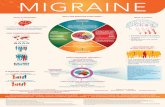
Migraine and You An Educational Guide for Migraine Headache Sufferers.
Migraine
-
Upload
drraajitchanana -
Category
Health & Medicine
-
view
3.424 -
download
7
description
Transcript of Migraine

MIGRAINE
-Dr. Raajit Chanana1

Migraine headache is a complex recurrent headache that is one of the most common complaints in medicine.
Introduction
2

Classification of Migraine
3

Migraine with Aura
4

Childhood periodic syndromes that are commonly precursors of migraine
5

Complications of migraine
6

Probable Migraine
7

Vascular theory
It was believed that ischemia induced by intracranial vasoconstriction is responsible for the aura of migraine and the subsequent rebound vasodilation and activation of perivascular nociceptive nerve resulted in headache.
Based on 3 observations -:1. Extracranial vessels become distended and pulsatile during an attack2. Stimulation of an intracranial vessels in an awake person induces
headache3. Vasoconstrictors improve the headache and vaso dilators provoke
an attack
Pathophysiology
8

Neurovascular theory Complex series of neural and vascular events initiates migraine Migraine is primarily a neurogenic process with secondary
changes in cerebral perfusion
Cortical spreading depression CSD is a well defined wave of neuronal excitation in the cortical
grey matter that spreads from its site of origin at the rate of 2-6mm/min
This cellular depolarization causes the primary cortical phenomenon aura phase, in turn, it activates trigeminal fibers causing headache.
Patho Physiology contd…
9

Vasoactive substances and Neurotransmitters Perivascular nerve activity results in release of substances
such as substance P, neurokinin A, CGRP and NO which produce vessel dilation, protein extravasation and sterile inflammation stimulating the trigeminocervical complex.
Cutaneous Allodynia Secondary pain pathways of the trigeminophthalamic system
become sensitized during a migraine attack.
Patho Physiology contd…
10

Dopamine pathway Some of the symptoms associated with migraine such as nausea,
vomiting, yawning, hyperactivitycan be attributed to dopaminergic stimulation.
Endothelial dysfunction Serotonin and migraine Plasma extravasation mediated by vasoactive substances is
blocked by ergots, sumatriptan, indomethacin, GABA agonists and benzodiazepines
5HT-1D receptors in trigeminal sensory neurons and 5HT 1B receptors are present on smooth vessels in the meningeal vessels
Patho Physiology contd…
11

Approx 70% of patients have a first degree relative with a history of migraine.
Familial Hemiplegic Migraine Migraine with aura that is preceded or followed by hemiplegia
that typically resolves FHM type 1 - Linked to mutations in the calcium channel gene –
chromosome 19.May be associated with cerebellar ataxia FHM type 2 - mutation in the sodium channel gene ATP1A2 on
chromosome 3 FHM type 3- mutation in a sodium channel alpha subunit coding
gene
Etiology
12

Migraine in inherited disorders -:
1. MELAS (mitochondrial myopathy, encephalopathy and lactic acidosis)
2. CADASIL (cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy)
3. Genetic vasculopathies like RVCL (retinal vasculopathy with cerebral leukodystrophy) etc.
Etiology contd…
13

Migraine accounts for 64% of severe headaches in females and 43% of severe headaches in males.
In individuals >12yr of incidence increases with age, reaching a peak at 30-40 yrs
F:M = 3.5:1 at 40yrs
Epidemiology
14
Boys Girls Boys GirlsPeaks at 5 years 12-13 years 10-11 years 14-17 years
Migrain Without Aura Migraine with Aura

History U/L, throbbing or pulsatile localized in the frontotemporal and
ocular areas but be felt anywhere around the head or neck. Pain builds over 1-2 hrs and become diffuse. Many patient prefer to lie in dark room
Other symptoms Nausea, vomiting, anorexia and food intolerance occur in about
50 % of patients. Photophobia and phonophobia are commonly associated with headache.
Hemiparesis, confusion, apathy and numbness.
Clinical presentation
15

Prodrome About 60% of patients report premonitory symptoms that occur
hours to days before headache onset. Heightened sensitivity to light, sounds and odors. Lethargy or uncontrollable yawning. Food cravings Mental and mood changes Excessive thirst and polyuria Anorexia Constipation or diarrhea
Clinical presentation contd…
16

It is a complex of neurologic symptoms that may precede or accompany the headache phase or may occur in isolation.
Usually develops over 5-20min and lasts less than 60 minutes. Can be visual, sensory, motor or combination of these Negative symptoms -: Negative scotoma Negative visual phenomenon such as homonymous hemianopia,
central scotoma, tunnel vision, altitudinal visual defects etc.
Aura
17

Positive symptoms Scintillating scotoma-highly characteristic of migraine Photopsia or flashes of light Heat waves Micropsia, macropsia
Paresthesia Occurring in 40%of cases constitute the next most common aura. Sensory symptoms rarely occurs in isolation and usually follows visual
aura. Motor symptoms may occur in 18% of patients Speech and language disturbances have been reported in 17-20% of
patients
Aura contd…
18

Scintillating Scotoma
19

Central Scotoma
20

Multiple spotty scotoma
21

Half visual field loss
22

Stress Excessive or insufficient sleep Medications (OCP, vasodilators) Strong odors eg. perfumes, cologne etc. Hormonal changes such as pregnancy, menstruation Head trauma Weather changes Metabolic or infectious disease Physical exertion Cold stimulus eg. ice cream
Migraine triggers
23

Foods containing tyramine may provoke migraine1. Aged cheese2. Yogurt3. Bananas 4. Vinegar5. Beans6. Peanuts
Migraine triggers contd…
24

Family history Approx 70% of patients have a first-degree relative with a
history of migraine
Disability assessment Simple questionnaires like MIDAS migraine disability
assessment can be used to quantify the disability and for follow up
25

Thorough neurologic examination is essential, results will be normal in majority
Possible findings may include Cranial/cervical muscle tenderness Horner syndrome Tachycardia/ bradycardia Conjunctival injection Hypertension/hypotension Hemisensory/ hemiparetic neurological deficits ( complicated
migraine)
Physical Examination
26

Findings that suggest a headache diagnosis other than migraine
Dim scotoma lasting a few seconds to several minutes ie amaurosis
Temporal artery tenderness Meningisnus Mental status changes Focal neurologic deficit eg confusion, seizures
Physical Examination contd…
27

Focal neurologic findings that occur with headache and persist temporarily after the pain resolves suggests a migraine variant
U/L paralysis or weakness-hemiplegic migraine Aphasia, dysarthria, vertigo, tinnitus, syncope, balance
problems-basilar migraine Third nerve palsy with sparing of pupillary response-
ophthalmoplegic migraine
Physical Examination contd…
28

Migraine without aura Diagnostic criteria: A. At least 5 attacks fulfilling criteria B-D B. Headache attacks lasting 4-72 hours (untreated or
unsuccessfully treated) C. Headache has at least two of the following characteristics: 1. unilateral location 2. pulsating quality 3. moderate or severe pain intensity 4. aggravation by or causing avoidance of routine physical
activity (eg. walking or climbing stairs)
Diagnostic criteria
29

D. During headache at least one of the following: 1. nausea and/or vomiting 2. photophobia and phonophobia
E. Not attributed to another disorder
Diagnostic criteria contd…
30

Migraine with aura
Diagnostic criteria -:A. At least 2 attacks fulfilling criterion B
B. Migraine aura fulfilling criteria B and C for one of the subforms 1.2.1-1.2.6 as per the IHS classification
C. Not attributed to another disorder
31

Typical aurawith migraine headache
A. At least 2 attacks fulfilling criteria B–D
B. Aura consisting of 1 of the following, but no motor weakness:1. fully reversible visual symptoms including positive and/or
negative features2. fully reversible sensory symptoms including positive and/or
negative features3. fully reversible dysphasic speech disturbance
32

Typical aurawith migraine headache contd…
C. At least two of the following:1. homonymous visual symptoms and/or unilateral sensory
symptoms2. at least one aura symptom develops gradually over 5 min
and/or different aura symptoms occur in succession over 5 min
3. each symptom lasts 5 and 60 minD. Headache fulfilling criteria B-D for 1.1 Migraine without aura
begins during the aura or follows aura within 60 minE. Not attributed to another disorder
33

Chronic migraine Migraine headache that occurs more than 15 days a month for
greater than 3 months Status migrainosus Migraine attacks persists for >72 hours. Persistent aura ( 30-60 min ) without infarction Migrainous infarction Migraine triggered seizures
Complications of migraine
34

Migraine is a clinical diagnosis. Diagnostic investigations are performed due to following reasons Exclude structural, metabolic and causes of heada Rule out comorbid disease that could complicate headache and
its treatment
Work up
35

Neuroimaging is usually not necessary except Onset of migraine after 5o years of age change in the pattern of previous migraine First or worst severe headache New onset of headache in a patient with cancer or HIV patient Headache with an abnormal neurologic examination Headache with fever Migraine and epilepsy New daily persistent headache Escalation of headache frequency/intensity in the absence of
medication overuse headache Posteriorly located headaches in children
36

Visual field testing should be performed in patients with persistent visual phenomenon
Indications for lumber puncture include -:1. First or worst headache of a patients life2. Severe, rapid onset, recurrent headaches3. Progressive headaches4. Atypical chronic intractable headaches
37

Acute attack Preventive
Management
38

Establish a diagnosis. Educate migraine sufferers about their condition and its
treatment. Encouraging patients to track their own progress through the use
of diary cards, flow charts, headache calendars and frequency and severity of attacks, the presence and degree of temporary disability, and associated symptoms such as nausea and vomiting.
Create a formal management plan and individualize management. Consider comorbidity/coexisting conditions (such as heart disease, pregnancy, and uncontrolled hypertension).
General principles of management
39

Encourage the patient to identify and avoid triggers. Guard against medication-overuse headache (“rebound
headache” or “drug-induced headache”). Frequent use of acute medications (ergotamine [not DHE], opiates, triptans, simple analgesics, and mixed analgesics) is generally thought to cause medication-overuse headache.
Use migraine-specific agents (triptans dihydroergotamine [DHE]) in patients with moderate or severe migraine or whose mild-to-moderate headaches respond poorly to nonsteroidal anti-inflammatory drugs (NSAIDs) or combinations such as aspirin plus acetaminophen plus caffeine
General principles of management contd..
40

Goals of acute migraine treatment are as follows: Treat attacks rapidly and consistently without recurrence. Restore the patient’s ability to function. Minimize the use of back-up and rescue medications. (A rescue
medication is used at home when other treatments fail and permits the patient to achieve relief without the discomfort and expense of a visit to the physician’s office or emergency department.)
Be cost-effective for overall management. Have minimal or no adverse events
Acute Treatment
41

Triptan (serotonin 1B/1Dreceptor agonists) Effective and safe acute management Appropriate initial choice in patients with moderate to severe
migraine Routes-oral, subcutaneous and nasal Drugs – sumatriptan-50-100mg tablet at onset , may repeat after
2hour (max 200mg/d) Rizatriptan –most efficacious, early onset of action, 5-10 mg
tablet at onset may repeat after 2hr max 30mg/d) Naratriptan, almotriptan,frovatriptan, zolmitriptan
Specific medications
42

Triptans should not be used more than 3 days weekly to avoid transformed migraine and medication overuse headache
Caution-avoid in patients of CAD Adverse effects Paresthesia, jaw or neck tightness, warm/cold sensation etc.
Specific medications contd…
43

Ergot alkaloids and derivatives-nonselective 5-HT1 agonists) Ergotamine PO/PR (and caffeine combination) may be considered
in the treatment of selected patients with moderate to severe migraine.
Dose 2mg PO, f/b 1-2mg every 30 min until attack is aborted, no more than 6mg/day
Adverse effects-vasospasm, angina, tachycardia, numbness of extremities, rebound headache, ergotism, gangrene etc
Specific medications contd…
44

Dihydroergotamine- alpha adrenergic blocking agent with a direct stimulating effect on smooth muscle of peripheral and cranial blood vessels. It is a non selective 5-HT1 agonist
Route- iv or nasal Dose- 1mg iv/im repeated 1 hrly , no more than 3 mg for im and
2mg for iv Nasal-1 spray 0.5mg in each nostril not more than 6 sprays/24hr DHE nasal spray is safe and effective for the treatment of acute
migraine attacks and should be considered for use in patients with moderate to severe migraine
DHE IV plus antiemetics IV is an appropriate treatment choice for patients with severe migraine
Specific medications contd…
45

Antiemetics -:Oral antiemetics are an adjunct to treat nausea associated with migraine .Metoclopramide IM/IV is an adjunct to control nausea and may be considered as IV monotherapy for migraine pain relief Prochlorperazine IV, IM, and PR may be a therapeutic choice for migraine in the appropriate setting Chlorpromazine IV Serotonin receptor (5-HT3) antagonists may be considered as adjunct therapy to control nausea in selected patients with migraine attacks
Non specific medications
46

NSAIDs, nonopiate analgesics, and combination analgesics. Acetaminophen, alone, is not recommended for migraine . NSAIDs (oral) and combination analgesics containing caffeine are
a reasonable first-line treatment choice for mild to moderate migraine attacks or severe attacks that have been responsive in the past to similar NSAIDs or nonopiate analgesics
Non specific medications contd…
47

Opiate analgesics. Butorphanol nasal spray is a treatment option for some patients
with migraine (Grade A). Butorphanol may be considered when other medications cannot be used or as a rescue medication when significant sedation would not jeopardize the patient
Other medications. Isometheptene and isometheptene combination agents may be a
reasonable choice for patients with mild-to-moderate headache . Corticosteroids (dexamethasone or hydrocortisone) are a
treatment choice for rescue therapy for patients with status migrainosus .
Non specific medications contd…
48

May be considered when -: Frequency of migraine is >2/months Duration of individual attack is longer than 24hrs Headache causes major disruption in patients lifestyle Abortive therapy fails or is overused Symptomatic medications are ineffective Use of abortive medications more than twice a week Migraine variants such as hemiplegic migraine
Preventive treatment
49

The goals of migraine preventive therapy are to1)reduce attack frequency, severity, and duration2)improve responsiveness to treatment of acute
attacks3)improve function and reduce disability
50

5 principal classes of drugs are used -: Antiepileptics Antidepressants Antihypertenseives Serotonin antagonists NSAIDS
Pharmacotherapy
51

ANTIEPILEPTICS
Well tolerated Valproic acid is useful as afirst line agent.400-600 mg BD Carbamazepine Gabapentin topiramate
52

ANTIDEPRESSANTS
Tricyclic antidepressants Amitriptyline- 10-75mg at night Nortriptyline
Selective serotonin reuptake inhibitors Fluoxetine
Other antidepressants Bupropion, mirtazepine, trazodone, venlafaxine
53

ANTIHYPERTENSIVES
Beta-blockers Propranolol -40-120mg BD Timolol
Calcium channel blockers Diltiazem Nimodipine Verapamil
54

SEROTONIN ANTAGONISTSMethysergide-1-4mg OD
Flunarizine5-15mg OD
NSAIDS Aspirin Mefenamic acid Ibuprofen Naproxen/naproxen sodium
Other Magnesium Vitamin B2
55

Special considerations Direct special attention to women who are pregnant or want to
become pregnant. Preventive medications may have teratogenic effects.
Take coexisting conditions into account. Some (comorbid/coexisting) conditions are more common in persons with migraine.
Eg-beta blocker are preferred in young anxious patients, hypertensive patients, history of angina
TCA’s are preferred in patients of depression, underweight Valproic acid is preferred in patients of epilepsy and mania
56

Biofeedback Cognitive-behaviour therapy Relaxation therapy
AVOIDANCE OF MIGRAINE TRIGGERS
Complimentary and alternative therapy Body work eg. massage Creative arts eg. dance, music Yoga Acupuncture and acupressure
Non-pharmacological treatment
57

Thank You!
58