Management Of Intestinal Obstruction
-
Upload
dr-harim- -
Category
Economy & Finance
-
view
28.408 -
download
4
description
Transcript of Management Of Intestinal Obstruction
History-Onset, acute/chronic, bleeding, constipation, weight loss, anorexia, changes in bowel habits, associated features, previous surgery, drug usage.
Physical examination- General physical, vital signs, abdominal distention/mass, tenderness/guarding, auscultation (Bowel sounds)-high pitched, tinkling sounds.
Complete blood count- A raised white cell count will indicate an infection. A raised hematocrit may indicate hemoconcentration while a decreased hematocrit will signify blood loss.
Serum Urea & electrolytes- Derangements may be seen with vomiting & diarrhea. Dehydration will be reflected in raised serum urea & creatinine.
Liver function test- Elevated serum bilirubin & alkaline phosphatase point towards an obstructed cause.
Serum amylase It is a non-specific test & may be raised in
cases of small intestinal obstruction.
Erect chest x-ray- Free air under the diaphragm, without recent abdominal surgery, shows perforated viscus.
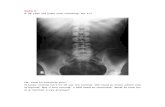
Supine abdominal x-ray- It may show abnormal bowel pattern (dilation of bowel loops in case of obstruction or sentinel loop). It may also show masses.
Erect Film- It shows fluid levels in case of obstructed bowel.
Ultrasound- It is less useful but may indicate presence of intraparitoneal fluid or mass. It can also detect gallstones or other biliary diseases.
CT- It is performed with oral or Intravenous contrast. Lower abdomen CT is useful in detection of acute appendicitis, acute diverticulitis, intestinal obstruction, aortic aneurysm & mesentric ischaemia.
Supportive NPO Rehydration & urine output monitoring Cross-match blood & transfusion if required Pass NG tube( diagnostic/therapeutic purpose) I.V antibiotics if indicated
Symptomatic Analgesia after confirming diagnosis
Specific Therapy directed at underlying disease
Investigations- Plain X-ray Duodenal obstruction- stomach & proximal
duodenum are distended- “double bubble” Jejunal & ileal obstruction- air fluid levels
present
Treatment: Correct electrolyte & fluid deficits Duodenal atresia requires
duodenojejuostomy & spliting of the anastomosis with a feeding tube.
Atretic segments in the jejunum or ileum may produce dilated proximal loops that require tapering prior to anastomosis.
Treatment: The volvulus is reduced, the
transduodenal band(Ladd’s band) divided, the duodenum mobilised & the mesentry freed.
Appendicectomy is routinely performed to avoid diagnostic difficulty with appendicitis in the future.
Infarcted bowel necessitates resection.
Investigation Differential white cell count is raised A Merkel’s radioisotope scan will reveal acid
producing gastric mucosa.
Treatment: Excision of the inflammed diverticulum Presence of gastric mucosa requires the
resection of the ileal loop containing the diverticulum to ensure complete excision of all acid producing mucosa.
Plain x-ray Shows small dilated bowel loops Gastrograffin enema (in the absence of
acute obstruction) shows up the meconium & excludes Hirshsprung’s disease.
Treatment: Colonic washouts may restore patency Proximal ileum is anastomosed end to side
to the colon with a distal ileostomy to clear the obstruction.
Gastrograffin enema demonstrates unhindered flow of contrast upto the cecum & beyond
Relief of constipation requires bowel washouts or manual evacuation.
Counselling
Investigations: Double contrast Gastrograffin enema (‘claw
sign’ of ileocolic intussusception) In adults, a contrast CT scan of the
abdomen or barium enema is confirmatory.
Rx: The diagnostic enema may be used to
reduce the intussusception by hydrostatic pressure (in children)
Surgical reduction by taxis; bowel resection if there is gross edema preventing reduction or vascular compromise.
Investigations: Plain x-ray may be diagnostic -Large gas-filled, ‘kidney bean-shaped’
swelling in the right upper zone: Sigmoid volvulus
-Large gas-filled, ‘kidney bean-shaped’ swelling in the left lower zone: Caecal volvulus.
Rx: Sigmoid volvulus may be relieved at right
sigmoidoscopy. Emergency laprotomy & resection of the
volvulus for strangulated or recurrent cases. Gangrenous bowel is exteriorised &
resected, with the formation of a ‘double barrel’ colostomy (Paul-Mikulicz procedure).
Investigations: White cell count: >20×109 /L Serum amylase: slightly raised (>200IU)Mesentric angiography
Rx: Laparotomy: superior mesentric
embolectomy; Resection of areas of non-viable bowel.‘second look’ laprotomy at 24 hours for
further resection of non-viable bowel.
Investigations:Plain x-ray abdomen: Characteristics of the
distended bowel from which the level of obstruction is identified
Contrast enhanced CT: Delineates the type & level of obstruction
Treatment: Nasogastric decompression of stomach &
bowel proximal to the obstruction. I/v Fluids & electrolyte therapy Analgesia Antibiotics( inflammatory or infectious
causes) Emergency surgery * Post operative adhesion obstruction usually
resolves on conservative measures.
Operative procedures vary according to cause of obstruction.
Resection- The diseased part of the small intestine (ileum) is removed. The two healthy ends are then sewn back together and the incision is closed.
Indications Gangrenous bowel
In cases of strangulated Inguinal/femoral hernias the standard groin incision is given & the weakness repaired using hernioplasty or herniorrhaphy, with bowel resection if required.
In adhesive obstructed cases, laproscopic adhesiolysis (adhesive band lysis) maybe performed in selected patients or using open procedure through an incision dictated by scar from previous surgery.
Bypass: Anastomosis of proximal small bowel or large intestine distal to the obstruction may be a good procedure in some cases of carcinoma or radiation injury.
Decompression-Done by use of gastrostomy or jejunostomy tube where adhesions can’t be freed & bypass can’t be done. Parentral nutrition is provided that
allows spontaneous resolution.
The tube can be passed orally orBy needle aspiration through the bowel wall.