Palatal fistula and syndromes associated with clcp part 1 by Dr. Amit Suryawanshi Oral &...
-
Upload
dr-amit-t-suryawanshi -
Category
Health & Medicine
-
view
81 -
download
2
description
Transcript of Palatal fistula and syndromes associated with clcp part 1 by Dr. Amit Suryawanshi Oral &...

Palatal Fistula and Syndromes associated with CLCP
Part - I
Dr. Amit T. Suryawanshi
Oral and Maxillofacial Surgeon
Pune, India
Contact details :Email ID - [email protected]
Mobile No - 9405622455

• The dictionary meaning of cleft is a crack, fissure, split or a gap.
• The zones affected by common orofacialclefts are as follows:– Upper lip
– Alveolar ridge
– Hard palate
– Soft palate
– Nose (not so common)
– Eyes (not so common).
INTRODUCTION

BIRTH DEFECTS
ParentsFamily Members
Patients
Severe
Psychological
stress

• Feeding problems
• Improper growth of face
• Delayed & Improper Speech
• Delayed or abnormal tooth eruption
• Ear infections & hearing problems
• Recurrent chest infections
• Social & Psychological problems
EFFECTS ON CHILD

• In India: (C.M.C. Vellore) 1:700
• Racial variations: (By Gopalkrishnan: Dharwad Cleft Unit)– American Black 0.21 - 0.41
– Japanese 1.14 – 2.13
– Caucasian 0.77 – 1.40
– Indian 0.13 – 1.90
INCIDENCE

• Clefts may be caused by hereditary
– Sex-linked recessive gene.
– Family history of cleft lip and palate (40%)
• Environmental
– Infections during pregnancy (viral)– Nutrition deficiencies ( Folic acid)– Anemia , seizures during pregnancy– Harmful drug intake– Excessive consumption of alcohol
ETIOLOGY

Cleft Lip:
Failure of fusion of medial nasal process and maxillary processes
Cleft Palate:
Failure of fusion of palatine processes of maxilla
EMBRYOLOGY

INTERMAXILLARY SEGMENT – formed by Median nasal process fusion at deeper level .
Composed of labial componentupper jaw componentPRIMARY PALATE portion of nasal septum
DEVELOPMENT OF PALATE

DEVELOPMENT OF PALATE
Palate develops from the primary palate & secondary palate
Secondary palate derived from maxillary prominences
Outgrowth of palatine shelves appear in sixth week & on each side of tongue

In 7th week palatine shelves attain horizontal position & fuse with each other to form secondary palate
Secondary palate fuse with nasal septum and posterior part of primary palate
Bone extend from maxilla to ossify hard palate
DEVELOPMENT OF PALATE

DEVELOPMENT OF PALATE
Posterior part of palatine process do not get ossified and extend posteriorly to form soft palate
The median palatine raphe indicates line of fusion of processes

Nasopalatine canal
persists in median
plane between
premaxilla and
secondary palate &
represented in adult
as incisive fossa.
DEVELOPMENT OF PALATE

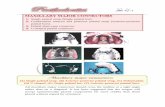
Incomplete cleft palate
Unilateral complete cleft lip and palate
Complete Cleft Palate
Bilateral complete CLP
TYPES OF CLEFT PALATE

• Kernahan has simplified it
• representing various clefts in the form of Y.
• Anterior portion of Y depict the lip (1 and 4)
• Middle alveolus (2 and 5)
• Incisive foramina and the posterior portion (3 and 6)
• Posterior to the incisive foramen, the hard (7 and 8) and the soft (9) palate.

MUSCLES OF PALATE

Tensor veli palatini (TVP)
• Function-stiffens soft palate and opens eustachian tube
• Innervation-Cranial nerve V3
Levator veli palatini (LVP)
• Function-elevates soft palate in speech and swallowing
• Innervation-Cranial nerve IX and X

Uvula• Fnction-elevates uvula• Innervation-Cranial nerve IX and X
Palatopharyngeus• Function-narrow and seal nasal pharynx• Innervation-Cranial nerve IX and X

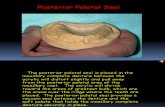
Complete Cleft Palate :
Palatal shelves fail to fuse
The greater palatine foramen is located more anteriorly and laterally
Gap in the soft palate does not always correspond to the gap of the hard palate
A layer of the mucosa can extend and conceal a long underlying cleft in the bone structure
The palatal aponeurosis is missing at the midline

Major muscles, levatorveli palatini and palatopharyngeus do not join on the midline, fibres run parallel to the margins of the cleft
Two halves of the uvula are converged towards one another
There is a difference in the colour of the mucosa, oral mucosa is paler, nasal mucosa is redder

Cleft Palate Team
– Cleft Audiologist
– Orthodontics
– Cleft surgeon
– Social worker
– Psychologist
20
Assessment and Treatment of Cleft Palate.

Cleft Palate Team
– Cleft Audiologist
– Orthodontics
– Cleft surgeon
– Social worker
– Psychologist
21
Assessment and Treatment of Cleft Palate.

Preoperative Evaluation• Pediatric evaluation • Anesthetic evaluation• Blood investigation• Ear infection• Malnutrition• Anaemia• Other congenital anomalies particularly
cardiac.• Milestones• Chest x-ray
– Upper respiratory tract infection

• Several Techniques- Trend is towards less scarring and less tension on palate
• Scarring of palate may cause impaired mid-facial growth(alveolar arch collapse, midface retrusion, malocclusion)
• Facial growth may be less affected if surgery is delayed until 18-24 months, but feeding, speech, socialization may suffer.
Surgical Repair- Cleft Palate

Complications
- Palatal Fistula

• Introduction:
Palatal defects are common complications seen after primary
cleft palate repair. Small fistulas may be asymptomatic while
large fistulas produce various symptoms. There are many
methods proposed for closure of palatal defects.

• Symptomatic fistula may cause :
Regurgitation of food and fluid to the nasal cavity,
Malodor
Escape of air during speech resulting in hyper nasality
Impaired suction
Increased nasal discharge
(Cleft palate journal, january 1978, vol. 15 No. 1 )

Most Common Site :Hard Palate ( most often at the junction of Hard &
soft Palate)
Incidence :
0% to 34%
(Cohen SR, Kalinowaski J et al : Cleft palate fistula: A multivariate stastical
analysis of prevalence, etiology & surgical management. Plast Reconstr Surg 87:
1041, 1991)
27

• Causes of fistula formation:
type of cleft,
type of repair,
wound tension,
single-layer repair,
infection and
dead space deep to the mucoperiosteal flap
(International Journal of Pediatric Otorhinolaryngology 74 (2010) 1054–1057)


Classification
A. By Shultz
1. Pinpoint
2. Slit
3. Oval or Total dehiscence

B. Based on anatomical location by Smith:
type I referred to bifid uvula;
type II means fistula in the soft palate;
type III means fistula at junction of the soft and hard palates;
type IV means fistula in the hard palate;

type V indicates that the fistula at junction of the primary and
secondary palates;
type VI means lingual alveolar fistula; and
type VII means labial alveolar fistula
(International Journal of Pediatric Otorhinolaryngology 74 (2010) 1054–1057)

B. According to site :
1. Anterior
2. Middle
3. Posterior

C. ( According to size)
1. Small ( < 3mm )
2. Medium ( 3-5mm)
3. Large ( > 5mm )
(Cohen SR, Kalinowaski J et al : Cleft palate fistula: A multivariate stastical
analysis of prevalence, etiology & surgical management. Plast Reconstr Surg 87:
1041, 1991)

Causes of Fistula
Improper Mobilization
Tension Across the Suture Line
Compromised Vascularity
Flap Necrosis
Infections
dead space deep to the mucoperiosteal flap
(International Journal of Pediatric Otorhinolaryngology 74 (2010) 1054–
1057)

Closure of Palatal Fistula

Principals of fistula closure:
1) Elevation of large palatal flaps based on the
original incisions

2) Excision of the scarred margins of the fistula;
No scar epithelium can be left traversing the
fistula anywhere around its perimeter,

3) Accurate tension free closure of the nasal &
oral mucosa

4 )Use of additional unscarred tissue to close
anterior defects or large palatal defects;
Mucobuccal flap & tongue flap are most
useful;

5) Bone graft when indicated;
But it is not necessary for successful fistula
closure.