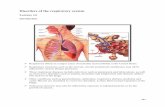
Respiratory Module Pathology
Transcript of Respiratory Module Pathology

Respiratory Module
Pathology 1

Hashemite University Faculty Of Medicine Second year students
Module of Respiratory System
Pathology : Total 9 Lectures Lectures prepared By : Dr.Ghada Nazar Aljussani MBCHB.,FRCPath UKIRAqi Board in pathology Jordanian Board in pathology European Board in pathology

Respiratory System ObjectivesPart IObstructive pulmonary diseases Acute Respiratory distress Syndrome Pneumoconiosis(occupational lung diseases) SarcoidosisAtelectasis (lung collapse) Pulmonary hypertension Good Pasture syndrome .Reference : Robbin’s Basic Pathology . Kumar ,ABBAS ,Aster. 10th edition .

Obstructive pulmonary diseasesObstructive Pulmonary Diseases* Characterized by limitation of airflow usually resulting from an
increase in resistance caused by partial or complete obstruction of bronchial tree at any level .*The major obstructive disorders are : Chronic BronchitisBronchiectasis AsthmaEmphysema.

ChronicBronchitis :Definition :A clinical condition characterized by a persistent productive cough forat least three consecutive months in at least two consecutive years .(WHO)It is common among cigarette smokers and urban dwellers in smog -ridden cities. (mixture of smock ,fog and chemical fumes)20% -25% of men between age groups of 40-65 years are mostly affected .

Chronic bronchitis can occur in several forms :1 Simple chronic bronchitis :Most patients with simple chronic bronchitis have a productive cough with mucoid sputum but airflow is not obstructed.2 Chronic asthmatic bronchitis :Some patients with chronic bronchitis may demonstrate hyper-responsive airways with intermittent bronchospasm and wheezing .3 Chronic obstructive bronchitis :Including heavy smokers who develop frank chronic outflow obstruction usually with associated emphysema .

Chronic bronchitisFeatures include :
-Cough continuous 3 months / 2 years
productive of sputum may persists indefinitely without ventilator dysfunction.
Pathology :bronchial lumen. Increase mucus in
Increase number of mucus glands (Reid Index) Increased intra epithelial goblet cells .Squamous metaplasia .

Pathogenesis : The destructive feature of chronic bronchitis is hyper secretion of
mucus , beginning in the large airways as trachea or major bronchi .In advanced disease even small bronchioles are involved .
Although the most important cause is cigarette smoking other air pollutants such as sulfur dioxide & nitrogen oxide may contribute . These environmental irritants induce hypertrophy of mucus glands in
the trachea & main stem bronchi & goblet cell metaplasia lead to a marked increase in mucus-secreting goblet cells replacing the ciliated epithelial cells in the surface epithelium of smaller bronchi & bronchioles .
In addition these irritants cause inflammation with infiltration of CD-8 T lymphocytes , macrophages & neutrophils .

It is postulated that many of the respiratory effects ofenvironmental irritants i.e. mucosal hyper secretion aremediated by local release of T-cell cytokines such as IL-13
the transcription of mucin gene & neutrophil elastaseMU5AC which is increased as a consequence of exposureto tobacco smoke in both in vitro & in vivo experimental modelsare in part mediated by signaling via the epidermal growth
factor receptor pathways. Microbial infection is oftenpresent but has a secondary role chiefly by maintaining theinflammation and exacerbating symptoms .

Because of reduced ciliary movement the mucus cannot becoughed out & since the stagnated mucus is a good medium forbacterial growth , secondary bacterial infection developsfrequently leading to inflammation, ulceration of bronchial mucosafollowed by fibrosis & scarring causing chronic obstructive
pulmonary disease. (COPD). The morphological basis of theadvanced chronic bronchitis is more peripheral and results from :1So called small-airways disease induced by goblet-cell
metaplasia with mucus-plugging of bronchiolar lumeninflammation and fibrosis.2 Co-existent emphysema:It is generally believed that while small airways disease also knownas chronic bronchiolitis is an important component , chronicbronchitis with a significant airflow obstruction is almost alwayscomplicated by emphysema.

Morphology:
Grossly:
The mucosal lining of larger airways is usually hyperemic & swollen by edema fluid. It is often covered by a layer of mucinous ormucopurulent secretion.The smaller bronchi & bronchioles may also be filled with similar secretions.
Histologically:The diagnostic feature of chronic bronchitis in the trachea and larger
hyperplasia of submucosal mucus-secreting glands .bronchi is goblet cell metaplasia of bronchial epithelium and
Themagnitude of the increase in size is assessed by the ratio of thethickness of the submucosal gland layer to that of the bronchial wallfrom epithelial layer down to cartilage . this ratio is called Reid index
normally is (0.4) . In chronic bronchitis it equals unityi.e. (1/1).


Figure 2 : Gross view of trachea and major bronchi
in chronic bronchitis , looking hyperemic & swollen
mucosa

Figure 3 : Gross view of chronic bronchitis showing
inflamed hyperemic bronchial mucosa with thick
purulent secretion filling the lumen.

Figure 4 : Gross appearance of lung tissue in chronic
bronchitis, dilated bronchi filled brownish mucoid
secretion .

Figure 5 : Microscopic view of normal bronchus .

Figure 6 : Measuring Reid index ,normal ¼ in chronic
bronchitis it is increased may be 1/1 .

A variable density of inflammatory cells largely mononuclearcells but sometimes with neutrophils is frequently present inbronchial mucosa, their number may be increased during
exacerbations. Chronic
are devoidbronchiolitis is
ofinflammatoryinflammationsubmucosal glands & cartilage
of small bronchioles, whichshow goblet cell
metaplasia, mucus plugging inflammation & fibrosis.In sever cases narrowing and obstruction with completeobliteration of the lumen due to fibrosis called bronchiolitis
Obliterans.

Figure 7 : Microscopic view of bronchial mucosa .Left : Normal ,
ciliated pseudostratified columnar epithelium . Right : chronic
bronchitis showing goblet cell metaplasia replacing the ciliated
epithelium .

Figure 8 : Microscopic view showing goblet cell metaplasia (right )
of bronchiolar epithelium (left) with inflammatory cells infiltrate in
surrounding tissue .

Figure 9 : Microscopic view of bronchial mucosa showing
goblet cell metaplasia , there is complete replacement of the
ciliated respiratory epithelium by goblet cells .

Figure 10 : Microscopic view of bronchial mucosa in chronic
bronchitis showing marked submucosal gland hyperplasia (arrow).

Figure 11: Microscopic view of chronic bronchitis,
showing florid mucous glands hyperplasia .

Figure 12 : Microscopic view of chronic bronchitis,
showing per bronchial inflammation and fibrosis .

Figure 13 : Microscopic view of chronic bronchitis , showing dense
inflammatory infiltrate in peri bronchial tissue & thick purulent material in
the lumen .

Clinical course :
Patients with chronic bronchitis complain of
prominent cough with the production of excessive
mucoid or mucopurulent sputum which may persistsindefinitely without ventilator dysfunction. Somepatients may develop chronic obstructive pulmonary disease (
COPD) with outflow obstruction , this is accompanied byhypercapnia, hypoxemia & in sever cases cyanosis (blue
bloater ), such conditions may be associated withemphysema. With progression chronic bronchitis maycomplicate by pulmonary hypertension & cardiac failure.
Recurrent infections & respiratory failure are constantthreat. Squamous metaplasia of epithelium ,with dysplasiamay complicate to squamous cell carcinoma of bronchus.

Figure 14: Microscopic view of bronchial mucosa showing
squamous metaplasia of respiratory epithelium.

Asthma
Definition :Is a chronic inflammatory disorder of the airways that causesrecurrent episodes of wheezing, breathlessness, chest
tightness and cough, particularly at night & / orearly in the morning. This clinical picture is caused by
repeated immediate hypersensitivity and late phasereactions in the lungs that gives rise to the triad ofintermittent and reversible airway obstruction , chronicbronchial inflammation with eosinophils and bronchialsmooth muscle hypertrophy and hyper reactivity.

Asthma is a heterogeneous disease triggered by a variety of inciting agents.Two types of asthma has been identified :
Extrinsic asthma :
Constitutes 70% of cases , called atopic due to IgE & TH2 lymphocytes -mediated immune response to environmentalantigens.
Intrinsic asthma :Constitutes 30% of cases or non-atopic and is triggered bynonimmune stimuli such as drugs like aspirin , penicillin,
pulmonary infections especially viral, cold,
psychological stress, exercise & inhaled irritants.

Atopic Asthma :
The most common type of asthma, usually begins in
childhood with a positive history of atopy, in
genetically predisposed individuals. Asthmatic attacks
are preceded by allergic rhinitis, urticarial, skin rash, or
eczema. The disease is triggered by environmental
antigens such as dust, pollens, animal dandruff and
foods. A skin test is positive when the offending
antigen is injected to the skin of the patient , this
results in an immediate wheal and flare reaction
caused by Type I, IgE - mediated hypersensitivity
reaction, it appears within 24 hours .

Figure 15: Skin test. Positive in individuals
with atopic asthma.

Pathogenesis :
The major etiologic factor in asthma is geneticpredisposition to type I hypersensitivity (atopy).
In the airways sensitization is induced by the inhaledallergen stimulate the helper T lymphocytes ( TH 2 )cells which release interleukins IL-4 & IL-5 lead to thesynthesis of IgE that bind to the submucosal mastcells which play an important role in thepathogenesis of asthma followed by acute & chronicairway inflammation and bronchospasm caused byconstriction of bronchial smooth muscle.

Pathogenesis o f atopic asthma can be summarized into four stages as follows:
1- Stage of sensitization :
Exposure to the inhaled inciting
(allergen) which will be attached to
antigen
allergen-
presenting cells (APC) called dendritic cells on
the surface of bronchial epithelium, this will lead
to activation of Helper T lymphocytes (TH2).
These cells will release (1) IL-4 that stimulates
plasma cells to produce IgE antibody which is
going to be attached to receptors on mast cell
membrane.

(2) IL-5 that is chemotactic to & activating
eosinophils, which will accumulate in the mucosa
and produce major basic protein or eosinophil
cationic protein both are toxic to epithelial cells
can induce their damage leading to opening of
gap junctions between them , this helps the
allergen to enter to bronchial mucosa to activate
more TH2 lymphocytes & mast cells already
present within bronchial mucosa. (3) IL-13 that
stimulates mucus production from goblet cells
and the submucosal glands.

Figure 16: Diagrammatic presentation of pathogenesis
of atopic asthma , initial stage of sensitization .

2- Stage of immediate –phase hypersensitivity
reaction :Starts immediately or within minutes after repeated exposure
to the same antigen characterized by increased
permeability and edema fluid accumulating in
mucosa with smooth muscle spasm causing
vascular
bronchial
broncho
constriction, the patient will have sever dyspnoea wheezing &
difficulty of expiration being evident within 5-30 minutes
following the second exposure to the same antigen and
subsides by 60 minutes. In this phase the reaction will be
triggered by antigen-induced cross linking of IgE antibodies
on mast cells in the airways leading to the release of their
granules .

Which are the mediators including Histamine,
eosinophil chemotactic factor (ECF), Leukotriens
B4 ,C4 ,D4 & E4. Platelets activating factor (PAF),
prostaglandins & thromboxane. These will induce
increased vascular permeability, edema more
eosinophils & neutrophils accumulation together
with bronchoconstriction. In addition ,stimulation
of subepithelial vagal (parasympathetic) receptors
as well as acetylcholine released
provoke
from
reflexintrapulmonary motor nerves
bronchoconstriction.

Figure 17 : Activation of mast cell by IgE .

3- Stage of Late phase reaction :
Starts 4-8 hours later and may persist for 12-24 hours.
In this phase eosinophils are particularly important in
addition to the major basic protein & eosinophil cationic
protein which cause epithelial cell damage, they also
peroxidaseproduce eosinophil
damage , and release mediators
that cause tissue
like
which causes bronchoconstriction. This phase
leukotriens C4
is
characterized by inflammation ,tissue destruction,
ulceration, smooth muscle spasm well asmucosal
increased inflammatory cells infiltration including
eosinophils, neutrophils & lymphocytes within mucosa ,
being induced by mediators like cytokines(IL-1) ,tumor
necrosis factor (TNF) & leukotrien B4 .

Figure 18: Diagrammatic view of IgE- mediated mast
cells reaction

4- Stage of Airway outflow remodeling :
This refers to the structural changes in the
bronchial wall occurring as a late secondary
deposition ofchange in asthma, including
collagen in the subepithelial
membrane, increased mucus
basement
production
together with hypertrophy of bronchial smooth
muscle and fibroblasts this have been attributed
to inherited predisposition associated with
polymorphism in gene called ADAM 33 which is
implicated in smooth muscle & fibroblast
proliferation.

Figure 19 : Comparison between normal bronchial wall
(top) & asthmatic bronchus (bottom).

Figure 20: Microscopic view ,showing normal compared to asthmatic
bronchitis (right) showing mucus hyperplasia of epithelium , thickening of
basement membrane & smooth muscle hypertrophy .

Figure 21: Microscopic view of asthmatic bronchitis showing
mucous metaplasia & thickened basement membrane .

Non-atopic asthma :The mechanism of bronchial inflammation and hyper responsivenessis less clear in this type. Viral infection & inhalation of irritant
pollutants as sulfur dioxide & nitrogen oxide, have beenincriminated. A positive family history is uncommon serum Ig E levelis normal . Skin test is negative. The ultimate mediators of airwayobstruction & eosinophilia are common .Drug-induced asthma :
Aspirin is the most common cause of asthma in aspirin sensitive patients. The precise mechanism is unknown, possibly related to theeffect of aspirin which inhibits cyclo-oxygenase pathway of arachidonic acid metabolism by shifting it towards lipoxygenasepathway resulting in production of the bronchonstrictor leukotriens .

Occupational asthma, Fumes, resins & plastics organicor chemical dust of ( wood, cotton, platinum ) gases
as toluene, exposure to such products induce asthmaticattacks in sensitive individuals.
Morphology :
Grossly :
In fatal cases with status asthmaticus or cases of
prolonged chronic asthma , the lungs look over
distended because of the over inflation there may
be also presents areas of atelectasis. The most
striking gross finding is occlusion of the bronchi &
bronchioles by thick mucus plugs .

Histologically :
The sputum of patient as well as in tissue sections
of bronchi show the mucus plugs contain whorls of
shed necrotic epithelial cells called (Curschmann’s
spiral). Also, seen
charcot-leyden crystals which are made up
are numerous eosinophils &
of
eosinophilic protein. Features of airway remodeling
including thickening of basement membrane of
bronchial epithelium by dense collagen deposition,
with edema & inflammatory infiltrate in which
eosinophils & mast cells predominate . Also present
increase in size of submucosal glands &
hypertrophy of bronchial muscle wall.

Figure 22: Charcot –leyden crystal seen in sputum of asthmatic
patient, consisting of eosinophils - derived crystalline protein .

Figure 23 : Curschman’s spirals seen in sputum of
asthmatic patients .

Clinically: The attack of asthma is characterized by sever
dyspnoea, the chief difficulty is during expiration , with
wheezing & cough. The patient can get air into the lungs but
cannot get it out, this leads to progressive over inflation of the
lungs & air is trapped distal to the bronchi which are
obstructed by mucus plugs & are constricted.The attack lasts
from one minute to several hours then gradually subsides
spontaneously or with therapy with interval between attacks
are free from symptoms. Occasionally severe paroxysms
occur that does not respond to therapy (like broncho-dilators
& steroids ) & persists for days this is called Status
asthmaticus . There is associated hypercapnoea increased
PaCO2 acidosis & sever hypoxia, but such attacks may be
fatal .

Bronchiectasis
Definition :
Is a permanent
bronchioles, caused by destruction
dilatation of bronchi &
of
muscle & elastic supporting tissue , resulting
from or associated with chronic necrotizing
infections. It is not a primary disease, but
rather a secondary sequel to persistent
infections or obstruction caused by a variety
of conditions

Etiology:
There are numerous predisposing disorders including:1Bronchial obstruction: caused by tumor, foreign body or by impaction by mucus. In such conditions thebronchiectasis tends to be confined to the obstructed lung segment.2 Bronchial asthma
3 Chronic bronchitis

4Congenital bronchiectasis: as in cystic
fibrosis which leads to a widespread bronchiectasisresulting from bronchial obstruction and infectioncaused by secretion of an abnormal viscid
mucus.
5Immune deficiency states: particularly immunoglobulin deficiency. Bronchiectasis developsdue to an increased susceptibility to repeatedbacterial infections.

6- Localised & diffuse bronchiectasis, can occur inKartegner’s syndrome which is an autosomal recessivedisorder, is frequently associated with bronchiectasis andsterility in males .Structural abnormalities of the cilia
impair muco-ciliary clearance in the airways leading topersistent infections , and reduce mobility of the spermatozoa.7- Necrotizing or suppurative pneumonias: caused bystaphylococcus aureus, Klebsiella spp, in children
cough &pneumonia complicating measles, whooping
influenza.
8- Tuberculous broncho-pneumonia.

Pathogenesis :
Two critical processes are involved:
Bronchial obstruction.
Chronic persistent infections.
In any cause of obstruction interference with theclearance mechanisms lead to secondary infectionsthat result in necrosis and weakening of thebronchial supporting tissues as the muscle coat andelastic tissue infections also involve the perbronchial tissue with fibrosis that cause traction ofthe bronchial walls towards the pleura andsurrounding connective tissues.

Morphology :
Grossly :
Bronchi of the lower lobes of both lungs are
frequently involved by bronchiectasis, they
become markedly dilated 4-5 times their normal
diameter, particularly the most vertical ones due
to gravitational accumulation of secretions ,they
can be followed towards the pleura , may look
cylindrical or cystic in appearance. Their Lumina
are filled with a dirty purulent exudates when
removed a reddish ulcerated mucosa seen.

Figure 24 : Gross appearance of lung in bronchiectasis (cylindrical
form ) markedly dilated bronchi reaching pleural surface .

Figure 25: Gross appearance of the lung showing cystic
bronchiectasis.

Figure 26: Gross appearance of lung showing bronchiectasis,
dilated bronchi filled with thick foul smelling secretions.

Microscopically :The histological changes vary with the severity andduration of the disease. In an active full-blown diseasean intense acute & chronic inflammatory exudateswithin the wall of the bronchi & bronchioles seen anddesquamation of lining epithelium cause extensiveulceration. In severe cases abnormal dilatation occursdue to necrosis & fibrosis of muscle coat with associatedper bronchial fibrosis. In severe cases lung abscesses
may develop.

Figure 27: Microscopic view of bronchiectasis , showing dense
chronic inflammatory cells infiltration and fibrosis of bronchial
wall.

Figure 28: Microscopic view of chronic advanced bronchiectasis

Clinical features :
The patient presents with sever persistent cough
with expectoration of a muco-purulent fowl-smelling
sputum which may contain flecks of blood, frank
hemoptysis may occur. Patients may present with
clubbing of fingers. In severe bronchiectasis
significant obstructive ventilator defects develop
including hypoxemia, hypercapnia, pulmonary
hypertension and cor pulmonale. Septic emboli may
arise from lung abscess may lead to brain abscess.
Amyloidosis can arise is severe prolongedbronchiectasis.

Complications of bronchiectasis :
1- Hypoxia, hypercapnia.
2 Hemoptysis.
3 Clubbing of fingers.
4Septic embolism (brain & splenic abscesses).
5- Amyloidosis.
6 Respiratory failure.
7 lung abscess.
8 Cor pulmonale .
9 Pulmonary hypertension.

Figure 29: Gross view of liver in amyloidosis .

Figure 30: Microscopic view of advanced amyloidosis in the
liver.

Figure 31 : Clubbing of fingers in patient with advanced
bronchiectasis .

Emphysema:Is characterized by abnormal permanent
enlargement of the airspaces distal to
the terminal bronchioles, accompaniedby destruction of their walls without
obvious fibrosis.

Figure 32: Gross appearance of emphysematous
lungs. Both lungs are over inflated covering the
heart .

Anatomic description:The main bronchi giving rise to progressivelysmaller airways called bronchioles, which aredistinguished from bronchi by lacking cartilage &
submucosal glands in their walls. Additionalbranching of the bronchioles lead to terminal
bronchioles, the part of the lung distal toterminal bronchiole is called acinus.

The pulmonary acini are composed of respiratory
bronchioles (emanating from terminal bronchioles ) that proceed into alveolar ducts which immediately branch into alveolar sac ,
the blind ends of the respiratory passages whose walls are formed entirely of alveoli, the ultimate site for gas exchange. A cluster of
3-5 acini is called a lobule. The alveolar wall consists entirely of capillary endothelium, basement membrane, and surrounding interstitial tissue separating the endothelium from the alveolar lining epithelium. The interstitial tissue, composed of fine elastic tissue, collage & fibroblast-like cells, smooth muscle cells, mast cells and few mononuclear cells .

The alveolar septa consists of continuouslayer of two types of cells. A flattened plate-like Type I pneumocytes, covering 95%
of alveolar surface, and rounded Type II
pneumocytes, which are source ofpulmonary surfactant and the main cellsinvolved in repair of pulmonary
epithelium.

Figure 33: Diagrammatic view of lung anatomy.

Figure 34: Alveolar acinus in the lung.

Types of emphysema :
Emphysema can be classified according to the anatomic distribution within the lobule .The four major types of emphysema are : 1- Centrilobular Emphysema.2 Panacinar Emphysema.3Distal acinar Emphysema. (Paraseptal E.) 4- Irregular Emphysema .Only the first two are clinically significant airwayobstruction , with centriacinar E. being 20-folds
more common than panacinar type.


Centri-acinar Emphysema :In this type of emphysema the central or the proximal part
of the acini , formed by the respiratory bronchioles are affected , while the distal alveoli are spared . Thus both
normal & emphysematous air spaces exist within the same acinus & lobule .The lesions are more common & sever in the upper lobes
particularly in the apical segments .In sever cases even the distal acinus becomes involved , thendifferentiation from pan-acinar E . becomes difficult.This type of E. is most commonly seen as a consequence of
cigarette smoking in people who donot have congenital deficiency of alfa 1 antitrypsin enzyme .It is 20-folds commoner than centri-acinar E.

Figure 40 : Gross appearance of lung with centriacinar emphysema
with black color due to carbon particles ,common among smokers &
coal mine workers .

(Figure 41 : Gross appearance of centriacinar emphysema showing
centrilobular dilatation surrounded by normal lung tissue .

Pan-acinar Emphysema :In this type of E. the acini are uniformly
enlarged from the level of the respiratory
bronchioles to the terminal blind alveoli .In contrast to centri-acinar E. it tends to
occur in the lower lung zones and is the
type
of E. that occurs in alfa 1 anti-trypsin
deficiency.

Figure 42 : Gross view of lung showing panacinar emphysema

Figure 43 : Gross view of panacinar emphysemaFigure 43 : Gross view of panacinar emphysema

Distal acinar Emphysema :Or paraseptal E.
In this form of E. , the proximal portion of
the acinus is normal , but the distal part is
primarily involved .The emphysema is more striking adjacent to the pleura along the lobular connective tissuesepta , and at the margin of the lobule .
It occurs adjacent to areas of fibrosis ,
scarring or atelactasis, and is more severe in
the upper half of the lungs.

Figure 44 : Distal acinar or paraseptal emphysema .

Paraseptal emphysema

Paraseptal & centriacinar emphysema

Irregular bulous emphysema .

The characteristic findings are the presence of multiple contiguous air-spaces that range from 0.5-2 cm. in diameter, sometimes forming a cyst-like spacescalled Bullae ,when ruptures is the most common cause ofspontenuous pneumothorax in young patients .
Irregular Emphysema
In this type the acinus is irregularly involved , it is associated with scarring In a healed inflammatory diseases.Although clinically asymptomatic, it is the most common form ofemphysema.

Irregular emphysema .

Gross view of lung showing irregular emphysema dilated
alveoli occurring at site of scarring at the apex of upper lobe .

Gross view of lung showing irregular emphysema
, dilatation seen near scarred & fibrotic lung tissue .

Pathogenesis :The recent theory regarding the pathogenesis of emphysemafavors a critical imbalances , the protease-anti protease
imbalance and the oxidase –
anti oxidase imbalance , such imbalances almost always coexist .The protease-anti protease imbalance hypothesisis based on the observation that patients withgenetic deficiency of anti-protease alfa 1 antitrypsin
have a marked increased tendency to develop pulmonary emphysema .

Liver biopsy in alfa 1 antitrypsin deficiency ,showing purple granules in
hepatocytes (arrows) .

Alfa 1 antitrypsin normally present in serum,tissue fluids & macrophages ,is a major inhibitor of protease particularly elastase which is secreted by neutrophils during inflammation . Alfa-1 antitrypsin is encoded by a gene on the proteinase inhibitor Pi -locus on chromosome 14, present as M allele , and Z allele .
Most people who are homozygous for Z allele (ZZ),have marked decrease in alfa 1 antitrypsin.Exposure to toxic agents such as tobacco or pollutants induce ongoing inflammation with infiltration of neutrophils , macrophages & lymphocytes in lung tissue .

Elastases , cytokines like IL-8 & oxidants are released by
these cells ,causing epithelial injury and proteolysis of the
Unless inhibited by )extracellular matrix (ECM) antitrypsin)
anti-elastase
and antioxidants , the cycle of inflammation & protelysis of
ECM continues .
More than 80% of patients with congenital α 1
antitrypsin deficiency develop symptomaticemphysema.
There is marked individual variation in susceptibility to
develop emphysema / Chronic obstructive pulmonary
diseases (COPD) .

Multiple genetic factors control the response to injury after smoking .
The transforming growth factor β (TGF β ) gene exhibits
polymorphisms that influence susceptibility to the development of
COPD by influencing the
response of the mesenchymal cells to injury .
With certain polymorphisms , mesenchymal cells response
to TGF β signaling is reduced result in an inadequate repair
of elastin injury caused by inhaled
toxins .
In addition to elastase , matrix metallo proteases MMP derived from macrophages & neutrophils have a role in tissue destruction . Especially MMP9 &MMP12 have also found to have a pathogenic role in emphysema .

In emphysema there is loss of both epithelial & endothelial cells as well as of mesenchymal cells leading to lack of extracellular matrix (ECM),the scaffold upon which epithelial cells would have been grown .Tobacco smoke contains abundant ROS i.e free radicals which deplete these anti-oxidants mechanisms , thereby inciting tissue damage .
Activated neutrophils add to the pool of ROS in the alveoli . Asecondary consequence of oxidative injury is inactivation of a native anti-protease resulting in functional alfa 1 antitrpsin deficiency even in normal individuals.

52 : Pathogenesis of emphysema .

Morphology of Emphysema :
The diagnosis & classification of E . largely depend on macroscopical appearance of thelung .In well-developed pan-acinar E. the lungs are pale voluminous hyperinflated it obscuresthe heart when
anterior chest wall is removed during autopsy .In centri -acinar E. the macroscopic features are less impressive , the lung look deeper pink than in pan-acinar E. and less voluminous , it tends to affectthe upper 2/3 of the lungs than the lower lung.

Histologically :
There is thinning & destruction of alveolar walls ,with advanceddisease the adjacent alveoli become confluent creating a large air-spaces .Terminal & respiratory bronchioles may be deformed because of loss of septa that help connecting them to the parenchyma, with loss of elastic tissue , there is a reduced radial traction of small airways resulting in their collapse duringexpiration, an important cause of chronic airflow obstruction in sever emphysema..In addition to alveolar loss a number of alveolar capillaries are diminished.

Microscopic view of emphysematous lung
tissue showing dilated alveolar spaces & destruction of
alveolar septa .

Clinical Features :
Dyspnoea is usually the first symptom , it begins insidiously but steadily progressive , with cough & wheezes .The patient with emphysema without concomitant chronicbronchitis usually presents with a barrel-chest & dyspnoea
and prolonged expiration .Dyspnoea & hyperventilation are prominent.The blood gases stay normal very late in disease due to prominent dyspnoea and hyperventilation there is adequate oxygenation of the blood caused by liberation oferythropoietin which stimulate the bone marrow to increase haematopoiesis leading to polycythemia and high level of haemoglobin .These patients are called Pink-puffer .

Photographic appearance
of pink puffer, an obese
patient with advanced
emphysema without
chronic bronchitis
having barrel-shaped
chest , dark red colored
skin due to
polycythemia .

On the other extreme are patients with emphysema who also have chronic bronchitis & a history of recurrent infections with purulent sputum .They usually have less prominent dyspnoea so they retain
carbon dioxide , they become hypoxic, often cyanotic
& for unknown reasons they tend to be obese .They are usually seeking medical help after theonset of congestive heart failure ( cor pulmonale ) . Such patients are called Blue bloater.

Photograph of emphysematous
patient with
chronic bronchitis (Blue bloater ),
a cyanotic patient with
bluish discoloration of skin &
mucous membranes .

Secondary pulmonary hypertension develops gradually arising from vascular spasm and loss of pulmonary
capillaries resulting from alveolar destruction.
Death in emphysema is related to either pulmonary failure with respiratory acidosis , hypoxia & coma or right heart failure i.e. cor
pulmonale .

Conditions related to Emphysema :
Compensatory emphysema :
A term used to describe a compensatory dilatation of alveoli in response to loss of lung substance as occurs inresidual lung parenchyma after surgical removal ofdiseased lung or lobe .

Obstructive over inflation :
Refers to a condition in which the lungs expand because air is trapped within it .A common cause is subtotal obstructiony atumor or foreign objects.
Obstructive over inflation can be life-threatening emergency if the affected portion extends to compress the remaining normal lung
Bullous emphysema :Refers to any form of emphysema that produce alarge sub pleural blebs or bullae i.e. air spaces large than 1cm. in diameter , when rupture lead to pneumothorax

Gross view of Bullous emphysema . Peripheral cystic
bulae may rupture causing pneum o thorax,i.e air within pleural cavities ,

Mediastinal ( interstitial ) emphysema :
Refers to entrance of air into the connective tissuestroma of the lung ,mediastinum & subcutaneous tissue .This may occur spontaneously due to increased in intra-alveolar pressure as withvomiting or cough that cause a tear with dissecting of air into the interstitium.May occur in children with whooping coughor fractured ribs.

When the interstitial air enters the subcutaneoustissues, the patient may literally blow up like a
balloon with marked swellingof the head and neck with crackling crepitations all over the chest .In most instances the air is resorbed spontaneouslywhen the site of entry is sealed.

Photograph of a patient
with interstitial
(mediastinal) emphysema.
Air is accumulating in
subcutaneous tissue of
mediastinum, the neck &
the face, following
fractured ribs.

Acute Respiratory distress syndrome
(ARDS):Also called shock lung ,or acute lung injury . It is a clinical
syndrome characterized by diffuse alveolar
capillary damage & clinically by sudden onset of severe
life- threatening respiratory insufficiency ,
cyanosis and severe arterial hypoxemia that is refractory to
oxygen therapy .
Chest X-ray shows diffuse alveolar infiltrate, due to diffuse
alveolar damage (DAD).

Pathogenesis :Clinical disorders are :
Direct lung injury :
Common causes :1 Pneumonias2 Aspiration of gastric content .
Uncommon causes :1 Pulmonary contusion.
2 Fat embolism.
3Near-drowning .
4- Inhalation injury .
5- Reperfusion after lung transplantation

Indirect lung injury :
1 Sepsis
2Severe trauma with shock.
3- Cardio-pulmonary bypass.
4- Acute pancreatitis .
5 Drug overdose .
6Transfusion of blood products .
7- Uremia

The alveolar capillary membrane is formed by two separate
barriers the microvascular endothelium and the alveolar
epithelium .
Pathogenesis :
In ARDS the integrity of this barrier is compromised either
by endothelial or epithelial injury or more commonly both.The acute consequence of the damage to this barrier include increased vascular permeability, alveolar
flooding i.e edema , loss of diffusion capacity & widespread
surfactant abnormalities caused by damage totype II pneumocytes .


As early as 30 minutes after acute injury there is increased synthesis of interleukin 8 by pulmonary macrophages . IL-8 is a potent neutrophil chemotactic& activating agent .
Neutrophils has an important role in pathogenesis of
ARDS .
The release of this mediator & other similar
compounds such as IL-1 & TNF leads to endothelial
activation & pulmonary micro-vascular sequestration Activated neutrophils release oxidants protease ,platelets activating factor and leukotriens that cause damage to alveolar epithelium .& maintain theinflammatory cascade .

Combined epithelial & endothelial injury lead to
increased vascular permeability & loss of surfactant
that render alveolar unit unable to expand .
The destructive force induced by neutrophils are
apposed by an array of endogenous antiprotease ,
anti-oxidants & anti- inflammatory cytokines e.g. IL-
10 that are unregulated by pro-inflammatory
cytokines
In the end the balance between the destructive
& the protective factors that determines the clinical
severity and the degree of tissue injury of ARDS.

Pathogen
es is of
ARDS

Morphology :
In the acute ARDS , the lungs are dark red ,firm airless and heavy .Microscopically:There is capillary congestion , necrosis of alveolar epithelialcells , interstitial and intraalveolar edema & hemorrhage andparticularly with sepsis i.e collection of neutrophils in capillaries .

The most characteristic finding is the presence of hayaline membrane particularly lining the distended alveolar ducts .Such membrane consists of fibrin- rich edema fluid admixed with reminants of necrotic epithelial cells .This is similar to that seen in respiratory distress
syndrome seen in the newborn in which
deficiency of pulmonary surfactant is the major
cause .

Microscopic view of ARDS ,showing hyaline membrane
deposition along alveolar septa (labeled with an arrow ) .

In the organizing stage there is marked proliferationof type II pneumocytes in an attempt to regeneratethe alveolar lining .Resolution is unusual , more commonly there is organization of the fibrin exudates with resulting intra-alveolar fibrosis .Marked thickening of alveolar septa ensues caused by proliferation of interstitial cells & deposition ofcollagen.

Clinical course :80% of patients develop the clinical symptoms of acute lung injury or ARDS within 72 hours of the initiating insult.The prognosis is gloomy and mortality rate reaches 100%.
The predicting factors in ARDS are-Age .- Underlying bacteremia or sepsis.- Development of underlying system failure as cardiac, renal or hepatic .If the patient could survive acute stage , then interstitial fibrosis occur and compromise respiratory function .If in patients who survive acute stage without the chronic sequelae , normal respiratory function returns within 6-12 months.

Pneumoconiosis
Is a non-neoplastic lung reaction to inhalation of mineral dusts.The term includes diseases caused by organic as well as inorganic particulates & some also include the chemical fumes and vapor-induced lung diseases.The most common & clinically significant lung diseases are those caused by the following mineraldusts :Coal dust SilicaAsbestos

Coal –mine workers are at high risk of
affected by anthracosis .

Pathogenesis of pneumoconiosis :The reaction of lung tissue to mineral dusts
depends on many variable :
(1)The amount of particles retained in the lung
&airways.
(2)The size the shape & the concentration of the
inhaled dust particles.
(3)Solubility & cytotoxicity of particles is influenced
by their size , the smaller the particles , the more
likely they appear in the pulmonary fluids & reach
the toxic levels rapidly.

Particles larger than 5-10 micrometer in diameter are unlikely
to reach distal airways , whereas particles smaller than 0.5
Mm tend to act like gases and move in & out of alveoli, often
without substantial deposition and injury .
Particles that are between 1-5 Mm in diameter are the most
dangerous , because they get lodged at the bifurcation of the
distal airways, and may reach the terminal small airways &
air sacs & settle in their linings .Most inhaled dusts are entrapped in mucus & rapidly removed from the lung by ciliary movement.Some dust particles become impacted at alveolar ducts bifurcations where macrophages accumulate andphagocytose the trapped particles .

Ultra structural view of Asbestos particles
( the Amphibole type ) straight stiff & brittle fibers .

The alveolar macrophages play a major role in the initiation
& perpetuation of lung injury & fibrosis .
The more reactive particles trigger the macrophages to
release a number of products that mediate an inflammatory
response & initiate fibroblastic proliferation & collagen
deposition .
Some of the inhaled particles may reach the lymphatics
either by direct drainage or the migrating macrophages &
thereby initiate an immune response to components of the
particles & or self proteins that are modified by the
particles.Tobacco smoking worsens the effects of all inhaled mineral dust, more severe with asbestos than with any other particle.

Coal- worker pneumoconiosis :
A condition affecting the coal- mine workers characterized by black lung usually with tuberculosis.Clinically it may be
1Asymptomatic anthracosis in which pigment accumulate without a perceptible cellular reaction .2simple coal worker pneumoconiosis (CWP) , in which accumulation of macrophages occur with littleto no pulmonary dysfunction .3Complicated CWP or progressive massive
fibrosis ( PMF) , in which fibrosis is extensive & lung function is compromised

Morphology :Pulmonary anthracosis is the most innocuous coal-induced pulmonary lesion in coal minors & is also seen in urban dwellers& tobacco smokers .Inhaled carbon particles are engulfed by alveolar & interstitial macrophages & then accumulate in the connective tissue along the lymphatics, including thepleural lymphatics &in lymph nodes .

Simple coal-worker pneumoconiosis :Is characterized b coal macules & somewhat larger
coal nodules.The coal macule consists of dust-laden macrophages inaddition the nodule contains small amount of a network of collagen fibers.Although these lesions are scattered throughout the lung, the upper lobes & upper zones of lower lobes are more heavily involved in due course,Centrilobular emphysema can coexist.

Gross appearance of the
lung in simple coal worker
pneumoconiosis. Black
carbon particles seen in
upper lobes.

Simple coal workers
pneumoconiosis i.e.
Anthracosis,
microscopic view
showing carbon
particles deposited
in peri bronchial
tissue within
macrophages &
extra cellularly.

Complicated CWP ,also called progressive
massive fibrosis (PMF):Occurs on a background of simple CWP by coalescence of coal nodules and generallyrequiresmany years to develop. It is characterized by intensely blackened scars larger than 2cm. sometimes up to10cm. in greater diameter. They are usually multiple. Microscopically: the lesion consists of dense collagenand pigment.

Gross view of massive
pulmonary fibrosis
dense fibrosis of lung
tissue, overlapping
dense carbon particles
deposition.

Microscopic view of complicated coal worker pneumoconiosis showing
black carbon particles deposits with fibrosis & emphysematous

Silicosis :Is currently the most prevalent chronic occupational disease in theworld. It is caused by inhalation of crystalline silica. Quartz is the most commonly implicated in silicosis.Morphology : Silicotic nodules are characterized grossly in their early stages by tiny palpable , discrete , pale to blackened nodules inthe upper zones of the lungs . Silicotic patients have increasedsusceptibility to tuberculosis . Combined silicosis & rheumatoid arithritis with pleural effusion is referred to as Caplan’s syndrome .Microscopically:The silicotic nodule demonstrate a concentrically arranged hyalinized collagen fibers surrounding the amorphous center .

Silica crystal .

Microscopic view of silicotic nodule consisting of dense
collagen deposition & fibrosis.

Asbestosis
Asbestos and asbestos-related diseases
Occupational exposure to asbestos is
linked to:
1Paranchymal interstitial fibrosis (
asbestosis ).
2Localised fibrous plaques .
3- Pleural effusions.
4 Bronchogenic carcinoma .
5Malignant pleural & peritoneal
mesothelioma .

Pathogenesis :
Concentration, size, shape & solubility of
the different forms of asbestos dictate
whether disease will occur. There are two
distinct forms of asbestos:
Serpentine chrysotile in which the fiber
is curly & flexible.
Amphibole in which the fiber is straight
stiff & brittle.

Ultra structural view of Asbestos particles (the Amphibole
type) straight stiff & brittle fibers.

Microscopic view of Asbestosis showing Asbestos body
within macrophages.

Asbestosis like other pneumoconiosis, causes
fibrosis by inter acting with lung
macrophages. In addition to cellular & fibrotic
lung reaction, asbestos also functions as both
a tumor initiator and a promoter. For example ,
the adsorption of carcinogens in tobacco
smoke on to asbestos fibers may well be
important to the remarkable synergy between
tobacco smoke and the development of
bronchogenic carcinoma in asbestos workers.

Morphology
Asbestos is marked by a diffuse pulmonary
interstitial fibrosis , with the presence of asbestos
bodies which are seen as golden brown fusiform or beaded rods with a translucent center, they consist ofasbestos fibers coated with an iron –containingproteinaceous material. Similarly the visceral pleura undergoes fibrous thickening and sometimes binds thelungs to the chest wall.

Microscopic view of pulmonary fibrosis with asbestos particles
within alveolar spaces labeled by arrow.

Pleural plaques:
• Are the most common manifestation of asbestos exposure and are awell circumscribed plaques of dense collagen often containing calciumthey develop on the anterior & posterior aspects of the parietal pleura &overlap the diaphragm. They do not contain asbestos bodies , they onlyrarely occur in persons who have no history of asbestos exposure.Uncommonly asbestos exposure induces pleural effusions which areusually serous but may be bloody. Both bronchogenic carcinoma as wellas both pleural & peritoneal mesotheliomas has an association withasbestos exposure.

Gross view of pleural plaques seen on diaphragms in
patient with chronic asbestosis.

Sarcoidosis :
A multisystem disease of unknown etiology characterized
by non-caseating granulomas in many tissues & organs.
The diagnosis of sarcoidosis is always by exclusion from
other conditions producing non-caseating granulomas
like Berylliosis, mycobacterial & fungal infections.
Bilateral hilar lymphadenopathy or lung involvement or
both, visible on chest x-ray is the major presenting
manifestation in most cases. Eye & skin involvement
each occurs in 25% of cases & may be the presenting
features of disease. The liver ,spleen ,bone marrow &
skeletal muscle, salivary glands ,CNS & other sites may
be involved.

Epidimiology:
Sarcoidosis occurs throughout the world affecting both sexes & all ages races. They tend to affectadults younger than 40 years of age. A high incidence among US African American in whom thefrequency of involvement is 10 times greater than US-American Caucasians. Sarcoidosis have higherprevalence among nonsmokers.

Etiology & pathogenesis :Although the etiology of sarcoidosis remain unknown , some of the evidence suggest that it is a disease ofdisordered immune predisposed individuals exposed to
regulation in geneticallycertain
environmental agents. Genetic influences in individualswith sarcoidosis are suggested by familial & racialclustering of cases & association with certain humanleukocytes antigens like Class 1 HLA1,HLB2 genotype.

Chest X-ray of
patient with
sarcoidosis
showing multiple
lung opacities.

Morphology : Non-caseating granulomas is the characteristichistological feature of sarcoidosis irrespective of organinvolved. This is discrete, compact collection ofepithelioid cells rimmed by an outer zone of CD+ Tcells. A thin layer of laminated fibroblasts is presentperipheral to granuloma over time these proliferate &lay down collagen. Two other microscopic features arecommonly seen in granuloma are:Schaumann bodies are laminated concressionscomposed of calcium & protein.Asteroid bodies: stellate inclusions enclosed withingiant cells .

Microscopic view of sarcoidosis . Non-caseating granulomas .

Microscopic view of non-caseating granuloma with giant cell in
sarcoidosis

The lungs are involved in 90% of patients . Thegranulomas frequently involve the interstitium ratherthan the airspaces with some tendency to localize inthe connective tissue around bronchioles & pulmonaryvenules & in the pleura i.e lymphangitic distribution.Intra thoracic & paratracheal lymph nodes areenlarged in 75% to 90% of patients.The lymph nodes are painless , firm rubbery , unlike TB
lymph nodes in sarcoidosis are non-adherent & non
caseating. Hypercalcemia & hypercalcuria , are
common features . This is not due to bone destruction ,
but due to increased calcium absorption secondary to
production of active vitamine D by mononuclear
phagocytes in the granuloma .

Microscopic
view of
sarcoidosis
showing
concentrically
calcified
Schaumann
body.

High power view of
Schaumann body, a
concentrically
calcified body seen
within giant cell in
sarcoidosis.

Clinical course:
In many individuals the disease is discoveredon routine chest film as bilateral hilarlymphadenopathy or incidently duringautopsy. Hepatomegally & splenomegally
may be present. In 1/3 of symptomatic casesthere is partial appearance of respiratorysymptoms (shortness of breath, cough &vague substernal discomfort). Constitutionalsymptoms including fever, fatique, nightsweats & anorexia. Lung & lymph node biopsyshow non-caseating granulomas.

Photograph showing eye & skin involvement by sarcoidosis .

Atelectasis ( Collapse):Is loss of lung volume caused
resultsby inadequate in shunting ofexpansion of airspaces. It
inadequate oxygenated blood from pulmonaryarteries into veins thus giving rise to a ventilation –
perfusion imbalance & hypoxia.

Classified into three forms :I-Resorption atelectasis :
Occurs when obstruction prevents air from reaching distal
airways . The air already present becomes absorbed &
alveolar collapse follows. Depending on the level of
airway obstruction an entire lung , a complete lobe or
one or more segments may be involved. The most
common cause of bronchial obstruction is mucus or
mucopurulent plug, accumulate post operatively , may
complicate bronchial asthma, bronchiectasis , chronic
bronchitis or aspiration of foreign bodies particularly in
children.

II. Compression atelectasis :
Sometimes called passive or relaxation atelectasis is usually
associated with accumulation of fluid , blood or air within the
pleural cavity, which mechanically collapse the adjacent
lung. This frequently occur with pleural effusion caused most
commonly by congestive heart failure . Leakage of air in
pleural cavity called pneumothorax also causes compression
atelectasis.
III. Contraction atelectasis :
Contraction or cicatrisation atelectasis occurs when either
local or generalized fibrotic changes in the lung or pleura.Atelectasis is potentially reversible & should be treatedpromptly to prevent hypoxia & super imposed infection of thecollapsed lung.

Diagram showing types of
lung atelactasis (collapse)
resorption, compression &
contraction types.


Pulmonary Hypertension
Normal pulmonary blood pressure is 1/8 of
systemic blood pressure i.e. 15/10mmHg.
Pulmonary hypertension is considered
when the mean pulmonary pressure
exceeds ¼ the systemic blood pressure.
(30/ 20mmHg). It is most frequently
secondary to structural cardiopulmonary
conditions that increase pulmonary blood
flow or pressure or both.

Causes of pulmonary hypertension :
1Chronic obstructive or interstitial lungdisease: cause hypoxia as well as destruction of lungparenchyma& hence have fewer alveolar capillariesthis increases pulmonary arterial resistance andincrease blood pressure.2Congenital or acquired heart diseases asmitral valve stenosis because of increase in left atrialpressure leading to increased pulmonary venouspressure & consequently increased pulmonary arterialpressure.

3- Recurrent thrombo-emboli: due to reduction inthe functional cross sectional area of pulmonaryvascular bed brought about by obstructing embolilead to increase in pulmonary vascular resistance .
4- Auto-immune disorders: as systemic sclerosisinvolving pulmonary vasculature leading to
inflammation, intimal fibrosis medial hypertrophy &pulmonary hypertension.
5- Primary or idiopathic pulmonary hypertension: when all the above causes are absent . 6% of cases are familial form due to autosomal dominant mode of inheritance.

Pathogenesis :
The primary familial pulmonary hypertension is caused by
mutations in Bone morphogenic protein receptor type 2(BMPR2) signaling pathway. In secondary pulmonaryhypertension: endothelial cell dysfunction is produced bythe process that initiate the disorder, & mechanical injuryassociated with left to right shunts or the biochemicalinjury produced by fibrin in thromboembolism. Decreasedelaboration of prostacycline and nitric oxide andincreased release of endothelin all promote pulmonaryvasoconstriction. Pulmonary hypertension as beenreported following ingestion of certain plants as Crotalariaspectabilisin tropics & used medicinally as bush tea , aswell as the apatite depressant agent aminorex ,adultrated olive oil and anti obesity drugs.

Morphology :
Vascular alterations in all forms of pulmonary hypertension
(primary or secondary) involve the entire arterial tree.
1 I n main elastic arteries atheroma seen.
2In medeium-sized muscular arteries proliferation of myo intimal
cells & smooth muscle cells causing thickening of the intima and
media with narrowing of the lumina.
3In smaller arteries & arterioles thickening , medial
hypertrophy & reduplication of the internal & external
elastic membranes may cause complete obliteration of the lumen.

Clinically :
Primary pulmonary hypertension is almost
always encountered in young persons more
common among women, marked by fatigue,
syncope on exercise, dyspnoea on
exertion & sometimes chest pain, may develop
severe respiratory insufficiency & cynosis.
Death result from right sided heart failure, cor
pulmonale develop within 3- 5 years after
diagnosis.

Good pasture syndrome :
A diffuse hemorrhagicinterstitial alveolar disease, an uncommon condition characterized by a proliferativeusually progressive glomerulonephritis & hemorrhagic interstitial pneumonitis. Both renal & pulmonary lesionscaused by an antibody targeted against collagen type IV
i.e. (basement membrane). These antibodies are seen in 90% of patients.

Morphology:
In classic diffuse alveolar hemorrhage , the lungs are heavy with areas of red brown consolidations.Microscopically: Necrosis of alveolar walls with thickening
of the septa & hypertrophy of septal lining cells. The
presence of hemosiderine either within macrophages or
extra cellularly is seen few days after presentation. IgG,
Igm & IgA seen in renal biopsy & in alveolar septa.
Plasmapheresis & immunosuppressive therapy improved
the prognosis of the disease.
Plasma exchange remove the offending antibodies &
immunosuppressive therapy inhibit antibody production.

Gross appearance of
lungs in Good Pasture
syndrome. Red lungs
due to pulmonary
hemorrhage.

Microscopic view of lung in Good Pasture syndrome showing
recent (left) & old (right) intra alveolar hemorrhage.





![Respiratory System [โหมดความเข้ากันได้] · PATHOLOGY OF RESPIRATORY SYSTEM นพ. อรรณพ นาคะป ท Respiratory system U it](https://static.fdocuments.in/doc/165x107/5fa578efd4e80f055f6b3401/respiratory-system-aaaaaaaaaaaaaaaaaa-pathology.jpg)