Oesophageal Atresia and Its Management
-
Upload
rajan-kumar -
Category
Documents
-
view
326 -
download
1
Transcript of Oesophageal Atresia and Its Management

SEMINARSEMINAR“OESOPHAGEAL ATRESIA AND ITS
MANAGEMENT ”
PRESENTED BY :MAHENDRA SINGH GOND
MODERATOR :Dr. DEEPTI BALA SHARMA

DEFINITIONEosophageal atresia is a congenital
interruption or discontinuity of the eosophagus resulting in eosophageal obstruction.

IntroductionIntroduction Eosophageal atresia is the most frequent
congenital anomaly of the eosophagus affecting about 1 in 4000 neonate of these more than 90% have an associated tracheo esophageal fistula.
The surgical solution to the problem of esophageal atresia referred as epitome of modern surgery certainly its evaluation is an example of incremental steps. Surgical inguinity and sheer persistence can eventually lead to remarkable success.
A congenital abnormality incompatible with life that was once referred to as hopeless from beginning and not of much practical importance to the surgeon is now successfully repair all over the world.

ETIOLOGY :Embryology of these anomalies is still debatable.
21-32 day of embryogenesis
elongation and growth separation of trachea branching and
from foregut growth of
bronchial tree
rapid elongation of trachea
and dimnition in esophagus
substance
oeiophageal atresia

Incidence:
Genetic contribution is relatively non specific.
Esophageal atresia has been noted in 1 of a set of twins by many observer.
Holder Survey
Atresia distal fistula (85%)
Atresia, proximal fistula (2%)
Atresia, fistula both segment (1%)
Atresia alone (6%)
Fistula alone (2%)
0 20 40 60 80 100

TYPES
A=Atresia without fistula – 6%
B=Atresia with fistula into proximal segment – 2%
C=Atresia with fistula into distal segment –85%
D=Atresia with fistula into both segment –1%
E=Fistula without atresia –2%

ANATOMY
1. In the common type of atresia with fistula into the distal segment the proximal pouch varies in length from 1-3.5 cm. This would result in pemaxilla of 10-13.5 cm. The diameter range from normal of about 5-10 mm or more.

2. The proximal pouch is usually hypertrophied due to process of foetal swallowing of amniotic fluid. It has an excellent blood supply and adherent to posterolateral wall of trachea. If the proximal pouch is not hypertrophic and is small and short, then there is possible existence of a fistula between it and trachea.

3. In atresia with distal fistula lower segment usually membranous part of trachea just cephalad of the carina within 1 cm but rarely be into right or left main bronchus.
Distal segment supplied by intercostal artery and branches from descending aorta.

MOST COMMON CONGENITAL ANOMALY ASSOCIATED WITH ESOPHAGEAL ATRESIA WITH OR WITHOUT FISTULA:
V- VERTEBRAL BODY SEGMENTATION DEFECT - 30%
A- ANORECTAL MALFORMATION – 20.5%
C- CARDIAC VASCULAR ANOMALY – 27.6% (VSD >PDA > TOF)
T- TRACHEO
E- ESOPHAGEAL
R- RADIAL, RENAL AGENESIS – 11.1%
L- LIMB ABNORMALITY – 2%
CHROMOSOMAL ABNORMALITY – 5-8%
(DOWN, EDWARD SYNDROME)
C- COLOBOMATA
H- HEART DISEASE
A- CHONAL ATRESIA
R- MENTAL RETARDATION
G- GENITAL HYPOPLASIA
E- EAR ANOMALY WITH DEAFNESS

DIAGNOSIS
Clinical feature:
- H/o maternal polyhydromnias
- First symptom noted immediately or soon after the birth is excessive saliva from mouth which require frequent aspiration (drooling of saliva)
- Episodes of chocking, coughing, regurgitation, respiration distress and even cynosis on feeding attempt
- Gastric distention is found with distal fistula
Associated with other anomaly like imperforated anus radial dysplasia

RADIOLOGICAL STUDY
Pass 10 or 12 french radiopaque catheter through oral or nostril route take X-ray in erect posture in PA and lateral view.
1. Coiling of catheter (obstruction will be met 9-13 cm from naros) i.e., oesophageal atresia
2. Coiling of catheter with air in stomach i.e., esophageal atresia with distal esophageal fistula
3. Coiling of catheter with no gas in stomach i.e., oesophageal atresia without fistula
Advantage :
1. To confirm the location of catheter and extent of proximal pouch, from lateral film the level of the blind end of pouch, relative to thoracic inlet. Lowest point of pouch usually reaches to level of body of T2 - T3 vertebrae.
2. Determine severity of pulmonary involvement aortic arch location
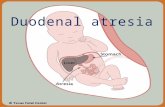
3. Exclude other concominent anamalies like duodenal atresia (double bubble sign), anorectal malformation

RADIOPAQUE DYE STUDY
Instillation of radiopaque dye (gastrograffin, micropaque dinosil) through catheter for further radiological study.
Advantage:
Precise size location of proximal pouch is accurately visualize and proximal fistula may be seen.
Disadvantage:
Dye aspirated into airway causing chemical pnemonitis.

TRACHEOBRONCHOSCOPY
Visualize the exact location of fistulous opening in the wall of the trachea but also access anatomy of air passage and to rule out second fistula.
Preoperative bronchoscopy is helpful when preliminary radiograph indicate short high proximal pouch
Endoscopy : Particular value in diagnosis of H type fistula which within spectrum of tracheoesophageal defect being consider difficult to diagnosis.
USG : Abdomen (to rule out congenital anomaly like renal agenosis, duodenal atresia, pyloric stenosis, anorectal malformation
Echocardiography : To rule out cardiac anomaly like (R) side aortic arch TOF, VSD, PDA.

SUSPECTED OA
(Prematurity and maternal polyhydromino) excessive mucousy at birth drooling) mild to moderate respiratory distress
Insert No. 10 gauze catheter through mouth become arrested at 9-13 cm from gum
Plain X-ray chest/abdomen
1. Gas in abdomen on plain x-ray 2. no gas in abdomen
Distal tracheoesophageal no distal fistula
Fistula (20% have proximal fistula)
Endoscopy or mild oesophageal contrast
study
Demonstrate proximal tracheo-
Oesophageal fistula if present
Fistula division and esophageal anastomosis

MANAGEMENTMedical care before and during transport.
1. Oxygen therapy
2. Care of upper pouch – proper suction of upper pouch
3. Posture – infant nursed in right lat position to assist the infant in maintaining a clear airway. This will minimise regurgitation of gastric contact upto the distal fistula and decrease work of breathing and improve oxygenation.
The neonate depends almost entirely on contraction of the diaphragm for effective ventilation which is more easily accomplished in this position.
4. I/M injection vitamin K
5. I/V Fluid, I/V antibiotic

SURGICAL TREATMENT
Following criteria to be useful in making the decision for primary repair.
1. Clear lung to ausculate
2. Clear lung by chest radiograph
3. No undefined cardiac anomalies
4. An arterial PaO2 of greater than 60 mmHg in
room air
5. A recent study identified LBW (1500 gm) and the presence of major cardiac anomaly as two factors that are greater influence on
survival

WARTERSTON CLASSIFICATIONGroup I = BW > 1500 gm without major cardiac disease
Group II = BW < 1500 gm or major cardiac disease
Group III = BW < 1500 gm and major cardiac disease
Using there criteria then survival rate for :
I = 97%
II = 59%
III = 22%

PROCEDUREThe aim of primary repair of both end is tension free anastomosis
without compromising the blood supply.
Right side extrapleural thoractomy through fourth intercostal space
Lung retracted medially by retractor
Azygous vein identying ligate and divide
TEF dissected circumterentially and then ligated using interrupted non absorbable suture
Proximal esophageal pouch is then mobilized as high as possible to afford a tension free esophageal anastomosis
Anastomosis perform using single or double layer


If the two end of esophagus cannot anastomoses without tension there are several options.
(1) Suture the divided end of distal esophagus to the prevertebral fascia mark its location with metal clip close the thoractomy. Over 2-3 months the proximal esophagous will anastomosis with adequate length.
(2) Circular or spiral myotomy of upper pouch. Done to gain esophageal length. Each myotomy add up 1 cm of length
Disadvantage : Formation of diverticulum

(3) Sump tube maintain in proximal pouch and with time the proximal blind segment elongates into mediastinum 6-12 weeks

(4) If the all maneour failed : cervical esophagostomy with gastrostomy will done.
(5) esophageal replacement using the stomach (greater curvature tube, gastric transposition), small intestine (jejunal transposition), colon (eosophagocoloplasty) performed at about 1 year of age or 10 kg weight.

COMPLICATION a. Dysphagia/stricture –
M/M – 1. Retrograde dilation guided by transanastomotic string approach.
1. Radial dilation with balloon catheters.
2. If stenosis with complete occlusion – double endoscopy preferred.
3. Esophageal replacement1. (transposition of gastric tube small intestine, colon)
b. Major Anastomotic Leak
Complete disruption - do reanastomosis
Complete disruption with infection – Cervical esophagotomy with esophageal replacement
c. Recurrent Tracheosophageal fistula
1. Pleural or pericardial flap and interposition of muscle all have been used to prevent another recurrence.
2. Endoscopy plugging with fibrin glue
d. Chylothorax
e. Gastroesophageal reflex – partial wrap fundoplication

CONCLUSION:Survival has become the norm with
good result of eosophageal anastomosis with fistula excision with undefined congenital anomaly.