Indications for Removable Partials Kennedy Classification ...€¦ · Major Connectors 1. A/P...
Transcript of Indications for Removable Partials Kennedy Classification ...€¦ · Major Connectors 1. A/P...

1
Ronni A. Schnell, DMD, MAGDBoston University Henry M Goldman School of Dental Medicine
February 8, 2014
University of AlabamaSchool of Dentistry Alumni Association
ALUMNI WEEKEND
Ronni A. Schnell, DMD, MAGDBoston University Henry M Goldman School of Dental Medicine
February 8, 2014
Retention or Rotation? The Art & Science of
Removable Cast Partial Denture Design © 2014
University of AlabamaSchool of Dentistry Alumni Association
ALUMNI WEEKEND 2014
Re-Introduction to
Cast Partial Dentures
Indications for Removable Partials
1. Distal Extensions2. Long Tooth Borne Spans3. Severe Bone Loss4. Recent Extractions5. High Caries Index6. Poor Crown/Root Ratio7. Cost
3
2
1
Kennedy Classificationof Partially Edentulous Arches
• Classified by:The most posterior spaceto be restored by the partial
• Modified by:The number of remaining spacesto be restored by the partial
Vertical Rotationalmovement movement
Distal ExtensionTooth Borne
Partial Denture Movement?
ROTATI
ON
?
Rotation & Classification
• All Class I partials rotate• All Class II partials rotate• Some Class III partials rotate• Some Class IV partials rotate

2
Important Facts #1-4
1. Rotation Causes Torque2.Torque causes tooth loss3.Tipped teeth are more likely to
torque4.Lone standing teeth are more likely
to torque
Teeth most likely to tipIncisors
Lone-Standingteeth
NeighboringTeeth haveIndependentRoot systems
Parts of a cast partial framework
1. Major connector2. Minor connector3. Meshwork4. Finish line5. Clasp6. Rest7. Tissue stop
6
3
41
2
5
5
14
3
2
6
7 7
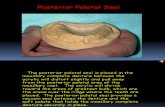
A/P Palatal Bars Broad Palatal Strap Full Palatal Coverage
Horseshoe Lingual Bar Lingual Blanket
Major Connectors
A
P
Anterior/Posterior Palatal Bars
• Most common• Most rigid• Anterior bar:
– broad & thin– between rugae– 6mm from gingival margin
• Posterior bar:– narrow & thick– ½ tear shaped– thickest at posterior– ant to jx of hard & soft palates
• No right < between bars• Bars ┴ to median suture
Broad Palatal Strap
• Thickness for rigidity may cause speech problem
• Anterior border as far posterior as possible
• Posterior border ┴ to median suture
• Used only when few teeth missing
Full Palatal Coverage• Ideal for Kennedy Class I• Includes Post Palatal Seal• May be all metal:
– good thermal conductor– decr bulk– no Post Dam– not adjustable
Horseshoe
• Rotates horizontally• Best with tooth borne• Best with many guide
planes• Gaggers last resort• Inoperable torus @ jx of
hard & soft palates• Thickness for rigidity may
cause speech problems
Lingual Bar• Most common• Relieved from tissue• ½ pear shape w/ bulk inferiorly• Superior margin 3mm from FGM• Bar is 3mm wide• Requires a min of 6mm fold depth
during tongue fx

3
Lingual Blanket• Indications include:
– High lingual frenum– Perio splinting– Past experience
• Contacts teeth, but not gingiva• Requires rest seats on all lower
anterior• Inferior border at depth compatible
with tongue movement
Major Connectors
1. A/P Palatal Bars: most rigid, 1st choice-max2. Broad Palatal Strap: thick, small case3. Full Palatal Coverage: upper Class I4. Horseshoe: inoperable torus @ H/S palate5. Lingual Bar: most comfortable, 1st choice-mand6. Lingual Blanket: shallow floor, splinting
A/P Palatal Bars Broad Palatal Strap Full Palatal Coverage
Horseshoe
TT
T
T
Metal must never covera palatal torus
Lingual Bar Lingual Blanket
TT T T
Metal must never cover Mandibular tori……if they cannot be avoided they must be removed
STEELE’S FACING
•Acrylic facing•Metal backing•Cemented or cured
Recommended for small anterior space
•Metal backing•Slot projection
STEELE’S FACING
TUBE TOOTH
•Single Posterior•Hollow ground tooth•Nail head projection
Recommended for small posterior space
Abutments
• Definition: any tooth which contacts the metal framework
• Primary (1º) abutment: has a clasp• Secondary (2º) abutment: has no clasp
The Direct Retainer (Clasp)
1. Rest2. Retainer3. Bracer
1
2
2
1
3
1
3

4
Type I vs Type II• Occlusal origin• From minor connector• Crosses bulge• 1/3rd retentive• B or L retention
• Gingival origin• From meshwork• Doesn’t cross bulge• All retentive• B retention only
“Suprabulge” “Infrabulge”
approach arm
Type I Direct Retainers Cast “C” clasp Wire “C” clasp (Combo)
Wireis 3Xmore flexiblethancast
XOther “Overwrought” Options
Likely to break
Likely to wedge
Likely to wedge
Two rests req’d
Too rigid
Extra-bracing
Type II Direct Retainers
approach arm
tube tooth
Note that both approach arm & tube tooth can occupy the same space.
Narrower spaces require longer approach arms
2mm
3mm Approach Arms
3mm 3mm 3mm 3mm
OK OK OK N/A N/A
Tooth = tissue Tissue undercut Tissue ledge Tissue undercut Severe tiltbelow 3mm above 3mm
Acceptable locations Unacceptable locations Severe tipping
Severe tissue undercut
Shallowfold
Approach Arms

5
Approach arm misuse
Reverse Skipping teeth Molars
Approach Arm Misuse
NO LINGUAL or PALATALapproach arm arms
NO approach arms positioned DISTALLY
NO DOUBLEapproach arms or SKIPPING of teeth
Inappropriate Uses
For Approach Arms
xx
NO approach arms on MOLARS
NO DOUBLEapproach arms or SKIPPING of teeth
Inappropriate Uses
For Approach Arms
xx
NO approach arms approaching from the mesial
Inappropriate Uses
For Approach ArmsImportant Fact #5
ClaspsCauseTorque
Clasp LocationTo reduce rotational or tipping forces,place clasps as gingivally as possible
Occlusal 1/3rd
Gingival 1/3rd
Effect of height of contour on Clasp location
Occlusal 1/3rd
Gingival 1/3rd
Effect of height of contour on Clasp location Important Fact #6
Lowering Clasps ReducesTorque

6
Bracing preventstooth movement
as clasp crosses bulge
Bracing (Reciprocation)
Absence of Bracingcauses tooth movement
Important Fact #7
BracingReducesTorque
2
1
3
Bracing Options1. Arm2. Blanket3. 2 Minor
Connectors
Bracing effectiveness must be evaluated from the occlusal
3 Bracing Options
Bracer shouldbe directlyoppositeRetainer
Heights of contour may be mismatched
idealideal
Bracing effectiveness must also be evaluated from the proximal
Important Fact #8
Lowering Bracer ReducesTorque
Rests
Cingulum rests
Occlusal rests
Functions of Rests
• Preventing cervical movement• Preventing rotational movement• Maintaining or establishing occlusion• Maintaining relationship of clasp to abutment
Rests may cause tooth movement

7
Important Fact #9
RestsCauseTorque
Rest Seats
Cingulum
MLMO
DO
Occlusal
Functions of Rest Seats
• Directing occlusal force along tooth long axiseven without opposing tooth present
• Decreasing torque on abutment• Preventing hyperocclusion of rest
Important Fact #10
Rest Seats ReduceTorque
During rotation Direct retainers = LeversThe Rest determines the type of lever
Important Fact #11
LeversCauseTorque
E E E
F F F
R R R
R R RE E E
Clasps as 1st Class Levers
C Bar RPI
E E E
F F F
F F F
R R R
R R RE E E
Clasps as 2nd Class LeversC Bar RPI
UP DOWN UP DOWN UP DOWN
DOWN DOWN DOWN DOWN DOWN DOWN
E E E
F F F
F F F
R R R
R R RE E E
1st Class Lever
2nd Class Lever

8
Important Fact #12
2nd Class Levers ReduceTorque
The rest closest to the rotation = the lever
One rest or two?The Indirect RetainerDuring rotationIndirect retainers seat &prevent lifting of the distal extension
seatingprevents lifting
SeatingPrevents liftingX
Axis of Rotation
During rotationIndirect retainers= “Anti-levers”
Lifting Lifting Lifting
Seating Seating Seating Seating
Indirect Retention
As the denture base lifts away from tissue,an opposing rest seats against tooth
lifting
seating
The effectiveness of indirect retention decreasesas the distance from the axis of rotation decreases
Indirect Retention helps keep the distal extension base down:1. Locate the most posterior rests on each side2. Connect them to form the axis of rotation3. Locate the midpoint of the axis4. Locate the tooth perpendicular to the midpoint5. Place a rest on that tooth or move laterally
to the nearest acceptable tooth
Important Fact #13
Indirect Retention ReducesTorque
O-R-A-C-G-U-B-TA partial denture design system
Occlusal analysis
Rotation analysis
Abutment selection
Clasp selection
Guide plane survey
Undercut survey
Bracing survey
Tripodization
Our“hypothesis”
Testing our“hypothesis”

9
OCCLUSAL ANALYSIS
1. Plane Correction?2. Extrusion Potential?3. Overbite Problem?4. Spaces Selected for PD?
O-R-A-C-G-U-B-T
1. Plane correction?2. Extrusion potential?3. Overbite problem?4. Spaces selected for PD?
2/3 RMP
Plane correction?
• √ same arch• √ opposing arch• √ retromolar pad• √ radiograph
?
Overbite problem?
Steele’s FacingSteele’s Facingsolution
Anterior overbite may result in Incisal Guidance
ROTATION ANALYSIS
1. Spaces to be restored by the partial?2. Size of those spaces?3. Support of those spaces?
O-R-A-C-G-U-B-T
Spaces selected for PD? Spaces selected for PD?
Kennedy Classification
1. Bilateral Distal Extension (+/- Mods)2. Unilateral Distal Extension (+/- Mods)3. Unilateral Tooth Borne (+/- Mods)4. Bilateral Tooth Borne (No Mods,X Midline)
O-R-A-C-G-U-B-T

10
X
X
+/-
+/-
Tooth borne
Tooth borne
Distal ext.
Distal ext.
Tooth borne
Tooth borne
Tooth borne
Tooth borne
ABUTMENT SELECTION1. As many guide planes as possible2. As far apart as possible3. Symmetry where possible4. No incisors5. No lone-standing premolars as 1º abut.6. No lone canine/molar if prox. contact poss.7. Extrusion prevention 8. Indirect retention9. Esthetics OK if design OK
O-R-A-C-G-U-B-T
ABUTMENT SELECTION1. As many guide planes as possible2. As far apart as possible3. Symmetry where possible4. No incisors5. No lone-standing premolars as 1º abut.6. No lone canine/molar if prox. contact poss.7. Extrusion prevention 8. Indirect retention9. Esthetics OK if design OK
O-R-A-C-G-U-B-T
1. As many guide planes as possible…exposed proximal surfaces2. As far apart as possible3. Symmetry where possible4. No incisors5. No lone-standing premolars as 1º abut.6. No lone canine/molar if prox. contact poss.7. Extrusion prevention 8. Indirect retention9. Esthetics OK if design OK
Adjacent to edentulous
spaces
NB- Guide Planes &Anterior Teeth:
Incisors and themesials of Caninesare not usedbecause of esthetic reasons
1. As many guide planes as possible…exposed proximal surfaces2. As far apart as possible3. Symmetry where possible4. No incisors5. No lone-standing premolars as 1º abut.6. No lone canine/molar if prox. contact poss.7. Extrusion prevention 8. Indirect retention9. Esthetics OK if design OK
1. As many guide planes as possible2. As far apart as possible…for stability3. Symmetry where possible4. No incisors5. No lone-standing premolars as 1º abut.6. No lone canine/molar if prox. contact poss.7. Extrusion prevention 8. Indirect retention9. Esthetics OK if design OK
X
1. As many guide planes as possible2. As far apart as possible…for stability3. Symmetry where possible4. No incisors5. No lone-standing premolars as 1º abut.6. No lone canine/molar if prox. contact poss.7. Extrusion prevention 8. Indirect retention9. Esthetics OK if design OK
1. As many guide planes as possible2. As far apart as possible3. Symmetry where possible…for comfort4. No incisors5. No lone-standing premolars as 1º abut.6. No lone canine/molar if prox. contact poss.7. Extrusion prevention 8. Indirect retention9. Esthetics OK if design OK
1. As many guide planes as possible2. As far apart as possible3. Symmetry where possible4. No incisors…to prevent tipping & speech problems5. No lone-standing premolars as 1º abut.6. No lone canine/molar if prox. contact poss.7. Extrusion prevention 8. Indirect retention9. Esthetics OK if design OK


12
1. As many guide planes as possible2. As far apart as possible3. Symmetry where possible4. No incisors5. No lone-standing premolars as 1º6. No lone canine/molar if prox. contact poss.7. Extrusion prevention 8. Indirect retention9. Esthetics OK if design OK…evaluate “high smile line”
CLASP SELECTION
1. Type I vs. Type II Clasps 2. Rotating vs. Non-rotating Partials3. Class I vs. Class II Levers
O-R-A-C-G-U-B-T
Non-rotating PD vs. Rotating PD
• Moves occluso-gingivally• Does not cause torque• Uses simplest clasp
• Moves antero-posteriorly• Causes torque• Must protect all abutments
Non-rotating Partial:C = clasp of choice2nd choice = any
Rotating Partial:RPI = clasp of choice2nd choice = Combo
Rotating Partial:RPI = clasp of choice2nd choice = Combo
wire
Class I vs. Class II Levers
CHANGING LEVER
CHANGING EFFECT ON TOOTH
UP DOWN UP DOWN UP DOWN
DOWN DOWN DOWN DOWN DOWN DOWN
E E E
F F F
F F F
R R R
R R RE E E
Rotating Clasps in Function:
Biting vs. Lifting36 psi vs. gravity

13
●
CDO RESTMB TIP
BITE
●
CDO RESTMB TIP
LIFT●
CDO RESTMB TIP
●
Protects tooth at ridge’s expense by “disengaging” from tooth
RPIMO RESTMidB TIP
●
RPIMO RESTMidB TIP
●
RPACombo*MO RESTMB TIP
*Wire clasp is up to 3 times more flexible than a cast clasp
●
Protects tooth at its own expense by flexing
*Wire clasp is up to 3 times more flexible than a cast clasp
RPACombo*MO RESTMB TIP
●
RPACombo*MO RESTMB TIP
●
BARMO RESTDB TIP

14
●
Protects tooth by having less contact than a C
BARMO RESTDB TIP
●
BARMO RESTDB TIP
●
RPAC*MO RESTMB TIP
* Cast clasp is up to 3 times less flexible than a wire clasp
●
Protects only by using a Class II lever
RPAC*MO RESTMB TIP ●
RPAC*MO RESTMB TIP ●
RPIMO RESTMidB TIP
1st Choice: has potential to disengage from tooth
●
RPAComboMO RESTMB TIP
2nd Choice: if wire, is more flexible than a cast clasp
●
BARMO RESTDB TIP
3rd Choice: is smaller than C, so reduces force on tooth
●
RPACMO RESTMB TIP
4th Choice: if cast, is less flexible than a wire clasp & is larger than a bar clasp

15
RPI
RPA
RPI vsRPA (Combo)
Breaks contact butuses Ridge as Fulcrum
Remains in contact butWire absorbs Stress
CHANGING CLASP SIZE
CHANGING LEVERCHANGING LEVER
CLASP SELECTION
1. Non-rotating? C = Clasp of Choice2nd Choice = any
2. Rotating? RPI = Clasp of Choice2nd Choice = Combo
3. Lever? 2nd Class Lever
O-R-A-C-G-U-B-T
IV.IV.
Non-rotating vs. Rotating PD• Moves occluso-gingivally• Does not cause torque• “C” is simplest,
but any may be usedif “C” cannot
• Moves antero-posteriorly• Causes torque• Must protect all abutments
@ ridge’s expense… RPI@ clasp’s expense… Combo
w/ 2nd class lever
Rotation requires protection!
Design Priorities
#1: Protect Bone if teeth strong#2: Protect Teeth if bone strong#3: If Teeth weak, treat as DE w/ RPI#4: If Bone weak, treat as DE w/ Combo
GUIDE PLANE SURVEY
1. Proximal Surfaces2. Occlusal 1/3rd
3. Disk Parallel to Path
O-R-A-C-G-U-B-T

16
incorrect
correct
Anterior tissue undercut…
…requires “Tail Down” tilt
↑ Tail down tilt mayrequire diskingof teethto create a newGuide Plane
Guide Plane
Guide “Point”
Important Fact #14
Guide Planes ReduceTorque
UNDERCUT SURVEY
1. Facial or Lingual Surfaces (+/- tissue)2. Gingival 1/3rd
3. Dimple Flat Surface → .01 (.02 → .03)4. Disk Non-parallel to lower Type I clasp5. Disk Parallel to lower Type II clasp
O-R-A-C-G-U-B-TClasp Location
To reduce rotational or tipping forces,place clasps as gingivally as possible
↑ Tail down tilt mayrequire “dimpling”of teeth to createa new undercut
Guide Plane
Guide “Point”
Loss of undercut
Creating an Undercut
To create a .01 undercut, dimple a flat area by .01
To create a .02 undercut, dimple a .01 undercut by .01
To create a .03 undercut, dimple a 02 undercut by .01

17
Lowering a Clasp orDecreasing Bulge
• Disk Non-Parallelto lower a Type I clasp
• Disk Parallelto lower a Type II clasp
Type I vs Type II
Lowering a Type I Clasp – Disk Non-Parallel
Lowering a Type I Clasp – Disk Parallel
Lowering a Type II Clasp – Disk Parallel
If a bulbous tooth createsa tissue undercut thatcannot be eliminated bychanging the tilt,the tooth may need
enamoplasty
Disk Parallel for a Type II clasp w/ a straight bur
?
•Path on proximal•View from proximal•Cut only on facial•Use tapered bur forType I clasp
Disk Non-parallel for a Type Iclasp w/ a tapered bur
BRACING SURVEY
1. Arm, Blanket or 2 Minor connector(more than 180º around circumference)
2. Gingival 1/3rd
3. Disk Non-parallel to Lower Ht. of Contour
O-R-A-C-G-U-B-T
3 Bracing Types:
●
BRACINGARM
May torque the tooth
●

18
● ●
BRACINGMINORCONNECTORS
Reduce torque – with less metal contact
●
●
Bracer shouldbe directlyoppositeRetainerideal
ideal
Teeth may be tilted or plastied to lowerthe height of contour.
Disk non-parallel to pathto lower the height of contour.
TRIPODIZATION
1. On 3 sides of cast2. Records A/P & Lateral Tilts3. Must be included in Crowned abutments
O-R-A-C-G-U-B-T
Tripodization
Partials by the Numbers1. Guide Planes:
as ____ as possible2. Clasps:
as ___ * as possibleas ____ as possibleas ____ as possible
3. Rests: as ____ as possible
4. Major connectors: as ____ as possible
* Ante’s Rule
References• Kratochvil, F.J.: Influence of occlusal rest position and clasp design on
movement of abutment teeth. J. Prosth. Dent. 13:114, 1963.
• Krol A.J. Clasp Design for Extension Base Removable Partial Dentures. J Prosthet Dent 29:408‐415, 1973.
• Berg, T., Jr.: Symposium on Common Failures in Removable Partial Prosthodontics, I‐Bar Myth and Countermyth, Dental Clinics of NA, Vol. 23, No. 1 Jan 1979 & Vol. 28 No. 2 April 1984
• Argerakis, G. P.,: Symposium on Semiprecision Attachments in Removable Partial Dentures, Functional Forces with Removable Partial Dentures, Dental Clinics of NA, Vol. 29, No. 1, Jan 1985.
• Carr, McGivney and Brown McCracken’s Removable Partial Prosthodontics, 12th ed. C.V. Mosby (2011)
• Brien, N.: Conception et trace des Prostheses Partielles Amovibles, 1st ed. Prostho (1996).