NPUAP-EPUAP Pressure Ulcer Prevention & Treatment Guidelines
Transcript of NPUAP-EPUAP Pressure Ulcer Prevention & Treatment Guidelines

NPUAPNPUAP--EPUAP Pressure Ulcer EPUAP Pressure Ulcer Prevention & Treatment GuidelinesPrevention & Treatment Guidelines
Janet Cuddigan, PhD, RN, CWCNAssociate Professor & Department Chair
University of Nebraska Medical CenterOmaha, NE USA
Editor-in-Chief, EPUAP-NPUAP Guideline
[[ [[

©NPUAP & EPUAP, 2009 2
Walk Through the Treatment Walk Through the Treatment Guidelines with Us!Guidelines with Us!
2

Treatment TopicsTreatment Topics
•
Classification•
Assessment & Monitoring Healing
•
Nutrition for Healing•
Pain Assessment & Management
•
Support Surfaces•
Cleansing
•
Debridement•
Dressings
•
Assessment & Treatment of Infection….
©NPUAP & EPUAP, 2009 3

Treatment TopicsTreatment Topics
•
Biophysical Agents•
Biological Dressings
•
Growth Factors•
Surgery for Pressure Ulcers
•
Pressure Ulcer Management in Individuals Receiving Palliative Care
©NPUAP & EPUAP, 2009 4

Treatment TopicsTreatment Topics
©NPUAP & EPUAP, 2009 5

©NPUAP & EPUAP, 2009 6
Classification of Pressure UlcersClassification of Pressure Ulcers
•
New Components–
Use validated system
•
NPUAP Staging & EPUAP Grading•
NPUAP-EPUAP International System
–
Educate professionals (B)–
Confirm inter-rater reliability (B)
–
Do not classify pressure ulcers on mucous membranes
6

©NPUAP & EPUAP, 2009
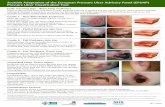
Educate professionals about special assessment Educate professionals about special assessment techniques in individuals with darkly pigmented skin. techniques in individuals with darkly pigmented skin. (B)(B)
1.
Skin Intact: Stage I and suspected deep tissue injury may be difficult to detect with visual inspection alone. Assess differences in skin temperature, skin color, tissue consistency (i.e. boggy or firm) and pain between affected areas and normal tissue.
2.
Skin Open: Inflammatory redness of the surrounding skin may be difficult to detect in Stage II through IV pressure ulcers. Assess for heat, tenderness, pain or change in tissue consistency to identify the extent of inflammation and possible cellulitis and/or undermining.
•
Baumgarten M, Margolis D, van Doorn C, Gruber-Baldini AL, Hebel JR, Zimmerman S, et al. Black/White differences in pressure ulcer incidence in nursing home residents. J Am Geriatr Soc. 2004 Aug;52(8):1293-8
77

©NPUAP & EPUAP, 2009
Stage/Category II Stage/Category II --
IVIV
88

©NPUAP & EPUAP, 2009
NPUAPNPUAP--EPUAP International EPUAP International Classification SystemClassification System©©
•
We agree on:–
Definition of pressure ulcers
–
Definition of four “stages, grades, or categories”
–
Additional categories for USA•
Suspected Deep Tissue Injury
•
The “Unstageables”–
Stage? Grade? Category?
99

©NPUAP & EPUAP, 2009
I: NonI: Non--blanchable erythema of intact blanchable erythema of intact skinskin
Intact skin with non- blanchable erythema
of a localized area usually over a bony prominence. Discoloration of the skin, warmth, edema, hardness or pain may also be present. Darkly pigmented skin may not have visible blanching.
1010

©NPUAP & EPUAP, 2009
II: Partial thickness skin loss or II: Partial thickness skin loss or blister blister
•
Partial thickness loss of dermis presenting as a shallow open ulcer with a red pink wound bed, without slough. May also present as an intact or open/ruptured serum or sero-sanguinous-filled blister.
1111

©NPUAP & EPUAP, 2009
III: Full thickness skin lossIII: Full thickness skin loss
•
Full thickness skin loss. Subcutaneous fat may be visible but bone, tendon or muscle are not
exposed. Some slough may be present. May
include undermining and tunneling.
1212

©NPUAP & EPUAP, 2009
IV: Full thickness tissue lossIV: Full thickness tissue loss
•
Full thickness tissue loss with exposed bone, tendon or muscle. Slough or eschar may be present. Often
includes undermining and tunneling.
1313

©NPUAP & EPUAP, 2009
Full thickness skin or tissue loss Full thickness skin or tissue loss –– Depth unknownDepth unknown•
Full thickness tissue loss in which actual
depth of the ulcer is completely
obscured
by slough (yellow, tan, gray, green or brown) and/or eschar (tan, brown or black) in the wound bed.
1414

©NPUAP & EPUAP, 2009
Suspected deep tissue injury Suspected deep tissue injury –– depth unknowndepth unknown
•
Purple or maroon localized area of discolored intact skin or blood-filled blister due to damage of underlying soft tissue from pressure and/or shear.
1515

©NPUAP & EPUAP, 2009 16
Assessment & Monitoring Healing Assessment & Monitoring Healing
•
New Components–
Holistic patient assessment
–
Pressure ulcer assessment (at least weekly)–
How to measure (B)
–
Expect some signs of healing in 2 weeks (B)–
Assessment findings should guide treatment
–
Changing assessment → changing treatment–
Assess progress toward healing with a validated tool (B)
•
Bates-Jensen Wound Assessment Tool (BWAT)•
Pressure Ulcer Scale for Healing (PUSH)
16

©NPUAP & EPUAP, 2009 17
Nutrition for Pressure Ulcer Healing Nutrition for Pressure Ulcer Healing
•
Most patients with PU suffer from undernutrition
•
Nutritional requirements usually increase to support PU healing.
•
Assess nutritional status–
Mini-Nutritional Assessment (MNA) validated & easy to use in multi-morbid geriatric patients.
–
MUST (Malnutrition Universal Screening Tool) –
to ID risk of undernutrition
–
Child: assess weight, height, head circumference, body mass index, skin fold plot, compare to age
–
Miffin-St Jeor equation for bariatric patients17

©NPUAP & EPUAP, 2009 18
Nutrition for Pressure Ulcer HealingNutrition for Pressure Ulcer Healing
•
Provide sufficient nutrients & fluids. –
Kilocalories (B)
(30-
35 kcal/kg/day)
–
Protein to promote anabolism (B)
(1.25 –
1.5 gm/kg/day). Assess renal function
–
Vitamins & minerals with balanced diet; supplements with deficiencies. (B)
–
Enhanced foods or oral supplements (B)–
Fluids. Assess for dehydration.
(Hartgrink, et. al, 1998; Lee, et al, 2006; Langenkamp-Henken, et al, 2000; Langer, et al, 2003)
18

©NPUAP & EPUAP, 2009 19
Pain Assessment & ManagementPain Assessment & Management
•
Minimal evidence for management of PrU pain
•
Individuals with a PrU experience pain; individuals with a Stage IV PrU experience greater pain than those with ↓stage PrU
•
Only 2% of patients in 1 study who reported PrU pain had received timely analgesia after c/o pain (Dallam et al., 1995)
19

Pain Assessment & ManagementPain Assessment & Management
•
Assess for pain•
Prevent pain
•
Manage general pain•
Reduce debridement pain
•
Manage chronic pain•
Educate Individuals, Family and Professionals
©NPUAP & EPUAP, 2009 20

©NPUAP & EPUAP, 2009 21
Prevent PainPrevent Pain
-
Avoid postures that increase pressure, such as Fowlers >30°
or
90°
side lying position, or the semi- recumbent position.
-Use dressings less likely to cause pain (HD, HDG, hydrofiber, alginates, foam, polymeric foam, soft silicone, ibuprofen-
impregnated [not available everywhere]).
21

©NPUAP & EPUAP, 2009 22
Local Treatment of Pain Local Treatment of Pain
•
Consider topical opioids (diamorphine or benzydamine 3%) to reduce or eliminate PU pain. (B)–
Topical anesthetics act on opioid receptors in peripheral nerves that are activated during inflammation
–
Morphine or Diamorphine gel, foam dressing with ibuprofen [not available everywhere]
(Flock, et al, 2003; Twillman, et al, 1999; Gottrup, et al, 2007)
22

©NPUAP & EPUAP, 2009 23
Chronic PainChronic Pain
-
For chronic pain, follow the World Health Organization Dosing Ladder-
Refer the individual with chronic
pain related to PU to the appropriate pain and/or wound clinic resources.
23

©NPUAP & EPUAP, 2009 24
Support Surfaces for Treatment of Support Surfaces for Treatment of Pressure Ulcers Pressure Ulcers
•
New Components–
S3I Terms & Definitions
–
Pressure Redistribution–
Growing Appreciation of Microclimate
•
Local tissue temperature & moisture at body- support surface interface.
–
Need for Standards: ISO Initiative–
Need to match patient needs to support surface features
24

©NPUAP & EPUAP, 2009 25
Support Surfaces for Treatment of Support Surfaces for Treatment of Pressure UlcersPressure Ulcers•
Replace the existing support surface with one that provides better pressure redistribution if the individual–
can’t be turned off the ulcer,
–
has PU on 2 or > surfaces, –
fails to heal or shows deterioration, I
–
is at hi risk for additional PU, or –
bottoms out on existing surface.
The term, “upgraded support surface”
is used throughout this document to prompt the professional to consider replacing the existing support surface
only one of several strategies. The individual and pressure ulcer should be re-evaluated. Preventive interventions and local wound care should
also b
25

©NPUAP & EPUAP, 2009 26
Support Surfaces for Treatment of Support Surfaces for Treatment of Pressure Ulcers Pressure Ulcers
•
When pressure ulcers deteriorate or fail to heal, changing the support surface is only one of several strategies. The individual and pressure ulcer should be re-evaluated. Preventive interventions and local wound care should also be changed as needed.
The term, “upgraded support surface”
is used throughout this document to prompt the professional to consider replacing the existing support surface
only one of several strategies. The individual and pressure ulcer should be re-evaluated. Preventive interventions and local wound care should
also b
26

©NPUAP & EPUAP, 2009 27
Support Surfaces for Treatment of Support Surfaces for Treatment of Pressure Ulcers Pressure Ulcers
•
General recommendations–
Support surfaces
–
Positioning•
Support surfaces for:
•
Stage I & II (bed & chair)•
Stage I & II of heels
•
Deep tissue injury•
Stage III, IV & unstageable (bed & chair, heels)
The term, “upgraded support surface”
is used throughout this document to prompt the professional to consider replacing the existing support surface
only one of several strategies. The individual and pressure ulcer should be re-evaluated. Preventive interventions and local wound care should
also b
27

©NPUAP & EPUAP, 2009 28
Support Surfaces for Treatment of Support Surfaces for Treatment of Pressure Ulcers Pressure Ulcers
•
Special Populations–
Critically ill •
Hemodynamic instability
–
Spinal cord injury–
Bariatric •
Fit individual to bed at admission
The term, “upgraded support surface”
is used throughout this document to prompt the professional to consider replacing the existing support surface
only one of several strategies. The individual and pressure ulcer should be re-evaluated. Preventive interventions and local wound care should
also b
28

©NPUAP & EPUAP, 2009 29
Wound Bed Preparation and Wound Bed Preparation and Biofilms Biofilms
•
Guiding Principles of Wound Bed Preparation–
Tissue
–
Infection/ inflammation–
Moisture
–
Epithelium/edges
Schultz GS, Sibbald RG, Falanga V, Ayello EA, Dowsett C, Harding
K, Romanelli M, Stacey MC, Teot L, Vanscheidt W. Wound bed preparation: a systematic approach to wound management. Wound Repair Regen 11 Suppl 1:S1-S28, 2003
29

©NPUAP & EPUAP, 2009
Cultures & BiofilmsCultures & Biofilms
•
Do standard specimen processing procedures detect biofilms and the organisms encased in biofilms?
•
How do we remove biofilms?•
Once removed, how to we prevent biofilms from re-forming?
30

©NPUAP & EPUAP, 2009
Five stages of biofilm development in Five stages of biofilm development in Pseudomonas aeruginosaPseudomonas aeruginosa. In Stage 1, bacterial cells attach reversibly to the . In Stage 1, bacterial cells attach reversibly to the surface. At Stage 2, the cells attach irreversibly, mediated bysurface. At Stage 2, the cells attach irreversibly, mediated by
exopolymeric substances, and loose flagellaexopolymeric substances, and loose flagella--driven driven motility. In Stage 3, the first biofilm architecture occurs, fomotility. In Stage 3, the first biofilm architecture occurs, forming microcolonies, while in Stage 4 the fully mature rming microcolonies, while in Stage 4 the fully mature biofilm architecture is achieved. In Stage 5, dispersion of sinbiofilm architecture is achieved. In Stage 5, dispersion of single motile cells occurs from the mature biofilm, which gle motile cells occurs from the mature biofilm, which ‘‘seedseed’’
other surfaces, reother surfaces, re--initiating the process. initiating the process. Graphic and photos by Peg Dirckx, David Davies and Karin Sauer Graphic and photos by Peg Dirckx, David Davies and Karin Sauer
How Do Bacterial Biofilms Form?How Do Bacterial Biofilms Form?
revers
ible a
ttach
ment
revers
ible a
ttach
ment
irrev
ersibl
e atta
chmen
t
irrev
ersibl
e atta
chmen
t
microc
olonie
s
microc
olonie
s mature
biofil
m
mature
biofil
m
polym
icrob
ial bi
ofilm
polym
icrob
ial bi
ofilm
31

©NPUAP & EPUAP, 2009 32
Cleansing Cleansing
•
New Components–
Cleanse pressure ulcer & surrounding skin (B)
–
Normal saline or potable water–
Consider solutions with surfactants and antimicrobials with
•
Debris•
Confirmed or Suspected Infection
•
High levels of bacterial contamination–
Konya, et al. 2005
32

©NPUAP & EPUAP, 2009 33
Debridement Debridement
•
Debride devitalized tissue when appropriate to individuals condition and goals–
Appropriate method
–
Choice of methods, but surgical for spreading infection–
Manage pain
–
Vascular assessment–
Stable heel ulcers
•
Maintenance debridement until wound bed is covered with granulation tissue and devoid of necrotic.
•
Pain management related to debridement
33

©NPUAP & EPUAP, 200911th National NPUAP Biennial Conference •
February 27–28, 2009 34
Dressings Dressings
•
Ulcer should be assessed at every dressing change & the appropriateness of the current dressing regimen should be confirmed.
•
Evidence was summarized for the following dressing types:–
Hydrocolloid (B)
–
Transparent film–
Hydrogel (B)
–
Alginate (B)–
Foam (B)
–
Polymeric membrane dressings (B)–
Impregnated dressings (silver, honey, cadexomer iodine) (B)
–
Gauze dressings–
Silicone coated dressings (B)
–
Collagen dressings–
Composite dressings
34

©NPUAP & EPUAP, 2009 35
Dressing Highlights Dressing Highlights
Protection from Friction & Shear•
Consider using dressings to protect body areas at risk for friction injury or risk of injury from tape.
•
Consider placing foam dressings on body areas & PUs at risk for shear injury.
Reduction of Bioburden•
Consider using silver dressings in infected or heavily colonized ulcers (B) (Munter, et al, 2006)
–
may be toxic to keratinocytes & fibroblasts–
Silver resistant strains of bacteria may be emerging–
Avoid prolonged use; discontinue when infection controlled•
Consider medical grade honey for II & III (Gunes & Esser, 2007)
•
Consider cadexomer iodine dressings in moderately to heavily exudating wounds (Moberg, et al., 1983)
35

©NPUAP & EPUAP, 200911th National NPUAP Biennial Conference •
February 27–28, 2009 36
Dressings Dressings --
HighlightsHighlights
•
When other forms of moisture retentive dressings are not available, continually moist gauze is preferable to dry gauze.
•
Consider silicone dressings to promote atraumatic dressing changes, especially when tissue is friable. (Meamue, 2003)
•
Consider collagen matrix dressings for non healing full thickness PrUs.
36

©NPUAP & EPUAP, 2009 37
Assessment & Treatment of Assessment & Treatment of Infection Infection
•
Infected ulcers don’t heal!•
Have a high index of suspicion for likelihood of infection if:
–
Ulcer
has necrotic tissue or foreign body; large and deep; long duration; frequently contaminated
–
Individual
has undernutrition, diabetes mellitus, hypoxemia, poor tissue perfusion, autoimmune disease or immunosuppression
37

©NPUAP & EPUAP, 20091 38
Assessment & Treatment of Assessment & Treatment of Infection Infection
Have a high index of suspicion for local infection in pressure ulcers when there are no signs of healing for 2 weeks, friable granulation tissue, foul odor, increased pain in the ulcer, increased heat in the tissue around the ulcer, increased drainage from the wound, an ominous change in the nature of the wound drainage (e.g., new onset of bloody drainage, purulent drainage), increased necrotic tissue in the wound bed, pocketing or bridging. (Strength of Evidence = B.)
Cutting KF, Harding KG. Criteria for identifying wound infection. J Wound Care. 1994;3(4):198-201.
Gardner SE, Frantz RA, Doebbeling BN. The validity of the clinical signs and symptoms used to identify localized chronic wound infection. Wound Repair Regen. 2001;9(3):178-86.
38

©NPUAP & EPUAP, 2009
How do we assess wound How do we assess wound infection?infection?
39

©NPUAP & EPUAP, 2009 40
Assessment & Treatment of Assessment & Treatment of Infection: Diagnosis Infection: Diagnosis
•
Early diagnosis of spreading acute infection: erythema beyond ulcer edge, induration, new or increasing pain, warmth, purulent drainage, crepitus or discoloration of skin, increasing ulcer size, signs of systemic infection.
•
Determine bacterial bioburden:–
Quantitative tissue culture (Gold Standard)
–
Quantitative swab technique (Levine technique)•
Consider the diagnosis of pressure ulcer infection if the culture results indicate bacterial bioburden of
> 105 CFU/g of
tissue and/or the presence of beta hemolytic streptococci.
40

©NPUAP & EPUAP, 2009 41
Assessment & Treatment of Assessment & Treatment of Infection: Management Infection: Management •
Optimize host. Prevent contamination.
•
Reduce bacterial load with cleansing & debridement. Drain local abscesses.
•
Consider the use of topical antiseptics that are properly diluted and appropriate for pressure ulcers. Antiseptics should be used for a limited time period to control the bacterial bioburden, to
clean the ulcer and reduce surrounding inflammation. The professional should be knowledgeable of proper dilutions, as well as risks of toxicity and adverse reactions.
•
Consider topical antiseptics for pressure ulcers that are not expected to heal and are critically colonized.
•
Consider the use of topical antimicrobial silver or medical-grade honey dressings for pressure ulcers infected with multiple organisms because these dressings offer broad antimicrobial coverage.
41

©NPUAP & EPUAP, 2009 42
Assessment & Treatment of Assessment & Treatment of Infection: Management Infection: Management
•
Limit
the use topical antibiotics on infected pressure ulcers except in special situations.
•
Use systemic antibiotics for individuals with clinical evidence of systemic infection, such as positive blood cultures, cellulitis,
fasciitis, osteomyelitis, systemic inflammatory response syndrome (SIRS) or sepsis if consistent with the individual’s goals.
•
Evaluate the individual for osteomyelitis if exposed bone is present; the bone feels rough or soft or the ulcer has failed to
heal with prior therapy.
42

©NPUAP & EPUAP, 2009 43
Biophysical AgentsBiophysical Agents
•
Consider a course of electrical stimulation for Stage III & IV and recalcitrant Stage II pressure ulcers. (A)
•
Consider pulsed electromagnetic treatment for recalcitrant Stage II-IV PUs.
•
Consider NPWT as an early adjuvant for deep, full thickness PUs. (B)
43

©NPUAP & EPUAP, 2009 44
Biophysical AgentsBiophysical Agents
•
Consider infrared therapy for recalcitrant full thickness ulcers.
•
Consider low frequency ultrasound spray for the treatment of clean recalcitrant full thickness PUs and low frequency ultrasound for debridement of soft devitalized tissue.
•
Consider a course of hydrotherapy & pulsed lavage.•
There is insufficient peer reviewed, published evidence to recommend topical oxygen, hyperbaric oxygen, laser or ultraviolet light therapies for the treatment of pressure ulcers.
44

©NPUAP & EPUAP, 2009 45
Biological Dressings & Growth Biological Dressings & Growth Factors Factors
•
Insufficient evidence to support biological dressings
•
PDGF-BB may improve healing–
insufficient evidence to support
recommendations. –
Lacks FDA approval for pressure ulcers
–
Approved for diabetic foot ulcers
45

©NPUAP & EPUAP, 2009
Surgery for Pressure Ulcers Surgery for Pressure Ulcers
•
Validate end-of-life decisions if anticipating surgery. •
Optimize physical & psychological factors that may impair surgical wound healing.
•
Assess for osteomyelitis; if present infected bone must be resected prior to or during surgical closure. (B)
•
Initiate a program of progressive sitting according to surgeon’s orders & position the individual on a pressure-
redistributing chair cushion. •
Ensure the individual has a positive social network at home (B)
as well as needed equipment, and the ability to maintain
the equipment and adhere to postoperative needs.
46

©NPUAP & EPUAP, 2009 47
PU Management in Individuals Requiring PU Management in Individuals Requiring Palliative Care Palliative Care
•
Dearth of RCTs comparing approaches in human subjects
•
Impossible to eradicate PrU due to multiple risk factors & co-morbidities
•
Healing of PU may be unrealistic goal & new ones may occur.
•
Goals of care to be established in collaboration with individual & family. To the extent possible, allow the individual to direct care.
47

©NPUAP & EPUAP, 2009 48
PU Management in Individuals Requiring PU Management in Individuals Requiring Palliative Care Palliative Care ––
Risk AssessmentRisk Assessment
•
Patient and Risk Assessment•
Pressure Redistribution
•
Nutrition and Hydration•
Skin Care
•
Pain Assessment and Management•
Pressure Ulcer Care–
Exudate
–
Odor–
Pain
48

Guideline Availability Guideline Availability (www.npuap.org)(www.npuap.org)
EPUAP NPUAPQuick Reference
Free on web* Free on webPrinted copy through NPUAP
Printed copy from NPUAP website
ClinicalPracticeGuideline
Printed copy through NPUAP
Printed copy from NPUAP website
©NPUAP & EPUAP, 2009 84
*Translations will be available in multiple languages.

““SpinSpin--offsoffs””
©NPUAP & EPUAP, 2009 85

Implementation & DisseminationImplementation & Dissemination
©NPUAP & EPUAP, 2009 86

©NPUAP & EPUAP, 2009
The End The End
5252