 Aspiration Pneumonia,
Pertusis
TB in children, Difteri
Class room
dr. Ayu
Setyorini
dr. Siadi
Purniti
10.00-11.30 12.00-13.30 Independent learning
11.30-13.00 13.30-15.00 SGD Disc room Facilitator
13.00-13.30 11.30-12.00 Break
13.30-14.00 11.00-11.30 Student project
14.00-15.00 15.00-16.00 Plenary session Class room dr. Siadi
Purniti

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
19
15
Friday
March 10,
2017
08.00-09.00
09.00-10.00
09.00-10.00
10.00-11.00
Lecture 15
Pulmonary TB and
Extrapulmonary TB,
TB in the
Immunocompromised
Host, Abses TB
Class room
dr. Sutha,
dr. Bagiada
10.00-11.30 12.00-13.30 Independent learning
11.30-13.00 13.30-15.00 SGD Disc room Facilitator
13.00-13.30 11.30-12.00 Break
13.30-14.00 11.00-11.30 Student project Hospital Visit
14.00-15.00 15.00-16.00 Plenary session Class room dr. Sutha,
dr. Bagiada
16
Monday
March 13,
2017
08.00-09.00 09.00-10.00
Lecture 16
Asthma,
COPD
Class room
Prof. IB Rai,
dr. Artana
09.00-10.30 12.00-13.30 Independent learning
10.30-12.00 13.30-15.00 SGD Disc room Facilitator
12.00-12.30 11.30-12.00 Break
12.30-14.00 10.00-11.30 Student project
14.00-15.00 15.00-16.00 Plenary session Class room Prof. IB Rai,
dr. Artana
17
Tuesday
March 14,
2017
08.00-09.00
09.00-10.00
09.00-10.00
10.00-11.00
Lecture 17
Pleural effusion,
Emfisema, edema paru
Pneumothorax,
Hematothorax
Class room
dr. Andrika,
dr, Yasa
10.00-11.30 12.00-13.30 Independent learning
11.30-13.00 13.30-15.00 SGD Disc room Facilitator
13.00-13.30 11.30-12.00 Break
13.30-14.00 11.00-11.30 Student project
14.00-15.00 15.00-16.00 Plenary session Class room dr. Andrika,
dr, Yasa
18
Wednesda
y
March 15,
2017
08.00-09.00
09.00-10.00
08.00-09.00
09.00-10.00
Lecture 18
Bronchitis and
Bronchiectasis,
Lung Ca and Education
of Smoking Cessation
Class room
dr.IB Suta,
dr. Saji
10.00-11.30 12.00-13.30 Independent learning
11.30-13.00 13.30-15.00 SGD Disc room Facilitator
13.00-13.30 11.30-12.00 Break
13.30-14.00 10.00-11.30 Student project
14.00-15.00 15.00-16.00 Plenary session Class room
dr.IB Suta,
dr. Saji

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
20
19
Thursday
March 16,
2017
08.00-08.30
08.30-09.00
09.00-09.30
09.30-10.00
Lecture 19
Disorder of nose,
sinus, Nose foreign
Bodies
Class room
dr. Ratna,
Sp.THT
09.00-10.30 12.00-13.30 Independent learning
10.30-12.00 13.30-15.00 SGD Disc room Facilitator
12.00-12.30 11.30-12.00 Break
12.30-14.00 10.00-11.30 Student project Hospital Visit
14.00-15.00 15.00-16.00 Plenary session Class room dr. Ratna,
Sp.THT
20
Friday
March 17,
2017
08.00-09.00 08.00-09.00
Lecture 20
Disorder of larynx,
Disorder of Pharynx,
Throat foreign bodies
Class room
Prof.
Suardana, dr.
Dewa Artha
Eka Putra,
Sp.THT
09.00-10.30 09.00-10.30 Independent learning
10.30-12.00 10.30-12.00 SGD Disc room Facilitator
12.00-12.30 12.00-12.30 Break
12.30-14.00 12.30-14.00 Student project Hospital Visit
14.00-15.00 14.00-15.00 Plenary session Class room
Prof.
Suardana, dr.
Dewa Artha
Eka Putra,
Sp.THT
21
Monday
March 20,
2017
08.00-15.00 08.00-15.00
BCS: Physical diagnostic
examination of Thorax’s in
adult patients
BCS: Radio Imaging
BCS: Pemasangan dan
Perawatan WSD
(Pre-test, lecture, demo
Practice, discussion)
Physiology
Dept. (2nd
floor
Joint Lab
(4th Floor)
Anatomy (1st
floor)
Dr. Saji
dr. Elysanti
dr. Yasa
22
Tuesday
March 21,
2017
08.00-15.00 08.00-15.00
BCS: Spirometri
BCS: Pengambilan cairan
Pleura, Punksi, Dekompresi
jarum
BCS: Nebulisasi dan terapi
oksigen
(Pre-test, Lecture, practice,
demo)
Physiology
Dept. (2nd
floor
Joint Lab (4th
Floor)
Anatomy (1st
floor)
dr. Muliarta
dr. Yasa
dr. Arya
Biantara

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
21
23
Wednesda
y
March 22,
2017
08.00-15.00 08.00-16.00
BCS: Radio imaging
BCS: Physical diagnostic
examination of Thorax’s in
baby-children patients
BCS: Physical diagnostic
examination of Thorax’s in
adult patients
(Pre-test, lecture, practice,
demo)
Physiology
Dept. (2nd
floor
Joint Lab (4th
Floor)
Anatomy (1st
floor)
dr. Elysanti
dr. Ayu
Setyorini
dr. Saji
24
Thursday
March 23,
2017
08.00-15.00 08.00-16.00
BCS: Bronchoscopy,
Provocation test, Radio
Imaging
BCS: CPEP pada Bayi
BCS: Physical diagnostic
examination of Thorax’s in
adult patients
(Pre-test, lecture, demo)
Physiology
Dept. (2nd
floor
Joint Lab (4th
Floor)
Anatomy (1st
floor)
dr Artana
dr. Elysanti
dr. Arya
Biantara
dr. Saji
25
Friday
March 24,
2017
08.00-15.00 08.00-16.00
BCS: Physical diagnostic
examination of Thorax’s in
baby-children patients
BCS: Perawatan WSD,
Decompresi Jarum
BCS: Rhinoskopi Posterior
(Practice, post-test)
Physiology
Dept. (2nd
floor
Joint Lab (4th
Floor)
Anatomy (1st
floor)
dr. Ayu
Setyorini
dr. Yasa
THT staff
26
Thursday
March 30,
2017
Examination
27
Thursday
Jule 27,
2017
Remidial
Examination
Class Room : R. 3.01 (3rd Floor)

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
22
LEARNING PROGRAMS
LECTURE 1
ANATOMY OF RESPIRATORY TRACT
dr. I Nyoman Gede Wardana, M.Biomed
The respiratory system consists of conducting zone and respiratory zone. Conducting
zone, whose walls are too thick to permit exchange of gases between the air in the tube and the
blood stream. The nostrils (nares), nasal cavity, pharynx, larynx, trachea, bronchi, and terminal
bronchioles are included in this zone. Respiratory zone, whose walls are thin enough to permit
exchange of gases between tube and blood capillaries surrounding them. Air travels to the
lungs through that zone. The right lung divided into three lobes: superior, middle, and inferior.
The left lung divided into two lobes: superior and inferior. Each lung cover by a membrane that
called pleura. Both lungs are inside the thoracic cage. The thoracic cage is formed by the
vertebral column behind, the ribs, and intercostal spaces on other side and the sternum and
costal cartilages in front. Below it separated from the abdominal cavity by diaphragm
Learning Task
Vignette 1:
Kesawa, 32 years old, was seen in the clinic ten days ago, was diagnosed with rhinitis and sent
home with instructions for increased fluids, decongestants, and rest. Kesawa presents today
with worsened symptoms of malaise, low-grade temperature, nasal discharge, night time
coughing, mouth breathing, early morning pain over sinuses, and congestion. The doctor
diagnose he is suffering sinusitis.
1. Describe the boundaries of the nasal cavity and its blood supply! 2. Describe the paranasal sinuses and its opening at nasal cavity!
Vignette 2: Gotawa, a singer-18 years old came to clinic with complain a hoarse voice for 3 days. She also suffers sore throat, nose block, and fever. She was diagnosed laryngitis
1. Describe the structure of larynx and location of vocal cord! 2. Describe the intrinsic and extrinsic muscle of larynx!
Vignette 3: Mande, 30 years old male came to clinic with chief complaint difficulty to breath start from this morning. He also suffers cough, runny nose and fever. He has history bronchial asthma when he was 2 years old. The doctor diagnose he is suffering bronchial asthma.
1. Describe the structure of trachea! 2. Describe the different between right and left main bronchus! 3. Describe the principal different between trachea, bronchi, and bronchioles!
Vignette 4:
A 57-year-old male is admitted to the hospital with a chief complaint of shortness of breath for 2
weeks. The radiology examination shows a large left-side pleural effusion.
1. Describe the different between right lung and left lung! 2. Describe the structure of pleura! 3. Describe the structure of thoracic wall!

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
23
LECTURE 2
HISTOLOGY OF RESPIRATORY TRACT
dr. Sri Wiryawan, M.Repro
The lower respiratory tract consists of: the lower part of the trachea, the two main
bronchi, lobar, segmental, and smaller bronchi, bronchioles and terminal bronchioles, and last
but not least is the end respiratory unit. These structure make up the tracheobronchial tree. As
for the structure distal to the main bronchi along with a tissue known as the lung parenchyma.
There are several structure we should also understand, when talking about lower
respiratory tract. Several structures such as thorax, mediastinum, pleurae and pleural cavity,
and lung. Thorax especially thoracic cavity and thoracic wall protect our lung and mediastinum
and also play an important role in respiratory process. The mediastinum, which has a role in
protecting our heart , located between the two lungs, and contains the heart and great vessels,
trachea and esophagus, phrenic and vagus nerves, and lymph nodes.
The pleurae covers the external surface of the lung, and is then reflected to cover the
inner surface of thoracic cavity. Pleurae divided into the visceral (lines the surface of the lung)
and parietal (lines the thoracic wall and diaphragm) one. The space between these two pleurae
called as pleural cavity which contains a thin film fluid to allow the pleurae to slip over each
other during breathing.
The lungs are placed within the thoracic cavity. The lungs contain airways structure,
vessels, lymphatic and lymph nodes, nerves, and supportive connective tissue. The trachea
divides and form the left and right primary bronchi, which in turn divide to form lobar bronchi.
Each lobar bronchi divide again to give segmental bronchi to supply air to bronchopulmonary
segments. The tracheobronchial tree can also be classified into two functional zones: the
conducting zone (proximal to the respiratory bronchioles) which involved in air movement, and
the respiratory zone (distal to the terminal bronchioles) which involved in gaseous exchange.
The other term to show functional structure of the lower respiratory tract is the acinus.
The acinus defined as the part of the airway that is involved in gaseous exchange. The acinus
consist of respiratory bronchioles, alveolar ducts, and alveoli as the smallest functional structure
of the lung. The areas of lung containing groups of between three to five acini surrounded by
parenchimal tissue are called lung lobules.
The alveolus is an blind-ending terminal sac of respiratory tract. Most gaseous exchange
occurs in the alveoli. The alveoli are lined with type I (structural) and type II (produce surfactant)
of pneumocytes cell. The understanding about histological pattern of these functional structures
of the lung is important in pathophysiology of lung problems.
Learning Tasks
A. Structure of The Upper Respiratory tract Krishna, a man, 25 years old came to doctor Arjuna clinic with fever, sore throat, sneezing,
runny nose and sometimes blocked nose. He also cannot smell well. The doctor diagnoses
Krishna with acut Rhinopharingitis.
1. Describe the histological structure of the upper respiratory tracts are involved?
2. Describe the histological structure and function of epiglottis!
3. Compare the histological structure and function between vestibular fold and vocal fold!

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
24
B. Structure of The Lower Respiratory tract
Radha, a 17 years old beautiful girl, came to doctor Laksmi clinic with shortness of breath,
wheezing and cough with phlegm. The doctor diagnoses Radha with Asthma.
1. Describe the histological structure of the lower respiratory tracts are involved?
2. Compare the histological structure and function between terminal bronchioles and
respiratory bronchioles!
3. Describe the histological structure of the interalveolar septum!
4. Describe the histological structure of blood-air barrier?
5. Describe about the pulmonary surfactant?
LECTURE 3 PHYSIOLOGY OF RESPIRATORY SYSTEM: VENTILATION
dr. I Made Muliarta, MKes
In living cells aerobic metabolism consumes oxygen and produces carbon dioxide. Gas
exchange requires a large , thin, moist exchange surface, a pump to move air circulatory
system to transport gases to cells. The primary function system are:
Exchange the gases between atmosphere and the blood.
Homeostatic regulation of body pH .
Protection from inhaled pathogens and irritation substance
Vocalization.
In addition to serving these function, the respiratory system also source of significant losses
of water and heat from the lung.
A single respiratory cycle consists of an inspiration and expiration. Relation with ventilation
had to know about compliance, surfactant, lung volume and capacities
Respiratory control resides in a central pattern generator, a net work of neurons in the pons
and medulla oblongata.

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
25
Learning Task
1. What is the sequence of event during quiet inspiration (muscle involvement, pressure
changes (intrapulmonary and intrapleura), volume changes)!
2. What is pulmonary ventilation and alveolar ventilation means?
3. Andi, male, 30 years old, has a puncture wound due to car accident in his right chest and
penetrate his pleural cavity. The patient has complained shortness of breathing and doctor
determine that his lung is collapsed.
a. What is this condition called?
b. Describe the mechanism of the lung collapse!
c. What kind respiratory system compensation to anticipate this condition (lung collapse)?
d. How can he still be alive in this condition?
4. Describe the Boyle’s Law!

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
26
LECTURE 4 PHYSIOLOGY OF RESPIRATORY SYSTEM: GAS EXCHANGE, DIVING, ALTITUDE
dr. I Made Muliarta, Mkes
Gas exchange during external respiration occurs in respiratory membrane. Several factors
may influence gas exchange. Dalton’s law and Henry’s law may apply during gas exchange.
Some physiologic responses on respiratory system at high altitude and during diving.
Some illnesses/injuries related pressure change may occurs at high altitude and during diving.
Learning Task
1. Describe the Dalton’s Law!
2. Describe the factors that influence oxygen diffusion from alveoli into the blood!
3. Predict the response of the pulmonary arterioles and bronchioles when PO2 increase and
PCO2 decrease!
4. Describe some illnesses/ injuries due to high altitude!
5. Describe some illnesses/ injuries due to diving!
LECTURE 5 CARRIAGE OF OXYGEN AND CARBON DIOXIDE
dr. Desak Wihandani
The supply of oxygen to the tissues is our most immediate physical need. We take in
about 250 ml of oxygen gas per minute and this is our most pressing physical need. If our
oxygen supply is interrupted for more than a few minutes, irreversible damage is done to some
tissues, notably the brain. Oxygen is abundantly available in the air around us but cannot diffuse
into our tissues at sufficient rate to meet our needs. It must be transported from the lung, the
specialized organ for gas exchange, by the blood to all the other tissue.
While oxygen has to be transported from lungs to tissues, carbon dioxide must be
transported from the tissues for excretion by the lungs. Carbon dioxide has physicochemical
properties that make its transport less difficult then transport of oxygen. Carbon dioxide can be
transported in the blood in three ways: in simple solution, by reversible conversion to
bicarbonate and by reversible combination with haemoglobin to form carbamino haemoglobin.
Learning Task:
1. Describe the structure and function of hemoglobin!
2. Describe the mechanism of oxygen binding to hemoglobin!
3. Describe the differences between hemoglobin and myoglobin!
4. Describe the mechanism of oxygen binding to myoglobin!
5. Describe conformational differences between deoxygenated and oxygenated Hb!
6. Summarize the processes by which carbondioxide is transported from peripheral tissues
to the lungs!

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
27
LECTURE 6 CONTROL OF ACID BASE BALANCE, ARTERIAL GAS ANALYSIS (AGA)
dr. Desak Wihandani
Acid-Base Balance
There is large daily flux of oxygen, carbon dioxide and hydrogen ion through the human body.
Carbon dioxide generated in tissues dissolves in H2O to form carbonic acid, which in turn
dissociates releasing hydrogen ion. The blood concentration of hydrogen ion is constant, it
remains between 36 and 46 nmol/L (pH 7,36-7,46). Changes in pH will affect the activity of
many enzyme and tissue oxygenation. Problems with gas exchange and acid-base balance
underlie many diseases of respiratory system.
Blood Gases
Blood gas measurement is an important first-line investigation performed whenever there is a
suspicion of respiratory failure or acid-base disorders. In respiratory failure, the results of such
measurements are also an essential guide to oxygen therapy and assisted ventilation. The key
clinically used parameters are pH, pCO2 and pO2, the bicarbonate concentration is calculated
from pH and pCO2 values.
Learning Task:
1. Describe organs in our body involved in acid-base balance, and how they work!
2. Describe acid-base balance disorders! What is mean by :
a. Respiratory alkalosis,
b. metabolic alkalosis,
c. respiratory acidosis, and
d. metabolic acidosis?
3. In which condition respiratory acidosis and respiratory alkalosis occurs?
4. What is the importance of blood gas measurement. To perform measurement where are
the blood sample taken from? What kind of measurements are done?

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
28
LECTURE 7 CONTROL OF RESPIRATORY FUNCTION
Prof. Dr. dr. Wiryana, SpAn
When considering contol of breathing, the main control variable is PaCO2 (we try to
control this value near to 40 mmHg). This can be carried out by adjusting the respiratory rate,
the tidal volume, or both. By controlling PaCO2 we are effectively controlling alveolar ventilation
(see Ch.3) and thus PACO2. Although PaCO2 is the main control variable, PaO2 is also
controlled, but normally to a much lesser extent than PaCO2. However, the PaO2 control system
can take over and become the main controlling system when the PaO2 drops below 50 mmHg.
Control can seem to be brought about by:
1. Metabolic demands of the body (metabolic control)-tissue oxygen demand and acid-
base balance.
2. Behavioural demands of the body (behavioral control) – singing, coughing, laughing
(i.e.control is voluntary).
These are essentially feedback and feed-forward control systems, respectively. The
behavioural control of breathing overalys the metabolic control. Its control is derived from higher
centres of the brain. The axons of neurons whose cell bodies are situated in the cerebral cortex
bypass the respiratory centres in the brainstem and synapse directly with lower motor neurons
that control respiratory muscles. This system will not be dealt with in this next;we shall deal only
with the the metabolic control of respiration.
Learning Tasks
1. Discuss the central control of breathing with reference to the pontine respiratory group
and the dorsal-ventral respiratory groups of medulla spinalis!
2. List the different types of receptors involved in controlling the respiratory system!
3. Describe factors that stimulate central and peripheral chemoreceptor!
4. Outline the response of the respiratory system to change in carbon dioxide
concentration, oxygen concentration and pH!
5. Discuss the mechanism thought to influence the control of ventilation in exercise!
6. Discuss the changes that occur in response to high altitude!

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
29
LECTURE 8 PATHOLOGY OF UPPER AND LOWER URINARY TRACT
dr. Ni Wayan Winarti, SpPA
The term “upper airways” is used here to include the nose, pharynx, and larynx and their related parts. Disorders of these structures are among the most common afflictions of humans, but fortunately the overwhelming majority are more nuisances than threats. Inflammatory diseases are the most common disorders of the upper respiratory tract, i.e. rhinitis, sinusitis, pharyngitis, tonsillitis and laryngitis. It may occur as the sole manifestation of allergic, viral, bacterial or chemical insult. Although most infections are self-limited, they may at times be serious, especially laryngitis in infancy or childhood, when mucosal congestion, exudation, or edema may cause laryngeal obstruction. Tumors in these locations are infrequent but include the entire category of mesenchymal and epithelial neoplasms. Some distinctive types are nasopharyngeal angiofibroma, Sinonasal (Schneiderian) Papilloma, Olfactory Neuroblastoma and Nasopharyngeal Carcinoma.
Classification of lower respiratory tract (lung) diseases can be made based on the result of lung function test, although some authors prefer etiology and pathogenesis background. Some important diseases are obstructive lung disease (asthma, COPD, bronchiectasis) and restrictive lung disease (ARDS), and also infections, diseases of vascular origin and tumors. Pleura as protective structure of the lungs, are sometimes involved as secondary complication of some underlying disease, but in rare case, can be primary.
Because of the complexity of respiratory disease, it is important to understand their pathogenesis, supported by recognizing their morphologic changes. LEARNING TASK
Case 1
A male patient, 16 year old, came to a doctor with chief complaint difficulties in breathing. It has
occurred since 1 month ago. This patient suffers from rhinitis alergica since he was 3 year old.
On physical examination, a pedunculated nodule in right nasal cavity was found. It was whitish
in color, 1.5 cm in diameter occluding the nasal cavity.
1. Based on clinical finding, what is the most possible diagnosis? 2. What are the DDs? 3. Describe the morphological appearance (macroscopy and microscopy) that supposed to
be found to confirm your diagnosis! 4. Explain the pathogenesis of this diasease!
Case 2
A male patient, 65 year old, has suffered from dyspnea and productive cough since 1 year ago.
Lung function test showed increased of FEV1 with normal FVC (confirm an obstructive lung
disease). He is a heavy smoker since he was 25 year old. No history of atopy. No evidence of
cardiac disorders.
1. Mention 4 diseases including in the spectrum of obstructive lung disease! 2. Explain their pathogenesis! 3. Distinguish their morphology!
Case 3
A female patient, 50 year old, has suffered from tumor of right lung with pleural effusion. As the
first step to confirm the diagnosis, doctor asked the patient to do cytology test.
1. Mention some cytology test can be choose for this patient! 2. Among the test mention above (A), which one is the most simple and non-invasive? 3. And, discuss how to collect the specimen!

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
30
LECTURE 9 LUNG DEFENCE MECHANISM
dr. Ni Wayan Winarti, SpPA
Respiratory tract is an organ that constantly exposed by contaminated air. It is there fore a
small miracle that the normal lung parenchyma remains sterile. Fortunately, a plethora of
immune and non immune defense mechanisms exist in the respiratory system, extending from
the nasopharynx all the way into alveolar airspaces.
The major categories of defense mechanisms to be discussed include : (1) physical or
anatomic factors related to deposition and clearance of inhaled materials, (2) antimicrobial
peptides, (3) phagocytic and inflammatory cells that interact with inhaled materials, (4) adaptive
immune response, which depends on prior exposure to recognize the foreign materials. Each
components appears to have a distinct role, but a tremendous degree of redundancy and
interaction exists among different components.
Any condition breaks down the lung defense mechanism may result in lung injury and
respiratory tract infections
Learning Tasks
1. Defense mechanism of the lung and respiratory tract ca be divided into four major categories. Mention them, their components and explain how each of them acts against foreign materials!
2. Explain about diseases or conditions that break the lung defense mechanism down which result in increase susceptibility to respiratory tract infections!
LECTURE 10 PHARMACOLOGICAL AND NON PHARMACOLOGICAL INTERVENSION I
Prof. dr. GM Aman
Drugs for cough, rhinitis, asthma bronchiale
Cough is a protective reflex mechanism that removes foreign material and secretions from
the bronchi and bronchioles. It can be inappropriately stimulated by inflammation in the
respiratory system or by neoplasia. In these cases, antitussive (cough suppressant) drugs are
sometimes used. It should be understood that these drugs merely suppress the symptom
without influencing the underlying condition. In cough associated with bronchiectasis or chronic
bronchitis, antitussive drugs can cause harmful sputum thickening and retention. They should
not be for the cough associated with asthma.
Most drugs used in rhinitis are effectively relief the symptom of rhinitis, not affect the
underlying disease. No drug can relief symptom completely. Drugs are more effective for
allergic rhinitis than non allergic rhinitis, and acute form of allergy respond more favorable than
chronic form of allergy. The most common drugs used for rhinitis are antihistamine, nasal
disodium cromoglycate, nasal decongestant, anticholinergic, intranasal corticosteroid.
Bronchial Asthma is a disease characterized by airway inflammation, edema and
reversible bronchospasm. Bronchodilator and anti-inflammatory are the most useful drugs used
in asthma. B2 selective agonists, muscarinic antagonists, aminophylline and leucotriene

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
31
receptor blockers are the most effective bronchodilator. Anti-inflamatory drugs such as
corticosteroid, mast cell stabilizers, leucotriene antagonists, and an anti IgE antibody are widely
used. Short acting B2 agonist are the most widely used for acute asthma attack, by relaxing
airway smooth muscle. Theophylline, aminophylline and antimuscarinic agent are also used for
acute asthma attack. Long term control can be achieved with an anti-inflammatory agent such
as corticosteroid (systemic or inhaled), with leucotriene antagonist, mast cell stabilizers
(cromolyn or nedocromil). Long acting B2 agonists such as Salmeterol and Formeterol, are
effectively in improving asthma control, when taken regularly.
Learning Tasks
The patient complained about a sore throat and a nasty cough. It started two weeks ago with a
cold. The cold was over within a week, but he continued coughing, especially at night. He is a
heavy smoker. After physical examination you diagnosed a dry, tickling cough.
Task 1
1) Differentiate between Antitussive, Expectorant, Mucolytic! 2) Differentiate the effects of Codeine, Dextromethorphan and Diphenhydramine! 3) List the side effects of Codeine! 4) In this patient, what kind of anti cough you give best?
Task 2
If the patient also has sneezing, rhinorrhea and congested nose and then you diagnosed as
rhinitis.
1) List the group of drugs used for Rhinitis! 2) List the drugs used as oral nasal decongestant, and describe the important side effects! 3) List the side effects of intranasal decongestant! 4) What is the drug of choice for patient suffer from Rhinitis Medicamentosa?
LECTURE 11 PHARMACOLOGICAL AND NON PHARMACOLOGICAL INTERVENSION II
Prof. dr. GM Aman
Learning Task
If the patient come with cough, breathless, and in your examination, you found wheezing. After
physical examination you diagnosed Acute attack of bronchial asthma.
1. Chose the drug of first choice for this patient! 2. List the side effects of this drug! 3. Compare the effect of this drug with Salmeterol! 4. Theophyllin is a bronchodilator, but has a narrow safety margin. List the side effects &
toxic effect of Theophyllin! 5. Ipratropium not as effective as Salbutamol in treating bronchial asthma. What is the main
use of Ipratropium? 6. Cromolyn and Nedocromil are often used for Asthma bronchial. Describe the mechanism
of action of Cromolyn (Disodium Cromoglycate)! 7. To decrease the side effet of Corticosteroid in asthma patient, Corticosteroid often use
as inhaled Corticosteroid. What are the side effect of inhaled Corticosteroid? 8. List the anticough that are contraindicated in acute asthma attack! 9. If you need anticough, what drug you give best?

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
32
LECTURE 12 RESPIRATORY IMAGING
dr. Elysanti, Sp.Rad
The imaging investigations of the chest may be considered under the following heading:
1. Simple X- ray (conventional X-ray).
2. Chest screening.
3. Tomography.
4. Bronchography.
5. Pulmonary angiography.
6. Isotope scanning.
7. Computed tomography(CT-scan).
8. MRI.
9. Needle biopsy.
The conventional Chest X-ray has to diagnose the anatomical disorders of the chest for
example:
1. Lungs disease-----pneumonia, mass, atelectasis etc.
2. Pleural disease----pleural effuse, pneumothorax etc.
3. Cardiac disease----cardiomegali.
4. Bone disorders-----fracture.
5. Soft tissue disease—emphysema cutis.
Sometimes conventional X-ray diagnostic can not enough for diagnostic of the chest disorders,
for this the CT scan, MRI, bronchography, and arteriography can be help.
Learning Tasks
A male patient, 68 years old, with chronic cough and hemoptoe.
1. What is the imaging choice for establish the diagnosis ?
2. What kind of diagnosis you will consider if the imaging revealed some consolidation at
the apex of the right lung accompanied by rib destruction?
A 1- month old female patient is suffered from fever and dyspneu.
1. What kind of abnormality you hope to see on the chect X ray film?
2. What do you thing about the diagnosis of the disease?

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
33
LECTURE 13 BRONCHIOLITIS AND ASTHMA IN CHILD
dr. IB Subanada, SpA
Bronchiolitis is an acute inflammatory disease of the lower respiratory tract (bronchioles)
caused predominantly by respiratory syncytial virus (RSV). The inflammation response
characterized by bronchiolar epithelial necrosis, bronchiolar occlusion, and peribronchiolar
collection of lymphocytes. Bronchiolus become edematous and obstructed with mucus and
celluler debris, which may lead to partial or complete collapse of the bronchioles. By the age 2
years nearly all children have been infected, with severe disease more common among infants
aged 1-3 months.
The clinical manifestation, initially upper respiratory signs and symptoms and followed by
obstructed bronchioles signs and symptoms.
The white blood cell and differential counts are usually normal. Chest x-ray reveals
hyperinflation, peribronchial cuffing, and atelectasis.
The mainstay of therapy is supplemented oxygen with close monitoring and supportive
care.
There are higher incidence of wheezing and asthma in children with history of
bronchiolitis. Pooled hyperimmune RSV intravenous immunoglobulin (RSV-IVIG) and
palivizumab intramuscular are effective to preventing severe RSV disease in high risk infants.
The case fatality rate is less than 1%.
Learning Tasks
A 6-months old male infant came to Outpatient Clinic, Department of Child Health, Medical
School, Udayana University, Sanglah Hospital, Denpasar with the chief complaint of difficult to
breath since yesterday. According to his mother, three days before, he suffered from coryza,
cough, and low grade fever. On physical examination, fast breathing, wheezing and a prolonged
expiratory phase were found. Please discuss his mother the disease of the infant!
Learning Tasks
1. Explain the pathological concept of asthma in child!
2. Explain the clinical manifestations of asthma in child!
3. Explain the diagnosis principles of asthma in child!
4. Determine the severity of asthma and the degree of asthma attack in child!
5. Construct management plans for asthma attack in child (reliever) and determine the
need for controller management!
6. Identify the need for referral!

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
34
LECTURE 14 TB IN CHILD
dr. Ni Putu Siadi Purniti, SpA
Tuberculosis (TB) is systemic infection cause by Mycobacterium tuberculosis complex : M
tuberculosis, M. Bovis, M. africanum, M. microti, and M. canetti. Tuberculosis infection occurs
after inhalation of infective droplet nuclei containing M. tuberculosis. A reactive tuberculin skin
test and the absence of clinical and radiographic manifestations are the hallmark of this stage.
Tuberculosis disease occurs when sign and symptoms or radiographic changes becaome
apparent. In the year 2001 prevalens rate of TB is 5,6/100.000 population, of these, 931 (6 % )
cases occurred in children < 15 year of age (rate 1,5/100.000 population). Transmission of M
tuberculosis is person to person, usually by airborne mucus droplet nuclei, particles 1-5 µm in
diameter that contain M tuberculosis. In the United States, most children are infected with M.
tuberculosis in their home by adult patient tuberculosis close to them. The tubercle bacilli
multiply initially within alveoli and alveolar duct. Most of bacilli are killed, but some survive within
nonactivated macrophages, which carry them through lymphatic vessels to the regional lymph
nodes. When the primary infection is the lung, the hilar lymph nodes ussualy are involved. The
primary complex of tuberculosis includes local infection at the portal of entry ( primary focus)
and the regional lymph nodes that drain the area. During the development of the primary
complex, tubercle bacilli are carried to most tissues of the the body through the blood and
lymphatic vessels.Pulmonary tuberculosis that occurs more than a year4 after the primary
infection is usually caused by endogenous regrowth of bacilli persisting in partially encapsulated
lesions. The majority of children with tuberculosis infection develop no signs or symptoms at any
time. Occasionally, infection is marked by low grade fever and mild cough, and rarely by high
fever, cough, malaise, and flu like symptoms. Several drugs are used to effect a relatively rapid
cure and prevent the emergence of secondary drug resistance during therapy. The standard
therapy of intrathoracic tuberculosis (pulmonary disease and/or hilar lymphadenopathy) in
children, recommended by the CDC and AAP, is 6 month regiment of isoniazid (INH), rifampin
(RIF) supplemented in the first 2 month of treatment by pyrazinamide (PZA).
Learning Tasks
In Outpatient Clinic Department of Pediatric, the baby 10 month of age carried by the
mother with the chief complaint is loss of weight since 3 month, suffered low grade fever,
chronic cough, malaise and flu like symptoms. The grandfather whom was diagnosed
pulmonary tuberculosis and she has been in recent closed contact. In physical examination
found that there were enlargement of neck lymph nodes.
Learning Resources
Nelson Textbook of Pediatrics Ed. 17 th 2004: pp 958-972

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
35
LECTURE 15 PULMONARY TB AND EXTRAPULMONARY TB
dr. IB Sutha, SpP
WHO estimates that about 9.27 million new cases in 2007 compared with 2.24 million
cases in 2006, with 44% or 4.1 million cases of the infectious cases (sputum smear new cases
with positive). TB problem in Indonesia is a national problem, the case is increasing and
increasingly concerned with the increasing HIV infection and AIDS are rapidly growing
emergence of multi-drug resistance TB problem.
Tuberculosis is an infectious disease directly caused by the bacteria Mycobacterium
tuberculosis that primarily attacks the lungs. TB bacteria are rod-shaped, aerobic with a
complex cell wall structure, it was mainly composed of fatty acids that are acid resistant and can
survive in a dormant form.
TB germs enter through inhalation of the bacteria will reach the alveoli and catched by
alveolar macrophages, the bacteria will die. If the germs stay alive it will proliferate to form
primary apex (Primer Apex) and will limphogen or hematogenous spread. Primary apex
surround by limphogen spreading form the "primary complex of Ghon" and formed specific
cellular immunity is characterized by a positive tuberculin test. If the immunity is low, complex
primary complications, the patient became ill and the symptoms and clinical signs of disease. M.
tuberculosis may attack any organ of the body and most importantly the lungs.
Clinical symptoms involve respiratory symptoms and prodromal symptoms, whereas
clinical signs obtained at once with the examination depends on the type and extent of lesions in
the lungs and surrounding organs. Radiological examination of the thorax will get the infiltrates,
fibrosis and kaverna. Bacteriological examination by smear and culture of sputum smear
examination.
TB treatment follow national treatment program. Tuberculosis control which refers to the
eradication of TB WHO guideline.
General Objectives
1. Knowing the microbiology, epidemiology and pathogenesis of tuberculosis.
2. Knowing the clinical symptoms, clinical and radiological signs of pulmonary TB and
extra-pulmonary TB.
3. Able to clasify Tuberculosis.
4. Able to explain treatment program of tuberculosis and side effect.
5. Able to describe the prevention of tuberculosis and MDR TB.
Triger
A male patient aged 25 years came to a health center with complaints of bloody cough every
time since one month ago. That was not originally phlegm but since two weeks ago a yellowish
productive cough. The coughing did not disappear with anti-cough medicine. Shortness of
breath and chest pain is absent. Patients feel the slightly fever and night sweating and also
weakness, no appetite. Patients had never been sick before, enough food, smoking and family
sometimes there is no similar illness. Physical examination has been found: look thin, alert
state, blood pressure 110/70 mmHg; pulse rate 108 x/mnt; Respiration rate 24 breaths/mnt

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
36
T.aksila 370C. Lymph nodes enlargement on the right neck. On chest examination: symmetrical
right-left chest, normal heart, vesicular breath sounds in the chest and rhales on the third
upright.
Learning Tasks:
1. What should you do to ensure the diagnosis of this patient?
2. What should you do for this patient with enlargement of gland in the neck?
3. If the sputum smear examination results - / +2 / -, what is diagnosis?
4. Explain the treatment program appropriate to this patient!
5. Explain about patient monitoring and Communication-Information-and Education for this
patient and his family?
TB IN THE IMMUNOCOMPROMISED HOST
dr. Made Bagiada, SpPD-KP
Sebagai seorang dokter yang bekerja di tingkat pelayanan primer, pemahaman tentang
diagnosis dan penatalaksanaan TB pada imunokompromais sangatlah penting. Kejadian TB
lebih tinggi pada imunokompromais dibanding dengan non-imunokompromais. Penyakit infeksi
kronik ini bila tidak ditangani dengan baik menyebabkan morbiditas dan mortalitas yang tinggi.
Di Indonesia dengan beban TB tinggi (nomor 5 di dunia) akan lebih tinggi lagi dengan
meningkatnya prevalensi penderita HIV/AIDS.
TB adalah penyakit infeksi kronis yang disebabkan oleh M.tuberculosis. Tempat masuk
dan target organ terbanyak adalah paru. Orang yang terinfeksi M.tuberculosis hanya sebagian
kecil yang menjadi sakit TB dan sebagian besar tidak menjadi sakit (latensi). Orang yang tidak
sakit (latensi) akan menjadi sakit (reaktivasi) atau TB aktif bila terjadi penurunan daya tahan
tubuh atau imunitas (imunokompromais). Secara umum klinis TB ditandai dengan batuk-batuk
produktif lebih dari 2 – 3 minggu disertai dengan gejala-gejala respiratorik lainnya dan gejala
non-respiratorik. Namun, manifestasi klinis dari TB pada individu imunokompromais terletak
pada derajat beratnya penurunan imunitas. Sering tanda dan gejala TB atipikal, sering terjadi
kesalahan diagnosis, sehingga prognosis menjadi lebih buruk.
Imunokompromais adalah suatu kondisi dimana sistem kekebalan tubuh seseorang
melemah atau tidak ada. Individu yang imunokompromais kurang mampu melawan atau
memerangi infeksi karena respon imun yang berfungsi tidak benar. Contoh orang
imunokompromais adalah mereka yang terinfeksi HIV atau AIDS, wanita hamil, atau sedang
menjalani kemoterapi atau terapi radiasi untuk kanker. Kondisi lain dengan imunokompromais,
seperti kanker tertentu dan kelainan genetik, diabetes mellitus, dan penderita yang
mendapatkan terapi TNF-α. Individu immunocompromised kadang-kadang lebih rentan
terhadap infeksi serius dan /atau komplikasi dibanding orang sehat. Mereka juga lebih rentan
untuk mendapatkan infeksi oportunistik, yaitu infeksi yang biasanya tidak mengenai orang yang
sehat.
Dalam keadaan penderita dengan imunokompromais, seorang dokter harus dapat
mengenali penyakit TB aktif. Diagnosis TB pada imunokompromais adalah dengan menemukan
kuman BTA pada sputum baik dengan pemeriksaan langsung BTA maupun kultur. Pengobatan
TB penderita imunokompromais sama dengan pada non-imunokompromais dan pengobatan

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
37
TB-nya diutamakan. Dokter harus mampu mengidentifikasi penderita TB pada
imunokompromais yang tidak respon (resisten) dengan obat TB, sehingga dapat melakukan
tindakan lebih dini untuk menurunkan perburukan prognosis (kematian).
General Objektif
1. Mampu menjelaskan penegakan diagnosis TB pada imunokompromais.
2. Mampu menyusun program pengobatan jangka panjang penderita TB pada
imunokompromais.
3. Mampu mengidentifikasi kemungkinan gagal respon pengobatan (resisten) penderita TB
pada imunokompromais.
4. Mampu menyusun pengobatan utama pada penderita TB dengan imunokompromais.
5. Mampu mengidentifikasi penderita TB dengan imunokompromais yang perlu rujukan
lebih lanjut.
Trigger
Anda sebagai seorang dokter yang bekerja di sebuah Puskemas, datang seorang pasien laki-
laki, usia 28 tahun. Dia mengeluhkan panas badan sejak lebih kurang 2 minggu. Demam tidak
begitu tinggi dan tidak sampai menggigil. Disamping demam juga ada batuk-batuk ringan tanpa
disertai dahak yang dialami lebih dari 1 minggu. Penderita sudah minum obat penurun panas
dan obat batuk yang dibeli di warung tapi tidak ada kesembuhan. Berat badan penderita
dirasakan menurun drastis belakangan ini. Napsu makan berkurang sehingga badan penderita
dirasakan semakin kurus. Penderita adalah seorang sopir pengangkut barang jawa – bali,
sudah menikah dan mempunyai anak wanita usia 4 tahun. Sesekali penderita minum bir.
Penderita mempunyai tattoo di badannya yang dibuat sewaktu penderita klas 1 SMA.
Learning Task
1. Jelaskan bagaimana saudara memastikan bahwa pasien tersebut memang menderita
TB dan imunokompromais!
2. Mengapa TB laten menjadi reaktivasi (TB aktif)?
3. Bagaimana saudara mengenali pasien TB imunokompromais mengalami Immune
Reconstitution Inflammatory Syndrome (IRIS)?
4. Jika ternyata pasien tersebut menderita TB dengan imunokompromais bagaimana cara
menyusun pengobatan penderita?
5. Bagaimana cara menilai respon pengobatan TB pada pasien dengan
imunokompromais?
6. Jelaskan kriteria TB pada imunokompromais!

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
38
LECTURE 16 ASTHMA
Prof. IB Rai
Airway hyper responsiveness is known as the denominator underlying all form of asthma.
The basis of this abnormal bronchial response is not fully understood. Most current evidence
suggests that bronchial inflammation is the substrate for this hyper responsiveness, manifested
by the presence of inflammatory cells and by damage of bronchial epithelium. In extrinsic
(allergic) asthma, bronchial inflammation is caused by type I hypersensitivity reactions, but in
intrinsic asthma, the cause is less clear. Incriminated in such cases are viral infections of the
respiratory tract and inhaled air pollutant such as sulfur dioxide, ozone and nitrogen dioxide.
General Objektif:
1. Mampu menjelaskan penegakan diagnosis asma. 2. Mampu menyusun program pengobatan jangka panjang asma. 3. Mampu mengidentifikasi pasien dengan serangan asma akut. 4. Mampu memberikan pengobatan awal pasien dengan serangan asma akut. 5. Mampu mengidentifikasi pasien asma akut yang perlu perawatan inap di rumah sakit,
dan merujuknya.
Triger
Anda sebagai seorang dokter yang bekerja di sebuah Puskesmas kota, datang seorang pasien
wanita, usia 36 tahun. Dia menyampaikan bahwa telah menderita asma sejak usia remaja.
Dalam 3 bulan terakhir ini, dia mengalami serangan asma hampir setiap 3 hari , termasuk
serangan di malam hari. Untungnya, kata pasien, serangan asmanya dapat diatasi dengan obat
semprot yang dia miliki. Pasien menginginkan agar terbebas dari penyakitnya ini.
Learning Task
1. Jelaskan bagaimana saudara memastikan bahwa pasien tersebut memang menderita asma!
2. Apakah asma pasien tersebut dalam keadaan terkontrol? Jelaskan! 3. Apakah inhaler yang dipergunakan oleh pasien tersebut termasuk ke dalam kelompok
pelega (reliever)? Jelaskan perbedaan fungsi antara reliever dan controller, dan sebutkan obat-obat dari kedua kelompok tersebut!
4. Susun rencana penatalaksanaan jangka panjang pasien tersebut! 5. Apabila suatu saat pasien tersebut mengalami suatu serangan asma akut, terapi apa
yang akan saudara berikan? 6. Jelaskan kreteria serangan asma akut berat!

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
39
LECTURE 16
CHRONIC OBSTRUCTIVE PULMONARY DISEASE
dr. IGN Bagus Artana, SpPD
Chronic Obstructive Pulmonary Disease (COPD) is a disease state characterized by
airflow limitation that is not fully reversible. COPD is the fourth leading cause of death in the
world and the number of patients is projected to increase worldwide in the future. Tobacco
accounts for an estimate of 90% to the risk of developing COPD. Patient with COPD first
complaining chronic cough with sputum and followed by dyspnea. This condition worsening
progressively until the patient unable to do his daily activities.
Treatment aim for COPD is to decrease symptom, without stopping the progression of this
disease. Prevention is more important in this condition, such as by smoking cessation program.
General Objektif:
1. Mampu menjelaskan penegakan diagnosis PPOK serta penilaian kombinasi pasien. 2. Mampu menyusun rencana pengobatan pada kasus PPOK stabil. 3. Mampu menangani factor risiko pasien PPOK. 4. Mampu menentukan eksaserbasi akut dari PPOK. 5. Mampu menjelaskan manajemen gawat darurat pasien dengan PPOK eksaserbasi akut.
Triger Seorang pasien laki-laki usia 70 tahun datang bersama anaknya kepoliklinik paru Rumah Sakit Daerah tempat anda bertugas dengan mengeluh sesak nafas. Sesak nafas dirasakan sangat berat, berpakaian pun pasien mengaku sesak. Sebelumnya pasien memang merokok sejak usia 20 tahun sebanyak 2 pak sehari. Pasien juga mengatakan sering opname di rumah sakit karena serangan sesak nafas yang sangat berat. Pasien dan keluarganya ingin mengetahui dengan pasti mengenai penyakitnya serta tindak lanjut penanganannya. Learning Task
1. Jelaskan bagaimana penegakan diagnosis pasien tersebut! 2. Bagaimanakan kombinasi penilaian pasien ini? Data apa saja yang saudara perlukan
untuk melengkapi kombinasi penilaian tersebut? 3. Sebutkan dan jelaskan obat-obat yang dapat digunakan untuk menangani kasus PPOK
stabil! 4. Bagaimana anda menyusun rencana penatalaksanaan pasien ini secara komprehensif? 5. Bagaimana penatalaksanaan pasien ini apabila mengalaami PPOK eksaserbasi akut?

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
40
LECTURE 17 PLEURAL EFFUSION
dr. Putu Andrika, SpPD-KIC
Membran tipis pleura terdiri dari dua lapisan yaitu pleura visceralis dan pleura parietalis.
Penumpukan cairan melebihi jumlah fisiologis 10-20 ml disebut efusi pleura, akibat dari
peningkatan produksi yaang melebihi kemampuan absorpsi.
Penting untuk menegakkan diagnosis berdasarkan anamnesis yang baik dan
pemeriksaan fisik yang teliti, pemeriksaan radiologi torak serta melakukan pungsi pleura.
Analisis cairan pleura akan sangat berguna untuk menuntun kearah penyebab efusi pleura.
Dibedakan cairan efusi yang transudat dan eksudat.
Volume efusi pleura yang banyak akan menimbulkan gangguan fungsi respirasi yang
memerlukan pengeluaran cairan efusi melalui aspirasi cairan pleura (torako sentesis) atau
melalui pemasangan chest cube (Water Seal Drainage).
Dalam mengelola pasien dengan efusi selain menangani keluhan akibat menumpuknya
cairan efusi juga harus menangani penyebab terjadinya efusi tersebut.
General Objektif:
1. Mampu menjelaskan penegakan diagnosis efusi pleura.
2. Mampu menilai analisis cairan pleura.
3. Mampu merencanakan pemeriksaan penunjang untuk mendapatkan penyebab
terjadinya efusi pleura.
4. Mampu mengidentifikasi kasus yang memerlukan penanganan segara dan kasus yang
harus dirujuk ke rumah sakit.
Triger:
Seorang wanita muda datang dengan keluhan sesak nafas yang semakin memberat sejak
seminggu. Pada pemeriksaan fisik didapatkan frekwensi nafas 24 x/mnt, suhu tubuh 37,5 o C,
pemeriksaan torak asimetris, kanan tertinggal, perkusi redup dan suara nafas melemah di
bagian kanan bawah. Penderita juga mengeluh batuk batuk sejak 3 bulan yang lalu dan pernah
batuk berisi darah segar sedikit, juga nampak semakin kurus.
Learning Task
1. Apakah kemungkinan penyebab keluhan pasien tersebut?
2. Pemeriksaan penunjang apa yang diperlukan?
3. Perlukah melakukan parasentesis? Jelaskan!
4. Perlukah pemasangan WSD? Apa alasannya?

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
41
PNEUMOTORAKS
dr. Yasa, SpBTKV
Pneumotoraks merupakan salah satu kegawatdaruratan di bidang paru yang berarti
terisinya rongga pleura oleh udara. Pneumotoraks ini perlu mendapatkan perhatian serius,
karena dengan penanganan yang cepat dan tepat akan sangat mengurangi angka
kematiannya. Sebagai seorang dokter yang ada di fasilitas kesehatan primer, sangat diperlukan
pengetahuan mengenai keadaan ini.
Diagnosis pneumotoraks dapat ditegakkan dari anamnesis, pemeriksaan fisik dan foto
polos dada. Pneumotoraks dapat dibagi berdasarkan berbagai kriteria, tetapi yang paling sering
adalah dibagi menurut terjadinya (pneumotoraks artifisial, traumatic, serta spontan) serta
berdasarkan jenis fistelnya (pneumotoraks terbuka, tertutup, dan ventil).
Beberapa kondisi pneumotoraks akan sangat mengancam nyawa, sehingga memerlukan
penanganan yang tepat dan segera. Penatalaksanaan pneumotoraks pada prinsipnya adalah
mengeluarkan udara yang ada di rongga pleura tersebut, terapi penyebabnya, serta edukasi
untuk mencegah berulangnya pneumotoraks pada pasien yang memiliki risiko.
General Objektif:
1. Mampu menjelaskan penegakan diagnosis pneumotoraks.
2. Mampu menyebutkan beberapa penyebab pneumotoraks yang sering dijumpai.
3. Mampu menjelaskan beberapa pembagian jenis pneumotoraks.
4. Mampu menyusun rencana penatalaksanaan pasien dengan pneumotoraks.
Triger
Seorang pasien laki-laki usia 30 tahun datang kePuskesmas tempat anda bertugas dengan
mengeluh sesak nafas tiba-tiba dan sangat berat. Pasien sebelumnya dengan riwayat
menderita penyakit TB paru dan sudah berobat dengan lengkap. Sebelumnya pasien sempat
terbatuk-batuk, kemudian tiba-tiba sesak nafas. Pasien ini tampak sesak dan sianosis.
Learning Task
1. Jelaskan temuan fisik dan foto polos dada yang kemungkinan ditemukan pada pasien
pneumotoraks tersebut!
2. Sebutkan beberapa penyebab pneumotoraks yang anda ketahui!
3. Bagaimana penatalaksanaan kasus dengan pneumotoraks tersebut?

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
42
LECTURE 18
BRONCHITIS AND BRONCHIECTASIS
dr. Dewa Artika, SpP
Untuk menentukan suatu Bronkitis dan Bronkiektasis tidaklah terlalu sulit, tapi diperlukan
suatu pemahaman untuk mendiagnosis dan penatalaksanaan Bronkitis dan Bronkiektasis
dengan baik dan benar. Disamping prevalensinya cukup tinggi, penyakit ini bila tidak ditangani
dengan baik, akan berlanjut menjadi lebih parah.
Bronkitis adalah inflamasi saluran napas sentral yang mengenai mukosa ditandai oleh
batuk dengan dahak, sering disertai dengan panas dan sesak.Bronkiektasis adalah kelainan
pada dinding bronkus besar dan sedang berupa kelemahan otot sehingga terjadi pelebaran
lumen, karena proses infeksi transmural dan pelepasan mediator.
Diagnosis Bronkitis berdasarkan pada anamnesa, pemeriksaan fisik dan foto toraks,
sedang bronkiektasis ditegakkan dengan anamnesa, pemeriksaan fisik, foto toraks, CT Scan,
dan kultur sputum.
Prinsip penatalaksanaan Bronkitis dan Bronkiektasis adalah dengan menghilangkan batuk
dan produksi dahak. Bila disertai tanda infeksi dapat ditambahkan antibiotika. Pada
Bronkiektasis perlu dilakukan Chest Fisioterapi atau bronkoskopi untuk mempermudah
pengeluaran sputum. Pada keadaan eksaserbasi sering disebabkan oleh infeksi apakah viral
atau bakteri.
General Obyektif
1. Mampu menjelaskan penegakan diagnosis bronkitis dan bronkiektasis. 2. Mampu menyususn program pengobatan jangka panjang. 3. Mampu mengidentifikasi pasien dengan keadaan eksaserbasi. 4. Mampu memberikan pengobatan awal pasien dengan serangan akut. 5. Mampu mengidentifikasi pasien eksaserbasi yang perlu rawat inap dan merujuknya.
Triger
Seorang penderita laki umur 35 th datang dengan keluhan : batuk berdahak sejak 3 bulan dan
memberat sejak 5 hari yang lalu dan disertai dengan panas badan. Bila diperhatikan dahaknya
ada 3 lapis yaitu dari atas sampai bawah mulai dari yang bening sampai keruh dan batuknya
terutama pagi hari. Dikatakan pula setahun lalu pernah menderita sakit seperti ini dan kadang
disertai sesak napas, bila dahaknya sulit dikeluarkan.
Learning Task
1. Jelaskan bagaimana saudara memastikan bahwa pasien tersebut menderita bronchitis! 2. Bagaimana sdr membedakan dengan bronkiektasis? 3. Apakah penderita tsb dalam keadaan eksaserbasi? Jelaskan! 4. Jelaskan prinsip pengobatan pasien dg bronkitis dan bronkiektasis! 5. Obat-obat apa saja yang diperlukan pada pasien tsb diatas? 6. Apa yang dikerjakan bila sputum pasien tsb diatas sulit dikeluarkan?

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
43
KANKER PARU (LUNG CANCER)
dr. Gede Ketut Sajinadiyasa, SpPD
Kanker Paru merupakan penyebab kematian tersering diantara kematian oleh karena
kanker di seluruh dunia baik pada laki-laki ataupun perempuan. Insiden kanker paru di dunia
diperkirakan 1,3 juta kasus per tahunnya. Kanker paru terjadi sebagai akibat proses yang
komplek antara paparan karsinogen dan kerentanan genetik. Faktor kebiasaan dan lingkungan
berhubungan dengan terjadinya kanker paru dan merokok merupakan faktor risiko utama. Jenis
histologi kanker paru sebagian besar adalah Small Cell Lung Cancer (SCLC) dan Non Small
Cell Lung Cancer(NSCLC) . NSCLC terdiri atas squamus cell carcinoma, adeno carcinoma dan
large cell carcinoma. Manifestasi klinis dari kanker paru dapat asimtomatik pada stadium awal
dan baru bergejal pada stadium lanjut. Pasien biasanya datang dengan keluhan batuk, batuk
darah, sesak, nyeri dada dan suar serak. Sering juga dijumpai tanda-tanda syndrome
paraneoplastik dan gejala umum seperti anoreksia, asthenia dan berat badan yang menurun.
Diagnosis kanker paru dapat ditegaknya dengan anamnesis, pemeriksaan fisik dan
pemeriksaan penunjang. Pemeriksaan penunjang yang umum dikerjakan seperti sitologi
sputum, rontgen dada, ct scan toraks, Biopsi(FNAB/TTB), bronkoskopi, PET scan dan lainnya.
Setelah diagnosis ditegakkan dan sebelum memulai pengobatan ditentukan stadium penyakit
dan status performan. Dengan diketahuinya jenis histology dan stadium penyakit kemudian
ditentukan modalitas terapi. Modalitas terapi pada pasien kanker paru diantaranya adalah
pembedahan, kemoterapi, radiasi dan target terapi.
General Objektif
1. Mengetahui patogenesis, faktor risiko, dan usaha preventif kanker paru.
2. Dapat mengetahui klasifikasi kanker paru.
3. Mengetahui proses penegakan diagnosis dan stadium kanker paru.
4. Mengetahui modalitas penunjang dalam penegakan diagnosis.
5. Mengetahui modalitas terapi kanker paru dan merujuk.
Triger
Seorang pasien laki-laki umur 65 tahun datang ketempat pratek saudara sendirian dengan
keluhan batuk berdarah. Satu minggu yang lalu pasien sempat menjalani cek up didapatkan
pada foto rontgen dada, tumor dengan ukuran diameter 2,5 cm pada hilus kiri menempel di
pinggang jantung kiri. Pada pemeriksaan USG abdomen didapatkan tumor multiple ukuran
diameter sekitar 1-1,5 cm pada hati, sedang pemeriksaan yang lain dalam batas normal. Pasien
memiliki kebiasaan merokok sejak umur 20 tahun dengan jumlah 1-2 bungkus per-harinya.
Learning Task
1. Apa yang saudara lakukan untuk memastikan diagnosis pasien ini?
2. Kalau diperlukan tindakan invasive, prioritas tindakan yang saudara usulkan? Jelaskan
alasannya!
3. Bila ini kanker paru, apa kemungkinan klasifikasi histologinya?
4. Tentukan stadium pasien ini dan status performannya serta alasannya!
5. Tentukan modalitas terapinya!

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
44
LECTURE 19 DISORDERS OF NOSE AND SINUS
dr. Ratna, SpTHT
Nasal foreign bodies are commonly encountered in emergency departments. Although
more frequently seen in the pediatric, they can also occur in adult. Children’s interests in
exploring their bodies make them more prone to lodging foreign bodies in their nasal cavities.
References
1. Textbook Diseases of the Ear, Nose and Throat edited by Martin Burton CHURCHILL LIVINGSTQNE 15TH ED 2000: Section 5 The Larynx, Pharynx and Oesophagus. Pp 165-206
LECTURE 20 DISORDERS OF PHARYNX AND LARYNX
Prof. Suardana, SpTHT, dr. Dewa Artha Eka Putra, SpTHT
The Adenoids (pharyngeal tonsils) are a triangular mass of lymphoid tissue located on the
posterior aspect of the boxlike nasopharynx. The nasopharynx serves as a conduit for Inspired
air and Sinonasal Sections that drain from the nasal cavity into the oropharynx. a resonance box
for for speech and a drainage area for the Eustachian tube — middle ear mastoid complex.
Adenoid have three types of Surface epithelium ciliated pseudostratified squamous, and
transitional.
The Adenoids and tonsils, like all lymphoid tissue, enlarge when infected. Although
lymphoid tissue does act to fight infection. Some time bacteria and viruses can lodge within it
and survive. Group A B—hemolytic streptococcus (GABHS) is classically described as the only
bacterium implicated frequently in acute Adenoiditis or tonsilitis.
Chronic infection, either viral or bacterial, can keep the pad of adenoids enlarged for
years, even into adulthood. Some viruses, Such as the Epstein Barr virus, can cause dramatic
enlargement of lymphoid tissue.
Clinical classification of the adenoid : Acute adenoiditis, recurrent Acute Adenoiditis,
chronic adenoiditis and obstructive Adenoid Hyperplasia. Clinical classification of the tonsils:
acute tonsillitis, recurrent acute tonsillitis, chronic tonsillitis, and obstructive tonsilar hyperplasia.
The main symptoms of adenoid diseases is Rhinorhea, chronic nasal obstruction
(associated with Snoring and obligate mouth breathing), malodorous, cough, post nasal drip,
sinusitis, otitis media and a hyponasal voice. The main symptomsof tonsils diseases are: sore
throat, dysphagia, fever, halithosis, muffled voices, snoring, and other symptomsof sleep
disturbance and tender cervical adenopathy.
Adenoiditis is best diagnosed by clinical history, physical examination,
nasopharyngoscopy, and radiography. The physical examination should include both anterior
and posterior rhinoscopy. A lateral neck radiograph and sinus radiography taken to show soft
tissue density, can show the adenoids and sinus. Tonsilitis is diagnosed by clinical history,
physical examination, throat culture, and flexible laryngoscope.

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
45
Management of diseases of the adenoids and tonsils: antimicrobial, intranasal steroids
and adenoidectomy. Indications for tonsillectomy and adenoidectomy are obstruction, infection
and Neoplasia.
The anatomy of the larynx consist of cart.Haginous framework bound together by
ligaments and covered with muscle and mucous membrane. The most important cartilage is the
arytenoid cartilages which is can rotate and slide on the cricoid cartilage and thus play an
important role in the movement of the vocal cords. The epiglottis is a leaf-shape cartilage of the
larynx which is attached to the base of the tongue by the glossoepiglottic ligament and inner
part of thyroid cartilage. The thyroid cartilage is that which makes the prominence upon the front
of the neck known as ‘Adam’s apple, particularly visible in man. Interior of the larynx can looking
down by laryngoscopy indirect or direct. The function of the larynx includes protection of lower
respiratory tract and phonation. The protection of respiratory tract acting by the epiglottis,
sensory nerve supply which is produce cough and vocal cords. Voices or phonation is produce
by vocal cords function consist adduction and abduction movement and vibration of the vocal
cords.
Patient with a foreign body in his/her pharynx, or oesophagus, usually knows what has
happened and is usually right. It can stick in his tonsils, his vallecula, his pyriform fossa, or in his
postcricoid region. Most fish bones stick in accessible regions, usually the back of the tongue or
tonsils. Foreign bodies seldom stick in the larynx itself, except when an affluent, elderly, and
often intoxicated diner gets a piece of steak caught in his larynx, as a result of which he gasps
and collapses. Treat him immediately.
Throat
Normal Vocal cord and disorders
The symptoms of laryngeal disorders are hoarseness, dysphonia and stridor. Hoarseness
is caused by an abnormal flow of air past the vocal cords. The voice is harsh when turbulence is
created by the irregularity of the vocal cords. The irregularity of the vocal cord caused by vocal
nodule, edema of the vocal cord and laryngitis. Dysphonia is weakness of the voice caused by
paresis or paralysis of the vocal cords. And aphonia is loss of voice. Stridor is a high pitch
sound, is produce by lesion that narrowing the airway. If narrowing of the airway upper the vocal
cord produce inspiratory stidor, and if narrowing the airway below the vocal cord will produce
inspiratory and expiratory stridor.

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
46
Some lesion will be discussed are vocal cord nodule, vocal cord paralysis, laryngeal
palillomas and gastrolaryngopharyngeal reflux disease. Vocal nodule or Singer’s nodes is
benign lesion in the vocal cord particularly at the site of the junction of the anterior third and
posterior two-thirds of the cord (halfway along the membranous cord). This condition is caused
by misuse of the voice or overuse as well as singers, teachers, priest, actors who have not
undergone formal voice training. Misuse of the voice also happen in the schoolchildren,
sometime call by screamer’s node.
Vocal cord paralysis causes of dysphonia symptom, define as weakness or even though
temporary loss of the voice (aphonia). A vocal cord may paralysed by mechanical fixation of the
arytenoids or vocalis muscle or by nerve paralysis. Paralysis may be unilateral or bilateral and
the cords paralysed in abduction or adduction. Abduction paralysis causes loss of the voice
because the cord can not move to the midline position and adduction paralysis, the cords can
not move to the lateral position and cause severe stridor.
Laryngeal papilloma is a benign lesion single or multiple, non keratinizing papilloma in
characteristic is due by infection of human papilloma virus type 6 and 11. Papillomatosis present
more frequently in children than in adult, the peak incidence occurring between 2 and 5 years of
age, and very common of high recurrent. Relaps or recurrent may be precipitated by trauma or
immunosuppressive condition.
Gastrolaryngeal reflux is very common condition to causes hoarseness. The pathology of
gastro-esophageal-laryngeal reflux disease may be a result of direct effect of gastric acid, bile
salts or enzymes on mucosa of the larynx.
Learning Tasks
1. Describe and discuss of specific symptoms of the larynx disease & disorders! 2. Describe and discuss etiology and patophysiology of hoarseness, dysphonia and stridor
with its clinical implication! 3. Manage and provide initial management or refer patient with certain larynx disease and
disordes!
Learning Tasks
1. Describe and discuss of etiology of adenoid diseases! 2. Explain pathogenesis of adenoid diseases! 3. Describe and discuss of clinical classification of diseases in the adenoids! 4. Describe clinical evaluation to support diagnosis of the adenoid diseases! 5. Manage and provide initial management or refer patient with certain adenoid diseases! 6. Explain indications for adenoidectomy! 7. Describe complications of adenoid diseases and adenoidectomy!
Learning Resources
1. Textbook Diseases of the Ear, Nose and Throat edited by Martin Burton CHURCHILL LIVINGSTQNE 15TH ED 2000: Section 5 The Larynx, Pharynx and Oesophagus. Pp 165-206.
2. Textbook Current Medical Diagnosis & Treatment Edited by Lawrence M.Tierney,Jr. Stephen J.Mc Phee, Maxine A.Papadakis 45 Ed 2006: Diseases of the Larynx p209-213.
3. Linda Brodsky. Christhopher Poje. Tonsilitis, Tonsillectomy and Adenoidectomy. In BaiIe BJ Editor. Head and Neck Surgery-Otolaryngologv 3 ed. Philadelphia Lippincort Williams and Willkins; 2001 p 979— 991.

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
47
BASIC CLINICAL SKILLS
Topik BCS PIC
Pemeriksan fisik toraks pasien dewasa dr. Saji
Radioimaging dr. Elysanti
Pemasangan dan perawatan WSD dr. Yasa
Pengambilan cairan pleura, pungsi pleura, dekompresi jarum dr. Yasa
Spirometri dr. Muliarta
Nebulisasi dan terapi oksigen dr. Sutha
Pemeriksaan fisik toraks pada pasien bayi dan anak dr. Ayu Setyorini
Bronchoscopy, Provocation test dr. Artana
CPEP pada bayi dr. Arya Byantara
Rhinoskopi posterior THT
Pelaksanaan BCS
Hari Ruang 1 Ruang 2 Ruang 3
1 Pemeriksaan Fisik Thorax
dewasa Radio Imaging
Pemasangan dan
perawatan WSD
2
Pengambilan Cairan
Pleura, Punksi Pleura,
Decompresi jarum
Spirometri Nebulisasi dan terapi
oksigen
3 Radio Imaging Pemeriksaan Fisik Thorax
Bayi-Anak
Pemeriksaan Fisik Thorax
dewasa
4
Bronchoscopy,
Provocation test, Radio
Imaging
CPEP pada Bayi Pemeriksaan Fisik Thorax
dewasa
5 Pemeriksaan Fisik Thorax
Bayi-Anak
Perawatan WSD,
Decompresi Jarum Rhinoskopi Posterior

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
48
PENGGUNAAN SPIROMETER MERA
1. Letakkan alat (Spirometer Mera) di atas meja di hadapan orang yang akan diperiksa.
2. Orang yang diperiksa berdiri tegak sambil memegang Spirometer.
3. Orang yang diperiksa menarik nafas maksimal kemudian masukkan mulut ke dalam
mouth piece spirometer. Lakukan maneuver (ekspirasi maksimal secepat-cepatnya,
sekuat-kuatnya, dan selama-lamanya selama satu kali maneuver).
4. Hitung FEV1 dan FVC dari grafik spirometer.
5. Hitung estimated FVC berdasarkan tabel di bawah.
6. Hitung %FVC dengan rumus:
%FVC= (FVC X Estimated FVC) x 100%
7. Hitung % FEV1 dengan rumus:
% FEV1= (FEV1/FVC) x 100%

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
49
PENGGUNAAN SPIROMETER
1. Letakkan alat (Spirometer) di atas meja di hadapan orang yang akan diperiksa.
2. Orang yang diperiksa berdiri tegak sambil memegang Spirometer.
3. Pasang noseclip seperti pada gambar .
4. Orang yang diperiksa menarik nafas maksimal kemudian masukkan mulut ke dalam
mouth piece spirometer. Lakukan Maneuver (Ekspirasi maksimal secepat-cepatnya,
sekuat-kuatnya, dan selama-lamanya selama satu kali maneuver.
5. Print hasil perekaman.
6. Catat %FVC.
7. Catat% FEV1.
8. Buat Kesimpulan terkait hasil pemeriksaan.

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
50
REFERENCES
1. Essential Clinical Anatomy, 2nd ed, Keith L. Moore and Anne M.R.Agur, Lippincott William & Willems, Philadhelpia, 2002.
2. Bloom & Fawcett’s Concise Histology, 2nd ed, Fawcett D.N., Jensh, R.P, London, 2002. 3. Textbook of Medical Physiology, 10th ed, A.C. Guyton, Hall, Philadelphia, WB Saunders
Co, 2000. 4. Medical Biochemistry, Baynes J and Dominiczak, London, 1999. 5. Katzung & Trevor’s Pharmacology, Examination & Board Review, 6th ed. A.J. Trevor,
B.G. Katzung, Susan B Masters. 6. Robbins Basic Pathology, 7th ed, Kumar V, Cotran RS, Robbins SL. WB Saunders,
Philadelphia, 2003. 7. Textbook of disorder and injuries of the musculoskeletal system, Robert B. Salter MD
Apley’s system Orthopaedics and Fractures. Apley, Solomon. 8. Harrison’s, 16th ed. 2005. 9. Nelson Textbook of Pediatrics Ed. 17 th 2004: pp 958-972
10. Textbook Diseases of the Ear, Nose and Throat edited by Martin Burton CHURCHILL LIVINGSTQNE 15TH ED 2000: Section 5 The Larynx, Pharynx and Oesophagus. Pp 165-206.
11. Textbook Current Medical Diagnosis & Treatment Edited by Lawrence M.Tierney,Jr. Stephen J.Mc Phee, Maxine A.Papadakis 45 Ed 2006: Diseases of the Larynx p209-213.
12. Linda Brodsky. Christhopher Poje. Tonsilitis, Tonsillectomy and Adenoidectomy. In BaiIe BJ Editor. Head and Neck Surgery-Otolaryngologv 3 ed. Philadelphia Lippincort Williams and Willkins; 2001 p 979— 991.
ADDITIONAL TEXTBOOK
13. Review of Medical Physiology, 10th ed, W.F. Ganong, California : LANGE Medical Publications.
14. Human Physiology – An Integrated Approach. 2nd ed. Silverthorn, 2001 New Jersey : Prentice-Hall Inc.
15. Pocket Companion to Textbook of Medical Physiology, 10th ed, A.C. Guyton, Hall, Philadelphia, WB Saunders Co, 2000, pp. 52 – 95

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
51
CURRICULUM MAP
Smstr Program or curriculum blocks
10 Senior Clerkship
9 Senior Clerkship
8 Senior clerkship
7
Medical Emergency (3 weeks) BCS (1 weeks)
Special Topic: -Travel medicine (2 weeks)
Elective Study III (6 weeks)
Clinic Orientation (Clerkship) (6 weeks)
6
The Respiratory System and Disorders (4 weeks) BCS (1 weeks)
The Cardiovascular System and Disorders (4 weeks) BCS (1 weeks)
The Urinary System and Disorders (3 weeks) BCS (1 weeks)
The Reproductive System and Disorders (3 weeks) BCS (1 weeks)
5
Elective Study II (1 weeks)
Alimentary & hepato- biliary systems & disorders (4 Weeks) BCS (1 weeks)
The Endocrine System, Metabolism and Disorders (4 weeks) BCS (1 weeks)
Clinical Nutrition and Disorders (2 weeks) BCS (1 weeks)
Special Topic : - Palliative medicine -Compleme ntary & Alternative Medicine - Forensic (3 weeks)
Elective Study II (1 weeks)
4
Musculoskeletal system & connective tissue disorders (4 weeks) BCS (1 weeks)
Neuroscience and neurological disorders (4 weeks) BCS (1 weeks)
Behavior Change and disorders (4 weeks) BCS(1 weeks)
The Visual system & disorders (2 weeks) BCS (1 weeks)
3
Hematologic system & disor- ders & clinical oncology (4 weeks) BCS (1 weeks)
Immune system & disorders (2 weeks) BCS(1 weeks)
Infection & infectious diseases (5 weeks) BCS (1 weeks)
The skin & hearing system & disorders (3 weeks) BCS(1 weeks)
2
Medical Professionalism (2 weeks) BCS (1 weeks)
Evidence-based Medical Practice (2 weeks)
Health System-based Practice (3 weeks) BCS (1 weeks)
Community-based practice (4 weeks)
Special Topic - Ergonomi - Geriatri
(2 weeks)
Elective Study I (2 weeks)
1
Stadium Generale and Humaniora (3 weeks)
Medical communication (3 weeks) BCS (1 weeks)
The cell as bioche- mical machinery (3 weeks) BCS(1 weeks)
Growth & development (4 weeks) BCS: (1 weeks)
Pendidikan Pancasila & Kewarganegaraan (3 weeks)

Study Guide Respiratory System and Disorders
Department of Medical Education - Faculty of Medicine - Universitas Udayana, 2017
52