Role of Dentist in Sleep Therapy
-
Upload
randy-clare -
Category
Health & Medicine
-
view
769 -
download
1
description
Transcript of Role of Dentist in Sleep Therapy

Randy Clare and Associates 1
Comprehensive Sleep Therapy
AASM Guidelines and what to make of them
1/21/12

Randy Clare and Associates 2
Who is Randy Clare Anyway
• 1990’s – The Silencer• 2000 – The Diagnostic years
– SensorMedics – Viasys– Cardinal Health– CareFusion– CPAP Accessories DME
• 2011 – SleepScholar– DDMEonline.com– Scottsdalestudyclub.com
1/21/12

Randy Clare and Associates 31/21/12

Randy Clare and Associates 41/21/12

Randy Clare and Associates 5
Positive airway pressure is the treatment of choice for mild moderate and severe OSA and should be offered as an option to all patients
1/21/12

Randy Clare and Associates 61/21/12

Randy Clare and Associates 7
Patient Motivated to Seek Help
Primary Care Physician80%
Other Specialist10%
Self Referral10%
Specialist Assessment
Otolaryngologist(ENT surgeon)
5%
Pulmonologist80%
Neurologist10%
Psychologist/Psychiatrist
Dentist
Diagnostic Stage at Sleep Lab or in Home
Attended Sleep Lab(USA)
Unattended Study – Home
SNSDiagnosis for half of the night and therapy for the second half
PSGFull sleep study in a sleep laboratory
PPSGLess sophisticated studies requiring simpler analysis
HST Device
Studies carried out at the patients home. Attended or unattended
Therapy typically provided by Home Care Provider
CPAP Device
OSA Patient Diagnostic & Therapy Flow
Masks (2-4 per year)
1/21/12

Randy Clare and Associates 8
CPAP at DME
• Competitive bidding is driving consolidation of providers (easy for payors not easy for patients)
• Largest DME providers are Lincare, Apria, Rotech
• 15-20% of Sleep Labs are now dispensing CPAP
1/21/12

Randy Clare and Associates 9
CPAP at Dental Office?
• Who better than a dentist• Need an RT due to the Pharmacy Board rules• 3 month recall• Steady income Stream• Unequivocal participation in the medical
model• Therapeutic neutrality fits the patient
expectation of superlative care
1/21/12

Randy Clare and Associates 10
Mask Replacement
• Ideally every 6 months• Minimum yearly• Insurance dictates• Notify customer• Compliance Program• Select a reasonably priced mask
1/21/12

Randy Clare and Associates 11
HOW OFTEN DO YOU REPLACE YOUR MASK? n= 2800 patients
• 5% - Every 3 months• 16% - Every 4 to 6 months• 14% - Every 7 to 9 months• 18% - Less than once a year• 48% - Never* TalkAboutSleep.Com Survey n=2800
1/21/12

Randy Clare and Associates 12
Cleaning & Care of Mask
• Select simplistic mask• Instruct on cleaning daily / weekly / monthly mild lanolin free soap no creams or Vaseline no rubbing alcohol no abrasives clean in A.M. rinse well
1/21/12

Randy Clare and Associates 13
HOW OFTEN DO YOU CLEAN YOUR MASK?
HOW OFTEN DO YOU CLEAN YOUR MASK?• 26% - Daily• 7% - 4 to 6 X per week• 22% - 1 to 3 X per week• 27% - 1 to 4 X per month• 15% - less than once a month• 4% - never
* TalkAboutSleep.Com Survey n=2800
1/21/12

Randy Clare and Associates 14
If CPAP use is considered inadequate based on objective monitoring and symptom evaluation, prompt and intensive efforts should be implemented to improve PAP use or consider alternative therapies.
1/21/12

Randy Clare and Associates 15
Weight loss should be recommended for all overweight OSA patients. Weight loss should be combined with a primary treatment of OSA, Because of the low success rate of dietary programs and the low cure rate by dietary approach alone.
1/21/12

Randy Clare and Associates 16
Sleep position can affect airway size and patency with a decrease in the area of the upper airway, particularly in the lateral dimension, while in the supine position.
Positional therapy, consisting of a method that keeps the patient in a non supine position is an effective secondary therapy or can be supplement to primary therapies for OSA in patients who have a low AHI in the non supine versus that in the supine position
1/21/12

Randy Clare and Associates 17
Behavioral Strategies
• Weight loss• Exercise• Positional Therapies• Avoidance of Alcohol and Sedatives
1/21/12

Randy Clare and Associates 18
• Obesity is the most powerful risk factor for obstructive sleep apnea (OSA)
• Obesity is essentially the only reversible risk factor• Potentially modifiable risk factors for OSA also
include alcohol, smoking, nasal congestion, and estrogen depletion in menopause.
• Data suggest that obstructive sleep apnea is associated with all these factors, but at present the only intervention strategy supported with adequate evidence is weight loss. ( Young et al. 2002)
Background
1/21/12

Randy Clare and Associates 19
Obesity and OSA
• About 70% of those with OSA are obese (Malhotra et al 2002)
• Prevalence of OSA in obese men and women is about 40% (Young et al 2002)
• Higher BMI associated with higher prevalence– BMI>30: 26% with AHI>15, 60% with AHI>5– BMI>40: 33% with AHI>15, 98% with AHI>5 (Valencia-flores 2000)
1/21/12

Randy Clare and Associates 20
Obesity and OSA
• Total body weight, BMI, and fat distribution all correlate with odds of having OSA– Every 10 kg increase in weight increases risk by 2X– Every increase in BMI by 6 increases risk by 4X– Every increase in waist or hip circumference by 13
to 15 cm increases risk by 4X (Young et al 1993)
1/21/12

Randy Clare and Associates 21
1 month on Take Shape for life program > 25 LBs lostBMI start 35BMI 3 months later 28Total weight loss to date 50Lbs
October 25 2011 November 28 2011 January 11 2012
1/21/12

Randy Clare and Associates 22
Body Position
1/21/12

Randy Clare and Associates 231/21/12

Randy Clare and Associates 24
A PM should at minimum, record airflow, respiratory effort, and blood oxygenation. The type of biosensors used to monitor these parameters for in-laboratory PSG are recommended for use in PMs and include an oronasal thermal sensor to detect apneas, a nasal pressure transducer to measure hypopneas, oxymetry, and ideally, calibrated or uncalibrated inductance plethysmography for respiratory effort (RIP). (Consensus)
1/21/12

Randy Clare and Associates 25
17 Channels- Simplified
1.Cannulla airflow2.RIP derived airflow (backup)3.Snore from cannulla4.PAP pressure5.Snore channel from audio recording6.Audio playback7.BPOS – 3 axis gravity sensor8.Actigraphy9.Pleth waveform - wireless10.Heart rate - wireless11.SPO2 – wireless12.Thoracic effort RIP13.Abdomen effort RIP14.ExG1 – user configurable (ie.,bruxism)15.ExG2 – user configurable (ie., ECG)16.Pulse Transit Time17.Heart Rate Variability
Redundancy(but in a good way)
1/21/12

Randy Clare and Associates 26
Validation Plot for T3-AHI
1/21/12

Randy Clare and Associates 27
Embletta and the T3 Evolution of HST
1/21/12

Randy Clare and Associates 28
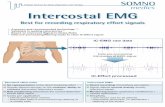
Measuring Bruxism
Software Setup
Electrode Placement
1/21/12

Randy Clare and Associates 29
Sample Bruxism Report There was bruxism, snoring, apneas and hypopneas associated with arterial oxygen desaturations. The number of bruxism events was 45 providing ABI of 0.9. The overall apnea/hypopnea index (AHI) was 17.5. The supine apnea/hypopnea index was 17.5. The mean arterial oxygen saturation was 94%. The lowest arterial oxygen saturation was 86% Findings are consistent with 1. Severe sleep related bruxism 327.53 2. Moderate obstructive sleep apnea syndrome 327.23. Recommendations: Since the ABI is relatively high, consider a dental consultation for an oral appliance. This patient has moderate OSA. Therapeutic options include: The patient may benefit from the use of a nocturnal mandibular repositioning
– appliance. If that line of therapy is to be pursued, the patient should be evaluated by – a dentist specialized in the treatment of sleep related breathing disorders taking into – account the presence of Bruxism…. (ask for a full copy of the report)
1/21/12

Randy Clare and Associates 301/21/12

Randy Clare and Associates 31
Three things to consider for Monday
• Do I consider Bruxism when I consult sleep patients? Sleep for Bruxism patients?
• When I talk sleep do my eyes wander to Neck? Hips and Belly? Do I estimate BMI?
• Should I talk to my office manager about our attitude around CPAP? Is there a local DME I can work with? Should I consider providing CPAP?
1/21/12