Perioperative%20%20%20%20%20%20%20%20 arrhythmias
-
Upload
drchiranji-khedia -
Category
Health & Medicine
-
view
184 -
download
0
Transcript of Perioperative%20%20%20%20%20%20%20%20 arrhythmias

PERIOPERATIVE ARRHYTHMIAS
Guided By- Dr. Vijeta khandelwal
Presented By-Dr. C.L. khedia

• Definition: Arrhythmia is defined as "Abnormality of cardiac rate, rhythm or conduction.
• Cardiac arrhythmias are the most frequent perioperative cardiovascular abnormalities in patients undergoing both cardiac and non-cardiac surgery.
• The occurrence of arrhythmias have been reported in 70% of patients subjected to general anaesthesia for various surgical procedures.

Mechanisms of Arrhythmia
Production• Re-entry (refractory tissue reactivated due to conduction
block, causes abnormal continuous circuit. eg accessory pathways linking atria and ventricles in Wolff-Parkinson-White syndrome)
• Injury or damage (pathology) to the cardiac conduction systems
• Abnormal pacemaker activity/ automaticity in non-conducting/conducting tissue (eg. ischaemia)
• Delayed after-depolarisation (automatic depolarisation of cardiac cell triggers ectopic beats, can be caused by drugs eg digoxin)

Contributing factors and causes1. Patient related factors-• preexisting cardiac disease• central nervous system disease• Old age2.Anaesthesia related factors• Tracheal intubation• general anaesthetics• regional anaesthesia• Electrolyte imbalance and abnormal arterial
blood gases• Central venous cannulation

Reversible cause of arrhythmia
• Hypoxemia
• Hypercarbia
• Hypotension
• Acidosis
• Light anesthesia
• Proarrhythemic drugs
• Cardiac ischemia
• Electrolyte imbalance
• Hypothermia
• Mechanical irritation:
PAC, Chest tube

Classification of Cardiac
Arrhythmias
• Heart rate (increased/decreased)
• Heart rhythm (regular/irregular)
• Site of origin (supraventricular / ventricular)
• Complexes on ECG (narrow/broad)

• Bradyarrhythmias
• Sinus bradycardia
• Sinoatrial block
• Sinus arrest
• Atroventricular block
• Bundle branch block
• Tachyarrhythmias
• Supraventricular arrhythmias
• Ventricular arrhythmias

Supraventricular tachyarrhythmias
• Sinus tachycardia
• Prematue atrial contractions (PACs)
• Atrial tachycardia
• Atrial flutter/fibrillation (AF)
• Atrioventricular nodal reentrant tachycardia (AVNRT)
• Atrioventricular reentrant tachycardia (AVRT)
Ventricular tachyarrhythmias
• Premature ventricular contractions (PVCs)
• Ventricular tachycardia (VT)
• Monomorphic vs Polymorphic VT
• Ventricular flutter/fibrillation (VF)

Anaesthetic considerations
• All patients undergoing anaesthesia and surgery should have ECG monitoring.
• Lead II and V 5 are superior for arrhythmia detection and diagnosis before the appearance of physical signs.


Waveform Analysis
– For each strip it is necessary to go through steps
to correctly identify the rhythm
1. Is there a P-wave for every QRS?
• P-waves are upright and uniform
• One P-wave preceding each QRS
2. Is the rhythm regular?
• Verify by assessing R-R interval
• Confirm by assessing P-P interval
3. What is the rate?
• Count the number of beats occuring in one minute
• Counting the p-waves will give the atrial rate
• Counting QRS will give ventricular rate

• Normal
– Heart rate = 60 – 100 bpm
– PR interval = 0.12 – 0.20 sec
– QRS interval <0.12
– SA Node discharge = 60 – 100 / min
– AV Node discharge = 40 – 60 min
– Ventricular Tissue discharge = 20 – 40 min

• Cardiac cycle
– P wave = atrial depolarization
– PR interval = pause between atrial and
ventricular depolarization
– QRS = ventricular depolarization
– T wave = ventricular depolarization

Normal Sinus Rhythm
Heart
RateRhythm P Wave
PR Interval
(sec.)
QRS
(Sec.)
60 -
100Regular
Before each QRS,
Identical.12 - .20 <.12
Sinus Rhythms

• Normal Sinus Rhythm
– Sinus Node is the primary pacemaker
– One upright uniform p-wave for every QRS
– Rhythm is regular
– Rate is between 60-100 beats per minute
Sinus Rhythms

Sinus Bradycardia
Heart
RateRhythm P Wave
PR Interval
(sec.)
QRS
(Sec.)
<60 RegularBefore each QRS,
Identical.12 - .20 <.12
Sinus Rhythms

• Sinus Bradycardia
– One upright uniform p-wave for every QRS
– Rhythm is regular
– Rate less than 60 beats per minute
• SA node firing slower than normal
• Normal for many individuals
• Identify what is normal heart rate for patient
Sinus Rhythms

Perioperative causes of Sinus Bradycardia-:
1. Vagal stimulation- Oculocardiac reflex, Celiac plexus stimulation(traction on mesentry), laryngoscopy, Abdominal insufflation, Nausea and ECT
2. Drugs- Beat blocker, Cal channel blocker, opioids(fentanyl/sufentanyl)
3. Succinylcholine 4.Hypothermia
5. Hypothyroidism 6. Atheletic heart syndrome
7. SA node disease or ischemia

Perioperative T/T-
- In asymptomatic pt no t/t requires
- In Mildly symptomatic pts, underlying factors should be eleminated
- In severly symptomatic pts, those with chest pain or syncope, immediate transcutaneous/transvenous pacing is required.
- Atropine 0.5 mg Iv every 3-5 min(max 3mg) may be given. It should be noted dose of atropine (<0.5mg) can cause further slowing of HR.
- An epinephrine or dopamine infusion may be titrated while awaiting cardiac pacing.

•
Sinus Tachycardia
Heart
RateRhythm P Wave
PR Interval
(sec.)
QRS
(Sec.)
>100 RegularBefore each QRS,
Identical.12 - .20 <.12
Sinus Rhythms

• Sinus Tachycardia
– One upright uniform p-wave for every QRS
– Rhythm is regular
– Rate is greater than 100 beats per minute due to increased SA node discharge sec. to sympathetic stimulation (physiological/pathological /pharmacological response)
• Usually between 100-160 (>160 SVT)
• Can be high due to anxiety, stress, fever, medications
(anything that increases oxygen consumption)
Sinus Rhythms

Treatment-:
-correcting underlying cause of symp. Stimulation.
-Beta blockers may be employed to lower heart rate and decrease myocardial o2 demand(if pt is not hypovolemic).
-supplemental O2 to increase supply in response to increase demand.
-Avoidance of vagolytic drug (pancuronium) intraoperatively

Sinus Arrhythmia
Heart
RateRhythm P Wave
PR Interval
(sec.)
QRS
(Sec.)
Var. IrregularBefore each QRS,
Identical.12 - .20 <.12
Sinus Rhythms

• Sinus Arrhythmia
– One upright uniform p-wave for every QRS
– Rhythm is irregular
• Rate increases as the patient breathes in
• Rate decreases as the patient breathes out
– Rate is usually 60-100 (may be slower)
– Variation of normal, not life threatening
Sinus Rhythms

Premature Atrial Contraction (PAC)
Heart
RateRhythm P Wave
PR Interval
(sec.)
QRS
(Sec.)
NA Irregular
Premature &
abnormal or
hidden
.12 - .20 <.12
Atrial Rhythms

– Premature Atrial Contraction (PAC)
• One P-wave for every QRS
– P-wave may have different morphology on ectopic beat,
but it will be present
• Single ectopic beat will disrupt regularity of
underlying rhythm
• Rate will depend on underlying rhythm
• Underlying rhythm must be identified
• Classified as rare, occasional, or frequent PAC’s
based on frequency
Atrial Rhythms

• Sign and symptoms
-PACs arises from ectopic foci in atria. Typical symptoms include an awareness of a fluttering or a heavy heart beat.
-Precipitated by excessive caffeine, stress, alcohol, nicotine and hyperthyroidism.
-Often occur at rest and become less frequent by exercise.
-second most arrhythmias asso. With MI.

Perioperative T/t-:
1. Avoidance of ppt. factors and sympathetic stimulation.
2. Pharmacological T/t required only if the PACs
trigger sec. dysrhythmias.
3. Usually suppressed by calcium channel blocker or Beta blocker.

Atrial Fibrillation
Heart
RateRhythm P Wave
PR Interval
(sec.)
QRS
(Sec.)
Var. Irregular Wavy irregular NA <.12
Atrial Rhythms

• Atrial Fibrillation– No discernable p-waves preceding the QRS complex
• The atria are not depolarizing effectively, but fibrillating
– Rhythm is grossly irregular
– If the heart rate is <100 it is considered controlled a-fib, if >100 it is considered to have a “rapid ventricular response”
– AV node acts as a “filter”, blocking out most of the impulses sent by the atria in an attempt to control the heart rate
Atrial Rhythms

• Atrial Fibrillation (con’t)
– Often a chronic condition, medical attention only
necessary if patient becomes symptomatic
– Patient will report history of atrial fibrillation.
– Symptoms range from palpitation to angina
pectoris, CHF, pul. Oedema and hypotension
– Often associated with fatigue and generalized
weakness.
– Predisposing factors are :RHD, hypertension,
thyrotoxicosis, IHD, chronic COPD, pericarditis
and pulmonary embolus.
Atrial Rhythms

Perioperative management-
-If new onset of AF, surgery should be postponed if possibleuntill control of dysrhythmia.
-T/t of AF during Sx depends on hemodynamic stability of pt.
-if hemodynamically significat, the T/t is cardioversion
-Synchronized electrical cardioversion (100 to 200 J) is mosteffective.
-Pharmacological cardioversion by IV amiodarone (pref.drug),diltiazem or verapamil may be attempted.
-Pt with chronic AF should be maintained on theirantidysrhythmic drugs with close attention to serumelectrolyte(K &Mg).
-Manage the transition on and off IV and oral anticoagulation.

Atrial Flutter
Heart Rate Rhythm P WavePR Interval
(sec.)
QRS
(Sec.)
Atrial=250
– 400
Ventricular
Var.
Irregular Sawtooth
Not
Measur-
able
<.12
Atrial Rhythms

• Atrial Flutter– More than one p-wave for every QRS complex
• Demonstrate a “sawtooth” appearance
– Atrial rhythm is regular. Ventricular rhythm will be regular if the AV node conducts consistently. If the pattern varies, the ventricular rate will be irregular
– Rate will depend on the ratio of impulses conducted through the ventricles
– Most commonly atrial rate compared to ventricular rate 2:1 (if atrial rate is 300bpm and 2:1 conduction,ptcan present with venticular rate of 150 with sign and symptoms)
Atrial Rhythms

• Peioperative T/t-
-T/t depends on hemodynamic stability of patient.
-If AF is hemodymamically sig. the T/t is cardioversion, synchronized elec. Cardioversion satarting at 50 J is indicated.
-Pharmacological control of ventricular response with IV amiodarone, diltiazem or verapamil may be tried, if vital signs are stable.

Atrial Rhythms
• Atrial Flutter
– Atrial flutter is classified as a ratio of p-waves
per QRS complexes (ex: 3:1 flutter 3 p-waves
for each QRS)
– Not considered life threatening, consult
physician if patient symptomatic

• Rhythms that originate at the AV junction
• Junctional rhythms do not have
characteristic p-waves.
Junctional Rhythms

Premature Junctional Contraction PJC
Heart
RateRhythm P Wave
PR Interval
(sec.)
QRS
(Sec.)
Usually
normalIrregular
Premature,
abnormal, may be
inverted or hidden
Short
<.12
Normal
<.12
Junctional Rhythms

• Premature Junctional Contraction (PJC)– P-wave can come before or after the QRS complex,
or it may lost in the QRS complex• If visible, the p-wave will be inverted
– Rhythm will be irregular due to single ectopic beat
– Heart rate will depend on underlying rhythm
– Underlying rhythm must be identified
– Classify as rare, occasional, or frequent PJC based on frequency
– Atria are depolarized via retrograde conduction
Junctional Rhythms

Accelerated Junctional
Heart
RateRhythm P Wave
PR Interval
(sec.)
QRS
(Sec.)
Var. RegularInverted, absent or
after QRS<.12 <.12
Junctional Rhythms

• Accelerated Junctional Rhythm
– P-wave can come before or after the QRS complex, or lost within the QRS complex• If p-waves are seen they will be inverted
– Rhythm is regular
– Heart rate between 60-100 beats per minute • Within the normal HR range
• Fast rate for the junction (normally 40-60 bpm)
Junctional Rhythms

Junctional Tachycardia
Heart
RateRhythm P Wave
PR Interval
(sec.)
QRS
(Sec.)
>100 RegularMay be inverted or
hidden
Short
<.12
Normal
<.12
Junctional Rhythms

• Junctional Tachycardia
– P-wave can come before or after the QRS complex or lost within the QRS entirely
• If a p-wave is seen it will be inverted
– Rhythm is regular
– Rate is between 100-180 beats per minute
• In the tachycardia range, but not originating from SA node
– AV node has sped up to override the SA node for
control of the heart
– Junctional rhythm often result in AV dyssynchrony
and a junctional tachycardia can severly impaired
Cardiac output.
Junctional Rhythms

• Perioperative T/t-
-Junctional rhythm is not frquent during GA.
-Transient Junctional rhythm require no T/t
-Loss of AV synchrony during a junctional rhythm may result in MI, heat failure or hypotension
-Atropine 0.5 mg can be used to treat hemodynamically significat junctional rhythms

Ventricular Rhythms
Premature Ventricular Contraction (PVC)
Heart
RateRhythm P Wave
PR
Interval
(sec.)
QRS
(Sec.)
Var. Irregular
No P waves
associated with
premature beat
NAWide
>.12

Ventricular Rhythms
• Premature Ventricular Contraction (PVC)
– The ectopic beat is not preceded by a p-wave
– Irregular rhythm due to ectopic beat
– Rate will be determined by the underlying rhythm
– QRS is wide and may be bizarre in appearance
– Caused by a irritable focus within the ventricle which
fires prematurely

Ventricular Rhythm
• Premature Ventricular Contraction
– Classify as rare, occasional, or frequent
– Classify as unifocal, or multifocal PVC’s
• Unifocal-originating from same area of the
ventricle; distinguished by same morphology

Ventricular Rhythm
• Premature Ventricular Contraction – Classify as unifocal, or multifocal PVC’s
– Unifocal-originating from same area of the ventricle; distinguished by same morphology
– Multifocal-originating from different areas of the ventricle; distinguished by different morphology

Ventricular Rhythm
• Premature Ventricular Contraction
– Bigeminy• A PVC occurring every other beat
– Also seen as Trigeminy, Quadrigeminy

Ventricular Rhythm• Dangerous PVC’s
– R on T
– Runs of PVC’s– 3 or more considered Vtach

• Causes of PVCs
- Arterial hypoxemia- MI- Myocarditis- SNS activation- Hypokalemia/Hypomagnesemia
- Digitalis toxicity- Caffeine, cocaine,Alcohol- Mechanical irritation-(CV or Pulm. Artery
catheter)

• Prioperative T/t-
-During anaesthesia, if pt exhibits 6 or more PVCs
per minute and repetetive or multifocal forms, there is increased risk of developing life threatining dysrhythmia.
-T/t include a D/d of possible cause and t/t of that cause, while t/t of cause, the immediate availability of a defibrillator should be confirmed.
-Beta blockers are the most successful drug, amiodarone,lidocaine and other antiarhythmic are indicated if the PVCs progress to VT or ferquent to cause hemodynamic instability.

Ventricular Rhythms
Ventricular Tachycardia
Heart
RateRhythm P Wave
PR Interval
(sec.)
QRS
(Sec.)
100 –
250Regular
No P waves
corresponding to QRS,
a few may be seen
NA >.12

Ventricular Rhythms
• Ventricular Tachycardia
– No discernable p-waves with QRS
– Rhythm is regular
– Atrial rate cannot be determined, ventricular
rate is between 150-250 beats per minute
– Must see 4-6 beats in a row to classify as v-
tach

Ventricular Rhythms
• Ventricular Tachycardia– THIS IS A DEADLY RHYTHM
• Check patient:
– If patient awake and alert, monitor patient and call physician
– Pt with symptomatic or unstable VT or SVT cardioverted
immediately.
– If vitals signs stable and VT is persistent or recurrent after
cardioversion, Amiodarone 150mg over 10min should be
given, other drugs may be used like procainamide,lignocaine
or sotalol.
– Pulseless VT requires immediate cardioversion/defibrillation
and CPR. (If patient has no vital signs, call code and start
CPR
» Defibrillate)

Ventricular Rhythms
Ventricular Fibrillation
Heart
RateRhythm P Wave
PR Interval
(sec.)
QRS
(Sec.)
0 Chaotic None NA None

Ventricular Rhythms
• Ventricular Fibrillation
– No discernable p-waves
– No regularity
– Unable to determine rate
– Multiple irritable foci within the ventricles all firing simultaneously
– May be coarse or fine
– This is a deadly rhythm
• Patient will have no pulse
• Call a code and begin CPR
• Survival is best if defbrillation occcurs within 3-5 min

Asystole
Heart
RateRhythm P Wave
PR Interval
(sec.)
QRS
(Sec.)
None None None None None

Asystole
• No p-waves
• No regularity
• No Rate
• This rhythm is associated with death
– Check patient and leads
– No pulse
• Begin CPR

Heart Block
First Degree Heart Block
Heart
RateRhythm P Wave
PR Interval
(sec.)
QRS
(Sec.)
Norm. RegularBefore each QRS,
Identical> .20 <.12

Heart Block– First Degree Heart Block
• P-wave for every QRS
• Rhythm is regular
• Rate may vary
• Av Node hold each impulse longer than normal before conducting normally through the ventricles
• Prolonged PR interval– Looks just like normal sinus rhythm
Cuases- increased vagal tone, digitalis toxicity, inferior wall MI and myocarditis.
-Usually asymptomatic and rarely require T/t.
-Elimination of drugs that slows AV conduction or clinical factors that enhance vagal tone can reverse 1st degree block.

Heart BlockSecond Degree Heart Block
Mobitz Type I (Wenckebach)
Heart
RateRhythm P Wave
PR Interval
(sec.)
QRS
(Sec.
)
Norm.
can be
slow
Irregular
Present but some
not followed by
QRS
Progressively
longer<.12

Heart Block
• Second Degree Heart Block
• Mobitz Type I (Wenckebach)– Some p-waves are not followed by QRS complexes
– Rhythm is irregular• R-R interval is in a pattern of grouped beating
– Rate 60-100 bpm
– Intermittent Block at the AV Node• Progressively prolonged p-r interval until a QRS is blocked
completely

Heart Block
Second Degree Heart BlockMobitz Type II (Classical)
Heart
RateRhythm P Wave
PR
Interval
(sec.)
QRS
(Sec.)
Usually
slow
Regular
or
irregular
2 3 or 4 before each
QRS, Identical.12 - .20
<.12
depends

Heart Block
• Second Degree Heart Block
• Mobitz Type II (Classical)
– More p-waves than QRS complexes
– Rhythm is irregular
– Atrial rate 60-100 bpm; Ventricular rate 30-100 bpm (depending on the ratio on conduction)
– Intermittent block at the AV node
• AV node normally conducts some beats while blocking others
• Mobitz type II block has high rate of progression to 3rd
degree heart block. A cardiac pacemaker is mandatory in this situation.

Heart Block
Third Degree Heart Block(Complete)
Heart
RateRhythm P Wave
PR
Interval
(sec.)
QRS
(Sec.)
30 –
60Regular
Present but no
correlation to QRS
may be hidden
Varies<.12
depends

Heart Block
• Third Degree Heart Block (Complete)– There are more p-waves than QRS
complexes– Both P-P and R-R intervals are regular
– Atrial rate within normal range; Ventricular rate between 20-60 bpm
– The block at the AV node is complete• There is no relationship between the p-waves and
QRS complexes.• Cardiac pacing is require in cases of 3rd degree
block

• Anaesthetic management
-Previous placement of a transvenous pacemacker oravailability of of transcutaneous cardiac pacing is requiredbefore an anesthetic is administered for insertion ofpermanent cardiac pacemaker ,
-Isoproterenol may be required to maintain acceptable HRand acts as “chemical pacemaker” untill the artificialpacemaker is functional

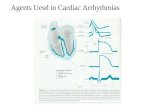
MODALITIES FOR TREATMENT OF ARRHYTHMIA
• Antiarrhythmic drugs
. All such drugs may aggravate or produce arrhythmias and they may also depress ventricular contractility and must, therefore, be used with caution.
• They are classified according to their effect on the action potential (Vaughan Williams' classification)


Drugs affecting different parts of the heart

Management of Arrythmia’s
• ECG and rhythm information
• should be interpreted within the context of total patient assessment
• Providers must evaluate
• Patient’s symptoms
• Clinical signs
• Ventilation, oxygenation, heart rate, blood pressure, signs of inadequate organ perfusion

• In both unstable and symptomatic cases
• Provider must make an assessment whether it is the arrhythmia that is causing the patient to be unstable
• Patient in septic shock with sinus tachycardia 140 / min is unstable
• Electric cardioversion will not improve this patient’s condition

• If patient with severe hypoxemia becomes hypotensive and develops bradycardia
• Bradycardia is not the primary cause of instability
• Treating the bradycardia without treating the hypoxemia is unlikely to improve the patient’s condition



Supraventricular Tachycardia
• (Supraventricular - a rhythm process in which the ventricles are activated from the atria or AV node/His bundle region)
• Refers to supraventricular tachycardia other than afib, aflutter and MAT
• Occurs in 35 per 100,000 person-years
• Usually due to reentry—AVNRT or AVRT

• QRS typically narrow (in absence of bundle branch block); thus, also termed narrow QRS tachycardia
• Usually paroxysmal, i.e, starting and stopping abruptly; called PSVT
• Aetiology should be considered before therapy is instituted

Vagal maneuver
• Valsalva maneuver or carotid sinus massage
• Terminate up to 25% of PSVTs
• For other SVTs
• May transiently slow the ventricular rate
• Potentially assist rhythm diagnosis but will not usually terminate such arrhythmias

Adenosine ( if regular)
• If PSVT does not respond to vagal maneuvers
• Give 6 mg of IV adenosine as a rapid IV push through antecubital vein followed by a 20 mL saline flush
• If the rhythm does not convert within 1 to 2 minutes
• Give a 12 mg rapid IV push using the method above

Narrow-complex irregulartachycardia
• Atrial fibrillation with uncontrolled ventricular response
• MAT
• sinus rhythm/tachycardia with frequent atrial premature beats

Rate Control
• Unstable patients
• Prompt electric cardioversion
• Stable patients
• Ventricular rate control as directed by patient symptoms
• IV nondihydropyridine calcium channel blockers
Diltiazem are drugs of choice for acute rate control in most individuals with atrial fibrillation and rapid ventricular rate

Ventricular arrhythmias
• Non-sustained ventricular arrhythmias
- routinely seen in the absence of cardiac disease- may not require drug therapy in the perioperative period.
- Conversely, in patients with structural heart disease, these non-sustained rhythms do predict subsequent life-threatening ventricular arrhythmias.

NSVT after - cardiopulmonary bypass, unstable patients with marginal perfusion may deteriorate with recurrent episodes of NSVT
may benefit from suppression with lidocaine or beta blockade.
repletion of post-bypass hypomagnesaemia (MgCl2 2 g i.v.) reduces the incidence of NSVT after cardiac surgery.

Sustained VT
• two categories: monomorphic and polymorphic.
• monomorphic VT - the amplitude of the QRS complex remains constant
• polymorphic ventricular tachycardia - the QRS morphology continually changes.

Therapy for monomorphic wide complex tachycardia
• If the etiology of the rhythm cannot be determined
• QRS monomorphic, regular
• IV adenosine is relatively safe for both treatment and diagnosis
• However, adenosine should not be given for unstable or irregular or polymorphic wide complex tachycardias
• • It may cause degeneration of the arrhythmia to VF

• If the wide-complex tachycardia proves to be SVT with aberrancy
• transiently slowed or converted by adenosine to sinus rhythm
• If due to VT there will be no effect on rhythm (except in rare cases of idiopathic VT)
• When adenosine is given for undifferentiated wide complex tachycardia
• Defibrillator should be available

For patients who are stable with likely VT
• IV antiarrhythmic drugs or elective
cardioversion is the preferred treatment strategy
• Amiodarone
• Procainamide
• Sotalol
• Procainamide and sotalol should be avoided in patients with prolonged QT, CHF

Wide-complex irregularrhythm
• Should be considered preexcited atrial fibrillation
• Expert consultation is advised
• Avoid AV nodal blocking agents
• adenosine, calcium channel blockers, digoxin, and possibly β-blockers

Polymorphic (Irregular) VT
• First step
• Stop medications known to prolong the QT interval
• Correct electrolyte imbalance
• Acute precipitants: drug overdose or poisoning

Prolong QT interval (Torsades de pointes)
• The management of torsades de pointes differs markedly from other forms of VT, and includes
• i.v. magnesium sulfate (2±4 g),
• repleting potassium,
• and manoeuvres aimed at increasing the heart rate (atropine, isoprenolol or temporary atrial or ventricular pacing).
• Haemodynamic collapse with torsades requires asynchronous DC counter shocks