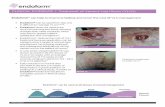
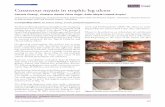
leg ulcers
-
Upload
suhail-rather -
Category
Health & Medicine
-
view
6.875 -
download
3
Transcript of leg ulcers

LEG ULCERS
Moderator:- Dr Vipin Gupta

ulcer

Causes of lower limb ulceration1. Venous insufficiency (45 -60%)
2. Arterial insufficiency (10 -20%)
3. Diabetes (15 -25%)
4. Vasculitis
5. Haematological dissease
6. Infections
7. Trauma
8. Drugs/therapy:-hydroxy urea
9. Skin conditions:- pyoderma gangrenosum, necrobiosis lipoidica
10. malignancies
11. Genetic :-prolidase deficiency, klinefelter`s syndrome

An Introduction:An Introduction:
Venous Leg UlcersVenous Leg Ulcers

• A non-healing open wound • Often at medial lower aspect of leg `gaiter region`• With or without visible varicose veins

• 45-60% of ulcers treated are venous
• 1-2% of the population above 65 (U.K.)
Venous Leg Ulcer FactsVenous Leg Ulcer Facts
• venous ulcer affect 0.2% of the population
• Average time to heal 12-30 weeks


With muscle contraction, deep veins are compressed, one way valves in deep system allow the high pressure flow to move against gravity
One way valves in perforators close to prevent pressure injury to the skin
In all patients with venous disease there is failure of these one way valves
Worsened by impairment of leg muscle function or ankle joint range of motion

Causes of venous ulcer

Risk factors

Signs and symptoms• Usually preceded by patchy erythema or discoloration of an intense
bluish red colour (capillary congestion)
• Ischemia of the skin finally leads to necrosis, often following a minor episode of trauma (scratching, small knocks, dermatitis)
• Ulcer is typically painless. Patients develop typical ischemic pain on elevation of the ulcerated leg, which is oedematous . Associated with arterial disease can ( 1/3 of cases).
• Ulcer is covered with yellowish exudate over granulation tissue
• Healing ulcers have a shallow sloping edge with healthy granulation tissue in their base and little slough. Pink lip of epithelium at the edge of ulcer is uniform and supplied by relatively uncongested capillaries (normal nail-fold and cuticle)
• Non-healing ulcer resembles severe paronychia being boggy, undermined and congested from oedema. Base is white and fibrous

• Signs:- Signs of venous hypertension are present- LDS, varicose
veins, varicose eczema or oedema An oedematous leg not responding to diuretics is a strong
clue to the diagnosis

Incompetent perforators and reflux
• Failure of venous valve (REFLUX) and poor calf muscle function leads to ambulatory venous hypertension and sustained capillary hypertension
• 60% of venous ulcer patients have isolated superficial vein insufficiency

Pathogenesis
1. Capillary stasis: `Homans` postulated that stasis of venous blood in post-thrombotic syndrome gave rise to anoxia and hence venous ulcers
2. Fibrin cuff theory: `Browse and Bermand` postulated that venous ulcer could be result of deposition of pericapillary fibrin due to leakage of fibrinogen through pericapillary spaces. fibrinogen polymerizes to form fibrin
Oxygen diffusion barrier Increase in collagen IV in and around capillary
3. White cell trapping: `Coleridge and Smith` suggested that
leukocytes may become trapped in capillaries in static blood,
obstructing the flow

4. Trapping growth factors: `Felanga and Eaglestein`
hypothesized that pericapillary fibrincuff , α-2 macroglobulin interfare
with growth factor transport
5. Multicausal model/ Maastricht model: Elevated pressures on vascular side of capillaries lead to structural changes in capillary wall
Interendothelial space broadens Collagen IV layer disintegrates Capillary wall becomes thicker
Water diffusion is effected- oedemaLarger molecules (fibrin ) escape- fibrin cuff formation α-2 macroglobulin escapes and traps TGF-β

Widened capillaries have decreased blood flow , WBC`s adhere to capillary walls , sometimes blocking circulation- microthrombi
LDS :- inflammatory response to proteins escaped into tissue , escaped leukocytes release proteolytic enzymes
Increased collagen breakdown , increased MMP1 & 2 activity, which cause plasminogen activation
Decreased fibrinolytic activity

Poor circulation decreases delivery of oxygen and nutrients, prevents removal of metabolic waste products such as carbon dioxide, and ultimately delays healing.
Blood Flow:Blood Flow:The key to The key to WoundWound HealingHealing

Diagnosis
• Clinical: Gaiter area Signs of venous hypertension Past history of venous thrombosis Past history of treatment for varicose veins Family history of venous disease
• Colour Doppler duplex USG: usually, after ulcer heals
Confirm venous reflux, superficial venous incompitance Confirm deep venous compliance

• Plethysmography: To investigate calf muscle pump function when Colour
Duplex is normal
• Skin biopsy: not indicated in venous ulcer Skin malignancy or vasculitis suspected
• Arterial disease must be excluded; ABPI Arterial duplex doppler scanning arteriography

ManagementManagement
Ist step is to assess PADIst step is to assess PAD
Check pedal pulses before compression
Use Doppler to check ABPI >0.8 (ankle/brachial press. index)
If ABI is <0.5 NO compression needs referral to vascular surgeon

Mechanical therapy

Compression bandaging Reduces venous pressure
Improves calf muscle pump function Opposing gravitational venous reflux
Improving lymph drainage Stimulates fibrinolytic activity TYPES:I. Non-elastic wraps (short stretch)
II. Elastic wraps (long stretch)
III.Stockings Graduated multilayer compression bandaging regimens capable of
sustaining pressure for 1 week should be 1st line Should exert pressure of 30 to 40 mmHg at ankle for effective
compression

Keep the pressure on: Keep the pressure on: Unna Boot Unna Boot
• A paste bandage withzinc oxide, glycerin, etc.
• Applied without tensiondistal to proximal ,below knee
• Primary dressing applied first
• Boot dries to a semirigid cast
• Changed 1-2x q week, depends on drainage

Pneumatic Compression Pneumatic Compression Pump Pump
• Inflatable boot and pumprhythmically fills with air
• Long-term use for ptsnoncompliant with othermethods
• For pts who have failedtreatment with other
compression devices

• Treatment of underlying cause of eczema: Varicose Contact allergy Contact irritant
Emollients , Steroids if inflammed
• Cleansing and debridement:1. Irrigation of ulcer with warm tap water, sterile saline
2. Debridement improves wound healing

TYPES OF DEBRIDEMENT:
I. SHARP DEBRIDEMENT:Using scalpel, scissors, curette is rapid and precise
II. AUTOLYTIC
III.ENZYMATIC DEBRIEMENT
IV.MAGGOTS
V. ULTRASOUND DEBRIDING INSTRUMENT

Advanced Cases:Advanced Cases:Maggot TherapyMaggot Therapy
• Maggots are currently one of the mosteffective means of treating ulcers with
MRSA • Specially bred fly larvae secrete enzymes to
break down dead tissue into a liquid they will ingest
• The FDA approved thistherapy in Jan, 2004.

Dressing and topical therapies Should keep ulcer moist not wet Simple ,low adherent Left undisturbed as long as possible
`strike through` of exudate to outside of the bandage is indication for change
1. Knitted viscose primary dressings + superimposed absorbent pad (secondary dressing)
2. Hydrocolloid dressing- dry sloughy wounds to reduce pain
3. Absorptive dressing (alginate, foam, hydrofibre) – highly exuding wound
4. Zinc paste bandage (unna boot)

Negative prognostic indicators
• 1. VLU: ulcer size ≥10cm2
• 2. ulcer duration ≥12 months
• 3. Presence of PAD
• 4. Greater than 50% of ulcer consisting of fibrous connective tissue

Skin and substitutes1. Autologous;
1. Split skin grafts
2. Punch grafts
3. Cultured autologous keratinocytes
2. Donor:1. Cadaver
2. Pig skin
3. Allogenic:1. Bilayered skin substitutes; allogenic keratinocytes and fibroblasts
in collagen gel (Apligraft)

microbiology
• Routine use of topical/oral antibiotics should be discouraged unless there is clinical evidence of infection:
i. Surrounding inflammation
ii. Increased pain
iii.Heavy or purulent exudate
iv.Rapid deterioration of ulcer
v. Fever Particularly if group A β-haemolytic streptococcus is
identified

Pain relief1. Compression and elevation
2. Opioids
3. Amitriptyline, gabapentin, guanethidine block- autonomic nervous system mediated deep pain
4. Quinine; night cramps

Systemic therapy
• Antibiotics:- only used if there is clear evidence of infection
• Pentoxyphylline:- Fibrinolytic Reduction in leukocyte adhesion Dose of 400 to 800mgs TDS
• Ortal enteric coated aspirin:- 300mg
• Flavonoid drugs (e.g. oxerutins)
• Daflon 500
• Stanazolol:-androgenic steroid with fibrinolytic property. Improves LDS
• Iloprost infusion

• Sodium dobesilate:- 500 mgs BD

Surgical treatment• Between 50-70 % of ulcers heal at 3 months, 80-90% by
12 months
• 50% overall recurrence rate by 5-7 yrs , mostly in post-thrombotic limbs
Surgical ligation of saphenous vein and incompetent communicating veins is `no better than` stanozolol and stockings in preventing ulcer
Various procedures used:
I. Ligation and stripping of saphenous veins
II. Compressive sclerotherapy
III.Complete extirpation of the communicating veins `feeding` the ulcer

IV- deep vein bypass
V – valvuloplasty
VI- brachial valve transplantShave therapy:
•Excision of ulcer and surrounding LDS followed by meshed split skin graft. Heals 88% of ulcers Skin grafting
•Punch grafting
•Split skin grafts
•Mesh grafts

Advanced Cases:Advanced Cases:Surgical TreatmentSurgical Treatment
• Subfascial endoscopic perforator surgery (SEPS)
• Improves healing rates, and reoccurence

Lifelong: Lifelong: Compression Compression TherapyTherapy
• After healing of ulcer,fit for custom stockings
• Remove and bathe each evening, apply moisturizer• Each morning put on
to prevent edema• Metal frame used to assist• Pt should purchase in pairs of two,
replace every 6 months

Associations and Complication of venous leg ulcer
1. General disease1. Obesity
2. Hypertension
3. Cardiovascular diseases
2. Anaemia, hypoproteinemia
3. Depression
4. Inverted foot, equinus ,calf muscle atrophy
5. Zinc depletion
6. Infections: staph. aureus, groupA β- haemolytic streptococci, pseudomonas, candida albicans
7. Contact dermatitis
8. haemorrage

9. Lymphoedema
10.Malignant change
11.Sub cutaneous calfication
12.Bone changes

Arterial ulceration

Causes


Clinical features• Frequently arise in pretibial area, foot, toes
• Severe pain is usual, as marked in small ischemic ulcers as in large ulcers
• Edge of the ulcer is sharply defined, punched out
• Base is pale, may have bare tendons

Peripheral arterial disease

Atheromatous embolism

Risk factors

management
• Risk reduction:- Smoking cessation (transdermal nicotine) Statin therapy (LDL<100 mg/dl), other lipid therapy Aspirin, clopidogrel Glycemic control Antihypertensive
• Symptom relief:- Exercise regimen Cilostazol:- platelet-aggregation inhibitors

treatmentTreatment:-assess by arterial duplex USG or AngiographyCondition is often indolent, healing only when blood supply is improved + ulcer base is excised and grafted
i.ABPI <0.5 :-immediate revascularization
ii.ABPI >0.5 but <0.85 :-modified compression, short stretch bandages with low resting pressures, intermittent pneumatic compression ?Revascularization should be considered in ulcer that do not healamputation



Clotting disorders
• Hypercoagulable disorders may cause ulceration – directly by thrombus formation in small arteries, arterioles,
capillaries, or venules
– Indirectly as a consequence of venous thrombosis
• Lab. Screening tests for clotting disorders– Activated partial thromboplastin time
– Prothrombin time
– Factor V (leiden) mutation
– Factor II (prothrombin) mutation
– Antithrombin III
– Protein C and Protein S
– Lupus anticoagulant
– Anticardiolipin

Hypertensive ulcer

Hypertensive ulcer/martorell`s ulcer• Associated with longstanding, poorly controlled
hypertension
• Female to male preponderance
• Often initiated by trauma and ischemia, failure to meet demand of repair
• CLINICAL FEATURES Preceded by small macular cyanotic lesion Bilateral superficial ulcerations over ant. aspect of leg b/w
middle and lower 1/3. livid edge is characteristic Extremely painful, alleviated by holding leg in dependent
position Normal peripheral pulses

• Pain and ulceration with livid reticulate edge but no LDS.
• Usually more proximal than venous ulcer

• BIOPSY:-
• Increased thickness of arteriolar wall with luminal narrowing by subendothelial hyaline degeneration
• Smooth muscle hyperplasia, most marked in media. Later replaced by collagen fibers
• TREATMENT:-
• Anti-hypertensives (ß-blockers avoided)
• Firm non-elastic (short-stretch) support bandage
• Leg should be placed in position to prevent oedema, not so high to promote ischemia
• smoking is to be stopped
• Excision of ulcer area with grafting advised

VASCULITIS/VASCULOPATHYMostly acute, sometimes subacute and chronic
Usually multiple
Palpable purpura is characteristic, may be polymorphous, even pustular
An irregular border, black necrosis, erythema, bluish or purple discoloration of adjacent skin are
suggestive of vasculitis

Cutaneous ulcerations is usually caused by medium sized to small vessel leucocytoclastic vasculitis
Small vessel vasculitis includeI. Cutaneous small vessel vasculitis
II. HSP
III. Wegener`s granulomatosis
IV. Essential mixed cryoglobulinemia
V. Rheumatoid nodules
Medium vessel vasculitis includeI. Classical PAN
I. Cutaneous form
II. Kawasaki disease

Lab screening tests for vasculitisi. Urine routine for proteinuria, haematuria, cylindruria
ii. Routine and immunohistopathology of skin
iii. ESR, haemoglobin, differential blood count, LFT, RFT
iv. ANA, RF
v. Complement C4, circulating immune complexes
vi. Paraproteins, immunoglobulin fractions
vii. ANCA
viii.Serological tests and cultures for underlying infections

treatment
• Conservative management
• Immunosuppressive therapy:- Persistent or progressive ulceration due to histologically confirmed vasculitis

Rheumatoid Disease• CAUSES
• Poor joint movement- impairs calf muscle pump/ imobility increases risk of DVT
• True ``Rheumatoid Ulcer`` because of rheumatoid arteritis
• Ulceration of rheumatoid nodule
• CLINICAL FEATURES
• Ulcer in gaiter region, sloughy base with poor granulation tissue
• D/D venous ulcer:-
• No surrounding LDS and other signs of venous ulcer
• Positive RF
• Normal Doppler pressure and venous duplex studies

OTHER AUTOIMMUNE DISEASES:-•Lupus erythematosus•Felty`s syndrome- associated with skin ulcers
1. Rheumatoid arthritis
2. Splenomegaly
3. neutropenia
•Still`s disease•Polyostotic fibrous dysplasia•s/c or muscular fibrosis
SARCOIDOSIS

• LIVEDO RETICULARIS• Fixed but broken pattern of mottling
1. Vasculitis
2. Intravascular thrombosis 1. Cryoproteniemia
2. Antiphospholipid syndrome
3. Sneddon`s syndrome

LIVEDOID VASCULOPATHY
• Occlusive vasculopathy limited to gaiter region extending down to the dorsum of foot
• Hyalinization and thrombosis of the microvasculature with scarce inflammatory infiltrate
• Ulcers are small painful, heal with ivory white scars (Atrophie Blanche)
• TREATMENT
• Immunosupression not effective, treatment of hypercoagulable state

Pyoderma gangrenosum
• Rare, non infectious, neutrophilic dermatosis commonly associated with underlying disease
• Classic/Ulcerative PG variant usually presents with painful ulcers ,commonly on legs (70%)
• Clinical features:
presents as solitory or multiple small, tender, red-blue papules, plaques or pustules that evolve into painful ulcers with charesteristic violaceous undermined edges
There may be granulation tissue, necrosis or purulent exudate at the ulcer base
Pathergy occurs in 25% Healing usually occurs with atrophic cribriform scar


causes
• Gastrointestinal- ulcerative colitis, crohns, collagenous colitis,gastritis, gastroduodenal ulcer
• Arthritides:- Rheumatoid arthritis, Seronegative arthritis, osteoarthritis
• Haematological:- Leukaemias, myelofibrosis, myelodysplastic syndromes, paraprotenemia,waldenstrom`s macroglobulinemia
• Hepatic:- chronic active hepatitis ,PBC, sclerosing cholingitis
• Other vasculitides, collagen vascular and related disorders

• Acne and related disorders• Autoimmune:- thyroid disease, DM
• Drugs:- CSF, gefinib, interferon, PTU, isotretinoin
• Solid organ tumors:- colon pancreas, breast, bronchus, carcinoid
• Miscellaneous:- sarcoidosis, HIV, hep. C, chorinic lung disease

Diagnostic criteria

Diagnosis

treatment
For early or mild lesions:- Wet compresses, hydrophilic occlusive dressings, antimicrobial agents
and topical corticosteroid Topical tacrolimus- mild early lesions Intralesional corticosteroids Benzoyl peroxide, 5-aminosalicylic acid, nitrogen mustard,
cromoglycate, PDGF, intralesional ciclosporin
For more severe/resistant to topical therapy Corticosteroids are mainstay of treatment Dapsone , low dose colchicine Ciclosporine, cyclophosphamide, chlorambucil, intravenous tacrolimus,
mycophenolate mofetil and thalidomide TNF-α inhibitors:- etanercept, adalimumab, infliximab Plasmapharesis, IVIg

Necrobiosis lipoidica• Age of onset is around 30 years, women three times more
cases
• Prevalence of 0.3 to 3.0 % in patients with diabetes
• Other than Diabetes (75%) and GA other reported associations include rheumatologic, endocrine, and haematologic disorders
• Presents as one to several sharply demarcated yellow-brown plaques on the anterior pretibial region, have violaceous, irregular border that may be raised and indurated.
• Clinical course is indolent spontaneous remission in 20%
• Ulceration is most severe complication (13 to 35%) ,

• Treatment: steroids, aspirin, topical retenoids , topical PUVA,fumaric acid esters, cyclosporine, surgical excision

tumors

Marjolin`s ulcer

• Marjolin's ulcer is a rare and often aggressive cutaneous malignancy (scc 75-96%) that arises in previously traumatized or chronically inflamed skin, particularly after burns
• Several theories including the toxin, chronic irritation, traumatic epithelial elements implantation, heredity, immunologic privileged site, co-carcinogen, ultraviolet rays, initiation and promotion and environmental and genetic interaction theories have been reported to explain the malignant transformation
• The latency period from the time of injury to the onset of malignant transformation averages 36 years

• Marjolin's ulcers are very aggressive tumors that necessitate a well thought out treatment plan to optimize care and assure patient survival. Early diagnosis and prompt surgical intervention is mandatory

HAEMATOLOGICAL DISORDERS
• CAUSESo Sickle cell anaemiao Hereditary spherocytosiso Other haemolytic diseaseso Myloproliferative diseases
o Cell size compromises capillary perfusiono If thrombosis developso Treatment (hydroxycarbamide)

HYDROXYCARBAMIDE
• Leg ulceration was reported in 9% of patients taking this drug in a prospective study
• Indicated for CML, CLL , polycythemia vera, essential thrombocythaemia, sickle cell anemia
• Ulcers develop after at least 1 year of treatment in dose dependent fashion
• Ulcers are located on or near the malleoli in ¾ of cases. Are very painful, resemble atrophie blanche
• Treatment:- after withdrawal of hydroxycarbamide 85% of ulcers heal spontaneously in 1-9 months
• Debridement, f/b split skin graft in non-healing ulcers

STEROID ULCER
CAUSES:-
• I/L steroid injections particularly over areas with impoverished blood supply
• Strong topical corticosteroid applied to venous or other ulcer of lower leg
CLINICAL FEATURE:-
• Indolent ulcer with characteristic greyish slough

INFECTIONS1. Primary uncomplicated pyococcal ulceration
2. Meleney`s ulcer
3. Tuberculous ulcer
4. Other mycobacterial infections
5. Leprosy
6. Tertiary syphilis
7. Yaws
8. `desert` or `veldt` sore
9. Tropical ulcer
10. Leishmaniasis
11. Glanders, tularemia, brucellosis, cat scratch fever

Primary pyococcal ulceration• Some microorganisms like β-haemolytic Streptococcus
pyogens can cause tissue necrosis
• Causes wide range of clinical symptoms– erysipelas
– punched out ulcers (Ecthyma)
– Deep cellulitis
– Fascitis necroticans, sepsis and multiorgan failure
• Treatment:-– Immediate high dose antibiotics
– Special attention to possibility of combined infection with Staph. aureus and anaerobic species

Meleney`s gangrene/ necrotizing fascitis
• It is a progressive bacterial synergistic gangrene
• infection located in the deep fascia, with secondary necrosis of the subcutaneous tissues
• Because of gas-forming organisms, subcutaneous air is classically described

treatment

Bazin`s disease/Tuberculous ulcer
• Usually present as subcutaneous nodules and plaques on calves in young adult female
• Gradually involve overlying skin, often with ulceration Ulcer has irregular bluish and friable undermined edges.
Generally multiple ,bilaterally symmetrical
• There is generally evidence of pulmonary or skeletal tuberculosis
• Develop in cold weather initially
• TREATMENT:-• ATT

Tropical/phagedenic ulcer• Synergistic bacterial infection by at least two organisms
fusobacterium species (F. ulcerans) and spirochete or some anaerobe
• Common hot and humid tropical regions, clustering of cases
CLINICAL FEATURES
• Most lesions follow minor trauma on exposed parts such as legs
• Papule rapidly breaks down to form sharply defined ulcer, most often with undermined edges
• Painful , constitutional symptoms are usual
• No lymphadenopathy

• Management– Rest, limb elevation– Treatment of underlying cause, malnutrition– Penicillins and/or metronidazole

PROLIDASE DEFICIENCY
• Autosomal Recessive condition caused by defect in prolidase gene on chromosome. 19q13.11
• Prolidase/iminodipeptidase degrades collagen .
• Cleaves dipeptides with hydroxyproline/proline at C-terminus
• Deficiency results in impaired recycling of proline residues
CLINICAL FEATURES:-
• Presents before 12yrs, multisystem disorder, primarily involves skin (85%)

• Recurrent, multiple ulcers of lower extremities are seen in over 50%
• Fragility of skin, easy breakdown, usually preceded by purpura or bruising
• Fine scarring, telangiectasis and eczematous lesions may be feature

• Characteristic facies:- hypertelorism, saddle nose in mentally retarded
• Other associations: dental caries, splenomegaly, hyperextensibility of ligaments, osteoporosis, respiratory infections, corneal opacities, amblyopia and optic atrophy
DIAGNOSIS: Iminodipeptiduria >5 mmol/24 hour Decreased prolidase activity in blood Thrombocytopenia, hypergammaglobulinemia, iron
deficiency anaemia

TREATMENT:Refractory to all forms of treatment, including graft rejectionOral and intravenous antibiotics in case of secondary infectionAscorbic acid and manganese (cofactors of prolidase)Diphenylhydantoin5% glycine and 5% proline ointmentApheresis exchangeTopical and systemic growth hormone

• Presenter :- suhail rather