RT: Case of the swollen Leg
description
Transcript of RT: Case of the swollen Leg

RT: CASE OF THE SWOLLEN LEG
Cimi AchiamMD, DTMH, FRCPC

FIRST VISIT: SEPT 14, 2011 12:25:
50 yr male cc: L leg swelling 6 days of L leg swelling Transient SOBOE w/ mildly pleuritic chest pain
yesterday, but completely resolved on presentation
PMHx: L DVT Jan 2011
Precipitated by flight to Hawaii Tx w/ 6/12 of Warfarin D/C in mid June
No meds currently Family Hx: nil

VISIT 1 O/E:
T37.2 HR 70 BP 145/78 RR20 Sat 96% RA Chest: GAEBL, clear CVS: S1S2 N, no murmur Abdo: Soft NT, not distended Neuro: Normal L Leg: proximal swelling

VIST 1 INVESTIGATIONS 6 Pack: -
D dimer: 646
Troponin: -

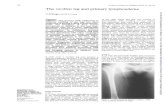
VISIT 1: IMAGING CTPA:
no PE, mildly prominent R hilar node of uncertain clinical significance
CT Abdo/Pelvis: No large pelvic mass causing obstruction of veins No acute intra-abdominal abnormality Questionable narrowing of the left common iliac vein at the level of
the overlying right common illiac artery ? May-Thurner syndrome. Recommend Interventional Radiology consult. If there is still significant
clinical concern, an MRV could be attempted or a CTV could be reattempted with a longer delay between contrast and imaging
Doppler US: - DVT, deep venous system widely patent No residual thrombus identified Normal waveforms, phasicity, augmentation, and compression were
obtained

VISIT 1 Given high clinical concern for DVT, case was
discussed with radiologist and plan was made for MR venogram next day
Pt was tx in the mean time with Enoxaparin 1.5mg/kg SC

VISIT 2: SEPT 16, 2011 13:42: Return for MRI results
Patient’s leg re-examined: Pt looks well, no pedal swelling, good circulation to L foot
MR Venogram of Pelvis & Thighs: Negative MR venogram with no evidence of DVT in the
pelvis and LE to just above the knees
Pt instructed to return on an as needed basis

VISIT 3: SEPT 20, 2011 Patient represented with progressive swelling
of his L leg, non- painful, no paraesthesias. No CP or SOB currently or since last evaluation
O/E: Abdomen: Soft NT, no masses or inguinal
lymphadenopathy LE: non-pitting edema from foot to mid thigh, no
erythema, normal pedal pulses and motor exam

VISIT 3 Given multiple investigations on previous
visits case was discussed with radiology Repeat Doppler U/S planned
Doppler U/S report: Occlusive thrombus seen within the left external iliac
vein Non-occlusive thrombus within one branch of both of
the duplicated superficial femoral, and popliteal veins
? May Thurner’s syndrome

VISIT 3 On suggestion of radiology, interventional radiology
consulted re: possibility of thrombolysis/stenting Was informed would have to consult vascular surgery and
that they would consult IR if required
Vascular surgery consult Pt was admitted and anticoagulated with IV heparin
protocol
Sept 21/11: Pt underwent thrombolysis & stenting of his left
iliac vein Pt advised to restart IV heparin and continue
coumadin x 6 mo minimum

PATHOPHYSIOLOGY OF MAY THURNER SYNDROME

VIRCHOW’S TRIAD

ANATOMY

MAY THURNER SYNDROME Most commonly seen in women between 20-50yrs
Episodes of DVT may be recurrent and/or poorly responsive to treatment with anticoagulation alone May require:
Catheter-directed thrombolysis Venous angioplasty and/or intravascular stenting
Visualization of a clot this high in the pelvis may be difficult to detect using ultrasound of LE If DVT is strongly suspected, further testing should be
performed

DIAGNOSIS OF SUSPECTED DVT OF LE Only a minority of patients (17 and 32 % in
two large series) actually have the disease
Accurate diagnosis is essential Potential risk of fatal PE in untreated proximal LE
DVTs Potential risk of fatal bleeding due to
anticoagulating a patient who does not have a DVT
Birdwell BG, et al. Ann Intern Med 1998; 128:1-5Huisman MV, et alN Engl J Med 1986; 314:823

DIAGNOSIS OF SUSPECTED LE DVT Pre-test probability:
Modified Well’s Score
Imaging: “Doppler” Compression U/S
Abnormal compressibility of the vein Abnormal Doppler color flow The presence of an echogenic band Abnormal change in diameter during valsalva
maneuver
Non-compressibility is 95% Sens & Spec for a proximal DVT

DIAGNOSIS OF SUSPECTED LE DVTS

DIAGNOSTIC IMAGING MODALITIES: BEYOND U/S Contrast Venography
Non-invasive Tests: Impedance Plethysmography
Sensitivity 91%; Specificity 96 %
MRI Venography Sens 100%; Spec 96%
CT Venography

AT RCH: HIGH SUSPICION & - DOPPLER U/S Options:
Order D-dimer: if positive bring patient back for repeat U/S in 5-7 days
Order more imaging: CT Venogram
May be best option to rule out causes of pelvis compression ie mass and to assess iliac vessels
MR Venogram Repeat U/S in 1 week without D-dimer

MANAGEMENT OF DVTS: BEYOND ANTICOAGULATION Thrombolytics Surgical thrombectomy Percutaneous mechanical thrombectomy
Potential indications: Hemodynamically unstable PE Massive iliofemoral thrombosis May Thurner syndrome

THROMBOLYTICS May result in more rapid and complete lysis
of LE DVT & less post-thrombotic syndrome
However, seldom used because: Clinical relevance of achieving earlier relief of
venous obstruction is uncertain Increased risk of major bleeding Low risk of death and early recurrence if
anticoagulants are started promptly at an appropriate dose
Increased risk of catastrophic bleeding may not be worth preventing post-thrombotic syndrome

THROMBOLYTICS Indications:
Massive proximal LE or iliofemoral thrombosis PLUS Severe symptomatic swelling or Limb-threatening ischemia (phlegmasia cerulea
dolens)

TAKE HOME POINTS In patients with recurrent left sided DVT
consider May Thurner syndrome
In patients with a high probability of DVT a single negative U/S study may be insufficient Repeat the U/S in 5-7 days or Consider adding a D-dimer at the time of the
initial workup or Consider other imaging modalities ie CT
venogram