Human Anatomy & Physiology CIRCULATORY & RESPIRATORY SYSTEMS 1.
Respiratory anatomy and Physiology
description
Transcript of Respiratory anatomy and Physiology

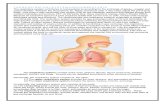
Respiratory anatomy and Physiology
Caia Francis
Chair RCN Respiratory Forum
Senior Lecturer- Respiratory Specialist
0117 32 88631

Outline of session Review and orientation to respiratory
anatomy and physiology. Learning outcomes:
– Understand fundamental law of diffusion and apply it to gas exchange.
– Understand the mechanics of breathing and how this is influenced to maintain ‘normal’ respiratory functioning.

Respiratory Physiology.
Lung is for gas exchange. Prime function is to allow oxygen to move
from the air into the venous blood and carbon dioxide to move out.
Metabolizes some compounds, filters toxic materials from the circulation and acts as a reservoir for blood.

Oxygen and carbon dioxide move between air and blood by simple diffusion, i.e. from an area of high to low partial pressure. (Fick’s law of diffusion). Blood- gas barrier is exceedingly thin and has an area of between 50- 100 m2.
Large surface area is obtained by wrapping capillaries around air sacs (form alveoli). 300 million alveoli in human lungs.

Airways consist of a series of branching tubes, becoming narrower, shorter and more numerous as they penetrate deeper into the lung.
Trachea divides into right and left main bronchi, divide into lobar, then segmental bronchi. This process continues down to terminal bronchioles, smallest airways outside the alveoli.

These make up the conducting airways. Function is to lead inspired air into gas exchanging regions of the lung.

Terminal bronchioles divide into respiratory bronchioles, finally arriving at the alveolar ducts, which are completely lined with alveoli.
This region is known as the respiratory zone. Portion of lung distal to a terminal bronchiole
forms an anatomical unit called acinus or lobule.

Ventilation
Static volumes of the lung can be measured mainly by spirometry.
Tidal volume Vital capacity. Minute volume. But some gas remains in the lungs, residual
volume and functional residual volume. Measured by body plesthysmography.

Ventilation -part 2
Volume exhaled with each breath is 500ml, 15 breaths per minute; total volume leaving the lung each minute is?
500*15 = 7500ml/min. =Total ventilation or minute volume. But not all air that passes lips reaches the
aleovlar gas compartment where gas exchange occurs.

Anatomic dead space.
Volume of the conducting airways. Normal value is circa 150ml, but depends
upon the size of inspiration and posture of subject.

Physiologic dead space.
Volume of the lung which does not eliminate CO2.
In normal subjects this is nearly the same as anatomic dead space.
However in patients with lung disease the physiologic dead space may be considerably larger because of inequality of blood flow and ventilation within the lung.

Regional differences in ventilation (V) (upright person)
Upper zone lowest ventilation
Lower zone greatest ventilation.

Blood flow (Q) through the lungs
Regional variations in blood flow through the lungs.
Lowest blood flow
Highest blood flow.

In ‘well’ human
O2 will have fully diffused across alveolar membrane to bind with Hb within 0.25s.
C02 will have diffused across the alveolar membrane within 0.25s to be expired.
Blood will take 0.5s to traverse pulmonary capillary in association with alveolar sac.

Respiratory disease.
Asthma… mucus, airway thickening (hypertrophy) will increase ‘width’ of alveolar membrane and thus delay diffusion across membrane of both CO2 and O2.
COPD as above plus pulmonary and cardiac circulation problems will delay the above.
Genetic conditions eg cystic fibrosis will compromise blood flow through alveolar.

What happens once oxygen is delivered to the alveoli? Oxygen dissociation curve. Dissolved oxygen in blood, in some cases
of significance in respiratory disease.

Oxygen dissociation curve.
Haemoglobin (Hb) 02 forms easily
reversible combination with Hb to give oxyhaemoglobin.
02 + Hb HbO2
Consider this in more detail.

Oxygen dissociation curve.
Consider: anaemia Hb 10gdl-1
Altitude. Paediatrics. Temperature. pH.


Why do you need to know this?
Understand normal respiration and its measurement, function.
Establish a common frame of reference. Revise known anatomy and physiology. Introduce some issues of importance in
respiratory disesase.

Mechanics of breathing.
Inspiration: lower intra-thoracic pressure to allow air to pass by diffusion into lungs. Usually only 1cmH20 lower but in respiratory disease can be many times greater.
Diaphragm moving down in quiet breathing. Expansion of rib cage in rapid deep breathing
and using accessory muscles.

Expiration. Diaphragm returning to rest. Ribs returning to status quo. Increases slightly intra- thoracic pressure
higher than the atmosphere and allows expiration. Usually only 1cmH20 higher but in respiratory disease can be many times greater.

Positive end expiratory pressure (PEEP) aides in complete expiration.
Occurs in ‘well individuals’ easily and automatically.

References.
Francis C., (2006) “Respiratory care” Blackwell Publishing Oxford Jevon P., Ewens B., (Eds) (2002) “Monitoring the critically ill
patient” Blackwell Science Oxford. Levitzky M. (2002) 7th Edition “Pulmonary Physiology” McGraw
Hill New York. West J., (2010) 8th Edition. “Pulmonary Pathophysiology” Lippincott
Williams & Wilkins London. West J., (2009) 10th Edition. “Respiratory Physiology the
essesentials” Lippincott Williams & Wilkins London. Woodcock A., Partridge M., (1995) “Respiratory Handbook”
Boehringer Ingelheim.














![Anatomy and Physiology Respiratory System [Tab 2] Respiratory System.](https://static.fdocuments.in/doc/165x107/56649ebd5503460f94bc631f/anatomy-and-physiology-respiratory-system-tab-2-respiratory-system.jpg)



