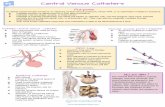
Advances in Tunneled Central Venous Catheters for Dialysis: Design
Placement of Subclavian Venous Catheters
-
Upload
courtneykd -
Category
Documents
-
view
232 -
download
0
Transcript of Placement of Subclavian Venous Catheters
-
7/25/2019 Placement of Subclavian Venous Catheters
1/36
Official reprint from UpToDate
www.uptodate.com2015 UpToDate
Authors
Alan C Heffner, MD
Mark P Androes, MD
Section Editors
Allan B Wolfson, MD
John F Eidt, MDJoseph L Mills, Sr, MD
Deputy Editor
Kathryn A Collins, MD, PhD,
FACS
Placement of subclavian venous catheters
All topics are updated as new evidence becomes available and our peer review processis complete.
Literature review current through: May 2015. | This topic last updated: Jan 20, 2015.
INTRODUCTION Central catheters provide dependable intravenous access and enable hemodynamic
monitoring and blood sampling [1-3]. The subclavian veins are a common site for temporary central venous
access, including tunneled catheters and subcutaneous ports for chemotherapy, prolonged antibiotic
therapy, and parenteral nutrition.
Subclavian venous cannulation and catheter placement will be reviewed here. General considerations,
complications of venous access, and issues related to other access sites are discussed elsewhere. (See"Overview of central venous access"and "Complications of central venous catheters and their prevention"
and "Placement of jugular venous catheters"and "Placement of femoral venous catheters".)
INDICATIONS The subclavian veins are reliable access points for temporary and permanent (eg,
tunneled central catheters and subcutaneous ports) venous cannulation to support hemodynamic
monitoring, fluid and medication administration, and parenteral nutrition (table 1). The left subclavian access
is particularly well suited for cardiac access, including placement of pulmonary artery catheters, transvenous
pacer leads, and implantable defibrillators.
Subclavian venous access may be preferred for subcutaneous port placement due to the short distance
between the subclavian vein and chest wall, making the catheter less prone to kinking.
Contraindications Relative contraindications to subclavian venous catheterization include coagulopathy
and altered local anatomy [4-8]. (See "Overview of central venous access", section on 'Contraindications'.)
Subclavian access should be avoided, if possible, at sites with altered local anatomy (eg, previous clavicle
fracture), prior access, or the presence of an indwelling pacemaker or internal defibrillator because these are
associated with a higher risk of failure, complication, and malposition [9,10].
In patients with significant unilateral lung disease, cannulation of the vessel ipsilateral to the compromised
lung is preferred to avoid decompensation in the event of a procedure-related pneumothorax.
The subclavian site should be avoided for large bore hemodialysis catheters due to the risk of venous
stenosis that limits outflow for future arteriovenous hemodialysis access [11,12]. (See "Overview of central
catheters for acute and chronic hemodialysis access", section on 'Access site considerations'.)
The subclavian access site is not appropriate for the short, relatively stiff catheters used for acute
hemodialysis or pheresis. These catheters do not have the flexibility needed to negotiate the curve from the
brachiocephalic vein into the superior vena cava. Perforation of the central veins can occur. (See
"Complications of central venous catheters and their prevention".)
Coagulopathy is a relative contraindication to central cannulation. However, there is little quality evidence to
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
2/36
support this preference [4]. Although significant bleeding is uncommon, the subclavian approach is generally
avoided in patients with significant coagulopathy, including therapeutic anticoagulation, if an alternative
access point is available. Bleeding from the subclavian vein or inadvertent subclavian artery puncture may
go unrecognized and cannot be treated with direct pressure due to the deep location of these vessels
beneath the clavicle.
SUBCLAVIAN VEIN ANATOMY The clavicle is the primary surface landmark for subclavian cannulation
(picture 1). Moving laterally from the suprasternal notch, the bulky sternal head takes an elongated S-shape(a double curve in the horizontal plane); the medial two-thirds are convex anteriorly, and the lateral third is
concave anteriorly. The anterior convexity at the junction of the medial and middle thirds is known as the
"bend" or "break" in the clavicle, and serves as an important palpable landmark. (See 'Subclavian vein
cannulation'below.)
The subclavian vein is the direct continuation of the axillary vein beginning at the lateral border of the first rib
(figure 1and picture 1). The vein arches cephalad behind the medial clavicle and then slopes caudally to join
the internal jugular vein to form the brachiocephalic (innominate) vein posterior to the sternoclavicular joint.
The vein is accompanied by the subclavian artery located superior and posterior to the vein, and separated
from the vein by the anterior scalene muscle.
The neck is a complex area with multiple structures traversing the thoracic outlet. Injury is avoided by
knowing the location of these structures relative to the subclavian cannulation sites.
SUBCLAVIAN SITE SELECTION Right-handed operators often prefer right-sided subclavian access
procedures. Right subclavian anatomy carries the theoretical advantage of lower risk of complications due to
the lower pleural apex and absence of the thoracic duct. However, right-sided subclavian access is
associated with higher rates of catheter malposition and vessel trauma compared with left-sided access [13].
A left-sided access may be preferred when immediate cardiac access is needed (eg, temporary transvenous
pacer placement, pulmonary artery catheter) since the guidewire and catheter are more easily directed into
the superior vena cava and right heart.
We access ipsilateral to the compromised lung in patients with significant unilateral lung disease to avoid
respiratory compromise in the event of a pneumothorax. (See 'Contraindications'above.)
In patients with prior catheter placement in the subclavian or internal jugular veins, or a history of upper
extremity deep venous thrombosis, consider ultrasound to assess venous patency prior to attempting
subclavian access. (See "Catheter-related upper extremity venous thrombosis", section on 'Duplex
ultrasonography'.)
GENERAL PREPARATION General considerations for patient preparation, including catheter and access
site selection, monitoring and sedation, measures to control infection, and consent, are discussed
elsewhere. (See "Overview of central venous access", section on 'Preparation'.)
The lung lies deep and inferior to the medial portion of the subclavian vein. The dome of the left lung
often extends above the level of the first rib on the left, but rarely on the right.
!
The phrenic nerve passes inferiorly along the anterior aspect of the anterior scalene muscle and
posterior to the origin of the brachiocephalic vein.
!
The brachial plexus is superior and deep to the medial portion of the subclavian artery.!
The left-sided thoracic duct and right-sided lymphatic duct course posterior to the subclavian vein and
enter the vessel near the confluence of the left subclavian vein with the left internal jugular vein.
!
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
3/36
Equipment Subclavian venous catheters and other subclavian venous devices are usually placed using a
modified Seldinger technique in a series of defined steps usually using a kit that contains all the materials
needed for their placement. Typical supplies are given in the table (table 2) [14]. For non-tunneled catheters,
the steps for central venous catheterization are given in the table ( table 3). For tunneled catheters and other
devices, the steps are similar except that a sheath is placed over the guidewire and the catheter (or other
device such as pacemaker leads, filter) is placed through the sheath, which is then removed.
Prior to the placement of subclavian venous catheters, assemble the following equipment:
The proper functioning of any fluoroscopic equipment that will be used should be verified. Fluoroscopy is
rarely needed for subclavian access, but is routine when placing implanted catheters or devices (eg,
pacemaker, defibrillator, pulmonary artery catheter, vena cava filter) to measure the length of the catheter
needed and to image the sheath or device as it is introduced into the vein.
Skin preparation For subclavian venous access, a wide skin preparation that includes the neck and
chest above the nipple line allows the operator to attempt cannulation at an alternative ipsilateral target (eg,
jugular), if the initial plan fails. If difficult access is anticipated, the neck and chest can be prepared
bilaterally.
Positioning For subclavian venous access, the clinician should position the patients bed or procedure
table at a comfortable height. The position of the operator depends upon the vein cannulation technique
chosen. We prefer to stand at the patients shoulder for infraclavicular access. Standing at the head of the
bed is an alternative for the supraclavicular technique. (See 'Approaches to the subclavian vein'below.)
Unlike the jugular vein, Trendelenburg positioning does not significantly affect subclavian diameter, but
Trendelenburg positioning may help prevent air embolus [15-18]. Most patients can be safely positioned
supine or in Trendelenburg position. However, critically ill and obese patients may develop respiratory
compromise and close monitoring is required. Successful supraclavicular subclavian cannulation has been
performed in upright and prone positions under extenuating circumstances [19]. Some patients may require
anesthesia with a controlled airway for safe placement of central venous catheters and devices. (See"Anesthesia for the obese patient", section on 'Patient positioning'.)
Various anatomic studies have shown that the relationship between the subclavian vein and clavicle change
with head, arm, and shoulder positioning [15,16,20-22].
Shoulder elevation shifts the point of intersection of the vein with the clavicle more medially, and the length
of overlap is reduced. Thus, to facilitate subclavian cannulation, we place the patients arms at their sides
Ultrasound machine (see "Principles of ultrasound-guided venous access", section on 'Ultrasound
machine preparation').
!
Sterile ultrasound transducer gel!
Central line kit with intravenous catheter (size and length based upon diameter and depth of vein)!
Sterile drapes, gloves, gown, surgical mask, and cap!
Topical antiseptic (eg, chlorhexidine, povidone iodine) (see "Adjunctive measures for prevention of
surgical site infection in adults", section on 'Skin antisepsis')
!
Local anesthetic (see "Topical anesthetics in children"and "Infiltration of local anesthetics").!
Isotonic saline and/or heparin for flushing the catheter!
Transparent adhesive dressing, tape!
Intravenous tubing and connectors (eg, needleless Luer connector, three-way stopcock)!
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
4/36
(adducted) and use a neutral to lower shoulder positioning, which increases the area of contact between the
subclavian vein and the undersurface of the clavicle providing a consistent landmark. A shoulder position 5
cm below neutral shoulder position appears to provide maximal amount of overlap [21]. The natural
tendency for the shoulders to assume a cephalad orientation with Trendelenburg position can be countered
by gentle caudal traction on the arm performed by a bedside assistant. One small clinical trial demonstrated
improved cannulation using caudal arm traction [21].
Recommendations to turn the head toward the side of the cannulation are based on anatomic studies andreduced catheter malposition in a single pediatric study, but such positioning has had no effect in trials on
adult patients [23-25].
Special considerations for positioning patients for infraclavicular versus supraclavicular access include:
SUBCLAVIAN VEIN CANNULATION The subclavian vein is generally cannulated using one of three
anatomic approaches with a large bore access needle using landmark techniques. Following cannulation,
subclavian catheters are placed using an orderly sequence of steps (table 3).
Needle access Although ultrasound-guided subclavian venous access has been described, no significant
benefit as yet has been identified for this access site, and thus, landmark techniques are used for needle
placement. (See 'Dynamic ultrasound guidance for subclavian access'below.)
General techniques Although less commonly used compared with internal jugular vein cannulation, a
seeker needle may, at times, be useful. Angiocatheters (catheter over a needle) are less commonly used to
access the subclavian vein. The general technique for each of these is described below. Isolated arterial
needle puncture is one of the most common complications of venous access, but is typically uneventful if
recognized prior to vessel dilation [28]. Confirmation that the access needle is in the vein is essential prior to
dilating the subcutaneous tissue and vein. (See 'Venous confirmation'below.)
There is a learning curve for central venous access procedures [29]. Experienced operators enjoy greater
success rates with fewer complications. Among both experienced and inexperienced operators, complication
rates increase with the number of introducer needle passes, and are significantly higher after two
unsuccessful passes [2,10,30]. If two attempts have been made, the needle should be completely removed
and the surface landmarks reassessed, a new access site chosen, or assistance from a more experienced
clinician obtained [2,9,26].
Access with introducer needle To access the subclavian vein with the 18 gauge introducer
needle:
For infraclavicular subclavian access (figure 2and picture 1), a small sandbag or rolled towel can be
placed between the scapulae to retract the shoulders and facilitate needle insertion by reducing the
deltoid prominence [26]. The maneuver also positions the vein closer to the clavicle for a more
consistent landmark [16,20]. Avoid excessive retraction because this reduces the anterior-posterior
dimension of the vein, flattening it [23].
!
For supraclavicular subclavian access (figure 3A-B), the lateral border of the clavicular head of thesternocleidomastoid muscle is the point of venous access. Contralateral rotation of the head away from
the site of access provides unobstructed access [27].
!
Insert the introducer needle into the skin and apply continuous negative pressure by pulling back on
the plunger of the syringe. Vein penetration will not be recognized unless negative pressure is applied,
but only a small amount of continuous negative pressure is needed (about 1 cc of a 10 cc syringe)
!
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
5/36
Using a seeker needle Although more commonly used for internal jugular vein localization, a
small caliber (21 to 22 gauge) exploratory seeker (or finder) needle, 3.5 cm in length, may help locate the
subclavian vein (picture 2) [9,32,33]. This technique minimizes injury in the event of inadvertent arterial
puncture. However, with the infraclavicular approach to the subclavian vein, the seeker needle may not be
long enough to reach the vessel in some patients.
To use a seeker needle to aid introducer needle placement:
Using an angiocatheter An angiocatheter consists of an 18 gauge plastic catheter mounted on a
20 gauge needle. It is not commonly used for infraclavicular subclavian vein access and may not be long
enough to reach the vessel in some patients. However, the angiocatheter is a useful adjunct for the
supraclavicular approach. The technique for using an angiocatheter to access the internal jugular or femoral
vein is described separately. (See "Placement of jugular venous catheters", section on 'Using an
angiocatheter'and "Placement of femoral venous catheters", section on 'Using an angiocatheter' .)
Approaches to the subclavian vein The subclavian vein can be approached from above or below
the clavicle. The landmarks and needle placement for each of these approaches are presented below.
Infraclavicular approach Three insertion points are described for the infraclavicular approach to
the subclavian vein. The midpoint approach is the most commonly used technique [ 3,20].
during advancement of the needle.
Always advance and withdraw the needle in the same vector. Lateral movement of an inserted needle
can lacerate vessels and should notbe done. Prior to any redirection of the needle, it should be
withdrawn to the skin surface.
!
Anticipate that venous backflow into the introducer needle will be sudden, and steady the position of
your hand to avoid dislodgement from the vein when this occurs.
!
Failure to aspirate blood during needle advancement is common. In this circumstance, withdraw the
needle slowly while maintaining continuous negative pressure. Venous puncture may only be
recognized during needle withdrawal as the compliant vein may not be punctured during initial needle
advancement in up to one-third of cases [31]. Once access is achieved, stabilize the hub of the needle
and carefully remove the syringe to avoid dislodging the introducer needle from the vessel.
!
Cover the hub of the needle between manipulations and coordinate hub exposure with the patients
exhalation to avoid air entry during the subclavian access. Encourage the patient to hum or perform
Valsalva maneuvers to augment central venous pressure.
!
As described above for large-bore needle access, insert the seeker needle while applying negative
suction on the plunger of the syringe; more suction will be required (about 2 to 3 cc of a 10 cc syringe).
Steady, unimpeded blood return confirms intraluminal venous placement.
!
Once the needle enters the vein, withdraw the seeker needle, noting the angle and depth needed to
reach the vein. Alternatively, remove the syringe leaving the seeker needle in place to anchor thevessel and provide a guide for venous access by the introducer needle. While applying negative
pressure to the syringe, advance the introducer needle in the same vector, or alongside the preceding
seeker needle, into the vein.
!
For the midpoint approach, the needle is inserted 2 to 3 cm inferior to the midpoint of the clavicle
(approximately 1 to 2 cm lateral to the bend of the clavicle) and directed just posterior to the
!
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
6/36
After the needle has penetrated the skin, the clavicle may be initially contacted. Take care not to push the
needle into the periosteum, as bone plug can occlude the lumen of the needle. The needle should be gently
walked deeper to reach the underside of the clavicle. The needle should remain parallel to the clavicle (in
the coronal plane) to allow it to pass cleanly beneath the bone and minimize the risk of pleural puncture. As
the needle passes beneath the junction of the middle and medial thirds of clavicle, it should enter the vein. If
the first needle pass is unsuccessful, orient the needle more cephalad on subsequent attempts.
An observational study at a large trauma center evaluated the most common errors during the placement of
infraclavicular subclavian venous access [35]. The most frequently observed errors during videotapedassessment of venous cannulation in 86 patients included improper or inadequate identification of anatomic
landmarks, improper needle insertion site, too shallow a needle trajectory, and insertion of the needle
through the periosteum of the clavicle.
Supraclavicular approach The supraclavicular approach aims to puncture the subclavian vein
near its junction with the internal jugular vein. The insertion of the clavicular head of the sternocleidomastoid
is the access landmark for this approach (figure 3Aand figure 3B).
The subclavian vein is 1 to 1.5 cm deep to the skin and easily reached using a seeker needle [ 36]. The
needle should be inserted 1 cm posterior to the sternocleidomastoid and 1 cm cephalad to the clavicle. The
needle is depressed 10 to 15 degrees below the coronal plane and oriented to bisect the angle between the
clavicle and the sternocleidomastoid (picture 4). The needle is advanced toward the venous confluencebehind the medial clavicle along a trajectory aimed just inferior to the contralateral nipple.
Axillary approach This approach is an uncommonly used technique accessing the vessel at the
junction of the subclavian and axillary veins via an ultrasound-guided infraclavicular approach.
Dynamic ultrasound guidance for subclavian access Although commonly used and recommended
for internal jugular and femoral venous access sites, real-time ultrasound guidance for both infra- and
supraclavicular approaches to the subclavian vein are described [31,37,38]. Technical complexity in
visualizing the vein due to acoustic shadowing from the overlying clavicle and rib is recognized, but one
small trial demonstrated improved infraclavicular cannulation and reduced mechanical complications using
ultrasound guidance compared with anatomic landmarks [37]. The principles of ultrasound in guiding venous
access are discussed in detail elsewhere. (See "Principles of ultrasound-guided venous access", section on
'Subclavian vein'.)
Venous confirmation An intraluminal position of the needle can be confirmed by observation of the
needle entering the vein with ultrasound-guided access coupled with a steady flow of dark blood into the
syringe. Bright red and high-pressure pulsatile bleeding are important but imperfect clues to arterial puncture
[39], which can occur, although less frequently, with ultrasound-guided access. Moreover, the absence of
these signs is not perfectly reliable for excluding inadvertent arterial puncture. Dark, nonpulsatile backflow of
suprasternal notch (figure 2and picture 3).
A lateral needle insertion (lateral to the midclavicular line) takes advantage of the thin anterior
convexity of the clavicle to facilitate a level coronal approach, which may improve safety if the vessel
can be reached by the cannulating needle [20,21,34].
!
The medial insertion point is along the inner third of the clavicle. The needle is directed cephalad
toward the suprasternal notch to penetrate the vessel at the broad confluence of the great veins. The
downside of this method is that medial positioning requires a steep approach beneath the thick medial
clavicle and passage through intervening soft tissue including the costoclavicular ligament.
!
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
7/36
blood may be seen with arterial puncture in the face of oxygen desaturation, hypotension, or needle
malposition. If there is any doubt, the needles location can be confirmed by pressure transduction. As an
alternative, a blood gas can be drawn from the accessed venous site and compared with an arterial sample;
however, blood gas analysis is more time consuming.
To transduce the blood pressure:
Steady, unimpeded blood return confirms intraluminal placement. The hub of the needle should be
stabilized, and the syringe carefully removed to avoid dislodgement from the vessel. The needle hub should
be covered between manipulations to avoid the entry of air. The patients can be encouraged to hum or
perform Valsalva maneuvers to augment central venous pressure, and hub exposure can be coordinated
with spontaneous exhalation to avoid aspiration of air.
If the subclavian artery is inadvertently punctured, the needle can be withdrawn and pressure applied over
the site for 5 to 10 minutes. Elevating the ipsilateral arm overhead may help to compress the vein. If
subclavian artery catheterization is confirmed, the catheter should be left in place and vascular consultation
obtained.
CATHETER PLACEMENT Most catheters and other central venous devices are placed using the
Seldinger method, which refers to the use of a guidewire placed into a vessel to provide a conduit for
intravascular device placement [14]. Seldinger first described the guidewire technique for arterial cannulation
in 1953 and it was subsequently adopted for venous access procedures [14].
Guidewire handling Once the subclavian vein has been successfully accessed, a guidewire should be
advanced through the needle or angiocatheter. Multiple types of wires are available to assist with venous
access procedures. The most commonly used wire for initial subclavian venous access is a flexible J-tip
guidewire, favored because it negotiates curvatures and minimizes vessel trauma during passage (picture
5).
The subclavian approach (particularly from the right side) has the highest rate of catheter malposition
compared with other access sites (jugular, femoral), which is due to errant positioning of the guidewire [1].
Head position alters the relationship of the subclavian vein and may affect guidewire placement. (See
'Positioning'above.)
The J-tip guidewire passage is influenced by the needle bevel and J-tip orientation. Orienting of the needle
bevel caudally for infraclavicular access and medially for supraclavicular access facilitates guidewire
passage from the subclavian vein into the superior vena cava [27]. Similarly, passage of guidewire with the
J-tip directed caudally improves correct placement [40].
Complaints of facial pain following guidewire placement often indicate passage into the internal jugular vein.
Manual occlusion of the ipsilateral jugular vein during guidewire placement may decrease malposition into it
Attach the needle directly to the pressure tubing system!
Alternatively, replace the needle over a guidewire with an appropriate length angiocatheter or 18-gauge
single-lumen transduction catheter (without any intervening dilation). Connect the transduction catheter
to a pressure line and transducer and evaluate the pressure and waveform tracings on the monitor.
Typical venous waveforms should be seen (figure 4).
!
If a pressure transduction system is not available, attach a short length of saline-filled intravenous
tubing to the needle and extended it vertically to measure the pressure, which should approximate
anticipated venous pressure and demonstrate respiratory variation.
!
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
8/36
[41].
The guidewire should always pass smoothly and easily thorough the needle, dilator, or catheter without
resistance. Methods to address resistance to guidewire advancement or withdrawal are discussed below.
To place the guidewire:
Tract dilation Central venous catheters are substantially larger caliber than the needle and guidewire
used for venous access. Dilation of the subcutaneous tissue tract is required for catheter insertion and is
accomplished by threading a single stiff tapered dilator or series of dilators over the wire to expand the
subcutaneous tissue and vein. The skin and fascia catheter tract should be dilated carefully with gentle
pressure. Only the soft tissue and vein wall need to be dilated. Overzealous efforts and guidewire kinking
(especially with stiff dilators) risk traumatic vein injury.
Many indwelling tunneled subclavian catheters are placed through a peel-away sheath. To place these
devices, a dilator-sheath combination is placed over the wire after the tract has been dilated. The dilator is
removed, and the catheter is placed through the sheath. Once the catheter is in place, the sheath is peeled
away from the catheter and discarded.
The dilator-sheath combination for large-bore tunneled catheters is stiff, and placement is facilitated with
fluoroscopy, which allows imaging of the tip of the dilator and sheath, ensuring that it is placed no further into
Position the tapered plastic introducer to straighten the distal J-tip (picture 6). The orientation of the
introducer needle bevel tip and the J-tip of the guidewire can help facilitate the direction of wirepassage.
!
Maintain the residual length of guidewire (50 cm standard length) under constant manual control to
maintain sterility and avoid its loss off the operating field.
!
Advance the guidewire only as far as needed to allow passage of the catheter over the wire.
Guidewires (and catheters) rarely require positioning more than 20 cm deep [5,42]. The atriocaval
junction averages 18 cm for right subclavian access, and 21 cm from the left subclavian [42]. These
average values vary depending upon stature. In an Asian study, average distances were slightly
shorter at 14 cm for the right subclavian vein and 17 cm for the left subclavian vein [ 43]. Advancing the
guidewire deeper risks intracardiac or inferior vena cava (IVC) wire placement with the potential for
cardiac arrhythmia, perforation, and snaring of other intravascular devices [44].
!
Never forcefully advance the guidewire, as this can kink and permanently deform the wire and risk
vessel injury. The guidewire should always pass smoothly and easily thorough the needle, dilator, or
catheter without resistance. Resistance to guidewire passage can be due to needle dislodgement,
compression of the guidewire against the vessel wall, or anatomic obstruction. Rotating the needle
and/or guidewire to reorient the bevel or J-tip may relieve impingement of the guidewire on the
posterior vessel wall.
!
If resistance persists, remove the guidewire and aspirate blood to confirm intraluminal needle position.
Reducing the angle of the needle against the skin may facilitate guidewire passage. Once the
guidewire is positioned, hold it firmly in place, and remove the needle.
!
Resistance during guidewire withdrawal can be managed by simultaneous removal of the needle and
indwelling wire. Continued resistance may indicate entrapment and warrants diagnostic radiography to
evaluate the wire appearance and position [45]. Withdrawing a kinked guidewire through the needle
can shear off the wire, allowing it to embolize [46].
!
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
9/36
the vein than is necessary. (See 'Equipment'above.)
To place the dilator:
Positioning the catheter After the subcutaneous tissues and vein have been dilated, the catheter is
placed over the wire and positioned (picture 8).
To place and position the catheter:
Ideal insertion distance varies by patient size and anatomic site. To minimize intracardiac placement, do not
insert catheters more than 20 cm from any upper body access site [ 5,42]. Initial insertion depth for most
adults should be 16 cm for right-sided subclavian catheters and 20 cm for left-sided subclavian vein
catheters [9]. Height-based formulas to determine insertion depth exist, but there are no well-controlled
studies supporting their use [48,49]. Rare case reports implicate intracardiac catheter tip placement as a
possible cause of cardiac tamponade [50,51].
Once the guidewire is in place, making a controlled 3 mm stab incision (#11 blade) in the skin at the
guidewire entry site will prevent the dilator from catching.
!
Thread the stiff tapered dilator over the wire, making certain the guidewire does not advance, and is
not pulled out at the skin exit site. The guidewire and dilator should neverbe advanced as a singleunit, to avoid venous injury. The wire should serve as an immobile monorail over which the dilator (or
catheter) is passed. Lateral traction of the skin helps to apply tension and avoid kinking the wire as the
dilator traverses tissue planes.
!
Hold the wire just above the dilator hub, grasp the dilator just above its tip and push it over the
guidewire with a firm corkscrew motion (picture 7). Mild resistance is normal. Excessive resistance may
represent an inadequate skin incision, a malpositioned guidewire, or guidewire or dilator deformation.
Kinking of the guidewire against the dilator is associated with vessel trauma and puncture [47].
!
As described above with needle placement, the opening of the dilator (or dilator/sheath combination)
should be covered, and the patient encouraged to Valsalva to prevent entry of air.
!
Advance the dilator only to the anticipated depth of the subclavian vein, notthe entire length of the
dilator. For the subclavian site, the dilator need only be advanced 3 to 5 cm into the vein depending
upon the thickness of the patients neck.
!
Withdraw the dilator while maintaining the guidewire position within the vessel. Apply direct pressure to
the exit site to maintain hemostasis prior to catheter insertion.
!
Steady traction on the skin during soft-tissue dilatation helps prevent wire kinking. Rotating the dilator
during advancement often facilitates tract dilatation (round dilators only). If resistance is met, it may be
related to a kink in the wire which can be remedied by advancing the wire deeper or withdrawing the
kink into the dilator. Overzealous efforts and guidewire kinking (especially with stiff dilators) risk
traumatic vein injury.
!
Thread the guidewire back through the end-hole of the catheter until it emerges from the distal port and
advance the catheter over the wire into the vessel (picture 9).
!
Resistance to catheter advancement through the soft tissue tract can be overcome by simultaneously
advancing the catheter and wire together for the first 2 to 3 cm. Advancing further risks subclavian vein
injury if the wire is inadvertently kinked. Withdrawal of the catheter and redilation of the tract is
preferred.
!
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
10/36
In contrast to right-sided catheters, catheters inserted from the left negotiate the angulation of the
brachiocephalic vein to enter the superior vena cava. For large bore catheters used for hemodialysis or
oncology, advancement under fluoroscopic guidance helps minimize the risk of central venous laceration.
The risk of complications is related to the angle of catheter impingement on the superior vena cava [ 9]. From
the left, catheters positioned above the pericardial reflection often abut the weak lateral wall of the superior
vena cava and risk erosion and perforation [52-55]. As such, left-sided catheters should be inserted to an
appropriate length to lie parallel in the long axis of the superior vena cava. This may require catheter tip
placement in the upper right atrium [56-58]. It is also important to realize that catheter tips are not fixed and
migrate 2 to 3 cm with head and arm movement and change in body position [ 59].
Catheter flushing and fixation Once the catheter is in place, the proper function of the catheter should
be confirmed by aspirating blood and subsequently flushing each port with saline (picture 10) [9,60].
The catheter can be secured into place by suturing (2-0 or 3-0 nylon or silk) it to the skin ( picture 11). If more
than 2 cm of catheter remain exposed, it can be sutured to the skin or to a separate catheter anchor that is
often included in the catheter kit. A transparent dressing should be placed over the catheter exit site to
protect it from contamination.
CONFIRMATION OF SUBCLAVIAN CATHETER POSITION Confirmation of subclavian catheter tip
location can use one or more of the following methods: chest radiography, fluoroscopy, and transesophageal
echocardiography (typically intraoperative setting) [61-67]. Chest radiography and fluoroscopy are the most
commonly used methods. In general, catheters function well with the tip situated in any major vein. However,
suboptimal tip position may be related to delayed complications.
Following subclavian access, the position and course of the catheter and tip should be confirmed prior to its
use. When using fluoroscopy for placement, a routine chest radiograph is unnecessary unless clinical
suspicion of pneumothorax/hemothorax is high. If fluoroscopy has not been used, we obtain a postprocedure
chest radiograph in non-life-threatening situations. If immediate catheter use is needed, venous positioning
(but not tip position) can be confirmed with transduction of the central venous pressure, display of the central
venous waveform or via ultrasound. Bedside ultrasound is under investigation as an alternative modality to
confirm catheter placement and detect pneumothorax [68].
The optimal catheter tip position is controversial, and controlled studies are lacking. The distal tip of jugular
catheters should lie in the lower superior vena cava [2,5]. To minimize the likelihood of cardiac
complications, some guidelines recommend catheter tip position outside the right atrium and above the
pericardial reflection. The right superior heart border on chest radiography is not a reliable determinant of
right atrial position [69]. The carina and right tracheobronchial angle represent reliable landmarks for the
pericardial reflection and right-sided catheters should generally be positioned above this point [69-71].
Malposition is common with subclavian access and is often related to an initially misplaced guidewire [1]. If a
catheter is malpositioned within the venous system, it can be used for fluid administration under emergency
circumstances, but should be re-positioned as soon as feasible. In contrast, inadvertent placement of a
catheter into the subclavian artery mandates surgical consultation [28].
If a subclavian catheter tip is positioned too deeply, it can be repositioned at the bedside using sterile
technique. Remove the sutures, withdraw the catheter, and re-suture the catheter into place.
!
If a catheter is not in far enough or is misplaced into the contralateral subclavian or internal jugular
vein, it will need to be replaced over a guidewire under sterile conditions. The portion of a catheter left
out of the body is unsterile and should never be advanced into the patient, not even if it is under a
!
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
0 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
11/36
CATHETER MANAGEMENT The management of central catheters is discussed elsewhere. (See
"Prevention of intravascular catheter-related infections", section on 'Site care'and "Prevention of
intravascular catheter-related infections", section on 'Catheter care'.)
COMPLICATIONS The complications related to subclavian venous access are discussed separately.
(See "Complications of central venous catheters and their prevention".)
SUMMARY AND RECOMMENDATIONS
Use of UpToDate is subject to the Subscription and License Agreement.
REFERENCES
Ruesch S, Walder B, Tramr MR. Complications of central venous catheters: internal jugular versus
subclavian access--a systematic review. Crit Care Med 2002; 30:454.
1.
McGee DC, Gould MK. Preventing complications of central venous catheterization. N Engl J Med
2003; 348:1123.
2.
sterile dressing.
Central catheters provide dependable intravenous access and enable hemodynamic monitoring and
blood sampling. The subclavian veins are reliable access points for temporary and permanent
cannulation, and device introduction. Several anatomical approaches to the subclavian vein are
described, and the method should be individualized to the patients clinical circumstances. (See
'Introduction'above.)
!
For subclavian access, the patient is placed supine or in Trendelenburg position with the arms placed
to the side (adducted) with a neutral to lower shoulder positioning. The natural tendency for the
shoulders to assume a cephalad orientation during Trendelenburg tilt should be countered by gentle
caudal arm traction performed by a bedside assistant. (See 'Positioning'above.)
!
Left-sided subclavian access is associated with lower rates of catheter malposition and vessel trauma
is also preferred when immediate cardiac access is needed (eg, temporary transvenous pacer
placement, pulmonary artery catheter) since the guidewire and catheter are more easily directed into
the superior vena cava and right heart.
!
Subclavian artery puncture during vein localization is not uncommon and can be managed by
withdrawing the needle and applying pressure over the site for 5 to 10 minutes. Elevation of the
ipsilateral arm overhead may help to compress the vein. If arterial catheterization is confirmed, the
catheter should be left in place and a vascular consult obtained. (See 'Venous confirmation'above.)
!
A postprocedure chest radiograph is typically performed to confirm catheter position and excludepneumothorax. The distal tip of subclavian catheters should lie in the lower superior vena cava. (See
'Confirmation of subclavian catheter position'above.)
!
If a subclavian catheter is placed too deeply, it can be withdrawn at the bedside using sterile
techniques. If the catheter is not placed deeply enough or is malpositioned, the catheter should be
replaced over a guidewire under sterile conditions. The portion of a catheter left out of the body is
unsterile and should never be advanced into the patient. (See 'Confirmation of subclavian catheter
position'above.)
!
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
1 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
12/36
AUBANIAC R. [Subclavian intravenous injection; advantages and technic]. Presse Med 1952;
60:1456.
3.
Fisher NC, Mutimer DJ. Central venous cannulation in patients with liver disease and coagulopathy--a
prospective audit. Intensive Care Med 1999; 25:481.
4.
McGee WT, Moriarty KP. Accurate placement of central venous catheters using a 16-cm catheter. J
Intensive Care Med 1996; 11:19.
5.
Doerfler ME, Kaufman B, Goldenberg AS. Central venous catheter placement in patients with
disorders of hemostasis. Chest 1996; 110:185.
6.
Mumtaz H, Williams V, Hauer-Jensen M, et al. Central venous catheter placement in patients with
disorders of hemostasis. Am J Surg 2000; 180:503.
7.
Foster PF, Moore LR, Sankary HN, et al. Central venous catheterization in patients with coagulopathy.
Arch Surg 1992; 127:273.
8.
Polderman KH, Girbes AJ. Central venous catheter use. Part 1: mechanical complications. Intensive
Care Med 2002; 28:1.
9.
Mansfield PF, Hohn DC, Fornage BD, et al. Complications and failures of subclavian-vein
catheterization. N Engl J Med 1994; 331:1735.
10.
Timsit JF. Central venous access in intensive care unit patients: is the subclavian vein the royal route?
Intensive Care Med 2002; 28:1006.
11.
Schillinger F, Schillinger D, Montagnac R, Milcent T. Post catheterisation vein stenosis in
haemodialysis: comparative angiographic study of 50 subclavian and 50 internal jugular accesses.
Nephrol Dial Transplant 1991; 6:722.
12.
The clinical anatomy of several invasive procedures. American Association of Clinical Anatomists,
Educational Affairs Committee. Clin Anat 1999; 12:43.
13.
SELDINGER SI. Catheter replacement of the needle in percutaneous arteriography; a new technique.
Acta radiol 1953; 39:368.
14.
Land RE. Anatomic relationships of the right subclavian vein. A radiologic study pertinent to
percutaneous subclavian venous catheterization. Arch Surg 1971; 102:178.
15.
Fortune JB, Feustel P. Effect of patient position on size and location of the subclavian vein for
percutaneous puncture. Arch Surg 2003; 138:996.
16.
Ely EW, Hite RD, Baker AM, et al. Venous air embolism from central venous catheterization: a need for
increased physician awareness. Crit Care Med 1999; 27:2113.
17.
Mirski MA, Lele AV, Fitzsimmons L, Toung TJ. Diagnosis and treatment of vascular air embolism.
Anesthesiology 2007; 106:164.
18.
Sunder-Plassmann G, Locker GJ, Muhm M, et al. Central venous catheterization in a patient in the
prone position. Crit Care Med 1997; 25:1439.
19.
Tan BK, Hong SW, Huang MH, Lee ST. Anatomic basis of safe percutaneous subclavian venouscatheterization. J Trauma 2000; 48:82.20.
Kitagawa N, Oda M, Totoki T, et al. Proper shoulder position for subclavian venipuncture: a prospective
randomized clinical trial and anatomical perspectives using multislice computed tomography.
Anesthesiology 2004; 101:1306.
21.
Land RE. The relationship of the left subclavian vein to the clavicle: practical considerations pertinent
to the percutaneous catheterization of the subclavian vein. J Thorac Cardiovasc Surg 1972; 63:564.
22.
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
2 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
13/36
Jesseph JM, Conces DJ Jr, Augustyn GT. Patient positioning for subclavian vein catheterization. Arch
Surg 1987; 122:1207.
23.
Jung CW, Bahk JH, Kim MW, et al. Head position for facilitating the superior vena caval placement of
catheters during right subclavian approach in children. Crit Care Med 2002; 30:297.
24.
Sanchez R, Halck S, Walther-Larsen S, Heslet L. Misplacement of subclavian venous catheters:
importance of head position and choice of puncture site. Br J Anaesth 1990; 64:632.
25.
Boyd R, Saxe A, Phillips E. Effect of patient position upon success in placing central venous catheters.
Am J Surg 1996; 172:380.
26.
Nevarre DR, Domingo OH. Supraclavicular approach to subclavian catheterization: review of the
literature and results of 178 attempts by the same operator. J Trauma 1997; 42:305.
27.
Guilbert MC, Elkouri S, Bracco D, et al. Arterial trauma during central venous catheter insertion: Case
series, review and proposed algorithm. J Vasc Surg 2008; 48:918.
28.
Sznajder JI, Zveibil FR, Bitterman H, et al. Central vein catheterization. Failure and complication rates
by three percutaneous approaches. Arch Intern Med 1986; 146:259.
29.
Lefrant JY, Muller L, De La Coussaye JE, et al. Risk factors of failure and immediate complication of
subclavian vein catheterization in critically ill patients. Intensive Care Med 2002; 28:1036.
30.
Orihashi K, Imai K, Sato K, et al. Extrathoracic subclavian venipuncture under ultrasound guidance.
Circ J 2005; 69:1111.
31.
Tripathi M, Tripathi M. Subclavian vein cannulation: an approach with definite landmarks. Ann Thorac
Surg 1996; 61:238.
32.
Albuquerque Jnior FC, Vasconcelos PR. Technical aspects of central venous catheterization. Curr
Opin Clin Nutr Metab Care 1998; 1:297.
33.
Tofield JJ. A safer technique of percutaneous catheterization of the subclavian vein. Surg Gynecol
Obstet 1969; 128:1069.
34.
Kilbourne MJ, Bochicchio GV, Scalea T, Xiao Y. Avoiding common technical errors in subclavian
central venous catheter placement. J Am Coll Surg 2009; 208:104.
35.
Jung CW, Seo JH, Lee W, Bahk JH. A novel supraclavicular approach to the right subclavian vein
based on three-dimensional computed tomography. Anesth Analg 2007; 105:200.
36.
Fragou M, Gravvanis A, Dimitriou V, et al. Real-time ultrasound-guided subclavian vein cannulation
versus the landmark method in critical care patients: a prospective randomized study. Crit Care Med
2011; 39:1607.
37.
O'Leary R, Ahmed SM, McLure H, et al. Ultrasound-guided infraclavicular axillary vein cannulation: a
useful alternative to the internal jugular vein. Br J Anaesth 2012; 109:762.
38.
Ezaru CS, Mangione MP, Oravitz TM, et al. Eliminating arterial injury during central venous
catheterization using manometry. Anesth Analg 2009; 109:130.
39.
Tripathi M, Dubey PK, Ambesh SP. Direction of the J-tip of the guidewire, in seldinger technique, is asignificant factor in misplacement of subclavian vein catheter: a randomized, controlled study. Anesth
Analg 2005; 100:21.
40.
Ambesh SP, Dubey PK, Matreja P, et al. Manual occlusion of the internal jugular vein during
subclavian vein catheterization: a maneuver to prevent misplacement of catheter into internal jugular
vein. Anesthesiology 2002; 97:528.
41.
Andrews RT, Bova DA, Venbrux AC. How much guidewire is too much? Direct measurement of the42.
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
3 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
14/36
distance from subclavian and internal jugular vein access sites to the superior vena cava-atrial junction
during central venous catheter placement. Crit Care Med 2000; 28:138.
Kim WY, Lee CW, Sohn CH, et al. Optimal insertion depth of central venous catheters--is a formula
required? A prospective cohort study. Injury 2012; 43:38.
43.
Stuart RK, Shikora SA, Akerman P, et al. Incidence of arrhythmia with central venous catheter
insertion and exchange. JPEN J Parenter Enteral Nutr 1990; 14:152.
44.
Wang HE, Sweeney TA. Subclavian central venous catheterization complicated by guidewire loopingand entrapment. J Emerg Med 1999; 17:721.
45.
Propp DA, Cline D, Hennenfent BR. Catheter embolism. J Emerg Med 1988; 6:17.46.
Robinson JF, Robinson WA, Cohn A, et al. Perforation of the great vessels during central venous line
placement. Arch Intern Med 1995; 155:1225.
47.
Czepizak CA, O'Callaghan JM, Venus B. Evaluation of formulas for optimal positioning of central
venous catheters. Chest 1995; 107:1662.
48.
Peres PW. Positioning central venous catheters--a prospective survey. Anaesth Intensive Care 1990;
18:536.
49.
Booth SA, Norton B, Mulvey DA. Central venous catheterization and fatal cardiac tamponade. Br J
Anaesth 2001; 87:298.
50.
Collier PE, Blocker SH, Graff DM, Doyle P. Cardiac tamponade from central venous catheters. Am J
Surg 1998; 176:212.
51.
Tocino IM, Watanabe A. Impending catheter perforation of superior vena cava: radiographic
recognition. AJR Am J Roentgenol 1986; 146:487.
52.
Dailey RH. Late vascular perforations by CVP catheter tips. J Emerg Med 1988; 6:137.53.
Duntley P, Siever J, Korwes ML, et al. Vascular erosion by central venous catheters. Clinical features
and outcome. Chest 1992; 101:1633.
54.
Mukau L, Talamini MA, Sitzmann JV. Risk factors for central venous catheter-related vascular
erosions. JPEN J Parenter Enteral Nutr 1991; 15:513.
55.
Fletcher SJ, Bodenham AR. Safe placement of central venous catheters: where should the tip of the
catheter lie? Br J Anaesth 2000; 85:188.
56.
Vesely TM. Central venous catheter tip position: a continuing controversy. J Vasc Interv Radiol 2003;
14:527.
57.
Stonelake PA, Bodenham AR. The carina as a radiological landmark for central venous catheter tip
position. Br J Anaesth 2006; 96:335.
58.
Kowalski CM, Kaufman JA, Rivitz SM, et al. Migration of central venous catheters: implications for
initial catheter tip positioning. J Vasc Interv Radiol 1997; 8:443.
59.
Chalkiadis GA, Goucke CR. Depth of central venous catheter insertion in adults: an audit and
assessment of a technique to improve tip position. Anaesth Intensive Care 1998; 26:61.
60.
Gillman LM, Blaivas M, Lord J, et al. Ultrasound confirmation of guidewire position may eliminate
accidental arterial dilatation during central venous cannulation. Scand J Trauma Resusc Emerg Med
2010; 18:39.
61.
Gu X, Paulsen W, Tisnado J, He Y, Li Z, Nixon JV: Malposition of a central venous catheter in the right
main pulmonary artery detected by transesophageal echocardiography. J Am Soc Echocardiogr 2009;
22:1420
62.
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
4 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
15/36
Lucey B, Varghese JC, Haslam P, Lee MJ. Routine chest radiographs after central line insertion:
mandatory postprocedural evaluation or unnecessary waste of resources? Cardiovasc Intervent Radiol
1999; 22:381.
63.
Gebhard RE, Szmuk P, Pivalizza EG, et al. The accuracy of electrocardiogram-controlled central line
placement. Anesth Analg 2007; 104:65.
64.
Abood GJ, Davis KA, Esposito TJ, et al. Comparison of routine chest radiograph versus clinician
judgment to determine adequate central line placement in critically ill patients. J Trauma 2007; 63:50.
65.
Wirsing M, Schummer C, Neumann R, et al. Is traditional reading of the bedside chest radiograph
appropriate to detect intraatrial central venous catheter position? Chest 2008; 134:527.
66.
Francis KR, Picard DL, Fajardo MA, Pizzi WF. Avoiding complications and decreasing costs of central
venous catheter placement utilizing electrocardiographic guidance. Surg Gynecol Obstet 1992;
175:208.
67.
Vezzani A, Brusasco C, Palermo S, et al. Ultrasound localization of central vein catheter and detection
of postprocedural pneumothorax: an alternative to chest radiography. Crit Care Med 2010; 38:533.
68.
Aslamy Z, Dewald CL, Heffner JE. MRI of central venous anatomy: implications for central venous
catheter insertion. Chest 1998; 114:820.
69.
Schuster M, Nave H, Piepenbrock S, et al. The carina as a landmark in central venous catheterplacement. Br J Anaesth 2000; 85:192.
70.
Albrecht K, Nave H, Breitmeier D, et al. Applied anatomy of the superior vena cava-the carina as a
landmark to guide central venous catheter placement. Br J Anaesth 2004; 92:75.
71.
Topic 15673 Version 6.0
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
5 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
16/36
GRAPHICS
Advantages and disadvantages of central vein approaches
Approach Advantages Disadvantages
External
jugular
Superficial vessel that is often
visible
Coagulopathy not prohibitive
Minimal risk of pneumothorax
(especially with US guidance)
Head-of-table access
Prominent in elderly patients
Rapid venous access
Not ideal for prolonged venous access
Poor landmarks in obese patients
High rate of malposition
Catheter may be difficult to thread
Internal
jugular
Minimal risk of pneumothorax
(especially with US guidance)
Head-of-table access
Procedure-related bleeding
amenable to direct pressure
Lower failure rate with novice
operator
Excellent target using US
guidance
Not ideal for prolonged access
Risk of carotid artery puncture
Uncomfortable
Dressings and catheter difficult to
maintain
Thoracic duct injury possible on left
Poor landmarks in obese/edematous
patients
Potential access and maintenance issues
with concomitant tracheostomy
Vein prone to collapse with hypovolemia
Difficult access during emergencies when
airway control being established
Subclavian Easier to maintain dressings
More comfortable for patient
Better landmarks in obese
patients
Accessible when airway control is
being established
Increased risk of pneumothorax
Procedure-related bleeding less
amenable to direct pressure
Decreased success rate with
inexperience
Longer path from skin to vessel
Catheter malposition more common
(especially right SCV)
Interference with chest compressions
Femoral Rapid access with high success
rate
Does not interfere with CPR
Does not interfere with
Delayed circulation of drugs during CPR
Prevents patient mobilization
Difficult to keep site sterile
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
6 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
17/36
intubation
No risk of pneumothorax
Trendelenburg position not
necessary during insertion
Difficult for PA catheter insertion
Increased risk of iliofemoral thrombosis
US: ultrasound; SCV: subclavian vein; CPR: cardiopulmonary resuscitation; PA: pulmonary artery.
With permission from: Factor P, Sznajder JI. Vascular cannulation. In: Principles of Critical Care,
Hall JB, Schmidt GA, Wood LDH (Eds), McGraw-Hill, New York, 1992. Copyright 1992 McGraw-Hill.
Graphic 71716 Version 6.0
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
7 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
18/36
External landmarks for the infraclavicular
approach to the subclavian vein
UpToDate acknowledges the invaluable assistance of the University of
Massacusetts Medical School, Department of Anatomy and Department of
Emergency Medicine, including Thomas Ellis, MD and Jean Marcelin, MD, for
the photographs of central venous catheter placement.
Graphic 62106 Version 7.0
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
8 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
19/36
Anatomy of the subclavian and internal jugular veins
Graphic 74801 Version 2.0
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
9 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
20/36
Equipment for central venous cannulation
2 percent chlorhexidine skin preparation solution
Sterile gown, gloves, face shield and cap
Sterile gauze pads: 4" x 4"
Sterile drapes
1 percent lidocaine; 5cc
25 Ga. needle with 3cc lock-tip syringe
Seeker needle: 3.5 cm 22 Ga. needle with 5cc slip-tip syringe
Introducer needle: 6 cm 18 Ga. large bore needle with 5cc slip-tip syringe
J-tip guidewire
Transduction catheter: 6 cm 18 Ga. catheter
Transduction tubing
Tissue dilator
Sterile catheter flush solution
Sheath
Catheter or other device (eg, port, pulmonary catheter)
Sterile sleeve for the catheter
2-0 silk sutures
Sterile dressing
Equipment needed for central venous cannulation, in order of use during procedure. For
certain procedures (eg, pulmonary artery catheter placement) additional supplies (drapes,
gowns) or additional catheter sets (introducer, sheath, pulmonary catheter, other venous
device) may be needed.
Graphic 54646 Version 4.0
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
0 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
21/36
Technique of central venous catheterization
Identify vessel or pertinent landmark
Prepare the site by scrubbing widely with antiseptic solution
Drape the site with sterile towels and surgical drapes
Infiltrate the skin with 1 percent lidocaine
Cannulate the vein using the introducer needle
Confirm position of needle by easy aspiration of venous blood; if doubt exists regarding
venous versus arterial cannulation, transduction of pressures or blood gas analysis is
recommended
Remove syringe from needle hub
Insert J-tipped guidewire through the needle into the vein and gently advance the wire;
neverforce the wire
Remove the needle while maintaining control of the guidewire
Make a small skin nick contiguous with the wire using an upward-facing scalpel blade
Advance the dilator over the wire using a twisting motion; always hold the guidewire
Withdraw dilator while guidewire is stabilized
Thread the catheter over the guidewire; always hold the guidewire
Stabilize the catheter and remove the guidewire
Evaluate ease of aspiration and flushing from each port of catheter
Suture the catheter securely, dress site with sterile technique and topical antiseptic ointment
Graphic 68138 Version 4.0
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
1 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
22/36
Infraclavicular approach to the subclavian vein
The midpoint approach to cannulation of the subclavian vein is most common. Insert
the needle 2 to 3 cm inferior to the midpoint of the clavicle. Advance the needle
aiming just deep to the suprasternal notch, keeping the needle parallel to the ground.
Graphic 82344 Version 3.0
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
2 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
23/36
Supraclavicular approach to the subclavian vein
The supraclavicular approach allows ready access to the subclavian vein. The point of
needle entry lies 1 cm posterior to the sternocleidomastoid and 1 cm superior to the
clavicle. Be sure the angle of the needle is depressed 10 to 15 degrees below the
coronal plane (ie, needle tip aimed upwards). Advance the needle behind the medial
clavicle along a trajectory directed just below the contralateral nipple.
Graphic 55896 Version 3.0
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
3 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
24/36
External landmarks for the supraclavicular
approach to the subclavian vein
UpToDate acknowledges the invaluable assistance of the University of
Massacusetts Medical School, Department of Anatomy and Department of
Emergency Medicine, including Thomas Ellis, MD and Jean Marcelin, MD, for
the photographs of central venous catheter placement.
Graphic 81595 Version 5.0
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
4 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
25/36
Finder needle for central line placement
This photograph depicts the use of a finder needle to locate the internal
jugular vein.
UpToDate acknowledges the invaluable assistance of the University of
Massacusetts Medical School, Department of Anatomy and Department of
Emergency Medicine, including Thomas Ellis, MD and Jean Marcelin, MD, for
the photographs of central venous catheter placement.
Graphic 55560 Version 2.0
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
5 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
26/36
Needle insertion for the middle approach to
subclavian vein
In the middle approach to the subclavian vein, the needle is inserted 2
to 3 cm inferior to the midpoint of the clavicle. The needle is advanced
while aiming for a point just deep to the suprasternal notch.
UpToDate acknowledges the invaluable assistance of the University of
Massacusetts Medical School, Department of Anatomy and Department of
Emergency Medicine, including Thomas Ellis, MD and Jean Marcelin, MD, for
the photographs of central venous catheter placement.
Graphic 73933 Version 2.0
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
6 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
27/36
Needle insertion for central venous catheter
placement using the supraclavicular approach
When using the supraclavicular approach for central venous catheter
placement, it is important that the needle be oriented properly. It
should lie 10 to 15 degrees below the coronal plane and oriented to
bisect the angle between the clavicle and the sternocleidomastoid. The
needle should not be inserted too deeply; the subclavian vein generally
lies 1 to 1.5 cm deep to the insertion point.
UpToDate acknowledges the invaluable assistance of the University of
Massacusetts Medical School, Department of Anatomy and Department of
Emergency Medicine, including Thomas Ellis, MD and Jean Marcelin, MD, for
the photographs of central venous catheter placement.
Graphic 53255 Version 2.0
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
7 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
28/36
Right atrial pressure tracing
This schematic diagram shows the different components of the right
atrial pressure tracing. A simultaneous ECG is shown to demonstrate the
timing of the different components.
Redrawn from Gore, JM, Alper, JS, Benotti, JR, et al. Handbook of
hemodynamic monitoring, 1st ed, Boston, Little Brown & Co, 1985.
Graphic 58343 Version 1.0
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
8 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
29/36
Guidewire with J tip for central venous catheter
placement
Proper orientation of the J tip towards the superior vena cava helps
prevent improper placement of central venous catheters. For subclavian
catheters, the J tip is oriented caudally; for internal jugular catheters,the J tip is oriented medially.
UpToDate acknowledges the invaluable assistance of the University of
Massacusetts Medical School, Department of Anatomy and Department of
Emergency Medicine, including Thomas Ellis, MD and Jean Marcelin, MD, for
the photographs of central venous catheter placement.
Graphic 82419 Version 2.0
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
9 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
30/36
Placement of a guidewire for a central venous
catheter
UpToDate acknowledges the invaluable assistance of the University of
Massacusetts Medical School, Department of Anatomy and Department of
Emergency Medicine, including Thomas Ellis, MD and Jean Marcelin, MD, for
the photographs of central venous catheter placement.
Graphic 72306 Version 2.0
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
0 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
31/36
Insertion of soft tissue dilator for central venous
catheter placement
The soft tissue dilator is advanced over the guidewire using a corkscrew
motion. Mild resistance is normal. The dilator does NOT need to be
advanced its entire length, but only to the anticipated depth of the
vessel.
UpToDate acknowledges the invaluable assistance of the University of
Massacusetts Medical School, Department of Anatomy and Department of
Emergency Medicine, including Thomas Ellis, MD and Jean Marcelin, MD, for
the photographs of central venous catheter placement.
Graphic 77656 Version 2.0
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
1 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
32/36
Central venous catheter being threaded onto
guidewire
UpToDate acknowledges the invaluable assistance of the University of
Massacusetts Medical School, Department of Anatomy and Department of
Emergency Medicine, including Thomas Ellis, MD and Jean Marcelin, MD, for
the photographs of central venous catheter placement.
Graphic 70002 Version 2.0
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
2 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
33/36
Central venous catheter being advanced over
guidewire
As the catheter is advanced, the guidewire emerges from the distal port.
Control should be maintained of both the catheter and the guidewire
throughout this process.
UpToDate acknowledges the invaluable assistance of the University of
Massacusetts Medical School, Department of Anatomy and Department of
Emergency Medicine, including Thomas Ellis, MD and Jean Marcelin, MD, for
the photographs of central venous catheter placement.
Graphic 51314 Version 3.0
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
3 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
34/36
Aspiration following central venous catheter
placement
Following placement of the catheter, blood should be aspirated from
each port and then each port should be flushed.
UpToDate acknowledges the invaluable assistance of the University of
Massacusetts Medical School, Department of Anatomy and Department of
Emergency Medicine, including Thomas Ellis, MD and Jean Marcelin, MD, for
the photographs of central venous catheter placement.
Graphic 56646 Version 4.0
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
4 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
35/36
Central venous catheter sutured in place
When suturing central venous catheters in place, avoid knots that place
excessive pressure on the skin, which can lead to skin necrosis.
UpToDate acknowledges the invaluable assistance of the University ofMassacusetts Medical School, Department of Anatomy and Department of
Emergency Medicine, including Thomas Ellis, MD and Jean Marcelin, MD, for
the photographs of central venous catheter placement.
Graphic 58552 Version 2.0
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/
5 of 36 6/21/15, 6:57
-
7/25/2019 Placement of Subclavian Venous Catheters
36/36
Disclosures:Alan C Heffner, MD Speaker's Bureau: Edwards Lifesciences [Hemodynamic monitoring, shock, sepsis
(Hemodynamic monitoring devices)]. Consultant/Advisory Boards: Edwards Lifesciences [Hemodynamic monitoring, shock, sepsis
(Hemodynamic monitoring devices)]. Mark P Androes, MD Nothing to disclose. Allan B Wolfson, MD Nothing to disclose. John F
Eidt, MD Nothing to disclose. Joseph L Mills, Sr, MD Grant/Research/Clinical Trial Support: NIH Institute of Aging (abdominal aortic
aneurysm study). Consultant/Advisory Boards: AnGes (critical limb ischemia); Cesca Therapeutics (critical limb ischemia). Speaker:
Gore (bypass seminar [Polytetrafluoroethylene]). Other financial interests: Elsevier (vascular surgery textbooks). Kathryn A Collins,
MD, PhD, FACS Nothing to disclose.
Contributor disclosures are reviewed for conflicts of interest by the editorial group. When found, these are addressed by vettingthrough a multi-level review process, and through requirements for references to be provided to support the content. Appropriately
referenced content is required of all authors and must conform to UpToDate standards of evidence.
Conflict of interest policy
Disclosures
Placement of subclavian venous catheters http://www.uptodate.com.ezproxy.pcom.edu:2048/contents/