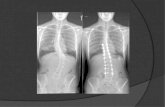
Orthopedic Clinics Na 2007 Vol 38 Scoliosis
Transcript of Orthopedic Clinics Na 2007 Vol 38 Scoliosis


Orthop Clin N Am 38 (2007) ix
Preface
Guest Editor
Anthony A. Stans, MD
Scoliosis treatment has undergone tremendouschange and innovation during the past 10 years.From elementary distraction-compression instru-
mentation methods have evolved sophisticatedinstrumentation systems that give the surgeon tre-mendous power to move individual vertebrae
three-dimensionally through space. Even as in-strumentation techniques become more advanced,there is renewed interest in nonoperative scoliosis
treatment. At risk of becoming a lost art, casttreatment is achieving encouraging results in theextremely challenging infantile and juvenile pa-
tient groups. Just as a national, randomized, pro-spective study is getting under way to questionwhether brace treatment is better than no treat-ment at all, centers are reporting favorable results
in compliant patients treated with a brace fash-ioned by a skilled orthotist.
The aims of this issue of the Orthopedic Clinics
of North America were to identify several contro-versial and exciting aspects of scoliosis treatmentand to recruit nationally and internationally re-
nowned authorities to share their wisdom and
0030-5898/07/$ - see front matter � 2007 Elsevier Inc. All r
doi:10.1016/j.ocl.2007.07.004
recommendations on these topics. Contributingauthors include two past Scoliosis Research Soci-ety presidents, and several authors who will un-
doubtedly be future SRS presidents. It has beena privilege to work with the wonderful authorswho have contributed to this edition on scoliosis,
and I would like to acknowledge them and thankthem for their hard work and excellent articles.Deb Dellapena, the editor of this issue, has been
patient, encouraging, and a pleasure to work with.Finally, I would like to thank my familydLena,Haakon, AnnaSofia, and Brittadfor their pa-
tience and support through early-morning editingsessions.
Anthony A. Stans, MD
Division of Pediatric OrthopedicsDepartment of Orthopedic Surgery
Mayo Clinic
200 First Street SWRochester, MN 55905, USA
E-mail address: [email protected]
ights reserved.
orthopedic.theclinics.com

Orthop Clin N Am 38 (2007) 469–475
Advances in Scoliosis Brace Treatmentfor Adolescent Idiopathic Scoliosis
William J. Shaughnessy, MDDepartment of Orthopedic Surgery, Mayo Clinic and Mayo School of Medicine,
Rochester, MN 55905, USA
Brace treatment of adolescent idiopathic scoli-
osis remains an excellent option for skeletallyimmature individuals with scoliosis curve magni-tudes between 20� and 40�. Among options avail-
able for managing spinal disorders in children areobservation, bracing, and surgery. The use ofa spinal orthosis was first documented in thesixteenth century by Pare [1]. The lack of imaging
techniques and the absence of an understanding ofspinal growth led to unpredictable results withorthotic treatment until the second half of the
twentieth century [2,3]. As the natural history ofscoliosis and the effects of growth and develop-ment became better understood, the indications
for bracing narrowed considerably. Bracing issignificantly limited by such factors as neuromus-cular disease, skin insensitivity, spasticity, osteo-
porosis, and congenital spinal disorders. Despitethese limitations and with a more refined under-standing of treatment indications, brace treatmentcontinues to play an important role in the man-
agement of adolescent idiopathic scoliosis.The goal of brace treatment is to prevent curve
magnitude progression and to avoid the need for
surgical spinal arthrodesis. Surgery is indicated forCobb angles of greater than 45� to 50�. While othernonoperative treatments have been reported, none
have shown efficacy in treating adolescent idio-pathic scoliosis. Methods that have not shownsuccess include electrical stimulation, exercise,and manipulation [4].
Brace treatment is used to prevent curve pro-gression during growth. As such, orthotic treat-ment ends with skeletal maturity and is not useful
E-mail address: [email protected]
0030-5898/07/$ - see front matter � 2007 Elsevier Inc. All r
doi:10.1016/j.ocl.2007.07.002
in adults. The brace must allow continued growth
of the spine while simultaneously preventing thespinal deformity from becoming worse. It shouldbe assumed that scoliosis will not be cured by
brace treatment. An acceptable ‘‘brace result’’ isfor the deformity to be no worse at skeletalmaturity than when brace treatment started.
During the past 20 years there have been many
studies of brace treatment for adolescent idio-pathic scoliosis. In addition to the Milwaukeebrace, multiple variants of the thoracolumbar
sacral orthosis (TLSO) brace have been describedand reported on, each variant being named for thecity of its origin [5–21]. Most of these studies
support the effectiveness of bracing in preventingcurve progression and the subsequent need forsurgery [5,6,8–10,13,14,16–18,20,21]. Several stud-
ies have suggested that bracing may not be effec-tive [11,12,15,19,21]. While these studies do notshow brace efficacy, they have been helpful. Likeelectrical stimulation, ineffective bracing reveals
the natural history of scoliosis, so these studieshave helped to refine the natural history and indi-cations for successful bracing.
Natural history
Few studies have attempted to document thenatural history of progression in adolescentidiopathic scoliosis. To correctly judge the efficacy
of any treatment, some knowledge of the naturalhistory is necessary. Several studies have identifiedthe population at risk of progression [22–27]. This
includes those with curves of greater than 20� atthe time of peak adolescent skeletal growth,classically reported as Risser 0 or 1 maturity and
premenarchal to 1 year postmenarchal in females
ights reserved.
orthopedic.theclinics.com

470 SHAUGHNESSY
[25–27]. For this group at risk, Rogala and col-leagues [24] found progression among 79% of im-mature patients with curves between 20� and 30�.Bunnell [26] found progression of 5� or more in68% of those with a Risser sign of 0. Lonsteinand Carlson [27] reported the same 68% progres-sion rate of greater than 5� for curves of 20� to 29�
in those with a Risser sign of 0 or 1. Nachemsonand colleagues [18] performed a randomized, mul-ticenter study comparing brace treatment to ob-
servation in 10- to 15-year-old females withthoracic curves. The investigators documentedprogression of at least 6� in 66% of the observa-
tion group. The best available data show, there-fore, that 66% to 79% of immature females withcurves of 20� to 35� will progress more than 5�
if observed. Progression has been shown to be
greater for curves of larger magnitude and lessprobable for curves smaller than 20�, Risser 3,or greater maturity, and for females more than 1
year postmenarchal [27].It is not known what percentage of the at-risk
population would progress to surgery if left
untreated. The ultimate goal of brace treatmentis not so much to prevent 5� of progression as it isto prevent the need for surgery. Virtually all
studies, including those noted above, use curveprogression of more than 5�, rather than surgicalrates, as an endpoint. Unfortunately, none ofthese natural history studies followed untreated
patients to surgery or to curve magnitudes ofmore than 45�, when surgery would ordinarily berecommended. It can be reasonably assumed,
however, that this information can be gleanedfrom well-done brace studies with poorly compli-ant patients or ineffective braces. Such studies
suggest that 60% to 79% of immature femaleswith curves larger than 25� may progress tosurgery [28]. It can also be assumed that resultswith lower progression and surgical rates than
these indicate a beneficial treatment effect anddemonstrate the efficacy of brace treatment. Whilea randomized, blinded study would be helpful, the
ethical and logistical difficulty in performing sucha study may be insurmountable.
Indications for brace treatment
The results of bracing in early studies wereinconsistent because many individuals now knownto be at low risk for progression were included
[29]. These included patients with skeletal matu-rity at brace initiation and small curve magnitudesthat were not likely to progress. Some studies also
included individuals with large curve magnitudesand nonidiopathic curves, which are not likely torespond to brace treatment.
As the natural history of scoliosis becomesbetter understood, the identification of thosepatients at risk of progression becomes moreaccurate [27,30–32]. Patients at greatest risk of
progression, and therefore those most likely tobenefit from bracing, include growing children(Risser 0–2 and, if female, either premenarchal
or less than 1 year postmenarchal) with primarycurve magnitude of 25� to 40�. Patients with curvemagnitudes of between 20� and 25� with docu-
mented progression should also be consideredfor brace treatment [17,29].
Initiation of brace treatment involves fittingthe orthosis, obtaining a standing posterior-ante-
rior radiograph with the patient wearing thebrace, and increasing the number of hours in thebrace over the course of 1 to 2 weeks. It is impor-
tant that the curve magnitude on the first in-braceradiograph be less than 50% of the original,prebrace curve magnitude [8]. Time-in-brace is
increased 1 to 4 hours each day until full-timebrace wear is achieved. Full-time wear is pre-scribed initially for all patients, except those using
the Charleston and Providence nighttime bendingbraces. Patients are encouraged to be active insports and allowed to be out of the brace if thesport cannot be performed in the brace.
Decreased orthotic effectiveness in overweightpatients has been demonstrated and may bea contraindication to bracing. O’Neill and col-
leagues [33] showed that individuals with bodymass indices greater than the 85th percentilewere three times more likely to fail brace treat-
ment than those who were not overweight.Brace treatment is continued until growth is
completed. This is determined by a variety ofindicators: typically unchanged height measure-
ments on two successive dates 6 months apart,18 to 24 months postmenarchal, Risser 4 status, orskeletal maturity on bone-age determination.
Bracing results
The use of a brace for scoliosis is complex, inpart because success depends on more than just
the skill of the surgeon. Quite the contrary,bracing success depends also on the dedicationof the patient and family, the skill of the orthotist,
the efficacy of the brace, growth, compliance withwear, regular follow-up evaluations, and an envi-ronment that encourages the brace to be worn for

471ADVANCES IN SCOLIOSIS BRACE TREATMENT
what may be a prolonged period. Given thismultitude of factors affecting success, it is not atall surprising that the published results of bracingspan a continuum ranging from seemingly in-
effective to excellent.In general, most brace studies show a similar
trend of curve magnitude improvement in the
brace, followed by slow loss of correction until theend of brace treatment, when the curve is similarto that at the start of bracing [5,25,34,35]. Several
studies have also identified a trend of decreasingbrace efficacy with increasing curve size [8,17,28].
In most reported series, full-time Milwaukee
brace treatment produces better results thannatural history studies. Carr and Noonanreported failure rates requiring surgery in 39%and 42%, respectively [5,19]. While Noonan ques-
tioned the efficacy of brace treatment, surgicalrates among his patients were still considerablybetter than natural history studies and several
recent brace studies in the literature.In one of the most complete brace studies to
date, Lonstein and Winter [17] reported a 40%
rate of curve progression of more than 5� anda surgical rate of 22% in a study of Risser 0-to-1 Milwaukee brace patients. The majority of pa-
tients had prebrace curves between 20� and 39�.The investigators noted a significant difference be-tween the reported radiographic failure rate of40% and their own natural history study predict-
ing 68% progression. Others have reported on theuse of the Milwaukee brace, but the studies arelimited by incomplete follow-up, small numbers,
the inclusion of nonidiopathic scoliosis and pa-tients of ages now known to not benefit frombracing [34–36]. Patient self-image issues, non-
compliance, and dissatisfaction with the cosmeticappearance of the neck ring ultimately led to thedevelopment of underarm braces [37,38].
Underarm braces include a variety of devices
collectively known as TLSOs. In general, theresults of TLSO treatment are similar to theMilwaukee brace studies. Several series have
evaluated the results of such devices. Bassettand colleagues [39] studied a mixed populationof juvenile and adolescents with curves of 20� to39� treated with the Wilmington TLSO and found30% progressed 5� or more. Emans and col-leagues [8] reported 295 patients, 4 to 18 years
of age, treated with a Boston brace. Only 12%of patients required surgery, although the failurerate was greater for curves greater than 40�
when bracing was started. Emans also noted less
favorable results in noncompliant patients. More
recently, Spoonamore and colleagues [21]reported the results of a study using the Rose-nberger brace, a front-opening TLSO. The inves-tigators found 56% of their patients progressed
more than 5� and 31% required surgery or metsurgical criteria. While the investigators acknowl-edge that the Rosenberger brace is effective in
preventing radiographic and clinical failure insome, they noted failure in others. Compliancewith brace treatment was not reported. The inves-
tigators noted this as a possible explanation forthe unsatisfactory results. Compared with nearlyidentical brace studies showing progression and
surgical rates of 80%, however, the Rosenbergerbrace appears to produce good results. Thereasons for the disparity among bracing resultsare unknown, but different rates of brace compli-
ance are likely the major culprit.Driven largely by the desire of many patients to
avoid daytime and school-time bracing, nighttime-
only braces have been developed that require only8 to 10 hours of wear. The Charleston andProvidence braces use bending or aggressive mold-
ing to apply corrective forces to the spine [6,20].Several studies have reported the efficacy of thesetwo novel braces. D’Amato and colleagues [6]
found that only 21% of patients progressed usingthe Providence brace, provided the curve apexwas caudal to T8. Katz and colleagues [16] com-pared the Charleston to the Boston brace. Both
braces were more effective with smaller prebracecurves of 25� to 35� than with larger curves.More than 5� of progression was noted in 29%
and 47% of the Boston and Charleston groups re-spectively. With larger prebrace curves of 36� to45�, both braces did less well. The investigators
found greater than 5� of progression in 43% ofthe Boston group and 83% of the Charleston pa-tients. The investigators recommend the Bostonbrace for large curve magnitudes and those with
thoracic curves [16]. Again recognizing that pro-gression of 5� may be an arbitrary measure of brac-ing failure and that radiographic failure may not
indicate clinical failure, Gepstein and colleagues[10] found no difference in surgical rates betweenthe Charleston brace (11%) and a TLSO (13%).
Surgical rates for both braces, however, are wellbelow that expected from natural history studies.
The only published prospective controlled
brace study was performed by Nachemson andPeterson [18]. The investigators compared TLSObracing to observation in a group of 10- to 15-year-old (skeletal age) girls with idiopathic scolio-
sis and single curves between 25� and 35�. Only

472 SHAUGHNESSY
36% of the braced patients showed progression ofmore than 5�, compared with 66% in those ob-served. Using survival analysis, the TLSO was
found to be statistically effective in altering thenatural history (P!.0001). While the study is rou-tinely cited as clearly and dramatically demon-strating the effectiveness of bracing, it has been
criticized for not being randomized or blindedand for the inclusion of only single thoracic curvesof limited size, up to 35� [21].
Unfortunately, there are many problems withmost bracing studies in the literature. Juveniles,adolescents, and mature individuals are included.
Different curve types, magnitudes, and lengths offollow-up are reported. Nonidiopathic scoliosis isoccasionally included. Even the landmark studyby Nachemson has been criticized for including
thoracic curves and not including curves ofgreater than 35�. To assess the effectiveness ofeach orthosis and to compare one study to others
requires consistent study parameters. The Scolio-sis Research Society (SRS) has recently publisheda stringent, uniform set of inclusion criteria for
bracing studies [29]. The standards for adolescentidiopathic scoliosis brace studies include an age of10 years and older, Risser 0 to 2, primary curve
size of 25� to 40�, no prior treatment, and, iffemale, either premenarchal or less than 1 yearpostmenarchal. The SRS also defines progressionand sets standards for reporting curve patterns,
curve rotation, compliance, and follow-up. It isto be hoped that additional studies using theSRS criteria will allow for an objective compari-
son of future brace studies.The first and only published study using the
recent, strict SRS criteria is a comparison of the
TLSO to the Providence nighttime orthosis ata single institution [28]. The poor results for bothbraces raise interesting questions. In the TLSOgroup, 85% showed progression of more than 5�
and 79% of braced patients required surgery.For the Providence brace, 69% progressed and60% required surgery. The results are so similar
to natural history studies that it can be arguedthe brace programs cited are ineffective and thatthe study is a natural history study of adolescent
idiopathic scoliosis. Similar assumptions weremade for patients treated with electrical stimula-tion in the past, leading those so treated to be
included in ‘‘observation’’ rather than treatmentpopulations [18,27,40,41]. The investigatorsspeculate that the poor results might be due todemographics, genetics, referral patterns, or com-
pliance, but the reasons remain unknown. The
extreme variation in reported brace success ratessuggests that some braces and brace programsare very good and that others have no effect on
the natural history of adolescent idiopathic scolio-sis. Further study is necessary to determine whyone center reports a surgical rate of 79% andanother 22%.
Bracing in males
Brace treatment in boys may not be as success-
ful as in girls. For boys willing to wear anorthosis, however, brace treatment can be success-ful. Most studies of scoliosis orthosis treatment
include both males and females, but the numberof males is small, statistical power is lacking, andthe results are difficult to interpret. Karol [15]
reported that brace treatment in males was inef-fective largely because of poor compliance. Arecent study confirmed the decreased compliance
in males when compared with females but foundbracing useful in both genders, with progressionof more than 5� in 31% of the compliant malesand 21% of the compliant females [42]. Both
results are two to three times better than expectedfrom natural history and other brace studies.
Compliance
As with other medical treatments, successdepends upon treatment actually being per-
formed. In the case of bracing for adolescentidiopathic scoliosis, it is often incorrectly assumedthat brace patients are compliant with their
treatment. In fact, compliance with bracing mayrun the range from absolute nonuse to full-timebracing. The experience of wearing a brace full-
time is substantially different, and more obviousto others, than that of taking daily medication oradhering to a diet. Unlike other orthopedic
surgical treatments, such as surgery, braces areaccessible and easily removed by the patient. Poorcompliance is not surprising given the negativeeffects of bracing on self-image [37]. Those who do
not wear their braces should be expected to haveresults similar to natural history studies. Compli-ant patients are likely to show the best results
and the most significant difference when com-pared with natural history. Given this reality,compliance is a major determinant of bracing
success. Compliance may explain the differencebetween brace treatment results in males andthose in females [15,42].

473ADVANCES IN SCOLIOSIS BRACE TREATMENT
Compliance, the ability of the patient to weara brace for the prescribed time, has a dramaticeffect on brace treatment effectiveness. Emans andcolleagues [8] noted poor results for noncompliant
patients in his Boston brace study. Wiley and col-leagues [43] also found that brace wear of morethan 18 hours per day led to less progression
than if the brace was worn 12 hours per day orless. In contrast, Allington and Bowen [44] foundno difference between full-time and part-time
bracing using the Wilmington brace.Until recently, compliance was difficult to
measure and often relied upon patient or parent
self-reporting. With the availability of pressuretransducers and temperature sensor loggers,reliable brace wear records may be recorded.Using instrumented braces, several studies have
determined that brace wear varies from 8% to90% of the prescribed time, averaging only 65%to 75% of the time prescribed [45,46]. Patients and
parents over-reported their hours of brace wear by150%. Additionally, there was an inverse correla-tion between age and compliance. Ten-year-olds
wore their braces 84% of the prescribed timecompared with only 77% for 12-year-old patientsand 60% for 14-year old patients.
Rahman and colleagues [47] reported on the as-sociation between brace compliance and outcomesusing a temperature sensor and data logger in Wil-mington TLSO braces. The investigators found
strikingdifferences between the compliant andnon-compliant patients. Among those with radio-graphic progression more than 5�, patients wore
their braces only 62% of the time prescribed. Forthose who did not progress, compliance was better,logging 85% of the prescribed time (P¼.004).Additionally, in those who wore their brace morethan 90% of the time prescribed, progression ofmore than 5� was seen in only 11%, better thanany other group in the literature. The results indi-
cate that those who are compliant with brace treat-ment have significantly more favorable outcomes.
Factors affecting brace compliance are not well
understood and have not been adequately studied.The role of the treating physician, orthotist, andparents require additional attention. Finally, while
the SRS has recommended that all noncompliantbrace patients be included in further brace studies,it will be important to distinguish between brace
failure, and failure of the patient or brace programtouse the brace. There is a tendency to label bracingas ‘‘ineffective’’ when noncompliant patients raisethe average radiographic progression rates in some
studies. Similar standards are not routinely applied
elsewhere in medicine or in orthopedics. As anexample, patients who refuse antibiotics for thetreatment of osteomyelitis are not usually includedin studies of antibiotic efficacy, nor are they cited as
‘‘failures’’ of drug treatment. While it is useful toknow how often brace patients wear their orthosis,the question that physicians, patients, and parents
want to know is, ‘‘If this brace is worn,what will theback look like and can surgery be avoided?’’
Summary
Brace treatment is the treatment of choice forsome, but not all, patients with adolescent idio-
pathic scoliosis. Indications for bracing includecurve magnitudes of 20� to 40� in growingindividuals with Risser 0 to 2 skeletal maturation
and, if female, either premenarchal or less-than-1-year postmenarchal status. Natural history andbrace studies suggest that 68% to 79% of these
individuals show progression of their scoliosis andsimilar numbers require surgery if untreated. Incontrast, those that are compliant with bracetreatment show radiographic progression of
more than 5� in just 11% and rarely requiresurgery. The importance of wearing the bracedso-called ‘‘compliance’’dcannot be overstated.
Poor compliance is the most likely source ofmany poor bracing results but it is difficult tomeasure as patients and their parents routinely
report more brace time than they actually achieve.Bracing is less effective in obese patients and in
those with curve magnitudes greater than 40�.Bracing is not effective in skeletally mature
individuals or in those with nonidiopathic scolio-sis. Good results have been reported with Mil-waukee, TLSO, and bending braces.
Successful brace treatment prevents radio-graphic progression of scoliosis and avoids theneed for spine surgery. In general, if brace
treatment is not effective for a patient or groupof patients, one or more of the following problemsis likely present:
The brace does not fit or is not effective.The patient is not wearing the brace.
The time-in-brace is insufficient.The diagnosis is incorrect.
It becomes the role of the treating physicianand orthotic specialist to sort these issues out andto make appropriate changes.
Brace treatment is a team activity that requiresthe active, willing participation of the prescribingphysician, orthotist, patient, family, and friends.

474 SHAUGHNESSY
If the physician does not prescribe and follow up,if the orthotist does not properly fit the brace, ifthe patient does not wear the brace, and if the
family and friends are not supportive, the treat-ment will not be effective. The literature discus-sion about ‘‘bracing efficacy’’ assigns far too muchcredit or blame to the orthosis and not nearly
enough responsibility to those involved with theprescribing, manufacturing, and, most impor-tantly, the wearing of the brace.
References
[1] Pare A. Opera ambrosil parei. Paris: Apud Jacobum
Dupuys; 1582 [in French].
[2] Arkin AM. Correction of structural changes in
scoliosis by corrective plaster jackets and prolonged
recumbency. J Bone Joint Surg Am 1964;46:33–54.
[3] Barr JS, Buschenfeldt K. Turnbuckel brace: 3 point
pressure brace for corrective treatment of ambulatory
cases of scoliosis. J Bone Joint Surg 1936;18:760–5.
[4] Lonstein J, Wilson S, Beattie C. Results of stimula-
tor treatment of 332 cases of adolescent idiopathic
scoliosis. Orthopaedic Transactions 1989;13:92.
[5] Carr WA, Moe JH, Winter RB, et al. Treatment of
idiopathic scoliosis in the Milwaukee brace. Long
term results. J Bone Joint SurgAm 1980;62:599–612.
[6] D’Amato CR, Griggs S, McCoy B. Nighttime brac-
ing with the Providence brace in adolescent girls with
idiopathic scoliosis. Spine 2001;26:2006–12.
[7] DanielssonAJ, Nachemson AL. Radiologic findings
and curve progression 22 years after treatment for
AIS: comparison of brace and surgical treatment
with matching control group of straight individuals.
Spine 2001;26:516–25.
[8] Emans JB, Kaelin A, Bancel P, et al. The Boston
bracing system for idiopathic scoliosis. Follow-up
results in 295 patients. Spine 1986;11:792–801.
[9] Gabos PG, Bojescul JA, Bowen JR, et al. Long-term
follow-up of female patients with idiopathic scoliosis
treated with the Wilmington orthosis. J Bone Joint
Surg Am 2004;86:1891–9.
[10] Gepstein R, Leitner Y, Zohar E, et al. Effectiveness
of the Charleston bending brace in the treatment of
single-curve idiopathic scoliosis. J Pediatr Orthop
2002;22:84–7.
[11] Goldberg CJ, Dowling FE, Hall JE, et al. A statisti-
cal comparison between natural history of AIS and
brace treatment in skeletally immature adolescent
girls. Spine 1993;18:902–8.
[12] Goldberg CJ, Moore DP, Fogarty EE, et al. AIS.
The effect of brace treatment on the incidence of
surgery. Spine 2001;26:42–7.
[13] Green NE. Part-time bracing of AIS. J Bone Joint
Surg Am 1986;68:738–42.
[14] Howard A, Wright JG, Hedden D. A comparative
study of TLSO, Charleston, and Milwaukee braces
for idiopathic scoliosis. Spine 1998;23:2404–11.
[15] Karol LA. Effectiveness of bracing in male patients
with idiopathic scoliosis. Spine 2001;26:2001–5.
[16] Katz DE, Richards BS, Browne RH, et al. A com-
parison between the Boston brace and the Charles-
ton bending brace in AIS. Spine 1997;22:1302–12.
[17] Lonstein JE,WinterRB.TheMilwaukeebrace for the
treatment of AIS. A review of one thousand twenty
patients. J Bone Joint Surg Am 1994;76:1207–21.
[18] Nachemson AL, Peterson LE, members of Brace
Study Group of the SRS. Effectiveness of treatment
with a brace in girls who have AIS. J Bone Joint Surg
Am 1995;77:815–22.
[19] Noonan KJ, Weinstein SL, JacobsonWC, et al. Use
of the Milwaukee brace for progressive idiopathic
scoliosis. J Bone Joint Surg Am 1996;78:557–61.
[20] Price CT, Scott DS, Reed FR, et al. Nighttime brac-
ing for AIS with the Charleston bending brace: long-
term follow-up. JPO J Pract Orthod 1997;17:703–7.
[21] Spoonamore MJ, Dolan LA, Weinstein SL. Use of
the Rosenberger brace in the treatment of progres-
sive AIS. Spine 2004;29:1458–64.
[22] Duval-BeaupereG. Pathogenic relationship between
scoliosis and growth. In: Zorab PA, editor. Scoliosis
and growth. Edinburgh (UK): Churchill Living-
stone; 1971. p. 58–64.
[23] Brooks HL, Azen SP, Gerberg E, et al. Scoliosis:
a prospective epidemiological study. J Bone Joint
Surg Am 1975;57:968–72.
[24] Rogala EJ, Drummond DS, Gurr J. Scoliosis: inci-
dence and natural history. A prospective epidemio-
logical study. J Bone Joint Surg Am 1978;60:173–6.
[25] Fustier T. Evolution radiologique spontanee des
scolioses idiopathiques de moins de 45 degrees en
periode de croissance. Etude graphique retrospective
de cent dossiers du Centre de readaptation fonction-
nelle des Massues. [Thesis]. Universitie Claude-Ber-
nard, Lyon, France. 1980.
[26] Bunnell WP. The natural history of idiopathic scoli-
osis before skeletal maturity. Spine 1986;11:773–6.
[27] Lonstein JE, Carlson JM. The prediction of curve
progression in untreated idiopathic scoliosis during
growth. J Bone Joint Surg Am 1984;66:1061–71.
[28] Janicki JA, Poe-Kochert C, Armstrong DG, et al. A
comparison of the thoracolumbosacral orthosis and
Providence orthosis in the treatment of adolescent
idiopathic scoliosis: results using the new SRS inclu-
sion and assessment criteria for bracing studies.
J Pediatr Orthop 2007;27:369–74.
[29] Richards BS, Bernstein RM, D’Amato CR, et al.
Standardization of criteria for adolescent idiopathic
scoliosis brace studies. Spine 2005;30:2068–75.
[30] Bunnell WP. The natural history of idiopathic scoli-
osis. Clin Orthop Relat Res 1988;229:20–5.
[31] Lonstein JE. Natural history and school screening
for scoliosis.OrthopClinNorthAm1988;19:227–37.
[32] Peterson LE,NachemsonAL. Prediction of progres-
sion of the curve in girls who have adolescent idio-
pathic scoliosis of moderate severity. J Bone Joint
Surg Am 1995;77:823–7.

475ADVANCES IN SCOLIOSIS BRACE TREATMENT
[33] O’Neill PJ, Karol LA, Shindle MK, et al. Decreased
orthotic effectiveness in overweight patients with
adolescent idiopathic scoliosis. J Bone Joint Surg
Am 2005;87:1069–74.
[34] Keiser RP, Shufflebarger HL. The Milwaukee brace
in idiopathic scoliosis. Evaluation of 123 completed
cases. Clin Orthop Relat Res 1976;118:19–24.
[35] Mellencamp DD, Blount WP, Anderson AJ. Mil-
waukee brace treatment of idiopathic scoliosis.
Late results. Clin Orthop Relat Res 1977;126:47–57.
[36] Edmonsson AS, Morris JT. Follow-up study of Mil-
waukee brace treatment in patients with idiopathic
scoliosis. Clin Orthop Relat Res 1977;126:58–61.
[37] Clayson D, Luz-Alterman S, Cataletto MM, et al.
Long-term psychological sequelae of surgically versus
nonsurgically treated scoliosis. Spine 1987;12:983–6.
[38] Fallstrom K, Cochran T, Nachemson A. Long-term
effects on personality development in patients with
adolescent idiopathic scoliosis. Influence of type of
treatment. Spine 1986;11:756–8.
[39] Bassett G, Bunnell W, MacEwen G. Treatment of
idiopathic scoliosis with the Wilmington brace.
Results in patients with a twenty to thirty-nine
degree curve. J Bone Joint Surg Am 1986;68:602–5.
[40] Akbarnia B, Keppler L. Lateral electrical surface
stimulation for the treatment of adolescent idio-
pathic scoliosis. Analysis based on progression
risk. J Pediatr Orthop 1986;6:369–70.
[41] Sullivan JA, Davidson R, Renshaw TS, et al. Fur-
ther evaluation of the scolitron treatment of idio-
pathic adolescent scoliosis. Spine 1986;11:903–6.
[42] Yrjonen T, Ylikoski M, Schlenzka D, et al. Results
of brace treatment of adolescent idiopathic scoliosis
in boys compared with girls: a retrospective study of
102 patients treated with the Boston brace. Eur
Spine J 2007;16:393–7.
[43] Wiley JW, Thomson JD, Mitchell TM, et al. Effec-
tiveness of the Boston brace in treatment of large
curves in adolescent idiopathic scoliosis. Spine
2000;25:2326–32.
[44] Allington NJ, Bowen JR. Adolescent idiopathic
scoliosis: treatment with the Wilmington brace. A
comparison of full-time and part-time use. J Bone
Joint Surg Am 1996;78:1056–62.
[45] Takkemitsu M, Bowen JR, Rahman T, et al.
Compliance monitoring of brace treatment for pa-
tients with idiopathic scoliosis. Spine 2004;29:
2070–4.
[46] Nicholson GP, Ferguson-Pell MW, Smith K, et al.
The objective measurement of spinal orthosis use
for the treatment of adolescent idiopathic scoliosis.
Spine 2003;28:2243–50.
[47] Rahman T, Bowen JR, Takemitsu M, et al. The
association between brace compliance and outcome
for patients with idiopathic scoliosis. J Pediatr
Orthop 2005;25:420–2.

Orthop Clin N Am 38 (2007) 477–484
Casting and Traction TreatmentMethods for Scoliosis
Jacques L. D’Astous, MD, FRCS(C)a,b,*, James O. Sanders, MDc
aDepartment of Orthopaedic Surgery, University of Utah Orthopaedic Center, 590 Wakara Way,
Salt Lake City, UT 84108, USAbShriners Hospitals for Children – Intermountain, Fairfax Road & Virginia Street,
Salt Lake City, UT 84103, USAcShriners Hospitals for Children, 1645 West 8th Street, Erie, PA 16505, USA
Casting for infantile or early-onset scoliosis
Casting for scoliosis was common until PaulHarrington introduced effective spinal instrumen-tation. Since then, casting largely has been rele-gated to history books along with racks, corsets,
and other medieval implements. As its role di-minished, knowledge of casting techniques dis-appeared, experienced surgeons passed on, and
the remaining historic relicsdcasting tablesdfellinto disuse and were discarded.
To a large degree, the abandonment of casting
is justified. Instrumentation is now solid andsecure, provides excellent curve correction, andallows rapid mobilization and return to activity. A
rigid cast can create pressure sores, significant ribor mandibular deformities, and constrict thechest. The historical term for superior mesentericartery syndrome is ‘‘cast syndrome.’’ Many of
these problems seem to be the result of indiscrim-inate casting of all types of scoliosis and impropertechnique combined with a limited understanding
of spinal, and, particularly, chest wall deformities.We have used serial casting in a small group of
our patients for several years, and our early results
indicate that in selected patients and with propertechnique, casting plays a useful role in ourtreatment armamentarium for early-onset scoliosis.
* Corresponding author. Shriners Hospitals for
Children – Intermountain, Fairfax Road & Virginia
Street, Salt Lake City, UT 84103.
E-mail address: [email protected]
(J.L. D’Astous).
0030-5898/07/$ - see front matter � 2007 Elsevier Inc. All r
doi:10.1016/j.ocl.2007.03.006
With few exceptions, we have confined scolio-
sis casting to patients who had infantile scoliosisand do not believe it has a role in adolescent,neuromuscular, or congenital scoliosis with therare indications for postoperative stabilization,
temporary correction, or immobilization to assesspain relief.
Scoliosis casting comes in several varieties. The
most commonly used method in the United States isthat of Risser [1]. Indeed, body casting in this coun-try often is called Risser casting. Risser developed
two types of casts. The initial method used turn-buckles, whereas the latter, termed a localizer cast,used a three-point mold and a pusher. Although it
is possible to obtain significant curve correctionwith this technique, it does not account sufficientlyfor rotational abnormality, and, especially in youn-ger children with flexible bones, it can cause signifi-
cant rib deformities and chest constriction.Scoliosis in young children has two classifica-
tions. The traditional classification used by the
Scoliosis Research Society divides these curves intoinfantile and juvenile, based on whether the curvewas diagnosedbefore or after the ageof 3 years. The
classification of Dickson [2] divides curves intoearly onset (diagnosed before age 5 years) and lateonset (diagnosed after age 5 years). Dickson’s logicwas that curves occurring after age 5 years were less
likely to result in pulmonary failure. We prefer theformer classification because of Pehrsson and col-leagues’ [3] work showing increased mortality in
the infantile and juvenile curves and because youn-ger age of treatment, in our experience, seems toimprove the results.
ights reserved.
orthopedic.theclinics.com

478 D’ASTOUS & SANDERS
Infantile idiopathic scoliosis occurs in twobasic types: resolving and progressive. Mehta [4]was able to distinguish resolving scoliosis from
progressive scoliosis by using the rib vertebral an-gle difference (RVAD) on an early supine radio-graph. The RVAD nearly follows the 80/20 rule:80% of curves with an RVAD of 20 or more con-
tinue to progress, whereas only 20% of those withlesser angles progress. This was confirmed byother investigators [5–7].
More recently,Mehta [8] described her results ofcasting in 136 patients who had infantile scoliosisusing the technique of Cotrel and Morel [9] with
the philosophy that early rapid growth, if guidedby the cast, would assist an initially curved spineto straighten. She grouped her patients into fourphysiologic patterns: a ‘‘sturdy phenotype’’ with
goodmuscle mass and tone; a ‘‘slender phenotype’’withmore delicate features, ligamentous laxity, andmore rapidly progressive curves; those with known
syndromes; and those with unknown syndromes.Her program consisted of cast changes under anes-thesia in younger patients every 8 to 16 weeks until
the curvewas nearly resolved followed by an under-arm brace that may be weaned if the patient’s curvecorrection continues. Treatment was related to the
patient’s phenotype; the sturdy patients respondedthebest, followedby the slender phenotype, andpa-tients with unknown syndromes responded theworst. Even more important was the age at treat-
ment onset. Casting resulted in full correction in94 patients, whereas 42 had only partial correction.Treatment was much more likely to be successful if
started before the age of 2 years.Dr. James Sanders learned the basic Cotrel
technique fromDr.Albert Sanders andbeganusing
it on several patients presenting with progressiveinfantile scoliosis. The technique was developedfurther in conjunction with Dr. Jacques D’Astousat the Salt Lake City Shriners Hospital through
study and personal instruction by Min Mehta. Atthe Erie Shriners Hospital, working with Dr. JoeKhoury and an excellent casting team, the tech-
nique has become effective and reproducible.The first requirement is a proper casting table.
Some hospitals still have vintage Risser or Cotrel
tables, although they are a rarity. Although weinitially worked on aRisser frame, the Risser frameis large for a small child. We are indebted to Min
Mehta for her design of a smaller, practical framethat leaves the head, arms, and legs supported butthe body free.
We have identified a few principles that we
believe help to create a better cast (Box 1).
We have a routine of doing the initial casts at 2-month intervals with a schedule based upon howfast the child is growing. Typically, casts are
changed every 2 months for those aged 2 yearsand younger, every 3months for those aged 3 years,and every 4 months for those aged 4 years andolder. It is particularly helpful to be accommodat-
ing for the families’s busy schedules when bookinga date for the casting.We do not knowwhen to stopcasting, but have aimed for curves nearing 10� andthen proceed with brace fitting. Occasionally, chil-dren are given a brace during the summer monthswith resumption of casting in the fall.
Our early results show significant promise withthe typical left thoracic infantile curve being themost likely to respond; however, we lack compar-ison with other treatment modalities (eg, bracing,
growing rods, or the Vertical Expandable Pros-thetic Titanium Rib [VEPTR, SYNTHES Spine,Paoli, PA]), and still requires longer follow-upprior
to arriving at any definitive conclusions. As Fig. 5shows, most patients have a significant response,particularly younger ones. The most significant
failure is a girl who has Prader-Willi syndromeand a stiff double thoracic curve. Until we have fur-ther follow-up, we cannot distinguish those pa-
tients who are most likely to respond from thosewho are likely to fail serial casting, although Meh-ta’s finding that younger children respond bettercorresponds with our experience. (Fig. 6)
Traction in early-onset scoliosis
‘‘Despite the fact that traction is rarely usedtoday, it does remain an important option for thetreatment of children with spinal disorders’’ [10].
Halo-gravity traction can restore coronal andsagittal balance in severely decompensated curvesand may decrease the neurologic risks associatedwith the surgical correction of these severe de-
formities, be it by casting, subcutaneous rods,VEPTR, or definitive instrumentation and fusion.Patients who have severe spinal deformities and
secondary cor pulmonalemay benefit fromaperiodof preoperative traction to allow aggressive pul-monary toilet. Improvements in vital capacity,
arterial blood gases, and right heart failure maydecrease postoperative complications and can helpwith patient selection in difficult cases [11–13].
Historical background
Traction is one of the oldest methods forcorrection of spinal deformity, going back to

479CASTING AND TRACTION TREATMENT FOR SCOLIOSIS
Box 1. Guidelines for applying an effective cast
One must have a casting table that stabilizes the body for the anesthesiologist whilepositioning the trunk and extremities for effective casting.
Light head halter and pelvic traction assist in stabilizing the patient and in narrowing thebody (Fig. 1).
A mirror slanted under the table is useful for visualizing the gibbus, the posterior cast, andthe molds (Fig. 2).
Traction should not be large. Although traction can correct the curve while applied, theposition cannot be retained in the cast once traction is released and the body recoils. Thepurpose of traction is to align the trunk and narrow the torso slightly for good cast fitting.
Proper casting requires an excellent purchase on the pelvis. Without this basic foundation,the cast will slip, create sores, and fail to support the curve.
Only a small amount of padding is necessary with a well-fitting cast. Mehta uses directplaster over crepe paper on the skin with occasional felt pads for significant bonyprominences, but we use a thin layer of webril over a silver-impregnated body shirt inaddition to thin layers of felt on significant bony prominences.
If there is a lumbar curve, we believe that flexion of the hips to decrease lumbar lordosisfacilitates curve correction.
The cast must not push the ribs toward the spine and narrow the space available for the lung.Rather, the posteriorly rotated ribs must be moved anteriorly to create a more normalchest configuration (Fig. 3). Counterrotation is applied through the pelvic mold and uppertorso or shoulders.
The original Cotrel/Morel technique uses rotational straps to obtain correction. In mostyoung children, using one’s hands works well, but we use the straps in more difficultcurves, particularly of the lumbar spine.
Although the Cotrel/Morel technique and Mehta’s modifications use an over-the-shouldercast, we have had excellent success staying below the shoulders because most infantilecurves have low apices, typically at T10 to T11.
Finally, well-positioned anterior and posterior windows are helpful in dynamic curvecorrection and cast comfort (Fig. 4).
Fig. 1. A proper casting table provides good patient sta-
bility with support of the head and lower extremities, full
access to the torso, and the ability to provide light
traction.
Fig. 2. Rotational correction occurs by rotating the rib
or lumbar prominence anteriorly while providing coun-
terrotation through the pelvis and upper torso or shoul-
ders. A slanted mirror is helpful in applying correct
molds.

480 D’ASTOUS & SANDERS
Hippocrates and possibly even earlier. Sayre de-
scribed gravity-assisted traction before applica-tion of a corrective plaster cast for scoliosis in1876. Harrington, in the 1950s, devised a form of
‘‘internal traction,’’ the Harrington rod to obtainand maintain correction of the scoliosis. In 1959,Nickel and Perry designed the halo device tostabilize the cervical spine in patients undergoing
cervical spine fusion. Cotrel introduced the
Fig. 3. The correct anterior rotation done manually or
with wide straps over the prominence. Forces applied
laterally will cause significant rib and chest deformity
and must be avoided.
Fig. 4. (A) The anterior window allows chest and ab-
dominal space while capturing the anterior ribs to pre-
vent their deformity. (B) The posterior window on the
concavity allows the curve to settle into the defect and
improve the rotation. The window does not cross the
midline.
concept of dynamic traction in 1960 to treatadolescent idiopathic scoliosis and loosen up rigid
curves before surgery. Kane devised halo-femoraltraction in 1967, whereas Stagnara is credited forthe introduction of halo-gravity traction in 1969.
In the early 1990s, Dubousset combined Stagna-ra’s elongation turnbuckle cast with halo-gravitytraction. He believed that this was the best way
of obtaining correction in a rigid early-onsetscoliosis; to maintain the correction, he used a cus-tom-fabricated modular, hard plastic adjustable
cervicothoracolumbosacral orthosis called ‘‘corsetGarchois’’ (Jean Dubousset, MD, personal com-munication, 1999).
Biomechanics
The spine is a complex structure composed of
vertebrae, ligaments, and intervertebral discs;biomechanically, it behaves as a viscoelastic ma-terial with a reproducible stress/strain curve. The
soft tissues undergo ‘‘creep’’ deformation whencontinuous traction is applied, and this leads togradual correction of the spinal deformity with
realignment of the coronal and sagittal balance[12]. From the work of White and Panjabi, weknow that transverses forces are effective forcurves less than 50�, whereas traction forces are
more effective for curves greater than 50�. A com-bination of axial traction and transverse forceswas the most effective means of correction for
small and large curves [14]. Casting, bracing, orsurgery is required to maintain the correction.
Techniques
Halo-femoral and halo-pelvic traction have
been used for the treatment of severe scoliosis.Head halter–pelvic traction is used for the initialtraction radiograph to assess the flexibility of the
Fig. 5. Early results with cast treatment.

481CASTING AND TRACTION TREATMENT FOR SCOLIOSIS
Fig. 6. Younger patients seem to have a better response than older children. (A) Eight-month-old girl who has infantile
idiopathic scoliosis just before the start of casting, T6–L1 51�, rib phase 2, RVAD 40�. (B) Radiograph showing the cor-
rection in the second cast. (C) The same patient at age 3 years with scoliosis completely corrected; careful follow-up is
still required.
scoliosis/kyphosis and again during the applica-
tion of the Risser cast. The discussion is limited tohalo-gravity traction because this is the mostcommon type of traction used in our patients
who have early-onset scoliosis.Axial skeletal traction to the spine may be
applied by a halo. In children younger than 2years of age, because of their thin calvarium, 10 to
12 pins should be used, and the torque should notexceed 2 inch-pounds or finger tightness [15].Multiple pins (6–8 pins) should be used in older
children, and 6 to 8 inch-pounds of torque are ap-plied. The pins are placed under general anesthe-sia if the child’s overall condition allows. It is not
necessary to shave the scalp or make a skin inci-sion. The skin and subcutaneous tissues are infil-trated with 1% xylocaine with epinephrine. The
anterior pin is placed 1 cm above the eyebrowsor between the supraciliary ridge and the frontalprominence. It is important to avoid the anteriorfrontal sinus with the most medial pin. Placement
too medially also can cause supraorbital or sup-ratrochlear nerve damage. Placement too farlaterally (behind the hairline) impinges on the
temporalis and masseter muscles, leading to possi-ble skull penetration and difficulty with mastica-tion. The posterior pin is placed 1 cm above and
posterior to the pinna, below the equator of theskull. The proper ring size allows 1 to 2 cm ofclearance between the skin and halo. This
alleviates problems caused by edema and facili-
tates proper pin care. The screws should be 180�
opposite from each other whenever possible.The pins should be retightened once at 24 hours
after halo application. Further tightening is dan-gerous, possibly leading to skull penetration.The exact method of pin care is less importantthan meticulous daily attention, taking care to re-
move all encrusted material and to examine forerythema or drainage. The pins are cleansedonce a day with half-strength hydrogen peroxide
or plain soap and water. Pins should be replacedif erythema and drainage do not improve withmeticulous pin care or oral antibiotics. The hair
and scalp should be washed at least once a week.Stagnara [16] is credited with the development
of halo-gravity traction; it is the mostly widely
used method of halo traction. This method usesthe patient’s own body weight as countertraction.Depending on the child’s size, 3 to 5 pounds is ap-plied, with daily additions of 1 to 2 pounds to
a maximum of 30% to 50% of body weight. Dur-ing the day, countertraction may be obtained bythe use of a wheelchair or walker. At night, we
use a bed in maximum reverse Trendelenburg po-sition, with blocks to elevate the head of the bed,which provides a 45� incline (Fig. 7). Alterna-
tively, a pelvic sling or a Circoelectric bed canbe used. This method allows the child to be up-right during the day, preventing decubiti and

482 D’ASTOUS & SANDERS
osteopenia and promoting renal drainage. It has
been used safely in children younger than 2 yearsof age. If a wheelchair is used, it may be necessaryto place counterweights on the footrests to pre-
vent tipping backward (Fig. 8). Halo-walker trac-tion is used to allow ambulation in traction(Fig. 9). We have not found it necessary to usea spring scale for traction as described by Sink
and colleagues [12], although it may act as a safetymechanism against excessive traction forces.
Fig. 8. Halo wheelchair.
Fig. 7. Bed in maximum reverse Trendelenburg
position.
Indications
Our indications for the use of halo-gravitytraction in early-onset scoliosis are early-onsetscoliosis greater than 80�, scoliosis associated with
kyphosis, and to ‘‘loosen up’’ the scoliosis andkyphosis before VEPTR or subcutaneous rodimplantation, because both of these methods arekyphogenic and are mechanically disadvantaged
in the presence of kyphosis.
Contraindications
Relative contraindications to halo-gravity trac-tion include short sharp rigid kyphosis, C-spine
abnormalities or instability because of their obvi-ous neurologic implications, cranial defects orthin skull, and age younger than 18 months
because of pin penetration problems.
Complications
Several complications have been associatedwith the use of halo-gravity traction; the mostcommon one in our series is pain and weakness of
neck musculature. Other complications includepin tract infections, pin loosening, and cranialnerve palsy (abducens, oculomotor, glossophar-
yngeal, hypoglossal). It is important to ask aboutdouble vision, difficulty swallowing, voice hoarse-ness, and tongue weakness. The cause of cranial
nerve symptoms is believed to be the result ofstretching or kinking of the nerve. Alternatively,an interference with the blood supply to the nerves
Fig. 9. Halo-walker traction is used to allow ambulation
in traction.

483CASTING AND TRACTION TREATMENT FOR SCOLIOSIS
Fig. 10. A 3-year-old girl who had severe early-onset kyphoscoliosis. Halo-gravity traction improved the coronal and
sagittal balance and decreased the kyphosis, allowing the use of a VEPTR device to maintain the correction.
secondary to traction may lead to cranial nerve
palsy. Other reported complications include skullpenetration and brain or epidural abscess, para-plegia, paraparesis, brachial plexus palsy, superior
mesenteric artery syndrome, and avascular necro-sis of the odontoid [17–20].
Practical advice
A thorough hair wash with shampoo is done thenight before surgery. If the patient has long hair, itshould be braided. Keep a chart at the bedside todocument the patient’s weight; chart the amount
of weight on bed traction and chair traction, andnote all increases in weight. Perform a quick neuro-logic examination and repeat at 2, 4, and 8 hours af-
ter increasing the traction weights.
Case example
A 3-year-old girl presented with severe early-
onset kyphoscoliosis. Halo-gravity traction im-proved the coronal and sagittal balance anddecreased the kyphosis, allowing the use ofa VEPTR device to maintain the correction
(Fig. 10) until the definitive fusion and instrumen-tation are undertaken.
Summary
The presence of a significant spinal deformity
in an infant or toddler with several years ofgrowth remaining has the potential to producea severe deformity with significant cardiopulmo-
nary consequences. We present alternative, albeitlabor-intensive, modalities to bracing, subcutane-ous rods, and VEPTR instrumentation. In milder
cases and if started before 2 years of age, casting
may correct the deformity completely, whereas inmore severe cases, it allows the child to grow,minimizing spinal and chest wall deformities, until
he/she is old enough to undergo definitive treat-ment of the spinal deformity.
Acknowledgments
In addition to Dr Sanders, casting in Erie hasbeen done by Drs. Joseph Khoury and Shyam
Kishan. We are indebted to them for theirassistance and insights. Marcie Fitzgerald PA,has been instrumental in helping us track our
early results in these patients. For the most part,the casting at Intermountain was done by Dr.D’Astous and Michael Pond, PA. We would like
to recognize Michael Pond, without whose enthu-siasm and multiple talents this work would havebeen near impossible. Finally, we thank RobertEldridge, CPO, who designed and built our
casting table and Matt Lowell, PT and theorthotic team who adapted the chairs, walkers,and beds for halo-traction.
References
[1] Risser JC. Scoliosis treated by cast correction and
spine fusion. Clin Orthop Relat Res 1976;116:86–94.
[2] Dickson RA. Early-onset idiopathic scoliosis. In:
Weinstein SL, editor. 1st edition. The pediatric
spine: principles and practice, vol 1. New York:
Raven Press, Ltd; 1994. p. 421–9.
[3] Pehrsson K, Larsson S, Oden A, et al. Long-term
follow-up of patients with untreated scoliosis. A
study of mortality, causes of death, and symptoms.
Spine 1992;17(9):1091–6.

484 D’ASTOUS & SANDERS
[4] MehtaMH. The rib-vertebral angle in the early diag-
nosis between resolving and progressive infantile
idiopathic scoliosis. J Bone Surg Br 1972;54:230–42.
[5] Ceballos T, Ferrer-Torrelles M, Castillo F, et al.
Prognosis in infantile idiopathic scoliosis. J Bone
Joint Surg Am 1980;62(6):863–75.
[6] Ferreira JH, Janeiro R, de James JI. Progressive and
resolving infantile idiopathic scoliosis. The differen-
tial diagnosis. J Bone Joint Surg Br 1972;54(4):
648–55.
[7] Thompson SK, Bentley G. Prognosis in infantile id-
iopathic scoliosis. J Bone Joint Surg Br 1980;62(2):
151–4.
[8] MehtaMH.Growth as a corrective force in the early
treatment of progressive infantile scoliosis. J Bone
Joint Surg Br 2005;87(9):1237–47.
[9] Cotrel Y, Morel G. [The elongation-derotation-flex-
ion technic in the correction of scoliosis]. Rev
Chir OrthopReparatrice ApparMot 1964;50:59–75.
[10] Crawford H. Traction. In: Weinstein SL, editor.
Pediatric spine surgery. Philadelphia: Lippincott,
Williams & Wilkins; 2001. p. 69–81.
[11] Arlet V, Papin P,Marchesi D. Halo femoral traction
and sliding rods in the treatment of a neurologically
compromised congenital scoliosis: technique. Eur
Spine J 1999;8(4):329–31.
[12] Sink EL, Karol LA, Sanders J, et al. Efficacy of peri-
operative halo-gravity traction in the treatment of
severe scoliosis in children. J Pediatr Orthop 2001;
21(4):519–24.
[13] Swank SM, Winter RB, Moe JH. Scoliosis and cor
pulmonale. Spine 1982;7(4):343–54.
[14] White AAPM. Clinical biomechanics of the spine.
2nd edition. Philadelphia: JB Lippincott; 1990.
[15] Mubarak SJ, Camp JF, Vuletich W, et al. Halo
application in the infant. J Pediatr Orthop 1989;
9(5):612–4.
[16] Stagnara P. [Cranial traction using the ‘‘Halo’’ of
Rancho Los Amigos]. Rev Chir Orthop Reparatrice
Appar Mot 1971;57(4):287–300.
[17] Garfin SR, Botte MJ, Nickel VL. Complications in
the use of the halo fixation device. J Bone Joint
Surg Am 1987;69(6):954.
[18] Rozario RA, Stein BM. Complications of halo-
pelvic traction. Case report. J Neurosurg 1976;
45(6):716–8.
[19] Tredwell SJ, O’Brien JP. Avascular necrosis of the
proximal end of the dens. A complication of halo-
pelvic distraction. J Bone Joint Surg Am 1975;
57(3):332–6.
[20] Wilkins C, MacEwen GD. Cranial nerve injury from
halo traction.ClinOrthopRelatRes1977;126:106–10.

Orthop Clin N Am 38 (2007) 485–496
New Strategies and Decision Makingin the Management of Neuromuscular Scoliosis
John Sarwark, MDa,b,*, Vishal Sarwahi, MDc
aThe Children’s Memorial Hospital, 2300 Childrens Plaza, Box 69, Chicago, IL 60614, USAbDepartment of Orthopaedic Surgery, Northwestern University, Evanston, IL 60208, USA
cDepartment of Orthopaedic Surgery, Montefiore Medical Center/Albert Einstein College of Medicine,
3400 Bainbridge Avenue, MAP6, Bronx, NY 10467, USA
Neuromuscular scoliosis occurs in patientswith traumatic spinal injuries and in patientswith one or several of a large number of neuro-
logical or muscular diseases, including cerebralpalsy, postmeningitis encephalopathy, posttrau-matic encephalopathy, poliomyelitis, myelome-
ningocele, spinal muscle dystrophy, musculardystrophies, and myopathies. The incidence ofscoliosis due to neuromuscular causes may range
between 25% to 90% compared with 2% to 4%for idiopathic scoliosis in the general population.
Natural history
Most children with cerebral palsy survive toadulthood [1]. Crichton and colleagues [2] re-
ported a mean 30-year survival rate of at least87%, varying from 95% in patients with hemiple-gia or monoplegia to 83.5% in those with quadri-
plegia. The incidence of scoliosis in adultinstitutionalized patients varies from 25% to64% [3,4]. There is an inverse relationshipbetween ambulation and incidence of scoliosis,
but a direct correlation between severity ofinvolvement and the incidence of scoliosis [5–11].The incidence and severity increases with the de-
gree of involvement, degree of mental retardation,and functional status [3]. Thometz and Simon [12]showed that scoliosis in patients with cerebral
* Corresponding author. The Children’s Memorial
Hospital, 2300 Childrens Plaza, Box 69, Chicago, IL
60614.
E-mail address: [email protected]
(J. Sarwark).
0030-5898/07/$ - see front matter � 2007 Elsevier Inc. All r
doi:10.1016/j.ocl.2007.07.001
palsy may progress even after skeletal maturity,in contrast to patients with mild and moderate id-iopathic scoliosis. Patients with curves less than
50� had curves increase about 0.8� per year, whilethose with curves greater than 50� had curves in-crease at 1.4� per year. Lumbar and thoracolum-
bar curves in bedridden quadriplegic patientswere most likely to progress. Progressive defor-mity interferes with general health and well-being,
ambulation, sitting balance, and wheelchair trans-fers. This disability can lead to decubiti, costopel-vic impingement pain, and worsening ofpulmonary status. Majd and colleagues [13] dem-
onstrated that a correlation exists between defor-mity size, functional decline, and decubiti.
Patients with spastic cerebral palsy have the
highest incidence of scoliosis [14]. Almost 70% ofthese patients have scoliosis that tends to progresseven after skeletal maturity [12–14]. Curves are
worse in nonambulators, in patients with totalbody involvement, and in patients with thoraco-lumbar curves [12,14,15]. Most scoliosis presents
before 10 years of age. Saito and colleagues [14]found that patients with curves greater than 40� be-fore 15 years of age ended up with larger curves.They recommended that fusion should be consid-
ered for curves greater than 40� before age 15 years.Hsu [16] studied progression of scoliosis in patientswith Duchenne muscular dystrophy (DMD).
Curve progressionwas seen in all patients and thosewith curve greater than 40� experienced decreasedsitting tolerance, decreased vital capacity, loss of
function, and limited use of hands.Bracing may not be a definitive method of
preventing progression in neuromuscular scoliosis,
ights reserved.
orthopedic.theclinics.com

486 SARWARK & SARWAHI
but bracing may be used for improving trunksupport, which perhaps can allow a delay the dateof surgery to a better time or improve seating
functionality. A custom total contact thoracolum-bosacral orthosis is themost commonorthosis usedand most effective in providing truncal support.The physician and patient families must under-
stand that despite brace treatment, curve progres-sion may continue to occur. Braces may alsocause further pulmonary restriction and may inter-
fere with feeding, especially gastronomy tubefeeding.
As scoliosis worsens, loss of sitting balance
makes patients functionally quadriplegic. Inde-pendent sitters may lose their sitting ability anddependent sitters may need more support, in-cluding constant repositioning. Nursing demands
increase in terms of dressing, positioning, andfeeding. When scoliosis is greater than 60�, carebecomes especially difficult.
Natural history after surgery
Surgery is indicated in children with progres-sive scoliosis or large curves that limit overall
function [8,9,11]. However, decision making forsurgery is challenging in the presence of pulmo-nary dysfunction, poor nutritional status, feeding
disorders, seizures, immune compromise, andcoagulopathies. Surgery is associated with a riskof life-threatening complications. Multiple appro-priate consultations should be sought in the pre-
operative and perioperative management phases.A number of long-term follow-up studies haveshown improvements in sitting position, quality
of life, and lung function; improvements in spinalcurves; and improvements in pelvic obliquity [17–22]. Spinal fusion, even in the more severely af-
fected pediatric patients with cerebral palsy, hasa documented high satisfaction rate among par-ents and caregivers, who appreciate the benefits
of this procedure, especially those resulting in eas-ier care and improvements in the patients’ sittingability, physical appearance, and comfort [19].
Kalen and colleagues [15] found that pulmo-
nary function and caregiver time for institutional-ized cerebral palsy patients with scoliosis did notdiffer from pulmonary function and caregiver
time for similar patients without scoliosis. Cassidyand colleagues [23] additionally found no differ-ence in use of pain and pulmonary medicines, in
decubiti, and in caring time between institutional-ized patients who underwent scoliosis surgery andthose who did not.
The complication rate of spinal fusion surgeryfor neuromuscular scoliosis is higher than that foridiopathic scoliosis [24–29]. Comstock and col-
leagues [19] have reported a 68% complicationrate in children with totally involved cerebralpalsy. Fourteen percent of their patients had pul-monary complications, 19% had wound compli-
cations, 18% had hardware complications, and19% had curve progression or pseudoarthrosis.Despite high complication rates, studies have
shown high rates of caretaker satisfaction aftersurgery [18–20,30]. Jones and colleagues [30] ar-rived at a similar conclusion after prospectively
evaluating caregiver satisfaction in children withtotal body involvement who underwent scoliosissurgery. Parents reported higher satisfactionwith the patient’s overall health status after sur-
gery. They found that the most common findingswere improvement in appearance, sleeping com-fort, pain relief, and self-attitude. Results showed
less pain, greater happiness, and less likelihood offeeling ‘‘sick and tired’’ among patients, andgreater satisfaction among parents. Complications
did not significantly affect questionnaire results.Larsson and colleagues [20] reported on a pro-
spective study of 82 patients with neuromuscular
scoliosis who underwent spine fusion and instru-mentation. The group consisted of patients withcerebral palsy [21], myelomeningocele [22], Rettsyndrome [8], myopathies [5], spinal muscular at-
rophy [9], and other diseases, who were followedup for 9.5 years. Fifty-five of these patients under-stood verbal instructions and 27 did not. For the
whole group, the investigators noted improve-ments in sitting balance, weight distributionwhen sitting, Cobb angle, lung function, activities
of daily living, time used for resting, and seatingsupports in a wheelchair. Long-term follow-up re-sults showed further improvements in sitting bal-ance and activities of daily living and reductions
in time required to provide care. The results be-tween the patients who understood verbal instruc-tions and patients who did not were almost the
same except for time required to give care, whichhad decreased in those who understood verbal in-structions but did not change for those who did
not understand verbal instructions.The most important determinants for reduced
life expectancy in patients with neuromuscular
scoliosis are the coexistence of pulmonary com-promise, epilepsy, feeding disorders requiringgastrostomy or nasogastric tube, significant neu-rological involvement, severe cognitive abnormal-
ity, and the lack of ambulation [1,31–37]. Tsirikos

487MANAGEMENT OF NEUROMUSCULAR SCOLIOSIS
and colleagues [38] demonstrated a relatively longmean predicted survival for children with severespastic cerebral palsy who underwent scoliosissurgery. Although their patients had severe im-
pairments, the investigators demonstrateda mean survival of 11 years 2 months. The mostaccurate determinants for survival rates were the
number of postoperation days in the intensivecare unit and the presence of excessive thoracichyperkyphosis. The investigators showed that
a child with kyphosis one standard deviationabove the mean (85.6�) was 122% more likely todie than a child with a kyphosis one standard de-
viation below the mean (26�). Also, children whospent 30 days in the intensive care unit were ata 10 times higher risk than those in the intensivecare unit for 5 days. In this study, such variables
as age, sex, ambulation status, cognition, pelvicobliquity, lumbar lordosis, blood loss, surgicaltime, and length of stay, did not significantly pre-
dict life expectancy.Before surgery, a multidisciplinary evaluation
is necessary to optimize medical management.
This involves evaluations of seizure control med-ications, nutritional supplementation, control ofgastroesophageal reflux, and methods for enhanc-
ing gastric motility. If swallowing status is notknown before surgery, such a study should beperformed to assess risk of aspiration.
A simple step in workup is weighing the
patient. If the child body weight is less than thefifth percentile, nutritional supplementation maybe required. This should be performed parenter-
ally for all patients at risk. Jevsevar and Karlin[39] found an increased postoperative infectionrate, longer length of intubation, and longer hos-
pital stays in patients with cerebral palsy who hadpreoperative serum albumin measurement lessthan 35 g/L and total blood lymphocyte countless than 1.5 g/L. While serum albumin and preal-
bumin are used, some investigators have foundthem unreliable indicators of the nutritional statusof a severely involved child. In fact, some contend
that a child who is overweight as a result of gas-trostomy tube feeding is more likely to have com-plications than an underweight child [26,40].
Bleeding
Children with neuromuscular scoliosis incur
greater intraoperative blood loss than childrenwith idiopathic scoliosis. Blood loss is correlatedwith the number of levels operated and the degree
of pelvic obliquity. Multiple other reasons areattributed to this increased bleeding, includingpoor nutritional status, venous pooling, impairedconnective tissue function, and antiseizure medi-
cation, such as valproic acid. Valproic acid isknown to decrease platelet count and factor VIIIlevels [41,42]. Brenn and colleagues [43] studied
17 patients with cerebral palsy and comparedthem with 17 patients with idiopathic scoliosis.They found that children with cerebral palsy de-
velop significant alterations in coagulation param-eters early, although they had normal coagulationprofiles. The baseline prothrombin time and par-
tial prothrombin time, although within normallimits, were significantly higher in patients withneuromuscular scoliosis than in patients with idi-opathic scoliosis. After 15% loss of blood volume,
investigators found differences between prothrom-bin time, partial prothrombin time, maximumamplitude on thromboelastography, ionized cal-
cium, and serum magnesium levels. Their reportindicated that increased bleeding caused an appar-ent coagulopathy instead of transient hypercoagu-
lable state seen in normal states. Children withcerebral palsy have increased bleeding that startsearlier in the procedure despite a normal coagula-
tion profile.
Monitoring
Ashkenaze and colleagues [44] reported
unreliable somatosensory spinal evoked potential(SSEP) data in neuromuscular scoliosis. Twenty-eight percent of their patients did not produce re-
liable monitoring data and two neurologic deficitswere missed by monitoring. DMD and poliomy-elitis patients had reliable monitoring data and
the use of sublaminar wires in their study pro-duced transient changes. Padberg and colleagues[45] found that use of multiple recording sites, in-
cluding a subcortical site, increased the reliabilityof SSEP, and the addition of another modality,such as the neurogenic motor evoked potential,improved the quality of their data. Eighty-nine
percent of their 74 patients had baseline SSEPs.The investigators recommended monitoring forneuromuscular scoliosis, especially for those with
preserved lower extremity function, preservedbowel and bladder function, or both.
DiCindio and colleagues [46] recently reported
on a pilot study using transcranial motor evokedpotential in nine patients with neuromuscularscoliosis. They found consistent reproducible

488 SARWARK & SARWAHI
responses thatwere low-amplitude signals andwerepresent in all of their patients, including those withcerebral palsy. In this study, all of the mild-to-
moderate cerebral palsy children and 86% ofpatients without cerebral palsy had monitorableresponses for at least one modality. Patients withcerebral palsy who also had weight-bearing ability
or usable motor function, had reliable monitoringdata. Multimodality monitoring is useful in chil-dren with neuromuscular scoliosis. However,
severely involved cerebral palsy patientswith severemental retardation may not benefit from it becauseof lack of reliable data.
Ventilator
Improved home pulmonary noninvasive sup-port has added greatly to the health of children
with neuromuscular spine deformities. Thepreoperative pulmonary function test is useful ifthe patient can perform it. Arm span instead of
height is used in these patients to calculate thepredictive value. Padman and McNamara [47]reported a correlation between decreased vital
capacity and increased complications in neuro-muscular scoliosis. Rawlins and colleagues [48]found 19% pulmonary complications in patients
undergoing reconstructive spinal surgery whenthe vital capacity was less than 40% of predictedcapacity. Yuan and colleagues [49] found thatchildren more than 13 years old with neuromuscu-
lar scoliosis or forced expiratory volume in 1 sec-ond (FEV1) less than 40% predicted were likely torequire prolonged postoperative mechanical venti-
lation. Children less than 13 years old with neuro-muscular scoliosis and FEV1 less than 40%predicted were also likely to need ventilator
postoperation.Patients with DMD have compromised lung
and heart function and a higher risk of complica-
tions [50–53]. Marsh and colleagues [50] reported30% complication rate in DMD patients irrespec-tive of their preoperative forced vital capacity.Almenrader and Patel [54] reported that 40% of
their patients with DMD needed ventilators. Mor-ris [51] has considered forced vital capacity lessthan 25% and left ventricular ejection fraction
of less than 50% a contraindication for electivesurgery. Gill and colleagues [55] studied myo-pathic patients who were on nighttime ventilatory
support and had a mean vital capacity of 20%.They did not report any pulmonary complicationsand concluded that ventilatory support for
respiratory failure presented no increased risk ofcomplications. Their patients returned to theirpreoperative level of function and had smooth
postoperative recovery.Almenrader and Patel [54] have made a case
for early extubation and use of noninvasive con-tinuous positive airway pressure if necessary. In
their series, 76.2% of patients were safely extu-bated at the end of surgery while only 9.5%needed ventilation for more than 3 days. Their
complication rate of 9.5% was lower than therate that has been previously reported. They sug-gested that early extubation was possible in cases
with forced vital capacity greater than 30% and(1) where transespohageal hemodynamic monitor-ing was used; (2) where postoperative pain controlwas optimized using epidural analgesia and intra-
venous morphine; and (3) where ultra-short-acting analgesics, such as remifentanil, andrapidly eliminated inhalation anesthetics, such as
sevoflurane, were used.
Anterior instrumentation
In selected curves that do not include the pelvisor with pelvic obliquity of less than 15�, stoppingfusion in the lumbar spine avoids complications
that can result when fusion extends to thesacropelvis and permits improved mobility [56–58]. The authors feel that, by stopping fusion inthe lumbar spine, the need for an anterior fusion
at L5-S1 is obviated and the patient is allowedthe flexibility to compensate through the lumbosa-cral and the sacropelvic joints. This residual
mobility may allow more comfortable seatingand compensation, especially when the hips aredislocated or subluxated. It also avoids the
problem of loosening of the pelvic fixationdthewindshield effect.
Anterior release leads to improved curve cor-
rection and provides a larger surface area forfusion. This is especially useful in myelomeningo-cele patients and patients with severe osteopenia.It also prevents crankshaft phenomenon in skel-
etally immature patients. The authors have re-viewed the risks and complications of anteriorprocedure in neuromuscular scoliosis in the past
[25]. Basobas and colleagues [56] and Tokala andcolleagues [57] have reported on anterior instru-mentation in neuromuscular scoliosis as an alter-
native in ambulatory as well as nonambulatorypatients Hopf and colleagues [58] have alsoreported on 33 neuromuscular patients treated

489MANAGEMENT OF NEUROMUSCULAR SCOLIOSIS
by anterior instrumentation. Seventeen patientsunderwent secondary posterior instrumentation.Tokala and colleagues [57] performed anterior in-strumentation for patients who had short flexible
curves with minimal pelvic obliquity (!15�) andwho were ambulatory. The investigators foundthat anterior instrumentation provided satisfac-
tory clinical and radiological outcome. In the au-thors’ series, 30% of patients underwent anteriorinstrumentation alone for neuromuscular scoliosis
while others underwent either combined or stagedprocedures for correction of scoliosis [25]. Patientstreated with both anterior and posterior instru-
mentation showed greater correction of scoliosisand improved sitting balance in comparison withpatients treated with anterior or posterior fixationalone [59].
Pelvic fixation
Broom and colleagues [60] considered it neces-
sary to fuse to the pelvis when (1) the case showedtruncal decompensation (plumb line falls lateral tothe sacroiliac joint), (2) the fixed pelvic obliquity
was greater than 15�, and (3) the sacrum waspart of the curve.
There are multiple methods of sacropelvic
fixation, namely the Galveston (L-rod) technique,the Dunn-McCarthy (S-rod) technique, transiliacscrews, intrasacral rods, iliosacral fixation, iliacscrews, and L5-S1 pedicle instrumentation [61–
70]. Unit rods are effective as is the Luque-Galves-ton technique of pelvic fixation, with or withoutanterior procedures [1,60,61,64,69]. Sacral screws,
iliosacral screws, and L5 and S1 pedicle screwshave become alternatives. These are placed inde-pendently of the rods, which do not need to be
bent as in the Galveston technique. Screws areplaced in the posterior ilium, which allows bone-graft harvesting. Camp and colleagues [28], in
a biomechanical and clinical study, reported thatthe Galveston method of sacral fixation is betterthan the Cotrel-Dubousset sacral fixation. Theyfound clinical failure rates of 44% for sacral
screws, 28% for iliosacral screws, and 0% forthe Galveston technique.
Gau and colleagues [63] reported on 58 pa-
tients undergoing Luque-Galveston instrumenta-tion and found a mean pelvic correction of 53%(range: 17�–8�). Yazici and colleagues [70] re-
ported a mean correction of 81% (range: 27�–5�)using Isola-Galveston instrumentation. Miladiand colleagues [66] showed a mean 71%
correction (range: 21�–6�) using iliosacral screwswith Cotrel-Dubousset instrumentation, whileNeustadt and colleagues [67] reported a mean50% correction, which worsened to 37% at fol-
low-up. Peelle and colleagues [68] reported bettercorrection of pelvic obliquity using iliac screwscompared with correction using the Galveston
technique.Vialle and colleagues [71] and Huang and
Lenke [72] have described using intraoperative
asymmetric halo-femoral traction to correct pelvicobliquity. Using this technique, the final correc-tions of scoliosis and pelvic obliquity were signif-
icant. Takeshita and colleagues [73] compared twogroups of patients treated with and without intra-operative halo-femoral traction. They found thatthe curve corrected to an average 37� from aver-
age 87� in the halo-femoral traction group andto 35� from 67� in the control group. Average cor-rection of pelvic obliquity was 78% in the halo-
femoral traction group, compared with 52% inthe control group.
There are many potential complications with
the Galveston technique. Sink and colleagues [74]reported a high incidence of proximal fixationpullout (32%) and distal migration of Galveston
rods (12%). They felt this was secondary to ky-phosing forces created by a long posterior leverarm. This lever arm produces considerable cantile-ver force at the lumbosacral junction, causing fail-
ure of fixation or junctional kyphosis. Failure wasseen even in the presence of anterior fusion.
Several investigators have suggested that
fusion extending to the pelvis should be avoidedfor ambulatory patients without severe pelvicobliquity [7,21,65,75,76]. However, Tsirikos and
colleagues [77] recommended fusion to the pelviseven in ambulatory patients and did not find itto be detrimental.
The authors normally do not extend instru-
mentation across the sacropelvic joint into thepelvis. The authors make every attempt toinstrument in the midline and extend fusion
down to S2. This means sometimes performingfacet joint osteotomies after opening the canal tobring the pelvis level with or at a 15� angle to the
horizontal. The S1 screws are placed convergingtoward the midline with the tip getting a purchasein the S1 endplate. This allows for a strong
tricortical purchase and, in the authors’ experi-ence, requires a C-arm to ensure adequate place-ment in the lateral plane. The S2 screws are placeddivergent, aiming cephalad, to obtain a purchase
in the sacral ala as described by Edwards [78]. In

490 SARWARK & SARWAHI
cases with pelvic obliquity greater than 15�, theauthors instrument to the pelvis.
Unilateral hip dislocation
A unilateral hip dislocation may cause prob-lems with sitting imbalance, pressure ulcers, hip
pain, and pelvic obliquity, which may influencedevelopment and progression of scoliosis. Thereis believed to be a dynamic interplay between hipdislocation, pelvic obliquity, and scoliosis. How-
ever, the exact relationship is unclear in theliterature. Pritchett [79] reported a direct correla-tion between pelvic obliquity and the presence
and severity of scoliosis. Lonstein and Beck[80], on the other hand, did not find any correla-tion between the dislocated hip and the amount
of pelvic obliquity. Recently, Senaran and col-leagues [81] did not find correlation between uni-lateral hip dislocation and scoliosis progression.
They reported that the mean rate of curveprogression in unilateral hip dislocation was12.9�/y, whereas in the control group it was12.2�/y. The progression of pelvic obliquity,
however, was significantly increased in the hipdislocation group in their study.
Unit rod
Bell and colleagues [6] first described use of theunit rod in 1989. This method has become popu-
lar for spine fixation and has been shown to pro-vide excellent correction. Several studies havedocumented the efficacy of this method in com-
parison to older instrumentation systems[62,82,83]. The unit rod has a prebent pelvic sec-tion for the Galveston fixation technique and
allows cantilever force to correct the pelvicobliquity and the scoliosis simultaneously usinga sublaminar wiring technique. The advantages
of the unit rod are its strong fixation and goodcorrection characteristics, its suitability forrelatively quick application, its ability to correctpelvic obliquity, and, because it fixes into the
pelvis, its usefulness as a good foundation. Diasand colleagues [82] reviewed 31 patients whounderwent unit rod instrumentation with subla-
minar wires and posterior spine fusion. Themean curve in their series was 79� preoperatively,19� postoperatively, and was maintained at 18�
at 2.8 years follow-up. The pelvic obliquity was25�, which was corrected to 3� and remained un-changed at follow-up. They reported no
pseudoarthroses or hardware failures with im-provement in sitting ability noted by caregivers,who also expressed high degree of satisfaction
with the procedure. Seven children with open tri-adiate cartilages had a posterior spinal fusiononly with only a 3� loss of correction at maturityand no loss of correction of pelvic obliquity.
Westerlund and colleagues [69] reviewed their ex-perience with the unit rod in skeletally immaturepatients. They also concluded that correction
was maintained at maturity and that this tech-nique may avoid anterior surgery and its associ-ated risks.
Long-term problems with the unit rod are lossof lower lumbar and pelvic fixation, which poten-tially can lead to pseudoarthrosis; failure ofconstruct; and worsening of deformity [74,82,84].
The distal fixation usually gets loose, presentingas a windshield wiper effect seen on radiographs,and is believed to be due to fixation across an un-
fused sacroiliac joint. The rod can also pull out atthe inferior aspect of the construct. This fixationcan be augmented by using pedicle screws at L5
and incorporating them in the unit rod construct.Erickson and colleagues [62] showed this to bebiomechanically superior and also suggested that
addition of cross-links added to the stiffness ofthe construct.
Fusion to L5
Unit rods, although popular, need exposure of
the crest bilaterally for insertion into the pelvis.This increases operating time, increases bloodloss, and limits area available for harvesting
bone graft. Also, in spina bifida patients, thepelvis is usually hypoplastic and may not besufficiently thick to insert the rod [85]. The neuro-
muscular pelvis is osteopenic and thus does notprovide adequate fixation. The unit rod’s correc-tive force employs a cantilever principle and is
based off an osteopenic pelvis. In large defor-mities, the force can lead to loss of fixation orbreakage. In the presence of stable lumbosacralarticulation, fixation into lumbar 5 allows correc-
tion without the need to span the sacroiliac joint.McCall and colleagues [86] reported their experi-ence with the U-rod with pedicular fixation at
lumbar 5 and found that it offered stability equalto the unit rod. They concluded that fusion onlyto L5 in neuromuscular scoliosis was equivalent
to fusion to the pelvis and that the presence ofmobile lumbosacral joint may assist in seatingand transfer activities.

491MANAGEMENT OF NEUROMUSCULAR SCOLIOSIS
Pedicle screw fixation
Wimmer and colleagues [87] reviewed their ex-perience with the Luque-Galveston and the Isolainstrumentations in 52 patients. They found com-
parable results in terms of correction. The Luquegroup had a scoliosis correction of 54% anda 64% correction in pelvic tilt, while the Isola
group had correction of 57% and 63% improve-ment in pelvic tilt. They found greater correctionin smaller curves (!60�) than in larger curves
(O100�) in both groups. Gaine and colleagues[88] have also reported similar corrections withthe Luque-unit rod and Isola instrumentations
in patients with DMD. Vialle and colleagues[71], using a hybrid system, reported a mean sco-liosis correction of 62%. Westerlund and col-leagues [69] reported a final correction of 66%
using Luque-Galveston instrumentation. Onimusand colleagues [89] reported comparable correc-tion with Cotrel-Dubousset instrumentation and
pelvic fixation with iliosacral screws.Teli and colleagues [90] reviewed 56 patients
operated using hybrid pedicle screw and hook sys-
tems. The pseudoarthrosis rate was 1.8%. Thatcompares to rates varying from 1.5% to 10%for the unit rod and Luque-Galveston systems.
The loss of correction of scoliosis, kyphosis, andlordosis in their series was 0% to 6% at follow-up. However, the loss of lordosis was more inpatients who had posterior-only surgery. The
investigators concluded that hybrid systems pro-vided satisfactory correction of coronal deformity,sagittal deformities, and pelvic obliquity, which
improved quality of life in patients with neuro-muscular scoliosis. Peelle and colleagues [68] feltthat a rod construct with iliac screws allows addi-
tional screw fixation points in the sacrum andlower lumbar vertebrae, which possibly allowsfor a stronger construct. They use iliac screwswith sacral screws and even lumbar pedicle screws
in all their patients with spastic neuromuscularscoliosis. Because this patient population showsprogression of spinal deformity following skeletal
maturity, rigid fixation and fusion is indicated[21,27,62,67,89,90].
Pedicle screws have the disadvantage of limited
purchase in an osteoporotic spine. Larger diame-ters should be used and, preferably, all levelsshould be instrumented, which allows greater
points of fixation as well as application of greatercorrective forces. Pedicle screws also providethree-column fixation, which helps achieve greatercorrection of rotation. In presence of exaggerated
lordosis or larger curves, the authors prefer to usereduction screws around the apex, which allowseasier rod capture and reduction and decreases therisk of screw pullout intraoperation.
The keys to greater alignment are extensivereleases. This approach may involve osteotomiesat the apical and juxta-apical region. The osteot-
omies must include the facet joints. In severe, rigidcurves or curves with a large amount ofdecompensation, the authors do not hesitate in
performing a vertebral column resection at theapex. This posterior-based approach is feasiblewith pedicle screws and saves the anterior expo-
sure. Resection at one or two levels provides greatmobility and improved alignment [85].
Staging of surgery is acceptable practice. In theauthors’ experience, halo traction between stages
is poorly tolerated and also involves prolongedhospital stay, which is not feasible in somesettings. An alternative is internal distraction
between stages. Thus the authors achieve themaximum correction feasible in stage one andthen lock the rod in place and close the incision.
The patient is brought back to the operating room2 to 3 weeks after an aggressive nutritionalregimen and hematologic regimen, including pro-
crit, are put in place. Sometimes the patient isdischarged to a rehabilitation facility or evenhome. In the second stage, more releases (usuallyosteotomies) are performed and, if need be,
a vertebral column resection is performed. Thecorrection is then attempted again. A similarapproach has been reported by Buchowski and
colleagues [91].
Staging
McDonnell and colleagues [29], in a mixedgroup of patients, reported a higher incidence ofcomplications with single-stage anteroposterior
surgery and with patients who had neuromuscularscoliosis. Shufflebarger and colleagues [92] andPowell and colleagues [93] reported less morbid-ity, better correction, and reduced cost with sin-
gle-stage anteroposterior surgery. Their studygroup, however, included multiple diagnoses,including neuromuscular diseases. Ferguson and
colleagues [94] found a lower complication ratewith single-stage surgeries in neuromuscularscoliosis. O’Brien and colleagues [95] found
comparable results and complications between theone-stage and two-stage groups. Hopf and col-leagues [58] reported increased pulmonary

492 SARWARK & SARWAHI
complications with single-stage procedures. Tsiri-kos and colleagues [83] more recently comparedpatients who had surgery done in a single stage
with those who had surgery done in two stages.They found that two-stage procedures have signif-icantly less blood loss, shorter surgical time, andfewer complications than one-stage procedures.
Meanwhile, no deaths occurred following two-stage procedures and the rates of infection associ-ated with two-stage procedures were the same as
those associated one-stage procedures. Stagingalso did not increase hospitalization time or stayin the intensive care unit. The investigators con-
cluded that two-stage procedures are safer andproduce consistent results in cerebral palsy pa-tients while single-stage procedures have increasedtechnical and medical complications, increased
morbidity and mortality, and can be overwhelm-ing for both the patient and the surgical team.
Vertical expandable prosthetic titanium rib
Hell and colleagues [96] reported on 15 chil-dren with progressive scoliosis who had a vertical
expandable prosthetic titanium rib (VEPTR) im-plantation at a mean age of 6 years. Six of thesechildren had severe thoracolumbar scoliosis and
pelvic obliquity due to neuromuscular scoliosis.The investigators found that the thoracolumbarcurve reduced in size and pelvic obliquity im-
proved both subjectively and on radiographs.The patients had better sitting ability in the wheel-chair and families and patients reported better sit-
ting abilities and radical cosmetic improvements.
Complications
Sarwahi, Sarwark and colleagues [25], incomparing children with neuromuscular and idio-pathic scoliosis to children with only neuromuscu-
lar scoliosis, found frequent problems with thedevelopment of postoperative pneumonia (3.5%versus 0.7%), respiratory failure (24.1% versus9.2%), urinary tract infections (5.3% versus
0.7%), and surgical wound infections (1.3%versus 0.3%). Complications of scoliosis surgeryin children with neuromuscular and idiopathic
scoliosis also include implant failure, pulmonarycomplications, gastrointestinal complications, in-fections, wound problems, and death. The compli-
cation rates vary from 44% to 80%, witha perioperative death rate of 0% to 7%. The au-thors reported on the complication rates of
anterior spine surgery in 111 patients and foundthat 21.6% of these children had major and22.5% had minor complications with pulmonary
complication being the most frequent [25]. Pulmo-nary complications stem from lung immaturity,pain, and the inability to participate in pulmonarycare, which can range from atelectasis, to pro-
longed ventilatory support or tracheostomy.Staged anterior–posterior procedures do not de-crease the incidence of respiratory complications.
Children who require long-term intensive carefor respiratory problems postoperatively havethe poorest long-term survival [38].
The next commonly seen complications arepancreatitis, ileus, superior mesenteric artery syn-drome, gall bladder disease, and poor gastricmotility. Wound complications occur more often
in patients with neuromuscular scoliosis than inaverage implant patients. Szoke and colleagues[26] described an 8.7% rate of postoperative
wound infection; 7 of 15 were deep infectionswith 1 late infection that needed implant removal.The implant is usually not removed even in the
presence of infection as it provides a stable envi-ronment for the spine, which in turn helps withthe healing and control of the infection. Implant
removal, however, is more commonly a practicein patients with myelomeningocele if the patientdevelops a wound infection.
Summary
Murphy and colleagues [24] found that chil-dren with neuromuscular scoliosis have longer
lengths of stay (9.2 versus 6.1 days), higher totalcharges ($66,953 versus $47,463), more diagnoses(6.3 versus 2.5), and more total procedures (4.2
versus 3.0) compared with those with idiopathicscoliosis. In their study, 1570 children with neuro-muscular scoliosis underwent spine fusion, which
cost $105 million in hospital charges and totaled1444 days in the hospital. They concluded thatchildren with neuromuscular scoliosis experiencesignificantly more complicated and costly hospi-
talizations than do children with idiopathicscoliosis.
The outcome of spinal fusion in neuromuscu-
lar scoliosis demonstrates a consistently highsatisfaction rate among parents and caretakers.It is somewhat more difficult to determine the
functional benefits in individual patients, espe-cially in those with the most severe involvement.Even in those children, a predicted 70% survival

493MANAGEMENT OF NEUROMUSCULAR SCOLIOSIS
rate at 11 years has been documented followingsurgery. Scoliosis is common in children withneuromuscular diseases, especially cerebral palsy.Most of these children need stabilization to
enhance their quality of life by improving sittingability. Studies continue to show a high familysatisfaction and caregiver satisfaction following
spine reconstructive surgery for neuromuscularscoliosis and other spine deformities.
References
[1] Evans PM, Evans SJ, Alberman E. Cerebral palsy:
why we must plan for survival. Arch Dis Child
1990;65:1329–33.
[2] Crichton JU, Mackinnon M, White CP. The life
expectancy of persons with cerebral palsy. Dev
Med Child Neurol 1995;37:567–76.
[3] Madigan RR, Wallace SL. Scoliosis in the institu-
tionalized cerebral palsy population. Spine 1981;6:
583–90.
[4] Samilson RL, Bechard R. Scoliosis in cerebral palsy:
incidence, distribution of curve patterns, natural his-
tory, and thoughts on etiology. Curr Pract Orthop
Surg 1973;5:183–205.
[5] Bradford DS. Neuromuscular spinal deformity. In:
Bradford DS, editor. Moe’s textbook of scoliosis
and other spinal deformities. Philadelphia: WB
Saunders; 1987. p. 271–305.
[6] Bell DF, Moseley CF, Koreska J. Unit rod segmen-
tal spinal instrumentation in the management of
patients with progressive neuromuscular spinal
deformity. Spine 1989;14:1301–7.
[7] Banta JV, Drummond DS, Ferguson RL. The treat-
ment of neuromuscular scoliosis. In: Zuckerman JD,
editor. AAOS Instructional Course Lectures, vol.
48. Rosemont (IL): American Academy of Ortho-
paedic Surgeons; 1999. p.551–61.
[8] Herring JA. Disorders of the brain. In: Herring JA,
editor. Tachjian’s pediatric orthopaedics. Philadel-
phia: WB Saunders; 2002. p. 1121–248.
[9] Labelle H, Grimard G. Pediatric spine. In:
Koval KJ, editor. Orthopaedic knowledge update
7: home study syllabus. Rosemont (IL): American
Academy of Orthopaedic Surgeons; 2002. p. 581–92.
[10] Rinsky LA. Surgery of spinal deformity in cerebral
palsy. Twelve years in the evolution of scoliosis man-
agement. Clin Orthop Relat Res 1990;253:100–9.
[11] Renshaw TS. Cerebral palsy. In: Morrissy RT,
Weinstein SL, editors. Lovell and Winter’s pediatric
orthopaedics. Philadelphia: Lippincott Williams &
Wilkins; 2001. p. 563–99.
[12] Thometz JG,SimonSR.Progressionof scoliosis after
skeletal maturity in institutionalized adults who have
cerebral palsy. JBoneJointSurgAm1988;70:1290–6.
[13] MajdME,MuldownyDS, Holt RT. Natural history
of scoliosis in the institutionalized adult cerebral
palsy population. Spine 1997;22:1461–6.
[14] Saito N, Ebara S, OhotsukaK, et al. Natural history
of scoliosis in spastic cerebral palsy. Lancet 1998;
351(6):1687–92.
[15] Kalen V, Conklin MM, Sherman FC. Untreated
scoliosis in severe cerebral palsy. J Pediatr Orthop
1992;12:337–40.
[16] Hsu JD. The natural history of spine curvature
progression in the nonambulatory Duchenne mus-
cular dystrophy patient. Spine 1983;8:771–5.
[17] Benson ER, Thomson JD, Smith BG, et al. Results
and morbidity in a consecutive series of patients
undergoing spinal fusion for neuromuscular scolio-
sis. Spine 1998;23:2308–18.
[18] Bridwell KH, Baldus C, Iffring TM, et al. Process
measures and patient/parents evaluation of surgical
management of spinal deformities in patients with
progressive flaccid neuromuscular scoliosis (Du-
chenne’s muscular dystrophy and spinal muscular
atrophy). Spine 1999;24:1300–9.
[19] Comstock CP, Leach J, Wenger DR. Scoliosis in
total-body involvement cerebral palsy: analysis of
surgical treatment and patient and caregiver satis-
faction. Spine 1998;23:1412–25.
[20] Larsson E, Aaro S, Normelli H, et al. Long-term
follow-up of functioning after spinal surgery in
patients with neuromuscular scoliosis. Spine 2005;
30(19):2145–52.
[21] Lonstein JE. Spine deformities due to cerebral palsy.
In: Weinstein SL, editor. The pediatric spine: princi-
ples and practice. Philadelphia: Lippincott Williams
& Wilkins; 2001. p. 797–807.
[22] Lonstein JE, Akbarnia BA. Operative treatment of
spinal deformities in patients with cerebral palsy or
mental retardation. J Bone Joint Surg Am 1983;65:
43–55.
[23] Cassidy C, Craig CL, Perry A, et al. A reassessment
of spinal stabilization in severe cerebral palsy.
J Pediatr Orthop 1994;14:731–9.
[24] Murphy NA, Firth S, Jorgensen T, et al. Spinal sur-
gery in children with idiopathic and neuromuscular
scoliosis. What’s the difference? J Pediatr Orthop
2006; 26(2):216–20.
[25] Sarwahi V, Sarwark JF, Schafer MF, et al. Stan-
dards in anterior spine surgery in pediatric patients
with neuromuscular scoliosis. J Pediatr Orthop
2001;21:756–60.
[26] Szoke G, Lipton G, Miller F, et al. Wound infection
after spinal fusion in children with cerebral palsy.
J Pediatr Orthop 1998;18(6):727–33.
[27] Boachie-Adjei O, Lonstein JE, Winter RB, et al.
Management of neuromuscular spinal deformities
with Luque segmental instrumentation. J Bone Joint
Surg Am 1989;71:548–62.
[28] Camp JF, Caudle R, Ashman RD, et al. Immediate
complications of Cotrel-Dubousset instrumentation
to the sacro-pelvis: a clinical and biomechanical
study. Spine 1990;15:932–41.
[29] McDonnell MF, Glassmann SD, Dimar JR, et al.
Perioperative complications of anterior procedures

494 SARWARK & SARWAHI
on the spine. J Bone Joint Surg Am 1996;78(6):
839–47.
[30] Jones KB, Sponseller PD, Shindle MK, et al. Longi-
tudinal parental perceptions of spinal fusion for neu-
romuscular spine deformity in patients with totally
involved cerebral palsy. J Pediatr Orthop 2003;23:
143–9.
[31] Eyman RK, Grossman HJ, Chaney RH, et al. The
life expectancy of profoundly handicapped people
with mental retardation. N Engl J Med 1990;323:
584–9.
[32] Eyman RK, Grossman HJ, Chaney RH, et al. Sur-
vival of profoundly disabled people with severe men-
tal retardation. Am J Dis Child 1993;147:329–36.
[33] Hutton JL, Cooke T, Pharoah PO. Life expectancy
in children with cerebral palsy. BMJ 1994;309:
431–5.
[34] Hutton JL, Colver AF, Mackie PC. Effect of sever-
ity of disability on survival in northeast England
cerebral palsy cohort. Arch Dis Child 2000;83:
468–74.
[35] Anderson TW. Life expectancy in cerebral palsy.
Lancet 1996;348(9040):1516.
[36] Plioplys AV, Kasnicka I, Lewis S, et al. Survival
rates among children with severe neurologic disabil-
ities. South Med J 1998;91:161–72.
[37] StraussDJ, Shavelle RM,Anderson TW. Life expec-
tancy of children with cerebral palsy. Pediatr Neurol
1998;18:143–9.
[38] Tsirikos AI, Chang W, Dabney K, et al. Life expec-
tancy in pediatric patients with cerebral palsy and
neuromuscular scoliosis who underwent spinal
fusion. Dev Med Child Neurol 2003;45:677–82.
[39] Jevsevar DS, Karlin LI. The relationship between
preoperative nutritional status and complications af-
ter an operation for scoliosis in patients who have
cerebral palsy. J Bone Joint Surg Am 1993;75:880–4.
[40] Lipton GE, Miller F, Dabney KW, et al. Factors
predicting postoperative complications following
spinal fusions in children with cerebral palsy. J Spi-
nal Disord 1999;12:197–205.
[41] Chambers HG, Weinstein CH, Mubarak SJ, et al.
The effect of valproic acid on blood loss in patients
with cerebral palsy. J Pediatr Orthop 1999;19:792–5.
[42] Winter SL,Kriel RL,Novacheck TF, et al. Perioper-
ative blood loss: the effect of valproate. Pediatr
Neurol 1996;15:19–22.
[43] Brenn BR, Theroux MC, Dabney KW, et al. Clot-
ting parameters and thromboelastography in chil-
dren with neuromuscular and idiopathic scoliosis
undergoing posterior spinal fusion. Spine 2004;
29(15):E310–4.
[44] Ashkenaze D, Mudiyam R, Boachie-Adjei O, et al.
Efficacy of spinal cord monitoring in neuromuscular
scoliosis. Spine 1993;18:1627–33.
[45] Padberg AM, Russo MH, Lenke LG, et al. Validity
and reliability of spinal cord monitoring in neuro-
muscular spinal deformity surgery. J Spinal Disord
1996;9:150–8.
[46] DiCindio S, Theroux M, Shah S, et al. Multimodal-
ity monitoring of transcranial electric motor and so-
matosensory-evoked potentials during surgical
correction of spinal deformity in patients with cere-
bral palsy and other neuromuscular disorders. Spine
2003;28(16):1851–6.
[47] PadmanR,McNamaraR. Postoperative pulmonary
complications in children with neuromuscular scoli-
osis who underwent posterior spinal fusion.DelMed
J 1990;62:999–1003.
[48] Rawlins BA, Winter RB, Lonstein JE, et al. Recon-
structive spine surgery in pediatric patients with ma-
jor loss in vital capacity. J Pediatr Orthop 1996;16:
284–92.
[49] Yuan N, Skaggs DL, Dorey F, et al. Preoperative
predictors of prolonged postoperative mechanical
ventilation in children following scoliosis repair.
Pediatr Pulmonol 2005;40:414–9.
[50] Marsh A, Edge G, Lehovsky J. Spinal fusion in
patients with Duchenne’s muscular dystrophy and
a low forced vital capacity. Eur Spine J 2003;12:
507–12.
[51] MorrisP.Duchennemusculardystrophy: a challenge
for the anaesthetist. Paediatr Anaesth 1997;7:1–4.
[52] Rice JJ, Jeffers BL, Devitt AT, et al. Management of
the collapsing spine for patients withDuchennemus-
cular dystrophy. J Med Sci 1998;167:242–5.
[53] Mubarak SJ, Morin WD, Leach J. Spinal fusion in
Duchenne muscular dystrophy: fixation and fusion
to the sacropelvis? J Pediatr Orthop 1993;13:752–7.
[54] Almenrader A, PatelD. Spinal fusion surgery in chil-
drenwith non-idiopathic scoliosis: Is there a need for
routine postoperative ventilation? Br J Anaesth
2006;97(6):851–7.
[55] Gill I, Eagle M, Mehta JS, et al. Correction of neu-
romuscular scoliosis in patients with preexisting
respiratory failure. Spine 2006;31(21):2478–83.
[56] Basobas L, Mardjetko S, Hammerberg K, et al. Se-
lective anterior fusion and instrumentation for the
treatment of neuromuscular scoliosis. Spine 2003;
28:S245–8.
[57] Tokala D, Lam KS, Freeman B, et al. Is there a role
for selective anterior instrumentation in neuromus-
cular scoliosis? Eur Spine J 2007;16:91–6.
[58] Hopf CG, Eysel P, Dubousset J. Operative treat-
ment of scoliosis with Cotrel-Dubousset-Hopf
instrumentation. New anterior spinal device. Spine
1997;22:618–27 [discussion: 627–618].
[59] Brown JC, Swank S, Specht L. Combined anterior
and posterior spine fusion in cerebral palsy. Spine
1982;7:570–3.
[60] Broom MJ, Banta JV, Renshaw TS. Spinal fusion
augmented by luque-rod segmental instrumentation
for neuromuscular scoliosis. J Bone Joint Surg Am
1989;71:32–44.
[61] Bulman WA, Dormans JP, Ecker ML, et al. Poste-
rior spinal fusion for scoliosis in patients with cere-
bral palsy: a comparison of luque rod and unit rod
correction. J Pediatr Orthop 1996;16:314–23.

495MANAGEMENT OF NEUROMUSCULAR SCOLIOSIS
[62] EricksonMA, Oliver T, Baldini T, et al. Biomechan-
ical assessment of conventional unit rod fixation ver-
sus a unit rod pedicle screw construct. A human
cadaver study. Spine 2004;29(12):1314–9.
[63] Gau YL, Lonstein JE, Winter RB, et al. Luque-
Galveston procedure for correction and stabiliza-
tion of neuromuscular scoliosis and pelvic
obliquity: a review of 68 patients. J Spinal Disord
1991;4:399–410.
[64] Maloney WJ, Rinsky LA, Gamble JG. Simulta-
neous correction of pelvic obliquity, frontal plane,
and sagittal plane deformities in neuromuscular sco-
liosis using a unit rod with segmental sublaminar
wires: a preliminary report. J Pediatr Orthop 1990;
10:742–9.
[65] McCarthy RE. Management of neuromuscular sco-
liosis. Orthop Clin North Am 1999;30:435–49.
[66] Miladi LT,Ghanem IB,DraouiMM, et al. Iliosacral
screw fixation for pelvic obliquity in neuromuscular
scoliosis: a long-term follow-up study. Spine 1997;
22:1722–9.
[67] Neustadt JB, Schufflebarger HL, Cammisa FP. Spi-
nal fusions to the pelvis augmented by Cotrel-
Dubousset instrumentation for neuromuscular
scoliosis. J Pediatr Orthop 1992;12:465–9.
[68] Peelle MW, Lenke LG, Bridwell KH. Comparison
of pelvic fixation techniques in neuromuscular spi-
nal deformity correction: Galveston rod versus iliac
and lumbosacral screws. Spine 2006;31(20):2392–8
[discussion: 2399].
[69] Westerlund LE, Gill SS, Jarosz TS, et al. Posterior-
only unit rod instrumentation and fusion for neuro-
muscular scoliosis. Spine 2001;26(18):1984–9.
[70] Yazici M, Asher MA, Mardacker JW. The safety
and efficacy of Isola-Galveston instrumentation
and arthrodesis in the treatment of neuromuscular
spinal deformities. J Bone Joint Surg Am 2000;
82A:524–43.
[71] Vialle R, Delecourt C, Morin C. Surgical treatment
of scoliosis with pelvic obliquity in cerebral palsy.
The influence of intraoperative traction. Spine
2006;31(13):1461–6.
[72] Huang MJ, Lenke LG. Scoliosis and severe pelvic
obliquity in a patient with cerebral palsy. Surgical
treatment utilizing halo-femoral traction. Spine
2001;26(19):2168–70.
[73] Takeshita K, Lenke LG, Bridwell KH, et al. Analy-
sis of patients with nonambulatory neuromuscular
scoliosis surgically treated to the pelvis with intrao-
perative halo-femoral traction. Spine 2006;31(20):
2381–5.
[74] Sink EL, Newton PO, Mubarak SJ, et al. Mainte-
nance of sagittal plane alignment after surgical cor-
rection of spinal deformity in patients with cerebral
palsy. Spine 2003;28:1396–403.
[75] Whitaker C, Burton DC, Asher M. Treatment of
selected neuromuscular patients with posterior
instrumentation and arthrodesis ending with lumbar
pedicle screw anchorage. Spine 2000;25:2312–8.
[76] Wild A, Haak H, Kumar M, et al. Is sacral instru-
mentation mandatory to address pelvic obliquity in
neuromuscular thoracolumbar scoliosis due to mye-
lomeningocele? Spine 2001;26:E325–9.
[77] Tsirikos AI, Chang WN, Shah SA, et al. Preserving
ambulatory potentialin pediatric patients with cere-
bral palsy who undergo spinal fusion using unit
rod instrumentation. Spine 2003;28(5):480–3.
[78] Edwards CC. Reduction of spondylolisthesis. In:
Bridwell KH, Dewald RL, editors. Textbook of spi-
nal surgery. Second edition. Philadelphia: Lippin-
cott-Raven; 1997. p. 1317–35.
[79] Pritchett JW. The untreated unstable hip in severe
cerebral palsy. Clin Orthop Relat Res 1983;173:
169–72.
[80] Lonstein JE, Beck K. Hip dislocation and subluxa-
tion in cerebral palsy. J Pediatr Orthop 1986;6:
521–6.
[81] Senaran H, Shah SA, Glutting JJ, et al. The associ-
ated effects of untreated unilateral hip dislocation
in cerebral palsy scoliosis. J Pediatr Orthop 2006;
26(6):769–72.
[82] Dias RC, Miller F, Dabney K, et al. Surgical correc-
tion of spinal deformity using a unit rod in children
with cerebral palsy. J Pediatr Orthop 1996;16:
734–40.
[83] Tsirikos AI, Chang W, Dabney KW, et al. Compar-
ison of one-stage versus two-stage anteroposterior
spinal fusion in pediatric patients with cerebral palsy
and neuromuscular scoliosis. Spine 2003;28(12):
1300–5.
[84] Sanders JO, EvertM, Stanley EA, et al. Mechanisms
of curve progression following sublaminar (Luque)
spinal instrumentation. Spine 1992;17:781–9.
[85] Guille JT, Sarwark JF, Sherk HH, et al. Congenital
and developmental deformities of the spine in chil-
dren with myelomeningocele. J Am Acad Orthop
Surg 2006;14(5):294–302 Review.
[86] McCall RE, Hayes B. Long-term outcome in neuro-
muscular scoliosis fused only to lumbar 5. Spine
2005;30(18):2056–60.
[87] Wimmer C, Wallnofer P, Walochnik N, et al. Com-
parative evaluation of Luque and Isola instrumenta-
tion for treatment of neuromuscular scoliosis. Clin
Orthop Relat Res 2005;439:181–92.
[88] Gaine WL, Lim J, Stephenson W, et al. Progres-
sion of scoliosis after spinal fusion in Duchenne’s
muscular dystrophy. J Bone Joint Surg 2004;86B:
550–5.
[89] Onimus M, Manzone P, Lornet JM, et al. Surgical
treatment of scoliosis in bed-ridden patients with
cerebral palsy. Rev Chir Orthop Reparatrice Appar
Mot 1992;78:312–8.
[90] Teli M, Elsebaie H, Biant L, et al. Neuromuscular
scoliosis treated by segmental third-generation
instrumented spinal fusion. J Spinal Disord Tech
2005;18(5):430–8.
[91] Buchowski JM, Bhatnagar R, Skaggs DL, et al.
Temporary internal distraction as an aid to

496 SARWARK & SARWAHI
correction of severe scoliosis. J Bone Joint Surg Am
2006;88(9):2035–41.
[92] Shufflebarger HL, Grimm JO, Bui V, et al. Anterior
and posterior spinal fusion: staged versus same-day.
Spine 1991;16:930–3.
[93] Powell ET IV,KrengelWF III, KingHA, et al. Com-
parison of same-day sequential anterior and poste-
rior spinal fusion with delayed two-stage anterior
and posterior spinal fusion. Spine 1994;19:1256–9.
[94] Ferguson RL, Hansen MM, Nicholas DA, et al.
Same-day versus staged anterior-posterior spinal
surgery in a neuromuscular scoliosis population:
The evaluation of medical complications. J Pediatr
Orthop 1996;16(3):293–303.
[95] O’Brien T, Akmakjian J, Ogin G, et al. Comparison
of one-stage versus two-stage anterior/posterior
spinal fusion for neuromuscular scoliosis. J Pediatr
Orthop 1992;12:610–5.
[96] Hell AK, Campbell RM, Hefti F. The vertical
expandable prosthetic titanium rib implant for the
treatment of thoracic insufficiency syndrome associ-
ated with congenital and neuromuscular scoliosis in
young children. J Pediatr Orthop B 2005;14:
287–93.

Orthop Clin N Am 38 (2007) 497–509
Surgical Treatment of Congenital ScoliosisDaniel J. Hedequist, MD
Department of Orthopedic Surgery, Children’s Hospital Boston, Harvard Medical School,
300 Longwood Avenue, Hunnewell 2, Boston, MA 02115, USA
The surgical options for congenital spinedeformities are numerous and depend on the typeof anomaly, the degree of deformity, and the age of
the patient. The mainstay of surgical treatmentremains early diagnosis before severe curvature anddeformity exist. Occasionally, patients present withlarge deformities that require more significant
procedures; however, early limited arthrodesisremains the safest and most reliable procedure.Patients who have significant decompensation of
the spine at a young age may benefit from a fusion-less procedure, as do patients who have coexistingrib deformities and chest wall insufficiency. This
article reviews the general surgical principles thatneed to be followed to treat these patients safely.The numerous surgical procedures available fortreating these patients also are reviewed.
Preoperative evaluation
The preoperative evaluation of a patient whohas a congenital spine abnormality begins witha history and physical examination. The history
includes a thorough past medical history given theassociation of congenital spine deformities withother organ system abnormalities (ie, of the
cardiac and genitourinary systems). The physicalexamination should begin with a complete skeletalexamination, with special attention focused on theneurologic examination and spinal examination.
The neurologic examination should include basictesting of motor strength, sensory function, andreflexes. Subtle signs should be looked for to
assess for underlying ataxia or myelopathy. Thespinal examination begins with the skin in thespinal midline, assessing for nevi, hemangiomas,
E-mail address: [email protected].
edu
0030-5898/07/$ - see front matter � 2007 Elsevier Inc. All r
doi:10.1016/j.ocl.2007.05.002
dimples, or hairy patches, which may be signs ofunderlying spinal dysraphism. Coronal and sagit-tal profiles should be evaluated, as should general
flexibility of the deformity with manual hyperex-tension testing and manual side-bending tests.The spinal examination also should focus on thecervical spine given the association of Klippel-Feil
syndrome with congenital scoliosis.Radiographs should include standard 36’’
standing radiographs in both planes as well as
supine bending films. Most deformities can beclassified readily with plain films, and any associ-ated rib fusions are evident on the radiographs.
The bending films give a sense of the amount offlexibility in adjacent areas of the spine. Somesurgeons recommend spot films of the deformityto further delineate the anatomy; however, the
advent of newer imaging modalities make thesefilm unnecessary. Plain films of the pelvis, lookingat the triradiate cartilages and the Risser sign of
the patient, as well as a left hand and wrist radio-graph for bone age, are important in the pubes-cent age child as an indicator of growth when
crankshaft is a concern [1,2].MRI of the entire spine and brainstem is
mandatory in any child undergoing surgical treat-
ment of a congenital spine deformity. The pres-ence of underlying spinal dysraphism is believed tobe upward of 30% in children who have congen-ital scoliosis [3,4]. MRI scans also may be studied
to look at the anatomy of the deformity. The pres-ence of any cord compression is best studied byMRI, and this largely has replaced myelography
as the imaging modality of choice (Fig. 1). Thecoronal and sagittal images may help to definethe segmentation and formation defects in the
anterior spine. The axial views also can be viewedto look at the pedicle anatomy of the patient whencontemplating transpedicular instrumentation.
ights reserved.
orthopedic.theclinics.com

498 HEDEQUIST
CT scanning has been studied and shown to beeffective as a preoperative imaging study forcongenital spine deformities (Fig. 2). In all cases,
preoperative three-dimensional (3-D) CT scans
Fig. 1. MRI of a patient with a congenital dislocation of
the spine. Note the angular kyphosis and resulting spinal
cord compression.
Fig. 2. 3-D CT of a patient who has multiple
hemivertebra.
correlated with the intraoperative anatomy inpatients undergoing hemivertebra excision [5].These scans are especially helpful in defining the
posterior anatomy anddwhen studied before theoperationdcan aid the surgeon greatly in the op-erating room. The scans also have been shownto be effective in more complex deformities; the
author and colleagues recommend them in all pa-tients undergoing a deformity operation for con-genital scoliosis. The radiation dosage required
for a CT scan is a concern and can be reducedgreatly by following a pediatric protocol; the soft-ware for creating 3-D images is readily available,
and no additional radiation is needed. CT scansalso have been shown to aid in assessing pulmo-nary volume before and after vertical expandableprosthetic titanium rib (VEPTR) placement [6,7].
General surgical principles
Monitoring
The use of neurologic monitoring is mandatory
for surgical procedures in patients who havecongenital spine deformities. The risk for neuro-logic injury associated with spine surgery is high-
est in patients who have congenital spinedeformities [8]. Kyphotic deformities place thespine at most risk. Preoperative MRIs can helpto rule out any coexisting spinal dysraphism.
The author and colleagues use motor-evokedpotential and somatosensory-evoked potential tominimize the risk for a neurologic deficit [9–11].
At the author’s institution, a wake-up test also isperformed on all patients at the end of any proce-dure; this has been shown to be effective in even
the youngest of patients [12,13]. Communicationwith the anesthesiologist and monitoring techni-cian is crucial to minimize the chance that anes-thetic agents impair the ability to monitor the
spinal cord. If a patient has a coexisting spinalaxis abnormality, referral to a neurosurgeon isparamount. In general, cord detetherings may be
done at the same time as hemivertebra resectionsor in situ fusions. More complex operationsrequiring osteotomies or corrections with instru-
mentation should be done after addressing any as-sociated dysraphism by the neurosurgeon.
Positioning
For most patients undergoing a posterior
fusion with instrumentation, standard positioningon a radiolucent spinal bed with headpiece, chestbolster, and iliac crest pads suffices. Usually,

499SURGICAL TREATMENT OF CONGENITAL SCOLIOSIS
younger patients are placed on a radiolucent flatoperating table with gel rolls to support the torso.The author and colleagues have found thatpatients who have significant kyphotic deformities
may be managed best with a Mayfield head rest orcervical tongs to have better control of the head;instrumenting or working on the upper thoracic
spine in these patients can be extremely difficult.Patients who are undergoing open or thoraco-scopic anterior surgery may be placed in the
standard lateral decubitus position. Thoraco-scopic surgery also may be done with the patientin the prone position with the anesthesiologist
using diminished tidal volume ventilation, therebyavoiding the pitfalls of single-lung ventilation [14].Patients who are undergoing simultaneous ante-rior and posterior procedures should be placed
in the lateral decubitus position (convex side up)on a flat radiolucent operating frame with theentire anterior and posterior fields draped out
[15]. These patients should be placed near theedge of the operating room table so that whenposterior field self-retaining retractors are placed,
the handles do not hit the table and block theability to retract (Fig. 3).
Instrumentation
The use of spinal instrumentation for congen-ital spine deformities was described first by JohnHall and colleagues [16], who used Harringtoninstrumentation. Instrumentation greatly aided in
obtaining fusion in these patients, and it was be-lieved to be safe and effective; however, the
Fig. 3. Intraoperative photo of a patient undergoing
hemivertebra resection by way of simultaneous ante-
rior–posterior exposures. Note the ability to work in the
anterior–posterior fields at the same time allows for
maximum visualization and control of the spine.
original article described difficulties in using thisinstrumentation in smaller children and cautionedagainst it. Before the use of instrumentation, thepseudarthrosis rate and loss of curve correction
were high in these patients [17]. Newer-generationimplants were manufactured to be size specificand were reported on first in small children under-
going hemivertebra resection [18]. Further studieshave shown that instrumentation is feasible andsafe in smaller patients who have congenital spine
deformities [19,20]. The rate of union and correc-tion maintenance for posterior arthrodesis isgreater with instrumentation than without instru-
mentation. The author and colleagues recommendusing titanium instrumentation in all patients whohave congenital spine deformities. This allows forfurther imaging of the spinal axis if needed as well
as the ability to clearly image other parts of thethorax and abdomen with MRI in patients whohave coexisting organ abnormalities, such as
congenital heart disease or urologic abnormalities.Pedicle screw instrumentation of the thoracic
spine has become more commonplace as reports
have documented the safety and efficacy ofsegmental pedicle instrumentation [21–24]. Pediclescrew placement has been shown to be technically
possible in children as young as 1 year of age [25].Their use in congenital spine deformities has beendescribed in children undergoing hemivertebraresection. Hemivertebra resection remains the
best scenario because frequently the instrumenta-tion is placed at the level above and below thehemivertebra, which frequently are anatomically
normal, rendering placement straightforward.The author and colleagues routinely use pediclescrews if the preoperative imaging studies suggest
that this is feasible; however, the anatomic start-ing points can be difficult to find when posteriorelement anatomy is abnormal. It is helpful tostudy the pedicle anatomy on the preoperative
CT scan. Surgeons should be prepared to usehook or screw fixation at available levels to createspinal stability for the maintenance of curve
correction and arthrodesis.
Allograft
Autograft has long been the bone graft of
choice in patients who have congenital scoliosis.Limitations of autograft include donor site mor-bidity when harvesting the iliac crest as well as the
small volume available secondary to the size of thepatient. Local grafts from rib excisions duringanterior exposure or from hemivertebra excisions

500 HEDEQUIST
are an important source of autograft and shouldbe used when possible. The author and colleagueshave extensive experience with allograft at their
institution in patients who have congenital scoli-osis. The rate of fusion and infection rate havebeen shown to be the same as in other series ofpediatric deformity surgeries [26]. The author and
colleagues use freeze-dried corticocancellous bonechips. These are readily available from numerousbone banks, are inexpensive, and there has never
been a reported case of HIV transmission fromfreeze-dried allograft in spinal surgery.
Crankshaft
The crankshaft phenomenon is caused bycontinued anterior growth of the spine in theface of a solid posterior arthrodesis [1]. This leads
to continued curve progression and deformity andwas described first in adolescent idiopathic scolio-sis. Crankshaft phenomenon exists in congenital
scoliosis as well; however, it is less predictablethan in idiopathic scoliosis [27]. The potentialfor crankshaft to occur depends on the qualityand number of discs anteriorly. Disc spaces that
are clear and definable signify the potential fornormal anterior growth; less definable disc spacesignifies less growth potential. In children under-
going surgery for congenital spine deformitieswho are at risk for crankshaft (Risser 0, open tri-radiate cartilage), the disc spaces should be stud-
ied on the preoperative radiographs, CT scan,and MRI. Significant growth potential requiresan anterior open or thoracoscopic procedure to
arrest growth.
Traction
In the past, preoperative traction was believed
to be contraindicated in congenital spine defor-mities given the potential for traction-inducedparalysis. Multiple investigators have revisited
traction in pediatric spinal deformity and haveshown it to be efficacious as a preoperative tool[28–30]. Traction may be halo gravity, halo femo-ral, or halo pelvic (Fig. 4). The author and
colleagues have found halo-gravity traction to beeffective because the patients are allowed out ofbed and into a wheelchair and are allowed to
ambulate behind the wheelchair. Being out ofbed and ambulatory has a positive effect on main-taining bone density, which may help to minimize
implant–bone failures. Traction should startslowly and be increased gradually with careful at-tention given to the neurologic examination. Any
neurologic deficit or neurologic complaint by thepatient calls for a diminishment of traction. Trac-tion also may be used after an anterior release to
get more correction of a deformity before a poste-rior instrumented fusion. The amount of timeneeded for traction to be efficacious is variable,and it should be used from 2 weeks to 2 months
if needed. A nutrition consult should be done be-fore the hospitalization in these patients becausethey are, or frequently become, nutritionally
depleted. Although traction has been shown tobe safe and efficacious, the author and colleaguesdo not recommend applying traction in cases of
short, rigid, and angular deformities, especiallywhen associated with kyphosis. These deformitiesdo not have a positive response to traction and areat high risk for developing a neurologic deficit.
In situ fusion
Fusion in situ remains the most reliable andsafe operation for congenital spine deformities.
The hallmark of treatment for congenital defor-mities is early diagnosis and recognition of a de-formity that will be progressive. In situ fusion
affords no correction of a deformity; however, it isan effective operation when done correctly onthe appropriate patient. Patients with a fully
segmented hemivertebra with no associated de-formity may be good candidates for this pro-cedure. The classic indication is a patient who hasa unilateral bar or a unilateral bar with contra-
lateral hemivertebra who is diagnosed early,before any significant deformity [31,32]. Patientsundergoing an in situ fusion need to have an
anterior procedure when there is the potentialfor anterior growth. This can be done thoraco-scopically or as an open procedure. The author
and colleagues recommend the use of posteriorinstrumentation because it negates or minimizesthe time needed for a cast or brace and improvesfusion rate. Patients who have congenital kypho-
sis that is due to failure of formation may be fusedin situ posteriorly. This allows for anterior growthover time to correct their deformity. The ideal
indication is a deformity that is due to a congenitalfailure of formation that is less than 50� in apatient with significant growth remaining [33,34].
Convex hemiepiphysiodesis
Convex hemiepiphysiodesis is a procedure thatrequires growth to obtain correction over time[35]. The classic indication is a patient with a fully

501SURGICAL TREATMENT OF CONGENITAL SCOLIOSIS
Fig. 4. A patient in wheelchair halo-gravity traction.
segmented hemivertebra without any associated
deformity. The procedure is done as an anteriorand posterior fusion on the convex side of thecurvature. The concave side retains its growth po-
tential and, in theory, allows for some correctionof the deformity; however, in practice, the amountof correction is negligible. It is not a reliableprocedure for many patients if any correction is
desired. It is contraindicated if there is no concavegrowth potential.
Hemivertebra excision
Hemivertebra excision remains an enticing
surgical option for a hemivertebra causing a pro-gressive curve and deformity. The authors andcolleagues have found that the ideal patient remains
a child younger than 5 years of age with a fullysegmented hemivertebra at the thoracolumbarjunction, lumbar spine, or lumbosacral spine. In
general, most hemivertebra in the thoracic spine
are not problematic. Hemivertebra at the cervico-thoracic or cervical region occasionally becomeproblematic, and excision in these areas has been
described [36]. Earlier publications on hemiverte-bra excision reported the occurrence of neurologicdeficits; however, recent series demonstrated thathemivertebra excision can be performed safely
[15,21,36–38]. Hemivertebra may be resected byan anterior–posterior procedure or by a posterior-only procedure. The author and colleagues des-
cribed simultaneous anterior–posterior approacheswith excision in two separate studies at their institu-tion; however, they have moved to a posterior-only
excision because Ruf and Harms [19] reportedsuccess using this technique.
The excision of a hemivertebra by way of an
anterior–posterior technique can be done reliablyby way of simultaneous exposures. The patientshould be placed in the lateral position with

502 HEDEQUIST
a bolster under the concave side of the deformityand the table slightly broken. The anterior expo-sure should be undertaken as a standard thora-
cotomy or with the transthoracic-retroperitonealor retroperitoneal approach, depending on thelevel of the hemivertebra. Once the anterior expo-sure is performed, the posterior spine is exposed,
and a spot radiograph is taken to confirm the cor-rect level. The author and colleagues place pediclescrews bilaterally at the levels above and below
the hemivertebra. Laminar hook sites also are pre-pared on the convex side of the spine for compres-sion across the deformity. Resection begins with
the anterior vertebral body after the discs aboveand below have been removed. The body shouldbe resected posteriorly toward the canal, and theposterior vertebral body should be resected back
to the posterior longitudinal ligament. Using a di-amond-tipped burr can facilitate safe resection ofthe posterior body. Then, the pedicle, as it enters
the vertebral body, can be resected under direct vi-sualization. Posterior resection begins with resec-tion of the hemilamina, which generally is done
with Kerrison rongeur. The transverse processcan be resected, and the resection can continueby working down the pedicle. The nerve roots
above and below the hemivertebra pedicle needto be protected. The remaining pedicle can be re-sected through both incisions. The bolster is re-moved and the table unbroken; the wedge
resection can be closed down with downwardpressure on the spine through the anterior inci-sion. The first rod is inserted into the laminar
hooks, which are used to compress across the de-formity, achieving correction. The author and col-leagues have found that the pedicles in young
patients who have congenital scoliosis do not tol-erate compression reliably, given the small pediclesize and small screw diameter. The remaining tworods are placed in the pedicle screws and seated.
This allows for maximum fixation with the threerods. The rod diameter is 3.2 or 3.5 mm in youn-ger children. The author and colleagues have not
had any implant-related problems with thethree-rod technique and have adapted it to theposterior-only resections as well.
Resection by way of a posterior-only approachis a challenging operation secondary to blood lossand the need to work around the cord or cauda
from the posterior side. These factors makevisualization more difficult than anterior–poste-rior procedures. The spine is exposed posteriorly,and the pedicle screws are placed into position.
Resection begins by dissecting over the transverse
process with a Cobb elevator and following thisplane with a Cobb elevator down the lateral as-pect of the vertebral body to the anterior portion,
which will help with retraction. Then, the hemila-mina can be resected followed by the transverseprocess. The pedicle resection can begin, withcare taken to place a retractor on the medial ped-
icle wall protecting the dural contents. The pediclecan be resected by burring down the cancellousbone and resecting the walls with rongeurs, taking
care to protect the nerve roots above and below.Moving anteriorly down the pedicle, the authorand colleagues have found it useful to use a bipolar
cautery to seal the epidural veins, which lie on theinner aspect of the pedicle and vertebral body.Continued anterior protection of visceral struc-tures anteriorly and anterolaterally is necessary
as one moves forward with the vertebral body re-section. The discs above and below can be re-sected, taking care to move across the midline to
the concave side to get a complete wedgeresection.
Complete correction of the deformity can be
performed using laminar hooks to compressacross the convexity. Rods can be placed intobilateral pedicle screws (Fig. 5). The author and
colleagues have found it advantageous to placethe child in a custom-molded TLSO for 3 months;children younger than 3 years of age may becandidates for a Risser-type cast for a period of
4 weeks.A comparison of posterior only-resection
versus simultaneous anterior–posterior resection
yields results that are similar with regard to curvecorrection, blood loss, and fusion. Earlier reportsof posterior-only resection with segmental fixation
had a higher implant failure rate; however, theauthor and colleagues’ experience with the three-rod technique has not borne this out. They preferto resect hemivertebra from a posterior-only
procedure when feasible, because this avoids ananterior procedure. Relative contraindicationsinclude the surgeon being uncomfortable with
a posterior-only technique or a patient who is atrisk for significant bleeding (eg, congenital heartdisease) that would render visualization from
a posterior procedure difficult.
Partial correction with instrumentation and fusion
The earliest series of patients who had congen-ital scoliosis that was treated with posteriorfusions were fraught with loss of correction and

503SURGICAL TREATMENT OF CONGENITAL SCOLIOSIS
Fig. 5. (A) Standing posteroanterior radiograph of a patient who has a fully segmented hemivertebra. (B) Standing
postoperative radiograph after posterior-only excision of the hemivertebra with excellent curve correction.
pseudarthrosis given the lack of implants
[17,31,39]. The use of instrumentation for congen-ital spine deformities has evolved into modernsegmental implants with improved maintenance
of correction and arthrodesis rate [20]. The abilityto afford any correction of a congenital anomalydepends on the type of anomaly and the amountof normally segmented spine adjacent to the
anomaly. The principles of stable vertebra applywhen trying to balance a decompensated spinein congenital scoliosis. Studying presurgical
standing radiographs and bending films can helpto define stable zones of instrumentation and fu-sion. Frequently, it is possible to obtain a balanced
spine by way of posterior (only) arthrodesis andinstrumentation. Positioning of the patient, thor-ough facetectomies, and stable instrumentationfrequently achieve an arthrodesis with a balanced
spine. Care must be taken not to apply distractiveforces with implants or to attempt significantcorrections with instrumentation in the case of
a rigid deformity. Transpedicular segmental in-strumentation can achieve large curve correctionsand possibly prevent crankshaft in patients who
have idiopathic scoliosis; however, segmentalscrew fixation frequently is not possible givenabnormal anatomic landmarks and pedicle anat-
omy in congenital deformities, and surgeonsshould be familiar with all available posteriorimplant anchors.
Occasionally, osteotomies (eg, Smith-Peterson
or pedicle subtraction) are necessary to obtainspinal balance; these also may need to be done inconcert with anterior releases. Osteotomies place
the patient are at a higher risk for neurologicdeficit and should be done only in concert withneurologic monitoring and the ability to achievesolid, stable fixation. The planning of the osteot-
omies is facilitated by preoperative CT scans(Fig. 6). These are highly challenging cases andshould be done only by experienced hands; occa-
sionally, the author and colleagues have found ituseful to have their neurosurgical colleaguesavailable when decompression is needed.
Although vertebral column resections areneeded rarely, when a patient has a severe de-formity that cannot be managed by other means,they have been performed safely with good results
[29,40]. Vertebral resection also may be indicatedwhen a kyphotic deformity is creating spinalcord compression that needs to be addressed. Fre-
quently, kyphotic deformities are best operated onthrough posterior approaches, such as a costo-transversectomy. Vertebral column resections
may be done as a staged anterior–posterior oper-ation or as a posterior–only resection. Usually,circumferential cases are staged because of the sig-
nificant blood loss and the technically demandingnature of the procedure. The anterior procedurebegins with a thorough exposure, and it should

504 HEDEQUIST
Fig. 6. (A, B) Preoperative standing radiographs of an adolescent patient who has progressive congenital kyphoscoliosis.
(C) 3-D CT scan of the patient showing the apical kyphoscoliotic anomaly. (D, E) Postoperative standing radiograph
after posterior wedge osteotomy with excellent correction of the deformity and spinal balance.
include an osteoperiosteal flap to safely dissectaround to the far side of the spine and to protectagainst visceral structures. Resection of the ante-
rior body is performed all the way back to theposterior longitudinal ligament. Once completeresection is done, gelfoam should be place over
the dura followed by abundant autograft and allo-graft. The posterior resection usually can be per-formed a week later. Stable fixation is placed
first during the posterior procedure, which is fol-lowed by resection of the posterior elements andcareful correction of the deformity. Neurologic

505SURGICAL TREATMENT OF CONGENITAL SCOLIOSIS
Fig. 6 (continued )
monitoring is essential during these cases; fre-quently, multiple wake-up tests are needed. Theauthor and colleagues have found it beneficial tokeep the arterial blood pressure elevated during
correction of the deformity to prevent cord ische-mia. Posterior-only vertebral column resectionshave come into favor to avoid any anterior sur-
gery. Frequently, this is the best option if thereis a corresponding kyphotic deformity that wouldmake access to the vertebral column difficult
through the standard anterior approach[29,40,41].
Growing rods
In the past, patients younger than 5 years ofage who had congenital deformities involving long
sections of the spine or with large compensatorycurves in normally segmented spine were treatedwith early arthrodesis to create a balanced spine.
Recent studies showed that early arthrodesisover a longer section of the thoracic spine before5 years of age may be associated with a significant
reduction in pulmonary function and chest height.This had led to interest in the use of growing rodsfor select congenital spine anomalies (Fig. 7).
Recent reports documented successful treatmentof early-onset deformities with growing rods[42–44]. Growing rods rely on normally seg-mented areas of spine to maintain growth while
instrumentation aids in curve control. Proximaland distal anchors are placed by using claw foun-dations, and spanning submuscular rods are used
to gain correction while allowing for growth.Lengthenings are done every 6 months. The idealpatient is younger than 5 years of age and has
a congenital deformity involving a long sectionof the spine in which an arthrodesis would havea detrimental affect on growth. In general, the
proximal and distal anchor points need to beestablished in reasonably normal areas of spineto allow for sufficient fixation. Patients whohave progressive curves that have congenital
anomalies that will not allow for stable anchorplacement or associated congenital rib fusionsthat need to be addressed with thoracostomy
may be better served with VEPTR placement.
Expansion thoracoplasty and vertical expandableprosthetic titanium rib
Occasionally, congenital spine anomalies areassociated with congenital rib fusions [45]. These

506 HEDEQUIST
Fig. 7. (A) Preoperative radiograph of a 4-year-old patient who underwent a previous hemivertebra resection. This
patient has had progressive decompensation above and below the resection site. (B) Postoperative radiograph after
placement of a dual growing-rod construct.
may act together and cause progressive curvatureof the spine with progressive diminishment in
pulmonary function and hemithorax volume.The resultant syndrome, termed ‘‘thoracic insuffi-ciency,’’ causes limitation of pulmonary function[7]. The progressive loss of hemithorax height is
believed to be responsible for this loss of function.Expansion of the hemithorax by opening wedgeosteotomies into the area of congenital rib fusions
or adhesions was shown to have a positive effecton lung function and lung volume [6,46]. Theexpansion of the hemithorax is held in place by
a VEPTR device. This device anchors proximallyaround the second or third ribs. Distally, theVEPTR may anchor into one of three places:around distal ribs, into the lumbar spine, or
around the ilium (Fig. 8). The device can beexpanded through connectors every 6 months.The effect is one of increasing thorax height,
improving lung function, and improving lungvolume. The device also allows for improvementin Cobb measurements over time and control of
corresponding spinal curvature. The ideal indica-tion is a patient who has a constricted hemithoraxsecondary to congenital rib fusions. In general,
the rib fusions create a stiff hemithorax; expansionthoracoplasty and VEPTR do not improve chestwall stiffness and, in fact, may make chest wall
compliance worse. Patients who do not have ribfusions and have a compliant chest wall may be
better served with other treatment modalities.
Summary
Successful surgical treatment of patients whohave congenital spine anomalies relies on applying
general principles to the correct operation. Athorough preoperative assessment is mandatoryand includes a standard history and physical
examination as well as obtaining appropriateimaging tests. The correct surgical proceduredepends on the anomaly itself and the degree
of deformity. Early recognition and surgicaltreatment before severe deformity develops is thehallmark of treatment. Curvatures associated witha moderate degree of deformity can be managed
successfully by fusion with instrumentation.Correction can be achieved by positioning andfacetectomies. Occasionally, osteotomies are
needed to obtain a balanced spine. More severedeformities may require traction with osteotomiesor vertebral column resection. Curvature in youn-
ger children involving long, normally segmentedareas of the spine may be managed best bygrowing rods. Patients with significant growth

507SURGICAL TREATMENT OF CONGENITAL SCOLIOSIS
Fig. 8. (A) Intraoperative photograph of a patient who underwent expansion thoracoplasty with placement of a rib-to-
rib VEPTR and rib-to-spine VEPTR. Pre- (B) and postoperative (C) radiographs after expansion thoracoplasty with
VEPTR placement for congenital rib fusions with congenital scoliosis.
remaining and associated chest wall anomaliesmay be best served by expansion thoracoplasty
and VEPTR.
References
[1] Dubousset J, Herring JA, Shufflebarger H. The
crankshaft phenomenon. J Pediatr Orthop 1989;
9(5):541–50.
[2] Sanders JO, Browne RH, McConnell SJ, et al. Ma-
turity assessment and curve progression in girls
with idiopathic scoliosis. J Bone Joint Surg Am
2007;89(1):64–73.
[3] Belmont PJ Jr, Kuklo TR, Taylor KR, et al. Intra-
spinal anomalies associated with isolated congenital
hemivertebra: the role of routinemagnetic resonance
imaging. J Bone Joint Surg Am 2004;86(8):1704–10.
[4] Prahinski JR, Polly DW Jr, McHale KA, et al. Oc-
cult intraspinal anomalies in congenital scoliosis. J
Pediatr Orthop 2000;20(1):59–63.
[5] Hedequist DJ, Emans JB. The correlation of
preoperative three-dimensional computed tomo-
graphy reconstructions with operative findings in
congenital scoliosis. Spine 2003;28(22):2531–4
[discussion: 1].
[6] Emans JB, Caubet JF, Ordonez CL, et al. The treat-
ment of spine and chest wall deformities with fused
ribs by expansion thoracostomy and insertion of ver-
tical expandable prosthetic titanium rib: growth of
thoracic spine and improvement of lung volumes.
Spine 2005;30(Suppl 17):S58–68.

508 HEDEQUIST
[7] Campbell RM Jr, Smith MD, Mayes TC, et al. The
effect of opening wedge thoracostomy on thoracic
insufficiency syndrome associated with fused ribs
and congenital scoliosis. J Bone Joint Surg Am
2004;86(8):1659–74.
[8] MacEwenGD, BunnellWP, SriramK.Acute neuro-
logical complications in the treatment of scoliosis. A
report of the Scoliosis Research Society. J Bone
Joint Surg Am 1975;57(3):404–8.
[9] Lubicky JP, Spadaro JA,YuanHA, et al. Variability
of somatosensory cortical evoked potential monitor-
ing during spinal surgery. Spine 1989;14(8):790–8.
[10] Dawson EG, Sherman JE, Kanim LE, et al. Spinal
cord monitoring. Results of the Scoliosis Research
Society and the European Spinal Deformity Society
survey. Spine 1991;16(Suppl 8):S361–4.
[11] Mooney JF 3rd, Bernstein R, Hennrikus WL Jr,
et al. Neurologic risk management in scoliosis sur-
gery. J Pediatr Orthop 2002;22(5):683–9.
[12] Brustowicz RM, Hall JE. In defense of the wake-up
test. Anesth Analg 1988;67(10):1019.
[13] Jones ET, Matthews LS, Hensinger RN. The wake-
up technique as a dual protector of spinal cord
function during spine fusion. Clin Orthop Relat
Res 1982;168:113–8.
[14] Sucato DJ, Elerson E. A comparison between the
prone and lateral position for performing a thoraco-
scopic anterior release and fusion for pediatric spinal
deformity. Spine 2003;28(18):2176–80.
[15] Hedequist DJ, Hall JE, Emans JB. Hemivertebra ex-
cision in children via simultaneous anterior and pos-
terior exposures. J Pediatr Orthop 2005;25(1):60–3.
[16] Hall JE, Herndon WA, Levine CR. Surgical
treatment of congenital scoliosis with or without
Harrington instrumentation. J Bone Joint Surg Am
1981;63(4):608–19.
[17] Winter RB, Moe JH, Lonstein JE. Posterior spinal
arthrodesis for congenital scoliosis. An analysis of
the cases of two hundred and ninety patients, five
to nineteen years old. J Bone Joint Surg Am 1984;
66(8):1188–97.
[18] Lazar RD, Hall JE. Simultaneous anterior and
posterior hemivertebra excision. Clin Orthop Relat
Res 1999;364:76–84.
[19] RufM, Harms J. Hemivertebra resection by a poste-
rior approach: innovative operative technique and
first results. Spine 2002;27(10):1116–23.
[20] Hedequist DJ, Hall JE, Emans JB. The safety and
efficacy of spinal instrumentation in children with
congenital spine deformities. Spine 2004;29(18):
2081–6 [discussion: 2087].
[21] Nakamura H, Matsuda H, Konishi S, et al. Single-
stage excision of hemivertebrae via the posterior ap-
proach alone for congenital spine deformity: follow-
up period longer than ten years. Spine 2002;27(1):
110–5.
[22] O’Brien MF, Lenke LG, Mardjetko S, et al. Pedicle
morphology in thoracic adolescent idiopathic
scoliosis: is pedicle fixation an anatomically viable
technique? Spine 2000;25(18):2285–93.
[23] Kim YJ, Lenke LG, Bridwell KH, et al. Free hand
pedicle screw placement in the thoracic spine: is it
safe? Spine 2004;29(3):333–42 [discussion: 342].
[24] Kuklo TR, Lenke LG, O’Brien MF, et al. Accuracy
and efficacy of thoracic pedicle screws in curvesmore
than 90 degrees. Spine 2005;30(2):222–6.
[25] Ruf M, Harms J. Pedicle screws in 1- and 2-year-old
children: technique, complications, and effect on
further growth. Spine 2002;27(21):E460–6.
[26] HedequistD, Emans J. Congenital scoliosis: a review
and update. J Pediatr Orthop 2007;27(1):106–16.
[27] Kesling KL, Lonstein JE, Denis F, et al. The crank-
shaft phenomenon after posterior spinal arthrodesis
for congenital scoliosis: a review of 54 patients.
Spine 2003;28(3):267–71.
[28] Sink EL, Karol LA, Sanders J, et al. Efficacy of peri-
operative halo-gravity traction in the treatment of
severe scoliosis in children. J Pediatr Orthop 2001;
21(4):519–24.
[29] Suk SI, Chung ER, Lee SM, et al. Posterior vertebral
column resection in fixed lumbosacral deformity.
Spine 2005;30(23):E703–10.
[30] Rinella A, Lenke L, Whitaker C, et al. Perioperative
halo-gravity traction in the treatment of severe sco-
liosis and kyphosis. Spine 2005;30(4):475–82.
[31] Winter RB, Moe JH. The results of spinal arthrode-
sis for congenital spinal deformity in patients youn-
ger than five years old. J Bone Joint Surg Am 1982;
64(3):419–32.
[32] McMaster MJ, David CV. Hemivertebra as a cause
of scoliosis. A study of 104 patients. J Bone Joint
Surg Br 1986;68(4):588–95.
[33] McMaster MJ, Singh H. Natural history of congen-
ital kyphosis and kyphoscoliosis. A study of one
hundred and twelve patients. J Bone Joint Surg
Am 1999;81(10):1367–83.
[34] McMaster MJ, Singh H. The surgical management
of congenital kyphosis and kyphoscoliosis. Spine
2001;26(19):2146–54 [discussion: 2155].
[35] Uzumcugil A, Cil A, Yazici M, et al. Convex growth
arrest in the treatment of congenital spinal defor-
mities, revisited. J Pediatr Orthop 2004;24(6):
658–66.
[36] Ruf M, Jensen R, Harms J. Hemivertebra resection
in the cervical spine. Spine 2005;30(4):380–5.
[37] Polly DW Jr, Rosner MK, Monacci W, et al. Tho-
racic hemivertebra excision in adults via a poste-
rior-only approach. Report of two cases.
Neurosurg Focus 2003;14(2):e9.
[38] Shaw BA. Neurological risk management in scolio-
sis surgery. J Pediatr Orthop 2003;23(4):564 [author
reply: 564].
[39] Winter RB, Moe JH, Lonstein JE. The surgical
treatment of congenital kyphosis. A review of 94
patients age 5 years or older, with 2 years or more
follow-up in 77 patients. Spine 1985;10(3):224–31.

509SURGICAL TREATMENT OF CONGENITAL SCOLIOSIS
[40] Suk SI, Chung ER, Kim JH, et al. Posterior verte-
bral column resection for severe rigid scoliosis. Spine
2005;30(14):1682–7.
[41] Smith JT, Gollogly S, Dunn HK. Simultaneous
anterior-posterior approach through a costotrans-
versectomy for the treatment of congenital kyphosis
and acquired kyphoscoliotic deformities. J Bone
Joint Surg Am 2005;87(10):2281–9.
[42] Blakemore LC, Scoles PV, Poe-Kochert C, et al.
Submuscular Isola rodwith or without limited apical
fusion in the management of severe spinal defor-
mities in young children: preliminary report. Spine
2001;26(18):2044–8.
[43] Akbarnia BA, Marks DS, Boachie-Adjei O, et al.
Dual growing rod technique for the treatment of
progressive early-onset scoliosis: amulticenter study.
Spine 2005;30(Suppl 17):S46–57.
[44] Thompson GH, Akbarnia BA, Kostial P, et al.
Comparison of single and dual growing rod tech-
niques followed through definitive surgery: a prelim-
inary study. Spine 2005;30(18):2039–44.
[45] Tsirikos AI, McMaster MJ. Congenital anomalies
of the ribs and chest wall associated with congenital
deformities of the spine. J Bone Joint Surg Am 2005;
87(11):2523–36.
[46] Campbell RM Jr, Smith MD, Hell-Vocke AK.
Expansion thoracoplasty: the surgical technique
of opening-wedge thoracostomy. Surgical tech-
nique. J Bone Joint Surg Am 2004;86(Suppl 1):
51–64.

Orthop Clin N Am 38 (2007) 511–520
Lenke 1C, King Type II Curves: SurgicalRecommendations
B. Stephens Richards, MDa,b,*aUniversity of Texas Southwestern Medical Center, 5323 Harry Hines Boulevard, Dallas, TX 75390, USA
bTexas Scottish Rite Hospital for Children, 2222 Welborn Street, Dallas, TX 75219, USA
The goals of surgical stabilization for spinal
deformity are to achieve a well-balanced spine inwhich the patient’s head and trunk are centeredover the pelvis, to preserve optimal function of the
patient, and to achieve an appearance that isacceptable to the patient and family. In recentyears, there has been substantial development ofspinal instrumentation systems and surgical tech-
niques, both of which allow for increasingamounts of scoliosis correction. All pedicle screwposterior constructs have gained increased use
by spinal deformity surgeons over the past decade[1–9]. To a lesser extent, thoracoscopic anteriorinstrumentation also has been used [10–13]. With
these newer devices, an increase in curve correc-tion is obtained and greater reduction of the ribprominence is possible; with the use of anterior
implants, preservation of more inferior motionsegments is possible because of shorter constructlengths.
The objectives of this article are twofold. The
first is to discuss the surgical experience in patientswho have Lenke 1C (King type II) curves, inclu-ding the experience with newer instrumentation.
These patients present a significant challenge to thedeformity surgeon because they have structuralthoracic deformities and significant, but nonstruc-
tural, lumbar curves. Over the years, selectiveinstrumentation and fusion of the thoracic curvehave been the primary approach to preservemotion of the lumbar segments, and thus, improve
the long-term outlook. This strategy has been
* Texas Scottish Rite Hospital for Children, 2222
Welborn Street, Dallas, TX 75219.
E-mail address: [email protected]
0030-5898/07/$ - see front matter � 2007 Elsevier Inc. All r
doi:10.1016/j.ocl.2007.05.004
undertaken with the expectation that the uninstru-
mented lumbar curve will allow for a well-balancedspinal column postoperatively. Unfortunately,spinal imbalance following surgery was recognized
in some patients and has been the topic ofnumerous reports in the literature. The secondobjective of this article is to present basic strategiesthat may be helpful when planning for surgery in
these patients.
Lenke 1C (King type II) curves: the terminology
In 1983, King and colleagues [14] introduceda radiographic classification system for adolescentidiopathic scoliosis in which five curve types weredescribed. The two more common curve patterns
were single thoracic curves (type III) and primarythoracic curves accompanied by similar, but sligh-tly smaller, lumbar curves (type II). This classifi-
cation system provided useful recommendationsfor surgical intervention using Harrington instru-mentation. The thoracic curves were fused down
to the stable vertebra (the vertebra in the thoraco-lumbar area that is bisected by the center sacralvertical line [CSVL]), and the overall spinal balance
remained intact. With the evolution of multiplehook or screw implant systems in the late 1980s,which allowed for increased three-dimensionalcurve correction, similar surgical recommendations
were followed. Unexpectedly, in some patientswho had King type II curves, postoperative spinalimbalance occurred following selective thoracic
fusions. At the same time, difficulty in distinguish-ing some curve patterns as King type III curves orKing type II curve patterns led to inconsistencies
in the reporting of the literature.
ights reserved.
orthopedic.theclinics.com

512 RICHARDS
The Lenke classification system for adolescentidiopathic scoliosis was introduced in 1997 andprovided, among other things, a better method to
differentiate King type II curves from King typeIII curves [15,16]. King types II and III curves areincluded in the Lenke type 1 curve pattern, inwhich the primary deformity is a structural main
thoracic curve. If a lumbar curve is also present,it is nonstructural (deemed nonstructural if itmeasures !25� on a supine bend radiograph).
Lumbar spine modifier A, B, or C describes thevariations seen in these lumbar curves (Fig. 1).If the CSVL is located between the pedicles, the
lumbar modifier is A. If the CSVL does not touchany part of the apical vertebral body of the lum-bar curve, the lumbar modifier is C. All othersare classified as having a lumbar modifier B; these
curves generated the most confusion in differenti-ating King type II curves from King type IIIcurves. Even today, some studies report single
overhang curves (like King type III) as Lenke1A/1B curve patterns [17], whereas others reportthoracic curves with significant nonstructural lum-
bar components (like King type II) as Lenke 1B/1C curve patterns [18,19]. Without question, theLenke 1C curve pattern is representative of the
originators’ initial intention of a King type IIcurve and is the primary deformity that is mostat risk for postoperative spinal imbalance
following selective thoracic instrumentation andfusion [1,20]. Furthermore, if the lumbar curvemeasures at least 25� on the preoperative bend ra-
diograph, it is deemed structural, and the scolioticdeformity is classified as a Lenke 3C curve type.Unlike Lenke 1C curves, patients who have Lenke3C curves nearly always require fusion of the tho-
racic and lumbar curves.Spinal deformity surgeons would agree that
Lenke 1A and 1B curves require fusion of the
thoracic curve only, and most, but not all, agreethat selective fusion of Lenke 1C curves is justified[1,19,21]. This article attempts to provide some
general guidelines to help the deformity surgeondecide when selective fusions are appropriate forLenke 1C curves.
Lenke 1C (King type II) curves: the literature
When selective posterior thoracic fusion to thestable vertebra was undertaken in King type II
curve patterns during the Harrington instrumenta-tion era, curve correction approaching 40% wasconsistently reported, and spinal balance was
maintained [22–24]. With the advent of the newer‘‘derotation’’ hook instrumentation systems in thelatter 1980s, selective thoracic fusion continued to
be the most common approach to treatment in thispopulation, often with satisfactory results (Fig. 2).
Fig. 1. (A) In Lenke 1A curves, the CSVL is located between the pedicles at the lumbar spine up to the stable vertebra.
(B) In Lenke 1B curves, CSVL touches the apex of the lumbar curve, between the medial border of the lumbar concave
pedicle and the concave lateral margin of the apical vertebral body. (C) In Lenke 1C curves, the CSVL falls completely
medial to the entire concave lateral aspect of the lumbar apical vertebral body. Lenke 1C curves are most clearly rep-
resentative of King type II curves.

513LENKE 1C, KING TYPE II CURVES
Fig. 2. This patient underwent selective thoracic fusion to the stable vertebra (T12) with excellent balance. The thoracic
curve correction approximated the preoperative supine side-bending radiograph. (A, B) Preoperative radiographs. (C, D)
Radiographs taken 2 years postoperatively.
Over time, reports of spinal imbalance sur-faced, manifested by a shift in the patient’s trunkor head (or both) to the left of midline [25–36].
This undesirable finding was believed to be the re-sult of too much correction of the thoracic curve,a finding usually not seen with Harrington instru-mentation. The uninstrumented lumbar curve be-
low did not spontaneously correct to the extentexpected by review of the preoperative bend ra-diographs. Explanations that have been proposed
to explain this finding include the improper choiceof distal fusion levels, unrecognized lumbar curvestiffness and progression, and the use of incorrect
hook/screw patterns. Instead of two points of fix-ation (as used with Harrington distraction instru-mentation), multiple hooks that rigidly attachedthe rod to the spine imparted stronger corrective
forces to the scoliotic deformity. Once the rodwas seated in the hooks and the scoliosis wascorrected by the 90� rod rotational maneuver, the
forces imparted to the flexible spine below hada deleterious effect on its ability to spontaneouslybalance the instrumented thoracic curve. The
lumbar curves remained larger after surgery thanthe instrumented thoracic curves, and the patientsdecompensated to the left. This was accompanied
by postoperative persistence of obliquity in thelumbosacral region (between L4 and the pelvis),a finding that often was identified preoperatively
butdbased on the bend radiographsdwas ex-pected to improve following surgery [30,34,37].Over time, in most cases in which there was some
postoperative imbalance, improvement occurredas the uninstrumented lumbar curve adapted(Fig. 3).
Failure to properly distinguish King type II
curves from true double major curves was re-sponsible for some instances of postoperativeimbalance following selective thoracic fusions.
Guidelines were developed to help differentiateKing type II and true double major curve patterns[29]. Relative ratios between the thoracic and
lumbar curves with regard to their size, rotation,and deviation from the midline were used to assistthe surgeon in choosing the appropriate candidatefor selective fusion. These relative ratios were
assessed preoperatively on a standing radiograph(ie, thoracic curve parameter/lumbar curve para-meter). If the ratios were less than 1.0, both curves
required fusion. If the ratios were greater than 1.2for curve size and for apical vertebral displace-ment and greater than 1.0 for curve rotation,
selective thoracic fusion could be performed safely.These guidelines were used regularly with thenewer hook–rod instrumentation systems before
the Lenke classification system was developed.Following the newer classification’s development,less emphasis was placed on the relative ratios

514 RICHARDS
Fig. 3. (A, B) This 12-year, 10-month-old girl underwent selective thoracic fusion to the stable vertebra. (C, D) Six weeks
after surgery, she had significant imbalance to the left. She was not braced for this. (E, F) Her balance improved spon-
taneously over time, as seen at the 4-year postoperative evaluation.
between the thoracic and lumbar curves and moreemphasis was again placed on the assessment oflumbar curve flexibility (structural/nonstructural)
and on the lumbar modifiers [16,38]. If the lumbarcurve bends to less than 25�, then it is considereda compensatory nonstructural curve (Lenke 1C or
King type II curve pattern) rather than a structuralcurve (Lenke 3C or double curve pattern). Withtrue double major curves (Lenke 3C), both curves
needed to be included in the posterior fusion toachieve a balanced spine using segmental fixationsystems.

515LENKE 1C, KING TYPE II CURVES
Selective anterior instrumentation has beencompared with posterior hook–rod instrumenta-tion in patients who had Lenke 1B and 1C curves[5,18–20,39,40]. In those undergoing anterior
fusion, the distal extent of the fusion usuallystopped at the end vertebra of the thoracic curveCobb measurement, thus preserving distal motion
segments (Fig. 4). When posterior fusion wasused with hook–rod constructs, the selectivefusion usually extended to the stable vertebra.
Thoracic curve correction (and spontaneouslumbar curve correction) is slightly greater withanterior fusion, but postoperative spinal balance
is similar in both groups. The best coronal bal-ance following surgery is noted when the thoraciccurve is corrected intraoperatively to a measure-ment close to, but not more than that of, the
preoperative thoracic push-prone Cobb measure-ment. In Lenke 1C curves with satisfactorybalance after surgery, patients who undergo pos-
terior fusion have approximately 40% thoraciccurve correction.
Selective posterior fusions using all-hook
constructs also have been compared with pediclescrew constructs in patients who had Lenke 1Ccurve patterns (Fig. 5) [1]. The total levels
instrumented did not vary significantly betweenthese two groups. The amount of correction ofthe thoracic curve obtained surgically and theamount of spontaneous lumbar curve correction
were greater in the pedicle screw group. The inci-dence of postoperative coronal decompensation,defined as a greater than 20-mm shift to the left
of the C7 plumbline, was higher in the hook group(average shift, 21 mm) than in the pedicle screwgroup (average shift, 17.3 mm). This report sug-
gested that increased thoracic curve correction,when using pedicle screws, does not lead to thesame amount of postoperative imbalance as noted
in previous studies using hook constructs. Theinvestigators postulated that screw fixation offersbetter control of the end vertebrae, which preventsdecompensation. They recommended that correc-
tion of the thoracic curve with pedicle screwsshould still mimic the correction obtained ona preoperative push-prone radiograph to mini-
mize potential decompensation of the unfusedcurve.
Not all scoliosis surgeons agree that selective
thoracic fusion in Lenke 1C (King type II) curvesis justified [19,21]. A 2003 multicenter study de-scribed factors that influenced surgeons’ decisions
Fig. 4. (A) Preoperative Lenke 1C curve type with 58� thoracic curve magnitude. (B) The anterior instrumentation ended
at the end vertebra of the thoracic curve (T11), resulting in satisfactory postoperative balance.

516 RICHARDS
Fig. 5. (A) Preoperative thoracic curve measures 60�. (B) Selective thoracic fusion using pedicle screws distally to the
stable vertebra resulted in satisfactory postoperative balance.
about whether to perform a selective thoracic
fusion or to include both curves in the fusion [19].Two hundred and five Lenke 1B and 1C curveswere reported on, all referred to as King-Moetype II curves. Anterior instrumentation and
fusion were performed in 75% of the patients.Posterior instrumentation and fusion were under-taken in the remaining 25%. The investigators
categorized a fusion as being selective if theimplant stopped at L1 or above and nonselectiveif the implant extended to L2 or below. The inci-
dence of including the lumbar curve in the fusionranged from 6% to 33% at the different patientcare sites. Lenke 1C curves had a much higherrate of nonselective fusion when compared with
Lenke 1B curves. Factors associated with nonse-lective fusion included larger preoperative lumbarcurve magnitude, greater displacement of the lum-
bar apical vertebra from the CSVL, and a smallerthoracic/lumbar curve magnitude ratio. The mostagreed upon radiographic determinant for choos-
ing the extent of distal fusion was the absolutemagnitude of the lumbar apical vertebral deviationfrom the CSVL. In those patients who underwent
nonselective fusion, the average displacement ex-ceeded 3 cm from midline. The investigators foundthat side-bending correction of the lumbar curve to
less than 25� was not a sufficient criterion to
perform a selective fusion in some cases.
Surgical recommendations for Lenke 1C
(King type II) curve patterns
When surgery is deemed necessary, all patientswho have Lenke 1C (King type II) curves should
be considered for selective thoracic fusion becausemost would have satisfactory outcomes; however,a small percentage of patients will be identified
preoperatively who may not qualify for selectivethoracic fusion. The criteria used to identifythem are listed later. For most patients who are
candidates for selective fusion, recommendationsfor the distal level of fusion vary little, regardlessof the type of posterior instrumentation used. Ifhook–rod constructs are used, the fusion should
be extended to, but never past, the stable vertebra.Fusing one or two levels lower than this tends toshift the patient’s trunk further to the left. If the
CSVL bisects a disk space instead of a vertebra,the instrumentation should end on the vertebraimmediately above. If the thoracic curve is fused
shorter than this when using hooks, postoperativeadding-on of the thoracic curve has been reported(Fig. 6). If posterior pedicle screw fixation is used,

517LENKE 1C, KING TYPE II CURVES
Fig. 6. (A, B) Preoperative radiographs of a 13-year-old girl who underwent selective thoracic fusion ending one level
above the stable vertebra. (C, D) Two weeks postoperatively, her balance was excellent. (E, F) One year following
surgery, adding-on of the thoracic curve was evident radiographically.

518 RICHARDS
similar criteria should be followed, despite theknowledge that pedicle screws may generategreater curve correction.
Overcorrection, or excessive straightening, ofthe thoracic curve must be avoided. This pointrequires a great deal of emphasis. A straighterspine immediately after surgery is not a better
result if it leads to postoperative decompensation.When hook–rod constructs are used, the moresuccessful outcomes with regard to spinal balance
are found in patients whose mean thoraciccorrection at 2-year follow-up is modest (40%).If rotation is used as the corrective maneuver,
the rotation maneuver of the primary rod shouldbe less than a complete 90�. If done this way,the uninstrumented lumbar curve has an excellentchance to compensate satisfactorily [18,22,27,
32,36]. Translational correction or distraction/compression correction, instead of rotational cor-rection, may reduce the chance of creating postop-
erative imbalance [41]. With the use of posteriorpedicle screw constructs, surgeons may considertrying to achieve an increased amount of thoracic
curve correction because greater amounts of spon-taneous lumbar correction have been reported.Despite this, the surgeon should be cautious
when considering correcting the thoracic curvebeyond the amount noted on a preoperative push-prone radiograph, the test most often referred to
as being predictive of the outcome [18]. If a push-prone radiograph has not been obtained, thethoracic curve correction noted on the preopera-
tive supine bend radiograph may give an estima-tion of desired correction.
In the past several years, more experience hasbeen gained with selective anterior thoracic fusion
in Lenke 1C curves using instrumentation onthe convexity of the thoracic curve. If anteriorinstrumentation and fusion are considered, the
distal level should stop at the end vertebra of themeasured thoracic curve. This will allow fora greater number of residual mobile segments
below the fusion than can be expected whenposterior instrumentation is used. As noted withposterior instrumentation, the desired correction ofthe instrumented segment should remain limited
(approximating the push-prone thoracic curvecorrection) to avoid spinal imbalance.
Some patients who have Lenke 1C patterns
may not be candidates for selective thoracicfusions. These patients have large lumbar curvesthat approximate the thoracic curve size and have
significant rotation, and they may present clini-cally with a notable convex-side clinical paralum-bar prominence. Although the flexibility of these
lumbar curves (as noted on side-bending radio-graphs) is sufficient to still be classified as Lenke1C, the lumbar deformity may be too prominent
Fig. 7. (A, B) Radiographs taken before selective thoracic fusion was performed, despite the notable kyphosis at
the thoracolumbar junction. (C, D) Six months postoperatively, the junctional kyphosis was more noticeable
radiographically.

519LENKE 1C, KING TYPE II CURVES
to be left unaddressed. Although patients whohave larger lumbar curves (O50�) have beentreated successfully with selective fusions, somewarrant strong consideration for fusion of tho-
racic and lumbar curves. Although no absolutelumbar curve magnitude has been identified thatalways requires lumbar fusion, the surgeon should
be cautious about performing selective fusionswhen a large amount of paraspinal lumbarprominence is noted clinically, the lumbar curve
exceeds 50� to 55�, and the lumbar apical vertebrais displaced more than 3 cm away from midline.
The sagittal contour at the thoracolumbar
junction also must be assessed preoperativelyfrom the radiographic and clinical perspectives[42]. If prominent kyphosis is noted in this loca-tion, the lumbar curve may need to be included
in the fusion to avoid exacerbating this localizedsagittal deformity following surgery (Fig. 7).With Lenke’s classification system, if the T10–L2
kyphosis measures more than 20�, the thoraco-lumbar region is considered ‘‘structural,’’ andthe recommendation is made to extend the fusion
distal to this level. Some spinal deformity sur-geons may elect to carry the fusion further inferi-orlydeven with lesser amounts of localized
thoracolumbar kyphosisdto limit the chance ofa postoperative junctional problem in the sagittalplane [19].
Summary
Lenke 1C (King type II) curves present a signi-ficant challenge to the scoliosis surgeon. Selectivethoracic fusions preserve motion of the lumbar
spine and often lead to a satisfactory outcome,particularly if overcorrection of the thoracic curveis avoided. Still, spinal imbalance following sur-
gery remains the most significant preoperativeconcern and requires detailed planning.
References
[1] Dobbs MB, Lenke LG, Kim YJ, et al. Selective
posterior thoracic fusions for adolescent idiopathic
scoliosis: comparison of hooks versus pedicle screws.
Spine 2006;31:2400–4.
[2] Lee S-M, Suk S-I, Chung E-R. Direct vertebral rota-
tion: a new techniqueof three-dimensional deformity
correction with segmental pedicle screw fixation in
adolescent idiopathic scoliosis. Spine 2004;29:343–9.
[3] Lenke LG. Debate: Resolved, a 55 degrees right
thoracic adolescent idiopathic scoliotic curve should
be treated by posterior spinal fusion and segmental
instrumentation using thoracic pedicle screws: Pro:
Thoracic pedicle screws should be used to treat a 55
degrees right thoracic adolescent idiopathic scoliosis.
J PediatrOrthop 2004;24:329–34 [discussion: 338–1].
[4] Liljenqvist UR, Halm HF, Link TM. Pedicle screw
instrumentation of the thoracic spine in idiopathic
scoliosis. Spine 1997;22:2239–45.
[5] Potter BK, Kuklo TR, Lenke LG. Radiographic
outcomes of anterior spinal fusion versus posterior
spinal fusion with thoracic pedicle screws for treat-
ment of Lenke Type I adolescent idiopathic scoliosis
curves. Spine 2005;30:1859–66.
[6] Storer SK, Vitale MG, Hyman JE, et al. Correction
of adolescent idiopathic scoliosis using thoracic ped-
icle screw fixation versus hook constructs. J Pediatr
Orthop 2005;25:415–9.
[7] Suk SI, Kim WJ, Lee SM, et al. Thoracic pedicle
screw fixation in spinal deformities: are they really
safe? Spine 2001;26:2049–57.
[8] Suk SI, Lee CK, Kim WJ, et al. Segmental pedicle
screw fixation in the treatment of thoracic idiopathic
scoliosis. Spine 1995;20:1399–405.
[9] Suk SI, Lee SM, Chung ER, et al. Selective thoracic
fusion with segmental pedicle screw fixation in the
treatment of thoracic idiopathic scoliosis: more
than 5-year follow-up. Spine 2005;30:1602–9.
[10] Newton PO. Thoracoscopic treatment of pediatric
spinal deformity. Seminars in Spine Surgery 2003;
15:244–51.
[11] Newton PO, Parent S, Marks M, et al. Prospective
evaluation of 50 consecutive scoliosis patients surgi-
cally treated with thoracoscopic anterior instrumen-
tation. Spine 2005;30:S100–9.
[12] Sucato DJ. Thoracoscopic anterior instrumentation
and fusion for idiopathic scoliosis. J Am Acad
Orthop Surg 2003;11:221–7.
[13] Wong HK, Hee HT, Yu Z, et al. Results of thoraco-
scopic instrumented fusion versus conventional pos-
terior instrumented fusion in adolescent idiopathic
scoliosis undergoing selective thoracic fusion. Spine
2004;29:2031–8 [discussion: 2039].
[14] KingHA,Moe JH, BradfordDS, et al. The selection
of fusion levels in thoracic idiopathic scoliosis.
J Bone Joint Surg Am 1983;65:1302–13.
[15] Lenke LG, Betz RR, Harms J, et al. A new and
reliable 3-dimensional classification system of ado-
lescent idiopathic scoliosis. St. Louis (MO): Scoliosis
Research Society; 1997.
[16] Lenke LG, Betz RR, Harms J, et al. Adolescent
idiopathic scoliosis: a new classification to determine
extent of spinal arthrodesis. J Bone Joint Surg Am
2001;83:1169–81.
[17] Kuklo TR, O’Brien MF, Lenke LG, et al. Compar-
ison of the lowest instrumented, stable, and lower
end vertebrae in ‘‘single overhang’’ thoracic adoles-
cent idiopathic scoliosis: anterior versus posterior
spinal fusion. Spine 2006;31:2232–6.
[18] Dobbs MB, Lenke LG, Walton T, et al. Can we
predict the ultimate lumbar curve in adolescent
idiopathic scoliosis patients undergoing a selective

520 RICHARDS
fusion with undercorrection of the thoracic curve?
Spine 2004;29:277–85.
[19] Newton PO, Faro FD, Lenke LG, et al. Factors
involved in the decision to perform a selective versus
nonselective fusionofLenke1Band1C(King-MoeII)
curves in adolescent idiopathic scoliosis. Spine 2003;
28:S217–23.
[20] EdwardsCC2nd,LenkeLG,PeelleM, et al. Selective
thoracic fusion for adolescent idiopathic scoliosis
with C modifier lumbar curves: 2- to 16-year radio-
graphic and clinical results. Spine 2004;29:536–46.
[21] Lenke LG, Betz RR, Haher TR, et al. Multisurgeon
assessment of surgical decision-making in adolescent
idiopathic scoliosis: curve classification, operative
approach, and fusion levels. Spine 2001;26:2347–53.
[22] McCance SE, Denis F, Lonstein JE, et al. Coronal
and sagittal balance in surgically treated adolescent
idiopathic scoliosis with the King II curve pattern.
A review of 67 consecutive cases having selective
thoracic arthrodesis. Spine 1998;23:2063–73.
[23] McCance SE, Winter RB, Lonstein JE. A King type
II curve pattern treated with selective thoracic fu-
sion: case report with 44-year follow-up. J Spinal
Disord 1999;12:262–5.
[24] Winter RB, Lonstein JE. A meta-analysis of the
literature on the issue of selective thoracic fusion
for the King-Moe type II curve pattern in adolescent
idiopathic scoliosis. Spine 2003;28:948–52.
[25] Arlet V, Marchesi D, Papin P, et al. Decompen-
sation following scoliosis surgery: treatment by de-
creasing the correction of the main thoracic curve
or ‘‘letting the spine go’’. Eur Spine J 2000;9:156–60.
[26] Bassett GS, Hensinger MC, Keiper MD. Effect of
posterior spinal fusion on spinal balance in idio-
pathic scoliosis. J Pediatr Orthop 1989;9:672–4.
[27] Benli IT, Tuzuner M, Akalin S, et al. Spinal imbal-
ance and decompensation problems in patients
treated with Cotrel-Dubousset instrumentation. Eur
Spine J 1996;5:380–6.
[28] Bridwell KH, McAllister JW, Betz RR, et al. Coro-
nal decompensation produced by Cotrel-Dubousset
‘‘derotation’’ maneuver for idiopathic right thoracic
scoliosis. Spine 1991;16:769–77.
[29] Lenke LG, Bridwell KH, Baldus C, et al. Preventing
decompensation in King type II curves treated with
Cotrel-Dubousset instrumentation. Strict guidelines
for selective thoracic fusion. Spine 1992;17:S274–81.
[30] Mason DE, Carango P. Spinal decompensation in
Cotrel-Dubousset instrumentation. Spine 1991;16:
S394–403.
[31] McCall RE, BronsonW. Criteria for selective fusion
in idiopathic scoliosis using Cotrel-Dubousset in-
strumentation. J Pediatr Orthop 1992;12:475–9.
[32] Moore MR, Baynham GC, Brown CW, et al.
Analysis of factors related to truncal decompensa-
tion following Cotrel-Dubousset instrumentation.
J Spinal Disord 1991;4:188–92.
[33] Patwardhan AG, Rimkus A, Gavin TM, et al.
Geometric analysis of coronal decompensation in
idiopathic scoliosis. Spine 1996;21:1192–200.
[34] Richards BS. Lumbar curve response in type II
idiopathic scoliosis after posterior instrumentation
of the thoracic curve. Spine 1992;17:S282–6.
[35] Richards BS, Birch JG, Herring JA, et al. Frontal
plane and sagittal plane balance following Cotrel-
Dubousset instrumentation for idiopathic scoliosis.
Spine 1989;14:733–7.
[36] Thompson JP, Transfeldt EE, Bradford DS, et al.
Decompensation after Cotrel-Dubousset instru-
mentation of idiopathic scoliosis. Spine 1990;15:
927–31.
[37] Schwender JD, Denis F. Coronal plane imbalance in
adolescent idiopathic scoliosis with left lumbar
curves exceeding 40 degrees: the role of the lumbosa-
cral hemicurve. Spine 2000;25:2358–63.
[38] Lenke LG, Edwards CC 2nd, Bridwell KH. The
Lenke classification of adolescent idiopathic scolio-
sis: how it organizes curve patterns as a template
to perform selective fusions of the spine. Spine 2003;
28:S199–207.
[39] Betz RR,Harms J, Clements DH 3rd, et al. Compar-
ison of anterior and posterior instrumentation for
correction of adolescent thoracic idiopathic scolio-
sis. Spine 1999;24:225–39.
[40] Lenke LG, Betz RR, Bridwell KH, et al. Spontane-
ous lumbar curve coronal correction after selective
anterior or posterior thoracic fusion in adolescent
idiopathic scoliosis. Spine 1999;24:1663–71 [discus-
sion: 1672].
[41] Goshi K, Boachie-Adjei O, Moore C, et al. Thoracic
scoliosis fusion in adolescent and adult idiopathic
scoliosis using posterior translational corrective
techniques (Isola): is maximum correction of the
thoracic curve detrimental to the unfused lumbar
curve? Spine J 2004;4:192–201.
[42] Lowe TG, Lenke L, Betz R, et al. Distal junctional
kyphosis of adolescent idiopathic thoracic curves
following anterior or posterior instrumented fusion:
incidence, risk factors, and prevention. Spine 2006;
31:299–302.

Orthop Clin N Am 38 (2007) 521–529
Classification of Operative Adolescent IdiopathicScoliosis: Treatment Guidelines
Peter S. Rose, MD, Lawrence G. Lenke, MD*Washington University Orthopedics, Washington University School of Medicine, Washington University
Medical Center, 660 South Euclid Avenue, Campus Box 8233, Suite 11300 West Pavilion,
St. Louis, MO 63110-1093, USA
Idiopathic scoliosis may present in infant,juvenile, or adolescent patients. Infantile idio-
pathic scoliosis presents in children age 0 to 3years and accounts for approximately 1% ofidiopathic curves. Juvenile idiopathic curves pres-
ent at between 4 and 9 years of age and accountfor 12% to 31% of curves [1]. Adolescent idio-pathic scoliosis (AIS) constitutes most remainingcases, presenting in patients between age 10 years
and adulthood. This article focuses on the classifi-cation and treatment of patients who have AIS.
Idiopathic scoliosis is a diagnosis of exclusion
made after a patient has been evaluated forunderlying congenital, syndromic, or neurologiccauses. By definition, a coronal curve of 10� or
more must be present to diagnose scoliosis, withlesser curves being termed spinal asymmetry toavoid overdiagnosing patients who have minimaldeformities. Approximately 80% of curves ulti-
mately are diagnosed as idiopathic [1].The prevalence of AIS is estimated at approx-
imately 2% to 3%; however, the prevalence de-
creaseswith increasing curve severity. For example,20� curves have a prevalence of approximately0.5%, whereas 40� curves have a prevalence of
only 0.1%. AIS is more common in girls than inboys, with a ratio of 9:1 in curves larger than 40�.
Treatment of AIS may be observational, brac-
ing, or surgical. Observation may be indicated incurves less than 25� in skeletally immature
* Corresponding author.
E-mail address: [email protected]
(L.G. Lenke).
0030-5898/07/$ - see front matter � 2007 Elsevier Inc. All r
doi:10.1016/j.ocl.2007.06.001
patients and for curves up to 45� to 50� inskeletally mature patients. Bracing is considered
in skeletally immature patients with curves be-tween 25� and 45� to 50�. Surgical treatment isconsidered in patients with progressive curves
greater than 40� that fail or cannot toleratebracing and those with curves greater than 45�
at skeletal maturity.
Classification
Researchers have sought to classify AIS curves
to allow comparison of outcome and to providetreatment guidelines. The King-Moe classifica-tion, published in 1983 after an evaluation ofmore than 400 patients who had AIS, was the first
broadly applied classification of patients in the eraof instrumented spinal fusions [2]. Although lim-ited in that it only analyzed thoracic curves and
only addressed coronal plane deformity, thiswork led to the development of the first AIS treat-ment guidelines. This classification system suf-
fered from only fair intra- and interobserverreliability, but provided the gold standard forcurve classification for 2 decades [3,4].
In 2001, Lenke and colleagues [5] provideda more comprehensive AIS classification system.This system provided for analysis of all AIS curvesrather than just thoracic curves, set forth objective
criteria for determining curve flexibility, and ad-dressed coronal and sagittal plane deformities.
The Lenke classification system consists of
a three-tiered analysis of curves based on curvetype, lumbar modifier, and sagittal modifier.Evaluation requires upright long-cassette coronal
and lateral radiographs as well as side-bending
ights reserved.
orthopedic.theclinics.com

522 ROSE & LENKE
radiographs. Once a curve is classified, this systemprovides a template for the selection of fusionlevels by curve type.
Curve classification
The first step of classification is to identify the
curve type (Table 1). The proximal thoracic (PT),main thoracic (MT), and thoracolumbar/lumbar(TL/L) curves are measured using the Cobb tech-
nique. The larger of the latter two is consideredthe major curve. Lesser curves are termed minorand are considered structural if they remain at
least 25� on side-bending films. Additionally,hyperkyphosis in the PT region (T2–T5R20�) orthoracolumbar junction (T10–L2R20�) rendersthese curves structural, regardless of their side-
bending measurement. PT curves are alwaysminor, but they may be structural or nonstruc-tural depending on their bending characteristics
and local kyphosis.Second, the lumbar spine modifier is deter-
mined by the position of the apex of the lumbar
curve with respect to the center sacral vertical line(CSVL) (Fig. 1). The CSVL is the vertical linefrom the geometric center of S1, which determines
the coronal position of the lumbar spine in rela-tion to the pelvis. For greatest accuracy, a shoelift should be used if there is more than 2 cm ofpelvic obliquity. The stable vertebra is the most
cephalad vertebra below the major curve whosecenter is most closely bisected by the CSVL. Ifthe CSVL falls between the pedicles of the verte-
bra up to the stable vertebra, the curve has a lum-bar modifier A. If the CSVL touches the pedicle ofthe apical vertebra, lumbar modifier B is used.
Finally, if the CSVL falls outside of the lateral as-pect of the lumbar apical vertebral body (or bod-ies if the apex is a disc), lumbar modifier C is used.
When in doubt as to the correct lumbar modifier,modifier B is used.
Third, the sagittal thoracic modifier is selectedas ‘‘�,’’ ‘‘N,’’ or ‘‘þ,’’ based on the T5–T12
kyphosis. If sagittal kyphosis is more than 10�,the ‘‘�’’ or hypokyphotic modifier is used; for 10�
to 40�, the ‘‘N’’ or normal modifier is used; and
for more than 40� of kyphosis, the ‘‘þ’’ orhyperkyphotic modifier is used.
In total, the six curve types, three lumbarmodifiers, and three sagittal modifiers define 42
curve patterns (one might expect 54, but becauseall operative TL/L curves are completely deviatedfrom themidline andhave typeC lumbarmodifiers,
only 42 result). A curve is specified as ‘‘type þlumbar modifier þ sagittal modifier,’’ such as1AN, 5CN, and so forth.
The type 1 (single thoracic) curve is the mostcommon (see Table 1). A recent study found thatfive classifications account for 60% of surgicallytreated curves (1AN ¼ 19%, 1BN ¼ 11%,
2AN ¼ 10%, 5CN ¼ 10%, and 1CN ¼ 8%).Overall, lumbar modifier A was the most common(41%) followed by B (37%) and C (22%). Normal
kyphosis was seen in 75% of curves, with 14%hypokyphotic and 11% hyperkyphotic [6].
This classification system has been evaluated
by the developers, an independent group ofsurgeons from the Scoliosis Research Society,and an international group of surgeons. On
premeasured radiographs, this system had betterintra- and interobserver reliability than the King-Moe system [7,8]. Both systems have decreasedreliability on unmeasured radiographs, consistent
with the known variability of Cobb angle levelselection and measurement [3].
Treatment guidelines
The Lenke classification system is designed to
allow surgeons to plan operative treatment basedon this curve classification. The general principleof the system is that the major curve and
structural minor curves should be fused and thatnonstructural minor curves may be allowed tocorrect spontaneously following fusion of thestructural curves.
Table 1
Description of 6 Lenke Curve Types
Curve type Proximal thoracic Main thoracic Thoracolumbar/lumbar Description Prevalence
1 Nonstructural Structural Nonstructural Main thoracic 51%
2 Structural Structural Nonstructural Double thoracic 20%
3 Nonstructural Structural Structural Double major 11%
4 Structural Structural Structural Triple major 3%
5 Nonstructural Nonstructural Structural Thoracolumbar/lumbar 12%
6 Nonstructural Structural Structural Thoracolumbar/lumbar–
main thoracic
3%

523OPERATIVE ADOLESCENT IDIOPATHIC SCOLIOSIS
Fig. 1. (A) Lenke classification system. (B) Lumbar spine modifier rules. (From Lenke LG, Betz RR, Harms J, et al.
Adolescent idiopathic scoliosis: a new classification to determine extent of spinal arthrodesis. J Bone Joint Surg Am
2001;83-A(8):1169–81; with permission.)

524 ROSE & LENKE
In preparation for selection of fusion levels,a careful assessment of the patient’s medicalstatus, activity level, and clinical appearance
should be made. It is the authors’ practice toobtain pulmonary function tests preoperatively onall patients. Known cardiopulmonary compro-mise may dictate that a posterior fusion is pre-
ferred over an anterior approach to avoidpulmonary insult of a thoracotomy. Similarly,the clinical appearance of shoulder height and
symmetry is important in the selection of fusionlevels. Simple correction of a thoracic curve ina patient with level shoulders before surgery often
results in postoperative shoulder imbalance. Care-ful preoperative consideration will lead to theselection of a more cephalad fusion level to allowbetter control over postoperative shoulder
balance.
Type 1: main thoracic curves
The general guideline for these commonly
encountered curves is to perform a selective ante-rior or posterior fusion of the MT curve, regard-less of the lumbar spine or sagittal thoracic
modifier. Segmental spinal instrumentation allowsexcellent correction of the MT curve and theultimate lumbar curve response after may be
predicted by the preoperative push-prone radio-graph [9]. In the absence of shoulder height con-siderations, the nonstructural proximal curveneed not be included in the fusion [10].
Instrumented posterior spinal fusion from theneutral vertebra above to the stable vertebrabelow (or stable minus one or two levels as defined
below) is the traditional treatment of these curves.Posterior segmental spinal instrumentation andfusion are indicated in type 1 curves with a normal
or hyperkyphotic sagittal profile and in patientswith diminished pulmonary function (in whomthis approach avoids violation of the chest cavity).
Pedicle screw fixation allows for true three-di-mensional deformity correction through a verte-bral derotation maneuver [11].
For the patient with right shoulder elevation,
proximal fusion to T4 or T5 usually allowsleveling of the shoulders in a right thoracic curve.Strong consideration should be given to extending
the upper instrumented vertebra (UIV) to T4 oreven T3 if the shoulders are level before surgery toprevent a high left shoulder postoperatively. If the
left shoulder is high before surgery, the UIV likelyneeds to be T2 to maintain adequate control ofshoulder alignment.
In selecting the lower instrumented vertebra(LIV), the stable vertebra is defined as the mostproximal vertebra whose pedicles are bisected by
the CSVL. The ‘‘stable minus one’’ vertebra is onelevel proximal to this and generally is the vertebratouched by the CSVL in the lateral body/pedicleregion. Alternatively, the lower end vertebra
(LEV) of the MT curve is another landmarkvertebra, with the LIV typically one level caudalto that.
Most type 1 MT curves can be fused to the‘‘stable minus one’’ vertebra. Suk and colleagues[12] analyzed the fusion level in 42 patients with
single thoracic curves followed for a minimumof 2 years. In this study, uniformly good resultswere obtained when patients were fused to theneutral vertebra when there was no more than
a two-level difference between the neutral vertebraand the end vertebra. In general, this corre-sponded to the ‘‘stable minus one’’ level. In
patients with more than a two-level difference be-tween the end vertebra and the neutral vertebra,success was predictable when fusions were ex-
tended to the ‘‘neutral minus one’’ level (generallyconsistent with the ‘‘stable minus two’’ level).When shorter fusions were attempted, there was
a high likelihood of lumbar decompensation.Consideration to limit the fusion to the ‘‘stableminus two’’ vertebra should be taken in thesecurves based on assessment of curve flexibility,
intraoperative correction, and residual angulationand parallelism of the LIV disc.
Anterior spinal fusion may be selected in type
1 curves, particularly when there is hypokyphosisor a ‘‘C’’ lumbar modifier. Anterior fusion may bepreferred in a patient who is skeletally immature
to minimize the risk for crankshaft phenomenonfrom subsequent growth. Because anterior fusiontends to increase kyphosis, whereas posteriorfusion tends to decrease it, anterior fusion may
not be suitable in patients with preoperative high-normal or hyperkyphosis [13].
In general, the results of appropriately selected
anterior fusion are equivalent to those of posteriorfusion [14]. Retrospective data showed that an an-terior approach to 1A/B curves can result in
a mean shorter fusion of 1.5 vertebral levels [15].The spontaneous correction of the PT curve maybe better following anterior fusion [16]; however,
the use of segmental thoracic pedicle screw fixa-tion increased instrumented curve correction,improved spontaneous lumbar compensatorycurve correction, and improved thoracic torsion
and rotation [17].

525OPERATIVE ADOLESCENT IDIOPATHIC SCOLIOSIS
Particular consideration should be paid to thetreatment of the type 1C curve (Fig. 2). Selectivethoracic fusion may be considered for thesecurves because the lumbar curve, although large
and deviated, generally is flexible with good po-tential for spontaneous correction. When contem-plating whether a 1C curve is a candidate for
a selective thoracic fusion, clinical and radio-graphic analysis is required. The thoracolumbarjunction should not be hyperkyphotic, the left
shoulder should not be high, and the thoracic
prominence and shift should dominate over thelumbar deformity. Comparison can be made tothe ratio of the Cobb measurement, scoliometermeasurement, and apical translation and rotation
of the MT and TL/L regions; ratios greater than1.25 predict successful thoracic fusion in these pa-tients [18–21].
A combined anterior and posterior approachto a type 1 curve is rarely required in the era ofposterior segmental spinal instrumentation [22].
Relative indications include severe, stiff curves
Fig. 2. 5Cþ curve treated with selective anterior fusion. (A–G) Preoperative radiographs and clinical photographs.
(A) Anteroposterior (AP). (B) Left side bending. (C) Right side bending. (D) Lateral. (E) Close posteroanterior (PA).
(F) Forward bend lumbar. (G) Forward bend thoracic. (H–K) Postoperative radiographs and clinical photographs.
(H) AP. (I) Lateral. (J) Close PA. (K) Forward bend.

526 ROSE & LENKE
Fig. 2 (continued)
(O90�–100� upright, O60�–70� residual curve onbending films), severe lordosis or hyperkyphosis,and highly skeletally immature patients.
Type 2: double thoracic curves
These curves are distinguished by structural PTand MT regions; they are the second most com-monly encountered operative AIS curves. Treat-
ment is posterior fusion of both curves.Determining the UIV requires careful assessmentof shoulder height before surgery. Increasing cor-
rection of the right MT curve tends to elevate theleft shoulder. Patients with a high left shoulderrequire instrumentation and fusion extending
proximally to T2. In patients with level shoulders,the UIV should be T2 or T3, depending on thecorrection and resulting shoulder balance achieved.
In patients with a high right shoulder, T3 usuallycan be used as the UIV. During correction,compression is placed on the convex side of thePT curve and distraction on the concavity. Because
the PT curve usually is hyperkyphotic, convexcompression is applied before concave distractionto avoid worsening the local kyphosis.
Suk and colleagues [23] reported results in ac-cordance with these recommendations in analyz-ing 40 patients with PT curves greater than 25�;they found improved results with fusion of theproximal curve whenever the shoulders were levelor higher on the side of the proximal thoracic
curve. In preoperative evaluation, the clavicleangle provides the best radiographic assessmentof shoulder balance [24].
The LIV is selected similarly to the selectionrules of type 1 curves. Generally, the mostproximal lumbar vertebra intersected by the
CSVL may serve as the LIV. Combined anteriorand posterior fusions are rarely needed in thetreatment of double thoracic curves.
Type 3: double major curves
Type 3 curves include a major MT curve and astructural TL/L curve. Type 3 curves are the thirdmost common (11%); they present most often
with a ‘‘C’’ lumbar modifier. Treatment generallyrequires posterior instrumentation and fusion ofboth curves. Hyperkyphosis of the thoracolumbar
junction is present frequently (T10–L2O20�) andshould be normalized intraoperatively.
The UIV selected may be T3–5, depending onthe size and stiffness of the nonstructural PT curve
and any shoulder asymmetry. The LIV is usuallyL3 or L4 with the level determined by the mostproximal lumbar level intersected by the CSVL.
The surgical goal should be horizontalization,centralization, and neutralization of the levelchosen as the LIV; critical attention should be
paid to making the LIV disc horizontal.Some 3C curves can be treated with selective
thoracic fusion. Prerequisites to this approach are

527OPERATIVE ADOLESCENT IDIOPATHIC SCOLIOSIS
lack of junctional kyphosis and a clinical de-formity that predominates in the thoracic spine.Additionally, a rare severe and stiff thoracic orlumbar curve may require anterior release or
circumferential fusion.
Type 4: triple major curves
Type 4 curves are rare, accounting for approx-imately 3% of all operative curves. The PT, MT,
and TL/L curves are all structural; the MT orTL/L may be the major curve. Treatment is byposterior segmental instrumentation and fusionfrom the upper thoracic spine to L3 or L4. The
UIV generally is T2 or T3, with the level de-termined in the same manner as the UIV for type 2double thoracic curves. The LIV should achieve
horizontalization, centralization, and stabilizationusing the same criteria as the LIV in type 3 doublemajor curves. In the rare case of a large and stiff
Fig. 3. (A–F) 1CN curve treated with fusion of major curve only. Preoperative radiographs and clinical photographs.
(A) Anteroposterior (AP). (B) Left side bending. (C) Right side bending. (D) Lateral. (E) Close posteroanterior (PA).
(F) Forward bend. (G–J) Postoperative radiographs and clinical photographs. (G) AP. (H) Lateral. (I) Close PA. (J) For-
ward bend.

528 ROSE & LENKE
MTor TL/L curve, anterior release and fusionmaybe needed. Optimal correction is achieved bypedicle screw fixation of all three curves to allow se-
cure fixation for correction and realignment.
Type 5: thoracolumbar/lumbar curves
Type 5 curves have only the TL/L region as
a structural curve, which may be fused anteriorlyor posteriorly (Fig. 3). When fused anteriorly,treatment is from the upper end vertebra (UEV)to the LEV (to include all levels with convex discs).
With transpedicular fixation, these curves can betreated posteriorly over the same levels or to oneadditional caudal level. In cases in which some re-
sidual MT or PT curve is expected to remain, theUIV may be left deliberately tilted to correspondto the amount of residual MT curve expected.
When fusing only the TL/L region of thecurve, secondary correction of the compensatorythoracic curve tends to elevate the left shoulder.
Additionally, there is little change in the ribdeformity with limited TL/L fusions, so theclinical appearance of the thoracic region beforesurgery must be acceptable to the patient.
Sanders and colleagues [25] reported on 49 pa-tients who underwent selective anterior fusion ofthoracolumbar curves with a minimum 2-year fol-
low-up. Successful selective fusion was dependenton patient maturity and curve characteristics.Forty-two of 43 patients with closed triradiate car-
tilages had a successful outcome following selectivecurve fusion. Similarly, 42 of 44 patients who hada thoracolumbar/thoracic Cobb angle ratio of at
least 1.25 or a thoracic curve that bent up to 20�
achieved a good outcome with selective fusion ofthe thoracolumbar curve.
Type 6: thoracolumbar/lumbar–main thoraciccurves
These curves combine a TL/L curve with
a structural minor, MT curve. General treatmentrecommendations are to treat the MT and TL/Lcurves posteriorly. The UIV varies from T3–5with the MT curve location and shoulder height.
The LIV is the most proximal lumbar vertebratouched by the CSVL, usually L3 or L4.
A selective anterior fusion of only the TL/L
curve can be considered (similar to a type 5 curve).Such treatment presupposes that the residual tho-racic curve has acceptable radiographic appearance
and that thoracic and shoulder clinical asymmetryare acceptable. Patients should have closed tri-radiate cartilages to consider such anapproach [25].
Outcomes
The Lenke classification is designed as a tool toguide the surgical treatment of AIS curves. Studies
have found good intra- and interobserver reliabil-ity of the system, particularly when the errors ofCobb measurement are eliminated [3,4,26]. A ret-rospective analysis of 606 surgical curves treated
before the development of this classification wasperformed to assess how well this new systemwould predict treatment. Overall agreement be-
tween the classification system and surgical treat-ment was 90%, with individual curve typesvarying between 75% and 95%. Similarly, Puno
and colleagues [27] retrospectively applied theLenke classification treatment recommendationsto 183 patients with a greater than 2-year follow-up. Better correctiondin avoiding undercorrection
of the structural secondary curves and in avoidingunnecessary fusion of nonstructural curvesdwasseen in patients treated in accordance with the
Lenke criteria recommendations.Disagreement remains in the selection of fusion
levels. In a roundtable discussion of 28 scoliosis
surgeons, exact treatment levels varied widely,even when agreement on curve types was reached[26]. Similarly, in analyzing data of 203 patients
from the Harms Study Group, Newton and col-leagues [28] reported considerable variations of se-lective fusion of Lenke 1B and 1C curves acrossthe five study sites.
Summary
The Lenke classification system providesa comprehensive and biplanar system to evaluate
patients who have AIS. The system has improvedintra- and interobserver reliability compared withthe King-Moe system and has the ability to directsurgical treatment for successful management.
Curve flexibility and the potential for selectivefusions may be assessed objectively. Additionally,the system provides for grouping of similar curve
types to facilitate research into various treatmentmethods. Reports in the literature suggest that theclassification guidelines provide appropriate guid-
ance for the selection of fusion levels.
References
[1] Newton PO, Wenger DR. Idiopathic scoliosis. In:
Morrissy RT, Weinstein SL, editors. Lovell and
Winter’s pediatric orthopaedics. 6th edition.

529OPERATIVE ADOLESCENT IDIOPATHIC SCOLIOSIS
Baltimore (MD): Lippincott Williams & Wilkins;
2006. p. 693–762.
[2] KingHA,Moe JH, BradfordDS, et al. The selection
of fusion levels in thoracic idiopathic scoliosis.
J Bone Joint Surg Am 1983;65:1302–13.
[3] Niemeyer T, Wolf A, Kluba S, et al. Interobserver
and intraobserver agreement ofLenke andKing clas-
sifications for idiopathic scoliosis and the influenceof
level of professional training. Spine 2006;31:2103–7.
[4] Richards BS, Sucato DJ, Konigsberg DE, et al.
Comparison of reliability between the Lenke and
King classification systems for adolescent idiopathic
scoliosis using radiographs that were not premeas-
ured. Spine 2003;28:1148–56.
[5] Lenke LG, Betz RR, Harms J, et al. Adolescent
idiopathic scoliosis: a new classification system to
determine extent of spinal arthrodesis. J Bone Joint
Surg Am 2001;83:1169–81.
[6] Lenke LG, Betz RR, Clements D, et al. Curve prev-
alence of a new classification of operative adolescent
idiopathic scoliosis: does classification correlate with
treatment? Spine 2002;27:604–11.
[7] Lenke LG, Betz RR, Bridwell KH, et al. Intraob-
server and interobserver reliability of the classifica-
tion of thoracic adolescent idiopathic scoliosis.
J Bone Joint Surg Am 1998;80:1097–106.
[8] Ogon M, Giesinger K, Behensky H, et al. Interob-
server and intraobserver reliability of Lenke’s new
scoliosis classification system. Spine 2002;27:858–62.
[9] DobbsMB, Lenke LG,Walton T, et al. Can we pre-
dict the ultimate lumbar curve in adolescent idio-
pathic scoliosis patients undergoing a selective
fusion with undercorrection of the thoracic curve?
Spine 2004;29:277–85.
[10] Cil A, Pekmezci M, Yazici M, et al. The validity of
Lenke criteria for defining structural proximal tho-
racic curves in patients with adolescent idiopathic
scoliosis. Spine 2005;30:2550–5.
[11] Lee SM, Suk SI, Chung ER. Direct vertebral rota-
tion: a new techniqueof three-dimensional deformity
correction with segmental pedicle screw fixation in
adolescent idiopathic scoliosis. Spine 2004;29:343–9.
[12] Suk SI, Lee SM, Chung ER, et al. Determination of
distal fusion level with segmental pedicle screw fixa-
tion in single thoracic idiopathic scoliosis. Spine
2003;28:484–91.
[13] Rhee JM, Bridwell KH, Won DS, et al. Sagittal
plane analysis of adolescent idiopathic scoliosis:
the effect of anterior versus posterior instrumenta-
tion. Spine 2002;27:2350–6.
[14] Betz RR, Harms J, Clements DH, et al. Comparison
of anterior and posterior instrumentation for correc-
tion of adolescent thoracic idiopathic scoliosis.
Spine 1999;24:225–39.
[15] Kuklo TR, O’Brien MF, Lenke LG, et al. Compar-
ison of the lowest instrumented, stable, and lower
end vertebrae in ‘‘single overhang’’ thoracic
adolescent idiopathic scoliosis: anterior versus pos-
terior spinal fusion. Spine 2006;31:2232–6.
[16] Kuklo TR, Lenke LG, Won DS, et al. Spontaneous
proximal thoracic curve correction after isolated
fusion of the main thoracic curve in adolescent idio-
pathic scoliosis. Spine 2001;26:1966–75.
[17] Potter BK, Kuklo TR, Lenke LG. Radiographic
outcomes of anterior spinal fusion versus posterior
spinal fusion with thoracic pedicle screws for treat-
ment of Lenke Type I adolescent idiopathic scoliosis
curves. Spine 2005;30:1859–66.
[18] Lenke LG, Betz RR, Bridwell KH, et al. Spontane-
ous lumbar curve coronal correction after selective
anterior or posterior thoracic fusion in adolescent id-
iopathic scoliosis. Spine 1999;24:1663–71.
[19] Lenke LG, Bridwell KH, Baldus C, et al. Preventing
decompensation in King type II curves treated with
Cotrel-Dubousset instrumentation. Strict guidelines
for selective thoracic fusion. Spine 1992;17:S274–81.
[20] Edwards CC II, Lenke LG, Peelle M, et al. Selective
thoracic fusion for adolescent idiopathic scoliosis
with C modifier lumbar curves: 2- to 16-year radio-
graphic and clinical results. Spine 2004;29:536–46.
[21] Lenke LG, Edwards CC II, Bridwell KH. The Lenke
classificationof adolescent idiopathic scoliosis: how it
organizes curve patterns as a template to perform se-
lective fusions of the spine. Spine 2003;28:S199–207.
[22] Luhmann SJ, Lenke LG, Kim YJ, et al. Thoracic
adolescent idiopathic curves between 70� and 100�.Is anterior release necessary? Spine 2005;30:2061–7.
[23] Suk SI, Kim WJ, Lee CS, et al. Indications of prox-
imal thoracic curve fusion in thoracic adolescent
idiopathic scoliosis: Recognition and treatment of
double thoracic curve pattern in adolescent idio-
pathic scoliosis treated with segmental instrumenta-
tion. Spine 2000;25:2342–9.
[24] Kuklo TR, Lenke LG, Graham EJ, et al. Correla-
tion of radiographic, clinical, and patient assessment
of shoulder balance following fusion versus nonfu-
sion of the proximal thoracic curve in adolescent
idiopathic scoliosis. Spine 2002;27:2013–20.
[25] Sanders AE, Baumann R, Brown H, et al. Selective
anterior fusion of thoracolumbar/lumbar curves in
adolescents: when can the associated thoracic curve
be left unfused? Spine 2003;28:706–13.
[26] Lenke LG, Betz RR, Haher TR, et al. Multisurgeon
assessment of surgical decision-making in adolescent
idiopathic scoliosis: curve classification, operative
approach, and fusion levels. Spine 2001;26:2347–53.
[27] PunoRM,AnKC,PunoRL, et al. Treatment recom-
mendations for idiopathic scoliosis: an assessment of
the Lenke classification. Spine 2003;28:2102–14.
[28] Newton PO, Faro FD, Lenke LG, et al. Factors
involved in the decision to perform a selective
versus nonselective fusion of Lenke 1B and 1C
(King-Moe II) curves in adolescent idiopathic
scoliosis. Spine 2003;28:S217–23.

Orthop Clin N Am 38 (2007) 531–540
Anterior and Thoracoscopic Scoliosis Surgeryfor Idiopathic Scoliosis
Vidyadhar V. Upasani, MDa, Peter O. Newton, MDb,*aDepartment of Orthopedic Surgery, University of California San Diego, 3020 Children’s Way,
MC5054, San Diego, CA 92123, USAbDepartment of Orthopedic Surgery, Rady Children’s Hospital San Diego, 3030 Children’s Way,
Suite 410, San Diego, CA 92123, USA
Orthopedic management of idiopathic scoliosisis based on knowledge of the natural history ofthis spinal disorder, identifying those patients
with a high likelihood of developing worseningdeformity. Long-term studies of untreated scolio-sis have associated severe deformity with poor
prognosis, increased morbidity and mortalityassociated with worsening cardiopulmonary com-promise, increased back pain, and psychosocial
issues related to the deformity [1,2]. Surgical treat-ment, with instrumentation and spinal arthrode-sis, was shown to achieve long-lasting deformityreduction at the cost of spinal flexibility [3,4]. Al-
though posterior spinal instrumentation and fu-sion continues to be the most commonly usedapproach in the surgical treatment of idiopathic
scoliosis, anterior procedures, both open andthoracoscopic, have proven to be a viable optionin selected patients.
Anterior scoliosis surgery
Open anterior surgical techniques for spinal
deformity correction were described first in thelate 1960s. Dwyer and colleagues [5] developeda vertebral screw and flexible cable system to
achieve coronal deformity correction by applyinga compressive force along the convexity of thespine. The Zielke system, developed in the 1970s,
replaced the Dwyer cable and used an anterior-threaded rod to treat short- and long-segment
* Corresponding author.
E-mail address: [email protected] (P.O. Newton).
0030-5898/07/$ - see front matter � 2007 Elsevier Inc. All r
doi:10.1016/j.ocl.2007.05.003
deformities [6]. Since that time, open anteriorsurgical techniques and instrumentation have ad-vanced considerably. Current implant systems
use rigid, single- or dual-rod constructs to achievespinal realignment and stabilization.
During the early 1990s, anterior video-assisted
thoracoscopy was described by Regan and Mackand colleagues [7,8]. This technique provides analternate approach, through a limited chest wall
dissection, to achieve multilevel thoracic spinalrelease and instrumentation. Once mastered, thistechnically challenging approach theoreticallyaffords several advantages over the traditional
thoracotomy, including reduced pulmonary mor-bidity and postoperative pain, better visualization,and improved cosmesis.
The ultimate goals of all anterior spinal de-formity correction procedures remain the same.The primary concern is to visualize the spine and
obtain exposure that will allow spinal release andinstrumentation without damaging the surround-ing neurovascular structures. Secondarily, a thor-ough disc and ligamentous excision must be
performed to mobilize the spine maximally.Lastly, a solid interbody arthrodesis must beachieved after instrumentation and correction of
the spinal deformity. In general, surgical fusionsshould be as short as possible to minimize the lossof spinal flexibility, yet be long enough to ensure
optimal correction and lasting spinal balance.
Indications
Surgical indications for patients who haveadolescent idiopathic scoliosis are dependent on
ights reserved.
orthopedic.theclinics.com

532 UPASANI & NEWTON
various factors. The risk for deformity progres-sion based on gender, bone age, and curvemagnitude plays a critical role when deciding
which patients need operative treatment [9–11].Studies of the natural history of this disease indi-cate that surgical treatment should be consideredin immature patients once the Cobb angle of their
major curve exceeds 40� to 45�, whereas more ma-ture patientsdwith a lower risk for curve progres-siondmay be observed until their major curve
exceeds 50� [1,2,12]. Curve pattern, trunk defor-mity (axial plane rotation), and balance alsoshould be considered when recommending surgi-
cal correction, because a single curve may creategreater trunk shift than a balanced double or tri-ple curve.
Combined anterior and posterior scoliosis pro-
cedures are primarily indicated in the treatmentof large (O75�) or rigid (bend correction !50�)spinal deformities. The anterior approaches (open
or thoracoscopic) enable maximal spinal mobili-zation before instrumentation, by allowing accessto the main anterior stabilizing structures of the
spine, including the annulus, the intervertebraldisc, and the anterior longitudinal ligament. Thedegree to which spinal flexibility can be increased
is dependent on the complete release of thesestabilizing structures. In the most severe cases,resection of the rib head and costovertebral jointmay be required to optimize spinal mobility.
Another indication for these combined ap-proaches is in the treatment of immature (Risser0 with an open triradiate cartilage) patients.
Unbalanced ablation of the posterior growthpotential, with continued anterior growth, isbelieved to cause a slowly progressive rotational
(‘‘crankshaft’’) deformity [13,14]. To prevent thisproblem, patients are treated often with an ante-rior release and fusion and a posterior instrumen-tation and fusion.
Combined procedures also are indicated inpatients who are at increased risk for pseudoarth-rosis formation, such as those with bone-healing
deficiency syndromes (eg, neurofibromatosis,Marfan syndrome) or a history of irradiation.An anterior discectomy provides a large surface
area of cancellous bone and allows for a circum-ferential fusion to increase the likelihood offorming a solid arthrodesis.
Anterior instrumentation has been associatedwith the potential to save one to three distal fusionlevels in the treatment of isolated major thoracic,thoracolumbar, or lumbar curves [15]. This proce-
dure also has been found to be kyphogenic and
ideally suited in the treatment of patients whohave a hypokyphotic or lordotic thoracic spine[16]; however, in the treatment of thoracolumbar/
lumbar curves, structural grafts are required tomaintain normal thoracolumbar sagittal align-ment. Double-rod, double-screw constructs alsomay allow additional control of the sagittal plane
in patients who have thoracolumbar curves [17].Anterior thoracoscopic techniques are more
amenable to the treatment of curves with certain
characteristics. For example, smaller curves (usu-ally !70�) with greater than 50% flexibility canbe treated appropriately with a single rod–screw
construct. Single structural thoracic curves andthose double or triple curves in which only thethoracic component is structural also are treatedmore readily with a single-rod anterior thoraco-
scopic procedure.
Contraindications
Impaired preoperative pulmonary function andthe presence of comorbidities associated with in-trathoracic or intra-abdominal visceral abnormal-
ities are two of the absolute contraindications toanterior scoliosis procedures. The pulmonary sta-tus of the patient must allow single-lung ventila-
tion; transthoracic and thoracoscopic approachesrequire selective deflation of one lung to allowadequate space within the chest cavity to exposeand instrument the spine. Vertebral body osteope-
nia, although rare in the adolescent idiopathicscoliosis population, is seen commonly in patientswho have neuromuscular disorders and may limit
anterior instrumentation options. Vertebral bodysize is another consideration; it may limit adequatefixation in small or underweight patients.
Obesity (O60–70 kg) may be another relativecontraindication to anterior thoracic instrumen-tation, because patients with an increased body
mass may be more prone to overstressing a single-rod anterior construct, resulting in implant failureor loss of deformity correction. Dual-rod anteriorconstructs may be more appropriate in obese
patients; they were shown to be more stiff bio-mechanically [18] and clinically equivalent [17] tosingle-rod instrumentation in achieving deformity
correction.Specific to anterior thoracoscopic surgery, the
existence of intrathoracic pleural adhesions from
prior thoracotomy procedures or pulmonaryinfections should be considered a relative contra-indication. Although minor adhesions can be

533ANTERIOR SURGERY FOR IDIOPATHIC SCOLIOSIS
divided, a near complete pleural symphysis be-tween the chest and lung can make adequate lungcollapse nearly impossible. In addition, althoughchildren weighing less than 30 kg have been
treated safely with the anterior thoracoscopicapproach, the relative benefit of this minimallyinvasive technique seems to be reduced in small
patients [19]. If visualization is inadequate at anypoint during the endoscopic procedure, conver-sion to an open approach must be considered. A
rigid spinal deformity or one that is too closely ap-proximated to the rib cage also is difficult to treatwith a thoracoscopic anterior procedure. Preoper-
ative radiographs should be reviewed to ensurea minimum working distance of 2 to 3 cm forthoracoscopic procedures.
Open anterior release and instrumentation
The thoracic spine is accessed most commonlythrough a single or double anterolateral thoracot-omy in patients who have idiopathic scoliosis.
Usually, a single thoracotomy is adequate toaccess seven or fewer levels between T4 throughT12, whereas a double thoracotomy may be
required to achieve exposure when more thanseven levels are going to be fused. In idiopathicscoliosis, the spine usually is approached from the
convexity of the curve (a right-sided thoracot-omy). Typically, the thoracolumbar/lumbar spine(T10–L5) is approached through a thoracoabdo-minal incision. This incision should cross the
costochondral junction before turning obliquelyacross the abdominal wall toward the lateralborder of the rectus abdominis sheath. A low
thoracotomy, with a tenth-rib resection, canfacilitate access to the thoracic cavity, the thor-acolumbar spine, and the retroperitoneal space.
After exposure of the spine has been achieved,the discs to be resected, and, if indicated, thevertebrae to be instrumented are verified usingintraoperative fluoroscopy or portable radio-
graph. A thorough discectomy is performed ateach subsequent level, with excision of the annu-lus and the anterior longitudinal ligament. In-
complete disc resection has been associated withsuboptimal mobilization of the spine and anincreased incidence of implant failure and pseu-
doarthrosis formation. At times, visualization ofthe posterior disc may require resection of the ribhead down to the base of the transverse process.
The cartilaginous superior and inferior endplatesalso must be separated completely from theadjoining vertebral bodies, and the bony end-plates should be decorticated with sharp curettes.
Fixed-head vertebral body screws, rangingfrom 5 to 7 mm in diameter, are used commonlyin patients who have idiopathic scoliosis. Prior to
screw placement, the superior and inferior end-plates, the anterior cortex, and the anterior aspectof the spinal canal should be understood clearly
for each vertebral body. Biomechanically,pronged staples and bicortical screw fixationsignificantly increased construct stiffness during
single-screw anterior vertebral body instrumenta-tion [20]. In addition, juxta-endplate screws pro-vided better fixation than did screws placed inthe traditional midvertebral location [21]. This
screw position seems to increase fixation strengthby butting the screw threads up against the supe-rior (or inferior) endplate of the vertebral body.
For dual-rod constructs, a two-hole vertebralbody staple should be placed carefully to allowappropriate positioning and trajectory of both
screws (Fig. 1A). All screw tips should be palpatedon the concavity of the deformity to ensure that
Fig. 1. (A) A two-hole vertebral body staple is used to allow appropriate positioning and trajectory of dual-screw im-
plants. (B) Dual-rod construct after deformity correction and rod implantation has been achieved.

534 UPASANI & NEWTON
they are not excessively long and are not causinginjury to adjacent neurovascular or visceral struc-tures. After all screws have been placed, the single
or dual rods (Fig. 1B) are prebent to the desiredcoronal and sagittal contour of the spine, looselyanchored within the screw heads, and then rotatedinto position to correct scoliosis and to restore the
normal sagittal contour of the spine. Beginningdistally, the disc spaces are wedged open, andthe interspaces are packed with bone graft.
Many bone-grafting materials are available: struc-tural and nonstructural grafts, autologous grafts,fresh-frozen and freeze-dried allografts, deminer-
alized bone matrices, and various synthetic bonesubstitutes. Regardless of the material used, it isimportant to ensure that both bony endplatesare well decorticated and able to provide good
vascularity to the graft material. Because the ante-rior approach tends to be kyphogenic, a structuralgraft may be necessary in the thoracolumbar and
lumbar spine to preserve the natural lordosis.Derotation, translation, and compression ma-
neuvers may be used during rod insertion to
achieve deformity correction. Scoliosis correctioncan be achieved directly by cantilevering the rodinto the vertebral screws or by rolling the precon-
toured rod from scoliosis into the sagittal plane.After tightening the proximal screws, furthercoronal correction can be obtained by sequen-tially compressing between screws along the
convexity of the curve. After the instrumentationis complete, the patient’s neurologic functionshould be assessed with a wake-up test or spinal
cord monitoring. Intraoperative radiographs alsoshould be obtained to confirm screw placementand evaluate the initial deformity correction.
Case example 1
A 14-year-old girl who has a progressive sco-liotic deformity presented after failed treatment
with a brace. Preoperative posteroanterior (PA)(Fig. 2A) and lateral (Fig. 2B) radiographs re-vealed that she was Risser 3 and had a 43� thora-columbar curve with a 32� compensatory rightthoracic curve. One-year after a left open anteriorspinal fusion from T11 to L3 with dual-rod instru-mentation, PA (Fig. 2C) and lateral (Fig. 2D) ra-
diographs revealed a 15� thoracolumbar curveand an 11� thoracic curve.
Thoracoscopic anterior release
and instrumentation
Similar to open anterior procedures, the leftlateral decubitus position allows optimal access to
the right thoracic spine and enables greatercircumferential access to the vertebral bodiesand discs during the thoracoscopic approach.
Maintaining spatial orientation is more difficult
Fig. 2. A 14-year-old girl who had a progressive scoliotic deformity presented after failed treatment with a brace. Pre-
operative PA (A) and lateral (B) radiographs revealed that she was Risser 3 and had a 43� thoracolumbar curve with
a 32� compensatory right thoracic curve. One year after a left open anterior spinal fusion from T11 to L3 with dual-
rod instrumentation, PA (C) and lateral (D) radiographs revealed a 15� thoracolumbar curve and an 11� thoracic curve.

535ANTERIOR SURGERY FOR IDIOPATHIC SCOLIOSIS
during endoscopic spinal surgery. Positioning thesurgeon and the assistant anterior to the patientwith the video monitor properly aligned and
oriented behind the patient allows access to thespine from the most natural viewing perspective.
Single-lung ventilation with a double-lumenendotracheal tube is performed to deflate the right
lung selectively before port placement. The loca-tion of the ports is determined using anatomiclandmarks and fluoroscopic guidance to optimize
access to all motion segments planned to beinstrumented. The number of ports required de-pends on the type of deformity being treated and
the number of levels being instrumented. Gener-ally, three portals along the posterior axillary lineare used for instrumentation, and two portals
along the anterior axillary line are used forexposure and release of the anterior spine. Ante-rior axillary ports allow greater exposure of the
Fig. 3. A harmonic scalpel is used to create a longitudi-
nal opening of the pleura.
Fig. 4. The initial pleural opening is performed superfi-
cial to the segmental vessels. A segmental artery and vein
is seen crossing the midportion of the vertebral body.
concave aspects of the deformity during disc exci-
sion and retraction of the great vessels.Angled optics should be used to ensure that the
tip of the working instrument is visualized at all
times. A fan retractor is placed through one of theposterior axillary ports to retract and protect thedeflated lung. After confirming anatomic levelsusing intraoperative fluoroscopy, a harmonic scal-
pel is used to create a longitudinal opening of thepleura (Fig. 3). The initial pleural opening isperformed superficial to the segmental vessels
(Fig. 4). Limited exposure of the discs is accom-plished by retracting the pleura between the vessels.To broaden the exposure anteriorly, the segmental
vessels are coagulated and divided with the har-monic scalpel (Fig. 5). To achieve optimal hemosta-sis, the energy from the harmonic scalpel is applied
slowly over a 3- to 5-mm length of the vessel.
Fig. 5. The segmental vessels are coagulated and divided
with the harmonic scalpel to minimize bleeding while
broadening the exposure.
Fig. 6. A packing sponge is inserted between the ante-
rior spine and pleura to create a space and protect adja-
cent neurovascular structures.

536 UPASANI & NEWTON
After dividing the pleura, the loose areolartissue is divided, and a space is created betweenthe anterior spine and pleura using packing
sponges (Fig. 6). Directly lateral to the anteriorspine, the azygos vein and other great vesselscan be identified and must be avoided during thediscectomy procedure (Fig. 7). Circumferential ex-
posure of the spine and discs should be completedbefore excising the discs. Distal exposure to theT12–L1 disc space may require division of the di-
aphragm insertion. To accomplish this, the longi-tudinal pleural incision is extended onto theinferiorly retracted diaphragm, and blunt dissec-
tion is used to strip the diaphragm off the anterioraspect of the spine.
Disc excision is initiated by performing a cir-cumferential annulotomy using the ultrasonic
blade. An up-biting rongeur is used first to removethe most anterior and concave aspect of theannulus. A complete discectomy requires optimal
visualization deep into the disc space, ensuringthat the integrity of the posterior longitudinalligament is maintained and that the neural ele-
ments are protected. The superior and inferiorcartilage endplates are dissected sharply, and anangled curette or rongeur is used to decorticate
the bone. An endplate shaver inserted into eachintervertebral space may be used to ensure thatcomplete disc excision has been performed andthat the spine is mobile (Fig. 8). Hemostasis is
maintained by placing an oxidized cellulose agentin each intervertebral space.
To prepare for screw/rod implantation, a
15-mm port is placed between the ribs throughthe skin incisions along the posterior axillary line(Fig. 9). Each screw should be started in the mid-
aspect of the vertebral body just anterior to the rib
head articulation (Fig. 10). An awl is used first todetermine the screw path. Then, the vertebral
body is tapped, and a ball-tipped calibrated probeis used to determine screw length. The screwsshould achieve bicortical purchase; however, ex-
cessive screw penetration should be avoided toprotect adjacent neurovascular structures (aorta).After insertion of all of the screws, the fixed-angle
screw heads are aligned for rod insertion, and theintervertebral spaces are packed with bone graftusing a tubular plunger device.
Deformity correction is accomplished by can-
tilevering a precontoured rod into position(Fig. 11), and segmental compression is per-formed using an endoscopic compressing device
(Fig. 12). Following rod insertion, the pleura is re-approximated and closed over the instrumenta-tion using the EndoStitch device. Beginning
distally, the suture needle is passed through bothsides of the cut pleura or diaphragm, and an
Fig. 7. The contralateral segmental vessels and azygos
vein can be identified directly under the anterior spine.
Fig. 8. (A) An endplate shaver is inserted into each intervertebral space to ensure that a complete discectomy has been
performed and that the spine is optimally mobilized. (B) The posterior longitudinal ligament can be visualized by open-
ing the disc space to ensure that the spinal cord is protected.

537ANTERIOR SURGERY FOR IDIOPATHIC SCOLIOSIS
externally tied knot is slid down securely intoplace. The suturing device allows a double-endedneedle to be passed from one jaw to the other,
and a simple running closure of the pleura is per-formed (Fig. 13).
Case example 2
A 12-year-old girl who had adolescent idio-
pathic scoliosis and a progressive deformity pre-sented with preoperative PA (Fig. 14A) andlateral (Fig. 14B) radiographs that revealed she
was Risser 0, had a 43� thoracic curve, and hada 28� thoracolumbar curve. One year after an an-terior thoracoscopic release, T6 to T12 single-rodinstrumentation, and fusion with iliac crest bone
graft, PA (Fig. 14C) and lateral (Fig. 14D) radio-graphs revealed a 19� thoracic curve and a 10�
thoracolumbar curve.
Fig. 9. A 15-mm port is placed between the ribs through
skin incisions along the posterior axillary line to prepare
for instrumentation.
Fig. 10. A tap is used to ensure that the vertebral body
screw insertion is juxta-endplate to provide for superior
fixation.
Complications
The incidence of major complications, includ-ing death, paraplegia, or deep wound infections
after open or thoracoscopic procedures to in-strument the anterior thoracic/thoracolumbarspine, are less than 1% [22]. As would be ex-
pected, pulmonary complications account formore than 50% of the morbidity associated withthese procedures [23,24]. Most of time, these pul-
monary issues are related to postoperative pleuraleffusions, pneumothorax, atelectasis, or excessivechest tube drainage. Preoperative pulmonary
function studies can be obtained to prevent orplan for postoperative respiratory issues. An eval-uation of pulmonary function after open versusthoracoscopic anterior procedures revealed that
pulmonary function recovered more quickly afterthe less invasive procedure; this difference wasmaintained at the 2-year follow-up [25]. Other
Fig. 11. The precontoured rod is cantilevered into posi-
tion to obtain deformity correction.
Fig. 12. Segmental compression is performed to obtain
coronal plane deformity correction.

538 UPASANI &
infrequently reported complications after anteriorscoliosis surgery include injury to the great vessels,
ureter, or spinal cord and development of a retro-peritoneal hematoma or fibrosis.
Outcomes
When evaluating anterior thoracoscopic re-
lease procedures, several animal studies reportedthe ability to achieve similar amounts of spinalmobilization compared with open techniques
Fig. 13. The EndoStitch device is used to suture the
pleura over the instrumentation.
[26–28]. A radiographic analysis also demon-strated a similar ability to achieve coronal andsagittal plane correction when comparing the
two techniques [29]; however, the thoracoscopicprocedure is technically challenging, and the steeplearning curve described by Newton and col-leagues [30] must be overcome to perform this
procedure safely and efficaciously. A series of112 consecutive cases of thoracoscopic anteriorrelease and fusion with more than 2-years of fol-
low-up revealed that clinical failures were exceed-ingly rare and that the primary goals of increasingspinal flexibility and achieving a solid arthrodesis
occurred in most cases [31].Several studies evaluated surgical outcomes in
patients who had idiopathic scoliosis by compar-ing anterior and posterior instrumentation
methods. In 1999, Lenke and colleagues [32] re-ported a greater main thoracic curve and sponta-neous thoracolumbar/lumbar curve correction
following selective anterior fusion comparedwith posterior instrumentation. Multiple investi-gators confirmed these findings and demonstrated
the ability of anterior instrumentation to achievesuperior radiographic results with the fusion offewer vertebral levels [33–35]; however, these early
studies compared anterior instrumentation tech-niques with posterior hook or hybrid constructs.
NEWTON
Fig. 14. A 12-year-old girl who had adolescent idiopathic scoliosis and a progressive deformity presented with preop-
erative PA (A) and lateral (B) radiographs that revealed she was Risser 0, had a 43� thoracic curve, and a 28� thoraco-lumbar curve. One year after an anterior thoracoscopic release, T6 to T12 single-rod instrumentation, and fusion with
iliac crest bone graft, PA (C) and lateral (D) radiographs revealed a 19� thoracic curve and a 10� thoracolumbar curve.

539ANTERIOR SURGERY FOR IDIOPATHIC SCOLIOSIS
In 2005, Potter and colleagues [36] evaluatedposterior instrumentation with thoracic pediclescrews; in some cases, posterior surgery providedbetter coronal and axial correction compared
with thoracic anterior instrumentation. Anteriorscoliosis procedures with single-rod constructsalso have been associated with an increased rate
of pseudoarthrosis and an increased rate of im-plant failure compared with posterior instrumen-tation [37]. Dual-rod constructs were developed
to provide more rigid fixation and were found toincrease mechanical stiffness [17,18]; however, ver-tebral body size restrictions make it difficult to
place these implants in the adolescent thoracicspine.
Two-year follow-up has been reported forthoracoscopic anterior instrumentation. In a series
of 50 consecutive patients [38], curve correctionaveraged 60%, with an average operating timeof 5.8 hours. This initial series of patients sug-
gested that thoracoscopic instrumentation wasa viable option in the treatment of adolescent idi-opathic scoliosis; however, success remained de-
pendent on patient selection and the surgeon’stechnical ability. Eighteen of the first 20 consecu-tive patients of this series now have more than
5-year follow-up; deformity correction and abso-lute pulmonary function have been maintained,and successful bony fusion has occurred at 92%of the motion segments (unpublished data).
Summary
The anterior surgical treatments for idiopathic
scoliosis continue to evolve and provide advan-tages over posterior procedures in specific in-stances. Open and thoracoscopic anterior
approaches allow direct access to the anteriorstabilizing structures of the spine, enable mobili-zation of a rigid deformity, and provide a large
surface area for arthrodesis; however, these pro-cedures are associated with increased rates ofpulmonary compromise, and long-term studieshave not been completed to determine their ability
to maintain deformity correction relative to mod-ern posterior segmental pedicle screw constructs.
Thoracoscopic procedures are technically de-
manding and surgeon experience must be consid-ered before recommending this procedure tocarefully selected patients; however, they do pro-
vide a more cosmetically appealing alternative toa large midline posterior or anterolateral thora-cotomy scar. Although the indications and
contraindications for anterior versus posteriorsurgical intervention (for thoracic and thoraco-lumbar curve patterns) have been defined to somedegree, there remains appropriate flexibility in the
decision-making process, allowing the surgeon tomake an optimal recommendation for each pa-tient based on surgeon experience and patient
needs.
References
[1] Nachemson A. A long term follow-up study of non-
treated scoliosis. Acta Orthop Scand 1968;39(4):
466–76.
[2] Nilsonne U, Lundgren KD. Long-term prognosis in
idiopathic scoliosis. Acta Orthop Scand 1968;39(4):
456–65.
[3] Andersen MO, Christensen SB, Thomsen K. Out-
come at 10 years after treatment for adolescent idio-
pathic scoliosis. Spine 2006;31(3):350–4.
[4] Benli IT, Ates B, Akalin S, et al. Minimum 10 years
follow-up surgical results of adolescent idiopathic
scoliosis patients treated with TSRH instrumenta-
tion. Eur Spine J 2007;16(3):381–91.
[5] Dwyer AF, NewtonNC, SherwoodAA.An anterior
approach to scoliosis. A preliminary report. Clin
Orthop Relat Res 1969;62:192–202.
[6] Moe JH, Purcell GA, Bradford DS. Zielke instru-
mentation (VDS) for the correction of spinal curva-
ture. Analysis of results in 66 patients. Clin Orthop
Relat Res 1983;(180):133–53.
[7] Mack MJ, Regan JJ, Bobechko WP, et al. Applica-
tion of thoracoscopy for diseases of the spine. Ann
Thorac Surg 1993;56(3):736–8.
[8] Regan JJ, Mack MJ, Picetti GD 3rd. A technical
report on video-assisted thoracoscopy in thoracic
spinal surgery. Preliminary description. Spine 1995;
20(7):831–7.
[9] Biondi J,Weiner DS, BethemD, et al. Correlation of
Risser sign and bone age determination in adolescent
idiopathic scoliosis. J Pediatr Orthop 1985;5(6):
697–701.
[10] Peterson LE,NachemsonAL. Prediction of progres-
sion of the curve in girls who have adolescent idio-
pathic scoliosis of moderate severity. Logistic
regression analysis based on data from The Brace
Study of the Scoliosis Research Society. J Bone Joint
Surg Am 1995;77(6):823–7.
[11] Lonstein JE, Carlson JM. The prediction of curve
progression in untreated idiopathic scoliosis during
growth. J Bone Joint Surg Am 1984;66(7):1061–71.
[12] Weinstein SL, Ponseti IV. Curve progression in
idiopathic scoliosis. J Bone Joint Surg Am 1983;
65(4):447–55.
[13] Dubousset J, Herring JA, Shufflebarger H. The
crankshaft phenomenon. J Pediatr Orthop 1989;
9(5):541–50.

540 UPASANI & NEWTON
[14] Sanders JO, Little DG, Richards BS. Prediction of
the crankshaft phenomenon by peak height velocity.
Spine 1997;22(12):1352–6 [discussion: 1356–7].
[15] Lowe TG, Betz R, LenkeL, et al. Anterior single-rod
instrumentation of the thoracic and lumbar spine:
saving levels. Spine 2003;28(20):S208–16.
[16] Lowe TG, Alongi PR, Smith DA, et al. Anterior sin-
gle rod instrumentation for thoracolumbar adoles-
cent idiopathic scoliosis with and without the use
of structural interbody support. Spine 2003;28(19):
2232–41 [discussion: 2241–2].
[17] HurfordRK Jr, Lenke LG, Lee SS, et al. Prospective
radiographic and clinical outcomes of dual-rod
instrumented anterior spinal fusion in adolescent
idiopathic scoliosis: comparisonwith single-rod con-
structs. Spine 2006;31(20):2322–8.
[18] Lowe TG, Enguidanos ST, Smith DA, et al. Single-
rod versus dual-rod anterior instrumentation for
idiopathic scoliosis: a biomechanical study. Spine
2005;30(3):311–7.
[19] Early SD, Newton PO, White KK, et al. The feasi-
bility of anterior thoracoscopic spine surgery in
children under 30 kilograms. Spine 2002;27(21):
2368–73.
[20] Lowe T, O’BrienM, Smith D, et al. Central and jux-
ta-endplate vertebral body screw placement: a bio-
mechanical analysis in a human cadaveric model.
Spine 2002;27(4):369–73.
[21] Horton WC, Blackstock SF, Norman JT, et al.
Strength of fixation of anterior vertebral body
screws. Spine 1996;21(4):439–44.
[22] Faciszewski T, Winter RB, Lonstein JE, et al. The
surgical and medical perioperative complications
of anterior spinal fusion surgery in the thoracic
and lumbar spine in adults. A review of 1223 proce-
dures. Spine 1995;20(14):1592–9.
[23] Anderson PR, PunoMR, Lovell SL, et al. Postoper-
ative respiratory complications in non-idiopathic
scoliosis. Acta Anaesthesiol Scand 1985;29(2):
186–92.
[24] Weis JC, Betz RR, Clements DH 3rd, et al. Preva-
lence of perioperative complications after anterior
spinal fusion for patients with idiopathic scoliosis.
J Spinal Disord 1997;10(5):371–5.
[25] Faro FD, Marks MC, Newton PO, et al. Periopera-
tive changes in pulmonary function after anterior
scoliosis instrumentation: thoracoscopic versus open
approaches. Spine 2005;30(9):1058–63.
[26] Newton PO, Cardelia JM, Farnsworth CL, et al. A
biomechanical comparison of open and thoraco-
scopic anterior spinal release in a goat model. Spine
1998;23(5):530–5 [discussion: 536].
[27] Wall EJ, Bylski-Austrow DI, Shelton FS, et al. En-
doscopic discectomy increases thoracic spine flexibil-
ity as effectively as open discectomy. A mechanical
study in a porcine model. Spine 1998;23(1):9–15 [dis-
cussion: 15–6].
[28] Huntington CF, Murrell WD, Betz RR, et al. Com-
parison of thoracoscopic and open thoracic discec-
tomy in a live ovine model for anterior spinal
fusion. Spine 1998;23(15):1699–702.
[29] Newton PO, Wenger DR, Mubarak SJ, et al. Ante-
rior release and fusion in pediatric spinal deformity.
A comparison of early outcome and cost of thoraco-
scopic and open thoracotomy approaches. Spine
1997;22(12):1398–406.
[30] Newton PO, Shea KG, Granlund KF. Defining the
pediatric spinal thoracoscopy learning curve: sixty-
five consecutive cases. Spine 2000;25(8):1028–35.
[31] Newton PO,White KK, Faro F, et al. The success of
thoracoscopic anterior fusion in a consecutive series
of 112 pediatric spinal deformity cases. Spine 2005;
30(4):392–8.
[32] Lenke LG, Betz RR, Bridwell KH, et al. Spontane-
ous lumbar curve coronal correction after selective
anterior or posterior thoracic fusion in adolescent
idiopathic scoliosis. Spine 1999;24(16):1663–71 [dis-
cussion: 1672].
[33] Kovac V, Puljiz A, Smerdelj M, et al. Scoliosis curve
correction, thoracic volume changes, and thoracic di-
ameters in scoliotic patients after anterior and after
posterior instrumentation. IntOrthop2001;25(2):66–9.
[34] Kuklo TR, Lenke LG, Graham EJ, et al. Correla-
tion of radiographic, clinical, and patient assessment
of shoulder balance following fusion versus nonfu-
sion of the proximal thoracic curve in adolescent
idiopathic scoliosis. Spine 2002;27(18):2013–20.
[35] Kuklo TR, Lenke LG, Won DS, et al. Spontaneous
proximal thoracic curve correction after isolated
fusion of the main thoracic curve in adolescent idio-
pathic scoliosis. Spine 2001;26(18):1966–75.
[36] Potter BK, Kuklo TR, Lenke LG. Radiographic
outcomes of anterior spinal fusion versus posterior
spinal fusion with thoracic pedicle screws for treat-
ment of Lenke Type I adolescent idiopathic scoliosis
curves. Spine 2005;30(16):1859–66.
[37] Betz RR,Harms J, Clements DH 3rd, et al. Compar-
ison of anterior and posterior instrumentation for
correction of adolescent thoracic idiopathic scolio-
sis. Spine 1999;24(3):225–39.
[38] Newton PO, Parent S, Marks M, et al. Prospective
evaluation of 50 consecutive scoliosis patients surgi-
cally treated with thoracoscopic anterior instrumen-
tation. Spine 2005;30(Suppl 17):S100–9.

Orthop Clin N Am 38 (2007) 541–545
Fusionless Treatment of ScoliosisJames T. Guille, MDa,b,*, Linda P. D’Andrea, MDa,b,
Randal R. Betz, MDb,c
aDivision of Spinal Disorders, Brandywine Institute of Orthopaedics, 600 Creekside Drive,
Suite 611, Pottstown, PA 19464, USAbTemple University School of Medicine, 1500 N. Broad Street, Philadelphia, PA 19140, USA
cShriners Hospital for Children, 3551 North Broad Street,
Philadelphia, PA 19140, USA
Scoliosis is a complex three-dimensional spinal
deformity that results from both known andunknown causes in patients of all ages. Youngchildren who present with large curves have a hightendency to progress as the child grows, but this
progression can vary. More is known about thenatural history of curve progression in adolescentidiopathic scoliosis, which is dependent on the pa-
tient’s skeletal maturity, the curve pattern, and thecurve magnitude. Children with congenital orneuromuscular forms of scoliosis can have an un-
predictable course, with most being progressive.Curves that present in the growing child may beamenable to a variety of treatments to address
curve progression during growth. The standardof care currently for skeletally immature patientswith progressive scoliosis measuring greater thanor equal to 25� is a thoracolumbosacral orthosis.
These braces are used in an attempt to preventcurve progression, but the results can be variable.
Brace wear can be associated with many
problems. As most braces exert their effect viapressure on the rib cage, their influence on thechest wall in the growing child creates concern.
Some children have a problem with the stigmataassociated with wearing a brace, especially chil-dren who have to wear a brace for many years.
* Corresponding author. Division of Spinal Disor-
ders, Brandywine Institute of Orthopaedics, 600 Creek-
side Drive, Suite 611, Pottstown, PA 19464.
E-mail address: [email protected] (J.T.
Guille).
0030-5898/07/$ - see front matter � 2007 Elsevier Inc. All r
doi:10.1016/j.ocl.2007.07.003
Also, while brace treatment is noninvasive and
preserves growth, motion, and function of thespine, it does not correct an established deformity.While most orthopaedists, families, and patientsagree that it is reasonable to wear a scoliosis brace
for 1 or 2 years if it means preventing anoperation, a more difficult situation is encoun-tered in the very young child who faces the
prospect of wearing a brace for many years withno guarantee of a favorable outcome. It is in thesechildren that fusionless treatment options hold the
greatest potential.To date, most fusionless treatment options
have centered on addressing a progressive scolio-
sis in the growing child. The fusionless treatmentof an established larger curve in the patient who isskeletally mature or is nearly so has been limited,but may hold some potential [1,2]. Fusionless
scoliosis surgery may provide substantial advan-tages over both bracing and definitive spinalfusion. The goal of this procedure is to harness
the patient’s inherent spinal growth and redirectit to achieve correction, rather than progression,of the curve. Several methods of treatment of
scoliosis without fusion have evolved and include(1) anterior vertebral body stapling, (2) anteriorspinal tethering, (3) convex scoliosis tethering,(4) mechanical modulation of spinal growth, and
(4) internal bracing. The anterior fusionlesstechniques are theoretically more advantageousthan external bracing because they address the
deformity directly at the spine and not via thechest wall and ribs, and because they eliminateproblems with patient noncompliance.
ights reserved.
orthopedic.theclinics.com

542 GUILLE et al
Furthermore, minimally invasive thoracoscopicaccess to the anterior thoracic spine is less exten-sive than that for posterior instrumented surgery.
For the purposes of this article the termfusionless scoliosis surgery is used to describeanterior spinal procedures that control the pro-gression of scoliosis during growth, but other
fusionless treatments are available. These moreestablished fusionless procedures employ poste-rior implants (growing rods and the vertical
expandable prosthetic titanium rib) that cancontrol the progression of spinal deformity butdo not correct an established deformity in the
younger child. These posterior growing systemsare fraught with complications and take a multi-year commitment of semiannual surgery from thefamily and patient to be successful. Single or dual
growing-rod techniques and the vertical expand-able prosthetic titanium rib are not only moreinvasive than anterior fusionless scoliosis surgery
but are associated with higher rates of complica-tions. Anterior fusionless scoliosis surgery avoidsmultiple procedures, as well as the requirement for
an eventual fusion, by offering a single interven-tion that may provide a more permanent solutionto the spinal deformity. Furthermore, correction
of a spinal deformity in the absence of a rigidfusion mass spanning multiple vertebral motionsegments may ameliorate some of the long-termproblems related to spinal fusion with instrumen-
tation, such as adjacent level degeneration.To date, many models of fusionless surgery
involving both the genesis of iatrogenic scoliosis
and its treatment have been studied [3–10]. Areview of the recent literature shows a markedincrease in interest in the topic and number of
publications on this subject in the past 2 years[11]. However, much of what has been done hasinvolved experimental methods in animal models,with no transition to the clinical realm or a patient
series. The authors first discuss the advent of ante-rior vertebral body stapling and its clinical experi-ence, followed by experimental works on other
fusionless scoliosis treatment options.
Anterior vertebral body stapling
The first recent study of a large patient series is
that of Betz and colleagues [12], who reported onthe Philadelphia Shriners Hospital experiencewith anterior vertebral body stapling in patients
with adolescent idiopathic scoliosis. This is a land-mark study in that previous attempts to correctscoliosis with anterior fusionless techniques had
been disappointing [13,14]. Convex apical verte-bral body (hemiepiphyseal) stapling theoreticallyaffords immediate and possibly reversible cessa-
tion of growth of the anterior vertebral physes[15,16]. Animal studies using a rat tail model con-firm its ability to modulate vertebral growth plateswith skeletal fixation devices [17–19].
In 1951, Nachlas and Borden [13] were initiallyoptimistic about their ability to create and correctlumbar scoliosis in a canine model using a staple
that spanned several vertebral levels. Many ofthe dogs exhibited some correction, and some ofthe animals exhibited arrest of their curve progres-
sion. Some of the staples failed because theyspanned three vertebrae. The enthusiasm for thisnew treatment was lost after the application oftheir stapling technique in three children with pro-
gressive scoliosis yielded poor results. Other inves-tigators have also been dissatisfied with convexstapling as a means of controlling progressive sco-
liosis. In 1954, Smith and colleagues [14] pre-sented disappointing results for human patientswith congenital scoliosis. The scoliosis correction
was limited because the children had little remain-ing growth and the curves were severe, with con-siderable rotational deformity. Some staples
broke or loosened, possibly because of motionthrough the intervertebral discs.
James M. Ogilvie, MD, reported (personalcommunication) that in 1997 he began perform-
ing anterior vertebral body stapling with thoraco-scopic assistance in six patients: three withinfantile scoliosis, two with juvenile scoliosis,
and one with spina bifida. Preoperatively, thepatients’ curves had progressed despite bracingfor the previous year. At 2-year follow-up, four
of the six curves stabilized following the proce-dure. In two patients the staples partially dis-lodged, requiring another operation to replacethe staple.
A likely cause of disappointing results in pre-vious series and experiments was the implant(staple). While the concept of stapling the anterior
vertebral endplates/physes for growth modulationand curve stabilization seems sound, the staplesdesigned for epiphyseal stapling about the knee
are prone to dislodge in the spine because they arenot designed for movement in the spine. Toaddress this concern, Medtronic Sofamor Danek
(Memphis, Tennessee) has designed a specificspine staple called the Nitinol (Nickel TitaniumNaval Ordinance Laboratory) staple, which has510K approval from the US Food and Drug
Administration specifically for use as an anterior

543FUSIONLESS TREATMENT OF SCOLIOSIS
spinal staple. The uniqueness of this staple is thatit is made out of a shape memory alloy in whichthe prongs are straight when cooled but, whenwarmed to body temperature, clamp down in
a ‘‘C’’ shape in the bone for secure fixation.Before its use in humans, the Nitinol staple hadbeen tested in a goat model by Braun and
colleagues [10] and was shown to be safe andhave utility for arresting iatrogenic scoliosis inthe goat.
In 2003, Betz and colleagues [12] reported onthe use of the Nitinol staple in 21 skeletally imma-ture patients with adolescent idiopathic scoliosis.
Indications for the procedure were either bracenoncompliance or the inability of the brace to pre-vent progression of the curve. They found the pro-cedure to be safe and effective, with the results
comparable with that of what would have beenexpected from bracing. In 2005, this groupreported on 39 patients and their increased experi-
ence with the procedure [20]. Eighty-seven percentof those patients older than 8 years at the time ofstapling who had a curve of 50� or less with at
least 1 year of follow-up had stabilization of theircurve. No curve less than 30� at the time of sta-pling progressed more than 10� at follow-up
[20]. Experience from more than 80 patients todate has taught that the entire Cobb angle of allof the curves needs to be stapled (Figs. 1 and 2),and staple implants with tines proportional to
the length of the staple (Fig. 3) have yielded betterresults than previous designs. Relative contraindi-cations include curves above T2 or below L4, very
small vertebral body size, thoracic kyphosisgreater than 40�, and coronal curves above 45�.MRI scans of several of these patients have shown
that the intervertebral discs remain hydrated andare normal in appearance (Fig. 4). The techniqueof anterior vertebral body stapling has been pub-lished [12,20,21].
Tethering procedures
Braun and colleagues [6,7,13] have done much
work with the goat model in the creation of exper-imental scoliosis with a posterior tether of theribs, and correction of this deformity with an
anterior fusionless technique using bone anchorswith ligament tethers. Braun’s group and Newtonand colleagues [22,23] have also shown that if the
bone-anchor–ligament-tether does not fail, itcauses vertebral body wedging and scoliosis cor-rection via growth modulation. Lowe and
colleagues [24] looked at the role of posteriortethers in sagittal plane (kyphotic) deformities in
sheep. While the posterior tether resulted in lesskyphosis, this was accompanied by significantlyless motion from heterotopic ossification. The au-
thors are unaware, however, of any published se-ries on the use of bone-anchors–ligament-tethersin human patients.
Braun and colleagues [22] recently comparedshape memory staples with bone-anchors–liga-ment-tethers in the fusionless treatment of iatro-genic scoliosis in the goat. Results of this study
demonstrate greater efficacy and integrity ofa bone-anchor–flexible-ligament-loop-tether com-pared with a more rigid shape memory alloy
staple in the fusionless treatment of a progressiveexperimental scoliosis. In contrast to the morerigid staple base, the ligament loop used with the
bone anchor provided a more flexible tether span-ning the disc space. This increased flexibility waslikely associated with decreased forces during
spinal motion. This decrease in force potentiallyprotected the bone anchor from loosening.Whereas the staple demonstrated no significant
Fig. 1. Posteroanterior radiograph of a 7-year-old girl
with idiopathic scoliosis having a 25� thoracic and 40�
lumbar curve.

544 GUILLE et al
change in axial pullout strength between the twotime-points, the bone anchor showed a significantincrease in pullout strength. It is postulated thatthis difference was related to two factors: (1) the
rigidity of the portion of the implant spanning
Fig. 3. Intraoperative fluoroscopy image showing ideal
placement of the proportional-sized staples.
Fig. 2. At the age of 12 years, both curves completely
corrected in girl shown in Fig. 1.
the motion segment and (2) the quality of the fix-ation to bone. The staple, though made of shapememory alloy, has a relatively rigid base spanningthe disc space compared with the ligament-loop–bone-anchor construct. Additionally, the smooth
tine is suboptimal for fixation to bone and reliesprimarily on the mechanical ‘‘crimping’’ effect ofthe deployed shape memory alloy staple. The au-
thors do not necessarily believe that the lack ofrigid fixation seen with staples is bad. The associ-ated halo that is seen around the tines on radio-
graphs in long-standing cases shows that there ismotion, and perhaps this is why there is sucha low rate of staple failure and why patients are
able to maintain spinal mobility.
Summary
The recent investigations of convex anteriorvertebral body stapling, both in animal modelsand in juvenile and adolescent scoliosis have
offered promising early results with use of im-proved implants and techniques. The use ofa shape memory alloy staple tailored to the size
of the vertebral body, the application of severalstaples per level, the instrumentation of the Cobblevels of all curves, and the employment of
Fig. 4. MRI of the patient in Fig. 2 showing normal-
appearing well-hydrated discs.

545FUSIONLESS TREATMENT OF SCOLIOSIS
minimally invasive thoracoscopic approaches alloffer substantial improvements over previousfusionless techniques. Patient selection may alsoplay a role in the current success of these fusion-
less treatments, with perhaps the ideal candidatesfor this intervention possessing smaller and moreflexible curves. Still, reports on the clinical success
of these stapling procedures are based on short-term results. Long-term results of the effects onthe instrumented motion segments and adjacent
spine are not yet available.
References
[1] Guille JT, Betz RR, Balsara RK, et al. The feasibil-
ity, safety, and utility of vertebral wedge osteotomies
for the fusionless treatment of paralytic scoliosis.
Spine 2003;28:S266–74.
[2] MaruyamaT,KitagawaT,TakeshitaK,et al.Fusion-
less surgery for scoliosis: 2–17 year radiographic and
clinical follow-up. Spine 2006;31:2310–5.
[3] Braun JT, Hines JL, Akyuz E, et al. Relative versus
absolute modulation of growth in the fusionless
treatment of experimental scoliosis. Spine 2006;31:
1776–82.
[4] Braun JT, Hoffman M, Akyuz E, et al. Mechanical
modulation of vertebral growth in the fusionless
treatment of progressive scoliosis in an experimental
model. Spine 2006;31:1314–20.
[5] Braun JT, Akyuz E, Ogilvie JW. The use of animal
models in fusionless scoliosis investigations. Spine
2005;30:S35–45.
[6] Braun JT, Akyuz E, Udall H, et al. Three-dimen-
sional analysis of 2 fusionless scoliosis treatments:
a flexible ligament tether versus a rigid-shape mem-
ory alloy staple. Spine 2006;31:262–8.
[7] Braun JT, Ogilvie JW, Akyuz E, et al. Creation of an
experimental idiopathic-type scoliosis in an imma-
ture goatmodel using a flexible posterior asymmetric
tether. Spine 2006;31:1410–4.
[8] Puttitz CM, Masaru F, Barkley A, et al. A biome-
chanical assessment of thoracic spine stapling. Spine
2007;32:766–71.
[9] Wall EJ, Bylski-AustrowDI, Kolata RJ, et al. Endo-
scopic mechanical spinal hemiepiphysiodesis mod-
ifies spine growth. Spine 2005;30:1148–53.
[10] Braun JT, Ogilvie JW, Akyuz E, et al. Fusionless
scoliosis correction using a shape memory alloy sta-
ple in the anterior thoracic spine of the immature
goat. Spine 2004;29:1980–9.
[11] Cunningham ME, Frelinghuysen PH, Roh JS, et al.
Fusionless scoliosis surgery. CurrOpin Pediatr 2005;
17:48–53.
[12] Betz RR, Kim J, D’Andrea LP, et al. An innovative
technique of vertebral body stapling for the treat-
ment of patients with adolescent idiopathic scoliosis:
a feasibility, safety, and utility study. Spine 2003;28:
S255–65.
[13] Nachlas IW, Borden JN. The cure of experimental
scoliosis by directed growth control. J Bone Joint
Surg [Am] 1951;33:24–34.
[14] Smith AD, von LackumHL,Wylie R. An operation
for stapling vertebral bodies in congenital scoliosis.
J Bone Joint Surg [Am] 1954;36:342–8.
[15] Roaf R. The treatment of progressive scoliosis by
unilateral growth-arrest. J Bone Joint Surg [Br]
1963;45:637–51.
[16] Roaf R. Vertebral growth and its mechanical con-
trol. J Bone Joint Surg [Br] 1960;42:40–59.
[17] Akyuz E, Braun JT, Brown NAT, et al. Static versus
dynamic loading in the mechanical modulation of
vertebral growth. Spine 2006;31:E952–8.
[18] Mente PL, Aronsson DD, Stokes IA, et al. Mechan-
ical modulation of growth for the correction of ver-
tebral wedge deformities. J Orthop Res 1999;17:
518–24.
[19] Stokes IA, Spence H, Aronsson DD, et al. Mechan-
ical modulation of vertebral body growth. Implica-
tions for scoliosis progression. Spine 1996;21:
1162–7.
[20] Betz RR, D’Andrea LP, Mulcahey MJ, et al. Verte-
bral body stapling procedure for the treatment of
scoliosis in the growing child. Clin Orthop Relat
Res 2005;434:55–60.
[21] D’Andrea LP, Guille JT, Betz RR. Intervertebral
stapling for spinal deformity. In: Vaccaro A,
Albert T, editors. Spine surgery: tricks of the
trade, in press.
[22] Braun JT, Akyuz E, Ogilvie JW, et al. The efficacy
and integrity of shape memory alloy staples and
bone anchors with ligament tethers in the fusionless
treatment of experimental scoliosis. J Bone Joint
Surg [Am] 2005;87:2038–51.
[23] Newton PO, Faro FD, Farnsworth CL, et al. Multi-
level spinal growthmodulation with an anterolateral
flexible tether in an immature bovine model. Spine
2005;30:2608–13.
[24] Lowe TG, Wilson L, Chien J-T, et al. A poste-
rior tether for fusionless modulation of sagittal
plane growth in a sheep model. Spine 2005;30:
S69–74.

Orthop Clin N Am 38 (2007) 547–552
The Use of Growth-Sparing Instrumentation inPediatric Spinal Deformity
John T. Smith, MDDepartment of Orthopaedics and Pediatrics, The University of Utah School of Medicine,
Primary Children’s Medical Center, 100 North Medical Drive, Suite 4550, Salt Lake City, UT 84113, USA
The management of severe spinal deformity in
the growing child remains a challenging problem.Methods to manage or correct spinal deformity inyoung children date back to Hippocrates. Non-
operative methods range from orthotics to castingto traction; however, in certain circumstances,these techniques cannot effectively prevent de-formity progression or are not tolerated by the
child and surgical methods are required.Current options for surgical management of
spinal deformity in the growing child include
definitive spinal fusion with or without instru-mentation, selective fusion (hemiepiphysiodesis),growth modulation (staples or growth tethers),
spinal instrumentation without fusion (growingrods, Luque trolleys), or more recently, the use ofthe vertical expandable prosthetic titanium rib
(VEPTR). Historically, all of these methods havea significant complication rate and despite ad-vances in technology and instrumentation, remainproblematic. This article provides an overview of
current methods and outcomes for spinal instru-mentation in the growing spine.
Normal growth of the spine and thorax
Understanding the normal growth of the spineand thorax is critical to understanding the de-
cision process for surgical management of severespinal deformity in the young child. Dimeglio [1]has contributed significantly to current under-standing of the growing spine. The prenatal devel-
opment of the spinal column is the result of
E-mail address: [email protected]
0030-5898/07/$ - see front matter � 2007 Elsevier Inc. All r
doi:10.1016/j.ocl.2007.03.009
a complex process of segmental development
and differentiation resulting in formation of eachvertebra. With a minimum of three growth zonesper vertebra, there are at least 100 growth plates
within the vertebral column that contribute tothe ultimate morphology of the adult spine. Thiscomplex process of segmental development offersthe potential for developmental errors, producing
an infinite variety of growth alterations anddeformity.
A fourth dimension of spinal growth is the
thorax. Thoracic distortion is a common sequelaof spinal deformity, resulting in alteration ofpulmonary growth and respiratory function. The
primary effect of scoliosis on pulmonary functionis believed to be mechanical, producing impairedmovement of the chest wall, decreased volume of
the thorax, and reduced compliance [2]. In addi-tion, it has been postulated that most alveolargrowth and multiplication occurs until about age8 years and that reduction of thoracic volume
may impair alveolar development and growth[3]. In early-onset scoliosis (before age 5 years),Pehrsson and colleagues [4] reported on a cohort
of patients who have unoperated scoliosis; therewas a significantly increased risk for mortality inpatients who have infantile (P!.001) and juvenile
(P!.01) scoliosis but not in patients who have ad-olescent scoliosis. It is believed that the increasedrisk for death is due to respiratory failure. There-fore, any treatment strategy for severe deformity
must consider the effect a given treatment wouldhave on the growth and shape of the thorax andits consequence on pulmonary function.
The rate of normal spinal growth varies withage. There is a rapid phase of spinal growthfrom birth to age 5 years and a slower phase of
ights reserved.
orthopedic.theclinics.com

548 SMITH
growth between 5 and 10 years, which isfollowed by a period of rapid growth untilcompletion of puberty (14.5 years in girls, 16.5
years in boys). The thoracic spine averages 11 cmin length at birth and reaches about 28 cm inmen and 26 cm in women at skeletal maturity.The lumbar spine averages 7 cm at birth and grows
to an average of 16 cm in men and 15.5 cm inwomen [1].
Early fusion of the growing spine effectively
stops the longitudinal growth of the spine. Dime-glio and Bonnel [5] published tables that predictthe overall effect of early fusion on ultimate sitting
height based on the age of fusion. For example,each thoracic vertebra contributes 2.5% to theoverall sitting height at skeletal maturity. Fromthese data, the surgeon can calculate the resultant
effect of fusion based on the number of vertebralsegments fused and the age of the child. Thisawareness is critical to the decision process of
growth-sparing procedures and the associatedrisks compared with the ultimate loss of heightwith a definitive fusion procedure.
The outcomes of early fusion
Historically, early fusion of progressive curves
has been advocated in young children with pro-gressive curves. The concept was that early fusionwould allow for a smaller number of spinalsegments to be fused preserving adjacent spinal
growth and a balanced spine; however, recentlong-term follow-up studies suggest that earlyfusion had deleterious effects on pulmonary func-
tion. Goldberg and colleagues [6] reported thatchildren whose spinal deformity required earlysurgery (mean age, 4.1 years; 11 patients) had re-
currence of their deformity and impaired respira-tory function at skeletal maturity. Emans andcolleagues [7] reported on a series of 13 patients
who underwent fusion of at least four thoracicvertebras before 5 years of age; they demonstratedsignificant impairment of pulmonary function.The extent of pulmonary impairment correlated
closely with the number of thoracic vertebraefused. Further operative intervention was requiredin 3 patients. Quality-of-life questionnaires indi-
cated that 7 of 13 patients had persistent pain,and 3 of 13 patients complained of major func-tional and cosmetic limitations. These papers
have resulted in recent increased interest ongrowth preservation of the spine and thorax inyoung children with severe spinal deformity.
Patient evaluation
Severe spinal deformity in children results frommany etiologies and is associated with a variety of
comorbidities. The preoperative evaluation of thispopulation requires a multidisciplinary team ofphysicians. Although the orthopedic surgeonoften is asked to be the team leader, additional
expertise is virtually always needed, includingradiology, pulmonary medicine, cardiology, nu-trition, and others. When considering a manage-
ment strategy that involves significant risks,repeated surgeries, and prolonged growth, thechild’s health and the family’s ability to cope
with and endure this form of treatment must beevaluated thoroughly.
Indications
The use of growth-sparing instrumentation isindicated in patients who have progressive spinal
deformity that cannot be controlled by nonoper-ative means, such as bracing, and where there issignificant spinal growth remaining. The surgeonmust consider the risk versus benefit of this course
of treatment. Factors, including age, curve sever-ity, curve type, growth remaining, and the child’sgeneral health and ability to tolerate multiple
surgeries, must be considered in relationship tothe benefit of continued growth of the spine.
Instrumentation options
The first use of spinal instrumentation withoutfusion dates back to the introduction of the
Harrington rod. Harrington [8] concluded that fu-sion should not be considered in children youngerthan 10 years of age. Moe and colleagues [9] re-
ported that a singleHarrington rod placed subcuta-neously through limited incisions without fusionresulted in preservation of growth in the instru-
mented spine. Further studies of this techniquewith newer-generation implants have shown im-provement inCobbangles and sagittal contour [10].
Luque ‘‘trolleys’’ have been used to control
progressive curves using segmental instrumenta-tion. Rinsky and colleagues [11] reported thatthere was an average 32% loss of correction at
a mean follow-up of 28 months, with minimalpreservation of spinal growth and a high incidenceof rod breakage; they concluded that these early
results were discouraging. Pratt and colleagues[12] reported that the use of a Luque trolley aloneresulted in a significant loss of correction over

549GROWTH SPARING INSTRUMENTATION
Fig. 1. (A) Five-year-old boy who had infantile (early-onset) scoliosis that failed nonoperative brace management. (B)
Postoperative posteroanterior radiograph after placement of dual growing rods using a hybrid hook pedicle screw con-
struct and tandem connectors for rod expansion.
time and noted only 32% of predicted spinalgrowth over the time of treatment.
The significant incidence of rod breakage and
hook failure with single growing-rod constructsled Akbarnia and colleagues [13] to develop thedual growing-rod technique (Fig. 1). This tech-
nique establishes anchor points in the upper andlower spine using hooks or pedicle screws and
passes rods subcutaneously, attached by parallelconnectors that allow for rod distraction withgrowth. Early results with this technique in a het-
erogenous group of patients documented the abil-ity to preserve spinal growth and improve theCobb angle over time. Thompson and colleagues
[14] compared single with dual growing rods;dual growing rods provided superior outcomes.
Fig. 2. (A) Five-year-old girl with a history of an omphalocele and progressive early-onset scoliosis resulting in pelvic
obliquity. She had failed brace treatment. (B) Standing posteroanterior (PA) view of the spine showing scoliosis and pel-
vic obliquity measuring 87�. (C) Standing PA view of the spine after placement of bilateral percutaneous rib to pelvis
VEPTR constructs.

550 SMITH
Fig. 3. (A) Twenty-month-old child who had a severe gibbus deformity associated with myelodysplasia and early skin
breakdown over the gibbus deformity. (B) Sagittal MRI showing the gibbus deformity. Lateral (C) and anteroposterior
radiographs (D) demonstrating short-term follow-up after placement of bilateral rib to pelvis VEPTR constructs. This
technique allows for control of the deformity while avoiding poor midline skin.
Additionally, they reported that the apical fusionwas detrimental to the overall growth of the spine
and should be avoided.A new alternative for the treatment of pro-
gressive scoliosis is the use of VEPTR. The
VEPTR was developed by Dr. Robert Campbell,Jr. for the treatment of thoracic insufficiencysyndrome (TIS), defined as the inability of the
thorax to support normal respiration and lunggrowth [15]. Typically, TIS is the result of thetethering effect of congenital rib fusions and
scoliosis that produces a constriction of the hemi-thorax and reduced lung volumes; it also can re-
sult from other syndromes associated witha hypoplastic thorax. This reduced volume re-stricts growth of the lung, especially during the
critical ages of lung growth during the first 8 yearsof life.
The interdependent relationship between sco-
liosis and chest wall deformity led to the de-velopment of expansion thoracoplasty andstabilization using the VEPTR device [16]. This

551GROWTH SPARING INSTRUMENTATION
procedure is able to promote lung growth and spi-nal growth without fusion and avoids the deleteri-ous effects of early fusion [7]. Gollogly andcolleagues [17] documented an increase in lung
volumes following expansion thoracoplasty mea-sured by CT scan.
The VEPTR device also has been used to treat
progressive scoliosis without fused ribs without theaddition of an expansion thoracoplasty. As a min-imally invasive alternative to growing rods, Smith
developed the bilateral percutaneous VEPTR tech-nique. In this technique, the VEPTR devices areattached to the ribs through a small proximal
midline incision. Distally, the implant is seated onthe pelvis using a modified Dunn McCarthy hookor is anchored to the spine using laminar hooks(Fig. 2). The devices are expanded at 6-month inter-
vals during growth. Smith and Smart [18] reportedthe early pilot data with this technique, noting sat-isfactory control of curve progression anda compli-
cation rate that is similar to other growinginstrumentation techniques. Long-term follow-updata are lacking with this technique. A recent re-
view of mid-term follow-up data suggested thatthis procedure should be used with caution in am-bulatory children because of a forward shift in sag-
ittal balance and resultant crouched gait (JT Smith,unpublished data, 2007). It has been useful in chil-dren who have neuromuscular disease, such asspina bifida (Fig. 3) [19]. Complications remain
problematic, as with all fusionless systems.
Future directions
The ability to control progressive spinal de-
formity and children using fusionless spinal in-strumentation systems remains a significantchallenge for the future. Current methods are
fraught with an unacceptable rate of complica-tions, most notably loss of fixation, implantbreakage, and device migration. There is a signifi-
cant need for self-expanding implants and bettermethods for fixation to the spine and chest wall,obviating the need for multiple surgeries for ex-
pansion of growing instrumentation.
References
[1] Dimeglio A. Growth in pediatric orthopaedics. In:
Morrissy RT,Weinstein SL, editors. Lovell andWin-
ter’s pediatricorthopaedics. 5th edition. Philadelphia:
Lippincott, Williams and Williams; 2001. p. 50–3.
[2] Jones RS, Kennedy JD, Hasham F, et al. Mechani-
cal inefficiency of the thoracic cate in scoliosis.
Thorax 1981;36:456–561.
[3] Davies G, Reid L. Effect of scoliosis on growth of
alveoli and pulmonary arteries on the right ventricle.
Arch Dis Child 1971;46:623–32.
[4] PehrssonK, Larsson S, OdenA, et al. Long term fol-
low up of patients with untreated scoliosis. A study
of mortality, causes of death and symptoms. Spine
1992;17(9):1091–6.
[5] Dimeglio A, Bonnel F. Le rachis en coissance [The
spinal column in growth]. Paris: Springer Verlag;
1990.
[6] Goldberg CJ, Gillic I, Connaughton O, et al. Respi-
ratory function and cosmesis atmaturity in infantile-
onset scoliosis. Spine 2003;28(20):2397–406.
[7] Emans J, Kassab F, Caubet JF, et al. Earlier and
more extensive fusion is associated with diminished
pulmonary function. Outcome after spinal fusion
of 4 or more thoracic spinal segments before Age
5. Scoliosis Research Society AnnualMeeting. Paper
101, Buenos Aires (Argentina), September 7, 2004.
[8] Harrington PR. Scoliosis in the growing spine.
Pedriatr Clin North Am 1963;10:225–45.
[9] Moe JH, Kharrat K, Winter RB, et al. Harrington
instrumentation without fusion plus external or-
thotic support for the treatment of difficult curvature
problems in young children. Clin Orthop Relat Res
1984;185:35–45.
[10] Blakemore LC, Scoles PV, Poe-Kochert C, et al.
Submuscular isola rod with or without limited apical
fusion in the management of severe spinal defor-
mities in young children: preliminary report. Spine
2001;26:2044–8.
[11] Rinsky L, Gamble JG, Bleck EE. Segmental instru-
mentation without fusion in children with progres-
sive scoliosis. J Pediatr Orthop 1985;5:687–90.
[12] Pratt RK, Webb JK, Burwell RG, et al. Luque trol-
ley and convex hemiepiphysiodesis in the manage-
ment of infantile and juvenile idiopathic scoliosis.
Spine 1999;25:1538–47.
[13] Akbarnia BA, Marks DS, Boachie-Adjei O, et al.
Dual growing rod technique for the treatment of
progressive early onset scoliosis: a multicenter study.
Spine 2005;30:S46–57.
[14] Thompson GH, Akbarnia BA, Kostial P, et al.
Comparison of single and dual growing rod tech-
niques followed through definitive surgery. A pre-
liminary study. Spine 2005;30:2039–44.
[15] Campbell RM, Smith MD, Mayes TC, et al. The
characteristics of thoracic insufficiency syndrome as-
sociated with fused ribs and congenital scoliosis.
J Bone Joint Surg Am 2004;85:399–408.
[16] Campbell RM, SmithMD,Mayes TC, et al. The effect
of opening wedge thoracostomy on thoracic insuffi-
ciency syndromeassociatedwith fusedribsandcongen-
ital scoliosis. J Bone Joint Surg Am 2004;86:1659–74.
[17] Gollogly S, Smith JT, Campbell RM. Determining
lung volume with three dimensional reconstructions

552 SMITH
of CT scan data: a pilot study to evaluate the effects
of expansion thoracoplasty on children with severe
spinal deformities. J Pediatr Orthop 2004;24:323–8.
[18] Smith JT, SmartMP. Treatment of progressive spinal
deformity using a bilateral dual VEPTR construct
fromribs topelviswithout thoracoplasty: a pilot study
of 10 patients. IMAST. Podium presentation, 2004.
[19] Smith JT, Smart MP. VEPTR in spina bifida.
IMAST. E-Poster. Scoliosis Research Society.
Athens (Greece), July 9, 2006.

Orthop Clin N Am 38 (2007) 553–562
Scoliosis Associated with NeurofibromatosisAlvin H. Crawford, MD, FACSa,*, Jose Herrera-Soto, MDb
aCincinnati Children’s Hospital, 3333 Burnet Avenue, ML 2017, Cincinnati, OH 45229-3039, USAbOrlando Regional Medical Center, 86 West Underwood Street, Orlando, FL 32806, USA
Neurofibromatosis type 1 (NF-1), also calledvon Recklinghausen disease or peripheral neuro-fibromatosis, is a multisystemic disease that pri-
marily affects cellular growth of neural tissue [1].The entity is one of the most common dominantlyinherited gene disorders of the nervous system in
humans, affecting 1 in 4000 individuals [2]. Thereis no gender or ethnic predilection [1,3]. Approxi-mately 50% of all cases of NF-1 are due to new
mutations, which is 100-fold higher than the usualrate for a single locus and may reflect the huge sizeof the NF-1 1ocus (estimated at 350,000 base
pairs). The gene responsible for NF-1 has beenidentified and is localized to chromosome 17q[3]. The product for this gene is neurofibromin.Neurofibromin is involved in controlling cellular
growth and its differentiation. Therefore, it worksas a tumor suppressor gene [4]. Prenatal testing isnow possible in some families, but its use is mini-
mal becausedin most patientsdmutations havenot been easy to identify. Patients who haveNF-1 develop Schwann cell tumors called ‘‘neuro-
fibromas’’ and pigmentation abnormalities [2].Cloning the gene has allowed the creation of ani-mal models that ultimately may be used to de-velop more effective therapy against the disease.
NF-1 is a multisystemic disease. It may man-ifest as abnormalities of the nervous tissue, bones,soft tissue, and skin. The manifestations of NF-1
vary from person to person and range fromsubclinical to severe. Individuals who carry thegene eventually exhibit some clinical feature of the
disease. The penetrance for NF-1 nears 100%during adulthood. Skeletal abnormalities are
* Corresponding author.
E-mail address: [email protected]
(A.H. Crawford).
0030-5898/07/$ - see front matter � 2007 Elsevier Inc. All r
doi:10.1016/j.ocl.2007.03.008
common in NF-1; most patients present withsome type of bony dysplasia. The orthopediccomplications usually appear early. They include
spinal deformities, such as scoliosis or kyphosis,congenital tibial dysplasia with bowing and pseu-darthrosis of the tibia, forearm, other bones, as
well as overgrowth phenomenon of an extremity,and soft tissue tumors [2,3,5,6].
The clinical criteria for the diagnosis were
determined in 1987 by the National Institute ofHealth Consensus Development Conference (Box 1)[7]. To establish the diagnosis for NF-1, two of the
seven criteria must be present. These criteria areuseful, even in young children.
Type 2 neurofibromatosis (NF-2) also is anautosomal dominant disorder. NF-2 is not as
common as NF-1, affecting about 1 in 100,000individuals. The NF-2 gene is located on chromo-some 22 [8]. Characteristically, individuals who
have NF-2 present bilateral schwannomas of thevestibular portion of the eighth cranial nerve.Schwannomas of other peripheral nerves, menin-
giomas, and ependymomas also are common [9].No patients who have NF-1 have the eighth cra-nial nerve tumors [3]. NF-2 does not seem tohave orthopedic manifestations.
Segmental NF is another form of NF in whichfeatures of NF-1 (ie, cafe au lait spots, freckling,and neurofibromas) are seen in only one segment of
the body. This is believed to be due to somaticmosaicism for the NF-1 gene mutation. A finalform, schwannomatosis, was described recently; it
involves multiple deep and painful schwannomas.It may be genetically distinct fromNF-1 andNF-2.
Imaging studies
Complete spinal radiographs should be scruti-nized closely for thoracic lordosis and
ights reserved.
orthopedic.theclinics.com

554 CRAWFORD & HERRERA-SOTO
cervicothoracic kyphosis. Spinal deformities in-clude dystrophic and nondystrophic changes. The
radiographic appearance of dystrophic changesinclude scalloping of the vertebral borders, severerotation of the apical vertebra, widening of the
spinal canal, enlargement of the neural foramina,hypoplastic or absent pedicles, paraspinal masses,spindling of the transverse process, and rotationof the ribs, which resemble twisted ribbons (Table
1) [6,10–12].All patients who have NF-1 who require
endotracheal anesthesia, who undergo halo trac-
tion, or who present with neck tumors should
Box 1. Diagnostic criteria forneurofibromatosis type 1
More than six cafe au lait spotsmeasuring at least 15 mm in adultsand 5 mm in children
Two or more neurofibromas of any typeor one plexiform neurofibroma
Freckling in the axillary or inguinalregions
Optic gliomaTwo or more Lisch nodules (ie, iris
hamartomas)A distinctive bony lesion, such as
sphenoid wing dysplasia, or thinningof the cortex of a long bone with orwithout pseudarthrosis
A first-degree relative with NF-1, assuggested by these criteria
Since the consensus panel meeting,specific kinds of learning disabilitiesand MRI abnormalities (especially inchildren) have been associatedspecifically with NF-1. The pediatricorthopedist encounters otherconditions associated with cafe au laitspots, namely, Watson’s syndrome,fibrous dysplasia (ie, McCune-Albrightsyndrome), LEOPARD (lentigines,electrocardiogram [EKG]abnormalities, ocular hypertelorism,pulmonary stenosis, abnormalities ofgenitalia, retardation of growth, anddeafness) syndrome, and Noonan’ssyndrome. Only the gene forWatson’s syndrome has been linkedto the NF-1 locus.
receive radiographic imaging of the cervical spine.Other reasons for obtaining cervical spinal radio-graphs in a patient who has NF-1 include theevaluation of torticollis or dysphagia possibly
secondary to tumors. If instability or subluxationis suspected, tomograms, CT scans, or MRIs areappropriate. MRI should be performed to evalu-
ate any progressive spinal deformity in NF-1 [3].
Spinal pathology
A high percentage of patients who have NF-1develop some type of spinal disorder during their
lifetime [3,13,14]. We discuss our approach to in-dividuals who have NF-1 under the followingtopics: cervical, thoracic/thoracolumbar, lumbo-
sacral, and spinal canal problems.
Cervical spine changes and associatedcomplications
Features of the cervical spine in patients whohave NF-1 have not received enough attention in
the literature [13,15]. The cervical spine should beevaluated at the initial scoliosis assessment. Cervi-cal abnormalities occur more frequently whenscoliosis or kyphoscoliosis is present in the thora-
columbar region where the examiner’s attention isfocused on the more obvious deformity.
Evidence of dystrophic changes may be present
on a true cervical lateral view. The manifestationsof NF-1 can be observed as dystrophic changes inthe vertebral body or they can be due to patho-
logic alignment [16]. If any suspicious area isnoted on plain radiographs, right and left obliqueviews should be obtained to look for widening of
Table 1
Nine radiographic characteristics of dystrophic defor-
mity as seen in 457 children
Characteristics % incidence
Rib penciling 62
Vertebral rotation 51
Posterior vertebral scalloping 31
Vertebral wedging 36
Spindling of transverse processes 31
Anterior vertebral scalloping 31
Widened interpediculate distance 29
Enlarged intervertebral foramina 25
Lateral vertebral scalloping 13
From Durrani AA, Crawford AH, Choudry SN,
et al. Modulation of spinal deformities in patients with
neurofibromatosis type 1. Spine 2000:25:69–75; with
permission.

SCOLIOSIS ASSOCIATED W
the neuroforamina. These may represent dumb-bell lesions caused by enlarged neurofibromas ex-iting from the spinal canal. MRI is the definitivestudy to evaluate these lesions.
The most common cervical abnormality ob-served is a severe cervical kyphosis, which, initself, is highly suggestive of the disorder. In the
study of Yong-Hing and colleagues [17] 17 pa-tients who had NF-1 had cervical abnormalities.Of these, 7 patients were asymptomatic, whereas
the rest had limited motion or pain in the neck.Four patients had neurologic deficits that were at-tributed to cervical instability. Four of the 17 pa-
tients required fusion of the cervical spine. Curtisand colleagues [18] described 8 patients who hadparaplegia and NF-1. Four of these patients hadcervical spine instability or intraspinal pathology
in the cervical spine.Attention also should be given to the atlan-
toaxial region. Isu and colleagues [19] described
three patients who had NF-1 who had C1–C2dislocation with neurologic deficit. All patientsimproved after decompression and fusion. Prob-
lems often occur after excision of cervical tumorswhen excision includes resection of the laminaeand posterior elements. Postoperatively, the spine
becomes unstable and progressive kyphosis de-velops. The best prevention is to avoid completelaminectomies or perform spinal instrumentationwith abundant bone grafting at the time of de-
compression to prevent instability [20]. Combinedanterior and posterior spinal fusion is recommen-ded for cervical kyphosis if there is severe defor-
mity and instability [21].Some patients may need fusion in the cervical
spine as well as in the thoracic region. This group
of patients may benefit from a ‘‘trap door’’ sternalsplit approach if anterior fusion is needed (Fig. 1)[22,23]. This approach allows anterior exposure ofthe lower cervical and upper thoracic spine.
Scoliosis
Scoliosis is the most common osseous defectassociated with NF-1 [3]. Weiss [24] andGould [25]
were the first to emphasize the high incidence of spi-nal deformities. It may vary in severity from mildand nonprogressive to severe curvatures. The exact
etiology is unknown, but it has been suggested to besecondary to osteomalacia, localized neurofibrom-atous tumor eroding and infiltrating bone, endo-
crine disturbances, or mesodermal dysplasia [1].In a general orthopedic clinic, 2% of patients
who have scoliosis have neurofibromatosis,
whereas in a neurofibromatosis clinic, 10% to20% of patients have some disorder of the spine.All preadolescent children who have neurofibro-matosis should be evaluated with scoliosis screen-
ing or the Adams forward bend test to excludea spinal deformity. Usually, scoliosis occursearlier in children who have neurofibromatosis
compared with idiopathic scoliosis.Two primary types of scoliosis are observed in
persons who have neurofibromatosis: dystrophic
and nondystrophic [1]. Dystrophic scoliosis inNF-1 is characterized by early-onset, rapid pro-gression that is difficult to treat. Nondystrophic
scoliosis behaves similar to idiopathic scoliosis,and the treatment is similar.
Natural historyIt is important to understand the natural
history of a condition to make good clinical and
surgical treatment decisions. Calvert and col-leagues [26] presented a series of treated (n ¼34) and untreated (n ¼ 32) patients who had
NF-1 and scoliosis. Seventy-five percent of pa-tients in the non-treated group had kyphoscolio-sis. The investigators reported that patients whohad severe anterior vertebral scalloping, noted
on the lateral view, progressed an average of 23�
per year for scoliosis and kyphosis. All other pa-tients had an average rate of scoliosis progression
of 7� and kyphosis progression of 8� per year.Despite solid spinal fusions, some dystrophic
patients demonstrate curve progression. A study
by Wilde and colleagues [27] showed that verte-bral subluxation, disc wedging, and peripheralskeletal dystrophy are additional prognostic fea-
tures that predict the progression of deformity af-ter arthrodesis of the spine. Patients who hadhyperkyphosis (kyphosisO50� and sharply angu-lated over three vertebrae), despite successful spi-
nal fusion, were noted to progress up to 38�
(range, 20�–60�) in one study [27].
Nondystrophic scoliosis
The most common curvature is nondystrophic,similar to curves observed in adolescent idiopathic
scoliosis in pattern and behavior [3]. This formusually involves 8 to 10 spinal segments. Most of-ten, the deformity is convex to the right. Some of
these curves acquire dystrophic changes (ie,‘‘modulate’’) over time. Early MRI of all progres-sive curves is recommended to evaluate for spinal
cord pathology and to examine apparent nondy-strophic curves for dystrophic changes. With earlyadvanced imaging, we believe that the modulation
555ITH NEUROFIBROMATOSIS

556 CRAWFORD & HERRERA-SOTO
Fig. 1. (A, B) Cervicothoracic deformity in a patient who has neurofibromatosis. (C, D) CT scan of the upper thoracic
spine demonstrates rib head subluxation. (E, F) Postoperative films following anterior cervicothoracic fusion performed
through a sternal splitting ‘‘trap door’’ procedure and posterior spinal instrumentation and fusion.
of some nondystrophic to dystrophic deformitiescan be detected before typical dystrophic changesare seen on plain radiographs.
Durrani and colleagues [28] reported that‘‘modulation’’ occurred in about 65% of patientsoverall. Modulation occurred in 81% of patients
who presented with scoliosis before 7 years ofage and in 25% of those diagnosed after 7 yearsof age. In this study, rib penciling acquired
through the modulation period was the only fac-tor that influenced progression of the deformity.The rate of progression for ‘‘modulated’’ scoliosisand kyphosis was 12� and 8�, respectively, versus5� and 3� for nonmodulated spines.
Nondystrophic curvatures of less than 25�
should be observed. Curves between 25� and 40�
can be treated with brace successfully [1,29]. Oncebeyond 40�, surgery by posterior spinal fusion isindicated (Fig. 2) [3].
Dystrophic scoliosis
Dystrophic scoliosis is characterized by early-onset, rapidly progressive curves that are difficultto treat [30,31]. The dystrophic curve is a short-segmented, sharply angulated type that includes
fewer than six spinal segments. It has a tendencyto progress to a severe deformity. Dystrophiccurves may be associated with kyphosis and
have a higher incidence of neurologic injury [3,30].Dystrophic vertebral changes develop over
time; on plain films, they are manifest by vertebral
scalloping, rib penciling (rotation of the rib about90�), spindling of the transverse processes, severeapical rotation, severe vertebral wedging, and
wide nerve root foramina (see Table 1). Most ofthese patients present with associated neurofi-bromas that envelope the bone or come from
the canal (dumbbell lesion). Dystrophic curvesare found most commonly in the thoracic region(Fig. 3) [1].
Enlargement of the spinal canal caused byintraspinal tumors or dural ectasia is common.Dural ectasia is an expansion of the thecal sac,
probably due to increased hydrostatic pressure. Iterodes the bony and ligamentous structures caus-ing vertebral scalloping and meningocele forma-tion [32].
Dystrophic curvatures of less than 20� shouldbe observed for progression at 6-month intervals[13]. Bracing of progressive dystrophic curvatures
is contraindicated simply because it has not beenfound to be effective [29,33,34]. For adolescent pa-tients with dystrophic curvature greater than 20�
to 40� of angulation, a posterior spinal fusionwith segmental spinal instrumentation is recom-mended [13,34]. In more severe dystrophic scolio-sis, anterior fusion often is performed in addition
to posterior fusion, to increase the fusion rate andto reduce the risk for progression despite solidposterior fusion.
Infantile, juvenile, and young adolescent pa-tients who have dystrophic scoliosis representchallenging treatment groups. Posterior spinal
fusion alone is now believed to be contraindicatedin young patients who have progressive dystro-phic deformities. A prevalence of pseudoarthrosis
of up to 60% has been reported in the literatureafter posterior spinal fusion only [13,30,35,36]. Al-though some surgeons may perform posterior

557SCOLIOSIS ASSOCIATED WITH NEUROFIBROMATOSIS
Fig. 2. This patient who has nondystrophic scoliosis shows several characteristics of possible early modulation, such as
a high apex left curve that is progressing rapidly. Other osseous changes diagnostic of dystrophic curves, such as rib pen-
ciling and vertebral scalloping, are not present (A,B). Nondystrophic scoliosis can be treated similarly to idiopathic ad-
olescent scoliosis, with posterior spinal instrumentation and fusion (C,D).
fusion with abundant autologous bone graft andpedicle screw instrumentation with good long-
term results, the more predictable and successfulprocedure is anterior and posterior spinal fusionwith segmental instrumentation and bone grafting
[13,22,29,31,33,34,37–40]. The anterior fusion canbe performed by thoracotomy or thoracoscopy
[41–43]. It is even appropriate to fuse the youngchild who has dystrophic scoliosis greater than
40�, based on the known natural history of certainprogression for this curve type [1,13,34]. An earlyfusion causes minimal stunting of growth that is
due to poor growth potential of the involved seg-ments [1].
Fig. 3. This dystrophic deformity has a similar curve location to that illustrated in Fig. 2; however, the curves are much
more severe, short, sharp, and associated with dystrophic osseous changes.

558 CRAWFORD & HERRERA-SOTO
In theory, the use of subcutaneous, so-called‘‘growing rods’’ allows for further growth, al-though some have questioned their value on the
basis of the small amount of growth achieved andthe number of procedures required. The authorshave used submuscular growing rods on early-onset dystrophic curves with or without anterior
annulotomies with a great deal of optimism. If thecurve is less than 60� and flexible, the rods areinserted directly with fusion of the cranial and
caudal anchors only followed by lengtheningevery 6 months (Fig. 4). In large stiff curves, ante-rior annulotomies without fusion (to preserve
growth) have been performed. Our early resultsare extremely encouraging. This is a promisingtechnique made especially useful because mostdystrophic curves are early onset.
Often, bracing following surgery is appropriate[44,45]. Bracing may need to be extended to thecervical region in cases of severe dysplastic curves
that are instrumented into the upper thoracic andcervicothoracic region. Cervical bracing, halo
vest, or Minerva casting may help to prevent thepossibility of screw/hook pullout. This is espe-cially true for dysplastic curves that have low
bone mineral density [4].Preoperative halo traction may be beneficial
for the treatment of severe curves, including thosewith kyphoscoliosis [34,44,46,47]. It allows grad-
ual and controlled soft tissue relaxation and curvecorrection before surgery or between staged sur-geries; however, it is contraindicated in patients
who have cervical kyphosis. Daily neurologicevaluations are mandatory to avoid spinal or cra-nial nerve injuries. When staged procedures are
planned, interim halo-femoral traction has beenused successfully [48]. Nutrition is also paramountduring this time. We use supplemental nasojejunalfeeding in between stages to decrease the protein
depletion that is seen in staged patients [49,50].During surgery, careful posterior subperiosteal
dissection is performed by using Bovie electro-
cautery dissectiondrelying less on subperiostealelevatorsdto reduce the risk for inadvertently
Fig. 4. (A) An early onset patient was treated unsuccessfully with brace-cast-brace treatment. (B–D) Subcutaneous
‘‘growing rods’’ were placed to prevent further progression and to allow growth of the spine until definitive surgery could
be performed closer to skeletal maturity (E).

559SCOLIOSIS ASSOCIATED WITH NEUROFIBROMATOSIS
plunging through areas of laminar defects orhypoplasia and directly damaging the spinalcord. Anterior spinal dissection may be compli-cated by venous lakes and engorgement of saccu-
lar, almost sinusoidal, vessels, which are difficultto control in and around the vertebral bodies.Extensive blood loss from the blood vessels in the
cancellous bone of the vertebral bodies is dis-tinctly possible. We recommend a putty of Avi-tine, Gelfoam, and Thrombin to assist in
achieving hemostasis. Surgicel and Flosseal alsohelp with hemostasis.
Discectomies should be performed with Bovie
dissection and the use of a rongeur through theannulus fibrosis instead of sharp dissections of theendplate apophysis. Sharp dissection may causesignificant bleeding from the often friable cancel-
lous matrix of the vertebral bodies. Care shouldbe taken to preserve the segmental vessels as muchas possible. If sectioning of segmental vessels is
necessary, the authors recommend staging pro-cedures to allow reperfusion of the anteriorcolumn.
Lordosis
Lordoscoliosis also has been identified andmay represent a subset of dystrophic deformity.
It is a poorly reported entity, but it may havesignificant long-term implications. Often, there isassociated posterior element erosion and dural
ectasia [6,51]. Thoracic lordosis has been associ-ated with decreased pulmonary function [52].
Kyphosis
Kyphoscoliosis is defined as scoliosis accompa-nied by a kyphosis of greater than 50�. It may occurby gradual scoliotic rotation and progression or it
can be found early in the disease with an abruptangular kyphotic curve [51]. Kyphosis observed inindividuals who have NF-1 is distinguished by
acute anteroposterior angulation. Vertebral bodiesmay be deformed so severely that they are confusedwith congenital deformities. Occasionally, weaken-ing of the spinal stabilizers (eg, facets, pedicles, and
ligaments) by dural ectasia with meningocele for-mation gives rise to kyphosis with subluxation,and, in extreme cases, dislocation of the spine
[53]. Even with severe ‘‘hair pin turn’’ angulation,neurologic status usually remains normal, and thespinal cord often is protected because the spinal ca-
nal is widened by dural ectasia.Traction may be dangerous when performed
on rigid deformities because it increases tension
on the midapical spinal cord. Traction followinganterior release is safe when monitored appropri-ately. For curves greater than 50�, anteriorsurgery (intervertebral discectomy, rib strut graft-
ing, and bone chip grafting) is recommended,followed by posterior segmental instrumentationone or two levels above and below the end
vertebrae [1,13,27,44]. For severe deformities (ie,O80�–90�), indefinite bracing may be required un-til solid union is achieved, even after anterior and
posterior spinal surgery.Severe kyphosis is the most common cause of
neurologic deficits in NF-1 [3]. Because of the as-
sociation of paraplegia with kyphosis, physicianshave tended to perform laminectomies. Laminec-tomy alone for kyphotic cord compression is ab-solutely contraindicated [3]. Posterior vertebral
element resection does not relieve the anteriorcompression on the spinal cord, and, in fact, hasnot been shown to improve the condition [44].
The offending neurofibromas usually are anterior,and decompression should be performed anteri-orly. The removal of posterior element predis-
poses the spine to instability and there is loss ofvaluable bone stock required for fusion. Anteriordecompression with posterior spinal fusion and
instrumentation should be performed [44,54].
Spondylolisthesis
Spondylolisthesis/spondyloptosis is a rare dis-
order that is associated most often with apathologic luxation of the vertebra caused byerosions or elongation of the pedicles or pars
from foraminal neurofibroma or dural ectasia[1,12,13,55–58]. This leads to forward progressionof the anterior spinal column elements (Fig. 5)[59]. Surgery is indicated with the progression of
the spondylolisthesis from grade II to grade IIIor with the presence of pain that cannot be con-trolled sufficiently by nonoperative means. Ante-
rior and posterior stabilization is recommendedfor progressive deformity [55]. An alternative toinstrumentation is to perform posterior spinal fu-
sion and autologous bone grafting augmentedwith pantaloon casting. It is imperative to reassessthe fusion mass approximately 6 months postop-eratively and repeat bone grafting performed if
necessary.
Soft tissue abnormalities
Subcutaneous plexiform neurofibromas oftenoverlie the incision area. When posterior spinalfusion surgery is performed, one should be aware

560 CRAWFORD & HERRERA-SOTO
Fig. 5. (A, B) NF-1 also can cause deformity in the low lumbar spine, such as scoliosis associated with severe spondy-
lolisthesis. (C) CT sagittal reconstruction confirms grade IV spondylolisthesis, posterior vertebral body scalloping, and
additional osseous changes. (D) 3-D reconstruction rendering illustrates dural ectasia in this region.
of the thin laminae that often are eroded by duralectasia surrounding the spinal cord in the thoracicregion. The laminae may be inadequate to accept
hooks; pedicle screws may be necessary. Consider-able bleeding may occur with dissection aroundsubcutaneous vascular tumors. The authors rec-
ommend using monopolar and bipolar electro-cautery for subperiosteal exposure of the posteriorelements.
Meningoceles, pseudomeningoceles, dural ec-
tasia, and dumbbell lesions are related to thepresence of neurofibroma or abnormal pressurephenomena in and around the spinal canal
neuraxis. High-volume myelography or MRIshould be used in the investigation of all dystro-phic curves before surgical treatment [3,32]. Occa-
sionally, these intraspinal elements maycompromise the cord directly when instrumenta-tion and stabilization are attempted, or theymay cause erosive changes in the bone, preventing
primary fusion.
Pitfalls in spinal deformities in neurofibromatosistype 1
There is a known increased prevalence ofosteoporosis among patients who have NF-1 [4].
This can create problems in fixation of dystrophiccurves [29]. The bone is soft and nonresistant tomanipulation.
Paraplegia is an uncommon finding in patientswho have dystrophic curves [18,33]. It is moreprevalent in patients who have severe vertebral
angulation (kyphosis), vertebral subluxation, andsoft tissue tumors in the spinal canal [18]. Arare, but important, cause of paraparesis in scoli-
otic patients is spinal cord compression due to ribpenetration [60–62]. It is imperative to evaluatefor such a condition in the preoperative period.A CT scan is the most sensitive tool to diagnose
intraspinal rib dislocation. A resection of the ribwill prevent or improve paraparesis in most pa-tients who have dislocation.
Failure to recognize intraspinal lesions inpatients who have neurofibromatosis and undergomanipulation and instrumentation of the spine
may result in neurologic compromise. Preopera-tive radiography, CT, or MRI is essential forpatients who have dystrophic vertebral elementsand curvatures requiring fusion. Be especially
alert to the possibility of subluxated ribs in thespinal canal. It the surgeon’s responsibility tostabilize the spine with the most expedient, safe,
and permanent method without causing neuro-logic injury [3].
References
[1] CrawfordAH.Neurofibromatosis. In:WeinsteinSL,
editor. The pediatric spine, principles and practice.

561SCOLIOSIS ASSOCIATED WITH NEUROFIBROMATOSIS
2nd edition. Philadelphia: Lippincott Williams &
Wilkins; 2001. p. 471–90.
[2] Crawford AH, Schorry EK. Neurofibromatosis up-
date. J Pediatr Orthop 2006;26(3):413–23.
[3] Crawford AH, Parikh S, Schorry EK, et al. The im-
mature spine in type-1 neurofibromatosis. J Bone
Joint Surg Am 2007;89:123–42.
[4] Lammert M, Kappler M, Mautner VF, et al. De-
creased bone mineral density in patients with neuro-
fibromatosis 1. Osteoporos Int 2005;16(9):1161–6.
[5] Gabriel KR. Neurofibromatosis. Curr Opin Pediatr
1997;9(1):89–93.
[6] Crawford AH, Schorry EK. Neurofibromatosis in
children: the role of the orthopaedist. J Am Acad
Orthop Surg 1999;7(4):217–30.
[7] National Institute of Health Consensus Develop-
ment Conference. NF-1. 1988. p. 172–8.
[8] Rouleau GA, Wertelecki W, Haines JL, et al. Ge-
netic linkage of bilateral acoustic neurofibromatosis
to a DNA marker on chromosome 22. Nature 1987;
329(6136):246–8.
[9] Mautner VF, TatagibaM, LindenauM, et al. Spinal
tumors in patients with neurofibromatosis type 2:
MR imaging study of frequency, multiplicity, and
variety. AJR Am J Roentgenol 1995;165(4):951–5.
[10] Vitale MG, Guha A, Skaggs DL. Orthopaedic man-
ifestations of neurofibromatosis in children: an up-
date. Clin Orthop Relat Res 2002;401:107–18.
[11] Crawford AH. Neurofibromatosis in children. Acta
Orthop Scand Suppl 1986;218:1–60.
[12] Crawford AH Jr, Bagamery N. Osseous manifesta-
tions of neurofibromatosis in childhood. J Pediatr
Orthop 1986;6(1):72–88.
[13] Crawford AH. Pitfalls of spinal deformities associ-
ated with neurofibromatosis in children. Clin
Orthop Relat Res 1989;245:29–42.
[14] Akbarnia BA, Gabriel KR, Beckman E, et al. Prev-
alence of scoliosis in neurofibromatosis. Spine 1992;
17(8 Suppl):S244–8.
[15] Haddad FS, Williams RL, Bentley G. The cervical
spine in neurofibromatosis. Br J Hosp Med 1995;
53(7):318–9.
[16] Stone JW, Bridwell KH, Shackelford GD, et al.
Dural ectasia associated with spontaneous disloca-
tion of the upper part of the thoracic spine in neuro-
fibromatosis. A case report and review of the
literature. J Bone Joint SurgAm1987;69(7):1079–83.
[17] Yong-HingK,Kalamchi A,MacEwenGD.Cervical
spine abnormalities in neurofibromatosis. J Bone
Joint Surg Am 1979;61(5):695–9.
[18] Curtis BH, Fisher RL, Butterfield WL, et al. Neuro-
fibromatosis with paraplegia. Report of eight cases.
J Bone Joint Surg Am 1969;51(5):843–61.
[19] Isu T, Miyasaka K, Abe H, et al. Atlantoaxial dislo-
cation associated with neurofibromatosis. Report of
three cases. J Neurosurg 1983;58(3):451–3.
[20] Garg S, Hosalkar H, Dormans JP. Quadriplegia in
a 10 year-old boy due to multiple cervical neurofi-
bromas. Spine 2003;28(17):E339–43.
[21] Yonezawa I, Arai Y, Tsuji T, et al. Anterior fusion
and posterior correction of severe cervical kyphosis
using pedicle screw fixation in a patient with neuro-
fibromatosis: a case report. J Spinal Disord Tech
2003;16(5):493–6.
[22] Mulpuri K, LeBlanc JG, Reilly CW, et al. Sternal
split approach to the cervicothoracic junction in chil-
dren. Spine 2005;30(11):E305–10.
[23] Nazzaro JM, Arbit E, Burt M. ‘‘Trap door’’ expo-
sure of the cervicothoracic junction. Technical
note. J Neurosurg 1994;80(2):338–41.
[24] Weiss RA. A curvature of the spine in von Recklin-
hausen’s disease, von Recklinghausen’s disease in
a Negro. Arch Dermatol Syph 1921;iii:144–51.
[25] Gould EP. The bone changes occurring in vonReck-
linhausen’s disease. Q J Med 1918;11:221–8.
[26] Calvert PT, EdgarMA,Webb PJ. Scoliosis in neuro-
fibromatosis. The natural history with and without
operation. J Bone Joint Surg Br 1989;71(2):246–51.
[27] Wilde PH, Upadhyay SS, Leong JC. Deterioration
of operative correction in dystrophic spinal neurofi-
bromatosis. Spine 1994;19(11):1264–70.
[28] Durrani AA, Crawford AH, Chouhdry SN, et al.
Modulation of spinal deformities in patients with
neurofibromatosis type 1. Spine 2000;25(1):69–75.
[29] KimHW,Weinstein SL. Spine update. The manage-
ment of scoliosis in neurofibromatosis. Spine 1997;
22(23):2770–6.
[30] Sirois JL 3rd, Drennan JC. Dystrophic spinal defor-
mity in neurofibromatosis. J Pediatr Orthop 1990;
10(4):522–6.
[31] Holt RT, Johnson JR. Cotrel-Dubousset instrumen-
tation in neurofibromatosis spine curves. A prelimi-
nary report. Clin Orthop Relat Res 1989;245:19–23.
[32] Tsirikos AI, Saifuddin A, NoordeenMH. Spinal de-
formity in neurofibromatosis type-1: diagnosis and
treatment. Eur Spine J 2005;14(5):427–39.
[33] Winter RB, Moe JH, Bradford DS, et al. Spine de-
formity in neurofibromatosis. A review of one hun-
dred and two patients. J Bone Joint Surg Am 1979;
61(5):677–94.
[34] Halmai V,Doman I, de Jonge T, et al. Surgical treat-
ment of spinal deformities associated with neurofi-
bromatosis type 1. Report of 12 cases. J Neurosurg
2002;97(3 Suppl):310–6.
[35] Betz RR, Iorio R, Lombardi AV, et al. Scoliosis sur-
gery in neurofibromatosis. Clin Orthop Relat Res
1989;245:53–6.
[36] Shen JX, Qiu GX, Wang YP, et al. Surgical treat-
ment of scoliosis caused by neurofibromatosis type
1. Chin Med Sci J 2005;20(2):88–92.
[37] Singh K, Samartzis D, An HS. Neurofibromatosis
type I with severe dystrophic kyphoscoliosis and its
operative management via a simultaneous anterior-
posterior approach: a case report and review of the
literature. Spine J 2005;5(4):461–6.
[38] Hopf CG, Eysel P. One-stage versus two-stage spinal
fusion in neuromuscular scolioses. J Pediatr Orthop
B 2000;9(4):234–43.

562 CRAWFORD & HERRERA-SOTO
[39] Parisini P, Di Silvestre M, Greggi T, et al. Surgical
correction of dystrophic spinal curves in neurofibro-
matosis. A review of 56 patients. Spine 1999;24(21):
2247–53.
[40] Al-Sayyad MJ, Crawford AH, Wolf RK. Early ex-
periences with video-assisted thoracoscopic surgery:
our first 70 cases. Spine 2004;29(17):1945–51 [discus-
sion: 52].
[41] Al-Sayyad MJ, Crawford AH, Wolf RK. Video-
assisted thoracoscopic surgery: the Cincinnati expe-
rience. Clin Orthop Relat Res 2005;434:61–70.
[42] Sucato DJ, Elerson E. A comparison between the
prone and lateral position for performing a thoraco-
scopic anterior release and fusion for pediatric spinal
deformity. Spine 2003;28(18):2176–80.
[43] Stagnara P, Biot B, Fauchet R. [Critical evaluation
of the surgical treatment of vertebral lesions due to
neurofibromatosis. 31 cases (1954–1973)]. Rev Chir
Orthop Reparatrice Appar Mot 1975;61(1):17–38
[in French].
[44] Winter RB, Lonstein JE, Anderson M. Neurofibro-
matosis hyperkyphosis: a review of 33 patients with
kyphosis of 80 degrees or greater. J Spinal Disord
1988;1(1):39–49.
[45] Sink EL, Karol LA, Sanders J, et al. Efficacy of peri-
operative halo-gravity traction in the treatment of
severe scoliosis in children. J Pediatr Orthop 2001;
21(4):519–24.
[46] Rinella A, Lenke L, Whitaker C, et al. Perioperative
halo-gravity traction in the treatment of severe sco-
liosis and kyphosis. Spine 2005;30(4):475–82.
[47] Mehlman CT, Al-Sayyad MJ, Crawford AH. Effec-
tiveness of spinal release and halo-femoral traction
in the management of severe spinal deformity.
J Pediatr Orthop 2004;24(6):667–73.
[48] Mooney JF 3rd. Perioperative enteric nutritional
supplementation in pediatric patients with neuro-
muscular scoliosis. J South Orthop Assoc 2000;
9(3):202–6.
[49] Lalueza MP, Colomina MJ, Bago J, et al. Analysis
of nutritional parameters in idiopathic scoliosis pa-
tients after major spinal surgery. Eur J Clin Nutr
2005;59(5):720–2.
[50] Funasaki H, Winter RB, Lonstein JB, et al.
Pathophysiology of spinal deformities in
neurofibromatosis. An analysis of seventy-one pa-
tients who had curves associated with dystrophic
changes. J Bone Joint Surg Am 1994;76(5):692–700.
[51] Winter RB, LovellWW,Moe JH. Excessive thoracic
lordosis and loss of pulmonary function in patients
with idiopathic scoliosis. J Bone Joint Surg Am
1975;57(7):972–7.
[52] Winter RB. Spontaneous dislocation of a vertebra in
a patient who had neurofibromatosis. Report of
a case with dural ectasia. J Bone Joint Surg Am
1991;73(9):1402–4.
[53] Shufflebarger HL. Cotrel-Dubousset instrumenta-
tion in neurofibromatosis spinal problems. Clin
Orthop Relat Res 1989;245:24–8.
[54] Toyoda K, Taguchi T, Kaneko K, et al. High-grade
L5 spondylolisthesis associated with dural ectasia in
neurofibromatosis. J Orthop Sci 2005;10(2):233–6.
[55] Bensaid AH, Dietemann JL, Kastler B, et al. Neuro-
fibromatosis with dural ectasia and bilateral sym-
metrical pedicular clefts: report of two cases.
Neuroradiology 1992;34(2):107–9.
[56] Wong-Chung J, Gillespie R. Lumbosacral spondy-
loptosis with neurofibromatosis. Case report. Spine
1991;16(8):986–8.
[57] Winter RB, Edwards WC. Case report. Neurofibro-
matosis with lumbosacral spondylolisthesis. J Pediatr
Orthop 1981;1(1):91–6.
[58] Mandell GA. The pedicle in neurofibromatosis. AJR
Am J Roentgenol 1978;130(4):675–8.
[59] Khoshhal KI, Ellis RD. Paraparesis after posterior
spinal fusion in neurofibromatosis secondary to rib
displacement: case report and literature review.
J Pediatr Orthop 2000;20(6):799–801.
[60] Deguchi M, Kawakami N, Saito H, et al. Parapare-
sis after rib penetration of the spinal canal in neuro-
fibromatous scoliosis. J Spinal Disord 1995;8(5):
363–7.
[61] Gkiokas A, Hadzimichalis S, Vasiliadis E, et al.
Painful rib hump: a new clinical sign for detecting
intraspinal rib displacement in scoliosis due to neu-
rofibromatosis. Scoliosis 2006;1:1–4.
[62] Major MR, Huizenga BA. Spinal cord compression
by displaced ribs in neurofibromatosis. A report of
three cases. J Bone Joint Surg Am 1988;70(7):
1100–2.

Orthop Clin N Am 38 (2007) 563–572
Spinal Deformities in Marfan SyndromeConstantine A. Demetracopoulos, MD, Paul D. Sponseller, MD*
Department of Orthopaedic Surgery, Johns Hopkins Medical Institutions, The Johns Hopkins Hospital,
601 North Caroline Street, Room 5253, Baltimore, MD 21287, USA
Marfan syndrome (MFS) is an autosomaldominant disorder of connective tissue that dis-plays complete penetrance but variable expression
[1]. Genetic studies localized the FBN1 gene re-sponsible for MFS disease to chromosome15q21 [1,2]. More than 135 mutations in the fibril-
lin gene have been identified, and 70% of affectedindividuals have an identifiable FBN1 mutation[3]. Patients who have Marfan disorder are be-
lieved to have a defect in the synthesis, secretion,or incorporation of fibrillin, a glycoprotein thatis a major component of various types of connec-
tive tissue, including bone [3]. Thus, MFS is a mul-tisystem disease, and manifestations are seen mostcommonly in the ocular, cardiovascular, and skel-etal systems.
The prevalence of MFS is estimated at two tothree cases per 10,000 individuals [4]. Approxi-mately 15% to 25% of patients do not have a fam-
ily history of MFS and may represent de novomutations [3,4]. MFS is a pleiotropic condition,and findings tend to become more apparent with
age. One end of the spectrum represents patientswho are affected only mildly, whereas the otherend represents patients who have a severe neona-tal form who may encounter cardiovascular com-
plications during the first year of life. The mostapparent clinical findings in MFS involve the skel-eton (arachnodactyly, scoliosis and thoracic lor-
dosis, dolichostenomelia, sternal deformities, andjoint laxity). Although these findings are not spe-cific when found individually, the presence of mul-
tiple findings should prompt a referral to geneticsor the echocardiography laboratory.
* Corresponding author.
E-mail address: [email protected] (P.D. Sponseller).
0030-5898/07/$ - see front matter � 2007 Elsevier Inc. All ri
doi:10.1016/j.ocl.2007.04.003
Diagnosis
Although genetic testing is available, it iscomplex and not highly sensitive. As a result,
MFS remains a clinical diagnosis. According tothe diagnostic (Ghent) criteria, the diagnosis canbe made with the presence of at least one major
criterion in two organ systems and the involve-ment of a third system or one major criterion in anorgan system and the involvement of a second
system when there is a positive family history ofMFS or documentation of a FBN1mutation (Box 1)[5]. Major criteria are named as such because they
are infrequent in other conditions and carry highdiagnostic specificity when present. The differen-tial diagnosis includes homocystinuria, congenitalcontractual arachnodactyly, Stickler syndrome,
Ehlers-Danlos syndrome, MASS (mitral, aortic,skin, and skeletal manifestations) phenotype,Loeys-Dietz syndrome, and Schprintzen-
Goldberg syndrome [6]. Early diagnosis is of theutmost importance to initiate prophylactic b-blockade therapy, which has been shown to be ef-
fective in slowing the rate of aortic dilatation andreducing the development of aortic complicationsin patients who have MFS [7].
Vertebral morphology
The classic ‘‘Marfan spine’’ features may in-
clude increased vertebral scalloping, a higherprevalence of lumbosacral transitional vertebrae,lengthened transverse process distance, and a re-
duction in pedicle width and laminar thickness[8,9]. Mean pedicle widths from L1–L3 weresmaller than the smallest available pedicle screw
(5 mm) in a study of 32 patients who had MFS.In addition, laminar thickness from L1–L5 wassignificantly less in patients who had MFS than
ghts reserved.
orthopedic.theclinics.com

564 DEMETRACOPOULOS & SPONSELLER
Box 1. The Ghent diagnostic criteriafor Marfan syndrome
Skeletal systemMajor criteria: presence of at least four of
the following:Pectus carinatumPectus excavatum requiring surgeryReduced upper to lower segment ratio
or arm span to height ratio>1.05Wrist sign (thumb and fifth digit
overlap circling the wrist) andthumb sign (distal phalanxprotrudes beyond border ofclenched fist)
Reduced extension at the elbows(<170�)
Scoliosis>20�
Pes planusProtrusio acetabuli of any degree
(ascertained on radiographs)Minor criteria
Pectus excavatumJoint hypermobilityHigh arched palateFacial
DolichocephalyMalar hypoplasiaEnophthalmosRetrognathiaDown-slanting palpebral fissures
Ocular systemMajor criterion
Ectopia lentisMinor criteria
Flat corneaIncreased axial length of the globe
(>23.5 mm)
Cardiovascular systemMajor criteria
Dilatation of the ascending aortaDissection of the ascending aorta
Minor criteriaMitral valve prolapse with or without
mitral valve regurgitationDilatation of the main pulmonary
artery in the absence of valvular orperipheral pulmonic stenosis (age<40)
Calcification of the mitral annulusbefore the age of 40 years
in normal controls [9]. Many patients also havesignificant scalloping of the sacrum inside the spi-nal canal (Fig. 1). Therefore, careful preoperativeplanning of fixation anchors, possibly including
CT, may be necessary.
Scoliosis and kyphosis
Because the spine depends upon a balance of
forces during growth, conditions that disrupt themusculoskeletal matrix will cause spinal defor-mity. In a large cross-sectional study, the
Dilatation or dissection of thedescending thoracic or abdominalaorta before the age of 50 years
Pulmonary systemMinor criteria (only)
Spontaneous pneumothoraxApical blebs
Skin and integumentary systemMinor criteria (only)
Striae atrophicaeRecurrent or incisional hernia
Neurologic systemMajor criterion
Lumbosacral dural ectasia by CT orMRI
Family/genetic historyMajor criteria
First-degree relative whoindependently meets the diagnosticcriteria
Presence of mutation in FBN1 genePresence of haplotype around FBN1
inherited by descent andunequivocally associated withdiagnosed MFS in the family
The index case requires major criteria intwo different organ systems andinvolvement of a third. If the FBN-1mutation is present, then one majorcriterion and involvement of a secondorgan system suffices.
A relative of the index case requires onemajor criterion in family history andone major criterion in an organsystem and involvement of a secondorgan system.

565SPINAL DEFORMITIES IN MARFAN SYNDROME
prevalence of scoliosis was 63% in MFS [10];however, many of the curves were minor, andonly 10% to 20% required treatment of any
kind. The curve patterns were similar to thoseseen in idiopathic scoliosis, with the most com-mon types being thoracolumbar and thoracic, al-
though there was a higher rate of triple curves[10]. Differences were seen in the sagittal plane,however (see later discussion). Scoliosis progresses
at a faster rate in MFS than in the general popu-lation in all age groups, with the greatest progres-sion occurring in patients who are 3 years old oryounger (19� � 17� per year) [10]. Virtually all
curves greater than 30� in immature patients reachat least 40� at maturity. Curves greater than 40�
increase during adulthood, at a slightly higher
rate than idiopathic scoliosis. Curves greaterthan 50� progress at a mean rate of 3� � 4� peryear in adulthood [10]. Patients who had MFS
and scoliosis had more back pain than thosewho did not have scoliosis.
Brace treatment does not seem to have as much
success in MFS as in idiopathic scoliosis. One
Fig. 1. Osseous scalloping in MFS.
study reported a 17% success rate for bracingscoliosis curves in MFS. Thus, bracing is recom-mended mainly for growing children with curvesin the range of 15� to 25�. Patients with curves of
25� to 45� may be offered the option of using thebrace; however, patients and physicians should beaware that there is only a one in five chance of
controlling the curve successfully. Bracing is notrecommended for curves greater than 40�, exceptas a temporizing option; the curve will likely
increase [11].Infantile scoliosis is a special challenge to treat
in MFS. Bracing has a limited role, especially in
smaller curves. It is mainly useful in promotingupright posture in patients with a coexistentkyphosis. Also, surgery is especially challengingfor patients younger than 4 years of age. In
addition to typical difficulties encountered whenoperating on the young child for scoliosis, becauseof thin body habitus and a paucity of local,
durable soft tissues, instrumentation is hard tocover in young patients who have MFS. The useof a growing rod using iliac fixation distally and
strong proximal anchorage has been successful inthese cases (Fig. 2). Eventual fusion will benecessary.
Sagittal plane deformities also are common inMFS. The mean kyphosis in the population thathas MFS is greater than in the general population.Forty percent of patients who have MFS have
a kyphosis greater than 50� [10]. Different types ofsagittal alignment were found: hypokyphosis, hy-perkyphosis, and thoracolumbar kyphosis with
compensatory thoracic lordosis [10]. Sponsellerand colleagues [10] proposed a classification
Fig. 2. Infantile scoliosis in MFS. (A) Preoperative anteroposterior (AP) radiograph. (B) Four-year postoperative AP
radiograph. (C) Preoperative lateral radiograph (D) Four-year postoperative lateral radiograph.

566 DEMETRACOPOULOS & SPONSELLER
system for the sagittal deformity associated withMFS (Fig. 3).
Dural ectasia
Dural ectasia (DE), a widening of the dural sacand nerve root sleeves in the caudal portion of thespine, is rare in the normal population but it has
a high prevalence (56% to 92%) in the adultpopulation that has MFS (Fig. 4) [12–14]. The du-ral sac is enlarged mainly below the level of L5
[13–18]. Among 73 patients who were diagnosedwith MFS, Rose and colleagues [19] found DE
Fig. 3. Types of sagittal profiles in patients who have
MFS. (A) In type I sagittal alignment, the transition
zone between the kyphotic and lordotic segments is at
or above L2. Subtype IA corresponds to normal kypho-
sis and lordosis, subtype IB describes thoracic kyphosis
less than 20�, and subtype IC refers to thoracic kyphosis
greater than 50�. (B) In type II sagittal alignment, the
transition zone is caudad to L2. Subtype IIA refers to
a thoracolumbar kyphosis that extends caudad to L2;
subtype IIB indicates a reversal of normal contours
with thoracic lordosis, thoracolumbar kyphosis, and
low lumbar lordosis. (From Sponseller PD, Hobbs W,
Riley LH 3rd, et al. The thoracolumbar spine in Marfan
syndrome. J Bone Joint Surg Am 1995;77(6):868; with
permission.)
to be the second most common major manifesta-tion. DE worsens with age, and a recent studyon a murine model of MFS suggests that DE is
the result of hydrostatic pressure exerted uponan inherently weakened dura [20]. In children,symptoms may be mild or not present at all. Ina prospective patient-control study of patients be-
tween 4 and 18 years of age, Knirsch and col-leagues [21] found MRI evidence suggestive ofDE in up to 40% of children. The consequences
of DE include bony erosion that may lead to an-terior meningocele or posterior meningocele. Clin-ically, patients who have DE may present with
headache, proximal leg pain, leg weakness andnumbness, abdominal pain, and genital and rectalpain [22]. DE also has been associated with mod-erate to severe back pain; however, as many as
41% of patients who have DE have no backpain at all [23]. Sometimes DE is completelyasymptomatic [23–30].
There are several definitions of DE. Fattoriand colleagues [31] used morphologic criteria con-sisting of bulging of the dural sac, lack of epidural
fat at the level of the posterior wall of at least oneposterior vertebral body, and the presence of ra-dicular cysts on MRI to grade the degree of dural
abnormality. Villeirs and colleagues [32] used CTof the spine to establish a quantitative method ofassessing for DE by defining the normal ratioof the transverse diameter of the dural sac to the
Fig. 4. DE in MFS.

567SPINAL DEFORMITIES IN MARFAN SYNDROME
transverse diameter of each lumbar vertebralbody. Oosterhof and colleagues [33] used MRIto calculate dural sac ratios in the anteroposteriorplane; they found that abnormal dural sac ratios
at L3 and S1 could be used to identify MFSwith 95% sensitivity and 98% specificity. Ahnand colleagues [15] suggested that the ‘‘gold stan-
dard’’ for the diagnosis of DE is a dural volumegreater than 7 cm3 when measured caudal to theinferior endplate of L5; however, because tech-
niques to calculate dural volume from recon-structed sacral spine MRIs are not widelyavailable, Ahn and colleagues [15] used MRI
and CT to identify two major criteria and two mi-nor criteria indicative of DE in patients who haveMFS. Major criteria included a sagittal diameterof the spinal canal at S1 or below greater than
the sagittal midaxis of L4 or above and the pres-ence of an anterior meningocele. Minor criteriaincluded scalloping at S1 and an enlarged L5
nerve root sleeve diameter. When at least one ma-jor or two minor criteria were present, DE was di-agnosed with a sensitivity of 87% and a specificity
of 95% using MRI, and a sensitivity of 83% and
a specificity of 90% using CT. In a separate study,Ahn and colleagues [34] examined the effective-ness of conventional radiography to detect DEin patients who had MFS. They determined that
the presence of an interpediculate distance at L4of at least 38.0 mm, a sagittal canal diameter atS1 of at least 18.0 mm, or a scalloping value at
L5 of at least 5.5 mm can detect DE with a speci-ficity of 91.7% and a sensitivity of 57.1%.
Weigang and colleagues [35] and others have
evaluated the efficacy of the MRI and CT criteriaproposed for the diagnosis of DE (Table 1). Wei-gang and colleagues [35] found only two patients
who had MFS who satisfied all criteria for DE us-ing the three methods proposed by Villeirs andcolleagues, Oosterhof and colleagues, and Ahnand colleagues in a group of 18 individuals who
had MFS and 23 individuals who did not haveMFS. Moreover, DE was found in up to 44% ofnormal controls. Because a ‘‘gold standard’’ was
not used, the sensitivity and specificity of eachmethod cannot be calculated from this study;however, it suggests that the various methods
available to assess for DE can produce varying
Table 1
Comparison of four methods for detecting dural ectasia on MRI in individuals who do and do not have Marfan
syndrome
Method Criterion MFS Non-MFS
Oosterhof et al [33] Increased dural sac ratioa at
L3 and S1
94% 44%
Villeirs et al [32] Increased spinal canal
indexb or dural sac indexc18% 0%
Fattori et al [31] Presence of a rectilinear
dural sac, bulging of the
dural sac, lack of epidural
fat at the posterior wall of
vertebral bodies,
radicular cysts, or
anterior sacral
meningocele
92% 0%
Ahn et al [15] Sagittal diameter of the
spinal canal at or below
S1 is greater than the
sagittal diameter at the
midaxis of L4 or above
72% 44%
a Dural sac ratio is the ratio of the anteroposterior (AP) diameter of the dural sac to the AP diameter of the vertebral
body.b Spinal canal index is the sum of the transverse diameters of the spinal canal measured from L1–S1 divided by the
sum of the transverse diameters of the vertebral bodies from L1–L4.c Dural sac index is the sum of the transverse diameters of the dural sac measured from L1–S1 divided by the sum of
the transverse diameters of the vertebral bodies from L1–L4.
Data from Weigang E, Ghanem N, Chang XC, et al. Evaluation of three different measurement methods for dural
ectasia in Marfan syndrome. Clin Radiol 2006;61(11):976.

568 DEMETRACOPOULOS & SPONSELLER
results, which makes the diagnosis of DE chal-lenging. In a similar study, Habermann and col-leagues [36] evaluated the available MRI criteria
for the diagnosis of DE in children and adoles-cents. They determined that abnormal ratios ofthe midsagittal diameter of the vertebral bodiesto the sagittal dural sac diameters at L5 and S1
and a sagittal dural sac width at S1 greater thanat L4 were the only statistically significant criteriafor DE when children and adolescents who had
MFS were compared with normal controls.
Surgical correction of kyphoscoliosis
Spine surgery is required in about 10% to 15%of patients (Fig. 5) [10,37]. A medical specialist
should be involved to comanage cardiac medica-tions and other issues and to assist with anticoa-gulation management if there is an artificial
heart valve. An MRI or CT should be done ofthe area of interest before any spine surgery to vi-sualize the bony and dural structures. Intraopera-tive complications include increased bleeding and
cerebrospinal fluid leak. A recent retrospective re-view of patients who had MFS who underwentsurgical correction for spinal deformity found
that patients who underwent posterior fusion forscoliosis had an average blood loss of 2150 mL,whereas patients who required revision had an av-
erage blood loss of 5300 mL [38]. We have foundaprotinin to be helpful in decreasing blood loss.Cerebrospinal fluid leak occurs because of theDE, and dural tears occurred in 8% of patients
Fig. 5. Severe kyphoscoliosis in a 16-year-old who has MFS. (A) Preoperative clinical appearance. (B) Lateral radio-
graph shows a 95� scoliosis. (C) CT shows bridging of vertebrae. (D) Clinical coronal appearance. (E) Coronal film
showing a 95� kyphosis. The patient underwent apical wedge resections and fusions from a posterior approach. (F) Post-
operative sagittal appearance. Postoperative lateral (G) and coronal (H) radiographs.

569SPINAL DEFORMITIES IN MARFAN SYNDROME
undergoing posterior fusion [38,39]. It can be min-
imized by keeping the patient in a slight Trende-lenburg position intraoperatively and minimizingdissection inside the canal. If a leak occurs,
Fig. 6. Adding-on deformity after correction of scoliosis
in a 12-year old.
closure is possible sometimes; if not, a dural patchand postoperative bed rest for 2 to 3 days havebeen successful. Postoperative complications in-clude failure of fixation, adding on of curvature,
and pseudarthrosis [37,40]. In a review of 39 pa-tients who had MFS and underwent surgical cor-rection, Jones and colleagues [38] reported
a fixation failure rate of 21% and a pseudarthrosisrate of 10%. When correcting spinal deformity, itis important not to fuse too short a segment of
spine (Fig. 6). If patients have dysplastic verte-brae, fusions that need to extend to L4 may bebetter off carried to the sacrum to prevent late
pain and decompensation (Fig. 7). The surgeonprobably should not use selective thoracic fusionfor double major curves unless the lumbar curveis minor. Lipton and colleagues [41] analyzed
data of patients who had MFS and underwentposterior spinal arthrodesis. They compared post-operative curve progression between patients who
had primary and secondary curves fused com-pletely and patients who had complete fusion ofthe primary curve and partial fusion of the sec-
ondary curve. Preoperative curve characteristicswere not compared between groups; therefore, itis unclear whether any differences existed between
the two groups preoperatively. Postoperatively,none of the 7 patients who had both curves fusedprogressed more than 10� at last follow-up; how-ever, 11 of the 16 patients who had partial fusion
of the secondary curve progressed more than 10�
at last follow-up. It also is important to takeinto account any unusual kyphosis that may be
Fig. 7. Fusion in a patient who has MFS with dysplastic vertebrae that was carried to the sacrum to prevent late pain
and decompensation. (A) Preoperative anteroposterior (AP) radiograph. (B) Postoperative AP coned view.

570 DEMETRACOPOULOS & SPONSELLER
present. Failure of fixation is common and is dueto ligamentous laxity that allows hooks to dis-lodge from laminae. In a review of 23 patients
who had MFS and underwent surgery for spinaldeformity, Di Silvestre and colleagues [39] founda distal hook dislodgement rate of 22%. Problemsalso may occur with pedicle screw fixation, with
screws at risk for losing fixation because of thinpedicles. The surgeon should critically assess thefixation and work to achieve a stable proximal
and distal foundation in every patient.
Spondylolisthesis
The prevalence of spondylolisthesis in the
general population is approximately 3%, and, ofthis population, the mean slip is approximately15% [42]. In one study, 6% of the population that
had MFS had spondylolisthesis of the fifth lumbarvertebra or the first sacral vertebra with a meanslip of 30% [10]. It is at this level where DE, sacral
scalloping, and potential cerebrospinal fluid leakshave the greatest clinical importance. Althoughthe frequency of spondylolisthesis in patientswho have MFS may not be markedly higher
than in the general population, if a slip is present,the altered tissue properties allow greater forwardslip to occur. In patients who have MFS and sco-
liosis of at least 10�, mean slip was 60% [10].
Cervical spine
Hobbs and colleagues [43] conducted a radio-
graphic analysis of the cervical spine in patientswho had MFS, which revealed an increased prev-alence of focal kyphosis and a slightly increased
atlantoaxial movement with flexion and exten-sion. Herzka and colleagues [44] reported threecases that suggested that children who have
MFS might be at risk for atlantoaxial rotatorysubluxation when muscle tone is attenuated bygeneral anesthesia or muscle relaxants. Special at-
tention to intubation and positioning, intraopera-tively and postoperatively, may be warranted, androtatory subluxation should be included in the dif-ferential diagnosis for patients who have MFS
and neck pain.
Bone density
Abnormal fibrillin in the population that hasMFS may play a role in bone mineralization.Carter and colleagues [45] demonstrated that
there is a reduced axial bone mineral density(BMD) in men and women who have MFS; theypostulated that this may be due to mutations of
the fibrillin gene or environmental issues, such asreduced exercise that leads to suboptimal peakbone mass. Giampietro and colleagues [46] re-viewed 51 patients who had MFS and found
that the average BMD in the femoral necks ofadult male patients was significantly less than innormal controls; however, average BMD mea-
surements for female and adolescent patientswho had MFS were within normal limits. There-fore, more research may be necessary before im-
plementing widespread BMD evaluations byDual Energy X-Ray Absorptiometry scans.
Screening and athletics
It is recommended that patients who haveMFS avoid physical stress, because many aorticdissections occur during these events [47–49].
Pyeritz and Dietz [47] recommended that the phy-sician counsel patients on an individual basis. Forexample, a child with only a slightly dilated aorticroot does not need outright restriction but should
be counseled away from competitive athletics.Conversely, an older patient with a dilated aorticroot should be advised against any sort of strenu-
ous exertion, especially activities with suddenstops (eg, basketball). Furthermore, reports of in-creased atlantoaxial translation in MFS suggest
they should avoid contact sports, which placehigh-impact loads on the cervical spine. Other ac-tivities, such as low-intensity isokinetic sports,should be encouraged.
Summary
MFS is a disease of connective tissue that
affects multiple organ systems. Skeletal manifes-tations are common at an early age and offerclinicians the opportunity to make a timely di-agnosis. Thus, the surgeon examining the spine
must be aware of the manifestations of MFS andbe able to recognize affected individuals. Spinaldeformities are frequent, progress with age, and
are less responsive to conservative treatment.Surgical management presents unique intraoper-ative and postoperative challenges because com-
plication and revision rates are greater in patientswho have MFS; however, with attention to detail,excellent results are possible.

571SPINAL DEFORMITIES IN MARFAN SYNDROME
References
[1] Dietz HC, Pyeritz RE.Mutations in the human gene
for fibrillin-1 (FBN1) in the Marfan syndrome and
related disorders. Hum Mol Genet 1995;4 Spec
No:1799–809.
[2] Tsipouras P, Del Mastro R, Sarfarazi M, et al. Ge-
netic linkage of theMarfan syndrome, ectopia lentis,
and congenital contractural arachnodactyly to the
fibrillin genes on chromosomes 15 and 5. The Inter-
national Marfan Syndrome Collaborative Study.
N Engl J Med 1992;326(14):905–9.
[3] Giampietro PF, Raggio C, Davis JG. Marfan syn-
drome: orthopedic and genetic review. Curr Opin
Pediatr 2002;14(1):35–41.
[4] Judge DP, Dietz HC. Marfan’s syndrome. Lancet
2005;366(9501):1965–76.
[5] De Paepe A, Devereux RB, Dietz HC, et al. Revised
diagnostic criteria for the Marfan syndrome. Am J
Med Genet 1996;62(4):417–26.
[6] Beighton P, de Paepe A, Danks D, et al. Interna-
tional nosology of heritable disorders of connective
tissue, Berlin, 1986. Am J Med Genet 1988;29(3):
581–94.
[7] Shores J, Berger KR,Murphy EA, et al. Progression
of aortic dilatation and the benefit of long-term beta-
adrenergic blockade inMarfan’s syndrome.NEngl J
Med 1994;330(19):1335–41.
[8] Tallroth K, Malmivaara A, Laitinen ML, et al.
Lumbar spine in Marfan syndrome. Skeletal Radiol
1995;24(5):337–40.
[9] Sponseller PD, Ahn NU, Ahn UM, et al. Osseous
anatomy of the lumbosacral spine in Marfan syn-
drome. Spine 2000;25(21):2797–802.
[10] Sponseller PD, Hobbs W, Riley LH 3rd, et al. The
thoracolumbar spine in Marfan syndrome. J Bone
Joint Surg Am 1995;77(6):867–76.
[11] Sponseller PD, BhimaniM, SolacoffD, et al. Results
of brace treatment of scoliosis in Marfan syndrome.
Spine 2000;25(18):2350–4.
[12] Pyeritz RE, Fishman EK, Bernhardt BA, et al.
Dural ectasia: a common pleiotropic feature of the
Marfan’s syndrome. Am J Hum Genet 1986;39S:
A75.
[13] Fishman EK, Zinreich SJ, Kumar AJ, et al. Sacral
abnormalities inMarfan syndrome. J ComputAssist
Tomogr 1983;7(5):851–6.
[14] Pyeritz RE, Fishman EK, Bernhardt BA, et al.
Dural ectasia is a common feature of the Marfan
syndrome. Am J Hum Genet 1988;43(5):726–32.
[15] AhnNU, Sponseller PD, AhnUM, et al. Dural ecta-
sia in the Marfan syndrome: MR and CT findings
and criteria. Genet Med 2000;2(3):173–9.
[16] Robinson L, Dominguez R, Cabrera J, et al. Multi-
ple meningeal cysts inMarfan syndrome. AJNRAm
J Neuroradiol 1989;10(6):1275–6.
[17] Savini R, Cervellati S, Beroaldo E. Spinal defor-
mities inMarfan’s syndrome. Ital J Orthop Trauma-
tol 1980;6(1):19–40.
[18] Strand RD, Eisenberg HM. Anterior sacral menin-
gocele in association withMarfan’s syndrome. Radi-
ology 1971;99(3):653–4.
[19] Rose PS, Levy HP, Ahn NU, et al. A comparison of
the Berlin and Ghent nosologies and the influence of
dural ectasia in the diagnosis of Marfan syndrome.
Genet Med 2000;2(5):278–82.
[20] Jones KB, Myers L, Judge DP, et al. Toward an un-
derstanding of dural ectasia: a light microscopy
study in a murine model of Marfan syndrome. Spine
2005;30(3):291–3.
[21] Knirsch W, Kurtz C, Haffner N, et al. Dural ectasia
in children with Marfan syndrome: a prospective,
multicenter, patient-control study. Am JMed Genet
A 2006;140(7):775–81.
[22] Foran JR, Pyeritz RE,DietzHC, et al. Characteriza-
tion of the symptoms associated with dural ectasia in
theMarfan patient. Am JMedGenet A 2005;134(1):
58–65.
[23] AhnNU, Sponseller PD, AhnUM, et al. Dural ecta-
sia is associated with back pain inMarfan syndrome.
Spine 2000;25(12):1562–8.
[24] Duncan RW, Esses S. Marfan syndrome with back
pain secondary to pedicular attenuation. A case re-
port. Spine 1995;20(10):1197–8.
[25] Ho NC, Hadley DW, Jain PK, et al. Case 47: dural
ectasia associated with Marfan syndrome. Radiol-
ogy 2002;223(3):767–71.
[26] Nallamshetty L, Ahn NU, Ahn UM, et al. Dural
ectasia and back pain: review of the literature and
case report. J Spinal Disord Tech 2002;15(4):326–9.
[27] Raftopoulos C, Delecluse F, Braude P, et al. Ante-
rior sacral meningocele and Marfan syndrome: a re-
view. Acta Chir Belg 1993;93(1):1–7.
[28] SmithMD. Large sacral dural defect in Marfan syn-
drome. A case report. J Bone Joint Surg Am 1993;
75(7):1067–70.
[29] Sonier CB, Buhe T, Despins P, et al. Sacral pseudo-
meningocele andMarfan’s disease. One case. J Neu-
roradiol 1993;20(4):292–6.
[30] Stern WE. Dural ectasia and the Marfan syndrome.
J Neurosurg 1988;69(2):221–7.
[31] Fattori R, Nienaber CA, Descovich B, et al. Impor-
tance of dural ectasia in phenotypic assessment of
Marfan’s syndrome. Lancet 1999;354(9182):910–3.
[32] Villeirs GM, Van Tongerloo AJ, Verstraete KL,
et al. Widening of the spinal canal and dural ectasia
in Marfan’s syndrome: assessment by CT. Neurora-
diology 1999;41(11):850–4.
[33] Oosterhof T, Groenink M, Hulsmans FJ, et al.
Quantitative assessment of dural ectasia as a marker
for Marfan syndrome. Radiology 2001;220(2):
514–8.
[34] Ahn NU, Nallamshetty L, Ahn UM, et al. Dural
ectasia and conventional radiography in the Marfan
lumbosacral spine. Skeletal Radiol 2001;30(6):
338–45.
[35] WeigangE,GhanemN,ChangXC, et al. Evaluation
of three different measurement methods for dural

572 DEMETRACOPOULOS & SPONSELLER
ectasia in Marfan syndrome. Clin Radiol 2006;
61(11):971–8.
[36] HabermannCR,Weiss F, Schoder V, et al.MR eval-
uation of dural ectasia in Marfan syndrome: reas-
sessment of the established criteria in children,
adolescents, and young adults. Radiology 2005;
234(2):535–41.
[37] Robins PR, Moe JH, Winter RB. Scoliosis in Mar-
fan’s syndrome. Its characteristics and results of
treatment in thirty-five patients. J Bone Joint Surg
Am 1975;57(3):358–68.
[38] Jones KB, Erkula G, Sponseller PD, et al. Spine de-
formity correction inMarfan syndrome. Spine 2002;
27(18):2003–12.
[39] Di SilvestreM,Greggi T,Giacomini S, et al. Surgical
treatment for scoliosis in Marfan syndrome. Spine
2005;30(20):E597–604.
[40] Birch JG, Herring JA. Spinal deformity in Marfan
syndrome. J Pediatr Orthop 1987;7(5):546–52.
[41] Lipton GE, Guille JT, Kumar SJ. Surgical treat-
ment of scoliosis in Marfan syndrome: guidelines
for a successful outcome. J Pediatr Orthop 2002;
22(3):302–7.
[42] Fredrickson BE, Baker D, McHolick WJ, et al. The
natural history of spondylolysis and spondylolisthe-
sis. J Bone Joint Surg Am 1984;66(5):699–707.
[43] HobbsWR, Sponseller PD,Weiss AP, et al. The cer-
vical spine in Marfan syndrome. Spine 1997;22(9):
983–9.
[44] Herzka A, Sponseller PD, Pyeritz RE. Atlantoaxial
rotatory subluxation in patients with Marfan syn-
drome. A report of three cases. Spine 2000;25(4):
524–6.
[45] Carter N, Duncan E, Wordsworth P. Bone mineral
density in adults with Marfan syndrome. Rheuma-
tology (Oxford) 2000;39(3):307–9.
[46] Giampietro PF, Peterson M, Schneider R, et al. As-
sessment of bone mineral density in adults and chil-
dren with Marfan syndrome. Osteoporos Int 2003;
14(7):559–63.
[47] Pyeritz RE, Dietz HC. Marfan syndrome and
other microfibrillar disorders. In: Royce PM,
Steinmann B, editors. Connective tissue and its her-
itable disorders: molecular, genetic, and medical as-
pects. 2nd edition. New York: Wiley-Liss; 2002.
[48] Bain MA, Zumwalt RE, van der Bel-Kahn J. Mar-
fan syndrome presenting as aortic rupture in a young
athlete: sudden unexpected death? Am J Forensic
Med Pathol 1987;8(4):334–7.
[49] Maron BJ, Epstein SE, Roberts WC. Causes of sud-
den death in competitive athletes. J Am Coll Cardiol
1986;7(1):204–14.