S1486: Progression of Barrett's Metaplasia to Adenocarcinoma Is Associated With the Expression of...
-
Upload
alexander-braun -
Category
Documents
-
view
215 -
download
1
Transcript of S1486: Progression of Barrett's Metaplasia to Adenocarcinoma Is Associated With the Expression of...

aaF2Rhespwpersw
SDSAVWB(tciJadt(ddmewweOhOw2sf(pdsoodnrceo
SAPaCMGGsBebtMrctE
Abstracts
A
ssessed by funnel plots. All studies were graded by Jadad score. Heterogeneitymong studies was assessed by calculating I2 measure of inconsistency.Results:our trials met inclusion criteria. Trials were of adequate quality (Jadad score �). Three trials used APC and one trial used photodynamic method for ablation.andom effects model was used for two outcomes due to significanteterogeneity. 2.4% of subjects progressed to either HGD or cancer in thendoscopic ablation group whereas 12.9% of subjects progressed in the regularurveillance group. Endoscopic ablation significantly decreased the odds forrogression to HGD or cancer (OR 0.21; 95% CI: 0.05-0.86, p�0.03; NNT�9)ithout increasing the odds for complications (OR 7.84; 95% CI: 0.87-70.74,�0.07). In addition, ablation increased the odds for eradication of Barrett’ssophagus with LGD (OR 12.97; 95% CI: 3.43-49.10, p�0.01). Funnel plotevealed no publication bias. Conclusions: Endoscopic ablation therapyuccessfully decreases risk of progression in Barrett’s esophagus with LGDithout increasing complications.
1483ilatation of the Upper Esophageal Sphincter via Retrograde ortatic Technique Is Safe and Effective: Results of a Retrospectivenalysis From 2006-2009 At a Tertiary Referral Centerinay Chandrasekhara, Joyce Koh, Lakshmi Lattimer, Kerry B. Dunbar,illiam J. Ravich, John O. Clarke
ackground: Upper esophageal sphincter (UES) dilatation for cricopharyngealCP) dysfunction is controversial and not well studied. Primary aim: To evaluatehe safety and efficacy of UES dilatation. Secondary aim: to determine if (1)riteria for dilatation or (2) technique of dilatation correlated with symptommprovement. Methods: All balloon dilatations performed at our institution fromuly 2006 - June 2009 were retrospectively analyzed for demographics, indicationnd dilatation site. All dilatations involving the UES underwent further review toetermine efficacy, complications, and factors that predict success. Dilatationechnique was separated into static (stationary balloon distention) and retrogradebrusque pull-back of a fully distended balloon across the UES). Results: 488ilatations were reviewed. 31 patients were identified who underwent UESilatation. Median age was 63 years (range 27-81) and 55% of patients wereale. Indications: radiographic (CP) bar with dysphagia (22 patients),ndoscopic UES tightness with dysphagia (3 patients), inclusion body myositisith dysphagia and prominent cricopharyngeus (3 patients), globus sensationith evidence of UES dysfunction (2 patients) and obstruction tochocardiography probe with CP bar but no symptoms (1 patient).ropharyngeal dysfunction was seen in 13 patients (52%) and 7 patients (23%)ad small Zenker’s diverticula (�2cm). Dilator size ranged from 15mm to 20mm.f the 31 patients, 11 had dilatation of other esophageal segments concurrentlyith UES dilatation and 20 had UES dilatation alone. Follow-up was available for4 patients for a mean of 7 months (range 0.5 - 28), of whom 19 reportedymptomatic improvement (79%). For patients undergoing UES dilatation alone,ollow-up was available for 15 patients, 12 of whom reported improvement80%). 19 patients underwent retrograde dilatation (84% response) while 5atients had static dilatation (60% response); however, there was no significantifference in symptom improvement between the techniques (p�0.5). Successfulymptom resolution was also not significantly affected by dilator size,ropharyngeal dysfunction, Zenker’s diverticulum, age or gender (P�0.05). Thenly complication noted was uvular edema and a shallow ulcer after staticilatation in one patient, which resolved spontaneously (no admissionecessary). Conclusions: UES dilatation with a TTS balloon by either static oretrograde technique is safe and effective for the treatment of dysphagia in theontext of CP dysfunction. To our knowledge, this is the largest study tovaluate this issue to date and the first to report on retrograde balloon dilatationf the UES.
1484ugmented Salivary Epidermal Growth Factor Secretion inatients With Negative Endoscopically Reflux Disease Could BeKey in Prevention of the Esophageal Mucosal Injury andomplicationsarek Majewski, Tomasz Jaworski, Tomasz Skoczylas,rzegorz Wallner, Richard Mccallum, Jerzy Sarosiekastroesophageal reflux disease represents a spectrum of clinical manifestations,
tarting from negative endoscopically reflux disease (NERD) and ending onarrett’ esophagus (BE). Although the mean value of the esophageal acidxposure time is greater in BE than NERD population, the individual values inoth groups overlap greatly. As the esophageal mucosal integrity depends uponhe balance between aggressive factors and protective mechanisms (Majewski
. et al. Clin. Gastroenterol. & Hepatol. 5:430-8, 2007), exploration of theate of salivary epidermal growth factor (EGF) secretion, the major protectiveomponent in saliva, may help to better understand the pathophysiology of
hese disorders as well as complications. Aim: To explore the rate of salivaryGF secretion in patients with NERD and to compare the results withB174 GASTROINTESTINAL ENDOSCOPY Volume 71, No. 5 : 2010
corresponding values in patients with BE. Subjects & Methods: The study wasconducted in 12 patients (5F, mean age of 41) with NERD with a positive 24hesophageal pH monitoring test and 17 patients (3F, mean age of 46) with longsegment (over 3cm) of BE. Salivary secretions were collected under basalconditions, during mastication and during intraesophageal mechanical (tubingwith soft inflated balloons) and chemical [initial saline, HCl/pepsin (pH 2.1) andfinal saline solutions] mimicking the natural gastroesophageal reflux scenario.The salivary EGF was measured using ELISA methodology employing thecommercially available kit (Biomed. Technol. Inc., MA). Statistical analysis wasperformed utilizing -Stat software (SyStat Inc. CA). Results: The rate of EGFsecretion in patients with NERD was 50% higher (P�0.05) than in patients withBE in basal saliva, 242% higher (P�0.001) during intraesophageal mechanicalstimulation, 84% higher (P�0.01) during intraesophageal exposure to acid andpepsin solution (pH 2.1) and 91% higher (P�0.01) during the final infusion ofsaline at the end of the experimental procedure, mimicking the naturalgastroesophageal reflux scenario. Conclusions: 1. The profoundly higher rate ofsalivary EGF secretion in patients with NERD versus subjects with BE, especiallyduring the esophageal mucosal challenge, mimicking the naturalgastroesophageal reflux scenario may indicate that their protective mechanismsare preventing mucosal injury. 2. Significantly lower salivary protective responsein terms of EGF secretion in patients with long segment of BE may at least partlyexplain their susceptibility to the loss of mucosal integrity ending in thedevelopment of intestinal metaplasia.
S1485Injurious Impact of Naproxen on the Esophageal Mucosa inHumans Could Be At Least Partly Mediated Through ItsDetrimental Effect on the Protective Quality of SalivarySecretion: Its Potential Clinical ImplicationJerzy Sarosiek, Tomasz Jaworski, Marek Majewski, Grzegorz Wallner,Cesar J. Garcia, Irene SarosiekChronic intake of non-steroidal anti-inflammatory drugs (NSAIDs) increasessignificantly the risk of the development erosions, ulcers and bleeding within thealimentary tract, including the esophagus. Salivary protective factors, defining itsviscous, gel-forming quality and its capacity to lubricate during swallowing, arewell known for their protective potential within the oral cavity as well asesophageal and gastric mucosa. Furthermore, mastication, i.e. chewing of thetasteless parafilm results in 150%-300% increase in the flow of salivary volume aswell as its protective factors in health and disease (Sarosiek et al.Gastroenterology, 110:675-81, 1996). Although the detrimental impact ofnaproxen on gastric mucus and mucin has been recently demonstrated(Jaworski et al. Dig. Dis. Sci., 50:357-65, 2005), its impact on protectivequality of salivary secretion remains to be explored. Aim: To explore thepotential impact of naproxen administration on viscosity of salivary secretion.Methods: The study was approved by HSC and conducted in 21 asymptomaticvolunteers (11F; mean age of 34). The salivary secretion was tested at baselineand after 7 days of naproxen (500 mg bid) administration in a double-blindstudy protocol. In freshly collected saliva its viscosity was recorded using Cone/Plate Digital Viscometer (Brookfield Inc., Stoughton, MA) with the 8 consecutiveshare rates, representing minimal and maximal share stress taking place duringthe solid food intake. Statistical analysis of data (Mean �SEM) was performedusing --StatSoftware (SyStat Inc., CA).Results: The baseline viscosity value ofsalivary secretion was 73.6 �9.30 at the lowest (0.3 rpm) and 3.53 �0.27 at thehighest (60 rpm) shear rate of the digital viscometer. The viscosity value ofsalivary secretion however, after 7 days of naproxen administration, declined by60% (29.1 �3.01 vs. 73.6 �9.30, P�0.001) at the lowest shear rate and declinedby 38% (2.21 �0.13 vs. 3.53 �0.27 mPa.s, P�0.001) at the highest shear rate.The average decline of salivary viscosity recorded within 8 consecutive sharerates during naproxen administration was 52% (P�0.001). Conclusions: 1. Aprofound and significant decline of salivary viscosity during administration ofnaproxen may at least partly explain a propensity of patients on chronic therapywith NSAIDs to the development of esophageal mucosal injury andcomplications. 2. Agents capable to stimulate the quantity and the quality ofsalivary secretion, like mastication, could be of value in potential protection ofthe esophageal mucosa and prevention of its injury and complications duringchronic NSAIDs therapy.
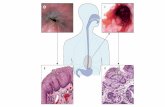
S1486Progression of Barrett’s Metaplasia to Adenocarcinoma IsAssociated With the Expression of UnphosphorylatedRetinoblastoma Gene Product (pRB)Alexander Braun, Hans J. Schrag, Ulrich T. Hopt, Andreas FischerBackground:Barrett’s esophagus (BE) is a premalignant lesion characterized byreplacement of normal squamous epithelium with columnar epithelium.Derangements in cell cycle control and apoptosis regulation might be
responsible for the progression from metaplasia to intraepithelial neoplasia andadenocarcinoma. This study was undertaken to examine the expression ofwww.giejournal.org

raagiE(twaeapipuTBIe
SWSIoCWHOBomytnschrcwb(nrn3driftrcms
SHSSHBsaumetotassm
Abstracts
w
etinoblastoma gene product (pRB) in the carcinogenesis of Barettdenocarcinoma.Methods:A total of 107 patients with adenocarcinoma (n � 60)nd intraepithelial neoplasia (n � 47) in BE were included. Finally, as controlroup, we selected 10 patients without intraepithelial neoplasia. Samples ofnvasive adenocarcinoma derived from 60 oesophagectomy specimens.ndoscopic mucosal resection (EMR) was used in 57 patients (342 samples) with196 samples) and without (146 samples) intraepithelial neoplasia. Expression ofhe phosphorylated / un(der)phosphorylated retinoblastoma gene product (pRB)ere measured by flow cytometry.Results:81,7% (49/60) of Barrettdenocarcinoma and 65,96% (31/47) of intraepithelial neoplasia showed anxpression of un(der)phosphorylated pRB whilst 23,3% (14/60) of Barrettdenocarcinoma and 6,38% (3/47) of intraepithelial neoplasia showed thehosphorylated pRB. The un(der)phosphylated pRB was found in 3,42% (5/146)
n BE without intraepithelial neoplasia whilst 59,59% (87/146) expression ofhosphorylated pRB was detected.Conclusions:Expression ofn(der)phosphorylated pRB are common events in Barrett adenocarcinoma.hese data adress that un(der)phosphorylated pRB may be a novel biomarker forE and that its expression may help to predict the prognosis of this pathology.n the future, the use of this procedure could play an important role in thevaluation of patients with BE.
1487hat Should We Do With the Remainder of the Barrett’s
egment After Endoscopic Resection of Early Barrett’s Cancer?ntermediate Results of the First Prospective-Randomized Trialn the APC Ablation of Residual Barrett’s Mucosa Withoncomitant Esomeprazole Therapy Versus Surveillanceithout Ablation After ER of Early Barrett’s Cancerendrik Manner, Thomas Rabenstein, Kirsten Braun, Andrea May,liver Pech, Juergen Pohl, Christian Ellackground: Retrospective data indicate that thermal ablation of the remainderf the Barrett’s segment after endoscopic resection (ER) of early Barrett’s canceray lead to a lower rate of metachronous lesions. Up to now, this issue has notet been clarified in a prospective randomized trial. Study aim: To evaluate theumor-free survival after argon plasma coagulation (APC) ablation of residualon-neoplastic Barrett’s mucosa with concomitant PPI treatment versusurveillance without ablation in patients cured from early Barrett’sancer.Methods: Patients cured from early Barrett’s cancer by means of ER andaving a remainder of the Barrett’s segment of at least 2 cm in extent wereandomely assigned to undergo either APC ablation of the Barrett’s segment withoncomitant PPI treatment (esomeprazole 2 x 40 mg daily) or surveillanceithout ablation. Endoscopic check-up examinations including 4-quadrantiopsies were performed in six-monthly intervals. Results: A total of 68 patients61 male, 89.7%; mean age 63�10 yrs) were included in the study (APC group�38; surveillance n�30). 12 patients withdrew from the study. 29 of theemaining 56 patients had been assigned to undergo APC ablation. The meanumber of APC sessions required to achieve Barrett’s ablation (�90%) was.9�1.4 (range 2-7; 1 patient under therapy). No metachronous lesions occureduring a mean follow-up of 19.5 months. In 8 of 27 patients (29.6%) assigned toeceive surveillance without ablation, metachronous lesions (high-gradentraepithelial neoplasia or early Barrett’s cancer) were observed during a meanollow-up of 18.9 months. The tumor-free survival differed significantly betweenhe two groups (p�0.003; log rank).Conclusions: According to these intermediateesults, thermal ablation of the remainder of the Barrett’s segment withoncomitant PPI treatment appears to effectively reduce the rate ofetachronous lesions after curative ER of early Barrett’s cancer.*This study was
upported by Astra Zeneca, Wedel, Germany
1488istopathologic Features of Early Barrett’s Cancer Invading theubmucosal Layer: Assessment of Endoscopic Resectionpecimens in a Large Cohort of Patientsendrik Manner, Oliver Pech, Christian Ell, Michael Viethackground: For measurement of invasion depth of Barrett’s cancer (BC) into theubmucosal layer and defining the risk of lymph node metastasis, the pragmaticpproach of dividing the submucosa (sm) in 3 equal thirds (sm1-sm3) is widelysed during the histological work-up of ER specimens. A measurement inicrons of depth of invasion may in general be more precise, but clinicalxperience is very limited. Data on histopathological features of tumors invadinghe deep submucosa are still lacking.Study aim: To evaluate the invasion depthf endoscopically resected BC into the submucosa in microns and to compare ito the semiquantitative approach of dividing the submucosa in 3 equal thirds;nd to assess grade of tumor differentiation (G-status), lymphangio invasion (L-tatus), and tumor-cell dissociation (TCD) at the invasion front.Methods: ER
pecimens of 46 patients (pt) treated between 1996 and 2005 and diagnosed byeans of ER to have early BC with sm invasion and tumor-free basal marginsww.giejournal.org Volu
were reassessed for quantitative measurement of depth of invasion in microns(�m) and tumor-cell dissociation at the invasion front. At the time of initialdiagnosis, the depth of infiltration had been estimated semiquantitatively intosm1-sm3. In case of piecemeal resection, maximum depth of invasion waschosen for analysis. According to experiences in early gastric cancer, the cutofflimits between sm1 and sm2 were defined to be 500�m, and between sm2 andsm3 1000�m, respectively. Results: 21/46 pt had sm1 lesions; the mean depth ofinvasion (MDI) into the sm was 506�279�m (range 101-1100). In the 8 pt withsm2 lesions, MDI was 730�205�m (400-1100; p�0.05). In the 16 pt with sm3lesions, it was 1029�513�m (230-2100; p�0.130). There was no significantdifference in the MDI when comparing sm1 to sm2, and sm2 to sm3 lesions. In 1pt, semiquantitative definition of invasion depth had not been possible (smXlesion). Using the cutoff limits defined, the MDI was above the limit of 500�m insm1 lesions. The number of G3 lesions was significantly higher in sm3 lesions(13/16, 81%) in comparison with sm1 lesions (5/21, 24%; p�0.000). L1 statuswas found in a significant higher proportion of sm3 (10/16; 63%) in comparisonwith sm1 lesions (4/21, 19%; p�0.012). TCD3 was found more often in sm3 (9,56%) than in sm1 lesions (1/21, 5%; p�0.000).Conclusions: Low tumordifferentiation, lymphangio invasion and a high grade of TCD is found morefrequently in case of deep submucosal invasion of early Barrett’s cancer. Thewidely used method of subdividing the submucosal layer in three equal thirdscannot automatically be replaced by a quantitative measurement in microns.
S1489Predictive Capabilities of APACHE III, MELD, and Rockall Scorein Acute Variceal HemorrhageHelen Fasanya-Uptagraft, Robert T. Lapp, Kenneth E. Wood,Deepak V. Gopal, Mark Reichelderfer, Patrick Pfau, Jennifer WeissBACKGROUND: Acute Variceal Hemorrhage (AVH) carries a high risk ofmortality. A number of scoring systems have been proposed to predict patientoutcomes. AIM: To assess the predictive capabilities of three prognostic models -APACHE III (Acute Physiology and Chronic Health Evaluation), MELD (Model forEnd-Stage Liver Disease) and Rockall in patients presenting with AVH.METHODS: 68 admissions to our ICU with AVH over a four year time periodwere studied. Patients were assigned an APACHE III Score on day of admissionto the ICU with subsequent calculation of MELD and Rockall scores. Data wascollected on the following outcomes for each patient: length of ICU stay, numberof endoscopies, EGD findings and therapy, need for SB (Sengstaken-Blakemore)tube, total blood transfusion requirements, rate of rebleeding, rate of readmissionwithin 30 days, 30 day and in-hospital mortality, and cost of hospitalization. Afteradjusting for age and sex, regression analysis was performed to evaluatepredictive capabilities of APACHE III, MELD and Rockall in AVH. RESULTS: Inthis cohort, in-hospital mortality rate was 16.2% with a rate of 19.1% at 30 days.35% of patients required more than one EGD. APACHE III score significantlycorrelated with 30 day mortality (p�0.0001), in-hospital mortality (p�0.0001),mean number of transfused pRBCs (p�0.001), length of ICU stay (p�0.001),need for SB tube (p�0.036), and cost of hospitalization (p�0.002). MELD scoresignificantly predicted 30 day and in-hospital mortality (both p�0.0001), meannumber of transfused pRBCs (p�0.006) and cost of hospitalization (p�0.016).Rockall significantly correlated with length of ICU stay (p�0.040), need forendoscopic therapy (p�0.022), mean number of transfused pRBCs (p�0.019)and cost (p�0.037), but did not correlate with 30 day or in-hospital mortality.CONCLUSION: APACHE III and MELD scores have accurate predictive capabilityof clinical outcomes in patients with AVH. Rockall score is limited by its inabilityto predict 30 day or in-hospital mortality in patients with variceal bleeding.
S1490High Prevalence of Columnar Lined Esophagus in Patients WithChronic Gastroesophageal Reflux Disease: Implications forDisease DefinitionsMandeep Singh, Srinivas Gaddam, Vikas Singh, Neil Gupta,Sachin B. Wani, Brian Moloney, April D. Higbee, Ajay Bansal,Amit Rastogi, Prateek SharmaBackground: Although Barrett’s esophagus (BE) has traditionally been defined asa columnar lined esophagus (CLE) with biopsies confirming intestinal metaplasia(IM), recently, there has been discussion to define all CLE as BE. We examinedthe clinical burden of the disease if BE was defined as all CLE irrespective of thepresence or absence of IM Aim: To prospectively determine the prevalence ofCLE in a large cohort of patients undergoing endoscopy for refluxsymptoms.Methods: Consecutive patients presenting to the endoscopy unit (at atertiary referral center) for their index endoscopy for evaluation of GERDsymptoms were enrolled in this prospective cohort study. Patients were asked tocomplete a validated GERD questionnaire (GERQ) that documents the onset ofGERD symptoms (heartburn, acid regurgitation) and grades the frequency andseverity of symptoms experienced over the past year. Demographic information,
BMI, smoking history, use of PPIs and aspirin/NSAIDs were recorded.Endoscopic details including length of CLE, presence and size of hiatal herniame 71, No. 5 : 2010 GASTROINTESTINAL ENDOSCOPY AB175