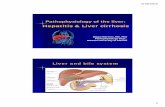
liver cirrhosis
-
Upload
ciciliya-joseph -
Category
Education
-
view
192 -
download
0
Transcript of liver cirrhosis

CIRRHOSIS

Cirrhosis is an irreversible result of various disorders that damage liver cells over time. Eventually, damage becomes so extensive that the normal structure of the liver is distorted and its function is impaired.
Cirrhosis is a chronic liver disease that is the result of damage to liver tissue with scarring of the liver (fibrosis - nodular regeneration) causing progressive decrease in liver function, excessive fluid in the abdomen (ascites), bleeding disorders (coagulopathy), increased pressure in the blood vessels (portal hypertension), and brain function disorders (hepatic encephalopathy). Excessive alcohol use is the leading cause of cirrhosis.

The disease process often takes the following path:
Scarring: The main damage in cirrhosis is triggered by scarring (fibrosis) that occurs from injuries due to alcohol, viruses, or others. The scar tissue and other changes in liver cells gradually replace healthy liver tissue and act like small dams to alter the flow of blood and bile in and out of the liver.
Altered Blood and Bile Flow. The changes in blood and bile flow have significant consequences, with both the liver and other organs responding to the altered flow:

• The spleen overproduces nitric oxide, a chemical that causes blood vessels in the spleen to widen (dilate).
• The small blood vessels and bile ducts in the liver itself, however, narrow (constrict). (Blood vessels in other organs, including the kidney, also narrow.)
• Blood flow coming from the intestine into the liver is slowed by the narrow blood vessels. It backs up through the portal vein and seeks other routes.

Enlarged, abnormally twisted and swollen veins called varices form in the stomach and lower part of the esophagus in order to compensate for the backup blood.
Bilirubin also builds up in the bloodstream, resulting in jaundice, a yellowish cast in the skin and eyes, as well as dark-colored urine.
Fluid buildup also occurs in the abdomen (called ascites), and swelling in the legs is common.

Structure of the LiverThe vital processes the liver performs rely on well-organized
liver architecture.The basic building blocks of the liver are the following structures:
• Bile ducts • Blood vessels • Working liver tissue (called the parenchyma) • Supportive (connective) tissueThe Liver's Blood Supply. The liver is rich in blood. It
holds about a pint, or 13% of the body's supply. It is furnished with blood from two large vessels, the hepatic artery and the portal vein, and is drained of blood by the hepatic vein. (The word "hepatic" derives from the Latin word for liver.)

CausesSeveral processes can lead to cirrhosis.Alcoholism Chronic alcoholism particularly endangers
the liver by causing alcoholic liver disease (also called alcohol-induced liver disease). Alcoholic liver disease includes fatty liver (build-up of fat cells in the liver), alcoholic hepatitis (inflammation of the liver caused by chronic drinking), and alcoholic cirrhosis.

Alcoholic cirrhosis is the primary type of cirrhosis in the U.S. It develops in 10 - 20% of heavy drinkers, usually after 10 - 15 years of heavy alcohol consumption. People who drink heavily and who also have hepatitis C are at particular risk of developing cirrhosis. In the liver, alcohol converts to toxic chemicals that trigger inflammation and tissue injury, which lead to cirrhosis.

Chronic Hepatitis Chronic hepatitis, both hepatitis B and
hepatitis C, is another primary cause of cirrhosis. Chronic hepatitis C is a more common cause of cirrhosis in developed countries, while hepatitis B is a more common cause of cirrhosis worldwide, People with chronic hepatitis B who are co-infected with hepatitis D are especially at risk for cirrhosis. The longer a patient has had chronic hepatitis, the greater the risk for eventually developing cirrhosis.

The hepatitis virus can produce inflammation in liver cells, causing injury or destruction. If the condition is severe enough, the cell damage becomes progressive, building a layer of scar tissue over the liver. In advanced cases, as with alcoholic cirrhosis, the liver shrivels in size, a condition called postnecrotic or posthepatic cirrhosis.
Autoimmune Hepatitis

Bile Ducts Disorders Disorders that block or damage the bile
ducts can cause bile to back up in the liver, leading to inflammation and cirrhosis. These diseases include primary biliary cirrhosis and primary sclerosing chlorangitis.
Primary Biliary Cirrhosis. Primary Sclerosing Cholangitis.

• Nonalcoholic Fatty Liver Disease (NAFLD) and Nonalcoholic Steatohepatitis (NASH)
NAFLD resembles alcoholic liver disease, but it occurs in people who do not drink a lot of alcohol. Obesity and type 2 diabetes are the two main causes of a fatty liver. Some evidence suggests that insulin resistance (the primary problem in type 2 diabetes) is a major factor in development of a fatty liver. A diet high in fatty foods may also be a risk factor, as dietary fat accumulates in the liver. Due to the recent rise in childhood obesity, NAFLD is increasingly occurring in children.

Hereditary DisordersHemochromatosis. Hemochromatosis is a disorder of
iron metabolism. This disease interferes with the way the body normally handles iron. People with hemochromatosis absorb too much iron from the food that they eat. The iron overload accumulates in organs in the body. When excess iron deposits accumulate in the liver, they can cause cirrhosis.
Other Hereditary Disorders. Other inherited diseases that can cause cirrhosis include Wilson’s disease (which causes an accumulation of copper in the body), alpha-1 antitrypsin deficiency (a genetic disorder caused by defective production of a particular enzyme), and glycogen storage diseases etc….

Other CausesSchistosomiasis, Long-term or high-level exposure to
certain chemicals and drugs, including arsenic, methotrexate, toxic doses of vitamin A, and certain types of prescription medication.


Symptoms• Cirrhosis is divided into two stages: Compensated
and decompensated.
• Compensated cirrhosis means that the body still functions fairly well despite scarring of the liver. Many people with compensated cirrhosis experience few or no symptoms.
• Decompensated cirrhosis means that the severe scarring of the liver has damaged and disrupted essential body functions. Patients with decompensated cirrhosis develop many serious and life-threatening symptoms and complications.

Early symptoms of compensated cirrhosis may include:Fatigue and loss of energy Loss of appetite and weight loss Nausea or abdominal pain Spider angiomas may develop on the skin. These are
pinhead-sized red spots from which tiny blood vessels radiate.
As cirrhosis progresses to a decompensated stage, patients may develop the following symptoms:
Fluid buildup in the legs and feet (edema) and in the abdomen (ascites). (Ascites is associated with portal hypertension, which is described in the Complications section of this report.)
Jaundice. This yellowish cast to the skin and eyes occurs because the liver cannot process bilirubin for elimination from the body.

• Jaundice is a condition produced when excess amounts of bilirubin circulating in the bloodstream dissolve in the subcutaneous fat (the layer of fat just beneath the skin), causing a yellowish appearance of the skin and the whites of the eyes. With the exception of normal newborn jaundice in the first week of life, all other jaundice indicates overload or damage to the liver, or inability to move bilirubin from the liver through the biliary tract to the gut.

• Itching. Itching (pruritus) develops from buildup of bile products.
• The palms of the hands may be reddish and blotchy, a condition known as palmar erythema
• In men, swelling of breasts or shrinkage of the testicles may occur.
• Easy bruising and excessive bleeding may occur.

Complications• Decompensated cirrhosis increases the risk
of serious and potentially life-threatening complications. (Once decompensation occurs, mortality rates without liver transplantation can be as high as 85% within 5 years.) The most serious complications are those associated with portal hypertension (increased pressure in the portal vein that carries blood from the intestine to the liver).

They include:• Ascites (fluid buildup in the abdomen) • Variceal hemorrhage (bleeding in the upper
stomach and esophagus from ruptured blood vessels)
• Spontaneous bacterial peritonitis is a form of peritonitis (inflammation of the membrane that lines the abdomen), which is associated with ascites. Other bacterial infections are also a common complication of cirrhosis.
• Hepatic encephalopathy (damage to the brain). Impaired brain function occurs when the liver cannot detoxify harmful substances, and can lead to coma.
• Liver cancer is a serious long-term risk with cirrhosis. Other complications also occur.

Ascites• Ascites is fluid buildup in the abdominal
cavity. It is uncomfortable and can impair breathing and other functions. Ascites is caused by a combination of portal hypertension (high pressure in the blood vessels of the liver) and low albumin levels. Albumin is a protein produced by the liver. Although ascites itself is not fatal, it is a marker for severe progression.

Variceal BleedingOne of the most serious consequences of portal
hypertension is the development of varices, veins that enlarge to provide an alternative pathway for blood diverted from the liver. In most patients, they form in the esophagus. They can also form in the upper stomach. Varices pose a high risk for rupture and bleeding because they are thin-walled, twisted, and subject to high pressure. Variceal intestinal bleeding is a life-threatening event. Symptoms include vomiting blood or black and tarry stools.

Spontaneous Bacterial Peritonitis• Spontaneous bacterial peritonitis is a life-threatening
bacterial infection of the ascitic fluid. The main symptoms include confusion and altered mental status, fever, chills, and abdominal pain.
Hepatic Encephalopathy• Mental impairment is a common event in advanced
cirrhosis. In severe cases, the disease causes encephalopathy (impaired brain function), with mental symptoms that range from confusion to coma and death. Hepatic encephalopathy is caused by a buildup in the blood of harmful intestinal toxins, particularly ammonia, which then accumulate in the brain.

• Early symptoms of hepatic encephalopathy include forgetfulness, unresponsiveness, and trouble concentrating. Sudden changes in the patient's mental state, including agitation or confusion, may indicate an emergency condition. Other symptoms include bad fruity-smelling breath and tremor. Late-stage symptoms of encephalopathy are stupor and eventually coma.

COAGULATION DEFECTS• Complex coagulation derangements can occur in
cirrhosis. These derangements include the reduction in the synthesis of coagulation factors,
excessive fibrinolysis, disseminated intravascular coagulation, thrombocytopenia,and platelet dysfunction.
• Vitamin K–dependent clotting factor, including factor VII, is affected early.
• The net effect of these events is the development of bleeding diathesis.

Liver CancerPeople with cirrhosis have an increased risk for
hepatocellular carcinoma, a type of liver cancer. Hepatitis B and C, alcoholism, hemochromatosis, and primary biliary cirrhosis -- all causes of cirrhosis -- are some of the major risk factors for liver cancer. Cirrhosis due to hepatitis C is the leading cause of hepatocellular carcinoma, while cirrhosis due to hepatitis B is the leading cause of deaths related to liver cancer.
Other ComplicationsKidney Failure. Portal hypertension can cause several
secondary complications, including kidney failure.Osteoporosis.

• Insulin Resistance and Type 2 Diabetes. Cirrhosis causes insulin resistance, a primary feature in type 2 diabetes. As insulin resistance progresses, it causes excess glucose to buildup in the blood, which leads to type 2 diabetes. Type 2 diabetes is also a risk factor for nonalcoholic fatty liver disease, one of the causes of cirrhosis
• Heart Problems. Cirrhosis may increase the risk for heart failure and other cardiovascular complications

DiagnosisA physical examination may reveal the following in a
patient with cirrhosis:The cirrhotic liver is firm and often enlarged in
early stages of the disease. The liver may feel rock-hard. (In advanced stages of cirrhosis, the liver may become small and shriveled.)
If the abdomen is swollen, the doctor will check for ascites by tapping the flanks and listening for a dull thud and feeling the abdomen for a shifting wave of fluid.
The doctor will also check for signs of jaundice, muscle wasting, and (in male patients) breast enlargement.

A patient’s medical history is another indicator of the risk for cirrhosis. Patients with a history of alcoholism, hepatitis B or C, or certain other medical conditions are at high risk.
Other tests (blood tests, imaging tests, liver biopsy) may also be performed. The results of these tests along with the presence of specific complications (ascites and encephalopathy) are used for calculating the Child-Pugh Classification. This is a staging system (A to C) that helps doctors determine the severity of cirrhosis and predict the development of future complications.

Blood TestsA patient’s medical history can reveal risk factors
(such as alcoholism) that warrant screening for conditions such as hepatitis. Blood tests are also performed to measure liver enzymes associated with liver function. Enzymes known as aminotransferases, including aspartate (AST) and alanine (ALT), are released when the liver is damaged. Blood tests may also measure:
• The ratio of AST to ALT also provides information in patients with suspected alcoholic liver disease. Seventy percent of patients with alcoholic liver disease had ratios greater than 2 compared to only 4% of patients with viral hepatitis.

Serum albumin concentration. Serum albumin measures protein in the blood (low levels indicate poor liver function).
Prothrombin time (PT). The PT test measures in seconds the time it takes for blood clots to form (the longer it takes the greater the risk for bleeding).
Alkaline phosphatase (ALP). High ALP levels can indicate bile duct blockage.
Bilirubin. One of the most important factors indicative of liver damage is bilirubin, a red-yellow pigment that is normally metabolized in the liver and then excreted in the bile. In patients with hepatitis, the liver cannot process bilirubin, and blood levels of this substance rise, sometimes causing jaundice.

Imaging Tests
• Magnetic resonance imaging (MRI), computed tomography (CT), and ultrasound are all imaging techniques that are useful in detecting and defining the complications of cirrhosis, such as ascites and hepatocellular carcinoma. (However, screening patients with cirrhosis or hepatitis for hepatocellular carcinoma has not yet been proven to be beneficial. The National Cancer Institute recommends against it.) These imaging tests can also provide information on the extent of liver damage.

Liver Biopsy A liver biopsy is the only definite method for
confirming a diagnosis of cirrhosis. It also helps determine its cause, treatment possibilities, the extent of damage, and the long-term outlook. For example, hepatitis C patients who show no significant liver scarring when biopsied may have a low risk for cirrhosis.
A biopsy involves a doctor inserting a biopsy fine needle, guided by ultrasound, to remove a small sample of liver tissue. Local anesthetic is used to numb the area. Patients may feel pressure and some dull pain. The procedure takes about 20 minutes to perform.

Other Tests Used to Detect Complications of Cirrhosis• Endoscopy. Some doctors recommend endoscopy for
patients newly diagnosed with mild-to-moderate cirrhosis in order to screen for esophageal varices. (These are enlarged veins in the esophagus that increase the risk for bleeding). In this test, a fiber optic tube is inserted down the throat. The tube contains tiny cameras to view the inside of the esophagus, where varices are most likely to develop.
• Paracentesis. If ascites is present, paracentesis is performed to determine its cause. This procedure involves using a thin needle to withdraw fluid from the abdomen. The fluid is tested for different factors to determine the cause of ascites:

• Bacteria cultures and white blood cell counts. (These are used to determine the presence of infection.)
• Protein levels. Low levels of protein in the fluid plus a low white blood cell count suggest that cirrhosis is the cause of the ascites.
• Tests for Liver Cancer. Patients diagnosed with cirrhosis should be screened every 6 months to check for the development of liver cancer. Your doctor will use both a blood test to check for levels of alpha-fetoprotein and an imaging test (ultrasound, MRI, or CT scan.)


Child-Pugh Classification of Severity of Liver Disease
Dr C.G. Child and Dr J.G. Turcotte of the University of Michigan first proposed the scoring system in 1964. It was modified by Pugh et al in 1972 . They replaced Child's criterion of nutritional status with the prothrombin time or INR, and thus eliminated the most subjective part of the score.

Parameter Points assigned1 2 3
Ascites Absent Slight ModerateBilirrubin, mg/dL
</= 2 2-3 >3
Albumin, g/dL >3.5 2.8-3.5 <2.8Prothrombin time* Seconds over control* INR
1-3<1.8
4-6
1.8-2.3
>6
>2.3
Encephalopathy None Grade 1-2 Grade 3-4

• A total score of • 5-6 is considered grade A (well-compensated
disease); • 7-9 is grade B (significant functional
compromise); and • 10-15 is grade C (descompensated disease).
These grades correlate with one- and two-year patient survival.

MELD SCORE MELD stands for The Model for End-stage Liver Disease system
that was created by the united network for Organ sharing (UNOS), on February 27, 2002, as a way to prioritize patients on the waiting list for a liver transplant.

• Interpretation: Postoperative Mortality for patients with Cirrhosis
• Score 0-5– Mortality at 7 days: 0.6%– Mortality at 30 days: 3.2%– Mortality at 90 days: 7.1%
• Score 6-10– Mortality at 7 days: 2.8%– Mortality at 30 days: 8.6%– Mortality at 90 days: 13.9%
• Score 11-15– Mortality at 7 days: 7.2%– Mortality at 30 days: 21.9%– Mortality at 90 days: 30.6%

• Score 16-20– Mortality at 7 days: 14.6%– Mortality at 30 days: 44.0%– Mortality at 90 days: 55.8%
• Score 21-25– Mortality at 7 days: 22.2%– Mortality at 30 days: 55.6%– Mortality at 90 days: 66.7%
• Score >26– Mortality at 7 days: 25.0%– Mortality at 30 days: 87.5%– Mortality at 90 days: 87.5%
•

Treatment• Cirrhosis is an irreversible condition.
Treatment goals are to slow the progression of liver damage and reduce the risk of further complications. There are currently no drugs available to treat liver scarring, although researchers are investigating various antifibrotic drugs.

Dietary and Lifestyle Changes• All patients with cirrhosis can benefit from certain types
of lifestyle interventions. These include:
Stop drinking alcohol: It is very important for people with cirrhosis to completely abstain from alcohol.
Restrict dietary salt: Salt can increase fluid buildup in the body. Eating a variety of foods every day can help you limit the amount of salt you are getting. It is best to eat fresh vegetables and fruits whenever possible and to avoid eating processed foods.

Eat a healthy diet: People with cirrhosis are typically malnourished and require increased calories and nutrients. (Excess protein, however, can trigger hepatic encephalopathy.) They also need to avoid certain foods, such as raw seafood or shellfish, which carry risks of blood poisoning (septicemia). A dietician may help provide you with dietary guidelines.

• Get vaccinations: Patients with cirrhosis should ask their doctors which vaccinations (such as hepatitis A, hepatitis B, influenza, pneumococcal pneumonia) they need.
• Discuss all medications with your doctor: Before you take any medications, (including nonprescription pain relievers such as acetaminophen, aspirin, naproxen, and ibuprofen), ask your doctor if they are safe for you. Liver damage affects the metabolization of drugs.

Inform your doctor of any herbs or supplements you are considering taking. Certain types of herbal remedies (kava, chaparral, kombucha mushroom, mistletoe, pennyroyal, and some traditional Chinese herbs) can increase the risk for liver damage. Although some herbs, such as milk thistle (silymarin) have been studied for possible beneficial effects on liver disease, there is no scientific evidence to show that they can help.

Treatment of Underlying Conditions
Treatment for cirrhosis depends on the cause of cirrhosis.
• Chronic Hepatitis. Many types of antiviral drugs are used to treat chronic hepatitis B, including pegylated interferon, nucleoside analogs, and nucleotide analogs. Patients with chronic hepatitis C are treated with combination therapy with pegylated interferon and ribavirin.
• Autoimmune Hepatitis. Autoimmune hepatitis is treated with the corticosteroid prednisone and also sometimes immunosuppressants, such as azathioprine.

• Bile Duct Disorders. Ursodeoxycholic acid , also known as ursodiol or UDCA, is used for treating primary biliary cirrhosis but does not slow the progression. Itching is usually controlled with cholesterol drugs such as cholestyramine and colestipol. Antibiotics for infections in the bile ducts and drugs that quiet the immune system (prednisone, azathioprine, cyclosporine, methotrexate) may also be used. Several surgical procedures may also be tried to open up the bile ducts.

• Nonalcoholic Fatty Liver Disease (NAFLD) and Nonalcoholic Steatohepatitis (NASH). Weight reduction through diet and exercise, and diabetes and cholesterol management are the primary approaches to treating these diseases. Investigators are also studying whether various drugs used to treat type 2 diabetes may help treat NAFLD and NASH.
• Hemochromatosis. Hemachromatosis is treated with phlebotomy, a procedure that involves removing about a pint of blood once or twice a week until iron levels are normal.

Treatment of Complications Treatment of AscitesFirst-line treatment of patients with ascites (fluid
accumulation in the abdomen) involves:• Dietary salt restriction (no more than 2,000 mg/day
of sodium) • Drug treatment with diuretics, usually
spironolactone (Aldactone) and furosemide (Lasix). • Complete abstention from alcohol • Fluid restriction is usually not necessary unless
sodium levels in the blood are low.

Treatment for Recurring or Refractory Ascites. Patients with ascites that does not respond to standard diuretics after a month (refractory ascites) may require procedures to reduce fluid:
Large-volume paracentesis, (which involves using a thin needle to withdraw fluid from the abdomen), may be used for ascites refractory to medical treatment or when complications are present.
Transjugular intrahepatic portosystemic shunt (TIPS) uses a stent placed in veins in the middle of the liver to keep open a passage connecting the hepatic and portal veins.

Treatment of Spontaneous Bacterial Peritonitis• Patients with ascites who have high white
blood cell counts should receive intravenous antibiotic therapy (usually cefotaxime) or oral antibiotic therapy with ofloxacin. Patients who have had an episode of spontaneous bacterial peritonitis are treated with long-term antibiotic therapy of norfloxacin or trimethoprim /sulfamethoxazole to prevent further infection.

Treatment of Hepatorenal Syndrome• Hepatorenal syndrome can occur in patients with
ascites. This is a life-threatening condition in which kidney failure develops because of altered blood flow in the liver. Patients with hepatorenal syndrome are treated with intravenous infusion of albumin. Drug therapy includes oral midodrine and octreotide. Studies suggest that the vasoconstrictor drug terlipressin, given in combination with albumin, may be helpful for treating hepatorenal syndrome.

Treatment of Hepatic EncephalopathyThe first step in managing encephalopathy
(damage to the brain) is to treat any precipitating cause, such as:
High ammonia levels Bleeding Low oxygen Dehydration Infection Use of sedatives

A protein-restricted diet may be used to lower ammonia production. The laxative lactulose, given as a syrup or enema, is used to empty the bowels and to help improve mental status. The antibiotic neomycin may be added for patients who do not improve with lactulose alone. Rifaximin (Xifaxan) is another antibiotic used for treatment of hepatic encephalopathy.

Treatment of Variceal Bleeding• Primary Prevention. Primary prevention
means treating the varices (swollen or distended veins) before they have bled. Varices that are present in the esophagus, stomach, or intestines are always at risk of bleeding. Nonselective beta-blockers drugs, which are commonly used to treat high blood pressure, may be given to prevent bleeding. Propanolol or nadolol are the standard beta-blockers used for variceal prevention.

• Patients with medium-to-large varices that have not bled may also be treated with a surgical procedure called endoscopic variceal ligation (EVL). EVL is also called band ligation. It involves inserting an endoscope or tube down through the esophagus. The equipment contains microcameras and tiny instruments. Latex bands are wrapped around the bleeding varices to shut off the blood supply.
• Other types of therapies, (such as nitrate drugs, shunts, or sclerotherapy), are generally not recommended for primary prevention of variceal bleeding.

• The primary treatment for variceal hemorrhage is drug therapy with ocreotide (Sandostatin). This drug is given for 3 - 5 days after the bleeding began to reduce the risk for rebleeding.
• If these treatments do not control the bleeding, or bleeding recurs, a transjugular intrahepatic portosystemic shunt (TIPS) procedure is performed. TIPS is not useful as the first choice for stopping an initial bleeding episode or for preventing rebleeding since it poses a high risk for encephalopathy.

Another procedure, called balloon tamponade, may be used to temporarily control bleeding prior to the TIPS procedure.
Secondary Prevention. Patients who survive an episode of variceal bleeding need to be treated with drugs to prevent bleeding recurrence. Patients are prescribed either a combination of a nitrate drug [such as isosorbide (Ismo), which is used to treat angina] and a nonselective beta-blocker (propanolol or nadolol) or a beta-blocker alone. Patients are also given several sessions of endoscopic variceal ligation over the course of several months. The TIPS procedure may be recommended for patients who experience recurrent bleeding despite drug and endoscopic therapy.

Liver Transplantation• When cirrhosis progresses to end-stage liver
disease, patients may be candidates for liver transplantation. Patients with liver cancer that has not spread beyond the liver are also candidates for transplant.
• Current 5-year survival rates after liver transplantation are about 75%. Patients report improved quality of life and mental functioning after liver transplantation. Patients should seek medical centers that perform more than 50 transplants per year and produce better-than-average results.

• A scoring system called Model for End-Stage Liver Disease (MELD) is used to determine which patients are most in need of a donor liver. A MELD score predicts 3-month survival based on laboratory tests of creatinine, bilirubin, and blood-clotting time. Priority is given to patients who are most likely to die without a liver transplant.