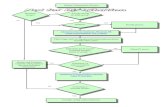
Pediatric Seizure and Status Epilepticus Management in the Emergency Setting.
-
Upload
josh-grammer -
Category
Documents
-
view
219 -
download
2
Transcript of Pediatric Seizure and Status Epilepticus Management in the Emergency Setting.

Pediatric Seizure and Status Epilepticus
Managementin the
Emergency Setting

Edward P. Sloan, MD, MPH
Associate Professor & Research Development Director
Dept of Emergency Medicine
University of Illinois College of Medicine
Chicago, IL

Attending Physician Emergency Medicine
University of Illinois Hospital
Our Lady of the Resurrection
Medical Center

Edward Sloan, MD, MPH
Pediatric Seizures & SEClinical Case • A 13 year old female presents with a frontal HA and prior
migraines that are relieved with ibuprofen• She had some AMS in the AM, with unusual motor
activity (restless, thrashing on bed)• She had no other systemic sx, recent illness, or head
trauma• She presented with normal vital signs and normal
neurologic exam• What should the emergency physician do?• What is the expected outcome of this patient?

Edward Sloan, MD, MPH
OverviewGlobal Objectives• Learn more about pediatric seizures
• Focus on peds sz etiologies
• Increase awareness of Rx options
• Enhance our ED management
• Improve patient care & outcomes
• Maximize MD & patient satisfaction

Edward Sloan, MD, MPH
OverviewSession Objectives
• Review main peds sz types, etiologies
• Briefly discuss Rx based on sz type
• Discuss relevant ED peds sz cases
• Summarize what Rx options exist
• Discuss rational treatment decisions

Edward Sloan, MD, MPH
OverviewPediatric Sz Epidemiology
• Common EMS & ED problem
• Szs are up to 6% of EMS encounters
• Up to 1% of all ED visits are peds sz
–Peds febrile: 1 in 125 visits (0.8%)
–Peds afebrile: 1 in 500 visits (0.2%)

Edward Sloan, MD, MPH
OverviewPediatric Sz Epidemiology• 2-5% have a febrile seizure
• 1% have an afebrile sz by age 14
• Highest afebrile sz rate before age 3
• 0.4-0.8% of children dvlp epilepsy
• SE most common before age 1

Edward Sloan, MD, MPH
OverviewPediatric SE Epidemiology• Mean age 3.2 yrs, median age 1 year
• 61% by age 3
• Etiology age dependent–25% is febrile SE
–Before age 1, 75% due to acute insult
–Epilepsy, fever, CNS infection common

Edward Sloan, MD, MPH
Pediatric Sz EtiologiesMeningitis
• Altered mental status universal
• Seizures in 23% of meningitis cases
• Complex & GTC seizures common
• Simple seizures rarely seen
• HIB vaccine makes this etiology rare

Edward Sloan, MD, MPH
Pediatric Sz EtiologiesHyponatremia
• Causes long duration szs and SE
• Infants < 6 months old, no clear etiol
• Too much water in formula
• Hypothermia (Temp < 36.5 degrees)

Edward Sloan, MD, MPH
Pediatric Sz EtiologiesCocaine Toxicity
• Consider in new onset seizures
• Crack cocaine rocks ingested
• Especially when no other etiology
• Common in urban EDs

Edward Sloan, MD, MPH
Pediatric SeizuresSeizure Outcome
• Immature CNS, myelinization–More prone to seizures
–More resistant to consequences
• Continuous seizures less toxic
• SE carries a low mortality (3-6%)

Edward Sloan, MD, MPH
Pediatric SeizuresSE Outcome
• Based on CNS status prior to SE
• Normal CNS, 64% remain intact
• Mortality related to two factors:–Acute neurologic insult
–Chronic CNS condition

Edward Sloan, MD, MPH
Pediatric SeizuresSeizure Type Classification• Generalized – Involves both cerebral hemispheres– Convulsive: tonic-clonic seizures– Non-convulsive: absence seizures
• Partial– Involves one cerebral hemisphere– Simple: no impaired consciousness– Complex: impaired consciousness

Edward Sloan, MD, MPH
Seizure ClassificationGeneralized Seizures• Convulsive seizures– Tonic sz: sustained contractions– Clonic sz: rhythmic flexor spasms– Tonic-clonic sz: combined mvmts
• Non-convulsive– Simple absence: impaired consciousness– Complex absence: brief motor mvmts

Edward Sloan, MD, MPH
Seizure ClassificationPartial Seizures• Simple seizures (no LOC)– Focal motor (Jacksonian)– Sensory or somatosensory– Autonomic– Psychic
• Complex (impaired consciousness)– Involves some cognitive, affective sx– Temporal lobe, psychomotor seizures

Edward Sloan, MD, MPH
Pediatric SeizuresOther Generalized Sz Types
• Neonatal seizures
• Benign childhood epilepsy (Rolandic)
• Infantile spasms (West syndrome)
• Lennox-Gastaut syndrome
• Atonic seizures
• Febrile seizures

Edward Sloan, MD, MPH
Pediatric SeizuresStatus Epilepticus Types• Convulsive SE : tonic-clonic sz• Non-convulsive SE: no tonic-clonic sz – Absence SE– Complex partial SE
• Subtle SE: prolonged convulsive SE– Worst prognosis, mortality > 30%– Persistent coma, focal motor mvmts only

Edward Sloan, MD, MPH
Specific Seizure Types Generalized Tonic-Clonic Sz
• Seizure described as a convulsion
• May occur primarily or secondarily
• May be preceded by prodrome or aura
• Tonic, then clonic phase
• Tongue biting, urinary incontinence
• Last for minutes, then post-ictal

Edward Sloan, MD, MPH
Specific Seizure Types Absence Seizure• Petit mal epilepsy
• Brief, limited motor activity
• Sudden interruption of consciousness
• Slight clonic mvmts, myoclonic jerks
• Automatisms also can be seen
• Last about 10 sec, not post-ictal

Edward Sloan, MD, MPH
Specific Seizure Types Partial Seizure• Focal motor sz (Jacksonian, frontal)
• Focus and/or lesion in cerebrum
• Sz clearly related to a lesion
• Sz type related to site of sz focus
• CT scan is useful
• Simple partial sz pts have no AMS

Edward Sloan, MD, MPH
Specific Seizure Types Complex Partial Seizure• Psychomotor, temporal lobe epilepsy
• Often a history of febrile seizures
• Complex aura, altered behavior
• Automatisms: lip smacking, chewing
• Not complete LOC, instead confused
• May secondarily generalize

Edward Sloan, MD, MPH
Specific Seizure Types Neonatal Seizure• Occur in first 28 days of life
• Most occur shortly after birth
• Subtle sz: lip smack, eye mvmt, apnea
• Perinatal asphyxia, metabolic abn
• Hypoglycemia, hypocalcemia
• CNS infection, hemorrhage, lesion

Edward Sloan, MD, MPH
Specific Seizure Types Benign Childhood Epilepsy
• Rolandic epilepsy
• Onset between 3 and 13 years of age
• Often occurs upon awakening
• Facial mvmts, grimacing, vocalizations
• EEG diagnosis

Edward Sloan, MD, MPH
Specific Seizure Types Infantile Spasms• West syndrome
• Occurs up to one year
• May be symptomatic or idiopathic
• Sudden tonic movements of the head, trunk, extremities
• Must do full work-up, incl metabolic
• Caution, AED hepatotoxicity a risk

Edward Sloan, MD, MPH
Specific Seizure Types Lennox-Gastaut Syndrome
• Onset from 1-8 years
• Peaks at 3-5 years
• Multiple seizure types
• GTC, tonic, absence, atonic szs
• ED Hx: exac of known sz disorder

Edward Sloan, MD, MPH
Specific Seizure Types Atonic Seizures• Astatic or akinetic seizures• Sudden loss of motor tone• Child falls to the floor• May have myoclonic jerks • No clear generalized seizure• No etiology of apparent syncopal episode

Edward Sloan, MD, MPH
Specific Seizure Types Febrile Seizures• Age: 6 months to 5 years
• Related to rapid rise in temperature
• Brief, self-limited generalized sz
• Complex: Focal, > 10-15 min, flurry
• 25% recurrence, esp if in child < 1 yr old
• Risk of epilepsy not significantly greater

Edward Sloan, MD, MPH
Specific Seizure Types Juvenile Myoclonic Epilepsy• Common in teens, young adults
• Etiology of generalized TC seizures
• History of staring spells
• History of AM clumsiness, myoclonus
• Sleep deprivation, EtOH precipitants
• Phenytoin: worse myoclonus, absence sz

Edward Sloan, MD, MPH
Specific SE Types Generalized Convulsive SE• Seizure lasting greater than 5-10 min
• Refractory to initial benzo therapy
• Flurry of seizures and coma
• CNS injury likely after 30-40 minutes
• Glutamate, cell death, tissue necrosis
• Injury even if systemic sx controlled

Edward Sloan, MD, MPH
Specific SE Types Non-convulsive SE• No generalized tonic-clonic sz – Absence SE– Complex partial SE
• No frank coma
• More common in children
• Not always due to co-morbidity
• Mortality ?? not as high as in GCSE

Edward Sloan, MD, MPH
Specific SE Types Subtle SE
• Late manifestation of GCSE, frank coma
• No longer with tonic-clonic mvmts
• Still actively seizing (electrical SE)
• Usu in older patients
• Marked co-morbidity (encephalopathic)
• Highest SE mortality

Edward Sloan, MD, MPH
Seizure Therapy Generalized Seizure Protocol• Benzodiazepines– PR diazepam, IM midazolam, IV lorazepam
• Phenytoins– Fosphenytoin can be given IV or IM
• Phenobarbital or valproate – Less sedation with valproate
• Propofol or midazolam infusions– EEG monitoring, BP support key

Edward Sloan, MD, MPH
Seizure Therapy Ongoing Therapies• Absence: Ethosuximide, valproate• Atonic: Valproate, clonazepam,
ethosuximide• Myoclonic: Valproate, clonazepam• Partial: Carbamazepine,
phenytoin, valproate• Generalized: Carbamazepine,
phenytoin, phenobarb, primidone, valproate

Edward Sloan, MD, MPH
Case PresentationsED Pediatric Seizure Cases
• Pediatric complex partial SE
• New onset SE in an adolescent
• New onset sz in a college student

Edward Sloan, MD, MPH
Pediatric SE: Pediatric Complex Partial SE
• How do we Dx complex partial SE?
• What is the optimal Rx protocol?
• Why?

Edward Sloan, MD, MPH
Pediatric SEHx• 7 year old male
• Seizure-like activity?
• Patient with staring spells
• Some headache and shaking movement, esp of hands
• Frontal headache, vomiting

Edward Sloan, MD, MPH
Pediatric SEHx (con’t)• Seen at 2130, 2230 sign-out
• AMS, r/o seizure disorder
• “Once all of the labs are back, he should be OK to go home…”

Edward Sloan, MD, MPH
Pediatric SEPx• 98.7 98/60 72 20
• Well hydrated
• CV, lung exams normal
• Neuro exam intact

Edward Sloan, MD, MPH
Pediatric SEClinical Course• 0220 “episode”
• Tachycardia, BP OK, airway OK
• Confused, staring off into space
• Episode lasted < 5 minutes
• Resolved without any Rx

Edward Sloan, MD, MPH
Pediatric SEClinical Course (con’t)
• Three more episodes over 40’
• Similar autonomic symptoms
• Some non-purposeful ext mvmts
• Diaphoresis, urinary incontinence
• Remained somnolent between episodes

Edward Sloan, MD, MPH
Pediatric SEDx• Repetitive episodes with AMS
• Autonomic symptoms noted
• Non-purposeful mvmts noted
• Rule out complex partial status epilepticus (CPSE)

Edward Sloan, MD, MPH
Pediatric SERx• IV lorazepam
• IV valproate
• Transfer to Children’s
• ICU observation
• Uncomplicated course

Edward Sloan, MD, MPH
Adolescent SE: New Onset AMS/Spells
• What is the AMS?
• Is it a seizure?
• How should we Rx new onset szs?
• What is the role of the ED EEG?
• When should it be ordered?

Edward Sloan, MD, MPH
Adolescent SEHx• 13 year old female
• Frontal HA and prior migraines
• HA relieved with ibuprofen
• AMS in AM, with ?? motor activity
• Restless at home, thrashing on bed
• No other systemic sx or recent illness

Edward Sloan, MD, MPH
Adolescent SEPx• Vitals OK, afebrile
• Alert, O x 3, NAD
• Head/Neck OK
• Chest/cor/abd OK
• Neuro: No focal deficit. MS OK

Edward Sloan, MD, MPH
Adolescent SEQuestion # 1
•What diagnostic tests are indicated at this point?

Edward Sloan, MD, MPH
Adolescent SEQuestion # 2
•Did the patient have a seizure? •Does it influence Dx, Rx?

Edward Sloan, MD, MPH
Adolescent SEQuestion # 3
•Does the patient require admission for observation for possible new onset seizures?

Edward Sloan, MD, MPH
Adolescent SEClinical Course• Labs, tox screen neg
• CT negative
• Neuro consult: EEG and then D/C
• Dx: AMS, r/o Seizure; migraine HA
• While EEG applied, pt with AMS
• Agitation, thrashing on cart

Edward Sloan, MD, MPH
Adolescent SEQuestion # 4
• Is this repeat spell a seizure? •What type?

Edward Sloan, MD, MPH
Adolescent SEQuestion # 5
•Does this AMS and motor activity require Rx? •What Rx?

Edward Sloan, MD, MPH
Adolescent SEQuestion # 6
•Does the patient now require admission for observation for possible new onset seizures?

Edward Sloan, MD, MPH
Adolescent SEClinical Course (con’t)
• During EEG, pt with R face focal sz• Leftward gaze noted• Seizure then generalized• Meds were given• Seizure terminated

Edward Sloan, MD, MPH
Adolescent SEQuestion # 7
•What med is to be used for seizure control / SE termination?

Edward Sloan, MD, MPH
Adolescent SEQuestion # 8
•What med is to be used once SE is terminated?•Why?

Edward Sloan, MD, MPH
Adolescent SEQuestion # 9
•How should the meds be given?
•Why?

Edward Sloan, MD, MPH
Adolescent SEClinical Course (con’t)
• SE terminated with Rx
• Pt stabilized, still somnulent
• ALS transfer team to Children’s
• Pt with resolving AMS at time of D/C

Edward Sloan, MD, MPH
Adolescent SEDx
• New onset SE
• Complex partial seizures with generalized seizure / SE
• Hx migraine headaches

Edward Sloan, MD, MPH
Adolescent SERx• Lorazepam to Rx the acute sz–2mg IVP x 2
• Valproate for ongoing protection–25 mg/kg load administered
– Infused over 20 minutes
• PRN meds during transfer

Edward Sloan, MD, MPH

Edward Sloan, MD, MPH

Edward Sloan, MD, MPH

Edward Sloan, MD, MPH

Edward Sloan, MD, MPH
Juvenile Myoclonic Sz: College Student, New Onset Sz
• What is the likely etiology?
• What is JME?
• What are the long-term implications?
• How to RX once the sz terminated?

Edward Sloan, MD, MPH
Juvenile Myoclonic SzHx• 21 year old college student
• No prior neuro history
• Final exams, sleepless
• Great party after the last exam
• Pt with single generalized sz
• Seizure upon awakening

Edward Sloan, MD, MPH
Juvenile Myoclonic SzPx• Vitals OK
• Neuro: slightly post-ictal
• Exam otherwise normal
• Patient has a 2nd seizure in the ED

Edward Sloan, MD, MPH
Juvenile Myoclonic SzDx
• Juvenile myoclonic epilepsy
• Related to sleep deprivation, alcohol consumption
• Occurs upon awakening
• Responds best to valproate
• Phenytoin may exacerbate sx

Edward Sloan, MD, MPH
Juvenile Myoclonic SzRx• Benzodiazepines to Rx the acute sz
• Ongoing protection an issue
• Valproate is likely the drug of choice
• Phenytoin may not be optimal
• Avoid status epilepticus

Edward Sloan, MD, MPH
ConclusionsClinical Pearls• Acute, repetitive spells = sz
• Ongoing altered mental status = complex partial SE
• Treat acute szs with lorazepam
• Valproate is the etiology-specific ongoing Rx in many young people
• Know the specific JME clinical setting

Edward Sloan, MD, MPH
RecommendationsManagement Implications
• Educate about sz etiologies
• Make multiple drugs available
• Alternate routes should be used
• A protocol should exist
• Utilize EEG when necessary
• Be aware of optimal Rx at disposition