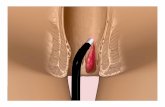
Revised Case Report- Hemorrhoids
-
Upload
christinalove08 -
Category
Documents
-
view
128 -
download
13
Transcript of Revised Case Report- Hemorrhoids

I. INTRODUCTION
“There are three wicks you know to the lamp of a man's life: brain, blood, and breath.
Press the brain a little, its light goes out, followed by both the others. Stop the heart a
minute, and out go all three of the wicks. Choke the air out of the lungs, and presently
the fluid ceases to supply the other centres of flame,
and all is soon stagnation, cold, and darkness.”
-Oliver Wendell Holmes, Sr.
Health is an essential part of a person; it is the fuel which gives every
individual the physical drive needed to conquer a day. Without it no man can
survive, a deficiency in health impairs the normal functioning of a person, it
becomes a hindrance. Health pertains to the person’s body systems as a whole,
it is not achieved if even only one body system is impaired, a good heart with
weak lung still does not signal health, there should be harmony and balance
between the systems to achieve ultimate health.
Hemorrhoids
Hemorrhoids are swollen veins in the anal canal. This common problem
can be painful, but it’s usually not serious. Veins can swell inside the anal canal
to form internal hemorrhoids. Or they can swell near the opening of the anus to
form external hemorrhoids. It is possible to have have both types at the same
time. The symptoms and treatment depend on which type is existent.
Internal hemorrhoids
With internal hemorrhoids, there is visible bright red streaks of blood on
toilet paper or bright red blood in the toilet bowl after a normal bowel movement.
Blood is also visible on the surface of the stool.
Internal hemorrhoids often are small, swollen veins in the wall of the anal
canal. But they can be large, sagging veins that bulge out of the anus all the
time. They can be painful if they bulge out and are squeezed by the anal
Hemorrhoids - Page | 1

muscles. They may be very painful if the blood supply to the hemorrhoid is cut
off. If hemorrhoids bulge out,mucus may also be seen on the toilet paper or stool.
External hemorrhoids
External hemorrhoids can bleed, and then the blood pools, causing a hard painful
lump. This is called a thrombosed, or clotted, hemorrhoid.
Prevelance statistics about Hemorrhoids:The following statistics relate to the
prevalence of Hemorrhoids:
47 per 1000 people (NHIS95);1.0% of male population self-reported having
haemorrhoids in Australia 2001 ;1.1% of population self-reported having
haemorrhoids in Australia 2001 ;1.2% of female population self-reported having
haemorrhoids in Australia 2001 ; 209,000 people self-reported having
haemorrhoids in Australia 2001; 120,000 women self-reported having
haemorrhoids in Australia 2001 ;89,000 men self-reported having haemorrhoids
in Australia 2001 (ABS 2001 National Health Survey, Australia’s Health 2004,
AIHW) (retrieved from the website:
http://www.wrongdiagnosis.com/h/hemorrhoids/stats.htm)
A different method for the treatment of haemorrhoids was introduced back
in the late 1990s, it is called “Stapling”. Stapling became a popular alternative for
hemorrhoidectomy because, it entailed faster healing, lesser pain, and lesser
occurrence of itching. Although a study was conducted wherein out of 269
stapling patients, 23 suffered recurrences, compared with four recurrences
among 268 patients in the surgical-removal group, it showed a higher recurrence
rate than that of the surgical removal procedure.
With this result, the authors still considered excisional surgery as the gold
standard of the surgical treatment of haemorrhoids. Excisional surgery came with
no or minimal recurrences, it may not entitle faster healing and lesser pain that of
Stapling but it guarantees the lesser risk of recurrence after the procedure and
Hemorrhoids - Page | 2

recovery. The article confronts the main concern of hemorrhoid surgical
treatment which is the longterm outcome.
(Source:
http://www.doctorslounge.com/surgery/news/hemorrhoid_stapling_risks.shtml)
This information about haemorrhoid Stapling gives both nurses and
doctors knowledge about the procedure, its benefits and consequences. Through
the facts they could be more knowledgeable and may give more info to their
patients regarding what procedure may be beneficial to them or which procedure
would the patient prefer. And for doctors, they can have better judgement and be
able to suggest a suitable procedure for a patient to undergo hemorrhoidectomy.
For nurses, it can help by giving them an idea as to what should they be
anticipating in terms of post-surgical outcomes, and give them a plan to create
their nursing care plans for a post-op hemorrhoidectomy patient, plus be able to
give effective health teachings.
Hemorrhoids - Page | 3

II. ANATOMY AND PHYSIOLOGY
Lower Gastrointestinal Tract
The lower gastrointestinal tract comprises most of the intestines and the anus.
Bowel or intestine
o Small intestine , two of the three parts:
Duodenum - Here the digestive juices from pancreas and
liver mix together
Jejunum - It is the midsection of the intestine, connecting
Duodenum to Ileum.
Ileum - It has villi. All soluble liquid absorbs here with blood.
o Large intestine , which has three parts:
Cecum (the vermiform appendix is attached to the cecum).
Colon (ascending colon, transverse colon, descending colon
and sigmoid flexure)
Rectum
Anus
Small Intestine
The small intestine extends from the pyloric sphincter to the ileocecal valve,
where it empties into the large intestine. The small intestine finishes the process
of digestion, absorbs the nutrients, and passes the residue on to the large
intestine. The liver, gallbladder, and pancreas are accessory organs of the
digestive system that are closely associated with the small intestine.
The small intestine is divided into the duodenum, jejunum, and ileum. The small
intestine follows the general structure of the digestive tract in that the wall has a
mucosa with simple columnar epithelium, submucosa, smooth muscle with inner
circular and outer longitudinal layers, and serosa. The absorptive surface area of
the small intestine is increased by plicae circulares, villi, and microvilli.
Hemorrhoids - Page | 4

Exocrine cells in the mucosa of the small intestine secrete mucus, peptidase,
sucrase, maltase, lactase, lipase, and enterokinase. Endocrine cells secrete
cholecystokinin and secretin.
The most important factor for regulating secretions in the small intestine is the presence
of chyme. This is largely a local reflex action in response to chemical and mechanical
irritation from the chyme and in response to distention of the intestinal wall. This is a
direct reflex action, thus the greater the amount of chyme, the greater the secretion.
Large Intestine
The large intestine is larger in diameter than the small intestine. It begins at the
ileocecal junction, where the ileum enters the large intestine, and ends at the
anus. The large intestine consists of the colon, rectum, and anal canal.
The wall of the large intestine has the same types of tissue that are found in
other parts of the digestive tract but there are some distinguishing characteristics.
The mucosa has a large number of goblet cells but does not have any villi. The
Hemorrhoids - Page | 5

longitudinal muscle layer, although present, is incomplete. The longitudinal
muscle is limited to three distinct bands, called teniae coli that run the entire
length of the colon. Contraction of the teniae coli exerts pressure on the wall and
creates a series of pouches, called haustra, along the colon. Epiploic
appendages, pieces of fat-filled connective tissue, are attached to the outer
surface of the colon.
Unlike the small intestine, the large intestine produces no digestive enzymes.
Chemical digestion is completed in the small intestine before the chyme reaches
the large intestine. Functions of the large intestine include the absorption of water
and electrolytes and the elimination of feces.
Rectum and Anus
The rectum continues from the sigmoid colon to the anal canal and has a thick
muscular layer. It follows the curvature of the sacrum and is firmly attached to it
by connective tissue. The rectum and ends about 5 cm below the tip of the
coccyx, at the beginning of the anal canal.
The last 2 to 3 cm of the digestive tract is the anal canal, which continues from
the rectum and opens to the outside at the anus. The mucosa of the rectum is
folded to form longitudinal anal columns. The smooth muscle layer is thick and
forms the internal anal sphincter at the superior end of the anal canal. This
sphincter is under involuntary control. There is an external anal sphincter at the
inferior end of the anal canal. This sphincter is composed of skeletal muscle and
is under voluntary control.
III. THE PATIENT AND HIS ILLNESS
Hemorrhoids - Page | 6

Hemorrhoids - Page | 7
Tenesmus
Increases intra-abdominal pressure Increases hemorrhoidal venous pressure
Non-modifiable
factors
Age (20-50y.o)
Gender
Family history
Pregnancy
Modifiable factors
Obesity
Sedentary lifestyle
Constipation
Chronic Diarrhea
Poor bathroom habits
Postponing bowel movement
Intake of fiber-deprived diet
Cirrhosis of the liver
Prolonged sitting or standing
Distention of the hemorrhoidal veins
Rectal ampulla is filled with formed stool
Venous obstruction
Repeated pressure and obstruction Prolonged pressure and obstruction

B.1. Definition of the disease
Hemorrhoids - Page | 8
Permanently dilation of hemorrhoidal
veins
Enlarged and thrombosed Bleeding and prolapsed
Severe bleeding Thrombosis Hemorrhoidal strangulation
Iron Deficiency Anemia
Intense Pain Cut off blood supply by anal sphincter
Severe pain
Extreme edema
Inflammation
Stapled Hemorrhoidectomy

Hemorrhoids are varicose (swollen or dilated) veins located in or around the
anus. Internal hemorrhoids are varicose veins that surround the rectum and,
when dilated, protrude inside, sometimes extending out of the anus.
Scientists aren't sure why people get hemorrhoids. They are usually not
painful, but they can be bothersome. Hemorrhoid sufferers can frequently and
safely push them back inside.
Certain conditions may cause internal hemorrhoids to bulge, become irritated
and bleed, including:
Trauma during childbirth
The extra weight of pregnancy
Obesity
Chronic constipation with straining
Anal intercourse
Rarely, a bulging internal hemorrhoid may thrombose, meaning a blood clot
may occur.
External hemorrhoids are varicose veins located under the skin on the
outside of the anus. They are frequently painful and usually arise when a blood
clot blocks off the vein.
Hemorrhoids caused by a blood clot, medically referred to as thrombosed
hemorrhoids, need to be treated right away by a doctor. The doctor usually will
remove the blood clot. Otherwise, most cases of hemorrhoids can be treated at
home, with the most important aspect of care being good hygiene. Rarely,
surgery is required to remove them.
B.2. Predisposing / Precipitating factors
Hemorrhoids - Page | 9

Predisposing factors
Age- 20-50 years of age typically have hemorrhoids because they are
within the working age and at the same time reproductive age for
women.
Gender- Females has greater tendency for having hemorrhoids due to
trauma during childbirth and extra weight during pregnancy.
Family History - If the patient has several close relatives who have had
hemorrhoids, the patient may be at an increased risk of hemorrhoids.
Pregnancy – It is due to the pressure on lower part of the body
because of the extra weight of the gravid uterus especially in the third
trimester.
Precipitating factors
Obesity- It is because of the pressure due to heavy weight.
Sedentary lifestyle- Immobility can lead to constipation which can
cause increased abdominal pressure during bowel movement.
Constipation- Straining during chronic constipation can cause internal
hemorrhoids to bulge.
Chronic Diarrhea- Repeated pressure and straining can irritate the
lining of the anus.
Poor bathroom habits- Overly aggressive wiping of the anus can
worsen hemorrhoids.
Postponing bowel movement- Re-absorption of water in the colon can
lead to constipation and possible fecal impaction.
Intake of fiber-deprived diet- No bulk in the food can lead to
constipation.
Cirrhosis of the liver- It can cause pooling of blood in the vessels
around the rectum.
Prolonged sitting or standing- It increases intra-abdominal pressure
and also causes relative venous return.
Hemorrhoids - Page | 10

B.3. Symptoms
Pain and pressure in the anal canal- This is due to cut off blood supply
by anal sphincter and thrombosis.
A grapelike lump on the anus- Collection of varicose (swollen or
dilated) veins located in or around the anus.
Itching and soreness in and around the anus- This is due to the
permanently dilation of hemorrhoidal veins.
Blood on underwear, toilet paper, the surface of the stool, or in the
toilet bowl- This happens when they are irritated during straining.
Symptoms can be made worse by straining during constipation and overly
aggressive wiping of the anus.
Diagnosis
Usually, an explanation of your symptoms is an important clue to your
doctor. On examination, external hemorrhoids and bulging hemorrhoids may be
visible.
When hemorrhoids are not visible beyond the anus, your doctor may examine
the inside of the anal canal using a lighted instrument called an anoscope.
Often your doctor will recommend a detailed examination of your sigmoid
colon and rectum using a lighted scope (flexible sigmoidoscopy to ensure that
there is no inflammatory disease such as Crohn's disease or ulcerative colitis or
cancer.
Treatment for pain and itching
Take warms soaks in the bath (sitz baths). Sit in plain warm water
for about 10 minutes several times a day.
Apply a hemorrhoid cream or use a suppository. Follow the
directions on the package.
Hemorrhoids - Page | 11

Don't strain during bowel movements.
Treatment for constipation
Increase the amount of fiber in your diet. Good sources of fiber are
fruits, vegetables, and whole grains. Five to ten servings of fruits
and vegetables are recommended each day. Fiber supplements
may be helpful -- examples include Metamucil and Citrucel.
Sparingly use over-the-counter laxatives or stool softeners. Stool
softeners like Colace are relatively safe, but prolonged use of
osmotic or stimulant laxatives may not be.
Exercise regularly. Even walking regularly helps improve the
normal flow of material through the intestine.
Empty the bowels when you feel the urge to do so. Immediately
following a meal the body will have a natural urge to defecate.
That's a good time to plan a visit to the bathroom.
Prevention
The best way to prevent hemorrhoids is to keep bowel movements regular and
stool soft. Try some of the tips for relieving constipation listed above. Also, avoid
prolonged standing, sitting, and heavy lifting, and chronic coughing, straining at
stool, and aggressive wiping.
IV. CLINICAL INTERVENTION
Hemorrhoids - Page | 12

1.1 Description of prescribed surgical treatment performed
According to Black and Hawks (2009), hemorrhoidectomy is a procedure
wherein the vein is excised, and the area is either left open to heal by granulation
or is closed with sutures. The open method is very painful but has a high rate of
success. The suture method, although far less painful, is more likely to cause
infection and result in poor healing. Complications include infection, stricture
formation as the lesion heals, and hemorrhage. Hemorrhage may occur
immediately after surgery or about 10 days later as a result of sloughing of
tissue. Also, bleeding may not be evident because it can occur into the rectum
without being passed immediately (p.722).
Hemorrhoids - Page | 13

Hemorrhoids can occur inside the rectum, or at its opening. To remove
them, the surgeon feeds a gauze swab into the anus and removes it slowly. A
hemorrhoid will adhere to the gauze, allowing its exposure. The outer layers of
skin and tissue are removed and then the hemorrhoid itself. The tissues and skin
are then repaired.
Hemorrhoids - Page | 14

1.2 Indication of prescribed surgical treatment
Hemorrhoidectomy is indicated for hemorrhoids with persistent
itching, anal bleeding, pain, and blood clots (thrombosis) not relieved by non-
surgical treatment (fiber rich diet, laxatives, stool softener, suppositories,
medications, warm baths), very large internal hemorrhoids, internal hemorrhoids
that still cause symptoms after nonsurgical treatment, large external hemorrhoids
that cause significant discomfort and make it difficult to keep the anal area clean,
both internal and external hemorrhoids, patients who have had other treatments
for hemorrhoids (such as rubber band ligation) that have failed. It is also
necessary for patients with severe bleeding, intolerable pain and pruritus, and
large prolapsed hemorrhoids.
Risk VS. Benefit of Hemorrhoidectomy
Hemorrhoidectomy has certain risks like constipation, Excessive discharge of
fluid from the rectum, fever of 101°F or higher, inability to urinate or have a bowel
movement, severe pain( especially when having a bowel movement), severe
redness and/or swelling in the rectal area, side effects of anesthesia (e.g., spinal
headache, reactions to medications, problem breathing, nausea), bleeding,
infection, additional risks include possible narrowing (stricture) of the anus or
stenosis, of the hemorrhoid; fistula formation; and nonhealing wounds, some
patients have temporary difficulty urinating due to swelling and the dressing.
Other relatively rare risks include the following:
Early problems
Bleeding from the anal area
Collection of blood in the surgical area (hematoma)
Inability to control the bowel or bladder ( incontinence)
Infection of the surgical area
Stool trapped in the anal canal (fecal impaction)
Late problems
Hemorrhoids - Page | 15

Narrowing (stenosis) of the anal canal
Recurrence of hemorrhoids
An abnormal passage (fistula) that forms between the anal or rectal canal
and another area
Rectal prolapse, which happens when the rectal lining slips out of the anal
opening
Benefits of patients from hemorrhoidectomy is based from a high rate of success;
most patients have an uncomplicated recovery with no recurrence of the
hemorrhoids. Complete recovery is typically expected with a maximum period of
two weeks.
1.3 Required instruments, devices, supplies, equipment, and facilities
Nonsterile tray for anesthesia
The following items are placed on a nonsterile drape covering a Mayo
stand:
The mayo stand utilizes a Tru-Loc friction-knob for manual locking at desired
height. It uses a lighter tray-support and stainless-steel base.It is covered and
used for placing surgical instruments that may be needed by the surgeon.
Hemorrhoids - Page | 16

o Sterile gloves
o 1 inch of 4x4 gauze
Gauze is a type of thin fabric with a very open weave. which is used to dress or
apply pressure to wounds and stop bleeding.
o 4x4 gauze soaked in povidone-iodine solution
o 1 inch of 2% lidocaine jelly (Xylocaine) placed on the corner of the
drape
Lidocaine is a local or topical anesthetic that can be applied to the skin or to
mucous membranes to reduce the immediate feeling of pain and produce
numbness or a 10ml syringe filled with 1% lidocaine with a 25 gauge, 1 ¼ inch
needle.
Hemorrhoids - Page | 17

o Sterile tray for the procedure:
o Sterile drape covering a Mayo stand
o 2 inches of 4x4 gauze
o 3 hemostats (mosquito )
also known as an arterial forceps or a hemostatic clamp, is one of the most
common tools which surgeons use during the course of an operation. Hemostats
are used to prevent and control bleeding of veins and arteries.
Hemorrhoids - Page | 18

o No.15 scalpel blade and handle
A scalpel is a thin, small, very sharp knife, which is used for cutting skin and
muscle in surgery,
o Needle holder
A needle holder, also called needle driver, is a surgical instrument, similar to a
hemostat, used by doctors and surgeons to hold a suturing needle for closing
wounds during suturing and surgical procedures.
o Adson forceps with teeth
Forceps are commonly held between the thumb and two or three fingers of one
hand, with the top end resting on the anatomical snuff box at the base of the
thumb and index finger. Some forceps have cross-hatched tips or serrated tips
(often called 'mouse's teeth').
Hemorrhoids - Page | 19

o Mayo scissors
Straight-bladed Mayo scissors are designed for cutting body tissues near the
surface of the wound. As the straight Mayo scissor is also used for cutting
sutures, or stitches, it’s also sold as suture scissors.
o Curved clamps -used for holding tissues
o 4-0 vicryl suture is an absorbable suture used for internal surgery
o Surgical stapler
Hemorrhoids - Page | 20

A surgical stapler is a medical device which is used to place surgical staples.
Staples are used to close wounds ranging from bowel resections to skin
incisions, and they are found widely all over the world in surgical settings.
Hemorrhoids - Page | 21

FACILITIES
`
`
1.4. Perioperative tasks and responsibilities of the Nurse
Hemorrhoids - Page | 22
P
A
T
I
E
N
T
SURGEON
ASSISTANT
BACK TABLE
Surgical
Light
Surgical
Light
SUTURE NURSE
SUCTIONMACHINE
EmergencyCart
Defibrillator Machine
ANESTHESIOLOGIST
CIRCULATING NURSE
SCRUB NURSE
MAYO TABLE
SUPPLY CABINET

PREOPERATIVE NURSING RESPONSIBILITIES:
Secure informed consent.
Provide gown for the patient.
Tape for wedding ring if necessary.
Any equipment and documents required by law and hospital policy.
Assess the pre operative education received by the patient and ensure
that it is complete and understood.
Record the patient’s pulse, temperature blood pressure respirations
and weight.
Those patients over the age of 45 will likely have to receive a
colonoscopy or x-ray of their colon. This is to make sure that the
bleeding the patient may be experiencing is not due to some other
factor.
Be sure the patient or immediate relative signed the consent for
operation
Shave the perineum
Two enemas will be needed prior to the surgery. Laxatives and
antibiotics, however, will not likely be administered prior to the
operation.
Prepare patient physically, must had full bath
Complete the pre operative check list by asking the patient and
checking records and notes before giving any pre medication.
Ensure that the patient has been fasting from food and drink for the
prescribed length of time.
Check whether the patient has micturated before pre medication.
Carry out pre -op medication as ordered by the surgeon
Ensure the patient is wearing an identification bracelet with the correct
information.
Hemorrhoids - Page | 23

INTRAOPERATIVE NURSING RESPONSIBILITIES:
SCRUB NURSE:
Set up sterile supplies and instruments
Assists the surgeons as needed throughout the surgery
Assists in gowning and gloving the surgical team
Assists in draping the patient and the fields
Hands instruments and, sutures, sponges etc. as needed in an efficient
manner
Keeps operative tidy during the case
Wipes blood from instruments
Keeps close watch on needles, instruments, and sponges so that none
will be misplaced or lost during the surgery
Keeps an accurate account of needles and instruments
Supplies sterile dressing materials
Discards soiled linen into hamper after checking it for any instruments
Cares for all instruments and supplies
CIRCULATING NURSE:
Functions as the overseer of the room during the procedure to
maintain sterility
Assists the entire team and the patient
Sends for the patient at appropriate time
Receives, greets and identifies the patient
Checks chart for completeness
Assists patient in moving safely to operating room table
Assist anesthesiologist when requested, stays with the patient during
induction
Ties scrubbed members’ gown
Checks operating room lights in advance for good working order turns
lights on at appropriate time and adjust when needed
Hemorrhoids - Page | 24

Prepares operative site
Connects catheter to drainage bottle, or catherize if desired by the
surgeon
Does the sponge count with the scrub nurse
Positions the client
Supplies foot stools if needed by the surgeon team
Watches forehead for perspirations
Fills out required operative records completely and legible
Remains in the room as much as possible to be constantly available
Watches progress of surgery, anticipates needs, reacts quickly to
emergency
Uses equipment and supplies economically and conservatively
Gathers supplies for case and opens sterile supplies for the scrub
nurse
Connects/ reminds those who breaks any technique
Directs cleaning of the room and preparations for the next operation
POSTOPERATIVE NURSING RESPONSBILITIES:
After surgery, the patient is taken to the postanesthesia care unit
(PACU). Patients are closely monitored by the nursing staff and remain
there until they are stable. The amount of time spent in the PACU
depends on the patient's progress and the type of anesthesia received.
General anesthesia must wear off and the patient must be awake and
coherent before they leave the PACU.
Outpatients are transferred to another room to finish their recovery,
and inpatients are taken to their hospital room. The intravenous line
remains in until clear liquids are taken and tolerated. This can be
almost immediately following surgery, especially if local anesthesia
was used. Sometimes general anesthesia induces nausea, which may
Hemorrhoids - Page | 25

delay taking oral fluids. Once clear liquids are tolerated, the diet
progresses to solid foods.
Spinal anesthesia usually wears off within a few hours. During the first
hour following surgery, patients lie flat on their back to decrease the
risk for an anesthesia-induced headache, which can be painful and
prolonged. Before being discharged, the patient must regain full
sensation in the lower part of the body.
Because of swelling and the dressing, some patients have temporary
difficulty urinating. If there is urgency, but the urine will not flow, a
catheter is used to empty the bladder. Outpatients may need to stay
overnight, if they are unable to urinate. Patients must be able to urinate
on their own before being discharged.
Even though the anesthesia has worn off, most patients remain groggy
for the rest of the day. Patients must arrange for a family member or
friend to be with them if they are being discharged the same day as the
surgery.
Patients experience pain and discomfort during the immediate
postoperative period (i.e., about 10 days). Pain medication is
prescribed and should be taken as directed. Sometimes relief can be
achieved with an over-the-counter preparation such as Tylenol®. If a
pack was inserted into the rectum following surgery, the physician
usually removes it in a day or two.
An ice pack can help reduce swelling. Soaking in a sitz bath (a shallow
bath of warm water) several times a day helps ease the discomfort.
Using a donut ring (cushion with a hole in the middle) can make sitting
upright more comfortable.
Hemorrhoids - Page | 26

It is important to avoid constipation at this time. So, the physician will
prescribe stool softeners and a laxative. Eating a high-fiber diet and
drinking plenty of liquids also helps. A small to moderate amount of
bleeding, usually when having a bowel movement, may occur for a
week or two following the surgery. This is normal and should stop
when the anus and rectum heal.
Complete recovery takes 6 weeks to 2 months. Most patients return to
work within 10 days. Heavy lifting should be avoided for 2 to 3 weeks.
1.5 Expected outcomes of surgical treatment performed
The outcome is usually very good in the majority of cases. Patients may
experience the following:
pain after surgery as the anus tightens and relaxes.
temporary difficulty in urinating due to swelling and the dressing.
discomfort during the immediate postoperative period (i.e., about 10 days).
A small to moderate amount of bleeding, usually when having a bowel
movement, may occur for a week or two following the surgery. This is normal and
should stop when the anus and rectum heal.
Complete recovery takes 6 weeks to 2 months. Most patients return to
work within 10 days. Heavy lifting should be avoided for 2 to 3 weeks.
***Postoperative Complications
Most patients are satisfied with the results of the surgery and recover without any
problems. Complications associated with hemorrhoidectomy are rare and
include:
Anal fistula or fissure
Constipation
Excessive bleeding
Excessive discharge of fluid from the rectum
Hemorrhoids - Page | 27

Fever of 101°F or higher
Inability to urinate or have a bowel movement
Severe pain, especially when having a bowel movement
Severe redness and/or swelling in the rectal area
Side effects of anesthesia (e.g., spinal headache)
Narrowing (stenosis) of the anal canal
Recurrence of hemorrhoids
An abnormal passage (fistula) that forms between the anal or rectal canal
and another area
Rectal prolapse, which happens when the rectal lining slips out of the anal
opening
***The surgeon should be notified if any of these symptoms are experienced
during the immediate postoperative period.
1.6 Medical management of physiologic outcomes
For pain - The doctor may prescribe narcotics to relieve the pain. The patient
should take stool softeners and attempt to avoid straining during both defecation
and urination. Soaking in a warm bath can be comforting and may provide
symptomatic relief.
Bleeding (if postoperatively) - never apply heat because of the increased risk
of hemorrhage.
For difficulty in urination - If there is urgency, but the urine will not flow, a
catheter is used to empty the bladder.
An ice pack can help reduce swelling. Discomfort is decreased thru
soaking in a sitz bath (a shallow bath of warm water) several times a day helps
ease the discomfort. Using a donut ring (cushion with a hole in the middle) can
make sitting upright more comfortable. Postoperatively, check for signs of
prolonged rectal bleeding, administer adequate analgesics, and provide sitz
baths as ordered. As soon as the patient can resume oral feelings, administer a
Hemorrhoids - Page | 28

bulk medication, such as psyllium, about 1 hour after the evening meal, to ensure
a daily stool. Warn against using stool-softening medications soon after
hemorrhoidectomy because a firm stool acts as a natural dilator to prevental and
stricture from the scar tissue (The patient may need repeated digital dilation to
prevent such narrowing).
Keep the wound site clean to prevent infection and irritation. Before
discharge, stress the importance of regular bowel habits and good anal hygiene.
Warn against too-vigorous wiping with washcloths and using harsh soaps.
Encourage the use of medicated astringent pads and white toilet paper (the
fixative in colored paper can irritate the skin). The anal area is very painful, and
the client may avoid defacating, resultin in hard stool or fecal impaction.
Encourage the client to take bulk laxatives, stool softeners, or mineral oil as
prescribed to promote stool passage. Monitor the stool for consistency and
blood.
Counsel the client to (1) eat fiber-containing foods and drink ample fluids
to prevent straining and (2) avoid laxatives as much as possible. remind the
client not to sit on the toilet longer than necessary; this position impairs blood
flow and puts added pressure on anal vessels.
Relieve pain and encourage 15 minute warm sitz baths three or four times
per day for 15 minutes. Witch hazel (a topical astringent) compresses are
soothing to the mucosa. Other over-the-counter preparations may temporarily
relieve pain. Hydrotherapy with a bathtub, bidet, or extend-able shower head.
Especially in the case of external hemorrhoids with a visible lump of small
size, the condition can be improved with warm bath causing the vessels around
the rectal region to be relaxed.
Hemorrhoids - Page | 29

Topical corticosteroid such as hydrocortisone. (May weaken the skin and
may contribute to further flare-ups.)
Topical vasoconstrictor such as phenylephrine.
Topical moisturizer.
Topical astringent, such as witch hazel
Stress the importance of regular bowel habits and good anal hygiene.
Warn against too-vigorous wiping with washcloths and using harsh soaps.
Encourage the use of medicated astringent pads and white toilet paper
(the fixative in colored paper can irritate the skin)
Keep the wound site clean to prevent infection and irritation.
Using the squatting position for bowel movements.
Dietary supplements can help treat and prevent many complications of
hemorrhoids, and natural botanicals such as Butchers Broom, Horse-chestnut,
Hem-eez and bioflavonoids can be an effective addition to hemorrhoid treatment.
Butcher's Broom extract, or Ruscus aculeatus, contains ruscogenins that
have anti-inflammatory and vasoconstrictor effects that help tighten and
strengthen veins. Butcher's Broom has traditionally been used to treat venous
problems including hemorrhoids and varicose veins.
Horse-chestnut extract, or Aesculus hippocastanum, contains a saponin
known as aescin, that has anti-inflammatory, anti-edema, and venotonic actions.
Aescin improves tone in vein walls, thereby strengthening the support structure
of the vein. Double blind studies have shown that supplementation with horse-
chestnut helps relieve the pain and swelling associated with chronic venous
insufficiency.
Hemorrhoids - Page | 30

1.7 Nursing Care Plans
a. Acute Pain (pre-operative)Assessment Nursing
DiagnosisScientific Explanation
Objectives Nursing interventions
Rationale Expected Outcome
S> ØO> The patient may manifest:- observed evidence of pain- facial mask-sleep disturbance- expressive behavior (restlessness, moaning, irritability)- diaphoresis-change in blood pressure- narrowed focus (impaired thought process, altered time perception)
Acute Pain Tenesmus increases intra-abdominal and hemorrhoidal venous pressures, leading to distention of the hemorrhoidal veins. When the rectal ampulla (pouch) is filled with formed stool, venous obstruction is believed to occur. As a result of the repeated and prolonged increase in
After 5 hours of Nursing Interventions and health teachings client will:- report pain is relieved or controlled.- follow prescribed pharmacological regimen.- verbalize nonpharmacologic methods that provide relief.- demonstrate use of relaxation skillsAnd diversional activities as indicated for individual situation.
-take client’s vital signs
- note client’s age, developmental level, and current condition
-note location of surgical procedures
- assess for referred pain
- use pain rating scale appropriate for
- to obtain baseline data
- to assess contributing factors
- this can influence the amount of post-operative pain experienced
- to help determine possibility of underlying organ dysfunction requiring treatment.
- to evaluate client’s response to pain
After 2 hours of Nursing Interventions and Health Teachings client shall have:- reported pain is relieved or controlled.- followed prescribed pharmacological regimen.- verbalized nonpharmacologic methods that provide relief.- demonstrated use of relaxation skills and diversional activities as indicated for individual situation.
Hemorrhoids - Page | 31

- positioning to avoid pain
this pressure and the obstruction, hemorrhoidal veins become permanently dialted. As a result of the distention, thrombosis and bleeding may also occur.
age
- monitor vital signs
- note when pain occurs
- provide comfort measures such as:= touch= repositioning= use of heat/cold packs= quiet environment= calm activities= nurse’s presence
- instruct use of relaxation techniques= focused breathing= imaging= music
- altered during acute pain
- to medicate prophylactically as appropriate
- to promote nonpharmacological pain management
- to distract attention and reduce tension
Hemorrhoids - Page | 32

- administer analgesics as indicated to maximum dose
- document client’s response to analgesics
- encourage adequate rest periods
- to maintain acceptable level of pain
- to determine increase or decrease dosage of analgesics
- to reduce fatigue
Hemorrhoids - Page | 33

b. Imbalanced nutrition less than body requirements related to poor nutrition before surgery
Assessment Nursing Diagnosis
Scientific Explanation
Objectives Interventions Rationale Expected Outcome
S>
O> The pt. manifested>body malaise
> body weight 20% or more under ideal
> weak-ness of muscles required for mastication or swallow-wing
> decreased subcutaneous fats/muscle mass
Imbalanced nutrition less than body requirements related to poor nutrition before surgery.
Before the operation, patients are required to be NPO for quite some time in order to decrease bulk in the alimentary tract that would impede sterility during surgery this affects the nutritional status of the client therefore decreasing nutritional intake. After the surgery still, the patient is under NPO due to post anesthesia and impaired GI motility. This would therefore alter the nutritional status of a client.
Short term:After 40 of NI the pt will verbalize understand-ding of causative factors when known and necessary interventions.
Long term: After 3 days of NI, the pt. will demonstrate progressive weight gain toward goal.
> Identify clients at risk for malnutrition (e.g., hypermetabolic state, restricted intake, etc.)
> Determine ability to chew, swallow, and taste. Note denture fit; presence of mechanical barriers; lactose intolerance; cystic fibrosis; pancreatic disease
> Ascertain understanding of individual nutritional needs
> Discuss eating habits, including food preferences, intolerances, aversions, etc.
> In order to know appropriate intervention needed
> Factors that can affect ingestion and/or digestion of nutrients should be determine n order to intervene properly
> To determine what information to provide client/SO
> To appeal to clients likes and dislikes.
Short term:The pt shall have verbalized understanding of causative factors when known and necessary interventions.
Long term: The pt. shall have demonstrated progressive weight gain toward goal
Hemorrhoids - Page | 34

> Assess drug interactions, disease effects, allergies, use of laxatives, diuretics.
> Determine psychological factors/ perform psychological assessment
> Assess weight, age, body build, strength, activity/rest level
> These factors may be affecting appetite, food intake, or absorption
> To assess body image and congruency with reality
> Provides comparative baseline
Hemorrhoids - Page | 35

c. Constipation (pre-operative)Assessment Nursing
DiagnosisScientific Explanation
Objectives Nursing Interventions
Rationale Expected Outcome
S> ØO>The patient may manifest:- hard, formed stool- straining with defecation- hypoactive/ hyperactive bowel sounds- distended abdomen-abdominal tenderness- palpable abdominal/ rectal mass- percussed abdominal dullness
Constipation r/t hemorrhoids
Tenesmus increases intra-abdominal and hemorrhoidal venous pressures, leading to distention of the hemorrhoidal veins. When the rectal ampulla (pouch) is filled with formed stool, venous obstruction is believed to occur. As a result of the repeated and prolonged increase in this pressure and the obstruction, hemorrhoidal veins become permanently dialted. As a
After 1 hour of Health Teachings the client will:- verbalize understanding of etiology and appropriate interventions for individual situation
After 5 days of Nursing Interventions client will:- regain normal pattern of bowel functioning- demonstrate lifestyle behavior which will prevent recurrence - participate in bowel program
-take client’s vital signs
- determine fluid intake
- review daily dietary regimen
- evaluate client’s medication regimen
- note activity level
- note color, odor, consistency, frequency, and amount
- to obtain baseline data
- to determine client’s hydration status
- to determine fiber sufficiency
- which could cause/. Exacerbate constipation
- sedentary lifestyle may affect elimination patterns
- provides baseline data for comparison
After 2 hours of Health Teachings the client shall have:- verbalized understanding of etiology and appropriate interventions for individual situation
After 5 days of Nursing Intervention the client shall have:- regained normal pattern of bowel functioning- demonstrated lifestyle behavior which will prevent recurrence - participated in
Hemorrhoids - Page | 36

result of the distention, thrombosis and bleeding may also occur.The anal area is very painful, and the client may avoid defecating, resulting in hard stool formation or fecal impaction.
- encourage diet of fiber and bulk
- promote adequate fluid intake
- encourage activity within individual limitations
- apply lubricant/ anesthetic ointment to anus
- provide sitz bath after defectaion
- discuss client’s current medication regimen
- to improve consistency
- to promote passage of soft stool
- to stimulate contraction of intestines
- to facilitate return of acceptable bowel pattern
- for soothing effect at rectal area
- to determine if drugs contributing to constipation can be changed or discontinued
bowel program
Hemorrhoids - Page | 37

d. Risk for Urinary Retention (post-operative)Assessment Nursing
DiagnosisScientific Explanation
Objectives Nursing Interventions
Rationale Expected Outcome
S> ØO>The patient may manifest:- bladder distention- small frequent voiding/ absence of urine output- residual urine (150mL or more)- dysuria
Risk for urinary Retention
Tenesmus increases intra-abdominal and hemorrhoidal venous pressures, leading to distention of the hemorrhoidal veins. When the rectal ampulla (pouch) is filled with formed stool, venous obstruction is believed to occur. As a result of the repeated and prolonged increase in this pressure and the obstruction, hemorrhoidal veins become permanently dialted. As a
After 1 hour of Health Teachings client will:- verbalize understanding of causative factors and appropriate interventions for individual situation.- demonstrate techniques to prevent retention.
- render health teachings to client such as:= recommend the client to void at frequent timed schedule = maintain consistent fluid intake= instruct use of crede’s maneuver
- adjust fluid amount and timing- refrain use of valsalva’s maneuver- increase fluid intake- provide privacy
- to promote prevention techniques-To maintain low bladder pressure
- to wash off bacteria, avoid infections.- to promote urination
- prevent bladder distention- to prevent further trauma in perineal area- to promote voiding- to allow client to have a comfortable environment for urination
After 1 hour of Health Teachings client will have:- verbalized understanding of causative factors and appropriate interventions for individual situation.- demonstrated techniques to prevent retention.
Hemorrhoids - Page | 38

result of the distention, thrombosis and bleeding may also occur.May induce perineal trauma.
Hemorrhoids - Page | 39

e. Deficient KnowledgeAssessment Nursing
DiagnosisScientific Explanation
Objective Nursing Interventions
Rationale Expected Outcome
S> ØO> The client may manifest:-Inaccurate follow through of instruction-inappropriate/ exaggerated behavior- misguided knowledge regarding disease condition- use of inappropriate interventions for disease condition
Deficient Knowledge
Absence or deficiency of cognitive information necessary for clients/SO to make informed choices regarding condition/ treatment. Due to common heresay and primitive knowledge about hemorrhoids which are retained and passed on to families, and lack of initiative, knowledge
Short Term:After 1 hour Health Teaching client will:- verbalize understanding of Hemorrhoid situation and certain lifestyle changes to promote comfort and alleviate pain.-verbalize understanding of corrected misconceptions regarding hemorrhoidectomy
Long Tern;After 3 days of interventions client will:-practice correct wiping of anal area which should
- ascertain level of knowledge includingAnticipatory needs
- determine blocks to learning:=language=age=mental capability=environment
- provide positive reinforcement
- identify information that needs to be remembered
- to assess readiness to learn and individual learning needs
- to assess client’s motivation
- can encourage continuation of efforts
- client can become sel-reliant
Short Term:After 1 hour of Health Teachings client shall have:- verbalized understanding of Hemorrhoid situation and certain lifestyle changes to promote comfort and alleviate pain.-verbalized understanding of corrected misconceptions regarding hemorrhoidectomy
Long Term:After 3 days of interventions client shall have:-practiced correct wiping of anal area which should
Hemorrhoids - Page | 40

and resources to seek medical assistance.
not be too hard- practice good perineal care-prevent excessive straining- eat food rich in fiber to prevent constipation and straining- know how to manage prevention of hemorrhoid occurrence or possible managements
= pregnancy, constipation with prolonged straining, obesity heart failure, prolonged sitting or standing and cirrhosis with portal hypertension raise the incidence of hemorrhoids
= increasing fluids and fiber in diet
= application of cold packs followed by sitz bath
= application of topical anesthetics
- be aware of the causes
- to soften stool and void straining
-to promote comfort
- to reduce pain
not be too hard- practiced good perineal care-prevented excessive straining- eaten food rich in fiber to prevent constipation and straining- known how to manage prevention of hemorrhoid occurrence or possible managements
Hemorrhoids - Page | 41

V. CONCLUSION
The case report has enlightened the group with much information
regarding hemorrhoidectomy along the lines of: anatomy of the digestive system,
pathophysiology of the disease, clinical and surgical interventions for
hemorrhoidectomy, and nursing care plans of a patient with hemorrhoids. For
future references, the group would know, the necessary interventions and health
teachings applicable to a patient with haemorrhoids or a patient post-op or pre-op
hemorrhoidectomy. Even without the actual interaction of the group with a patient
with hemorrhoids, the case report still bears its benefits on the group not only,
through knowledge gain but also with character gain. The case report brought to
the group: patience, perseverance, logical thinking, and a thirst for knowledge,
diligence, cooperation and camaraderie. For the whole part the group delighted
in the completion of the case report.
Hemorrhoids - Page | 42

VI. LEARNING DERIVED
Hemorrhoids may not be a life-threatening disorder, but disrupts the daily
routine of a patient, and so it still is a medical concern and should not be treated
lightly, since it is the nurse’s role to provide comfort and help ease the pain a
client is experiencing. It gave me knowledge gain and made me less ignorant
about hemorrhoids and at least I won’t be empty-handed if I ever get assigned to
a patient with hemorrhoids.
Doing the case report book based and without any patient interaction, was
like going around a dark room, feeling your way around and not knowing when to
stop, what to expect or what you are actually looking for. It held me up blind, and
sort of lost since I didn’t know what to expect, but once I got some information
and began learning about hemorrhoids along the way, it came moderately fine.
And it was great being able to work with my group mates, and now I’ve gained
new friends, and their trust. As a student nurse, aside from completing this
requirement, it helped me be more knowledgeable, and enlightened to the topic
of hemorrhoids.
- Bianca Patricia O. Santiago
BSN III-10 Gr.37
Hemorrhoids - Page | 43

This work is done within the new environment with a new clinical
instructor, new group mates during the new experiences we encounter each day.
Hemorrhoids are familiar problems faced by many in the Philippines most
especially with females primarily due to pregnancy. Though it is commonly
experienced, it is rarely being talked or discussed about. Not much is known
about hemorrhoids and so, misconceptions are widespread. Throughout the
completion of this work, more information was provided to us. This included the
causes, signs and symptoms and the managements, both medical and surgical,
are being done. This case report may benefit us when the time for us to
encounter such comes. If that occurs, then we could be more confident in doing
our responsibilities in rendering the maximum care we can because we are
somehow equipped with knowledge about hemorrhoids.
It was hard for us to come up with a case report without observing a
patient on actual. References from the internet and books became useful for us
to complete this report and understanding it at the same time. Even though
hemorrhoids are not life-threatening it is important to alleviate the pain
experienced by the client. I have also learned that the best way to eliminate the
condition permanently cannot be achieved after the operation but is attained by
changing lifestyle most especially with the diet.
As a student nurse at the present time and hopefully a registered nurse in
the future, it is our responsibility to keep ourselves updated with the new trends.
Everyday should be a learning moment for us to be able to provide optimum care
to our patients.
-Christina Marie D. Ocampo
BSN III-10 Gr.37
Hemorrhoids - Page | 44

"... Observation and experience will teach us the ways to maintain or to bring
back the state of health." -Florence nightingale
Hemorrhoids whether external or internal is a condition wherein the patient
must be closely monitored for pain and bleeding. I learned that in doing this case
study it takes great patience and compassion to render care to the patients.
Caring for patients is not a big joke, we should treat our patients the way we
wanted our loved ones be treated. I learned that the pain experienced by the
patient results from the hemorrhoids in their anus, now I know what this condition
really is because when I was in high school my dad and untie had the same
condition and they experienced the same signs like pain in the anus and even
bleeding, before then they even manually inserted the hemorrhoids, good thing
they dealt with it then. Dealing with patients of this condition is like dealing with
chipped glass, the patients are so fragile that the care given should be effective
and efficient. In doing the case study, I think time management is second to
compassion in rendering one's service because the main focus should be the
client. I learned that forcing ourselves to defecate should be avoided even though
the effect seems good because we don’t need to worry that we will defecate in
public or somewhere we aren’t comfortable. Hemorrhoids are also caused by
prolonged standing or seating which I think a lot of us don’t enjoy. In this case I
learned that squatting, warm sitz bath, and even fiber rich foods should be done
not just by people with hemorrhoids but also people like us to avoid having
hemorrhoids. Observation and experience will teach us the ways to maintain or
to bring back the state of health, just like what Florence Nightingale have said, in
this case I have learned thru the experience of my relatives, our case, and even
our books and other reference. Observing and acting on the patient’s condition
truly helps the patient, the SO, and the other Health Care Provider in improving
the patient's condition.
-Pamela Jane Simbulan
BSN III-10 Gr.37
Hemorrhoids - Page | 45

VII. REFERENCES
Websites:
http://www.wellsphere.com/digestive-health-article/hemorrhoids/69667po1
http://www.surgerychannel.com/hemorrhoidectomy/post.shtml
http://www.hemorrhoidsinplainenglish.com/hemorrhoid/total-hemorrhoidectomy.htm
http://health.allrefer.com/health/hemorrhoid-surgery-hemorrhoid-surgery-series-2.html
http://health.allrefer.com/health/hemorrhoids-info.html
http://www.surgeryencyclopedia.com/Pa-St/Sclerotherapy-for-Varicose-
Veins.html#ixzz0WsvkiyMW
http://www.surgeryencyclopedia.com/Fi-La/Hemorrhoidectomy.html#ixzz0WslnRnWg
http://www.wales.com.au/haemorrhoids_internal.html
http://www.surgerychannel.com/hemorrhoidectomy/index.shtml
http://www.webmd.com/a-to-z-guides/hemorrhoidectomy-for-hemorrhoids
http://en.wikipedia.org/wiki/Hemorrhoidectomy
http://www.proctocure.com/f9_hemorrhoidectomy.htm
Books:
Black, Joyce M., et al. Medical Surgical Nursing Clinical Management of Positive
Outcomes 8th edition. Singapore: Elsevier, 2009.
Hemorrhoids - Page | 46