Rheumatic Fever by Adnan Bhutto
-
Upload
adnan-bhutto -
Category
Documents
-
view
8.358 -
download
2
description
Transcript of Rheumatic Fever by Adnan Bhutto

RHEUMATIC FEVER
PRESENTED BY
ADNAN AHMED BHUTTOHamdard University Karachi, Pakistan
04/12/23 1

OBJECTIVES
• ETIOLOGY• EPIDEMIOLOGY• PATHOGENESIS• CLINICAL FEATURES• INVESTIGATIONS• DIAGNOSIS• TREATMENT
04/12/23 2

ETIOLOGY
• Acute Rheumatic Fever is an inflammatory disease with devastating sequalae.
• It resulting from infection of upper respiratory tract by group A beta hemolytic streptococcal infection.
• It is a diffuse inflammatory disease of connective tissue, primarily involving heart, blood vessels, joints, subcutaneous tissue and brain.
04/12/23 3

EPIDEMIOLOGY• Important cause of chronic heart
disease and death in developing countries.
• More common in third world countries.• Commonly occurs in 5-15 years of age.• Male and Female are equally effected.• Overcrowding, poverty, lack of access
to medical care contributes to transmission.
• Incidence is more in cold months
04/12/23 4

PATHOGENESIS
• Delayed immune response to infection with group A beta hemolytic streptococci.
• After a latent period of 1-3 weeks, antibody induced immunological damage occur to heart valves, joints, subcutaneous tissue & basal ganglia of brain.
• Antibodies made against group A strep cross react with human tissue.
04/12/23 5

Group A Beta Hemolytic Streptococcus
• Strains that produces rheumatic fever -
M types l, 3, 5, 6,18 & 24• Pharyngitis- produced by GABHS can lead to-
acute rheumatic fever , rheumatic heart disease & post strept. Glomerulonepritis
• Skin infection- produced by GABHS leads to post streptococcal glomerulo nephritis only. It will not result in Rh.Fever or carditis as skin lipid cholesterol inhibit antigenicity
04/12/23 6

04/12/23 7
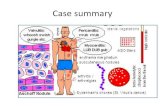
Diagrammatic structure of the group A beta hemolytic streptococcus
Cytoplasm
Cyto.membrane
Peptidoglycan
Group carbohydrate
Protein antigens
Cell wall
Capsule
Antigen of outer protein cell wall of GABHS induces antibody response in victim which result in autoimmune damage to heart valves, sub cutaneous tissue,tendons, joints & basal ganglia of brain

Pathologic lesions • Fibrinoid degeneration of connective
tissue,inflammatory edema, inflammatory cell infiltration & proliferation of specific cells resulting in formation of Ashcoff nodules, resulting in-
- Pancarditis in the heart
- Arthritis in the joints
- Ashcoff nodules in the
subcutaneous tissue
- Basal gangliar lesions resulting in chorea
04/12/23 8

Rheumatic Carditis Histology
04/12/23 9

Histology of Myocardium in Rheumatic Carditis
04/12/23 10

CLINICAL FEATURES1. ARTHIRITIS • Most common feature occurs in 80%
of patients.• Flitting & fleeting migratory
polyarthritis, involving major joints• Commonly involved joints knee,
ankle, shoulders, elbow & wrist• Involved joints becomes tender.• In children below 5 yrs arthritis usually mild
but Carditis more prominent• Arthritis do not progress to chronic disease
04/12/23 11

04/12/23 12Showing ARTHIRITIS In knee joint

2. Carditis
04/12/23 13
• Manifest as pancarditis(endocarditis, myocarditis and pericarditis),occur in 40-50% of cases
• Carditis is the only manifestation of rheumatic fever that leaves a sequelae & permanent damage to the organ
• Valvulitis occur in acute phase• Chronic phase- fibrosis, calcification &
stenosis of heart valves (fishmouth valves)

• Clinical Signs:• High Pulse rate• Murmurs• Cardiomegaly• Rhythm disturbances(Prolonged PR
intervals • Pericardial Friction rubs• Cardiac Failure
04/12/23 14
1.Carditis (Contd.)

04/12/23 15
Rheumatic heart disease. Abnormal mitral valve. Thick, fused chordae

04/12/23 16
Another view of thick and fused mitral valves in Rheumatic heart disease

04/12/23 17

3. Sydenham’s Chorea
• Occur in 10-15% of patients with rheumatic fever.
• Mainly in girls resulting from disorder of extra pyramidal system.
• Fast, Clonic, involuntary movements (especially face and limbs)
• Emotionally liability• Muscular Hypotonus• Clinically difficulty in Walking, Talking and
Writing.• It is self limiting but may last from few
weeks to six months and rarely up to 1-2 years.
04/12/23 18

04/12/2319
•It is self limiting but may last from few weeks to six months and rarely up to 1-2 years.• Chances of reoccurrence are recorded. Shown in table.
3. Sydenham’s Chorea

04/12/23 20

4.Subcutaneous Nodules• Occur in 5% of patients • Painless, pea-sized, palpable
nodules.• Mainly over extensor surfaces of
joints, spine, scapulae & scalp.• Associated with strong seropositivity• Always associated with severe
Carditis
04/12/23 21

5.Erythema Marginatum
• Occur in 5%of children.• Unique, transient, serpiginous-looking
lesions of 1-2 inches in size.• Pale center with red irregular margin• More on trunks & limbs & non-itchy• Worsens with application of heat• Often associated with chronic Carditis
04/12/23 22

04/12/23 23
OTHER CLINICAL FEATURES
• Fever• Arthralgia• Epistaxis• Abdominal pain due to Peritonitis• Hematuria due to involvement of kidneys• Pneumonitis• Mild Pleuritis (5-10%)• Encephalitis (extremely rare)

04/12/23 24
LABORTARY INVESTIGATIONS•High ESR•Anemia, leucocytosis•Elevated C-reactive protien•ASO titre >200 Todd units. (Peak value attained at 3 weeks, then comes down to normal by 6 weeks)• Anti-DNAse B test• Throat culture-GABHstreptococci
• ECG- prolonged PR interval, 2nd or 3rd degree blocks,ST depression, T inversion
•2D Echo cardiography- valve edema, mitral regurgitation, LA & LV dilatation,pericardial effusion, decreased contractility

Diagnosis
• Rheumatic fever is mainly a clinical diagnosis
• No single diagnostic sign or specific laboratory test available for diagnosis
• Diagnosis based on MODIFIED JONES CRITERIA
04/12/23 25

04/12/23 26
Jones Criteria (Revised) for Guidance in the Diagnosis of Rheumatic Fever*
Major Manifestation Minor Manifestations
Supporting Evidence of Streptococal Infection
Carditis Polyarthritis
Chorea Erythema Marginatum
Subcutaneous Nodules
Clinical Laboratory
Increased Titer of Anti-Streptococcal Antibodies ASO (anti-streptolysin O), others Positive Throat Culture for Group A Streptococcus Recent Scarlet Fever
Previous rheumatic fever or rheumatic heart disease Arthralgia Fever
Acute phase reactants: Erythrocyte sedimentation rate, C-reactive protein, leukocytosis Prolonged P-R interval
*The presence of two major criteria, or of one major and two minor criteria, indicates a high probability of acute rheumatic fever, if supported by evidence of Group A streptococcal nfection.

Exceptions to Jones Criteria
Chorea alone, if other causes have been excluded
Insidious or late-onset Carditis with no other explanation
Patients with documented RHD or prior rheumatic fever, one major criterion, or of fever, arthralgia or high CRP suggests recurrence
04/12/23 27

Differential diagnosis
• Juvenile rheumatoid arthritis
• Septic arthritis
• Sickle-cell arthropathy
• Kawasaki disease
• Myocarditis
• Scarlet fever
• Leukemia04/12/23 28

treatment
• Step I - primary prevention (eradication of streptococci)
• Step II - anti inflammatory treatment (aspirin, steroids)
• Step III- supportive management & management of
complications• Step IV- secondary prevention
(prevention of recurrent attacks)04/12/23 29

04/12/23 30
STEP I: Primary Prevention of Rheumatic Fever
(Treatment of Streptococcal Tonsillopharyngitis)
Agent Dose Mode Duration
Benzathine penicillin G 600 000 U for patients Intramuscular Once 27 kg (60 lb) 1 200 000 U for patients >27 kg
or Penicillin V Children: 250 mg 2-3 times daily Oral 10 d (phenoxymethyl penicillin) Adolescents and adults: 500 mg 2-3 times daily
For individuals allergic to penicillin
Erythromycin: 20-40 mg/kg/d 2-4 times daily Oral 10 d Estolate (maximum 1 g/d
or Ethylsuccinate 40 mg/kg/d 2-4 times daily Oral 10 d
(maximum 1 g/d)

Step II: Anti inflammatory treatment
04/12/23 31
Arthritis only
Aspirin 75-100 mg/kg/day,give as 4 divided doses for 6 weeks (Attain a blood level 20-30 mg/dl)
Carditis Prednisolone 2-2.5 mg/kg/day, give as two divided doses for 2 weeks Taper over 2 weeks & while tapering add Aspirin 75 mg/kg/day for 2 weeks. Continue aspirin alone 100 mg/kg/day for another 4 weeks
Clinical condition Drugs

Step III: Supportive Management & Management of complications
• Bed rest • Treatment of congestive cardiac
failure: -digitalis, diuretics• Treatment of chorea:
diazepam or haloperidol • Rest to joints & supportive
splinting
04/12/23 32

04/12/23 33
STEP IV : Secondary Prevention of Rheumatic Fever
(Prevention of Recurrent Attacks)
Agent Dose Mode
Benzathine penicillin G 1 200 000 U every 4 weeks* intramuscularor
Penicillin V 250 mg twice daily Oral
or
Sulfadiazine 0.5 g once daily for patients 27 kg (60 lb Oral 1.0 g once daily for patients >27 kg (60 lb)
For individuals allergic to penicillin and sulfadiazine
Erythromycin 250 mg twice daily Oral
*In high-risk situations, administration every 3 weeks is justified and recommended

04/12/23 34
Duration of Secondary Rheumatic Fever Prophylaxis
Category Duration
Rheumatic fever with carditis and At least 10 y since last residual heart disease episode and at least until (persistent valvar disease*) age 40 y, sometimes lifelong
prophylaxis
Rheumatic fever with carditis 10 y or well into adulthood, but no residual heart disease whichever is longer (no valvar disease*)
Rheumatic fever without carditis 5 y or until age 21 y,
whichever is longer
*Clinical or echocardiographic evidence.

Prognosis• Rheumatic fever can recur
whenever the individual experience new GABH streptococcal infection, if not on prophylactic medicines
• Good prognosis for older age group & if no carditis during the initial attack
• Bad prognosis for younger children & those with carditis with valvular lesions
04/12/23 35

04/12/23 36