Imaging of the neck part ii
-
Upload
wafik-ebrahim -
Category
Health & Medicine
-
view
1.558 -
download
1
Transcript of Imaging of the neck part ii

IMAGING OF THE NECK
DR/ Wafik Ebrahim, MDAssistant Professor of Rradiodiagnosis
Faculty of MedicineAlazhar University

Imaging modalities: CT MRI US: Plain X ray and conventional studies. Isotope scan. Angiography.
Multiplanner capability allows good anatomical description. Vascularity of lesion. Consistency of the lesion.

CT scan: IV contrast is important for better
cracterization of the mass. Start from superior orbital rim to apex of
the lung. Extension to carina may be accomplished according to suspected disease.
To avoid artifacts of dental filling, planes are parallel to skull base down to alveolar ridge then parallel to body of mandible.

MRI: Use dedicated surface colis better than
cervical coil for better resolution. T1 in the 3 planes followed by T2 in planes
best depict the lesion. 4-6mm thickness with 1-2mm gap. IV contrast is not routine due to inherent
tissue characterization of MRI. If IV contrast is used, fat sat sequences
are added.

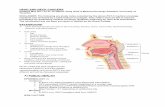
Neck triangles :

Lymph nodes: Enlarged lymph node is the most
common neck mass in adults. About 300 nodes are located in the head
and neck. They are divided in groups described by the anatomist Rouviere.
20-40 years—lymphoma>40 years----metastasis
6. Submental 1. Occipital7. Sublingual 2. Mastoid
8. Retropharyngeal 3. Parotid
9. Anterior cervical 4. Facial
10. Lateral cervical. 5. Submandibular
The first 6 form lymphoid collar at junction between head and neck

Lymph nodes groups:

Lymph nodes: NORMAL nodes are oval with fatty sinus. Size criteria for benign nodes:
< 1.5cm for IJC near angle of mouth.< 0.8cm for retropharyngeal nodes.< 1cm for the rest of groups.
Pathological signs: Central necrosis (DD fatty hilum “peripheral
fat density”)Matting.Infiltrated surrounding fat planes.
We consider the short axis
of nodes.

Lymph nodes stations:
IA & IB submental and
submandibular
II IJC posterior to PB
digastric:A: around IJV (any
direction)
B: posterior to IJV with
fat planes separation III: Between hyoid bone and inferior cricoid margin
V: PCS: SAC:A: skull base to cricoid.B: cricoid to clavicle.
IV cricoid to clavicle
VI: visceral s. nodes (hyoid to manubr)
VII: Super. Mediast.

LN: Other groups include:
Parotid group: Retropharyngeal group.Facial group:

LN

PMS: Anatomy

Pharyngeal mucosal space (PMS) Psudomass:
Asymmetry of fossa of Rosenmuller (lateral pharyngeal recesses) may result from inflammatory debris or asymmetry in the amount of lymphoid tissue thereby giving the impression of a mass.
A mass is ruled out when: 1. The adjoining soft tissue planes in the PPS and
RPS are maintained.2. The nasopharyngeal mucosa is clinically intact.3. The collapsed recess opens when rescanning
by CT scan is used during the Valvalva maneuver.

Adenoid hypertrophy: It represents normal immunolgical
activity that starts at age of 2-3 years and regresses during adolescence.
Absence of adenoid tissue in young children should alert for immune disease.
Smoking can produce adenoid hypertrophy in adults.

Adenoid: Hypertrophied
adenoid should be confined to mucosal space with intact underlying fascia.

Thornwaldt cyst:
CT: Hypodense lesion:CECT: May be wall enhancement. •MRI:
• TI: intermediate to high according to protein contents.
• T2: High signal• +C: may be wallenhancement.

Tonsillar abscess:
Cellulitis versus abscess: As a rule in cervical infection: Thickening of overlying skin or mucosa, smudging of the fat planes (or linear opacities), thickening of adjacent muscles, and enhancement of fascial planes WITHOUT fluid collection denote cellulitis but if WITH fluid seen it means abscess. LOOK CAREFULLY TO FAT PLANES BY ADUSTING WINDOW AND LEVEL.

Tonsillar abscess:

Tonsillar abscess: DD:
Tonsillar retntion cyst. Lymphoid hyperplasia.Retropharyngeal abscess.Benign mixed tumor of salivary gland.Tonsillar SCCA.NHL.

Retention cyst:

Retention cyst:

Benign mixed tumors of minor salivary gland tumors (BMT):
NO invasion of surrounding structures

MST
CT:Isodense mass lesion.Minimally enhancing.Necrosis and calcifications may be seen.Bone remodeling (benign longstanding
feature).

BMTPEARL
SHAPED
NO PALATE DESTRUCTION
RIGHT MASTOIDITIS NO muscle
invasion
T1: isointense to muscleT2: variable mostly hyperIf calcified, foci of low signal. T1+C: intense enhancement

BMT: Age: 30-60 years. But may be any age
even in neonate. DD:
Thyroglossal duct cyst in foramen coecom.Retention cyst. SCCA.Malignant salivary gland tumor (poorly
defined).

Minor salivary gland malignancy: Rare aggressive tumor (1/10 of minor
salivary glandstumors. Occurs in adults.

Minor salivary gland malignancy: Pathology: adenoid cystic carcinoma
and mucoepidermoid carcinoma. Rarely complicates pleomorphic
adenoma. Treatment is wide surgical excision.

Minor salivary gland malignancy:

Minor salivary gland malignancy: MRI:
T1 WI: Isoointense mass.T2: Variable signal.
Low signal (more cellular poorer prognosis).High signal (less cellular better prognosis).
T1+C enhancing with infiltrating margin. Add fat sat sequence for better assessment of
perineural spread).

Minor salivary gland malignancy:
T1+C T2
PPS
RPS:LN

Minor salivary gland malignancy:
Perineural spread CN V3 through F. Ovale

Minor salivary gland malignancy: DD:
Benign mixed salivary gland tumors (well defined and regular non-invasive margin).
SCCA (usually with malignant adenopathy).Lymphoma (usually with associated non-
necrotic nodes).

Squamous cell carcinoma “SCCA” Nasopharynx SCCA arising from nasopharynx has
three histological subtypes:1. Keratinizing SCCA (WHO type 1).2. Non-Keratinizing SCCA (WHO type 2).3. Undifferentiated SCCA (WHO type 3).
Size: Usually multiple CMs when discovered.

SCCA Nasopharynx: Spread
Anterior: Nasal cavity then ptrygopalatine fossa
Anteroinferior to levator velli paltini ms with eustachian T. dysfunction
Lateral to PPS then to MS
(then foramen ovale up)
Posterior to RPS to PVS
and spineInferior to oropharynx
Superior to skull base

SCCA Nasopharynx: Spread Lymphatic spread: usually seen at
presentation: retropharyngeal nodes, jagular nodes and spinal accsssory nodes.
Blood spread (10% at time of presentation): to bone > lung > liver. )

SCCA: Imaging: CT scan: Isodense
poorly enhancing masslook also at bone
window to assess skull base.
Show the mass and extension.
Look at skull base foramina

MRI: Low T1 signal and internediate to high T2 signal with intense postcontrast enhancement.
Add fat sat. for Better depiction of bone marrow invasion.Better evaluation of perineural spread.

SCCA: Imaging: NSCCA starts usually in the fossa of
Rusenmuller and has same signal and density to normal mucosa. First signs are:Asymmetry of nasopharyngeal mucosa (regarding
cautions said before), attention is applied to:○ Fat stripe between levator and tensor velli palatine
muscles. Obliteration mass. ○ Middle ear collection warning sign.○ Associated lymphadenopathy especially
retropharyngeal nodes.

SCCA: Imaging: Fat stripe between levator and tensor velli
palatine muscles. Obliteration mass.


Staging:

DD Benign mixed tumor (non invasive). Malignant salivary tumor (may be
indistinguishable). . NHL.

Squampos cell carcinoma Oropharynx: Location:
Lingual tonsils (posterior to circumvillate papillae). The mass is more invasive with difficult early detection because it has same density and signal like the lymphoid tissue of normal lingual tonsils.
Palatine tonsils and facuial arches.

Lingual tonsil SCCA spread pattern: Anterior: root of tongue, subliungal space (neurovascular bundle) and floor of mouth.
Posterolateral: palatine tonsils and tonsillar pillars.
Inferior to supraglottic larynx and preepiglottic
fossa .

Lingual tonsils SCCA :

MRI

Palatine tonsils SCCA: Tonsils > Anterior pillar } posterior pillar. Asymmetry of tonsils may be seen
normally however mass is suspected when there is obliteration of fat planes in PPS and / or associated lymph node enlargement.
Mass may spread to PPS, masticator space (foramen ovale) or carotid space.

Palatine tonsils SCCA:

Palatine tonsils SCCA:

Non-Hodjkin lymphoma:

NHL

Non-Hodjkin lymphoma:
Benign mixed salivary tumor
was suspected

Parotid space: Anatomic considerations:

Parotid space :

Parotid space: Acute parotitis Bacterial:
Suppurative infection abscess.Usually unilateral.
Viral:75% bilateral though one is earlier involve.May be associated other sialadenitis.
Calcular induced:Stone impacted in the duct. Unilateral

Acute parotitis: imaging : CT: Cuts taken parallel to mandible to avoid artifacts of
dental filling. Enlarged ill-defined hyper dense gland with
smudging of adjacent fat planes. Cystic changes denote abscess formation. search for a stone in the duct.
MRI:Diffuse gland enlargement: Liquefaction means abscess.

Acute parotitis: imaging :

Acute parotitis: imaging :

Sjogren disease:
Bilateral parotid enlargement with multiple intraglandular cysts and occasional calcifications.
Diffuse disease is usual but sometimes single localized disease: DD from tumor.
Age: 50-70 YJuvenile type < 20 Y mostly cures at puberty.
Higher incidence in females.

Sjogren disease: Stages:
Early: the glands may look normal.Intermediate: Multiple small intraparotid
cysts.Late: gland destruction with variable sized
cysts. At any stage there may be solid masses
related to lymphocytes aggregations. Calcifications are common.

Sjogren disease:

Benign mixed tumors: Parotid
Small lesion: is sharply demarcated ovoid intraparotid mass with homogeneous enhancement.
Large mass >2cm is lobulated heterogeneously enhancing.
Deep lobe mass is pear shaped pushing PPS medially. .
Usually unilateral mass.Age> 40 years.

Benign mixed tumors: Parotid
Facial nerve palsy is rare.

Warthin Tumor:
Sharply marginated mass mostly in parotid tail.
Parenchymal inhomogeneity is a rule with cystic components. Cyst with solid nodule is also seen.
Multicentericity and bilaterality: 20%.

Warthin Tumor:Inhomogeneity
is a ruleCyst with solid
nodule

Malignant tumors: Mucoepidermoid carcinoma:
Low grade: well circumscribed mass lesion.High grade: infiltrative heterogeneous mass.
Adenoid cystic carcinoma: Low grade: well circumscribed mass lesion.High grade: infiltrative heterogeneous mass.
Lymphoma: may be primary or secondary with associated multiple bilateral lymph nodes enlargement.

Mucoepidermoid carcnoma
Adenoid cystic carcinoma

Carotid space:
SHN IHN

CS: Pathology: Arterial disease:
Thrombosis, dissection aneurysm or pseudoaneurysm.
Venous disease:Thrombosis or thrombophlibitis.
Benign tumors:Glomus jagulare and glomus vegale paragangliomas.Carotid body paraganglioma.CN 9-11 Schowanoma and neurofibroma.Jugular foramen meningioma.
Malignant tumorsSpreading SCCA or lymphoma.

CS
Kissing ICAs Ectatic ,medially migrating ICA (RPS)

IJV thrombosis

Paragangliomas (glomus tumors): They are neoplasms of neural crest cell origin
that arise within the adventitial layer of blood vessels at multiple sites in the head and neck.
They include the middle ear (glomus tyrnpanicum, parapharyngeal space (glomus jugulare) and larynx.
The two most common paragangliomas to present as a neck massCarotid body tumor (carotid bifurcation)Glomus vagale (along the nodosa ganglion of the
vagus nerve).

Paragangliomas The constant features:
CT: intense progressive enhancement.MRI: pepper (flow void blood vessels) and
salt (foci of hemorrhage) appearance on T1 WI.
Mass in the neck showing signal void blood vessel signal should alert for paraganglioma (considering anatomical location).

Paragangliomas: Carotid body tumor arise juxtahyoid and
splays the ICA and ECA.
Multiplicity is common (10-30%)

Paragangliomas: Glomus vagale arises in the SHN and
displaces ICA anteromedially and IJV posterolaterally.

Neurogenic tumors: Vagal Neurofibroma and Schwanomas:
without history of neurofibromatosis they could not be differentiated.
They have same location like glomus vagale displacing the ICA anteromedially and the IJV posteromedially.
They show any pattern of enhancement from non to avid enhancement.
DD from paraganglioma by absence of flow void and pattern of enhancement.

Vagal Schwanoma

Vagal neurofibroma

Masticator space :

Benign masticator space hypertrophy:
Smooth enlargement of the muscles of mastication.
May be up to 3 times volume increase.
May be bilateral with asymmetry.

Motor denervation: Denervation of muscles supplied by
mandibular division of trigeminal nerve (only motor branch).
The involved muscles are:Muscles of mastication:
○ Masseter, Ptrygoid, Temporalis muscles.Others supplied by V3 nerve:
○ Mylohyoid and anterior belly of digastric muscle.
○ Tensor veli palatini and tensor tympani.

Motor denervation: stages Acute stage: (<1 month):
Muscle enlargement with edema and enhancement.
Subacute stage: (<12- 20 months);Fatty replacement with starting atrophy. Enhancement may be noted.
Chronic: (>12-20 months):Fatty replacement with volume loss.


Motor denervation

Motor denervation

Masticator space infection: Mostly secondary to molar tooth
infection. Same like all infections in head and
neck:CellulitisAbscess formation.

Masticator space infection:

Mandibular nerve schwanoma:
May involve the mandibular nerve through its course from Meckel’s cave and downward.
May involve mandibular nerve branch including inferior alveolar and mental nerves.
It widens the foramen if it is site of involvement.

Schwanoma: Imaging CT:
Isodense ovoid smooth mass lesion with occasional cystic changes.
Mild to moderate homogeneous or heterogeneous enhancement (due to cystic changes).
Muscle denervation changes may be noted.

Scwanoma: CT

Schwanoma: MRI:
T1: isointense mass. Hypointense cystic areas may be seen. Nemorrhagic bright foci may be also noted.
T2: Iso to hyperintense. Cystic changes may be also senen.
T1+C: variable enhancement.

MRI

Chondrosarcoma: Malignant tumor of cartilage. Soft tissue mass in masticator space close to
mandible with bone erosion and variable calcification pattern.
CT: Soft tissue density with calcification:
○ Low grade crescents and rings.○ High grade amorphous or no calcifications.
Heterogeneous peripheral enhancement.

CT

MRI T1:
Homogeneous intermediate signal. Cartilage matrix or calcifications make it heterogeneous.
Bone marrow infiltration (best seen on T1). T2:
High signal is characteristic. Calcifications make it heterogeneous.
T1+C: enhancement increases with grade.

MRI

Mandibular nerve perineural infiltration: Can occur at any point from mental
foramen to root entery zone of CN V on lateral pons.

Perineural spread: CT:
Widened neural foramen of nerve bony canal.Nerve thickening and enhancement.
MRI:Nerve thickening with low T1 signal, high T2 signal
and intense postcontrast enhancement. Infiltration of masticator space with involvement of
the fat planes especially the perineural fat. Infiltration of fat planes below foramen ovale.Evidence of denervation of the muscles in the
space.
Be aware from enhancing vasa vasorum and ptrygoid plexus of veins. Here, enhancement around dark nerve.


Retropharyngeal space:
SHN IHN

RPS

Non-abscess fluid: May be reactive to nearby pathology:
IJV thrombosis.Longus colli tendinosis.Neck surgery.
Early infection pre-abscess. General principle:
Smooth expansion of the space without enhancement.

DD from RPS abscess:

Abscess formation (RPS): < 6years or immunocompromised. Like abscess elsewhere. Tense fluid collection distending the
space with variable enhancement.

RPS: Lymphadenopathy: Benign: smooth homogeneous < 0.8cm. Malignant: oval to round mass with
occasional enhancement and possible necrosis.

VISCRAL SPACE:

Hashimoto thyroiditis: Chronic autoimmune-mediated lymphocytic
inflammation of thyroid gland. Non-specific enlargement of the gland without
calcification or necrosis. CT scan:
Diffuse non-specific enlargement. Hypodensity is typical finding.
MRI: Non-specific finding with high signal during T2WI.

US Real time:
Early Stages: Non-specific: ○ Enlarged Heterogeneous Hypoechoic gland.○ Hypoechoic foci may be seen (micronodulation).
Late: small hypoechoic heterogenous fibrotic gland. Uncommon: focal disease within normal gland. Color Doppler:
Early: increased vascularity.Late: absent blood flow signal.


Multinodular goiter: Enlarged gland with multiple nodules. The gland is well marginated. Calcification, necrosis, cystic degeneration
and hemorrhage may be seen. US shows cystic and solid nodules
Hemorrhage may be seen as high echogenecities CT shows cystic and solid nodules with Ca.
Hemorrhage may be seen as high densities .



Thyroid adenoma: Thyroid adenoma: (true neoplasm with
complete capsule): Single well defined intrathyroid mass within normal gland.
Adenomatous polyp: adenomatous hyperplasia with incomplete capsule: less distinct and may be multiple.


Malignant thyroid mass: Types:
Differentiated carcinoma:○ Papillary (70%).○ Follicular and carcinoma (10%).
Aggressive tumors:○ Medullary carcinoma (5%).○ Anaplastic carcinoma (5%).
Others including lymphoma and metastasis (10%).

Thyroid malignancy: Unfortunately the appearance of thyroid
malignancy is usually non-specific. Nodules with irregular margin or mass invading
surrounding structures should alert for malignancy.
60% of malignant nodules have irregular border and also 45% of benign nodules have irregular border.
Calcifications:Microcalcifications malignancyEgg shell calcifications benignity.

Thyroid malignancy: Role of imaging:
Evaluation of thyroid capsule integrity.Detection of infiltration of surrounding
structures. Identification of malignant lymph nodes.

Differentiated carcinoma: Invasive mass with
thyroid capsular invasion and metastatic lymph nodes.
Hypoechoic mostly solid tumor but cystic changes are seen in follicular type

Malignant thyroid:
Medullary carcinoma Anaplastic carcinoma

Parathyroid gland: Adenoma
It is well defined small mass in expected location. Associated hyperparathyroidism.


Posterior cervical space:

Spinal accessory schwanoma:
Oblong well defined mass along the course of spinal accessory nerve.