Pathology of Hypertension
-
Upload
darya-daoud -
Category
Health & Medicine
-
view
13 -
download
1
Transcript of Pathology of Hypertension

Hypertension (HBP/HTN)
Pathology4th year pharmacy
Dr: Nemat Mohammed
By: Darya Osman, Eman Salah, Moaz Ahmed, Manal Saeed

o Force exerted by circulating blood on the arterial walls.
o One of principal vital signs.
o Maximum (systolic) pressure – pressure in the artery when the left ventricle is contracting to force the blood into aorta and other arteries.
o Minimum (diastolic) pressure – pressure in the artery when the ventricles are relaxing and the heart is filling up, receiving blood from veins.
o Sphygmomanometer – device used to measure BP
Blood pressure

Heart Rate Stroke volume
Cardiac output Peripheral resistance
Blood Pressure
+
+

Regulation of BPo Baroreceptor reflex – changes in arterial pressure –
medulla (brain stem)◦ Location : left and right carotid sinuses, aortic arch
o Renin – angiotensin system (RAS)◦ Long – term adjustment of arterial pressure◦ Kidney - compensation◦ Endogenous vasoconstrictor – angiotensin I
o Aldosterone release (adrenal cortex)◦ Stimulates sodium retention and potassium excretion by the
kidney◦ Increases fluid retention and indirectly arterial pressure

Hypertension (HTN)o Chronic medical condition in which blood pressure is
elevated
o A systolic blood pressure >139 mmHg and diastolic > 89 mmHg
o Based on the average of two or more properly measured, seated BP reading on two different doctor’s visits

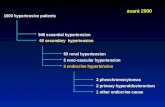
Types of HTNPRIMARY HTN
o also known as essential HTN.
o Accounts for 95% cases of HTN.
o No universally established cause known.
SECONDARY HTN
o less common cause of HTN ( 5%).
o secondary to other potentially rectifiable causes.

Primary HTN
oNo medical cause
o Risk factors :o Sedentary lifestyleo Obesity ( body mass index
greater than 25)o Salt ( sodium) sensitivityo Alcohol, smokingo Family history

Secondary HTN Common
◦ Intrinsic renal disease
◦ Renovascular disease
◦ Mineralocorticoid excess
◦ Sleep Breathing disorder
Uncommon◦ Pheochromocytoma
◦ Glucocorticoid excess
◦ Coarctation of Aorta
◦ Hyper/hypothyroidism

Pathophysiology of HTNo Inability of the kidneys to excrete sodium
o An overactive renin – angiotensin system, vasoconstriction and retention of sodium and water – hypertension
o An overactive sympathetic nervous system

The ANSo Increased production of catecholamines (epinephrine
and norepinephrine) results in SNS overactivity.
o This results in an increased heart rate, increased peripheral vascular resistance due to systemic vasoconstriction, and hypertension.
o Additionally, an overactive SNS effects insulin resistance, vascular remodeling, has procoagulant effects, which can lead to neospasm and narrowing of the blood vessels

Vascular remodelling

The RAAS

Endothelial Dysfunction
• Oxidative stress upsets balance between endothelin and Nitric oxide
• leads to changes in the endothelium and sets up a “vicious cycle” that contributes to the maintenance of high blood pressure
• Alterations in endothelial function are a reliable indicator of target organ damage and atherosclerotic disease, as well as prognosis


Geneticso Caused by single gene mutations which leads to several forms of high blood
pressure
o Ten genes have been identified which cause these monogenic forms of hypertension.
o HTN has been linked with several chromosomal regions, including regions linked to familial combined hyperlipidemia, was found.


Risk factorso Non Modifiable:
o Age
o Sex
o Race
o Family history
o Modifiable:
o Weight
o Physical fitness
o Smoking and alcohol
o Diet
o Stress
o diabetes
o Certain chromic conditios (e.g. kidney disease, sleep apnea)

Complications of Prolonged Uncontrolled HTN
o Changes in the vessel wall leading to vessel trauma and arteriosclerosis throughout the vasculature
o Complications arise due to the “target organ” dysfunction and ultimately failure.
o Damage to the blood vessels can be seen on fundoscopy.

Target Organs o CVS (Heart and Blood Vessels)
o The kidneys
o Nervous system
o The Eyes

Effects On CVS o Ventricular hypertrophy, dysfunction and failure
o Arrhithymias
o Coronary artery disease, Acute MI
o Arterial aneurysm, dissection, and rupture

Effects on The Kidneyso Glomerular sclerosis leading to impaired kidney function and finally end stage kidney disease
o Ischemic kidney disease especially when renal artery stenosis is the cause of HTN

Nervous Systemo Stroke
o intracerebral and subaracnoid hemorrhage
o Cerebral atrophy and dementia

The Eyeso Retinopathy, retinal hemorrhages and impaired vision
o Vitreous hemorrhage, retinal detachment
o Neuropathy of the nerves leading to extraoccular muscle paralysis and dysfunction

SIGNS AND SYMPTOMS
o No symptoms – many people unaware they have hypertension until accidentally found
o Non–specific symptoms – mild symptoms
Headache, Morning headache, Tinnitus, Dizziness, Confusion, Fatigue, Shortness of breath, Changes in vision – blindness, Nausea

Treatment of HTNo Antihypertensive drugs – act by lowering blood pressure
o Aim of treatment - <140/ 90
o Reduction of blood pressure by 5-6 mm/Hg decreases the risk of stroke by 40%, coronary heart disease by 15- 20%, heart failure and mortality from vascular disease

Antihypertensive drugs
ACE – IARBs
Beta blockersThiazide diuretics
VasodilatorsLong acting CCBAlp
ha blockersCentral agents

Preventiono Weight reduction
o Aerobic exercise (e.g. walking)
o Reducing sugar intake
o Reducing sodium (salt) and fat/fat free food
o Fruits, vegetables
o Stopping smoking
o Reducing stress (relaxation therapy – meditation)