Radial nerve palsy clinical features and diagnosis
-
Upload
subhakanta-mohapatra -
Category
Health & Medicine
-
view
694 -
download
5
description
Transcript of Radial nerve palsy clinical features and diagnosis

Radial Nerve Palsy
Clinical features & Diagnosis
Dr Subhakanta MohapatraIPGME&R,Kolkata.INDIA

Anatomy

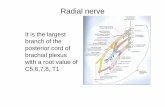
• Largest branch of the brachial plexus• Arises from the posterior cord of the
brachial plexus (C5–8)• Mixed nerve
Radial Nerve

Course of Radial Nerve (RN) in the arm
In the axilla, RN lies anterior to subscapularis,
teres major and LD
• Sensory supply: Posterior cutaneous nerve of arm
RN leaves the axilla via the triangular space
• Motor supply: long head of Triceps
It then comes to lie along spiral groove on
posterior aspect of humeral shaft along with arteria profunda brachii
• Motor: medial and lateral heads of triceps, Anconeus
• Sensory: posterior cutaneous nerve of forearm, lower lateral cutaneous nerve of arm

RN then leaves the spiral groove by piercing the lateral
intermuscular septum to enter the anterior compartment of the arm, 10-12 cm above the lateral
epicondyle
• Motor supply: Brachialis (lateral part), BR, ECRL
Anterior to lateral epicondyle, RN divides into its terminal branches
• Terminal branches: Posterior Interosseous Nerve (PIN) and Dorsal or Superficial radial sensory nerve
Here it lies b/w brachialis and BR

Radial nerve (C5, 6, 7 , 8, T1) exiting axilla via the triangular space
Brachialis (lateral part)
Anconeus
Triceps brachii
Posterior cutaneous nerve of forearm
Posterior cutaneous nerve of arm
Lower lateral cutaneous nerve of arm
Radial nerve in the spiral groove (posterior aspect of humeral shaft)
Brachioradialis (BR)
ECRL (last branch of radial nerve proper)
Lateral intermuscular septum

BR
ECRL
Dorsal Radial Sensory Nerve
Dorsal digital nerves
Radial styloid
8 cm
Dorsal radial nerve courses through the forearm immediately
deep to the BR
It emerges b/w tendons of BR and
ECRL ≈ 8 cm proximal to radial styloid, to
become subcutaneous
It crosses the anatomical snuffbox
b/w EPB and EPL, dividing into multiple
branches to supply sensation to hand
Course of Radial Nerve (RN) in the forearm

Deep terminal branch → Posterior interosseous nerve (PIN)
Supinator
EIP
EDC and EDM
ECU
ECRB
Superficial terminal branch
Radial Nerve Proper
EPL
EPB
APL
PIN reaches the back of forearm by passing around the lateral aspect of the radius b/w the superficial and deep heads of the Supinator to supply all extensor compartment muscles
Finally, PIN ends by supplying carpal joint sensation

Lower lateral cutaneous nerve of arm
Posterior cutaneous nerve of arm
Posterior cutaneous nerve of forearm
Dorsal radial sensory nerve
Gives sensibility to the dorsum of the hand over the radial two-thirds, the dorsum of the thumb, and the index, long, and half of the ring finger proximal to the distal interphalangeal joint.
Cutaneous innervation from radial nerve

Clinical Features

Functional motor deficitInability to extend the wrist (in case of injury at level of PIN, wrist extension is weak with radial deviation since ECRL innervation is intact)
Inability to extend the fingers at the MCP joints
Inability to extend and radially abduct the thumb
Weakness of grip strength d/t loss of mechanical advantage that wrist extension provides for grasp and power grip

Area of sensory loss in radial nerve injury in the axilla
Unlike the median and ulnar nerves, sensory loss following radial nerve injury is not functionally disabling unless the patient develops a painful neuroma
Sensory Loss
Autonomous sensory zone for radial nerve → dorsum of 1st webspace
The Lateral cutaneous nerve of forearm has a significant overlap pattern with the Superficial radial sensory nerve

Radial Nerve Compression Syndromes

Wartenberg’s syndrome
• Aka: Cheiralgia paresthetica• D/t compression of Superficial radial nerve as it
emerges b/w ECRL and BR, 8 cm proximal to radial styloid

isolated pain or paresthesias over the dorsoradial aspect of the hand
preceding history of trauma to the area (i.e., handcuffs, forearm fracture)
Differentiating Wartenberg’s syndrome from de Quervain’s tenosynovitis
A Tinel’s sign over the superficial sensory radial nerve is the most common exam finding
Clinical features
presence of motor weakness suggests a more proximal site of compression
Also seen in patients who use forearms in pronated position for extended periods → in pronation, the tendons of BR and ECRL approximate and may compress the nerve
▪In WS, pain is exacerbated by pronation, while in DQT pain is elicited with changes in thumb and wrist position▪DQT - normal sensation in the dorso-radial hand▪DQT - pain on percussion over the 1st extensor compartment
Electrodiagnostic testing is of limited value in Wartenberg’s syndrome

Posterior interosseous nerve (PIN) syndrome
• D/t compression of PIN in the radial tunnel• Most common causes include:
▪Tumors such as lipomas, ganglia ▪Rheumatoid synovitis ▪Septic arthritis ▪Vasculitis

The radial tunnel is a 5 cm space bounded by:▪Dorsally: capsule of the radiocapitellar joint ▪Volarly: the BR▪Laterally: the ECRL and ECRB muscles ▪Medially: the biceps tendon and brachialis muscles
Within radial tunnel, there are 5 potential sites of compression: ▪fibrous bands to the radiocapitellar joint between the brachialis and BR ▪the recurrent radial vessels (leash of Henry)▪the proximal edge of the ECRB ▪the proximal edge of the Supinator (arcade of Fröhse)▪the distal edge of the Supinator
BR
Supinator
arcade of Fröhse
ECRL
PIN

Diagnosis
loss of finger and thumb extension
Weak wrist extension with radial deviation (since ECRL innervation is intact)
Intact passive tenodesis effect (rules out extensor tendon rupture)
EMG testing is helpful to confirm the diagnosis and monitor motor recovery

Radial Tunnel syndrome
• Similar to PIN syndrome, it is also d/t compression of PIN in the radial tunnel
• Not considered a true compression neuropathy by some

Radial Tunnel Syndrome is a clinical diagnosis
Radial Tunnel
Syndrome
Tenderness over radial tunnel (lateral proximal
forearm, 3-4 cm distal to lateral epicondyle over the mobile wad)
Pain at ECRB origin with resistance of
middle finger extension
Pain with resisted forearm
supination↑ Pain on combined elbow extension,
forearm pronation, and wrist flexion

Proximal Radial nerve compression
• Compression of the radial nerve proximal to the elbow is uncommon
• Causes: ▪Fibrous arch from the lateral head of triceps ▪After strenuous muscular activity ▪Bony exostosis of humerus ▪Injury in spiral groove: ▫# shaft humerus ▫‘Saturday night palsy’ (neuropraxia) ▫Post injection palsy (chemical neurotmesis)
• Patients present with variable degrees of radial nerve dysfunction

Diagnosis

Mechanism of injury (e.g. sharp penetrating vs. blunt trauma)
Timing of injury
Loss of motor and sensory function
Presence of pain
Interval recovery of function in patients presenting late
History

Assessment of motor function
Assessment of sensory function
Assessment of involved joints
Physical Examination
Individual muscles innervated by the nerve are tested to determine what is functioning and what is not:▪Helps to determine the level of injury▪Guides future surgical planning
▪Elicitation of Tinel’s sign▪Specific sensory testing
Each joint is taken through its passive range of motion to assess for suppleness → presence of fixed joint contractures in delayed presentations is associated with poor treatment outcomes

Specific sensory testsTest Perception Main receptor Comments
Static 2 point discrimination (2PD)
Tactile Merkel cell ▪Evaluates sensory receptor innervation density▪Normal distance: 6mm
Moving 2PD Tactile Meissner corpuscle ▪Normal distance: 3mm
Tuning fork (250 Hz) Vibration Pacinian corpuscle
Tuning fork (30 Hz) Vibration Meissner
Semmes-Weinstein monofilament test
Pressure Merkel
Ten test (moving light touch)
Pressure Merkel ▪Reliability comparable to monofilament test
Cold-heat test Temperature Free nerve endings
•Changes in Vibration and Pressure thresholds are seen in early nerve compression but are unreliable for evaluating nerve lacerations•Changes in sensory receptor innervation density (2PD) are seen in chronic nerve compression but are reliable for evaluating nerve lacerations

Electromyography (EMG)
Nerve conduction studies (NCS) Electrodiagnosti
c testing
Helpful in arriving at a diagnosis in presence of atypical presentations or equivocal clinical findings
Limitations of EDT:▪Evaluates only large myelinated fibres → smaller axons conveying pain and temperature are not assessed▪Changes in unmyelinated nerve fibres, which are the first to be affected in nerve compressions, are not evaluated▪Performing the test before 3-6 weeks post injury can give inaccurate results▪Very proximal or distal nerve injuries are difficult to assess▪Unreliable assessment of multi-level injuries▪Examiner dependant

Nerve conduction studies (NCS)2 electrodes are placed along the course of the nerve. The first electrode stimulates the nerve to fire, and the second electrode records the generated action potential
Amplitude• represents the size of the response• proportional to the number of
depolarizing axons in the nerve
Latency• the delay in response following
stimulation
Conduction velocity
Sensory nerve action potential (SNAP)• Response obtained when the
recording electrodes is placed proximally along the sensory nerve, toward the spinal cord

Electromyography (EMG)
Insertional activity • Activity observed when a needle electrode is inserted into the muscle
▪Fibrillation potentials ▪Fasciculations
• Seen when the muscle is at rest• Absent in normal muscles
Motor unit potentials (MUPs)
• Generated by the muscle during a voluntary contraction
• Evaluates the integrity of neuro-muscular junction

Sequence of events in nerve compression
Focal demyelination
Axonal damage at the compression site
Further axonal loss
Axonal sprouting producing collateral re-innervation
Remyelination following decompression
▪↑Latency▪↓Nerve conduction velocity
Associated Electrodiagnostic findings
▪↓SNAP▪↓CMAP
▪↑Insertional activity▪Fibrillation potentials and fasciculations
▪’Giant’ MUPs
▪Normalization of NCV▪Loss of ‘giant’ MUPs